Anatomy 2019/2020 THORAX
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
The Structure and Function of Breathing
CHAPTERCONTENTS The structure-function continuum 1 Multiple Influences: biomechanical, biochemical and psychological 1 The structure and Homeostasis and heterostasis 2 OBJECTIVE AND METHODS 4 function of breathing NORMAL BREATHING 5 Respiratory benefits 5 Leon Chaitow The upper airway 5 Dinah Bradley Thenose 5 The oropharynx 13 The larynx 13 Pathological states affecting the airways 13 Normal posture and other structural THE STRUCTURE-FUNCTION considerations 14 Further structural considerations 15 CONTINUUM Kapandji's model 16 Nowhere in the body is the axiom of structure Structural features of breathing 16 governing function more apparent than in its Lung volumes and capacities 19 relation to respiration. This is also a region in Fascla and resplrstory function 20 which prolonged modifications of function - Thoracic spine and ribs 21 Discs 22 such as the inappropriate breathing pattern dis- Structural features of the ribs 22 played during hyperventilation - inevitably intercostal musculature 23 induce structural changes, for example involving Structural features of the sternum 23 Posterior thorax 23 accessory breathing muscles as well as the tho- Palpation landmarks 23 racic articulations. Ultimately, the self-perpetuat- NEURAL REGULATION OF BREATHING 24 ing cycle of functional change creating structural Chemical control of breathing 25 modification leading to reinforced dysfunctional Voluntary control of breathing 25 tendencies can become complete, from The autonomic nervous system 26 whichever direction dysfunction arrives, for Sympathetic division 27 Parasympathetic division 27 example: structural adaptations can prevent NANC system 28 normal breathing function, and abnormal breath- THE MUSCLES OF RESPIRATION 30 ing function ensures continued structural adap- Additional soft tissue influences and tational stresses leading to decompensation. -

Netter's Musculoskeletal Flash Cards, 1E
Netter’s Musculoskeletal Flash Cards Jennifer Hart, PA-C, ATC Mark D. Miller, MD University of Virginia This page intentionally left blank Preface In a world dominated by electronics and gadgetry, learning from fl ash cards remains a reassuringly “tried and true” method of building knowledge. They taught us subtraction and multiplication tables when we were young, and here we use them to navigate the basics of musculoskeletal medicine. Netter illustrations are supplemented with clinical, radiographic, and arthroscopic images to review the most common musculoskeletal diseases. These cards provide the user with a steadfast tool for the very best kind of learning—that which is self directed. “Learning is not attained by chance, it must be sought for with ardor and attended to with diligence.” —Abigail Adams (1744–1818) “It’s that moment of dawning comprehension I live for!” —Calvin (Calvin and Hobbes) Jennifer Hart, PA-C, ATC Mark D. Miller, MD Netter’s Musculoskeletal Flash Cards 1600 John F. Kennedy Blvd. Ste 1800 Philadelphia, PA 19103-2899 NETTER’S MUSCULOSKELETAL FLASH CARDS ISBN: 978-1-4160-4630-1 Copyright © 2008 by Saunders, an imprint of Elsevier Inc. All rights reserved. No part of this book may be produced or transmitted in any form or by any means, electronic or mechanical, including photocopying, recording or any information storage and retrieval system, without permission in writing from the publishers. Permissions for Netter Art figures may be sought directly from Elsevier’s Health Science Licensing Department in Philadelphia PA, USA: phone 1-800-523-1649, ext. 3276 or (215) 239-3276; or e-mail [email protected]. -

