The Presentation and Management of Neonatal Obstructive Uropathies J
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Renal Agenesis, Renal Tubular Dysgenesis, and Polycystic Renal Diseases
Developmental & Structural Anomalies of the Genitourinary Tract DR. Alao MA Bowen University Teach Hosp Ogbomoso Picture test Introduction • Congenital Anomalies of the Kidney & Urinary Tract (CAKUT) Objectives • To review the embryogenesis of UGS and dysmorphogenesis of CAKUT • To describe the common CAKUT in children • To emphasize the role of imaging in the diagnosis of CAKUT Introduction •CAKUT refers to gross structural anomalies of the kidneys and or urinary tract present at birth. •Malformation of the renal parenchyma resulting in failure of normal nephron development as seen in renal dysplasia, renal agenesis, renal tubular dysgenesis, and polycystic renal diseases. Introduction •Abnormalities of embryonic migration of the kidneys as seen in renal ectopy (eg, pelvic kidney) and fusion anomalies, such as horseshoe kidney. •Abnormalities of the developing urinary collecting system as seen in duplicate collecting systems, posterior urethral valves, and ureteropelvic junction obstruction. Introduction •Prevalence is about 3-6 per 1000 births •CAKUT is one of the commonest anomalies found in human. •It constitute approximately 20 to 30 percent of all anomalies identified in the prenatal period •The presence of CAKUT in a child raises the chances of finding congenital anomalies of other organ-systems Why the interest in CAKUT? •Worldwide, CAKUT plays a causative role in 30 to 50 percent of cases of end-stage renal disease (ESRD), •The presence of CAKUT, especially ones affecting the bladder and lower tract adversely affects outcome of kidney graft after transplantation Why the interest in CAKUT? •They significantly predispose the children to UTI and urinary calculi •They may be the underlying basis for urinary incontinence Genes & Environment Interact to cause CAKUT? • Tens of different genes with role in nephrogenesis have been identified. -

Acute Onset Flank Pain-Suspicion of Stone Disease (Urolithiasis)
Date of origin: 1995 Last review date: 2015 American College of Radiology ® ACR Appropriateness Criteria Clinical Condition: Acute Onset Flank Pain—Suspicion of Stone Disease (Urolithiasis) Variant 1: Suspicion of stone disease. Radiologic Procedure Rating Comments RRL* CT abdomen and pelvis without IV 8 Reduced-dose techniques are preferred. contrast ☢☢☢ This procedure is indicated if CT without contrast does not explain pain or reveals CT abdomen and pelvis without and with 6 an abnormality that should be further IV contrast ☢☢☢☢ assessed with contrast (eg, stone versus phleboliths). US color Doppler kidneys and bladder 6 O retroperitoneal Radiography intravenous urography 4 ☢☢☢ MRI abdomen and pelvis without IV 4 MR urography. O contrast MRI abdomen and pelvis without and with 4 MR urography. O IV contrast This procedure can be performed with US X-ray abdomen and pelvis (KUB) 3 as an alternative to NCCT. ☢☢ CT abdomen and pelvis with IV contrast 2 ☢☢☢ *Relative Rating Scale: 1,2,3 Usually not appropriate; 4,5,6 May be appropriate; 7,8,9 Usually appropriate Radiation Level Variant 2: Recurrent symptoms of stone disease. Radiologic Procedure Rating Comments RRL* CT abdomen and pelvis without IV 7 Reduced-dose techniques are preferred. contrast ☢☢☢ This procedure is indicated in an emergent setting for acute management to evaluate for hydronephrosis. For planning and US color Doppler kidneys and bladder 7 intervention, US is generally not adequate O retroperitoneal and CT is complementary as CT more accurately characterizes stone size and location. This procedure is indicated if CT without contrast does not explain pain or reveals CT abdomen and pelvis without and with 6 an abnormality that should be further IV contrast ☢☢☢☢ assessed with contrast (eg, stone versus phleboliths). -
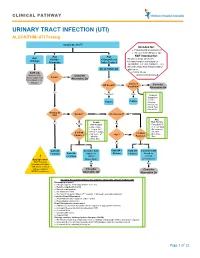
URINARY TRACT INFECTION (UTI) ALGORITHM- UTI Testing
CLINICAL PATHWAY URINARY TRACT INFECTION (UTI) ALGORITHM- UTI Testing Suspicion of UTI Intended for: • Patients with presumed UTI • Greater than 60days of age Age Age NOT intended for: Age 60days- >36months or • Known urologic anomalies <60days • 36months Toilet Trained Chronic/complex conditions (ie. spinabifida, self cath, hardware, etc.) • Recent urinary tract instrumentation Clean Catch UA placement Cath UA • Critical Illness Refer to CCG Consider • Immunocompromised Fever? NO “Fever, infant (less Alternative Dx than 28days or 28- 90days)” Index of UA Result? Neg Low Consider Suspicion* Alternative Dx Yes Pos/Equiv High *Index of Suspicion • Febrile Culture Culture • Dysuria • Frequency • Flank Pain • Hx of UTI History of No Gender? Male Circumcised? YES UTI? Male Female Risk Factors Yes NO Female Risk Factors • Temp ≥ 39°C • Age <12mo • Fever ≥2 days • Temp ≥ 39°C • No source of • ≥ 3 Risk Fever ≥ 2 days infection • No source of ≥ 3 Risk • Non-black Factors? <1yr? No infection Factors? Race • White Race Yes Yes No Yes No Cath UA Consider Cath Cath UA + Cath UA Consider Cath + Culture Cath UA based on Culture + Culture based on ! + Culture clinical clinical Bag Specimen presentation presentation NOT Preferred Neg Neg (consider with labial adhesions, or failed catheterizations) Consider Consider NEVER send culture Alternative Dx Alternative Dx Imaging Recommendations for patients >2months after 1st Febrile UTI No imaging required o Prompt response to therapy (afebrile in 72 hrs) o Reliable outpatient follow up o Normal voiding pattern -

