Anemic Syndrome and White Blood Cells Disorders
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Viral Hepatitis with Acute Hemoglobinuria
22 Case Report Viral Hepatitis with Acute Hemoglobinuria Jagabandhu Ghosh1 Joydeep Ghosh2 1 Department of Paediatrics, I.P.G.M.E.R and S.S.K.M Hospital, Kolkata, Address for correspondence Jagabandhu Ghosh, MD (PAED), Ushashi West Bengal, India Housing Society, 245 Vivekananda Road, Kolkata 700006, India 2 Department of Biotechnology, Heritage Institute of Technology, (e-mail: [email protected]). Kolkata, West Bengal, India J Pediatr Infect Dis 2015;10:22–24. Abstract A 7-year-old male child presented with moderate degree fever, yellowish discoloration of eyes and urine. Examination on admission revealed severe anemia, jaundice, hepato- Keywords megaly, and splenomegaly. On the day following admission, the child showed evidence ► hepatitis of blackish discoloration of urine. The diagnosis was established as viral A hepatitis with ► G6PD glucose-6-phosphate dehydrogenase (G6PD) deficiency. The child recovered with ► viral supportive therapy. We suggest that either universal immunization against hepatitis ► hemolysis A, or routine newborn screening for G6PD deficiency, could prevent the serious ► intravascular morbidity or mortality that can occur when these two conditions coexist. Introduction of eyes, and urine for the past 5 days before admission. There was no history of hematemesis, melena, or any other bleed- Acute viral hepatitis A is widely prevalent in India.1 Viral ing, swelling of body, convulsion, and drug ingestion just hepatitis is the leading of acute hepatitis in children in our before present illness or any previous blood transfusion. His country, and hepatitis A is the most common type of viral urine volume was satisfactory. On examination, the child was hepatitis. Hepatitis A does not commonly present with severe deeply icteric, severely anemic, and drowsy. -

• Cytosis: O Neutrophilia: Defined As an Increase in the Neutrophilic Count in the Peripheral Blood Above Reference Range for Age
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS-UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD NONNEOPLASTIC DISEASES OF THE WHITE BLOOD CELLS • There are five major types of WBCs in the blood: neutrophils, lymphocytes, eosinophils, basophils and monocytes. • The normal function of the white blood cells depends on a tight regulation of their count and their function. Therefore, disease develops if there is a derangement of the cells count or function, it takes one of the following forms: o Cytosis: increase in the number of circulating cells above reference range. (Note: leukocytosis means an increase in the WBC count, neutrophilia means increase in the neutrophilic count, lymphocytosis means increase in the lymphocytic count, monocytosis means increase in the monocytic count, basophilia means increase in the basophilic count and eosinophilia means in crease in the eosinophilic count). o Cytopenia: decrease in the number of circulating cells below reference range. (Note: neutropenia means decreased neutrophils, lymphocytopenia, or simply lymphopenia, means decrease in lymphocytes, monocytopenia means decrease in monocytes, eosinopenia means decrease in eosinophils, and basopenia means decrease in basophils). o Abnormal or absent function • Cytosis: o Neutrophilia: defined as an increase in the neutrophilic count in the peripheral blood above reference range for age. o Causes: bacterial infection is the most common and most important etiology. Tissue necrosis in cases of burns or trauma and medications such as epinephrine and corticosteroids are also additional causes for neutrophilia. § Some physiologic conditions can lead to neutrophilia such as stress, smoking and pregnancy. o Pathophysiology: neutrophils are present in the blood in two populations: circulating and marginal (meaning neutrophils stuck to the vessel wall). -