Basic Biomechanics
Posture analysis • A quick evaluation of structure and function • Doctor views patient from behind (P-A) and from the side (lateral) • References points of patient’s anatomy relative to plumb (a position of balance) 9/3/2013 1 Posture analysis • Lateral View – Knees (anterior, posterior, plumb, genu recurvatum) – Trochanter (anterior, posterior, plumb) – Pelvis (anterior, posterior, neutral pelvic tilt) – Lumbar lordosis (hypo-, hyper-, normal) – Mid-axillary line (anterior, posterior, plumb) – Thoracic kyphosis (hyp-, hyper- normal) – Acromion (anterior, posterior, plumb) – Scapulae (protracted, retracted, normal) – Cervical lordosis (hypo-, hyper-, normal) – External auditory meatus (anterior, posterior, plumb) – Occiput (extended, neutral, flexed) 9/3/2013 2 Posture analysis • Posterior – Anterior View – Feet (pronation, supination, normal) – Achilles tendon (bowed in/out, normal) – Knees (genu valga/vera, normal - internal/external rotation) – Popliteal crease heights (low, high, level) – Trochanter heights (low, high, level) – Iliac crest heights (low on the right/left, normal) – Lumbar scoliosis (right/left, or no signs of) – Thoracic scoliosis (right/left, or no signs of) – Shoulder level (low on the right/left, or normal) – Cervical scoliosis (right/left, or no signs of) – Cervical position (rotation, tilt, neutral) – Mastoid (low on the right/left, or normal) 9/3/2013 3 …..poor postures 9/3/2013 4 Functional Anatomy of the Spine • The vertebral curvatures – Cervical Curve • Anterior convex curve (lordosis) develop in infancy -

Anatomical Variants in the Termination of the Cephalic Vein Stoyan Novakov1*, Elena Krasteva2
Institute of Experimental Morphology, Pathology and Anthropology with Museum Bulgarian Anatomical Society Acta morphologica et anthropologica, 25 (3-4) Sofia • 2018 Anatomical Variants in the Termination of the Cephalic Vein Stoyan Novakov1*, Elena Krasteva2 1 Department of Anatomy, Histology and Embryology, 2Department of Propaedeutics of Surgical Di- seases, Medical Faculty, Medical University of Plovdiv * Corresponding author e-mail: [email protected] Jugulocephalic vein is atavistic structure which is very rare. The low incidence of the variations of the cephalic vein in deltopectoral triangle and its position on the anterior surface of the clavicle and the neck doesn’t make it less important for the clinical practice. Phylo- and ontogenesis explain the formation of the above mentioned variations. We followed the pattern of the cephalic vein in its proximal part and termination to describe possible variations. In this long term study on 140 upper limbs of 70 cadavers, 4 or 2,9% of the cephalic veins were variable. The direct empting of the cephalic vein into internal jugular is an exception with few descriptions at the moment. The rareness of this anatomical variation doesn’t make it less important for clinical practice. It is described as a possible obstacle in catheter implantation, clavicle fractures and creation of arteriovenous fistula in patients on hemodialysis. Key words:cadavers, human anatomy variation, cephalic vein, external jugular vein, jugulocephalic vein Introduction Cephalic vein (CV) belongs to the group of superficial veins of the upper limb. It usually forms over the anatomical snuff-box on the radial side of the wrist from the radial end of the dorsal venous plexus. -

Infraclavicular Topography of the Brachial Plexus Fascicles in Different Upper Limb Positions
Int. J. Morphol., 34(3):1063-1068, 2016. Infraclavicular Topography of the Brachial Plexus Fascicles in Different Upper Limb Positions Topografía Infraclavicular de los Fascículos del Plexo Braquial en Diferentes Posiciones del Miembro Superior Daniel Alves dos Santos*; Amilton Iatecola*; Cesar Adriano Dias Vecina*; Eduardo Jose Caldeira**; Ricardo Noboro Isayama**; Erivelto Luis Chacon**; Marianna Carla Alves**; Evanisi Teresa Palomari***; Maria Jose Salete Viotto**** & Marcelo Rodrigues da Cunha*,** ALVES DOS SANTOS, D.; IATECOLA, A.; DIAS VECINA, C. A.; CALDEIRA, E. J.; NOBORO ISAYAMA, R.; CHACON, E. L.; ALVES, M. C.; PALOMARI, E. T.; SALETE VIOTTO, M. J. & RODRIGUES DA CUNHA, M. Infraclavicular topography of the brachial plexus fascicles in different upper limb positions. Int. J. Morphol., 34 (3):1063-1068, 2016. SUMMARY: Brachial plexus neuropathies are common complaints among patients seen at orthopedic clinics. The causes range from traumatic to occupational factors and symptoms include paresthesia, paresis, and functional disability of the upper limb. Treatment can be surgical or conservative, but detailed knowledge of the brachial plexus is required in both cases to avoid iatrogenic injuries and to facilitate anesthetic block, preventing possible vascular punctures. Therefore, the objective of this study was to evaluate the topography of the infraclavicular brachial plexus fascicles in different upper limb positions adopted during some clinical procedures. A formalin- preserved, adult, male cadaver was used. The infraclavicular and axillary regions were dissected and the distance of the brachial plexus fascicles from adjacent bone structures was measured. No anatomical variation in the formation of the brachial plexus was observed. The metric relationships between the brachial plexus and adjacent bone prominences differed depending on the degree of shoulder abduction. -

