Congenital Abnormalities of the Fetal Face
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Otocephaly: Agnathia-Microstomia-Synotia Syndrome Tanya Kitova1, Borislav D Kitov2
CASE REPORT Otocephaly: Agnathia-Microstomia-Synotia Syndrome Tanya Kitova1, Borislav D Kitov2 ABSTRACT The aim of the study is to present otocephaly, which is a rare congenital lethal malformation. Until this moment, only a little bit more than 100 cases worldwide were reported, and only 22 cases of prediagnosed otocephaly. Background: Otocephaly or agnathia-microstomia-synotia syndrome (SAMS) is characterized by agenesis of mandible (agnathia), disposition or fusion of the auricle (synotia), microstomia, and complete or partial lack of language (aglossia), which often ends up lethal. Case description: A 499.7 g male fetus was obtained after a therapeutic abortion during the 23rd gestational week at the Center for Maternity and Neonatology, Embryo-fetopathology Clinic, Tunis, Tunisia. The mother is an 18-year-old with close relative marriage with first-degree incest, primigravida. Examination of the fetus revealed microcephaly with craniosynostosis, hypertelorism, closed eyelid exophthalmos, one nostril, point microstomia, mandibular agenesis, bilateral, and auditory cysts of neck. The ears are located at the level of the neck. A study of the brain and the base of the skull revealed holoprosencephaly and sphenoid bone agenesis. There are no internal organ abnormalities. Conclusion: In cases where, at the end of the second trimester of pregnancy, polyhydramnios is detected, inability to visualize the mandible, and malposition of ears, otocephaly should be suspected. In these cases, the decision to interrupt pregnancy should be taken by a multidisciplinary team, after an magnetic resonance imaging, which is much better in visualizing location of the ears and other facial malformations and the presence of other associated anomalies. -

Diseases of the Digestive System (KOO-K93)
CHAPTER XI Diseases of the digestive system (KOO-K93) Diseases of oral cavity, salivary glands and jaws (KOO-K14) lijell Diseases of pulp and periapical tissues 1m Dentofacial anomalies [including malocclusion] Excludes: hemifacial atrophy or hypertrophy (Q67.4) K07 .0 Major anomalies of jaw size Hyperplasia, hypoplasia: • mandibular • maxillary Macrognathism (mandibular)(maxillary) Micrognathism (mandibular)( maxillary) Excludes: acromegaly (E22.0) Robin's syndrome (087.07) K07 .1 Anomalies of jaw-cranial base relationship Asymmetry of jaw Prognathism (mandibular)( maxillary) Retrognathism (mandibular)(maxillary) K07.2 Anomalies of dental arch relationship Cross bite (anterior)(posterior) Dis to-occlusion Mesio-occlusion Midline deviation of dental arch Openbite (anterior )(posterior) Overbite (excessive): • deep • horizontal • vertical Overjet Posterior lingual occlusion of mandibular teeth 289 ICO-N A K07.3 Anomalies of tooth position Crowding Diastema Displacement of tooth or teeth Rotation Spacing, abnormal Transposition Impacted or embedded teeth with abnormal position of such teeth or adjacent teeth K07.4 Malocclusion, unspecified K07.5 Dentofacial functional abnormalities Abnormal jaw closure Malocclusion due to: • abnormal swallowing • mouth breathing • tongue, lip or finger habits K07.6 Temporomandibular joint disorders Costen's complex or syndrome Derangement of temporomandibular joint Snapping jaw Temporomandibular joint-pain-dysfunction syndrome Excludes: current temporomandibular joint: • dislocation (S03.0) • strain (S03.4) K07.8 Other dentofacial anomalies K07.9 Dentofacial anomaly, unspecified 1m Stomatitis and related lesions K12.0 Recurrent oral aphthae Aphthous stomatitis (major)(minor) Bednar's aphthae Periadenitis mucosa necrotica recurrens Recurrent aphthous ulcer Stomatitis herpetiformis 290 DISEASES OF THE DIGESTIVE SYSTEM Diseases of oesophagus, stomach and duodenum (K20-K31) Ill Oesophagitis Abscess of oesophagus Oesophagitis: • NOS • chemical • peptic Use additional external cause code (Chapter XX), if desired, to identify cause. -

