Continuum of Phenotypes in HMSN-P and CMT Patients with TFG Mutation
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Molecular Profile of Tumor-Specific CD8+ T Cell Hypofunction in a Transplantable Murine Cancer Model
Downloaded from http://www.jimmunol.org/ by guest on September 25, 2021 T + is online at: average * The Journal of Immunology , 34 of which you can access for free at: 2016; 197:1477-1488; Prepublished online 1 July from submission to initial decision 4 weeks from acceptance to publication 2016; doi: 10.4049/jimmunol.1600589 http://www.jimmunol.org/content/197/4/1477 Molecular Profile of Tumor-Specific CD8 Cell Hypofunction in a Transplantable Murine Cancer Model Katherine A. Waugh, Sonia M. Leach, Brandon L. Moore, Tullia C. Bruno, Jonathan D. Buhrman and Jill E. Slansky J Immunol cites 95 articles Submit online. Every submission reviewed by practicing scientists ? is published twice each month by Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts http://jimmunol.org/subscription Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html http://www.jimmunol.org/content/suppl/2016/07/01/jimmunol.160058 9.DCSupplemental This article http://www.jimmunol.org/content/197/4/1477.full#ref-list-1 Information about subscribing to The JI No Triage! Fast Publication! Rapid Reviews! 30 days* Why • • • Material References Permissions Email Alerts Subscription Supplementary The Journal of Immunology The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 Copyright © 2016 by The American Association of Immunologists, Inc. All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. This information is current as of September 25, 2021. The Journal of Immunology Molecular Profile of Tumor-Specific CD8+ T Cell Hypofunction in a Transplantable Murine Cancer Model Katherine A. -

A Computational Approach for Defining a Signature of Β-Cell Golgi Stress in Diabetes Mellitus
Page 1 of 781 Diabetes A Computational Approach for Defining a Signature of β-Cell Golgi Stress in Diabetes Mellitus Robert N. Bone1,6,7, Olufunmilola Oyebamiji2, Sayali Talware2, Sharmila Selvaraj2, Preethi Krishnan3,6, Farooq Syed1,6,7, Huanmei Wu2, Carmella Evans-Molina 1,3,4,5,6,7,8* Departments of 1Pediatrics, 3Medicine, 4Anatomy, Cell Biology & Physiology, 5Biochemistry & Molecular Biology, the 6Center for Diabetes & Metabolic Diseases, and the 7Herman B. Wells Center for Pediatric Research, Indiana University School of Medicine, Indianapolis, IN 46202; 2Department of BioHealth Informatics, Indiana University-Purdue University Indianapolis, Indianapolis, IN, 46202; 8Roudebush VA Medical Center, Indianapolis, IN 46202. *Corresponding Author(s): Carmella Evans-Molina, MD, PhD ([email protected]) Indiana University School of Medicine, 635 Barnhill Drive, MS 2031A, Indianapolis, IN 46202, Telephone: (317) 274-4145, Fax (317) 274-4107 Running Title: Golgi Stress Response in Diabetes Word Count: 4358 Number of Figures: 6 Keywords: Golgi apparatus stress, Islets, β cell, Type 1 diabetes, Type 2 diabetes 1 Diabetes Publish Ahead of Print, published online August 20, 2020 Diabetes Page 2 of 781 ABSTRACT The Golgi apparatus (GA) is an important site of insulin processing and granule maturation, but whether GA organelle dysfunction and GA stress are present in the diabetic β-cell has not been tested. We utilized an informatics-based approach to develop a transcriptional signature of β-cell GA stress using existing RNA sequencing and microarray datasets generated using human islets from donors with diabetes and islets where type 1(T1D) and type 2 diabetes (T2D) had been modeled ex vivo. To narrow our results to GA-specific genes, we applied a filter set of 1,030 genes accepted as GA associated. -