Bilateral Sternalis Muscles Were Observed During Dissection of the Thoraco-Abdominal Region of a Male Cadaver
Case Reports Ahmed F. Ibrahim, MSc, MD, Saeed A. Makarem, MSc. PhD, Hassem H. Darwish, MBBCh. ABSTRACT Bilateral sternalis muscles were observed during dissection of the thoraco-abdominal region of a male cadaver. A full description of the muscles, as well as their attachments and innervations were reported. A brief review of the existing literature, regarding the nomenclature, incidence, attachments, innervations and clinical relevance of the sternalis muscle, is also presented. Neurosciences 2005; Vol. 10 (2): 171-173 he importance of continuing to record and Case Report. A well defined sternalis muscle Tdiscuss anatomical anomalies was addressed (Figures 1 & 2) was found, bilaterally, during recently1 in light of technical advances and dissection of the thoraco-abdominal region of a interventional methods of diagnosis and treatment. male cadaver in the Department of Anatomy, The sternalis muscle is a small supernumerary College of Medicine, King Saud University, Riyadh, muscle located in the anterior thoracic region, Kingdom of Saudi Arabia. Both muscles were superficial to the sternum and the sternocostal covered by superficial fascia, located superficial to fascicles of the pectoralis major muscle.2 In the the corresponding sternocostal portion of pectoralis literature, sternalis muscle is called "a normal major and separated from it by pectoral fascia. The anatomic variant"3 and "a well-known variation",4 left sternalis was 19 cm long and 3 cm wide at its although in most textbooks of anatomy, it is broadest part. Its upper end formed a tendon insufficiently mentioned. Yet, clinicians are continuous with that of the sternal head of left surprisingly unaware of this common variation. -

MULTIPLE OSSIFIED COSTAL CARTILAGES for 1ST RIB Raghavendra D.R
International Journal of Anatomy and Research, Int J Anat Res 2014, Vol 2(4):744-47. ISSN 2321- 4287 Case Report DOI: 10.16965/ijar.2014.538 MULTIPLE OSSIFIED COSTAL CARTILAGES FOR 1ST RIB Raghavendra D.R. *1, Nirmala D 2. *1 Post graduate student, Department of anatomy, J J M Medical College, Davangere, Karnataka, India. 2 Associate Professor, Department of anatomy, J J M Medical College, Davangere, Karnataka, India. ABSTRACT Costal cartilages are flattened bars of hyaline cartilages. All ribs except the last two, join with the sternum through their respective costal cartilages directly or indirectly. During dissection for 1st MBBS students in the Department of Anatomy, JJMMC, Davangere, variation was found in a male cadaver aged 45 –50 years. Multiple ossified costal cartilages for 1st rib were present on left side. There were 3 costal cartilages connecting 1st rib to manubrium. There were two small intercostal spaces between them. The lower two small costal cartilages fused together to form a common segment which in turn fused with large upper costal cartilage. The large upper costal cartilage forms costochondral joint with 1st rib. All costal cartilages showed features of calcification. The present variation of multiple ossified costal cartilages are due to bifurcation of costal cartilage. It may cause musculoskeletal pain, intercostal nerve entrapment or vascular compression. Awareness of these anomalies are important for radiologists for diagnostic purpose and for surgeons for performing various clinical and surgical procedures. KEYWORDS: Costal cartilage, bifurcation of Rib, Sternum. Address for Correspondence: Dr. Raghavendra D.R. Post graduate student, Department of anatomy, J J M Medical College, Davangere, 577004, Karnataka, India. -

