Reversible Renal Failure Due to Psychogenic Urinary Retention
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Mimickers of Urothelial Carcinoma and the Approach to Differential Diagnosis
Review Mimickers of Urothelial Carcinoma and the Approach to Differential Diagnosis Claudia Manini 1, Javier C. Angulo 2,3 and José I. López 4,* 1 Department of Pathology, San Giovanni Bosco Hospital, 10154 Turin, Italy; [email protected] 2 Clinical Department, Faculty of Medical Sciences, European University of Madrid, 28907 Getafe, Spain; [email protected] 3 Department of Urology, University Hospital of Getafe, 28905 Getafe, Spain 4 Department of Pathology, Cruces University Hospital, Biocruces-Bizkaia Health Research Institute, 48903 Barakaldo, Spain * Correspondence: [email protected]; Tel.: +34-94-600-6084 Received: 17 December 2020; Accepted: 18 February 2021; Published: 25 February 2021 Abstract: A broad spectrum of lesions, including hyperplastic, metaplastic, inflammatory, infectious, and reactive, may mimic cancer all along the urinary tract. This narrative collects most of them from a clinical and pathologic perspective, offering urologists and general pathologists their most salient definitory features. Together with classical, well-known, entities such as urothelial papillomas (conventional (UP) and inverted (IUP)), nephrogenic adenoma (NA), polypoid cystitis (PC), fibroepithelial polyp (FP), prostatic-type polyp (PP), verumontanum cyst (VC), xanthogranulomatous inflammation (XI), reactive changes secondary to BCG instillations (BCGitis), schistosomiasis (SC), keratinizing desquamative squamous metaplasia (KSM), post-radiation changes (PRC), vaginal-type metaplasia (VM), endocervicosis (EC)/endometriosis (EM) (müllerianosis), -

Disclosures Objectives
1/16/2015 RbRober tLHllt L. Holley, MSMDFPMRSMSc, MD, FPMRS Professor of Obstetrics and Gynecology Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama at Birmingham School of Medicine Disclosures I have no conflicts of interest pertinent to this lecture. Objectives Appreciate the history associated with the development of the cystoscope Review indications for diagnostic cystourethroscopy Become familiar with instrumentation for diagnostic and operative cystoscopy Become familiar with normal bladder/urethral anatomy and identify abnormal cystoscopic findings 1 1/16/2015 Howard Kelly Bladder distension Scope introduced using an obturator, with pt in kneeknee--chestchest position Negative intraintra--abdominalabdominal pressure allowed air to distend bladder Head mirror to reflect light Greatly improved visualization 20th Century and Today Hopkins/Kopany 1954 FiberFiber--opticoptic scope Rod lens system Angled scopes Complex instrumentation Flexible cystoscope General surgeons developed Urology subspecialty Ob/Gyn combined program decreased cystoscopy training by gynecologists Granting Of Privileges For Cystourethroscopy “Should be based on training, experience and demonstrated competence” “Implies that the physician has knowledge and compete ncy in t he inst ru me ntat io n a nd su r gi cal technique; can recognize normal and abnormal bladder and urethral findings: and has knowledge of pathology, diagnosis and treatment of specific diseases of the lower -