Impact of Urolithiasis and Hydronephrosis on Acute Kidney Injury in Patients with Urinary Tract Infection
bioRxiv preprint doi: https://doi.org/10.1101/2020.07.13.200337; this version posted July 13, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY 4.0 International license. Impact of urolithiasis and hydronephrosis on acute kidney injury in patients with urinary tract infection Short title: Impact of urolithiasis and hydronephrosis on AKI in UTI Chih-Yen Hsiao1,2, Tsung-Hsien Chen1, Yi-Chien Lee3,4, Ming-Cheng Wang5,* 1Division of Nephrology, Department of Internal Medicine, Ditmanson Medical Foundation Chia-Yi Christian Hospital, Chia-Yi, Taiwan 2Department of Hospital and Health Care Administration, Chia Nan University of Pharmacy and Science, Tainan, Taiwan 3Department of Internal Medicine, Fu Jen Catholic University Hospital, Fu Jen Catholic University, New Taipei, Taiwan 4School of Medicine, College of Medicine, Fu Jen Catholic University, New Taipei, Taiwan 5Division of Nephrology, Department of Internal Medicine, National Cheng Kung University Hospital, College of Medicine, National Cheng Kung University, Tainan, Taiwan *[email protected] 1 bioRxiv preprint doi: https://doi.org/10.1101/2020.07.13.200337; this version posted July 13, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY 4.0 International license. Abstract Background: Urolithiasis is a common cause of urinary tract obstruction and urinary tract infection (UTI). This study aimed to identify whether urolithiasis with or without hydronephrosis has an impact on acute kidney injury (AKI) in patients with UTI. -

Obstructive Nephropathy Saulo Klahr
REVIEW ARTICLE Obstructive Nephropathy Saulo Klahr Abstract ages. The incidence of hydronephrosis reported by Bell (1) in a series of32,360 autopsies was 3.8% (3.9% in males, 3.6% in Obstructive nephropathy is a relatively commonentity females). The incidence of clinical manifestations of obstruc- that is treatable and often reversible. It occurs at all ages tive uropathy prior to death was not reported, and it is likely from infancy to elderly subjects. Obstructive uropathy is that hydronephrosis was an incidental finding in many of these classified according to the degree, duration and site of the patients. The incidence of hydronephrosis at autopsy is some- obstruction. It is the result of functional or anatomic le- what lower in children than in adults, being 2%in one series of sions located in the urinary tract. The causes of obstructive 16, 100 autopsies (2). Over 80% of children with hydronephro- uropathy are many. Obstruction of the urinary tract may sis at autopsy were less than 1 year old, with the balance of decrease renal blood flow and the glomerular filtration rate. childhood cases being distributed uniformly through the child- Several abnormalities in tubular function mayoccur in hood years. About 166 patients per 100,000 population had a obstructive nephropathy. These include decreased reab- presumptive diagnosis of obstructive uropathy on admission sorption of solutes and water, inability to concentrate the to hospitals in the United States in 1985 (3). Amongmale pa- urine and impaired excretion of hydrogen and potassium. tients with kidney and urologic disorders, obstructive uropa- Renal interstitial fibrosis is a commonfinding in patients thy ranked fourth at discharge (242 patients/100,000 dis- with long-term obstructive uropathy. -