1 Supporting Information for a Microrna Network Regulates
Supporting Information for A microRNA Network Regulates Expression and Biosynthesis of CFTR and CFTR-ΔF508 Shyam Ramachandrana,b, Philip H. Karpc, Peng Jiangc, Lynda S. Ostedgaardc, Amy E. Walza, John T. Fishere, Shaf Keshavjeeh, Kim A. Lennoxi, Ashley M. Jacobii, Scott D. Rosei, Mark A. Behlkei, Michael J. Welshb,c,d,g, Yi Xingb,c,f, Paul B. McCray Jr.a,b,c Author Affiliations: Department of Pediatricsa, Interdisciplinary Program in Geneticsb, Departments of Internal Medicinec, Molecular Physiology and Biophysicsd, Anatomy and Cell Biologye, Biomedical Engineeringf, Howard Hughes Medical Instituteg, Carver College of Medicine, University of Iowa, Iowa City, IA-52242 Division of Thoracic Surgeryh, Toronto General Hospital, University Health Network, University of Toronto, Toronto, Canada-M5G 2C4 Integrated DNA Technologiesi, Coralville, IA-52241 To whom correspondence should be addressed: Email: [email protected] (M.J.W.); yi- [email protected] (Y.X.); Email: [email protected] (P.B.M.) This PDF file includes: Materials and Methods References Fig. S1. miR-138 regulates SIN3A in a dose-dependent and site-specific manner. Fig. S2. miR-138 regulates endogenous SIN3A protein expression. Fig. S3. miR-138 regulates endogenous CFTR protein expression in Calu-3 cells. Fig. S4. miR-138 regulates endogenous CFTR protein expression in primary human airway epithelia. Fig. S5. miR-138 regulates CFTR expression in HeLa cells. Fig. S6. miR-138 regulates CFTR expression in HEK293T cells. Fig. S7. HeLa cells exhibit CFTR channel activity. Fig. S8. miR-138 improves CFTR processing. Fig. S9. miR-138 improves CFTR-ΔF508 processing. Fig. S10. SIN3A inhibition yields partial rescue of Cl- transport in CF epithelia. -

The TFG-TEC Oncoprotein Induces Transcriptional Activation of the Human B-Enolase Gene Via Chromatin Modification of the Promoter Region
MOLECULAR CARCINOGENESIS 55:1411–1423 (2016) The TFG-TEC Oncoprotein Induces Transcriptional Activation of the Human b-Enolase Gene Via Chromatin Modification of the Promoter Region Ah-young Kim, Bobae Lim, JeeHyun Choi, and Jungho Kim* Laboratory of Molecular and Cellular Biology, Department of Life Science, Sogang University, Seoul, Korea Recurrent chromosome translocations are the hallmark of many human cancers. A proportion of human extraskeletal myxoid chondrosarcomas (EMCs) are associated with the characteristic chromosomal translocation t(3;9)(q11–12;q22), which results in the formation of a chimeric protein in which the N-terminal domain of the TRK-fused gene (TFG) is fused to the translocated in extraskeletal chondrosarcoma (TEC; also called CHN, CSMF, MINOR, NOR1, and NR4A3) gene. The oncogenic effect of this translocation may be due to the higher transactivation ability of the TFG-TEC chimeric protein; however, downstream target genes of TFG-TEC have not yet been identified. The results presented here, demonstrate that TFG-TEC activates the human b-enolase promoter. EMSAs, ChIP assays, and luciferase reporter assays revealed that TFG-TEC upregulates b-enolase transcription by binding to two NGFI-B response element motifs located upstream of the putative transcription start site. In addition, northern blot, quantitative real-time PCR, and Western blot analyses showed that overexpression of TFG-TEC up-regulated b-enolase mRNA and protein expression in cultured cell lines. Finally, ChIP analyses revealed that TFG-TEC controls the activity of the endogenous b-enolase promoter by promoting histone H3 acetylation. Overall, the results presented here indicate that TFG-TEC triggers a regulatory gene hierarchy implicated in cancer cell metabolism. -