WES Gene Package Multiple Congenital Anomalie.Xlsx
Whole Exome Sequencing Gene package Multiple congenital anomalie, version 5, 1‐2‐2018 Technical information DNA was enriched using Agilent SureSelect Clinical Research Exome V2 capture and paired‐end sequenced on the Illumina platform (outsourced). The aim is to obtain 8.1 Giga base pairs per exome with a mapped fraction of 0.99. The average coverage of the exome is ~50x. Duplicate reads are excluded. Data are demultiplexed with bcl2fastq Conversion Software from Illumina. Reads are mapped to the genome using the BWA‐MEM algorithm (reference: http://bio‐bwa.sourceforge.net/). Variant detection is performed by the Genome Analysis Toolkit HaplotypeCaller (reference: http://www.broadinstitute.org/gatk/). The detected variants are filtered and annotated with Cartagenia software and classified with Alamut Visual. It is not excluded that pathogenic mutations are being missed using this technology. At this moment, there is not enough information about the sensitivity of this technique with respect to the detection of deletions and duplications of more than 5 nucleotides and of somatic mosaic mutations (all types of sequence changes). HGNC approved Phenotype description including OMIM phenotype ID(s) OMIM median depth % covered % covered % covered gene symbol gene ID >10x >20x >30x A4GALT [Blood group, P1Pk system, P(2) phenotype], 111400 607922 101 100 100 99 [Blood group, P1Pk system, p phenotype], 111400 NOR polyagglutination syndrome, 111400 AAAS Achalasia‐addisonianism‐alacrimia syndrome, 231550 605378 73 100 100 100 AAGAB Keratoderma, palmoplantar, -

Blueprint Genetics Craniosynostosis Panel
Craniosynostosis Panel Test code: MA2901 Is a 38 gene panel that includes assessment of non-coding variants. Is ideal for patients with craniosynostosis. About Craniosynostosis Craniosynostosis is defined as the premature fusion of one or more cranial sutures leading to secondary distortion of skull shape. It may result from a primary defect of ossification (primary craniosynostosis) or, more commonly, from a failure of brain growth (secondary craniosynostosis). Premature closure of the sutures (fibrous joints) causes the pressure inside of the head to increase and the skull or facial bones to change from a normal, symmetrical appearance resulting in skull deformities with a variable presentation. Craniosynostosis may occur in an isolated setting or as part of a syndrome with a variety of inheritance patterns and reccurrence risks. Craniosynostosis occurs in 1/2,200 live births. Availability 4 weeks Gene Set Description Genes in the Craniosynostosis Panel and their clinical significance Gene Associated phenotypes Inheritance ClinVar HGMD ALPL Odontohypophosphatasia, Hypophosphatasia perinatal lethal, AD/AR 78 291 infantile, juvenile and adult forms ALX3 Frontonasal dysplasia type 1 AR 8 8 ALX4 Frontonasal dysplasia type 2, Parietal foramina AD/AR 15 24 BMP4 Microphthalmia, syndromic, Orofacial cleft AD 8 39 CDC45 Meier-Gorlin syndrome 7 AR 10 19 EDNRB Hirschsprung disease, ABCD syndrome, Waardenburg syndrome AD/AR 12 66 EFNB1 Craniofrontonasal dysplasia XL 28 116 ERF Craniosynostosis 4 AD 17 16 ESCO2 SC phocomelia syndrome, Roberts syndrome -

Evaluation of Fetal Orbits and Ears
Evaluation of Fetal Orbits and Ears Maria A. Calvo-Garcia, MD. Associate Professor of Radiology Cincinnati Children’s Hospital Medical Center Disclosure • I have no disclosures Goals & Objectives • Review basic US anatomic views for the evaluation of the orbits and ears • Describe some of the major malformations involving the orbits and ears Background on Facial Abnormalities • Important themselves • May also indicate an underlying problem – Chromosome abnormality/ Syndromic conditions Background on Facial Abnormalities • Assessment of the face is included in all standard fetal anatomic surveys • Recheck the face if you found other anomalies • And conversely, if you see facial anomalies look for other systemic defects Background on Facial Abnormalities • Fetal chromosomal analysis is often indicated • Fetal MRI frequently requested in search for additional malformations • US / Fetal MRI, as complementary techniques: information for planning delivery / neonatal treatment • Anatomic evaluation • Malformations (orbits, ears) Orbits Axial View • Bony orbits: IOD Orbits Axial View • Bony orbits: IOD and BOD, which correlates with GA, will allow detection of hypo-/ hypertelorism Orbits Axial View • Axial – Bony orbits – Intraorbital anatomy: • Globe • Lens Orbits Axial View • Axial – Bony orbits – Intraorbital anatomy: • Globe • Lens Orbits Axial View • Hyaloid artery is seen as an echogenic line bisecting the vitreous • By the 8th month the hyaloid system involutes – If this fails: persistent hyperplastic primary vitreous Malformations of -