Acute Onset Flank Pain-Suspicion of Stone Disease (Urolithiasis)
Date of origin: 1995 Last review date: 2015 American College of Radiology ® ACR Appropriateness Criteria Clinical Condition: Acute Onset Flank Pain—Suspicion of Stone Disease (Urolithiasis) Variant 1: Suspicion of stone disease. Radiologic Procedure Rating Comments RRL* CT abdomen and pelvis without IV 8 Reduced-dose techniques are preferred. contrast ☢☢☢ This procedure is indicated if CT without contrast does not explain pain or reveals CT abdomen and pelvis without and with 6 an abnormality that should be further IV contrast ☢☢☢☢ assessed with contrast (eg, stone versus phleboliths). US color Doppler kidneys and bladder 6 O retroperitoneal Radiography intravenous urography 4 ☢☢☢ MRI abdomen and pelvis without IV 4 MR urography. O contrast MRI abdomen and pelvis without and with 4 MR urography. O IV contrast This procedure can be performed with US X-ray abdomen and pelvis (KUB) 3 as an alternative to NCCT. ☢☢ CT abdomen and pelvis with IV contrast 2 ☢☢☢ *Relative Rating Scale: 1,2,3 Usually not appropriate; 4,5,6 May be appropriate; 7,8,9 Usually appropriate Radiation Level Variant 2: Recurrent symptoms of stone disease. Radiologic Procedure Rating Comments RRL* CT abdomen and pelvis without IV 7 Reduced-dose techniques are preferred. contrast ☢☢☢ This procedure is indicated in an emergent setting for acute management to evaluate for hydronephrosis. For planning and US color Doppler kidneys and bladder 7 intervention, US is generally not adequate O retroperitoneal and CT is complementary as CT more accurately characterizes stone size and location. This procedure is indicated if CT without contrast does not explain pain or reveals CT abdomen and pelvis without and with 6 an abnormality that should be further IV contrast ☢☢☢☢ assessed with contrast (eg, stone versus phleboliths). -
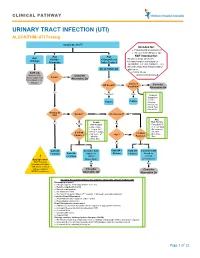
URINARY TRACT INFECTION (UTI) ALGORITHM- UTI Testing
CLINICAL PATHWAY URINARY TRACT INFECTION (UTI) ALGORITHM- UTI Testing Suspicion of UTI Intended for: • Patients with presumed UTI • Greater than 60days of age Age Age NOT intended for: Age 60days- >36months or • Known urologic anomalies <60days • 36months Toilet Trained Chronic/complex conditions (ie. spinabifida, self cath, hardware, etc.) • Recent urinary tract instrumentation Clean Catch UA placement Cath UA • Critical Illness Refer to CCG Consider • Immunocompromised Fever? NO “Fever, infant (less Alternative Dx than 28days or 28- 90days)” Index of UA Result? Neg Low Consider Suspicion* Alternative Dx Yes Pos/Equiv High *Index of Suspicion • Febrile Culture Culture • Dysuria • Frequency • Flank Pain • Hx of UTI History of No Gender? Male Circumcised? YES UTI? Male Female Risk Factors Yes NO Female Risk Factors • Temp ≥ 39°C • Age <12mo • Fever ≥2 days • Temp ≥ 39°C • No source of • ≥ 3 Risk Fever ≥ 2 days infection • No source of ≥ 3 Risk • Non-black Factors? <1yr? No infection Factors? Race • White Race Yes Yes No Yes No Cath UA Consider Cath Cath UA + Cath UA Consider Cath + Culture Cath UA based on Culture + Culture based on ! + Culture clinical clinical Bag Specimen presentation presentation NOT Preferred Neg Neg (consider with labial adhesions, or failed catheterizations) Consider Consider NEVER send culture Alternative Dx Alternative Dx Imaging Recommendations for patients >2months after 1st Febrile UTI No imaging required o Prompt response to therapy (afebrile in 72 hrs) o Reliable outpatient follow up o Normal voiding pattern -

Impact of Urolithiasis and Hydronephrosis on Acute Kidney Injury in Patients with Urinary Tract Infection
bioRxiv preprint doi: https://doi.org/10.1101/2020.07.13.200337; this version posted July 13, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY 4.0 International license. Impact of urolithiasis and hydronephrosis on acute kidney injury in patients with urinary tract infection Short title: Impact of urolithiasis and hydronephrosis on AKI in UTI Chih-Yen Hsiao1,2, Tsung-Hsien Chen1, Yi-Chien Lee3,4, Ming-Cheng Wang5,* 1Division of Nephrology, Department of Internal Medicine, Ditmanson Medical Foundation Chia-Yi Christian Hospital, Chia-Yi, Taiwan 2Department of Hospital and Health Care Administration, Chia Nan University of Pharmacy and Science, Tainan, Taiwan 3Department of Internal Medicine, Fu Jen Catholic University Hospital, Fu Jen Catholic University, New Taipei, Taiwan 4School of Medicine, College of Medicine, Fu Jen Catholic University, New Taipei, Taiwan 5Division of Nephrology, Department of Internal Medicine, National Cheng Kung University Hospital, College of Medicine, National Cheng Kung University, Tainan, Taiwan *[email protected] 1 bioRxiv preprint doi: https://doi.org/10.1101/2020.07.13.200337; this version posted July 13, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY 4.0 International license. Abstract Background: Urolithiasis is a common cause of urinary tract obstruction and urinary tract infection (UTI). This study aimed to identify whether urolithiasis with or without hydronephrosis has an impact on acute kidney injury (AKI) in patients with UTI. -