Evolving Concepts in Human Renal Dysplasia
DISEASE OF THE MONTH J Am Soc Nephrol 15: 998–1007, 2004 EBERHARD RITZ, FEATURE EDITOR Evolving Concepts in Human Renal Dysplasia ADRIAN S. WOOLF, KAREN L. PRICE, PETER J. SCAMBLER, and PAUL J.D. WINYARD Nephro-Urology and Molecular Medicine Units, Institute of Child Health, University College London, London, United Kingdom Abstract. Human renal dysplasia is a collection of disorders in correlating with perturbed cell turnover and maturation. Mu- which kidneys begin to form but then fail to differentiate into tations of nephrogenesis genes have been defined in multiorgan normal nephrons and collecting ducts. Dysplasia is the princi- dysmorphic disorders in which renal dysplasia can feature, pal cause of childhood end-stage renal failure. Two main including Fraser, renal cysts and diabetes, and Kallmann syn- theories have been considered in its pathogenesis: A primary dromes. Here, it is possible to begin to understand the normal failure of ureteric bud activity and a disruption produced by nephrogenic function of the wild-type proteins and understand fetal urinary flow impairment. Recent studies have docu- how mutations might cause aberrant organogenesis. mented deregulation of gene expression in human dysplasia, Congenital anomalies of the kidney and urinary tract and the main renal pathology is renal dysplasia (RD). In her (CAKUT) account for one third of all anomalies detected by landmark book Normal and Abnormal Development of the routine fetal ultrasonography (1). A recent UK audit of child- Kidney published in 1972 (7), Edith Potter emphasized that one hood end-stage renal failure reported that CAKUT was the must understand normal development to generate realistic hy- cause in ~40% of 882 individuals (2). -

Primary Obstructive Megaureter in a Child: a Case Report and Review of Literature
Case Report Annals of Pediatric Research Published: 10 May, 2019 Primary Obstructive Megaureter in a Child: A Case Report and Review of Literature Volkan Sarper Erikci* and Tunahan Altundag Department of Pediatric Surgery, Tepecik Training Hospital, Turkey Abstract Ureterovesical Junction Obstruction (UVJO) is a rare but important cause of hydroureteronephrosis in childhood. A 2-years-old boy suffered from giant hydroureteronephrosis originating from idiopathic ureterovesical junction obstruction. He was treated with excision of narrow ureteric segment with tapering ureteroplasty and a ureteral reimplantation was performed. This case is presented and discussed with reference to etiology of this rather rare anomaly. Keywords: Hydroureteronephrosis; Ureterovesical junction obstruction; Children Introduction Congenital Ureterovesical Junction Obstruction (UVJO) may be observed during fetal age or any stage at the time of childhood. It is aimed in this report to present a male child with obstructive megaureter due to congenital UVJO. He was surgically treated with excision of narrowed distal ureter in addition to tapering ureteroplasty with ureteroneocystostomy. The topic is discussed with special reference to the etiology of this rather rare entity under the light of relevant literature. Case Presentation A 27-months-old boy was admitted to our department with an antenatal history of right Hydroureteronephrosis (HUN). Laboratory tests were otherwise normal except signs of Urinary OPEN ACCESS Tract Infection (UTI) including leucocyturia. -