Supratentorial Brain Malformations
Supratentorial Brain Malformations Edward Yang, MD PhD Department of Radiology Boston Children’s Hospital 1 May 2015/ SPR 2015 Disclosures: Consultant, Corticometrics LLC Objectives 1) Review major steps in the morphogenesis of the supratentorial brain. 2) Categorize patterns of malformation that result from failure in these steps. 3) Discuss particular imaging features that assist in recognition of these malformations. 4) Reference some of the genetic bases for these malformations to be discussed in greater detail later in the session. Overview I. Schematic overview of brain development II. Abnormalities of hemispheric cleavage III. Commissural (Callosal) abnormalities IV. Migrational abnormalities - Gray matter heterotopia - Pachygyria/Lissencephaly - Focal cortical dysplasia - Transpial migration - Polymicrogyria V. Global abnormalities in size (proliferation) VI. Fetal Life and Myelination Considerations I. Schematic Overview of Brain Development Embryology Top Mid-sagittal Top Mid-sagittal Closed Neural Tube (4 weeks) Corpus Callosum Callosum Formation Genu ! Splenium Cerebral Hemisphere (11-20 weeks) Hemispheric Cleavage (4-6 weeks) Neuronal Migration Ventricular/Subventricular Zones Ventricle ! Cortex (8-24 weeks) Neuronal Precursor Generation (Proliferation) (6-16 weeks) Embryology From ten Donkelaar Clinical Neuroembryology 2010 4mo 6mo 8mo term II. Abnormalities of Hemispheric Cleavage Holoprosencephaly (HPE) Top Mid-sagittal Imaging features: Incomplete hemispheric separation + 1)1) No septum pellucidum in any HPEs Closed Neural -

MR Imaging of Fetal Head and Neck Anomalies
Neuroimag Clin N Am 14 (2004) 273–291 MR imaging of fetal head and neck anomalies Caroline D. Robson, MB, ChBa,b,*, Carol E. Barnewolt, MDa,c aDepartment of Radiology, Children’s Hospital Boston, 300 Longwood Avenue, Harvard Medical School, Boston, MA 02115, USA bMagnetic Resonance Imaging, Advanced Fetal Care Center, Children’s Hospital Boston, Harvard Medical School, 300 Longwood Avenue, Boston, MA 02115, USA cFetal Imaging, Advanced Fetal Care Center, Children’s Hospital Boston, Harvard Medical School, 300 Longwood Avenue, Boston, MA 02115, USA Fetal dysmorphism can occur as a result of var- primarily used for fetal MR imaging. When the fetal ious processes that include malformation (anoma- face is imaged, the sagittal view permits assessment lous formation of tissue), deformation (unusual of the frontal and nasal bones, hard palate, tongue, forces on normal tissue), disruption (breakdown of and mandible. Abnormalities include abnormal promi- normal tissue), and dysplasia (abnormal organiza- nence of the frontal bone (frontal bossing) and lack of tion of tissue). the usual frontal prominence. Abnormal nasal mor- An approach to fetal diagnosis and counseling of phology includes variations in the size and shape of the parents incorporates a detailed assessment of fam- the nose. Macroglossia and micrognathia are also best ily history, maternal health, and serum screening, re- diagnosed on sagittal images. sults of amniotic fluid analysis for karyotype and Coronal images are useful for evaluating the in- other parameters, and thorough imaging of the fetus tegrity of the fetal lips and palate and provide as- with sonography and sometimes fetal MR imaging. sessment of the eyes, nose, and ears. -

