Laboratory Approach to Anemia Laboratory Approach to Anemia
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Viral Hepatitis with Acute Hemoglobinuria
22 Case Report Viral Hepatitis with Acute Hemoglobinuria Jagabandhu Ghosh1 Joydeep Ghosh2 1 Department of Paediatrics, I.P.G.M.E.R and S.S.K.M Hospital, Kolkata, Address for correspondence Jagabandhu Ghosh, MD (PAED), Ushashi West Bengal, India Housing Society, 245 Vivekananda Road, Kolkata 700006, India 2 Department of Biotechnology, Heritage Institute of Technology, (e-mail: [email protected]). Kolkata, West Bengal, India J Pediatr Infect Dis 2015;10:22–24. Abstract A 7-year-old male child presented with moderate degree fever, yellowish discoloration of eyes and urine. Examination on admission revealed severe anemia, jaundice, hepato- Keywords megaly, and splenomegaly. On the day following admission, the child showed evidence ► hepatitis of blackish discoloration of urine. The diagnosis was established as viral A hepatitis with ► G6PD glucose-6-phosphate dehydrogenase (G6PD) deficiency. The child recovered with ► viral supportive therapy. We suggest that either universal immunization against hepatitis ► hemolysis A, or routine newborn screening for G6PD deficiency, could prevent the serious ► intravascular morbidity or mortality that can occur when these two conditions coexist. Introduction of eyes, and urine for the past 5 days before admission. There was no history of hematemesis, melena, or any other bleed- Acute viral hepatitis A is widely prevalent in India.1 Viral ing, swelling of body, convulsion, and drug ingestion just hepatitis is the leading of acute hepatitis in children in our before present illness or any previous blood transfusion. His country, and hepatitis A is the most common type of viral urine volume was satisfactory. On examination, the child was hepatitis. Hepatitis A does not commonly present with severe deeply icteric, severely anemic, and drowsy. -

Kawasaki Disease with Glucose-6-Phosphate Dehydrogenase Deficiency, Case Report
Saudi Pharmaceutical Journal (2014) xxx, xxx–xxx King Saud University Saudi Pharmaceutical Journal www.ksu.edu.sa www.sciencedirect.com CASE REPORT Kawasaki disease with Glucose-6-Phosphate Dehydrogenase deficiency, case report Hesham Radi Obeidat a,*, Sahar Al-Dossary b, Abdulsalam Asseri a a Pharmacy Department, Saad Specialist Hospital, Alkhobar 31952, Saudi Arabia b Pediatric and Neonatology Department, Saad Specialist Hospital, Alkhobar 31952, Saudi Arabia Received 28 August 2014; accepted 11 November 2014 KEYWORDS Abstract Kawasaki disease (KD) is an acute, self-limited vasculitis of unknown etiology that Kawasaki disease; occurs predominantly in infants and children younger than 5 years of age. Coronary artery abnor- G6PD; malities are the most serious complication. Aspirin Based on the literatures infusion of Intravenous Immunoglobulin of 2 g/kg and a high dose of oral aspirin up to 100 mg/kg/day are the standard treatment for Kawasaki disease in the acute stage, and should be followed by antiplatelet dose of aspirin for thrombocytosis. Glucose-6-Phos- phate Dehydrogenase (G6PD) deficiency is an inherited X-linked hereditary disorder, and aspirin can induce hemolysis in patients with G6PD deficiency. We report a case of a 5 year and 8 month old male with KD and G6PD deficiency. ª 2014 The Authors. Production and hosting by Elsevier B.V. on behalf of King Saud University. This is an open access article under the CC BY-NC-ND license (http://creativecommons.org/licenses/by-nc-nd/3.0/). 1. Introduction genetic predisposition or infectious agents are likely to be the cause. Kawasaki disease was first described in 1967 by Tomisaku Recently, guidelines were published by the American Heart Kawasaki and has replaced acute rheumatic fever as the lead- Association (AHA) to aid in the diagnosis and management of ing cause of acquired heart disease among children in devel- Kawasaki disease. -

