Differential and Altered Spatial Distribution of Complement Expression in Age-Related Macular Degeneration
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Complement Factor B Antibody Cat
Complement Factor B Antibody Cat. No.: 16-846 Complement Factor B Antibody Immunohistochemistry of paraffin-embedded human mammary cancer using Immunohistochemistry of paraffin-embedded mouse lung using Complement Factor B Complement Factor B antibody (16-846) at dilution of 1:200 (40x lens). antibody (16-846) at dilution of 1:200 (40x lens). Immunofluorescence analysis of Raw264.7 cells using Complement Factor B Polyclonal Antibody (16-846) at dilution of 1:100 (40x lens). Blue: DAPI for nuclear staining. September 29, 2021 1 https://www.prosci-inc.com/complement-factor-b-antibody-16-846.html Specifications HOST SPECIES: Rabbit SPECIES REACTIVITY: Human, Mouse, Rat Recombinant fusion protein containing a sequence corresponding to amino acids 80-420 IMMUNOGEN: of human Complement Factor B (NP_001701.2). TESTED APPLICATIONS: IF, IHC, IP, WB WB: ,1:500 - 1:2000 IHC: ,1:50 - 1:200 APPLICATIONS: IF: ,1:50 - 1:200 IP: ,1:20 - 1:50 POSITIVE CONTROL: 1) HT-29 2) K-562 3) 293T 4) A-549 5) HepG2 6) Mouse liver PREDICTED MOLECULAR Observed: 86kDa WEIGHT: Properties PURIFICATION: Affinity purification CLONALITY: Polyclonal ISOTYPE: IgG CONJUGATE: Unconjugated PHYSICAL STATE: Liquid BUFFER: PBS with 0.02% sodium azide, 50% glycerol, pH7.3. STORAGE CONDITIONS: Store at -20˚C. Avoid freeze / thaw cycles. Additional Info OFFICIAL SYMBOL: CFB September 29, 2021 2 https://www.prosci-inc.com/complement-factor-b-antibody-16-846.html Complement factor B, C3/C5 convertase, Glycine-rich beta glycoprotein, GBG, PBF2, ALTERNATE NAMES: Properdin factor B, Complement factor B Ba fragment, Complement factor B Bb fragment, CFB, BF, BFD GENE ID: 629 USER NOTE: Optimal dilutions for each application to be determined by the researcher. -

S41467-020-18249-3.Pdf
ARTICLE https://doi.org/10.1038/s41467-020-18249-3 OPEN Pharmacologically reversible zonation-dependent endothelial cell transcriptomic changes with neurodegenerative disease associations in the aged brain Lei Zhao1,2,17, Zhongqi Li 1,2,17, Joaquim S. L. Vong2,3,17, Xinyi Chen1,2, Hei-Ming Lai1,2,4,5,6, Leo Y. C. Yan1,2, Junzhe Huang1,2, Samuel K. H. Sy1,2,7, Xiaoyu Tian 8, Yu Huang 8, Ho Yin Edwin Chan5,9, Hon-Cheong So6,8, ✉ ✉ Wai-Lung Ng 10, Yamei Tang11, Wei-Jye Lin12,13, Vincent C. T. Mok1,5,6,14,15 &HoKo 1,2,4,5,6,8,14,16 1234567890():,; The molecular signatures of cells in the brain have been revealed in unprecedented detail, yet the ageing-associated genome-wide expression changes that may contribute to neurovas- cular dysfunction in neurodegenerative diseases remain elusive. Here, we report zonation- dependent transcriptomic changes in aged mouse brain endothelial cells (ECs), which pro- minently implicate altered immune/cytokine signaling in ECs of all vascular segments, and functional changes impacting the blood–brain barrier (BBB) and glucose/energy metabolism especially in capillary ECs (capECs). An overrepresentation of Alzheimer disease (AD) GWAS genes is evident among the human orthologs of the differentially expressed genes of aged capECs, while comparative analysis revealed a subset of concordantly downregulated, functionally important genes in human AD brains. Treatment with exenatide, a glucagon-like peptide-1 receptor agonist, strongly reverses aged mouse brain EC transcriptomic changes and BBB leakage, with associated attenuation of microglial priming. We thus revealed tran- scriptomic alterations underlying brain EC ageing that are complex yet pharmacologically reversible. -