Frontonasal Dysplasia
Frontonasal Dysplasia Frontonasal dysplasia is a developmental field defect of cran- f. Ocular anomalies iofacial region characterized by hypertelorism and varying i. Hypertelorism degrees of median nasal clefting. In 1967, DeMeyer first ii. Epicanthal folds described the malformation complex ‘median cleft face syn- iii. Narrowing of the palpebral fissures drome’ to emphasize the key midface defects. Since then several iv. Accessory nasal eyelid tissue with secondary terms have been introduced: frontonasal dysplasia, fron- displacement of inferior puncti colobomas tonasal syndrome, frontonasal dysostosis, and craniofrontonasal v. Epibulbar dermoids dysplasia. vi. Upper eyelid colobomas vii. Microphthalmia GENETICS/BASIC DEFECTS viii. Vitreoretinal degeneration with retinal detachment ix. Congenital cataracts 1. Inheritance g. Facial anomalies a. Sporadic in most cases i. Widow’s peak configuration of the anterior hair- b. Rare autosomal dominant inheritance with variable line in the forehead expression ii. Median cleft of upper lip c. Rare autosomal recessive inheritance iii. Median cleft palate d. Rare X-linked dominant inheritance iv. Preauricular tag 2. Rare association with chromosome anomalies v. Absent tragus a. Partial trisomy 2q and partial monosomy 7q from a vi. Low-set ears balanced maternal t(2;7)(q31;q36) h. Other anomalies b. 22q11 microdeletion i. Conductive deafness c. Reciprocal translocation t(15;22)(q22;q13) ii. Hypoplastic frontal sinuses d. Complex translocation involving chromosomes 3, 7, iii. Cardiac anomalies, especially teratology of and 11 Fallot 3. Rare variants of frontonasal dysplasia/malformation with iv. Limb anomalies variable inheritance patterns a) Clinodactyly 4. Embryologically classified as a developmental field b) Polydactyly defect c) Syndactyly 5. Extreme variable phenotypic expression d) Tibial hypoplasia v. -

Chromosome 13 Introduction Chromosome 13 (As Well As Chromosomes 14, 15, 21 and 22) Is an Acrocentric Chromosome. Short Arms Of
Chromosome 13 ©Chromosome Disorder Outreach Inc. (CDO) Technical genetic content provided by Dr. Iosif Lurie, M.D. Ph.D Medical Geneticist and CDO Medical Consultant/Advisor. Ideogram courtesy of the University of Washington Department of Pathology: ©1994 David Adler.hum_13.gif Introduction Chromosome 13 (as well as chromosomes 14, 15, 21 and 22) is an acrocentric chromosome. Short arms of acrocentric chromosomes do not contain any genes. All genes are located in the long arm. The length of the long arm is ~95 Mb. It is ~3.5% of the total human genome. Chromosome 13 is a gene poor area. There are only 600–700 genes within this chromosome. Structural abnormalities of the long arm of chromosome 13 are very common. There are at least 750 patients with deletions of different segments of the long arm (including patients with an associated imbalance for another chromosome). There are several syndromes associated with deletions of the long arm of chromosome 13. One of these syndromes is caused by deletions of 13q14 and neighboring areas. The main manifestation of this syndrome is retinoblastoma. Deletions of 13q32 and neighboring areas cause multiple defects of the brain, eye, heart, kidney, genitalia and extremities. The syndrome caused by this deletion is well known since the 1970’s. Distal deletions of 13q33q34 usually do not produce serious malformations. Deletions of the large area between 13q21 and 13q31 do not produce any stabile and well–recognized syndromes. Deletions of Chromosome 13 Chromosome 13 (as well as chromosomes 14, 15, 21 and 22) belongs to the group of acrocentric chromosomes. -
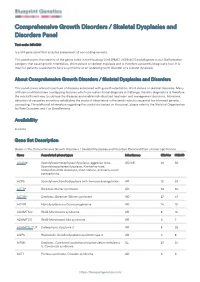
Blueprint Genetics Comprehensive Growth Disorders / Skeletal
Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders Panel Test code: MA4301 Is a 374 gene panel that includes assessment of non-coding variants. This panel covers the majority of the genes listed in the Nosology 2015 (PMID: 26394607) and all genes in our Malformation category that cause growth retardation, short stature or skeletal dysplasia and is therefore a powerful diagnostic tool. It is ideal for patients suspected to have a syndromic or an isolated growth disorder or a skeletal dysplasia. About Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders This panel covers a broad spectrum of diseases associated with growth retardation, short stature or skeletal dysplasia. Many of these conditions have overlapping features which can make clinical diagnosis a challenge. Genetic diagnostics is therefore the most efficient way to subtype the diseases and enable individualized treatment and management decisions. Moreover, detection of causative mutations establishes the mode of inheritance in the family which is essential for informed genetic counseling. For additional information regarding the conditions tested on this panel, please refer to the National Organization for Rare Disorders and / or GeneReviews. Availability 4 weeks Gene Set Description Genes in the Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders Panel and their clinical significance Gene Associated phenotypes Inheritance ClinVar HGMD ACAN# Spondyloepimetaphyseal dysplasia, aggrecan type, AD/AR 20 56 Spondyloepiphyseal dysplasia, Kimberley -