The Lower Urinary Tract & Male Reproductive System
Chapter 21 Hematopathology Nam Deuk Kim, Ph.D. Pusan National University 1 Contents I. Red blood cells II. Hemostasis III. White blood cells IV. Disorders of the lymphopoietic system V. Spleen VI. Thymus 2 THE HEMATOPOIETIC SYSTEM Composition of Human Blood Blood • Transports oxygen, nutrients, hormones, leukocytes (white cells), red cells, platelets and antibodies to tissues in the body and carbon dioxide and other waste products of cell metabolism to the excretory organs of the body • Volume of blood: Represents about 8% of total body weight • approximately 5 quarts, but it varies according to size of individual (5 liters in women; 5.5 liters in men) • Almost half of the blood consists of cellular elements suspended in plasma (viscous fluid) 3 4 Hemopoiesis Cellular differentiation and maturation of the lymphoid and myeloid components of the hematopoietic system. Only the precursor cells (blasts and maturing cells) are identifiable by light microscopic evaluation of the bone marrow. BFU = burst-forming unit; CFU = colony-forming unit (Ba = basophils; E = erythroid; Eo = eosinophils; G = polymorphonuclear leukocytes; GM = granulocyte-monocyte; M = monocyte/macrophages; Meg = megakaryocytic); EPO = erythropoietin; Gm-CSF = granulocyte-macrophage colony-stimulating factor; IL = interleukin; NK = natural killer; SCF = stem cell factor; TPO = thrombopoietin. 5 Composition of Human Blood • All blood cells arise from precursor cells within the bone marrow, called stem cells • These undergo further differentiation to form red cells, white cells, -
Hematology Unit Lab 1 Review Material
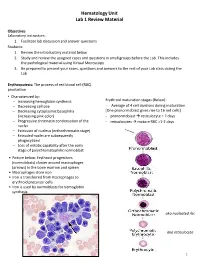
Hematology Unit Lab 1 Review Material Objectives Laboratory instructors: 1. Facilitate lab discussion and answer questions Students: 1. Review the introductory material below 2. Study and review the assigned cases and questions in small groups before the Lab. This includes the pathological material using Virtual Microscopy 3. Be prepared to present your cases, questions and answers to the rest of your Lab class during the Lab Erythropoiesis: The process of red blood cell (RBC) production • Characterized by: − Increasing hemoglobin synthesis Erythroid maturation stages (Below): − Decreasing cell size - Average of 4 cell divisions during maturation − Decreasing cytoplasmic basophilia [One pronormoblast gives rise to 16 red cells] (increasing pink color) - pronormoblast → reticulocyte = 7 days − Progressive chromatin condensation of the - reticulocytes → mature RBC =1-2 days nuclei − Extrusion of nucleus (orthochromatic stage) − Extruded nuclei are subsequently phagocytized − Loss of mitotic capability after the early stage of polychromatophilic normoblast • Picture below: Erythroid progenitors (normoblasts) cluster around macrophages (arrows) in the bone marrow and spleen • Macrophages store iron • Iron is transferred from macrophages to erythroid precursor cells • Iron is used by normoblasts for hemoglobin synthesis aka nucleated rbc aka reticulocyte 1 Mature Red Blood Cell 7-8 microns; round / ovoid biconcave disc with orange-red cytoplasm, no RNA, no nucleus; survives ~120 days in circulation Classification of Anemia by Morphology 1. -

Hemophagocytic Lymphohistiocytosis in a Child with Sickle Cell Disease
Hematology & Transfusion International Journal Case Report Open Access Hemophagocytic lymphohistiocytosis in a child with sickle cell disease Keywords: hemophagocytic lymphohistiocytosis, FHL, EBV, hemoglobin S, sickle cell disease, X-ray Volume 6 Issue 5 - 2018 Introduction Walaa Shoman,1 Yasmine El Chazli,2 Asmaa Elsharkawy,2 Neveen Mikhael,3 Akram Hemophagocytic lymphohistiocytosis (HLH) is a life-threatening deghaidy,3 Abeer Al-Battashi,4 Yasser Wali2 hyper-inflammatory syndrome which represents the extreme end of 1Department of Pediatrics, Immunology/Rheumatology unit, a severe uncontrolled hyperinflammatory reaction that can occur in Alexandria University, Egypt many underlying conditions.1 HLH can be divided into primary and 2Department of Pediatrics, Hematology/Oncology unit, secondary HLH. Primary HLH is caused by gene mutation, either at Alexandria University, Egypt 3 one of the Familial HLH (FHL) loci or in a gene responsible for one Department of Clinical pathology, Alexandria University, Egypt 4Department of Child Health, Royal Hospital, Oman of several immunodeficiency syndromes.2 The most common form of secondary HLH is infection associated HLH. Infectious triggers Correspondence: Yasser Wali, Department of Pediatrics, include viruses (as EBV, cytomegalovirus, HHV8, HIV), bacteria (as Hematology/Oncology unit, Alexandria University, Egypt, mycobacteria, mycoplasma), parasites (as leishmania, plasmodium), Email [email protected] 3,4 and fungi (as candida, cryptococcus). Sickle cell disease (SCD) Received: September 02, 2018 | Published: September 27, and its variants are genetic disorders resulting from the presence 2018 of a mutated form of hemoglobin, hemoglobin S (HbS), which can be detected by hemoglobin electrophoresis. SCD is suggested by a high-grade unremitting fever, grunting, marked pallor, jaundice, the typical clinical picture of chronic hemolytic anemia and vaso- and marked re-enlargement of both liver and spleen despite improved occlusive crisis.5,6 We present a case of HLH in an Egyptian boy who chest condition and radiogram. -

