Storiform Collagenoma: Case Report Colagenoma Estoriforme: Relato De Caso
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Cytomorphology of Pleomorphic Fibroma of Skin: a Diagnostic Enigma
Case Report Cytomorphology of pleomorphic fibroma of skin: A diagnostic enigma ABSTRACT Pleomorphic fibroma (PF) is a benign, polypoid, or dome‑shaped cutaneous neoplasm with cytologically atypical fibrohistiocytic cells. We describe the cytomorphological features of PF retrospectively with histopathological diagnosis in a 38‑year‑old male who presented with 3 × 1.5 cm swelling in the soft tissues of the thigh for 6 months. This lesion is benign despite the presence of pleomorphic or bizarre cells. We review the differential diagnosis of PF with other mesenchymal tumors. To the best of our knowledge, cytomorphological features on fine needle aspiration cytology of this tumor are not yet documented in literature. Key words: Fine needle aspiration cytology; pleomorphic cells; pleomorphic fibroma. Introduction thigh. Fine needle aspiration cytology (FNAC) was done and slides were stained with Giemsa stain. The aspirate yielded Pleomorphic fibroma (PF) of the skin is a rare benign fibrous cellular smears. Background showed metachromatic stromal tumor.[1] The lesion is usually polypoid, located in the dermis, fragments. Cells were pleomorphic having very large nuclei and is formed by coarse collagen bundles with sparse cells. (monster cells) with scanty cytoplasm. Few of the nuclei It is also characterized by the presence of marked cellular showed single nucleoli [Figure 1]. Nuclear membranes atypia and pleomorphism without mitosis.[1] We describe the frequently showed notches, creases, or folds. Cells were cytomorphological features on fine needle aspiration (FNA) lying singly and occasionally forming clusters. These were smears of a histologically and immunohistochemically proven admixed with the spindle cell component along with few case of PF. -

Immunohistochemical Analysis of S100-Positive Epidermal
An Bras Dermatol. 2020;95(5):627---630 Anais Brasileiros de Dermatologia www.anaisdedermatologia.org.br DERMATOPATHOLOGY Immunohistochemical analysis of S100-positive ଝ,ଝଝ epidermal Langerhans cells in dermatofibroma Mahmoud Rezk Abdelwhaed Hussein Department of Pathology, Assuit University Hospital, Assuit, Egypt Received 3 February 2020; accepted 12 April 2020 Available online 12 July 2020 Abstract Dermatofibroma is a dermal fibrohistiocytic neoplasm. The Langerhans cells are the KEYWORDS immunocompetent cells of the epidermis, and they represent the first defense barrier of the Histiocytoma, benign immune system towards the environment. The objective was to immunohistologically compare fibrous; the densities of S100-positive Langerhans cells in the healthy peritumoral epidermis against Skin neoplasms; those in the epidermis overlying dermatofibroma (20 cases), using antibodies against the S100 S100 Proteins molecule (the immunophenotypic hallmark of Langerhans cells). The control group (normal, healthy skin) included ten healthy age and sex-matched individuals who underwent skin biopsies for benign skin lesions. A significantly high density of Langerhans cells was observed both in the epidermis of the healthy skin (6.00 ± 0.29) and the peritumoral epidermis (6.44 ± 0.41) vs. those in the epidermis overlying the tumor (1.44 ± 0.33, p < 0.05). The quantitative deficit of Langerhans cells in the epidermis overlying dermatofibroma may be a possible factor in its development. © 2020 Sociedade Brasileira de Dermatologia. Published by Elsevier Espana,˜ S.L.U. This is an open access article under the CC BY license (http://creativecommons.org/licenses/by/4.0/). Langerhans cells (LCs) are the exclusive antigen-presenting tions stained with hematoxylin and eosin as ‘‘clear cells’’ cells of the normal human epidermis. -