Congenital Anomalies 899 Which Tend to Decrease in Caliber After Excision of the Aperistaltic Distal Segment
I. UPPER URINARY TRACT A. Abnormalities of the Kidney Position and Number 1. Simple ectopia a) Incidence is approximately 1 per 900 (autopsy) (pelvic, 1 per 3000; solitary, 1 per 22,000; bilateral, 10%). Left side favored. b) Associated findings include small size with persistent fetal lobations, anterior or horizontal pelvis, anomalous vasculature, contralateral agenesis, vesicoureteral reflux, Mu¨llerian anomalies in 20–60% of females; undescended testes, hypospadias, urethral duplication in 10– 20% males; skeletal and cardiac anomalies in 20%. c) Only workup, ultrasound, voiding cystourethrography. 2. Thoracic ectopia a) Comprises less than 5% of ectopic kidneys. b) Origin is delayed closure of diaphragmatic angle versus ‘‘overshoot’’ of renal ascent. c) Adrenal may or may not be thoracic. 3. Crossed ectopia and fusion a) Incidence is 1 per 1000 to 1 per 2000; 90% crossed with fusion; 2:1 male, 3:1 left crossed; 24 cases solitary, five cases bilateral reported to date. b) Origin from abnormal migration of ureteral bud or rotation of caudal end of fetus at time of bud formation c) Associated findings include multiple or anomalous vessels arising from the ipsilateral side of the aorta and vesicoureteral reflux; with solitary crossed kidney only; genital, skeletal, and hindgut anomalies . 4. Horseshoe kidney c) Associated findings include anomalous vessels; isthmus between or behind great vessels hindered by the inferior mesenteric artery; skeletal, cardiovascular, and central nervous system (CNS) anomalies (33%); hypospadias and cryptorchidism (4%), bicornuate uterus (7%), urinary tract infection (UTI) (13%); duplex ureters (10%), stones (17%); 20% of trisomy 18 and 60% of Turner’s patients have horseshoe kidney. -

Acute Necrotizing Ureteritis with Obstructive Uropathy Following Instillation of Silver Nitrate in Chyluria: a Case Report
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Elsevier - Publisher Connector C.M. Su, Y.C. Lee, W.J. Wu, et al ACUTE NECROTIZING URETERITIS WITH OBSTRUCTIVE UROPATHY FOLLOWING INSTILLATION OF SILVER NITRATE IN CHYLURIA: A CASE REPORT Chin-Ming Su, Yung-Chin Lee, Wen-Jen Wu, Hung-Lung Ke, Yii-Her Chou, and Chun-Hsiung Huang Department of Urology, Kaohsiung Medical University, Kaohsiung, Taiwan. Chyluria occurs as a result of communication between the lymphatics and the renal pelvis. It is believed that instillation of silver nitrate into the renal pelvis is a safe, minimally invasive and effective treatment for chyluria. We report an unusual complication of acute necrotizing ureteritis following instillation of silver nitrate in a case of chyluria. It resolved completely with non-surgical intervention. The diagnosis and management of chyluria is discussed, with a brief review of the literature. Key Words: chyluria, silver nitrate instillation, necrotizing ureteritis (Kaohsiung J Med Sci 2004;20:512–5) Chyluria occurs as a result of communication between the radiation, or parasite infection were known. The patient lymphatics and the renal pelvis. Its etiology may be classi- underwent cystoscopic examination following a fatty fied as parasitic or non-parasitic. Although the disease is meal. A milky efflux was observed from the right ureteral not life-threatening, it may cause hypoproteinemia, weight orifice. Retrograde pyelography was normal, with no loss, and immunologic disorders due to severe proteinuria pyelolymphatic backflow (Figure 1). Under the diagnosis of [1]. The treatment of chyluria includes limitation of diet to chyluria, 10 mL of 1% silver nitrate was instilled through a mid-chain triglycerides, instillation of silver nitrate, and ureteric catheter. -

Congenital Anomalies of Kidney and Ureter
ogy: iol Cu ys r h re P n t & R y e s Anatomy & Physiology: Current m e o a t Mittal et al., Anat Physiol 2016, 6:1 r a c n h A Research DOI: 10.4172/2161-0940.1000190 ISSN: 2161-0940 Review Article Open Access Congenital Anomalies of Kidney and Ureter Mittal MK1, Sureka B1, Mittal A2, Sinha M1, Thukral BB1 and Mehta V3* 1Department of Radiodiagnosis, Safdarjung Hospital, India 2Department of Paediatrics, Safdarjung Hospital, India 3Department of Anatomy, Safdarjung Hospital, India Abstract The kidney is a common site for congenital anomalies which may be responsible for considerable morbidity among young patients. Radiological investigations play a central role in diagnosing these anomalies with the screening ultrasonography being commonly used as a preliminary diagnostic study. Intravenous urography can be used to specifically identify an area of obstruction and to determine the presence of duplex collecting systems and a ureterocele. Computed tomography and magnetic resonance (MR) imaging are unsuitable for general screening but provide superb anatomic detail and added diagnostic specificity. A sound knowledge of the anatomical details and familiarity with these anomalies is essential for correct diagnosis and appropriate management so as to avoid the high rate of morbidity associated with these malformations. Keywords: Kidney; Ureter; Intravenous urography; Duplex a separate ureter is seen then the supernumerary kidney is located cranially in relation to the normal kidney. In such a case the ureter Introduction enters the bladder ectopically and according to the Weigert-R Meyer Congenital anomalies of the kidney and ureter are a significant cause rule the ureter may insert medially and inferiorly into the bladder [2]. -