The TRK-Fused Gene Is Mutated in Hereditary Motor and Sensory Neuropathy with Proximal Dominant Involvement
REPORT The TRK-Fused Gene Is Mutated in Hereditary Motor and Sensory Neuropathy with Proximal Dominant Involvement Hiroyuki Ishiura,1 Wataru Sako,3 Mari Yoshida,4 Toshitaka Kawarai,3 Osamu Tanabe,3,5 Jun Goto,1 Yuji Takahashi,1 Hidetoshi Date,1 Jun Mitsui,1 Budrul Ahsan,1 Yaeko Ichikawa,1 Atsushi Iwata,1 Hiide Yoshino,6 Yuishin Izumi,3 Koji Fujita,3 Kouji Maeda,3 Satoshi Goto,3 Hidetaka Koizumi,3 Ryoma Morigaki,3 Masako Ikemura,7 Naoko Yamauchi,7 Shigeo Murayama,8 Garth A. Nicholson,9 Hidefumi Ito,10 Gen Sobue,11 Masanori Nakagawa,12 Ryuji Kaji,3,* and Shoji Tsuji1,2,13,* Hereditary motor and sensory neuropathy with proximal dominant involvement (HMSN-P) is an autosomal-dominant neurodegener- ative disorder characterized by widespread fasciculations, proximal-predominant muscle weakness, and atrophy followed by distal sensory involvement. To date, large families affected by HMSN-P have been reported from two different regions in Japan. Linkage and haplotype analyses of two previously reported families and two new families with the use of high-density SNP arrays further defined the minimum candidate region of 3.3 Mb in chromosomal region 3q12. Exome sequencing showed an identical c.854C>T (p.Pro285- Leu) mutation in the TRK-fused gene (TFG) in the four families. Detailed haplotype analysis suggested two independent origins of the mutation. Pathological studies of an autopsied patient revealed TFG- and ubiquitin-immunopositive cytoplasmic inclusions in the spinal and cortical motor neurons. Fragmentation of the Golgi apparatus, a frequent finding in amyotrophic lateral sclerosis, was also observed in the motor neurons with inclusion bodies. -

Role of Ets-2 Phosphorylation in Inflammation, Development and Cancer
ROLE OF ETS-2 PHOSPHORYLATION IN INFLAMMATION, DEVELOPMENT AND CANCER DISSERTATION Presented in Partial Fulfillment of the Requirement for the Degree Doctor of Philosophy in the Graduate School of The Ohio State University By Guo Wei, M.S. * * * * * The Ohio State University 2003 Dissertation Committee: Approved by: Dr. Michael C. Ostrowski, Adviser Dr. Lee F. Johnson ___________________________________ Adviser Dr. Gustavo Leone Department of Molecular Genetics Dr. Michael Weinstein ABSTRACT Ets family transcription factors are regulated by signal transduction pathways. Phosphorylation of the Ets-1 and Ets-2 at a single conserved threonine residue (T38 and T72, respectively) by ras-MAPK pathways leads to their activation and persistent target genes expression. The phosphorylation of Ets-2 affected its activity, as well as its protein partnership. Ets-2 interacted with Brg-1 or BS69 co-repressors in a phosphorylation dependent manner, and repressed target gene expression. Ets-2 knockout mice are embryonic lethal due to an extra-embryonic defect, whereas ets-2T72A/T72A mice are viable and fertile, with no obvious abnormality. Ets-2 is constitutively phosphorylated in macrophages derived from motheaten-viable (mev) mice, while its phosphorylation is tightly regulated in wt cells. The aberrant Ets-2 phosphorylation correlated with increased target gene expression and cell survival. To directly test the role of Ets-2 phosphorylation in inflammation, the ets-2T72A allele was introduced into mev mice. In contrast to ets2+/+, mev/mev mice, ets-2T72A/T72A, mev/mev mice were fertile, had increased life span and body weight, elevated macrophage apoptosis in the absence of CSF-1, but reduced inflammation and expression of inflammatory genes, including cytokines (TNFα), chemokines (MIP1α, β), extracellular matrix proteases (MMP9), cell adhesion molecule (integrin αM) in lungs and macrophages. -