Dermatofibrosarcoma Protuberans and Dermatofibroma: Dermal Dendrocytomas? a Ultrastructural Study
Dermatofibrosarcoma Protuberans and Dermatofibroma: Dermal Dendrocytomas? A Ultrastructural Study Hugo Dominguez-Malagon, M.D., Ana Maria Cano-Valdez, M.D. Department of Pathology, Instituto Nacional de Cancerología, Mexico. ABSTRACT population of plump spindled cells devoid of cell processes, these cells contained intracytoplasmic lipid droplets and rare Dermatofibroma (DF) and Dermatofibrosarcoma subplasmalemmal densities but lacked MVB. Protuberans (DFSP) are dermal tumors whose histogenesis has not been well defined to date. The differential diagnosis in most With the ultrastructural characteristics and the constant cases is established in routine H/E sections and may be confirmed expression of CD34 in DFSP, a probable origin in dermal by immunohistochemistry; however there are atypical variants dendrocytes is postulated. The histogenesis of DF remains of DF with less clear histological differences and non-conclusive obscure. immunohistochemical results. In such cases electron microscopy studies may be useful to establish the diagnosis. INTRODUCTION In the present paper the ultrastructural characteristics of 38 The histogenesis or differentiation of cases of DFSP and 10 cases of DF are described in detail, the Dermatofibrosarcoma Protuberans (DFSP) and objective was to identify some features potentially useful for Dermatofibroma (DF) is controversial in the literature. For differential diagnosis, and to identify the possible histogenesis of DFSP diverse origins such as fibroblastic,1 fibro-histiocytic2 both neoplasms. Schwannian,3 myofibroblastic,4 perineurial,5,6 and endoneurial (7) have been postulated. DFSP in all cases was formed by stellate or spindled cells with long, slender, ramified cell processes joined by primitive junctions, Regarding DF, most authors are in agreement of a subplasmalemmal densities were frequently seen in the processes. -

Fundamentals of Dermatology Describing Rashes and Lesions
Dermatology for the Non-Dermatologist May 30 – June 3, 2018 - 1 - Fundamentals of Dermatology Describing Rashes and Lesions History remains ESSENTIAL to establish diagnosis – duration, treatments, prior history of skin conditions, drug use, systemic illness, etc., etc. Historical characteristics of lesions and rashes are also key elements of the description. Painful vs. painless? Pruritic? Burning sensation? Key descriptive elements – 1- definition and morphology of the lesion, 2- location and the extent of the disease. DEFINITIONS: Atrophy: Thinning of the epidermis and/or dermis causing a shiny appearance or fine wrinkling and/or depression of the skin (common causes: steroids, sudden weight gain, “stretch marks”) Bulla: Circumscribed superficial collection of fluid below or within the epidermis > 5mm (if <5mm vesicle), may be formed by the coalescence of vesicles (blister) Burrow: A linear, “threadlike” elevation of the skin, typically a few millimeters long. (scabies) Comedo: A plugged sebaceous follicle, such as closed (whitehead) & open comedones (blackhead) in acne Crust: Dried residue of serum, blood or pus (scab) Cyst: A circumscribed, usually slightly compressible, round, walled lesion, below the epidermis, may be filled with fluid or semi-solid material (sebaceous cyst, cystic acne) Dermatitis: nonspecific term for inflammation of the skin (many possible causes); may be a specific condition, e.g. atopic dermatitis Eczema: a generic term for acute or chronic inflammatory conditions of the skin. Typically appears erythematous, -

8.5 X12.5 Doublelines.P65
Cambridge University Press 978-0-521-87409-0 - Modern Soft Tissue Pathology: Tumors and Non-Neoplastic Conditions Edited by Markku Miettinen Index More information Index abdominal ependymoma, 744 mucinous cystadenocarcinoma, 631 adult fibrosarcoma (AF), 364–365, 1026 abdominal extrauterine smooth muscle ovarian adenocarcinoma, 72, 79 adult granulosa cell tumor, 523–524 tumors, 79 pancreatic adenocarcinoma, 846 clinical features, 523 abdominal inflammatory myofibroblastic pulmonary adenocarcinoma, 51 genetics, 524 tumors, 297–298 renal adenocarcinoma, 67 pathology, 523–524 abdominal leiomyoma, 467, 477 serous cystadenocarcinoma, 631 adult rhabdomyoma, 548–549 abdominal leiomyosarcoma. See urinary bladder/urogenital tract clinical features, 548 gastrointestinal stromal tumor adenocarcinoma, 72, 401 differential diagnosis, 549 (GIST) uterine adenocarcinomas, 72 genetics, 549 abdominal perivascular epithelioid cell tumors adenofibroma, 523 pathology, 548–549 (PEComas), 542 adenoid cystic carcinoma, 1035 aggressive angiomyxoma (AAM), 514–518 abdominal wall desmoids, 244 adenomatoid tumor, 811–813 clinical features, 514–516 acquired elastotic hemangioma, 598 adenomatous polyposis coli (APC) gene, 143 differential diagnosis, 518 acquired tufted angioma, 590 adenosarcoma (mullerian¨ adenosarcoma), 523 genetics, 518 acral arteriovenous tumor, 583 adipocytic lesions (cytology), 1017–1022 pathology, 516 acral myxoinflammatory fibroblastic sarcoma atypical lipomatous tumor/well- aggressive digital papillary adenocarcinoma, (AMIFS), 365–370, 1026 differentiated -