Obstructive Nephropathy Saulo Klahr
REVIEW ARTICLE Obstructive Nephropathy Saulo Klahr Abstract ages. The incidence of hydronephrosis reported by Bell (1) in a series of32,360 autopsies was 3.8% (3.9% in males, 3.6% in Obstructive nephropathy is a relatively commonentity females). The incidence of clinical manifestations of obstruc- that is treatable and often reversible. It occurs at all ages tive uropathy prior to death was not reported, and it is likely from infancy to elderly subjects. Obstructive uropathy is that hydronephrosis was an incidental finding in many of these classified according to the degree, duration and site of the patients. The incidence of hydronephrosis at autopsy is some- obstruction. It is the result of functional or anatomic le- what lower in children than in adults, being 2%in one series of sions located in the urinary tract. The causes of obstructive 16, 100 autopsies (2). Over 80% of children with hydronephro- uropathy are many. Obstruction of the urinary tract may sis at autopsy were less than 1 year old, with the balance of decrease renal blood flow and the glomerular filtration rate. childhood cases being distributed uniformly through the child- Several abnormalities in tubular function mayoccur in hood years. About 166 patients per 100,000 population had a obstructive nephropathy. These include decreased reab- presumptive diagnosis of obstructive uropathy on admission sorption of solutes and water, inability to concentrate the to hospitals in the United States in 1985 (3). Amongmale pa- urine and impaired excretion of hydrogen and potassium. tients with kidney and urologic disorders, obstructive uropa- Renal interstitial fibrosis is a commonfinding in patients thy ranked fourth at discharge (242 patients/100,000 dis- with long-term obstructive uropathy. -

Case Report Pseudomembranous Trigonitis in a Male with Klinefelter Syndrome: a Case Report and Evidence of a Hormonal Etiology
Int J Clin Exp Pathol 2014;7(6):3375-3379 www.ijcep.com /ISSN:1936-2625/IJCEP0000435 Case Report Pseudomembranous trigonitis in a male with Klinefelter syndrome: a case report and evidence of a hormonal etiology Derrick WQ Lian1, Fay X Li2, Caroline CP Ong2, CH Kuick1, Kenneth TE Chang1 Departments of 1Pathology and Laboratory Medicine, 2Paediatric Surgery, KK Women’s and Children’s Hospital, Singapore Received April 6, 2014; Accepted May 26, 2014; Epub May 15, 2014; Published June 1, 2014 Abstract: Klinefelter syndrome is a clinical syndrome with a distinct 47, XXY karyotype. Patients are characterized by a tall eunuchoid stature, small testes, hypergonotrophic hypogonadism, gynecomastia, learning difficulties and infertility. These patients have also been found to have raised estrogen levels. We report a 16 year old boy with Kline- felter syndrome presenting to our institution with gross hematuria. Cystoscopy and biopsy revealed the diagnosis of pseudomembranous trigonitis. Immunohistochemical stains showed an increase in estrogen and progesterone receptors in the trigone area but not in the rest of the bladder. In view of the patient’s mildly raised estrogen levels and the histological findings, we postulate that estrogen is the driver of the development of pseudomembranous trigonitis. This is the first reported case of pseudomembranous trigonitis seen in association with Klinefelter syn- drome, and also the first case of pseudomembranous trigonitis occurring within the male adolescent age group. Keywords: Klinefelter syndrome, pseudomembranous trigonitis, pediatric Introduction with a sense of incomplete voiding. These epi- sodes were initially treated with a course of oral Klinefelter syndrome is the most common chro- antibiotics by a primary care physician with no mosomal aberration in males and the most resolution of symptoms. -

