Pathology of Soft Tissue and Skin. Bone and Joint Pathology. Pathology of Soft Tissue and Skin
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

General Pathomorpholog.Pdf
Ukrаiniаn Medicаl Stomаtologicаl Аcаdemy THE DEPАRTАMENT OF PАTHOLOGICАL АNАTOMY WITH SECTIONSL COURSE MАNUАL for the foreign students GENERАL PАTHOMORPHOLOGY Poltаvа-2020 УДК:616-091(075.8) ББК:52.5я73 COMPILERS: PROFESSOR I. STАRCHENKO ASSOCIATIVE PROFESSOR O. PRYLUTSKYI АSSISTАNT A. ZADVORNOVA ASSISTANT D. NIKOLENKO Рекомендовано Вченою радою Української медичної стоматологічної академії як навчальний посібник для іноземних студентів – здобувачів вищої освіти ступеня магістра, які навчаються за спеціальністю 221 «Стоматологія» у закладах вищої освіти МОЗ України (протокол №8 від 11.03.2020р) Reviewers Romanuk A. - MD, Professor, Head of the Department of Pathological Anatomy, Sumy State University. Sitnikova V. - MD, Professor of Department of Normal and Pathological Clinical Anatomy Odessa National Medical University. Yeroshenko G. - MD, Professor, Department of Histology, Cytology and Embryology Ukrainian Medical Dental Academy. A teaching manual in English, developed at the Department of Pathological Anatomy with a section course UMSA by Professor Starchenko II, Associative Professor Prylutsky OK, Assistant Zadvornova AP, Assistant Nikolenko DE. The manual presents the content and basic questions of the topic, practical skills in sufficient volume for each class to be mastered by students, algorithms for describing macro- and micropreparations, situational tasks. The formulation of tests, their number and variable level of difficulty, sufficient volume for each topic allows to recommend them as preparation for students to take the licensed integrated exam "STEP-1". 2 Contents p. 1 Introduction to pathomorphology. Subject matter and tasks of 5 pathomorphology. Main stages of development of pathomorphology. Methods of pathanatomical diagnostics. Methods of pathomorphological research. 2 Morphological changes of cells as response to stressor and toxic damage 8 (parenchimatouse / intracellular dystrophies). -

2016 Essentials of Dermatopathology Slide Library Handout Book
2016 Essentials of Dermatopathology Slide Library Handout Book April 8-10, 2016 JW Marriott Houston Downtown Houston, TX USA CASE #01 -- SLIDE #01 Diagnosis: Nodular fasciitis Case Summary: 12 year old male with a rapidly growing temple mass. Present for 4 weeks. Nodular fasciitis is a self-limited pseudosarcomatous proliferation that may cause clinical alarm due to its rapid growth. It is most common in young adults but occurs across a wide age range. This lesion is typically 3-5 cm and composed of bland fibroblasts and myofibroblasts without significant cytologic atypia arranged in a loose storiform pattern with areas of extravasated red blood cells. Mitoses may be numerous, but atypical mitotic figures are absent. Nodular fasciitis is a benign process, and recurrence is very rare (1%). Recent work has shown that the MYH9-USP6 gene fusion is present in approximately 90% of cases, and molecular techniques to show USP6 gene rearrangement may be a helpful ancillary tool in difficult cases or on small biopsy samples. Weiss SW, Goldblum JR. Enzinger and Weiss’s Soft Tissue Tumors, 5th edition. Mosby Elsevier. 2008. Erickson-Johnson MR, Chou MM, Evers BR, Roth CW, Seys AR, Jin L, Ye Y, Lau AW, Wang X, Oliveira AM. Nodular fasciitis: a novel model of transient neoplasia induced by MYH9-USP6 gene fusion. Lab Invest. 2011 Oct;91(10):1427-33. Amary MF, Ye H, Berisha F, Tirabosco R, Presneau N, Flanagan AM. Detection of USP6 gene rearrangement in nodular fasciitis: an important diagnostic tool. Virchows Arch. 2013 Jul;463(1):97-8. CONTRIBUTED BY KAREN FRITCHIE, MD 1 CASE #02 -- SLIDE #02 Diagnosis: Cellular fibrous histiocytoma Case Summary: 12 year old female with wrist mass. -