Basal Cell Carcinoma Associated with Non-Neoplastic Cutaneous Conditions: a Comprehensive Review
Volume 27 Number 2| February 2021 Dermatology Online Journal || Review 27(2):1 Basal cell carcinoma associated with non-neoplastic cutaneous conditions: a comprehensive review Philip R Cohen MD1,2 Affiliations: 1San Diego Family Dermatology, National City, California, USA, 2Touro University California College of Osteopathic Medicine, Vallejo, California, USA Corresponding Author: Philip R Cohen, 10991 Twinleaf Court, San Diego, CA 92131-3643, Email: [email protected] pathogenesis of BCC is associated with the Abstract hedgehog signaling pathway and mutations in the Basal cell carcinoma (BCC) can be a component of a patched homologue 1 (PCTH-1) transmembrane collision tumor in which the skin cancer is present at tumor-suppressing protein [2-4]. Several potential the same cutaneous site as either a benign tumor or risk factors influence the development of BCC a malignant neoplasm. However, BCC can also concurrently occur at the same skin location as a non- including exposure to ultraviolet radiation, genetic neoplastic cutaneous condition. These include predisposition, genodermatoses, immunosuppression, autoimmune diseases (vitiligo), cutaneous disorders and trauma [5]. (Darier disease), dermal conditions (granuloma Basal cell carcinoma usually presents as an isolated faciale), dermal depositions (amyloid, calcinosis cutis, cutaneous focal mucinosis, osteoma cutis, and tumor on sun-exposed skin [6-9]. However, they can tattoo), dermatitis, miscellaneous conditions occur as collision tumors—referred to as BCC- (rhinophyma, sarcoidal reaction, and varicose veins), associated multiple skin neoplasms at one site scars, surgical sites, systemic diseases (sarcoidosis), (MUSK IN A NEST)—in which either a benign and/or systemic infections (leischmaniasis, leprosy and malignant neoplasm is associated with the BCC at lupus vulgaris), and ulcers. -

Concurrence of a Fibroma and Myxoma in an Oranda Goldfish (Carassius Auratus)
Bull. Eur. Ass. Fish Pathol., 36(6) 2016, 263 Concurrence of a fibroma and myxoma in an oranda goldfish (Carassius auratus) S. Shokrpoor1*, F. Sasani1, H. Rahmati-Holasoo2 and A. Zargar2 1 Department of Pathology, Faculty of Veterinary Medicine, University of Tehran, Tehran, Iran; 2 Department of Aquatic Animal Health, Faculty of Veterinary Medicine, University of Tehran, Tehran, Iran Abstract Concurrence of fibroma and myxoma in an oranda goldfish (Carassius auratus) is described. The fish had two lesions on the dorsal region of the head and the base of the dorsal fin. Histologically, in the lesion on the head the presence of stellate and reticular cells lying in a mucoid matrix was diagnosed as a myxoma. The lesion on the base of dorsal fin was composed of mature fibrocytes producing abundant collagen in interwoven fascicles and was diagnosed as a fibroma. This is the first report of concurrence of fibroma and myxoma in a fish. Introduction Fibromas are benign neoplasms of fibrocytes 2009). Fibromas have been described in electric with abundant collagenous stroma. Myxomas catfish (Malapterurus electricus) (Stolk, 1957), are tumours of fibroblast origin distinguished southern flounder (Paralichthys lethostigma) and by their abundant myxoid matrix rich in muco- the hardhead sea catfish (Arius felis) (Overstreet polysaccharides (Goldschmidt and Hendrick, and Edwards, 1976), flathead grey mullet (Mugil 2002). Among domestic animals, fibromas have cephalus) (Lopez and Raibaut, 1981), redband been frequently described in dogs. However, parrotfish (Sparisoma aurofrenatum) (Grizzle, they are uncommon neoplasms in large animals 1983), common carp (Cyprinus carpio) (Manier (Goldschmidt and Hendrick, 2002). Fibromas et al., 1984) and goldfish (Carassius auratus) in white-tailed and mule deer (Sundberg et (Constantino et al., 1999). -