Unifying the Genomics-Based Classes of Cancer Fusion Gene Partners: Large Cancer Fusion Genes Are Evolutionarily Conserved
CANCER GENOMICS & PROTEOMICS 9: 389-396 (2012) Unifying the Genomics-based Classes of Cancer Fusion Gene Partners: Large Cancer Fusion Genes Are Evolutionarily Conserved LIBIA M. PAVA, DANIEL T. MORTON, REN CHEN and GEORGE BLANCK Department of Molecular Medicine, Morsani College of Medicine, University of South Florida, Tampa, FL, U.S.A. Abstract. Background: Genes that fuse to cause cancer have fusion of NPM and ALK in anaplastic large-cell lymphoma been studied to determine molecular bases for proliferation, to (3); ABL and BCR in chronic myelogenous leukemia (CML) develop diagnostic tools, and as targets for drugs. To facilitate (4, 5); and C-MYC and IgH in Burkitt’s lymphoma in (6), identification of additional, cancer fusion genes, following among many others. The detection and understanding of the observation of a chromosomal translocation, we have ABL-BCR fusion protein, which stimulates unregulated cell characterized the genomic features of the fusion gene partners. division and leads to leukemia, led to the development of Previous work indicated that cancer fusion gene partners, are Gleevec, a drug able to block the ATP-binding site of the either large or evolutionarily conserved in comparison to the tyrosine kinase domain of ABL-BCR, halting CML (7). This neighboring genes in the region of a chromosomal extraordinary success has led to the hope of designing drugs translocation. These results raised the question of whether targeted against other cancer fusion proteins. large cancer fusion gene partners were also evolutionarily There are about 50,000 unstudied translocations, raising conserved. Methods and Results: We developed two methods the question of whether that information can continue to be for quantifying evolutionary conservation values, allowing the used to facilitate the identification of fusion genes. -

The Neurodegenerative Diseases ALS and SMA Are Linked at The
Nucleic Acids Research, 2019 1 doi: 10.1093/nar/gky1093 The neurodegenerative diseases ALS and SMA are linked at the molecular level via the ASC-1 complex Downloaded from https://academic.oup.com/nar/advance-article-abstract/doi/10.1093/nar/gky1093/5162471 by [email protected] on 06 November 2018 Binkai Chi, Jeremy D. O’Connell, Alexander D. Iocolano, Jordan A. Coady, Yong Yu, Jaya Gangopadhyay, Steven P. Gygi and Robin Reed* Department of Cell Biology, Harvard Medical School, 240 Longwood Ave. Boston MA 02115, USA Received July 17, 2018; Revised October 16, 2018; Editorial Decision October 18, 2018; Accepted October 19, 2018 ABSTRACT Fused in Sarcoma (FUS) and TAR DNA Binding Protein (TARDBP) (9–13). FUS is one of the three members of Understanding the molecular pathways disrupted in the structurally related FET (FUS, EWSR1 and TAF15) motor neuron diseases is urgently needed. Here, we family of RNA/DNA binding proteins (14). In addition to employed CRISPR knockout (KO) to investigate the the RNA/DNA binding domains, the FET proteins also functions of four ALS-causative RNA/DNA binding contain low-complexity domains, and these domains are proteins (FUS, EWSR1, TAF15 and MATR3) within the thought to be involved in ALS pathogenesis (5,15). In light RNAP II/U1 snRNP machinery. We found that each of of the discovery that mutations in FUS are ALS-causative, these structurally related proteins has distinct roles several groups carried out studies to determine whether the with FUS KO resulting in loss of U1 snRNP and the other two members of the FET family, TATA-Box Bind- SMN complex, EWSR1 KO causing dissociation of ing Protein Associated Factor 15 (TAF15) and EWS RNA the tRNA ligase complex, and TAF15 KO resulting in Binding Protein 1 (EWSR1), have a role in ALS. -