Primary Obstructive Megaureter in a Child: a Case Report and Review of Literature
Case Report Annals of Pediatric Research Published: 10 May, 2019 Primary Obstructive Megaureter in a Child: A Case Report and Review of Literature Volkan Sarper Erikci* and Tunahan Altundag Department of Pediatric Surgery, Tepecik Training Hospital, Turkey Abstract Ureterovesical Junction Obstruction (UVJO) is a rare but important cause of hydroureteronephrosis in childhood. A 2-years-old boy suffered from giant hydroureteronephrosis originating from idiopathic ureterovesical junction obstruction. He was treated with excision of narrow ureteric segment with tapering ureteroplasty and a ureteral reimplantation was performed. This case is presented and discussed with reference to etiology of this rather rare anomaly. Keywords: Hydroureteronephrosis; Ureterovesical junction obstruction; Children Introduction Congenital Ureterovesical Junction Obstruction (UVJO) may be observed during fetal age or any stage at the time of childhood. It is aimed in this report to present a male child with obstructive megaureter due to congenital UVJO. He was surgically treated with excision of narrowed distal ureter in addition to tapering ureteroplasty with ureteroneocystostomy. The topic is discussed with special reference to the etiology of this rather rare entity under the light of relevant literature. Case Presentation A 27-months-old boy was admitted to our department with an antenatal history of right Hydroureteronephrosis (HUN). Laboratory tests were otherwise normal except signs of Urinary OPEN ACCESS Tract Infection (UTI) including leucocyturia. -

The Presentation and Management of Neonatal Obstructive Uropathies J
Postgrad Med J: first published as 10.1136/pgmj.48.562.486 on 1 August 1972. Downloaded from Postgraduate Medical Journal (August 1972) 48, 486 -492. The presentation and management of neonatal obstructive uropathies J. H. JOHNSTON F.R.C.S. Alder Hey Children's Hospital, Liverpool Presentation urinary, alimentary and genital tracts share a The existence of a congenital urinary obstruction common evacuatory channel is similarly frequently may be suggested when routine examination of the associated with upper urinary tract lesions. newborn infant reveals such signs as enlargement of one or both kidneys, distension of the bladder or (3) Anomalies of the female genital tract slow, dribbling micturition. The paediatrician should Congenital absence of the vagina is associated also be alerted to the possibility of obstructive uro- with urinary tract anomalies in some 500 of cases pathy when there are present non-urological con- (Bryan, Nigro & Counsellor, 1949). A similar high genital anomalies which often secondarily involve incidence occurs with such conditions as duplication the urinary tract or which are known commonly to ofthe vagina and uterus but these may not be obvious co-exist with congenital urinary tract lesions. clinically in the young child. Secondary involvement, with obstruction, of the urinary tract occurs with space-occupying masses in Deficient abdominal mucsculature (4) by copyright. the pelvis such as hydrometrocolpos or a large intra- Urinary tract anomalies of various degrees of pelvic component of a sacrococcygeal teratoma. are The pelvic tumour, by displacing the bladder, leads severity always present. to chronic urinary retention and upper tract dilata- Cardiac anomalies tion. -

Topical Use of Cortisone in Urology T
Topical Use of Cortisone in Urology T. L. SCHULTE, M.D., LLOYD R. REYNOLDS, M.D., and HOWARD J. HAMMER, M.D., San Francisco TOPICAL APPLICATION of cortisone acetate has been * Cortisone was instilled into the bladder in used by the authors in treatment of interstitial the treatment of interstitial cystitis and con- cystitis including contracted bladder, inflammation tracted bladder, trigonitis and urethritis in fe- of the wall of the bladder, trigonitis and urethritis males, nonspecific urethritis in males, and in- in females, and non-specific urethritis in males. flammation of the wall of the bladder. In infec- To determine whether or not any of the results tious cases the hormonal therapy was used after of topical therapy might be owing to systemic ab- antibacterial measures had failed. Improvement sorption of cortisone, study was made of the eosino- occurred quickly in most cases soon after corti- phil content of the blood of patients receiving topical sone therapy was given. In a few cases of inter- therapy. The eosinophil content was determined at stitial cystitis and contracted bladder the relief hourly intervals for six hours after treatment, and obtained was inadequate and it was necessary no significant change was noted. It was concluded to carry out overdistention procedures under that if there was systemic absorption it was so slight visualization. When that was done, however, it that it could not be considered a factor in results. was noted that the condition of the bladder was In all cases in which there were indications of improved as compared with the conditions us- infectious disease of the urinary tract, attempt was ually observed in cases in which cortisone treat- made to clear it by use of antibacterial drugs, but ment is not given before the procedure. -