Robust Surgical Approach for Cutaneous Neurofibroma in Neurofibromatosis Type 1
Robust surgical approach for cutaneous neurofibroma in neurofibromatosis type 1 Bahir H. Chamseddin, … , Juan Vega, Lu Q. Le JCI Insight. 2019. https://doi.org/10.1172/jci.insight.128881. Clinical Medicine In-Press Preview Dermatology Neuroscience BACKGROUND. Cutaneous neurofibromas (cNF) are physically disfiguring, painful, and cause extensive psychologic harm in patients with neurofibromatosis type 1 (NF1). There is currently no effective medical treatment and surgical procedures are inaccessible to most NF1 patients globally. OBJECTIVE. While research is underway to find an effective medical treatment for cNF, there is an urgent need to develop surgical approach that is accessible to all NF1 patients in the world with the skill set and equipment found in most general medical office settings. Here, we present a robust surgical approach to remove cNF that does not require sterile surgical field, utilizes accessible clinical equipment, and can be performed by any health care providers including family practitioners, and physician assistants. METHODS. In a prospective case-series, patients with NF1 underwent this surgical procedure which removes multiple cutaneous neurofibromas. The Dermatology Life Quality Index was given to subjects before and after the procedure as surrogate for patient satisfaction. RESULTS. 83 tumors were removed throughout the body from twelve individuals. Examination at follow-up visits revealed well-healed scars without infection or adverse events including aberrant scarring. Patient satisfaction with the procedure was high with significant improvements […] Find the latest version: https://jci.me/128881/pdf Robust Surgical Approach for Cutaneous Neurofibroma in Neurofibromatosis Type 1 Bahir H. Chamseddin1, La’Nette Hernandez1, Dezehree Solorzano1, Juan Vega1, Lu Q. -

Seborrheic Keratosis
Benign Epidermal and Dermal Tumors REAGAN ANDERSON, DO- PROGRAM DIRECTOR, COLORADO DERMATOLOGY INSTITUTE, RVU PGY3 RESIDENTS- JONATHAN BIELFIELD, GEORGE BRANT PGY2 RESIDENT- MICHELLE ELWAY Seborrheic Keratosis Common benign growth seen after third/fourth decade of life Ubiquitous among older individuals Tan to black, macular, papular, or verrucous lesion Occur everywhere except palms, soles, and mucous membranes Can simulate melanocytic neoplasms Pathogenesis: Sun exposure- Australian study found higher incidence in the head/neck Alteration in distribution of epidermal growth factors Somatic activating mutations in fibroblast growth factor receptor and phosphoinositide-3-kinase Seborrheic Keratosis Sign of Leser-Trelat: Rare cutaneous marker of internal malignancy • Gastric/colonic adenocarcinoma, breast carcinoma, and lymphoma m/c • Abrupt increase in number/size of SKs that can occur before, during, or after an internal malignancy is detected • 40% pruritus • M/C location is the back • Malignant acanthosis nigricans may also appear in 20% of patients • Should resolve when primary tumor is treated, and reappear with recurrence/mets Seborrheic Keratosis 6 Histologic types Acanthotic Hyperkeratotic Reticulated Irritated Clonal Melanoacanthoma Borst-Jadassohn phenomenon Well-demarcated nests of keratinocytes within the epidermis Seborrheic Keratoses Treatment Reassurance Irritated SKs (itching, catching on clothes, inflamed) Cryotherapy, curettage, shave excision Pulsed CO2, erbium:YAG lasers Electrodessication Flegel -

Genital Lesions
Nick Van Wagoner, MD PhD Department of Infectious Diseases University of Alabama at Birmingham By the end of the lecture, the participant should be familiar with: Commonly used dermatological terms Common dermatological conditions seen in STD Clinics Dematology language Genital anatomy Categories of lesions Dermatological conditions seen in the STD clinic Not all individuals presenting to STD Clinics have STDs. Consider other causes for symptoms. History and examination are important in diagnosing non-STD genital findings. How long has it been present? What have you been doing to the skin in that area? Do you have any skin trouble anywhere else? Does this this look like an STD? Has this person been treated for STDs? Did it help? Know your limitations: Ask and Refer Symptoms perceived to be an STD Drips Discharge Dysuria Pain Redness Ulcers Bumps “I have spots on my head where hair won’t grow.” “I have a bump on my arm that hurts.” “I have painful sores on my back. I was told it was herpes.” History Exam Treat STD Reassure Not an STD Treat Refer Macule Patch area of color change area of color change <1.5cm, nonpalpable >1.5cm, nonpalpable From: www.acponline.org From: www.merck.com From: www.dermatology.cdlib.org From: www/missinglink.ucsf.edu From: www.visualdxhealth.com From: www.dermubc.ca From: www.dermubc.ca Papule Plaque area of elevation area of elevation <1.0cm, palpable >1.0cm, palpable elevated From: www.dermatology,about.com From: www.mycology.adelaide.edu/au/gallery From: www/missinglink.ucsf.edu www.dermatology.about.com -