Hereditary Spherocytosis with Gilbert's Syndrome
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-ISSN: 2279-0853, p-ISSN: 2279-0861.Volume 20, Issue 4 Ser.6 (April. 2021), PP 25-28 www.iosrjournals.org Hereditary Spherocytosis with Gilbert’s Syndrome – a case report. Dr Deepan Panneerselvam Intern, Department of Internal Medicine. Dr Thabuna Sivaprakasam Intern, Department of Internal Medicine. Dr Raja sekar PGY2 Internal Medicine Resident. Dr Govindarajulu Ethirajulu Chief, Department of Internal Medicine. Government Kilpauk Medical College and Hospital. Abstract: A 23 year old previously diagnosed female with Gilbert’s syndrome on treatment with Prednisone, presented with a lower respiratory tract infection for the past 4 days with additional complaints of significant lethargy and fatigue, palpitation and intermittent yellowish discolouration of sclera since 9 years old. The patient’s mother and elder sister also had similar history of intermittent jaundice. Routine investigations of the patient revealed normal values except a hemoglobin level of 6.0 g/dl, HCT of 19.5%, MCV of 75.6 fL, serum total bilirubin of 6.3 mg/dl ( Direct: 1.3mgdl, Indirect: 5.0 mg/dl ). This made us suspect another basic hematologic abnormality that contributed to such elevated indirect bilirubin levels. Further investigations revealed a peripheral smear with moderate microcytic hypochromic anemia, anisopoikilocytosis, leucopenia and a reticulocyte count of 2.3%, negative Direct coombs test and a serum LDH of 345U/L. Ultrasound sound abdomen revealed multiple calculi in gall bladder largest measuring 3mm and splenomegaly. Peripheral smear was repeated only to reveal a dimorphic blood picture with eosinophilia, normocytic normochromic anemia with a few fragmented RBCs and spherocytes. -

Laboratory Approach to Anemia Laboratory Approach to Anemia
DOI: 10.5772/intechopen.70359 Provisional chapter Chapter 12 Laboratory Approach to Anemia Laboratory Approach to Anemia Ebru Dündar Yenilmez and Abdullah Tuli Ebru Dündar Yenilmez and Abdullah Tuli Additional information is available at the end of the chapter Additional information is available at the end of the chapter http://dx.doi.org/10.5772/intechopen.70359 Abstract Anemia is a major cause of morbidity and mortality worldwide and can be defined as a decreased quantity of circulating red blood cells (RBCs). The epidemiological studies suggested that one-third of the world’s population is affected with anemia. Anemia is not a disease, but it is instead the sign of an underlying basic pathological process. However, the sign may function as a compass in the search for the cause. Therefore, the prediag- nosis revealed by thorough investigation of this sign should be supported by laboratory parameters according to the underlying pathological process. We expect that this review will provide guidance to clinicians with findings and laboratory tests that can be followed from the initial stage in the anemia search. Keywords: anemia, complete blood count, red blood cell indices, reticulocyte 1. Introduction Anemia, the meaning of which in Greek is “without blood,” is a relatively common sign and symptom of various medical conditions. Anemia is defined as a significant decrease in the count of total erythrocyte [red blood cell (RBC)] mass, although this definition is rarely used in clinical settings. According to the World Health Organization, anemia is a condition in which the number of red blood cells (RBCs, and consequently their oxygen-carrying capacity) is insufficient to meet the body’s physiologic needs [1, 2]. -