Myofascial Trigger Points of the Shoulder
Johnson McEvoy and Jan Dommerholt Myofascial Trigger Points of the Shoulder Shoulder problems are common, with a 1-year prevalence in developing a more comprehensive approach to shoulder ranging from 4.7% to 46.7% and a lifetime prevalence of rehabilitation. Inclusion of MTrPs in the assessment and 6.7% to 66.7%.1 Many different structures give rise to shoulder management of shoulder pain and dysfunction does not pain, including the structures in the subacromial space, such necessarily replace other techniques and approaches, but it does as the subacromial bursa, the rotator cuff, and the long head of add an important dimension to the management plan. biceps,2,3 and are presented in various lessons. Muscle and spe- cifically myofascial trigger points (MTrPs), have been recog- nized to refer pain to the shoulder region and may be a source TRIGGER POINTS of peripheral nociceptive input that gives rise to sensitization and pain. MTrP referral patterns have been published for the A myofascial trigger point is defined as a hyperirritable spot in shoulder region.4-6 skeletal muscle, which is associated with a hypersensitive Often, little attention is paid to MTrPs as a primary or sec- palpable nodule in a taut band.4 When compressed, a MTrP ondary pain source. Instead, emphasis is placed only on muscle may give rise to characteristic referred pain, tenderness, motor mechanical properties such as length and strength.7,8 dysfunction, and autonomic phenomena.4 MTrPs have been The tendency in manual therapy is to consider muscle pain as described as active or latent. Active MTrPs are associated with secondary to joint or nerve dysfunctions. -

1 the Thoracic Wall I
AAA_C01 12/13/05 10:29 Page 8 1 The thoracic wall I Thoracic outlet (inlet) First rib Clavicle Suprasternal notch Manubrium 5 Third rib 1 2 Body of sternum Intercostal 4 space Xiphisternum Scalenus anterior Brachial Cervical Costal cartilage plexus rib Costal margin 3 Subclavian 1 Costochondral joint Floating ribs artery 2 Sternocostal joint Fig.1.3 3 Interchondral joint Bilateral cervical ribs. 4 Xiphisternal joint 5 Manubriosternal joint On the right side the brachial plexus (angle of Louis) is shown arching over the rib and stretching its lowest trunk Fig.1.1 The thoracic cage. The outlet (inlet) of the thorax is outlined Transverse process with facet for rib tubercle Demifacet for head of rib Head Neck Costovertebral T5 joint T6 Facet for Tubercle vertebral body Costotransverse joint Sternocostal joint Shaft 6th Angle rib Costochondral Subcostal groove joint Fig.1.2 Fig.1.4 A typical rib Joints of the thoracic cage 8 The thorax The thoracic wall I AAA_C01 12/13/05 10:29 Page 9 The thoracic cage Costal cartilages The thoracic cage is formed by the sternum and costal cartilages These are bars of hyaline cartilage which connect the upper in front, the vertebral column behind and the ribs and intercostal seven ribs directly to the sternum and the 8th, 9th and 10th ribs spaces laterally. to the cartilage immediately above. It is separated from the abdominal cavity by the diaphragm and communicates superiorly with the root of the neck through Joints of the thoracic cage (Figs 1.1 and 1.4) the thoracic inlet (Fig. -

Rib Mobilizations Kat Hayes, SPT
Rib Mobilizations Kat Hayes, SPT A) Anatomy a. 12 Thoracic Vertebrae i. Superior facet facets anteraior/lateral ii. Inferior facet facets posterior/medial iii. Plane of motion alows more lateral flexion but limited due to ribs iv. T2-10 have a superior and inferior demifacet where rib articulates with two vertebrae b. 12 Ribs i. Costovertebral facet 1. T2-10 rib head has an inferior and superior facet to articulates with 2 vertebrae 2. T1, T11-12 articulates with only one costal facet 3. Kinematics: gliding and rotation ii. Costotransverse Joint 1. Tubercle of rib articulates with on transverse processes 2. Kinematics: gliding wih some rotation c. Sternum i. Ribs 1-7 attach at sternum via costochondral joint ii. Ribs 8-10 articulate to costal cartilage iii. Ribs 11, 12 are not attached B) Young et al. mapped referral patterns for costotransverse joint patterns a. 8 asymptomatic male subjects b. Received consecutive, same day injections to either right T2,4,6 or to their left T3,5,7 c. OmnipaqueTM was injected using fluoroscopy into joint d. Subects were asked to desribe the pian using given descriptors and also VAS including description of referred pain C) Indications a. Rib or Thoracic hypomobility b. Pain c. Shallow breathing D) Contraindications a. Rib fracture b. Osteoperosis c. Hypermobility d. Malignancy e. Systemic inflamitory disease f. Ligamentous laxity E) Precautions a. Pulmonary Disease b. Severe Scoliosis c. Spinal fussion d. Pregnancy F) Assessment a. While patients sitting, assess breathing patern and palpate ribs for movement during inhilation/exhalation i. Are they a chest or belly breather ii. -