Hemolytic Anemia Caused by Hereditary Pyruvate Kinase Deficiency in a West Highland White Terrier Dog
Arch Med Vet 44, 195-200 (2012) COMMUNICATION Hemolytic anemia caused by hereditary pyruvate kinase deficiency in a West Highland White Terrier dog Anemia hemolítica causada por la deficiencia de piruvato quinasa hereditaria en un perro West Highland White Terrier NRC Hlavaca, LA Lacerdaa*, FO Conradob, PS Hünninga, M Seibertc, FHD Gonzálezd, U Gigere aPostgraduate Program in Veterinary Sciences, Universidade Federal Rio Grande do Sul, Porto Alegre, RS, Brasil. bVeterinary Clinic Pathology, Universidade Federal Rio Grande do Sul, Porto Alegre, RS, Brasil. cClinic Pathology, PetLab Ltda, Porto Alegre, Brasil. dDepartment of Veterinary Clinic Pathology, Faculty of Veterinary, Universidade Federal Rio Grande do Sul, Porto Alegre, RS, Brasil. eLaboratory of Genetic Diseases, University of Pennsilvania, Philadelphia, United States. RESUMEN La deficiencia de piruvato quinasa (PK) es un desorden hemolítico autosómico recesivo descrito en perros y gatos. La piruvato quinasa es una de las enzimas regulatorias esenciales de la glicólisis anaeróbica, la deficiencia de esta enzima causa una destrucción prematura de los eritrocitos. El presente es un estudio de caso y relata los hallazgos clínicos y paraclínicos en un perro brasileño de la raza West Highland White Terrier (WHWT) con historia de debilidad e intolerancia al ejercicio. El paciente presentaba mucosas pálidas, anemia hemolítica bastante regenerativa y osteoclerosis. La deficiencia de PK fue confirmada a través de una prueba de ADN raza específica para la inserción 6bp en el extremo 3’ del exón 10 de la secuencia del gen de la piruvato quinasa eritrocitaria (R-PK) como fue descrito. Al perro se le practicó eutanasia a los 20 meses de edad debido al deterioro de su estado clínico, el cual incluyó anemia e incompatibilidad sanguínea. -

The Lower Urinary Tract & Male Reproductive System
Chapter 21 Hematopathology Nam Deuk Kim, Ph.D. Pusan National University 1 Contents I. Red blood cells II. Hemostasis III. White blood cells IV. Disorders of the lymphopoietic system V. Spleen VI. Thymus 2 THE HEMATOPOIETIC SYSTEM Composition of Human Blood Blood • Transports oxygen, nutrients, hormones, leukocytes (white cells), red cells, platelets and antibodies to tissues in the body and carbon dioxide and other waste products of cell metabolism to the excretory organs of the body • Volume of blood: Represents about 8% of total body weight • approximately 5 quarts, but it varies according to size of individual (5 liters in women; 5.5 liters in men) • Almost half of the blood consists of cellular elements suspended in plasma (viscous fluid) 3 4 Hemopoiesis Cellular differentiation and maturation of the lymphoid and myeloid components of the hematopoietic system. Only the precursor cells (blasts and maturing cells) are identifiable by light microscopic evaluation of the bone marrow. BFU = burst-forming unit; CFU = colony-forming unit (Ba = basophils; E = erythroid; Eo = eosinophils; G = polymorphonuclear leukocytes; GM = granulocyte-monocyte; M = monocyte/macrophages; Meg = megakaryocytic); EPO = erythropoietin; Gm-CSF = granulocyte-macrophage colony-stimulating factor; IL = interleukin; NK = natural killer; SCF = stem cell factor; TPO = thrombopoietin. 5 Composition of Human Blood • All blood cells arise from precursor cells within the bone marrow, called stem cells • These undergo further differentiation to form red cells, white cells, -
Hematology Unit Lab 1 Review Material
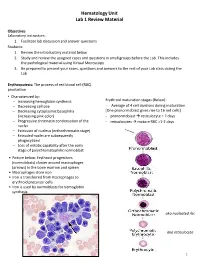
Hematology Unit Lab 1 Review Material Objectives Laboratory instructors: 1. Facilitate lab discussion and answer questions Students: 1. Review the introductory material below 2. Study and review the assigned cases and questions in small groups before the Lab. This includes the pathological material using Virtual Microscopy 3. Be prepared to present your cases, questions and answers to the rest of your Lab class during the Lab Erythropoiesis: The process of red blood cell (RBC) production • Characterized by: − Increasing hemoglobin synthesis Erythroid maturation stages (Below): − Decreasing cell size - Average of 4 cell divisions during maturation − Decreasing cytoplasmic basophilia [One pronormoblast gives rise to 16 red cells] (increasing pink color) - pronormoblast → reticulocyte = 7 days − Progressive chromatin condensation of the - reticulocytes → mature RBC =1-2 days nuclei − Extrusion of nucleus (orthochromatic stage) − Extruded nuclei are subsequently phagocytized − Loss of mitotic capability after the early stage of polychromatophilic normoblast • Picture below: Erythroid progenitors (normoblasts) cluster around macrophages (arrows) in the bone marrow and spleen • Macrophages store iron • Iron is transferred from macrophages to erythroid precursor cells • Iron is used by normoblasts for hemoglobin synthesis aka nucleated rbc aka reticulocyte 1 Mature Red Blood Cell 7-8 microns; round / ovoid biconcave disc with orange-red cytoplasm, no RNA, no nucleus; survives ~120 days in circulation Classification of Anemia by Morphology 1. -