Blueprint Genetics Comprehensive Skeletal Dysplasias and Disorders
Comprehensive Skeletal Dysplasias and Disorders Panel Test code: MA3301 Is a 251 gene panel that includes assessment of non-coding variants. Is ideal for patients with a clinical suspicion of disorders involving the skeletal system. About Comprehensive Skeletal Dysplasias and Disorders This panel covers a broad spectrum of skeletal disorders including common and rare skeletal dysplasias (eg. achondroplasia, COL2A1 related dysplasias, diastrophic dysplasia, various types of spondylo-metaphyseal dysplasias), various ciliopathies with skeletal involvement (eg. short rib-polydactylies, asphyxiating thoracic dysplasia dysplasias and Ellis-van Creveld syndrome), various subtypes of osteogenesis imperfecta, campomelic dysplasia, slender bone dysplasias, dysplasias with multiple joint dislocations, chondrodysplasia punctata group of disorders, neonatal osteosclerotic dysplasias, osteopetrosis and related disorders, abnormal mineralization group of disorders (eg hypopohosphatasia), osteolysis group of disorders, disorders with disorganized development of skeletal components, overgrowth syndromes with skeletal involvement, craniosynostosis syndromes, dysostoses with predominant craniofacial involvement, dysostoses with predominant vertebral involvement, patellar dysostoses, brachydactylies, some disorders with limb hypoplasia-reduction defects, ectrodactyly with and without other manifestations, polydactyly-syndactyly-triphalangism group of disorders, and disorders with defects in joint formation and synostoses. Availability 4 weeks Gene Set Description -

Abstracts from the 51St European Society of Human Genetics Conference: Electronic Posters
European Journal of Human Genetics (2019) 27:870–1041 https://doi.org/10.1038/s41431-019-0408-3 MEETING ABSTRACTS Abstracts from the 51st European Society of Human Genetics Conference: Electronic Posters © European Society of Human Genetics 2019 June 16–19, 2018, Fiera Milano Congressi, Milan Italy Sponsorship: Publication of this supplement was sponsored by the European Society of Human Genetics. All content was reviewed and approved by the ESHG Scientific Programme Committee, which held full responsibility for the abstract selections. Disclosure Information: In order to help readers form their own judgments of potential bias in published abstracts, authors are asked to declare any competing financial interests. Contributions of up to EUR 10 000.- (Ten thousand Euros, or equivalent value in kind) per year per company are considered "Modest". Contributions above EUR 10 000.- per year are considered "Significant". 1234567890();,: 1234567890();,: E-P01 Reproductive Genetics/Prenatal Genetics then compared this data to de novo cases where research based PO studies were completed (N=57) in NY. E-P01.01 Results: MFSIQ (66.4) for familial deletions was Parent of origin in familial 22q11.2 deletions impacts full statistically lower (p = .01) than for de novo deletions scale intelligence quotient scores (N=399, MFSIQ=76.2). MFSIQ for children with mater- nally inherited deletions (63.7) was statistically lower D. E. McGinn1,2, M. Unolt3,4, T. B. Crowley1, B. S. Emanuel1,5, (p = .03) than for paternally inherited deletions (72.0). As E. H. Zackai1,5, E. Moss1, B. Morrow6, B. Nowakowska7,J. compared with the NY cohort where the MFSIQ for Vermeesch8, A.