Obstructive Uropathy in Children – an Update RANJIT RANJAN ROY1, MD FIROZ ANJUM2, SHAHANA FERDOUS3
BANGLADESH J CHILD HEALTH 2017; VOL 41 (2): 110-116 Obstructive Uropathy in Children – An Update RANJIT RANJAN ROY1, MD FIROZ ANJUM2, SHAHANA FERDOUS3 Abstract: Obstructive nephropathy is a structural or functional hindrance of normal urine flow, sometimes leading to renal dysfunction. Urinary tract obstruction can result from congenital (anatomic) lesion or can be caused by trauma, neoplasia, calculi, inflammation or surgical procedures, although most childhood obstructive lesions are congenital.The clinical features in most of the patients are due to consequences of the obstruction2. Obstruction of the urinary tract generally causeshydronephrosis, which is typically asymptomatic in its early phase. Renal USG gives information about urinary tract dilatation, renal cortical thickness, calyx size, diameter of pelvis, ureter, bladder thickness, tumor & calculi and doppler USG for evaluation of aberrentvessles. Once obstructive nephropathy has been identified therapy focuses on the rapid restoration of normal urine flow either by medical or surgical intervention. Key words: Obstructive Uropathy, Posterior urethral valve, pyelonephritis, IVU, MCU Introduction: urinary tract obstruction impairs renal growth & Urinary tract obstruction refers to as restriction to the development.1 The approach to obstructive urinary outflow that if not managed satisfactorily, leads nephropathy should be to detect site of obstruction, to progressive renal damage. Obstructive uropathy is to find out whether obstruction is complete or partial, an important cause of end stage renal disease unilateral or bilateral, to findthe cause of obstruction requiring renal replacement therapy.1 The kidney is and to decide need forsurgery and to plan the medical an indispensable organ for maintaining homeostasis. treatment.4 The renal system plays diverse role including hormonogenesis, metabolism, detoxification & Etiology: excretion of urine which contains agents that may be Urinary tract obstruction can result from congenital injurious to the body. -

Hydronephrosis
Patient and Family Education Hydronephrosis What is Hydronephrosis? Hydronephrosis is a dilation of the kidney, specifically in the renal pelvis or the place in the kidney where urine is stored after its production. It occurs in 1-2% of all pregnancies. This extra fluid can be the result of some type of abnormality in or below the kidney or it may be a variant of normal. Hydronephrosis can be caused by many factors. Some of the most common reasons include obstruction or urinary reflux. Obstruction of the kidneys can occur at the level of the kidney (uretero-pelvic junction obstruction or UPJ) or at the level of the bladder (uretero-vesical junction or UVJ). It can also include a megaureter. Urinary reflux is the abnormal back flow of urine from the bladder back towards the kidneys. Obstruction: Reflux: How is hydronephrosis diagnosed? Hydronephrosis is usually diagnosed in one of two ways. 1. A prenatal ultrasound (ultrasound during pregnancy). This may reveal that the unborn baby has dilated or enlarged kidneys. This occurs in about 1 out of 100 pregnancies. 2. An ultrasound done after the baby is born. This sometimes is found after a routine evaluation for another medical problem or concern such as urinary tract infection or incontinence. Once hydronephrosis is noted, additional tests may be needed in order to find out why there is extra fluid in the kidneys. Early diagnosis and treatment of such an abnormality can prevent future urinary tract infections and permanent kidney damage or scarring. How is hydronephrosis graded and why it this important? Hydronephrosis is graded on a scale ranging from 1-4, with one being the mildest form and four being the most severe.