Autocrine IFN Signaling Inducing Profibrotic Fibroblast Responses By
Downloaded from http://www.jimmunol.org/ by guest on September 23, 2021 Inducing is online at: average * The Journal of Immunology , 11 of which you can access for free at: 2013; 191:2956-2966; Prepublished online 16 from submission to initial decision 4 weeks from acceptance to publication August 2013; doi: 10.4049/jimmunol.1300376 http://www.jimmunol.org/content/191/6/2956 A Synthetic TLR3 Ligand Mitigates Profibrotic Fibroblast Responses by Autocrine IFN Signaling Feng Fang, Kohtaro Ooka, Xiaoyong Sun, Ruchi Shah, Swati Bhattacharyya, Jun Wei and John Varga J Immunol cites 49 articles Submit online. Every submission reviewed by practicing scientists ? is published twice each month by Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts http://jimmunol.org/subscription Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html http://www.jimmunol.org/content/suppl/2013/08/20/jimmunol.130037 6.DC1 This article http://www.jimmunol.org/content/191/6/2956.full#ref-list-1 Information about subscribing to The JI No Triage! Fast Publication! Rapid Reviews! 30 days* Why • • • Material References Permissions Email Alerts Subscription Supplementary The Journal of Immunology The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 Copyright © 2013 by The American Association of Immunologists, Inc. All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. This information is current as of September 23, 2021. The Journal of Immunology A Synthetic TLR3 Ligand Mitigates Profibrotic Fibroblast Responses by Inducing Autocrine IFN Signaling Feng Fang,* Kohtaro Ooka,* Xiaoyong Sun,† Ruchi Shah,* Swati Bhattacharyya,* Jun Wei,* and John Varga* Activation of TLR3 by exogenous microbial ligands or endogenous injury-associated ligands leads to production of type I IFN. -

Proximal Dominant Hereditary Motor and Sensory Neuropathy Association with Mutation in the TRK-Fused Gene
Supplementary Online Content Lee S-S, Lee HJ, Park J-M, et al. Proximal dominant hereditary motor and sensory neuropathy association with mutation in the TRK-fused gene. JAMA Neurol. Published online March 18, 2013. doi:10.1001/jamaneurol.2013.1250. eTable 1. Sample list in FC457 family eTable 2. Microsatellites used for chromosomal mapping of 3q1-q2 and their primers for PCR eTable 3. Nonsynonymous variants which are present in three affected individuals (III-23, -27, -29), but not in an unaffected individual (III-25) eTable 4. Nonsynonymous variants found in CMT genes from the proband (III-27) exome data eFigure 1. Diagram of chromosome 3 mapping region for HMSN-P eFigure 2. TFG expression in the distal sural nerve eReferences. This supplementary material has been provided by the authors to give readers additional information about their work. © 2013 American Medical Association. All rights reserved. Downloaded From: https://jamanetwork.com/ on 09/25/2021 eTable 1. Sample list in FC457 family Samples Sex/age Affected Onset DNA testingb CMT Statusa age(year) phenotype (A/U) II-6 F/89 U - No, L - II-16 M/72 U - No - III-3 F/69 U - No - III-4 F/67 U - No - III-7 F/65 U - No, L - III-12 F/68 U - No, L - III-16 F/52 U - No, L - III-18 F/62 U - No, L - III-23 M/56 A 45 Yes, L, E HMSN-P III-25 M/55 U - No, L, E - III-27 M/51 A 48 Yes, L, E HMSN-P III-28 F/48 U - No, L - III-29 F/48 A 46 Yes, L, E HMSN-P III-30 M/50 U - No, L - III-32 M/59 U - No - III-34 F/58 U - No - IV-1 F/50 U - No - IV-4 M/45 U - No - IV-8 F/34 U - No - IV-9 F/32 C/U - No - IV-10 F/33 C/U - No - IV-11 M/31 A 29 Yes, L HMSN-P IV-12 F/28 C/U - Yes - IV-13 M/27 U - No - IV-17 M/23 C/U - Yes, L - IV-18 F/20 U - No, L - IV-19 M/27 A 27 Yes, L HMSN-P IV-20 M/21 U - No, L - aA: affected, U: unaffected, C/U: clinically unaffected. -