Complete Blood Count in Primary Care
Complete Blood Count in Primary Care bpac nz better medicine Editorial Team bpacnz Tony Fraser 10 George Street Professor Murray Tilyard PO Box 6032, Dunedin Clinical Advisory Group phone 03 477 5418 Dr Dave Colquhoun Michele Cray free fax 0800 bpac nz Dr Rosemary Ikram www.bpac.org.nz Dr Peter Jensen Dr Cam Kyle Dr Chris Leathart Dr Lynn McBain Associate Professor Jim Reid Dr David Reith Professor Murray Tilyard Programme Development Team Noni Allison Rachael Clarke Rebecca Didham Terry Ehau Peter Ellison Dr Malcolm Kendall-Smith Dr Anne Marie Tangney Dr Trevor Walker Dr Sharyn Willis Dave Woods Report Development Team Justine Broadley Todd Gillies Lana Johnson Web Gordon Smith Design Michael Crawford Management and Administration Kaye Baldwin Tony Fraser Kyla Letman Professor Murray Tilyard Distribution Zane Lindon Lyn Thomlinson Colleen Witchall All information is intended for use by competent health care professionals and should be utilised in conjunction with © May 2008 pertinent clinical data. Contents Key points/purpose 2 Introduction 2 Background ▪ Haematopoiesis - Cell development 3 ▪ Limitations of reference ranges for the CBC 4 ▪ Borderline abnormal results must be interpreted in clinical context 4 ▪ History and clinical examination 4 White Cells ▪ Neutrophils 5 ▪ Lymphocytes 9 ▪ Monocytes 11 ▪ Basophils 12 ▪ Eosinophils 12 ▪ Platelets 13 Haemoglobin and red cell indices ▪ Low haemoglobin 15 ▪ Microcytic anaemia 15 ▪ Normocytic anaemia 16 ▪ Macrocytic anaemia 17 ▪ High haemoglobin 17 ▪ Other red cell indices 18 Summary Table 19 Glossary 20 This resource is a consensus document, developed with haematology and general practice input. We would like to thank: Dr Liam Fernyhough, Haematologist, Canterbury Health Laboratories Dr Chris Leathart, GP, Christchurch Dr Edward Theakston, Haematologist, Diagnostic Medlab Ltd We would like to acknowledge their advice, expertise and valuable feedback on this document. -

Hemolytic Anemia Presenting As Hemoglobinuria from Intentional Paradichlorobenzene Mothball Ingestion
Hemolytic Anemia from Intentional ParadichlorobenzeneCASE Mothball REPORT Ingestion Hemolytic Anemia Presenting as Hemoglobinuria from Intentional Paradichlorobenzene Mothball Ingestion Mary Ondinee U. Manalo,1 Cherie Grace G. Quingking2 and Carissa Paz C.Dioquino2 1Department of Medicine, College of Medicine and Philippine General Hospital, University of the Philippines Manila 2National Poison Management and Control Center, University of the Philippines-Philippine General Hospital less acutely toxic of the two. However, like naphthalene, it has also been known to induce hemolytic anemia because it possesses one benzene ring.1 We report a case of a man who intentionally ingested three mothballs made of paradicholorobenzene who experienced severe hemolytic anemia that necessitated blood transfusion. Case A 24-year-old male inmate from Manila was admitted for persistent vomiting three days after ingestion of three crushed mothballs. Three days prior to admission, the patient intentionally swallowed three crushed mothballs. After an hour, he experienced nausea and vague abdominal pain. A day prior to admission, he presented with persistent vomiting and passed out dark stools. Eight hours prior to admission, Introduction vomiting became more frequent and was now associated Mothballs could be made of naphthalene, with coffee-ground material. Abdominal pain became more paradichlorobenzene, or camphor. Differentiation among intense as well. He was then brought to the Emergency mothballs is difficult because they may have similar odors Room of the Philippine General Hospital for consultation. and are all white, crystalline solids at room temperature. The patient presented at the emergency room awake but Paradichlorobenzene is commonly found here in the weak-looking, tachypneic but with otherwise stable vital Philippines as a component of toilet deodorant blocks, but signs. -