Hypofractionated Irradiation of Infra
Guenzi et al. Radiation Oncology (2015) 10:177 DOI 10.1186/s13014-015-0480-y RESEARCH Open Access Hypofractionated irradiation of infra-supraclavicular lymph nodes after axillary dissection in patients with breast cancer post-conservative surgery: impact on late toxicity Marina Guenzi1, Gladys Blandino1*, Maria Giuseppina Vidili3, Deborah Aloi1, Elena Configliacco1, Elisa Verzanini1, Elena Tornari1, Francesca Cavagnetto2 and Renzo Corvò1 Abstract Background: The aim of the present work was to analyse the impact of mild hypofractionated radiotherapy (RT) of infra-supraclavicular lymph nodes after axillary dissection on late toxicity. Methods: From 2007 to 2012, 100 females affected by breast cancer (pT1- T4, pN1-3, pMx) were treated with conservative surgery, Axillary Node Dissection (AND) and loco-regional radiotherapy (whole breast plus infra-supraclavicular fossa). Axillary lymph nodes metastases were confirmed in all women. The median age at diagnosis was 60 years (range 34–83). Tumors were classified according to molecular characteristics: luminal-A 59pts(59%),luminal-B24pts(24%),basal-like10pts(10%),Her-2like7pts(7%).82pts(82%)received hormonal therapy, 9 pts (9 %) neo-adjuvant chemotherapy, 81pts (81 %) adjuvant chemotherapy. All patients received a mild hypofractionated RT: 46 Gy in 20 fractions 4 times a week to whole breast and infra- supraclavicular fossa plus an additional weekly dose of 1,2 Gy to the lumpectomy area. The disease control and treatment related toxicity were analysed in follow-up visits. The extent of lymphedema was analysed by experts in Oncological Rehabilitation. Results: Within a median follow-up of 50 months (range 19–82), 6 (6 %) pts died, 1 pt (1 %) had local progression disease, 2 pts (2 %) developed distant metastasis and 1 subject (1 %) presented both. -
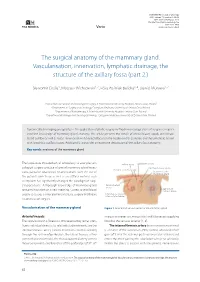
The Surgical Anatomy of the Mammary Gland. Vascularisation, Innervation, Lymphatic Drainage, the Structure of the Axillary Fossa (Part 2.)
NOWOTWORY Journal of Oncology 2021, volume 71, number 1, 62–69 DOI: 10.5603/NJO.2021.0011 © Polskie Towarzystwo Onkologiczne ISSN 0029–540X Varia www.nowotwory.edu.pl The surgical anatomy of the mammary gland. Vascularisation, innervation, lymphatic drainage, the structure of the axillary fossa (part 2.) Sławomir Cieśla1, Mateusz Wichtowski1, 2, Róża Poźniak-Balicka3, 4, Dawid Murawa1, 2 1Department of General and Oncological Surgery, K. Marcinkowski University Hospital, Zielona Gora, Poland 2Department of Surgery and Oncology, Collegium Medicum, University of Zielona Gora, Poland 3Department of Radiotherapy, K. Marcinkowski University Hospital, Zielona Gora, Poland 4Department of Urology and Oncological Urology, Collegium Medicum, University of Zielona Gora, Poland Dynamically developing oncoplasty, i.e. the application of plastic surgery methods in oncological breast surgeries, requires excellent knowledge of mammary gland anatomy. This article presents the details of arterial blood supply and venous blood outflow as well as breast innervation with a special focus on the nipple-areolar complex, and the lymphatic system with lymphatic outflow routes. Additionally, it provides an extensive description of the axillary fossa anatomy. Key words: anatomy of the mammary gland The large-scale introduction of oncoplasty to everyday on- axillary artery subclavian artery cological surgery practice of partial mammary gland resec- internal thoracic artery thoracic-acromial artery tions, partial or total breast reconstructions with the use of branches to the mammary gland the patient’s own tissue as well as an artificial material such as implants has significantly changed the paradigm of surgi- cal procedures. A thorough knowledge of mammary gland lateral thoracic artery superficial anatomy has taken on a new meaning.