Acute Necrotizing Ureteritis with Obstructive Uropathy Following Instillation of Silver Nitrate in Chyluria: a Case Report
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Elsevier - Publisher Connector C.M. Su, Y.C. Lee, W.J. Wu, et al ACUTE NECROTIZING URETERITIS WITH OBSTRUCTIVE UROPATHY FOLLOWING INSTILLATION OF SILVER NITRATE IN CHYLURIA: A CASE REPORT Chin-Ming Su, Yung-Chin Lee, Wen-Jen Wu, Hung-Lung Ke, Yii-Her Chou, and Chun-Hsiung Huang Department of Urology, Kaohsiung Medical University, Kaohsiung, Taiwan. Chyluria occurs as a result of communication between the lymphatics and the renal pelvis. It is believed that instillation of silver nitrate into the renal pelvis is a safe, minimally invasive and effective treatment for chyluria. We report an unusual complication of acute necrotizing ureteritis following instillation of silver nitrate in a case of chyluria. It resolved completely with non-surgical intervention. The diagnosis and management of chyluria is discussed, with a brief review of the literature. Key Words: chyluria, silver nitrate instillation, necrotizing ureteritis (Kaohsiung J Med Sci 2004;20:512–5) Chyluria occurs as a result of communication between the radiation, or parasite infection were known. The patient lymphatics and the renal pelvis. Its etiology may be classi- underwent cystoscopic examination following a fatty fied as parasitic or non-parasitic. Although the disease is meal. A milky efflux was observed from the right ureteral not life-threatening, it may cause hypoproteinemia, weight orifice. Retrograde pyelography was normal, with no loss, and immunologic disorders due to severe proteinuria pyelolymphatic backflow (Figure 1). Under the diagnosis of [1]. The treatment of chyluria includes limitation of diet to chyluria, 10 mL of 1% silver nitrate was instilled through a mid-chain triglycerides, instillation of silver nitrate, and ureteric catheter. -

The Acute Scrotum 12 Module 2
Department of Urology Medical Student Handbook INDEX Introduction 1 Contact Information 3 Chairman’s Welcome 4 What is Urology? 5 Urology Rotation Overview 8 Online Teaching Videos 10 Required Readings 11 Module 1. The Acute Scrotum 12 Module 2. Adult Urinary Tract Infections (UTI) 22 Module 3. Benign Prostatic Hyperplasia (BPH) 38 Module 4. Erectile Dysfunction (ED) 47 Module 5. Hematuria 56 Module 6. Kidney Stones 64 Module 7. Pediatric Urinary Tract Infections (UTI) 77 Module 8. Prostate Cancer: Screening and Management 88 Module 9. Urinary Incontinence 95 Module 10. Male Infertility 110 Urologic Abbreviations 118 Suggested Readings 119 Evaluation Process 121 Mistreatment/Harassment Policy 122 Research Opportunities 123 INTRODUCTION Hello, and welcome to Urology! You have chosen a great selective during your Surgical and Procedural Care rotation. Most of the students who take this subspecialty course enjoy themselves and learn more than they thought they would when they signed up for it. During your rotation you will meet a group of urologists who are excited about their medical specialty and feel privileged to work in it. Urology is a rapidly evolving technological specialty that requires surgical and diagnostic skills. Watch the video “Why Urology?” for a brief introduction to the field from the American Urological Association (AUA). https://youtu.be/kyvDMz9MEFA Urology at UW Urology is a specialty that treats patients with many different kinds of problems. At the UW you will see: patients with kidney problems including kidney cancer