432 Medicine Team Leaders 3:C
Reviewed By: Done By: Naif Aleid Abdulhameed Alsaawy Abdulrahman AlZahrani COLOR GUIDE: • Females' Notes • Males' Notes • Important • Additional 432MedicineTeam Anemia Objectives: (not given) General Outline Microcytic-hypochromic anaemias Normocytic-normochromic Morphology anaemias Macrocytic- normochromic anaemias Dyshaemopoietic anaemia Classification (deficiencies impairing development) Decrease red cell production Hypoproliferative anaemias Anemia (BM failure ): Haemolytic anaemia Etioilogy Acute post haemorrhagic anaemia DilutIonal anaemia 1 432MedicineTeam Anemia Introduction: Blood formation: 1. Intrauterine life: Blood cells are formed in the liver and spleen up to the fifth months. After 5th month: bone marrow shares in the formation of these cells. 2. After birth: Formation of these cells will be restricted to the bone morrow. 3. Adulthood The active bone morrow will be restricted to axial skeleton: flat bones, vertebrae, ribs, sternum and ilia. Some extension to the proximal ends of long bone mainly femur. Extramedullary haemopoiesis: When demand for blood formation is increased the active red BM extends into the shafts of the long bones. The spleen and liver will regain their ability to produce blood elements when bone morrow is affected by some diseases. Blood Constituents: Organelles (formed elements): o RBCs o WBCs o Thrombocytes Fluid components: plasma in which the above elements are suspended and contain fibrinogen. 2 432MedicineTeam Anemia Erythrocytopoiesis Normal erythrocytopoiesis depends on: 1. Healthy BM: normal stem cells and architecture. 2. Regulatory hormones: GPO, Androgen thyroxin, cortisol and ACT. 3. Nutritional elements: Protein (high biological value), 4. Minerals (Iron, copper, zinc, selenium) 5. Vitamins (B, Folic acid, vit. C) Anaemia: Reduction of O2 carrying capacity of the blood with inadequate O2 supply to tissues. -

TNF-Independent Development of Transient Anemia of Chronic
0023-6837/03/8312-1743$03.00/0 LABORATORY INVESTIGATION Vol. 83, No. 12, p. 1743, 2003 Copyright © 2003 by The United States and Canadian Academy of Pathology, Inc. Printed in U.S.A. TNF-Independent Development of Transient Anemia of Chronic Disease in a Mouse Model of Protracted Septic Peritonitis Thomas Schubert, Bernd Echtenacher, Ferdinand Hofstädter, and Daniela N. Männel Department of Pathology (TS, BE, FH, DNM), University of Regensburg, Regensburg, Germany SUMMARY: TNF is considered one of the inflammatory cytokines and contributes mainly to the generation of anemia of chronic disease (ACD). In nude mice TNF has been reported to impair iron metabolism and erythropoiesis, leading to anemia with a low serum iron and preserved iron stores. In this work, we established a murine model for ACD based on sublethal cecal ligation and puncture (CLP) with ensuing protracted peritonitis. Starting on Day 3 after CLP, a severe protracted depression of erythropoiesis in the bone marrow was noted. Two weeks after CLP, we observed a moderate normochromic anemia, low serum iron concentration, and preserved iron stores consistent with transient ACD. To determine whether TNF contributes to the development of ACD in vivo, we neutralized TNF after CLP shortly before and during the phase of most severe bone marrow depression to prevent anemia. Additionally, we studied TNF-deficient mice undergoing CLP. Two weeks after CLP, we determined red blood count, hemoglobin concentration, hematocrit, serum iron concentration, and iron stores in spleens of wild-type mice, TNF-deficient mice, and mice after neutralization of TNF. Neutralization of TNF after CLP could not prevent mice from contracting anemia. -

Pub 100-04 Medicare Claims Processing
Department of Health & CMS Manual System Human Services (DHHS) Pub 100-04 Medicare Claims Centers for Medicare & Processing Medicaid Services (CMS) Transmittal 990 Date: JUNE 23, 2006 Change Request 5142 Subject: Medicare Contractor Annual Update of the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) I. SUMMARY OF CHANGES: This instruction is CMS' annual reminder to the contractors of the ICD-9-CM update that is effective for the dates of service on and after October 1, 2006, as well as discharges on or after October 1, 2006 for institutional providers. New / Revised Material Effective Date: October 1, 2006 Implementation Date: October 2, 2006 Disclaimer for manual changes only: The revision date and transmittal number apply only to red italicized material. Any other material was previously published and remains unchanged. However, if this revision contains a table of contents, you will receive the new/revised information only, and not the entire table of contents. II. CHANGES IN MANUAL INSTRUCTIONS: (N/A if manual is not updated) R=REVISED, N=NEW, D=DELETED-Only One Per Row. R/N/D Chapter / Section / Subsection / Title N/A III. FUNDING: No additional funding will be provided by CMS; Contractor activities are to be carried out within their FY 2006 operating budgets. IV. ATTACHMENTS: Recurring Update Notification *Unless otherwise specified, the effective date is the date of service. Attachment – Recurring Update Notification Pub. 100-04 Transmittal: 990 Date: June 23, 2006 Change Request 5142 SUBJECT: Medicare Contractor Annual Update of the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) I.