Oral Benign Fibrous Histiocytoma – a Review of Literature from 1964-2016
Review Article Adv Dent & Oral Health Volume 8 Issue 5 - May 2018 Copyright © All rights are reserved by Prasanna Kumar DOI: 10.19080/ADOH.2018.08.555748 Oral Benign Fibrous Histiocytoma – A Review of Literature from 1964-2016 Prasanna Kumar* Rajiv Gandhi University of Health Sciences, India Submission: March 18, 2017; Published: May 17, 2018 *Corresponding author: Prasanna Kumar, Rajiv Gandhi University of Health Sciences, Dept of Oral & MAxillofacial Surgery, Sullia, Bangalore, India, Tel: ; Email: Introduction It all began way before the 1960’s, however on one fateful incidence of metastasis or recurrences if any. day in the year of 1961, Kauffman ST and Stout AP changed the the diagnostic techniques, current protocols in treatment and Discussion way the world looked at fibrous soft tissue tumours by being the separate clinical entity [1]. first to report about Fibrous Histiocytoma and recognising it as a the mean age of patients was 55 years ranging from 12 to 71 years. The oral and perioral cases of BFH, Gray et al. [8] found that Benign fibrous histiocytoma designates a group of quasi- [9] Women are more frequently affected than men. Bielamowicz et differentiation. Whether the lesions originate from histiocytic or neoplastic lesions that show both fibroblastic and histiocytic al. [9] in their study of BFH in the head and neck region found M: F ratio of 2.5:1 [10]. fibroblasticSome experts tissues hypothesize has not been that clearly the determined cells originate yet [2].from the depending upon the location, duration and possible aetiology. The clinical picture as seen in literature varies significantly while others argue that immunohistochemical evidence of factor tissue histiocytes and then assume fibroblastic properties [3] Various causes have been speculated in the aetiology of BFH XII a positivity favours a dermal dendrocytic cell origin [4]. -
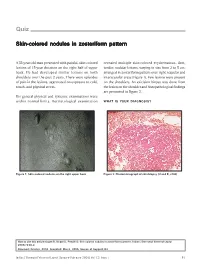
Skin-Colored Nodules in Zosteriform Pattern
Quiz Skin-colored nodules in zosteriform pattern A 33-year-old man presented with painful, skin-colored revealed multiple skin-colored erythematous, firm, lesions of 15-year duration on the right half of upper tender, nodular lesions, varying in size from 2 to 5 cm, back. He had developed similar lesions on both arranged in zosteriform pattern over right scapular and shoulders over the past 2 years. There were episodes interscapular areas (Figure 1). Few lesions were present of pain in the lesions, aggravated on exposure to cold, on the shoulders. An exicision biopsy was done from touch, and physical stress. the lesion on the shoulder and histopathological findings are presented in Figure 2. His general physical and systemic examinations were within normal limits. Dermatological examination WHAT IS YOUR DIAGNOSIS? Figure 1: Skin-colored nodules on the right upper back Figure 2: Photomicrograph of skin biopsy (H and E, x100) How to cite this article: Gupta R, Singal A, Pandhi D. Skin colored nodules in zosteriforms pattern. Indian J Dermatol Venereol Leprol 2005;72:81-2. Received: October, 2004. Accepted: March, 2005. Source of Support: Nil. Indian J Dermatol Venereol Leprol|January-February 2006|Vol 72|Issue 1 81 Quiz Diagnosis: Type-2 segmental leiomyoma cutis via sympathetic nervous system. Muscle contraction ensues, triggered by the influx of calcium ions. Hence, Histopathological findings nifedipine, a calcium channel blocker has a role in Biopsy showed a tumor composed of irregularly relieving pain associated with cutaneous leiomyoma. arranged smooth-muscle fibers, with elongated nuclei and rounded ends, interlaced with variable amounts of Several conditions are associated with piloleiomyoma,[4] collagen in the reticular dermis.