My Approach to Superficial Inflammatory Dermatoses K O Alsaad, D Ghazarian
1233 J Clin Pathol: first published as 10.1136/jcp.2005.027151 on 25 November 2005. Downloaded from REVIEW My approach to superficial inflammatory dermatoses K O Alsaad, D Ghazarian ............................................................................................................................... J Clin Pathol 2005;58:1233–1241. doi: 10.1136/jcp.2005.027151 Superficial inflammatory dermatoses are very common and diagnosis of inflammatory skin diseases, there are limitations to this approach. The size of the comprise a wide, complex variety of clinical conditions. skin biopsy should be adequate and representa- Accurate histological diagnosis, although it can sometimes tive of all four compartments and should also be difficult to establish, is essential for clinical include hair follicles. A 2 mm punch biopsy is too small to represent all compartments, and often management. Knowledge of the microanatomy of the skin insufficient to demonstrate a recognisable pat- is important to recognise the variable histological patterns tern. A 4 mm punch biopsy is preferred, and of inflammatory skin diseases. This article reviews the non- usually adequate for the histological evaluation of most inflammatory dermatoses. However, a vesiculobullous/pustular inflammatory superficial larger biopsy (6 mm punch biopsy), or even an dermatoses based on the compartmental microanatomy of incisional biopsy, might be necessary in panni- the skin. culitis or cutaneous lymphoproliferative disor- ders. A superficial or shave biopsy should be .......................................................................... -

Progressive Widespread Warty Skin Growths
DERMATOPATHOLOGY DIAGNOSIS Progressive Widespread Warty Skin Growths Patrick M. Kupiec, BS; Eric W. Hossler, MD Eligible for 1 MOC SA Credit From the ABD This Dermatopathology Diagnosis article in our print edition is eligible for 1 self-assessment credit for Maintenance of Certification from the American Board of Dermatology (ABD). After completing this activity, diplomates can visit the ABD website (http://www.abderm.org) to self-report the credits under the activity title “Cutis Dermatopathology Diagnosis.” You may report the credit after each activity is completed or after accumu- lating multiple credits. A 33-year-old man presented with progres- sive widespread warty skin growths that had been present copysince 6 years of age. Physical examination revealed numerous verrucous papules on the face and neck along with Figure 1. H&E, original magnification ×40. Figure 2. H&E, original magnification ×40. verrucous, tan-pink papules and plaques diffuselynot scattered on the trunk, arms, and legs. A biopsy of a lesion on the neck Dowas performed. H&E, original magnification ×200. The best diagnosisCUTIS is: a. condyloma acuminatum b. epidermodysplasia verruciformis c. herpesvirus infection d. molluscum contagiosum e. verruca vulgaris PLEASE TURN TO PAGE 99 FOR DERMATOPATHOLOGY DIAGNOSIS DISCUSSION Mr. Kupiec is from the State University of New York (SUNY) Upstate Medical University, Syracuse. Dr. Hossler is from the Departments of Dermatology and Pathology, Geisinger Medical Center, Danville, Pennsylvania. The authors report no conflict of interest. Correspondence: Patrick M. Kupiec, BS, 50 Presidential Plaza, Syracuse, NY 13202 ([email protected]). 82 CUTIS® WWW.CUTIS.COM Copyright Cutis 2017. No part of this publication may be reproduced, stored, or transmitted without the prior written permission of the Publisher. -

Wednesday Slide Conference 2008-2009
PROCEEDINGS DEPARTMENT OF VETERINARY PATHOLOGY WEDNESDAY SLIDE CONFERENCE 2008-2009 ARMED FORCES INSTITUTE OF PATHOLOGY WASHINGTON, D.C. 20306-6000 2009 ML2009 Armed Forces Institute of Pathology Department of Veterinary Pathology WEDNESDAY SLIDE CONFERENCE 2008-2009 100 Cases 100 Histopathology Slides 249 Images PROCEEDINGS PREPARED BY: Todd Bell, DVM Chief Editor: Todd O. Johnson, DVM, Diplomate ACVP Copy Editor: Sean Hahn Layout and Copy Editor: Fran Card WSC Online Management and Design Scott Shaffer ARMED FORCES INSTITUTE OF PATHOLOGY Washington, D.C. 20306-6000 2009 ML2009 i PREFACE The Armed Forces Institute of Pathology, Department of Veterinary Pathology has conducted a weekly slide conference during the resident training year since 12 November 1953. This ever- changing educational endeavor has evolved into the annual Wednesday Slide Conference program in which cases are presented on 25 Wednesdays throughout the academic year and distributed to 135 contributing military and civilian institutions from around the world. Many of these institutions provide structured veterinary pathology resident training programs. During the course of the training year, histopathology slides, digital images, and histories from selected cases are distributed to the participating institutions and to the Department of Veterinary Pathology at the AFIP. Following the conferences, the case diagnoses, comments, and reference listings are posted online to all participants. This study set has been assembled in an effort to make Wednesday Slide Conference materials available to a wider circle of interested pathologists and scientists, and to further the education of veterinary pathologists and residents-in-training. The number of histopathology slides that can be reproduced from smaller lesions requires us to limit the number of participating institutions. -