Hemophagocytic Lymphohistiocytosis in a Child with Sickle Cell Disease
Hematology & Transfusion International Journal Case Report Open Access Hemophagocytic lymphohistiocytosis in a child with sickle cell disease Keywords: hemophagocytic lymphohistiocytosis, FHL, EBV, hemoglobin S, sickle cell disease, X-ray Volume 6 Issue 5 - 2018 Introduction Walaa Shoman,1 Yasmine El Chazli,2 Asmaa Elsharkawy,2 Neveen Mikhael,3 Akram Hemophagocytic lymphohistiocytosis (HLH) is a life-threatening deghaidy,3 Abeer Al-Battashi,4 Yasser Wali2 hyper-inflammatory syndrome which represents the extreme end of 1Department of Pediatrics, Immunology/Rheumatology unit, a severe uncontrolled hyperinflammatory reaction that can occur in Alexandria University, Egypt many underlying conditions.1 HLH can be divided into primary and 2Department of Pediatrics, Hematology/Oncology unit, secondary HLH. Primary HLH is caused by gene mutation, either at Alexandria University, Egypt 3 one of the Familial HLH (FHL) loci or in a gene responsible for one Department of Clinical pathology, Alexandria University, Egypt 4Department of Child Health, Royal Hospital, Oman of several immunodeficiency syndromes.2 The most common form of secondary HLH is infection associated HLH. Infectious triggers Correspondence: Yasser Wali, Department of Pediatrics, include viruses (as EBV, cytomegalovirus, HHV8, HIV), bacteria (as Hematology/Oncology unit, Alexandria University, Egypt, mycobacteria, mycoplasma), parasites (as leishmania, plasmodium), Email [email protected] 3,4 and fungi (as candida, cryptococcus). Sickle cell disease (SCD) Received: September 02, 2018 | Published: September 27, and its variants are genetic disorders resulting from the presence 2018 of a mutated form of hemoglobin, hemoglobin S (HbS), which can be detected by hemoglobin electrophoresis. SCD is suggested by a high-grade unremitting fever, grunting, marked pallor, jaundice, the typical clinical picture of chronic hemolytic anemia and vaso- and marked re-enlargement of both liver and spleen despite improved occlusive crisis.5,6 We present a case of HLH in an Egyptian boy who chest condition and radiogram. -

Hereditary Spherocytosis with Gilbert's Syndrome
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-ISSN: 2279-0853, p-ISSN: 2279-0861.Volume 20, Issue 4 Ser.6 (April. 2021), PP 25-28 www.iosrjournals.org Hereditary Spherocytosis with Gilbert’s Syndrome – a case report. Dr Deepan Panneerselvam Intern, Department of Internal Medicine. Dr Thabuna Sivaprakasam Intern, Department of Internal Medicine. Dr Raja sekar PGY2 Internal Medicine Resident. Dr Govindarajulu Ethirajulu Chief, Department of Internal Medicine. Government Kilpauk Medical College and Hospital. Abstract: A 23 year old previously diagnosed female with Gilbert’s syndrome on treatment with Prednisone, presented with a lower respiratory tract infection for the past 4 days with additional complaints of significant lethargy and fatigue, palpitation and intermittent yellowish discolouration of sclera since 9 years old. The patient’s mother and elder sister also had similar history of intermittent jaundice. Routine investigations of the patient revealed normal values except a hemoglobin level of 6.0 g/dl, HCT of 19.5%, MCV of 75.6 fL, serum total bilirubin of 6.3 mg/dl ( Direct: 1.3mgdl, Indirect: 5.0 mg/dl ). This made us suspect another basic hematologic abnormality that contributed to such elevated indirect bilirubin levels. Further investigations revealed a peripheral smear with moderate microcytic hypochromic anemia, anisopoikilocytosis, leucopenia and a reticulocyte count of 2.3%, negative Direct coombs test and a serum LDH of 345U/L. Ultrasound sound abdomen revealed multiple calculi in gall bladder largest measuring 3mm and splenomegaly. Peripheral smear was repeated only to reveal a dimorphic blood picture with eosinophilia, normocytic normochromic anemia with a few fragmented RBCs and spherocytes. -