Clinicopathologic and Genomic Characterization of Inflammatory
ORIGINAL ARTICLE Clinicopathologic and Genomic 05/24/2021 on B1Ie3HEQKAtYlViOB6v9JkXYwHPCf2wpOZ6Gj4zLHHows5c8Cwy9/GE8tenobMw6o+askVh8Okj8o5aNeJrpPG5G953b+vs1dmmVmYK5o60oNhSlAcCbJMhr/+1KYGRtyjCfO+GDnjJqT4eFHq0Rgg== by http://journals.lww.com/ajsp from Downloaded Characterization of Inflammatory Myofibroblastic Downloaded Tumors of the Head and Neck from Highlighting a Novel Fusion and Potential Diagnostic Pitfall http://journals.lww.com/ajsp Darcy A. Kerr, MD,*† Lester D.R. Thompson, MD,‡ Laura J. Tafe, MD,*† Vickie Y. Jo, MD,§ Azfar Neyaz, MD,∥ Prashanthi Divakar, MD,¶ Joseph A. Paydarfar, MD,†¶ David A. Pastel, MD,†# Keisuke Shirai, MD, MSc,†** Ivy John, MD,†† Raja R. Seethala, MD,†† by B1Ie3HEQKAtYlViOB6v9JkXYwHPCf2wpOZ6Gj4zLHHows5c8Cwy9/GE8tenobMw6o+askVh8Okj8o5aNeJrpPG5G953b+vs1dmmVmYK5o60oNhSlAcCbJMhr/+1KYGRtyjCfO+GDnjJqT4eFHq0Rgg== Claudia M. Salgado, MD, PhD,‡‡ Vikram Deshpande, MD,∥ Julia A. Bridge, MD,§§∥∥ Karl Kashofer, PhD,¶¶ Iva Brčić, MD,¶¶ and Konstantinos Linos, MD*† event was identified in 92% (n = 11/12) of cases and an additional fl fi Abstract: In ammatory myo broblastic tumor (IMT) is a distinc- case was ALK-positive by IHC but could not be evaluated mo- fi fi tive broblastic and myo broblastic spindle cell neoplasm with an lecularly. ALK represented the driver in all but 1 case. Re- fl fi accompanying in ammatory cell in ltrate and frequent receptor arrangement of ALK, fused with the TIMP3 gene (n = 6) was most tyrosine kinase activation at the molecular level. The tumor may commonly detected, followed by 1 case each of the following fusion recur and rarely metastasizes. IMT is rare in the head and neck gene partnerships: TPM3-ALK, KIF5B-ALK, CARS-ALK, region, and limited information is available about its clin- THBS1-ALK, and a novel alteration, SLC12A2-ROS1.Theex- icopathologic and molecular characteristics in these subsites. -
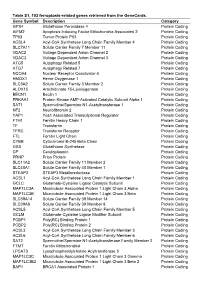
Table S1. 103 Ferroptosis-Related Genes Retrieved from the Genecards
Table S1. 103 ferroptosis-related genes retrieved from the GeneCards. Gene Symbol Description Category GPX4 Glutathione Peroxidase 4 Protein Coding AIFM2 Apoptosis Inducing Factor Mitochondria Associated 2 Protein Coding TP53 Tumor Protein P53 Protein Coding ACSL4 Acyl-CoA Synthetase Long Chain Family Member 4 Protein Coding SLC7A11 Solute Carrier Family 7 Member 11 Protein Coding VDAC2 Voltage Dependent Anion Channel 2 Protein Coding VDAC3 Voltage Dependent Anion Channel 3 Protein Coding ATG5 Autophagy Related 5 Protein Coding ATG7 Autophagy Related 7 Protein Coding NCOA4 Nuclear Receptor Coactivator 4 Protein Coding HMOX1 Heme Oxygenase 1 Protein Coding SLC3A2 Solute Carrier Family 3 Member 2 Protein Coding ALOX15 Arachidonate 15-Lipoxygenase Protein Coding BECN1 Beclin 1 Protein Coding PRKAA1 Protein Kinase AMP-Activated Catalytic Subunit Alpha 1 Protein Coding SAT1 Spermidine/Spermine N1-Acetyltransferase 1 Protein Coding NF2 Neurofibromin 2 Protein Coding YAP1 Yes1 Associated Transcriptional Regulator Protein Coding FTH1 Ferritin Heavy Chain 1 Protein Coding TF Transferrin Protein Coding TFRC Transferrin Receptor Protein Coding FTL Ferritin Light Chain Protein Coding CYBB Cytochrome B-245 Beta Chain Protein Coding GSS Glutathione Synthetase Protein Coding CP Ceruloplasmin Protein Coding PRNP Prion Protein Protein Coding SLC11A2 Solute Carrier Family 11 Member 2 Protein Coding SLC40A1 Solute Carrier Family 40 Member 1 Protein Coding STEAP3 STEAP3 Metalloreductase Protein Coding ACSL1 Acyl-CoA Synthetase Long Chain Family Member 1 Protein