Regressing Basal-Cell Carcinoma Masquerading As Benign Lichenoid Keratosis
DERMATOLOGY PRACTICAL & CONCEPTUAL www.derm101.com Regressing basal-cell carcinoma masquerading as benign lichenoid keratosis Aleksandra Kulberg1, Wolfgang Weyers2 1 Department of Dermatology, Venerology, and Allergology, Klinikum Hildesheim, Germany 2 Center for Dermatopathology, Freiburg, Germany Key words: Basal-cell carcinoma, benign lichenoid keratosis, lichen planus-like keratosis. Citation: Kulberg A, Weyers W. Regressing basal-cell carcinoma masquerading as benign lichenoid keratosis. Dermatol Pract Concept 2016;6(4):3. doi: 10.5826/dpc.0604a03 Received: May 25, 2016; Accepted: June 21, 2016; Published: October 31, 2016 Copyright: ©2016 Kulberg et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Funding: None. Competing interests: The authors have no conflicts of interest to disclose. All authors have contributed significantly to this publication. Corresponding author: Wolfgang Weyers, MD, Center for Dermatopathology, Engelbergerstr. 19, 79098 Freiburg, Germany. Tel. 01149- 761-31696; Fax. 01149-761-39772. Email: [email protected] ABSTRACT Background: Benign lichenoid keratosis (BLK, LPLK) is often misdiagnosed clinically as superficial basal-cell carcinoma (BCC), especially when occurring on the trunk. However, BCCs undergoing re- gression may be associated with a lichenoid interface dermatitis that may be misinterpreted as BLK in histopathologic sections. Methods: In order to assess the frequency of remnants of BCC in lesions interpreted as BLK, we per- formed step sections on 100 lesions from the trunk of male patients that had been diagnosed as BLK. Results: Deeper sections revealed remnants of superficial BCC in five and remnants of a melanocytic nevus in two specimens. -

Inflammatory Skin Disease Every Pathologist Should Know
Inflammatory skin disease every pathologist should know Steven D. Billings Cleveland Clinic [email protected] General Concepts • Pattern recognition – Epidermal predominant vs. dermal predominant • Epidermal changes trump dermal changes – Distribution of the inflammatory infiltrate • Superficial vs. superficial and deep • Location: perivascular, interstitial, nodular – Nature of inflammatory infiltrate • Mononuclear (lymphocytes and histiocytes) • Mixed (mononuclear and granulocytes) • Granulocytic • Correlation with clinical presentation • Never diagnose “chronic nonspecific dermatitis” Principle Patterns: Epidermal Changes Predominant • Spongiotic pattern • Psoriasiform pattern – Spongiotic and psoriasiform often co-exist • Interface pattern – Basal vacuolization • Perivascular infiltrate or • Lichenoid infiltrate Principle Patterns: Dermal Changes Predominant • Superficial perivascular • Superficial and deep perivascular • Interstitial pattern – Palisading granulomatous – Nodular and diffuse • Sclerosing pattern • Panniculitis • Bullous disease • Miscellaneous Spongiotic Dermatitis • Three phases – Acute – Subacute – Chronic • Different but overlapping histologic features Spongiotic Dermatitis • Acute spongiotic dermatitis – Normal “basket-weave” stratum corneum – Pale keratinocytes – Spongiosis – Spongiotic vesicles (variable) – Papillary dermal edema – Variable superficial perivascular infiltrate of lymphocytes often with some eosinophils – Rarely biopsied in acute phase Spongiotic Dermatitis • Subacute spongiotic dermatitis – Parakeratosis -
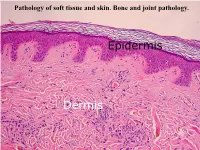
Pathology of Soft Tissue and Skin. Bone and Joint Pathology. Pathology of Soft Tissue and Skin
Pathology of soft tissue and skin. Bone and joint pathology. Pathology of soft tissue and skin. Bone and joint pathology. I.Microspecimens: № 188. Capillary hemangioma. (H.E. stain). Indications: 1. Epidermis. 2. Dermis 3. Spindle cells arranged compactly with spaces containing blood. 4. Reduced connective stroma. In the microspecimen is presented a well-defined subepidermal tumoral node, consisting of proliferating capillary blood vessels, poor loose stroma; epidermis with normal histological structure. Hemangioma is a benign tumor of vascular origin, histological variants are capillary, venous and cavernous hemangioma. It is located mainly in the skin, the mucosa of the gastrointestinal tract, the liver. Capillary hemangioma is the most common benign tumor in children and has a disembryoplazic character, being interpreted as a hamartoma - a tumor from the embryonic tissues. Macroscopically it has the appearance of a red-purple node or plaque. Cutaneous hemangiomas can be complicated by exulceration, bleeding, the association of secondary infection. 3 2 4 1 № 188. Capillary hemangioma. (H.E. stain). № 43. Fibrosarcoma. (H.E. stain). Indications: 1.Epidermis. 2.Dermis. 3.Atypical tumor cells (fibroblast-like). 4.Bundles of collagen fibers. In the skin, under the epidermis there is a rich cellular tumoral node, consisting of predominantly spindle-shaped cells, of the fibroblasts type, arranged in bundles, which intersect in different directions, the tumor has no precise limits, many mitoses, giant cells, foci of necrosis, hemorrhage, stroma is poor. Fibrosarcoma is a malignant tumor, which derives from fibroblasts, may have different degrees of differentiation. It is found in adults between the ages of 40 and 70, located more frequently in the deep tissues of the hip, knee, in the retroperitoneal area. -