SEED Haematology Sysmex Educational Enhancement and Development October 2012
SEED Haematology Sysmex Educational Enhancement and Development October 2012 The red blood cell indices The full blood count has been used in conjunction with the traditional red The complete blood count (CBC) is central to clinical deci- cell indices in order to narrow down the possible causes sion making. This makes it one of the commonest laboratory of anaemia in an individual patient. investigations performed worldwide. Whilst the definition of what constitutes an CBC is influenced by the number Impedance technology and type of parameters measured by different haematology The RBC, HCT and MCV are all closely interrelated as they analysers, the traditional red cell indices that are widely are derived from information obtained from the passage used to classify anaemias are common to all. of cells through the aperture of the impedance channel of an automated haematology analyser. The impedance The laboratory approach to anaemia technology is based on the principle that an electrical field, Anaemia is an extremely common global healthcare prob- created between two electrodes of opposite charge, can lem. However, anaemia is merely a symptom which can be used to count and determine the size of cells. Blood result from a multitude of causes. Effective treatment is cells are poor conductors of electricity. The diluent in which only possible if the underlying cause is correctly identified. they are suspended as they pass through the aperture To this end, several classification systems have been devis- during counting is an isotonic solution which is a good ed. The most useful and widely used classification system conductor of electricity. -

Anemic Syndrome and White Blood Cells Disorders
27. 11. 2020 Anemic syndrome and white blood cells disorders Kristína Repová, M.D., PhD. [email protected] Institute of Pathophysiology, Faculty of Medicine, Bratislava Prepared exclusively for the purposes of distance education at the Faculty of Medicine, Comenius University in Bratislava in 2020/21 Hematopoeisis • Hematopoietic organs: • Bone marrow: • forming of erythrocytes, granulocytes, monocytes, thrombocytes, partially lymphocytes • Thymus: • forming of T-lymphocytes • Lymphatic nodes, tonsils, spleen: • forming of B-lymphocytes lymphoid multipotent stem cell pluripotent progenitor cell precursor cell stem cell myleoid multipotent stem cell 1 27. 11. 2020 Hematopoeisis 3 Pluripotent hematopoietic stem cell (self-renewal) Myeloid multipotent Lymphoid multipotent stem cell stem cell Megacaryocyte and Granulocyte and T-cell and NK B-cell erythroid progenitor Macrophage progenitor cell progenitor progenitor Megacaryocyte Erythrocyte Granulocyte Monocyte progenitor progenitor progenitor progenitor (CFU-Meg) (CFU-E) (CFU-G) (CFU-M) Myeloblast NK-cell Proerythroblast Monoblast Lymphoblast Lymphoblast Promyelocyte Megacaryoblast Erythroblast Myelocyte Promonocyte Prolymphocyte Prolymphocyte Megacaryocyte Reticulocyte Metamyelocyte Monocyte T-cell B-cell Thrombocyte Erythrocyte Band cell Basophil Eosinophil Macrophage Dendritic cell Neutrophil 2 27. 11. 2020 I. Disorders of red blood cells II. Disorders of white blood cells III. Myeloproliferative and lymphoproliferative disorders I. Disorders of red blood cells 1. Anemia 2. -

Hemolytic Anemia Presenting As Hemoglobinuria from Intentional Paradichlorobenzene Mothball Ingestion
Hemolytic Anemia from Intentional ParadichlorobenzeneCASE Mothball REPORT Ingestion Hemolytic Anemia Presenting as Hemoglobinuria from Intentional Paradichlorobenzene Mothball Ingestion Mary Ondinee U. Manalo,1 Cherie Grace G. Quingking2 and Carissa Paz C.Dioquino2 1Department of Medicine, College of Medicine and Philippine General Hospital, University of the Philippines Manila 2National Poison Management and Control Center, University of the Philippines-Philippine General Hospital less acutely toxic of the two. However, like naphthalene, it has also been known to induce hemolytic anemia because it possesses one benzene ring.1 We report a case of a man who intentionally ingested three mothballs made of paradicholorobenzene who experienced severe hemolytic anemia that necessitated blood transfusion. Case A 24-year-old male inmate from Manila was admitted for persistent vomiting three days after ingestion of three crushed mothballs. Three days prior to admission, the patient intentionally swallowed three crushed mothballs. After an hour, he experienced nausea and vague abdominal pain. A day prior to admission, he presented with persistent vomiting and passed out dark stools. Eight hours prior to admission, Introduction vomiting became more frequent and was now associated Mothballs could be made of naphthalene, with coffee-ground material. Abdominal pain became more paradichlorobenzene, or camphor. Differentiation among intense as well. He was then brought to the Emergency mothballs is difficult because they may have similar odors Room of the Philippine General Hospital for consultation. and are all white, crystalline solids at room temperature. The patient presented at the emergency room awake but Paradichlorobenzene is commonly found here in the weak-looking, tachypneic but with otherwise stable vital Philippines as a component of toilet deodorant blocks, but signs. -

Microcytic Hypochromic Anemia Patients with Thalassemia: Genotyping Approach
101 MICROCYTIC HYPOCHROMIC ANEMIA PATIENTS WITH THALASSEMIA: GENOTYPING APPROACH FAKHER RAHIM ABSTRACT BACKGROUND: Microcytic hypochromic anemia is a common condition in clinical practice, and alpha-thalassemia has to be considered as a differential diagnosis. AIMS: This study was conducted to evaluate the frequency of α-gene, β-gene and hemoglobin variant numbers in subjects with microcytic hypochromic anemia. SETTING AND DESIGNS: Population-based case-control study in the Iranian population. MATERIALS AND METHODS: A total of 340 subjects from southwest part of Iran were studied in the Research Center of Thalassemia and Hemoglobinopathies (RCTH), Iran. Genotyping for known α- and β-gene mutations was done with gap-PCR and ARMS. In cases of some rare mutations, the genotyping was done with the help of other techniques such as RFLP and ARMS-PCR. STATISTICAL ANALYSIS: Statistical analysis was carried out by SPSS 11.5 and an independent-sample t test. RESULTS: Out of the total 340 individuals, 325 individuals were evaluated to have microcytic hypochromic anemia based on initial hematological parameters such as MCV<80 fl; MCH <27 pg; the remaining 15 patients were diagnosed with no definite etiology. The overall frequency of -α3.7 deletion in 325 individuals was 20.3%. The most frequent mutations were IVS II-I, CD 36/37 and IVS I-110 with frequencies of 6.31%, 5.27% and 1.64%, respectively. Only, there was a significant difference between beta-thalassemia trait and beta-thalassemia major with regard to MCV (P < 0.05) and MCH (P < 0.05) indices, and also MCH index between beta-thalassemia trait and Hb variants (P < 0.05). -

G6PD LEVEL DEFICIENCY in MALRIA Sarfraz Mash1, Muhammad Afzal2, Ms
IAJPS 2019, 06 (08), 15436-15440 Sarfraz Mash et al ISSN 2349-7750 CODEN [USA]: IAJPBB ISSN: 2349-7750 INDO AMERICAN JOURNAL OF PHARMACEUTICAL SCIENCES http://doi.org/10.5281/zenodo.3380512 Available online at: http://www.iajps.com Research Article G6PD LEVEL DEFICIENCY IN MALRIA Sarfraz Mash1, Muhammad Afzal2, Ms. Hajra Sarwar3 1 Post RN (BSN) 2nd semester student Sarfraz Mash, Lahore school of Nursing, 2 Head of Department of Lahore School of Nursing, 3 (MSN) Lahore school of Nursing. Article Received: June 2019 Accepted: July 2019 Published: August 2019 Abstract: Glucose-6-phosphate dehydrogenase (G6PD) deficiency is the most common hereditary enzyme disorder and morethan 200 million people have a deficiency of this enzyme. G6PD deficiency is an X-linked enzyme defect, and one of its main signs is the presence of hemolytic anemia. It is a worldwide important cause of neonatal jaundice and causes life threatening hemolytic crisis in childhood. At later ages, certain drugs such as anti-malarial drugs and fava beans cause hemolysis among G6PD deficiency patients. The frequency and severity is influenced by genetic and cultural factors. It is common in Mediterranean, African and some East Asian populations but rare in Bangladeshi peoples. Genetic counseling may be of benefit for patients and their families. Other treatment is symptomatic and supportive. Corresponding author: Sarfraz Mash, QR code Post RN (BSN) 2nd semester student Sarfraz Mash, Lahore school of Nursing. Please cite this article in press Sarfraz Mash et al., G6PD Level Deficiency In Malria., Indo Am. J. P. Sci, 2019; 06(08). www.iajps.com Page 15436 IAJPS 2019, 06 (08), 15436-15440 Sarfraz Mash et al ISSN 2349-7750 INTRODUCTION: phosphate dehydrogenase.