Tern, It Was Felt of Use to Record the Experience in This Matter
PERSISTENT "INSECT BITES" (DERMAL EOSINOPHILIC GRANU- LOMAS) SIMULATING LYMPHOBLASTOMAS, HISTIOCYTOSES, AND SQUAMOUS CELL CARCINOMAS * ARrHUR C. ALLEN, MD. t (From the Army instute of Pathology, Washingtox 25, D.C.) In 1942, opportunity was afforded at the Army Institute of Pathol- ogy to review the histologic slides of a lesion said to have been pro- duced by a tick bite. The microscopic sections seemed at the time indistinguishable from mycosis fungoides or Hodgkin's disee, espe- cialy in view of the presence of multiple lesions in the patient. How- ever, following the study of the cutaneous reactions to arthropods (ticks, mosquitoes, and chiggers), it was quickly appreciated that not only were these diagnoses of neoplasia wrong but that the misinterpretation of these reactions was a common and serious error.' The errors in- volved the misconstruction not only of the dermal reaction but also of the epidermal changes. The latter response was confused with squa- mous cell carcinoma; the dermal infitrate was mistaken for mycosis fungoides, Hodgkin's disease, lymphosacoma, giant follicular lympho- blastoma, and Spiegler-Fendt sarcoid. Undoubtedly the principal rea- son for the failure to attnbute these reactions properly to bites of arachnida and insects was referable to the general impression, despite dear-cut cinical histories, that such reactions last only for days, whereas, in truth, they may persist for as long as 2 years. More re- cently, the problem has been further complicated by introduction into the literature of a lesion called "eosinophilic granuloma of skin," an entity of questionable nosologic justification.' Therefore, because of the major importance of establishing a definitive diagnosis and because of the interest in the pathogenesis of a much mimicked histologic pat- tern, it was felt of use to record the experience in this matter. -

ECZEMA) Shankar Pratap K
Research Article International Ayurvedi c Medical Journal ISSN:2320 5091 A HISTOPATHOLOGICAL STUDY ON LEECH APPLICATION IN THE MANAGEMENT OF VICARCIKA (ECZEMA) Shankar Pratap K. M.1 Rao Dattatreya 2 Sai Prasad 3 1Dept. of Shalya Tantra , Santhigiri Ayurvedic College , Palakkad, Kerala, India 2Dept. of Shalya Tantra, S.V. Ayurvedic College, Tirupati , Andhra Pradesh , India 3Dept. of Pathology, S. V. Medical College, Tirupati, Andhra Pradesh, India ABSTRACT To assess the efficacy of Leech application in the management of Vicarcik a (Eczema) with Histopathological study, the present study with 10 patients having the classical symptoms of Vicarcika, were randomly selected as per the inclusion and exclusion criteria from O.P.D. & I.P.D. sections of Shalya department, S.V. Ayurvedic Hospital, Tirupati. Minimum 4 sittings of Leech application was carried out with seven days interval. Total duration of treatment was 6 weeks. Biopsy samples were collected from the lesion site before and after treatment. Histopathological examination was done by the pathologist. In eczema (dermatitis) the leech application therapy gives excellent response by reducing the inflammatory component, hyperkeratosis, spongiosis, irregular acanthosis and by evoking a granulation tissue response in the dermis and in most of the cases with complete recovery from the lesion. Most of the cases in the study were chronic dermatitis and sebhoric keratosis, almost all local/focal pigmented lesion is totally relieved by leech therapy especially in cases of sebhoric keratos is. In the present study it was found that, leech application evokes significant changes at histological level specifically in reduction of inflammatory component, hyperkeratosis, spongiosis and irregular acanthosis. -

Diffuse Drug-Induced Dermatitis Following Sclerotherapy for Telangiectasias Libby MW, Caitlin WH, Deniz OA and Heller JA*
Case Report iMedPub Journals Journal of Vascular and Endovascular Surgery 2016 http://www.imedpub.com/ Vol.1 No.3:17 DOI: 10.21767/2573-4482.100017 Diffuse Drug-Induced Dermatitis following Sclerotherapy for Telangiectasias Libby MW, Caitlin WH, Deniz OA and Heller JA* Department of Surgery, Johns Hopkins Vein Center, Johns Hopkins Medical Centers, Baltimore, USA *Corresponding author: Jennifer A Heller, 10755 Falls Road, Pavilion 1 Suite 360, Lutherville, MD 21903, Tel: 4105500415; Email: [email protected] Received date: June 14, 2016; Accepted date: July 26, 2016; Published date: August 02, 2016 Copyright: © 2016 Libby MW, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Sclerotherapy is an effective treatment modality for the management of lower extremity telangiectasias. Although localized dermatologic reactions are known complications of this procedure, systemic reactions are rare. Here, we present a case of a diffuse drug eruption following sclerotherapy for the treatment of bilateral lower extremity telangiectasias. Salient clinical and physical exam findings are described. Management strategies for the treatment of drug eruptions are outlined. This is the first case report that we know of describing a diffuse drug eruption associated with sclerotherapy. It is important to recognize the possibility of diffuse drug eruptions secondary to sclerotherapy treatment so that expectant management may be initiated expeditiously in affected patients. Figure 1: Drug eruption following sclerotherapy. The patient was referred for evaluation by a dermatologist, Case Report who initially diagnosed diffuse dermatitis based on clinical A 64-year-old woman with hypertension and bilateral lower exam. -

JMSCR Vol||07||Issue||03||Page 281-286||March 2019
JMSCR Vol||07||Issue||03||Page 281-286||March 2019 www.jmscr.igmpublication.org Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v7i3.51 Histopathological Evaluation of Collagen Profiles in Spongiotic Dermatitis Authors Anjali Patankar, Ramya Gandhi*, Erli Amel Ivan Department of Pathology, Sri Manakula Vinayagar Medical College and Hospital, Kalitheerthalkuppam, Puducherry, 605 107 India *Corresponding Author Dr Ramya Gandhi Associate Professor, Department of Pathology, Sri Manakula Vinayagar Medical College and Hospital, Kalitheerthalkuppam, Puducherry, 605 107, India Email: [email protected], Mobile no- 9787740891 Abstract Context: Spongiotic Dermatitis is a common clinical condition also known as eczema, characterized by rashes and itching further may progress to scarring. The terms eczema and dermatitis are often used interchangeably to denote a polymorphic inflammatory reaction pattern involving the epidermis and dermis. Spongiosis refers to intraepidermal edema. Aim: To assess the orientation of collagen in eczematous spongiotic dermatitis. Material and Methods: The present study was done in the Department of Pathology, Sri Manakula Vinayagar Medical College, Pondicherry. Sixty diagnosed cases of spongiotic dermatitis diagnosed over a period of five years were taken in the study. Orientation of collagen was evaluated using Masson’s trichrome stain. Results: Spongiotic dermatitis occurred in all age groups but commonly seen in middle age to elderly. Male to female ratio was 1:1.2 The most common symptom was itching (85%) followed by scaling (63.3%). Most common site was upper extremities (80%). subacute cases were predominantly seen (38.3%) followed by chronic cases (33.3%).