Wild-Type Bone Marrow Cells ) Mice with −/− in C1q-Deficient (C1qa
Reconstitution of the Complement Function in C1q-Deficient C1qa؊/؊) Mice with Wild-Type Bone Marrow Cells1) Franz Petry,2* Marina Botto,† Rafaela Holtappels,‡ Mark J. Walport,† and Michael Loos* Besides Ab-independent and Ab-dependent activation of the complement classical pathway in host defense, C1q plays a key role in the processing of immune complexes and in the clearance of apoptotic cells. In humans, C1q deficiency leads to systemic lupus erythematosus-like symptoms in over 90% of the cases, thus making this defect a strong disease susceptibility factor. Similarly, -C1q-deficient mice (C1qa؊/؊) develop systemic lupus erythematosus-like symptoms, such as autoantibodies and glomerulone phritis. We have previously provided evidence that C1q is produced by cells of the monocyte-macrophage lineage. In this study, .we have tested whether transplantation of bone marrow cells would be sufficient to reconstitute C1q levels in C1qa؊/؊ mice C1qa؊/؊ mice received a single graft of 107 bone marrow cells from wild-type (wt) donors after irradiation doses of 6, 7, 8, or 9 .Gy. Engraftment was monitored by a Y chromosome-specific PCR and a PCR that differentiated wt from C1qa؊/؊ genotype Serum levels of C1q Ag and C1 function increased rapidly in the recipient mice, and titers reached normal levels within 6 wk after bone marrow transplantation. In wt mice that received C1qa؊/؊ bone marrow, serum levels of C1q decreased constantly over time and became C1q deficient within 55 wk. These data clearly demonstrate that bone marrow-derived cells are the source of serum C1q and are competent to reconstitute normal C1q serum levels in C1q-deficient mice. -

Review Article Complement System and Age-Related Macular Degeneration: Implications of Gene-Environment Interaction for Preventive and Personalized Medicine
Hindawi BioMed Research International Volume 2018, Article ID 7532507, 13 pages https://doi.org/10.1155/2018/7532507 Review Article Complement System and Age-Related Macular Degeneration: Implications of Gene-Environment Interaction for Preventive and Personalized Medicine Andrea Maugeri ,1 Martina Barchitta ,1 Maria Grazia Mazzone,2 Francesco Giuliano,2 and Antonella Agodi 1 1 Department of Medical and Surgical Sciences and Advanced Technologies “GF Ingrassia”, University of Catania, Via S. Sofa 87, 95123 Catania, Italy 2SIFI SpA, Research and Development Department, Via Ercole Patti 36, 95025 Catania, Italy Correspondence should be addressed to Antonella Agodi; [email protected] Received 18 May 2018; Accepted 18 July 2018; Published 26 August 2018 Academic Editor: Sajib Chakraborty Copyright © 2018 Andrea Maugeri et al. Tis is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Age-related macular degeneration (AMD) is the most common cause of visual loss in developed countries, with a signifcant economic and social burden on public health. Although genome-wide and gene-candidate studies have been enabled to identify genetic variants in the complement system associated with AMD pathogenesis, the efect of gene-environment interaction is still under debate. In this review we provide an overview of the role of complement system and its genetic variants in AMD, summarizing the consequences of the interaction between genetic and environmental risk factors on AMD onset, progression, and therapeutic response. Finally, we discuss the perspectives of current evidence in the feld of genomics driven personalized medicine and public health. -

Supplementary Table S4. FGA Co-Expressed Gene List in LUAD
Supplementary Table S4. FGA co-expressed gene list in LUAD tumors Symbol R Locus Description FGG 0.919 4q28 fibrinogen gamma chain FGL1 0.635 8p22 fibrinogen-like 1 SLC7A2 0.536 8p22 solute carrier family 7 (cationic amino acid transporter, y+ system), member 2 DUSP4 0.521 8p12-p11 dual specificity phosphatase 4 HAL 0.51 12q22-q24.1histidine ammonia-lyase PDE4D 0.499 5q12 phosphodiesterase 4D, cAMP-specific FURIN 0.497 15q26.1 furin (paired basic amino acid cleaving enzyme) CPS1 0.49 2q35 carbamoyl-phosphate synthase 1, mitochondrial TESC 0.478 12q24.22 tescalcin INHA 0.465 2q35 inhibin, alpha S100P 0.461 4p16 S100 calcium binding protein P VPS37A 0.447 8p22 vacuolar protein sorting 37 homolog A (S. cerevisiae) SLC16A14 0.447 2q36.3 solute carrier family 16, member 14 PPARGC1A 0.443 4p15.1 peroxisome proliferator-activated receptor gamma, coactivator 1 alpha SIK1 0.435 21q22.3 salt-inducible kinase 1 IRS2 0.434 13q34 insulin receptor substrate 2 RND1 0.433 12q12 Rho family GTPase 1 HGD 0.433 3q13.33 homogentisate 1,2-dioxygenase PTP4A1 0.432 6q12 protein tyrosine phosphatase type IVA, member 1 C8orf4 0.428 8p11.2 chromosome 8 open reading frame 4 DDC 0.427 7p12.2 dopa decarboxylase (aromatic L-amino acid decarboxylase) TACC2 0.427 10q26 transforming, acidic coiled-coil containing protein 2 MUC13 0.422 3q21.2 mucin 13, cell surface associated C5 0.412 9q33-q34 complement component 5 NR4A2 0.412 2q22-q23 nuclear receptor subfamily 4, group A, member 2 EYS 0.411 6q12 eyes shut homolog (Drosophila) GPX2 0.406 14q24.1 glutathione peroxidase -

Adiponectin and Related C1q/TNF-Related Proteins Bind Selectively to Anionic Phospholipids and Sphingolipids
Adiponectin and related C1q/TNF-related proteins bind selectively to anionic phospholipids and sphingolipids Jessica J. Yea,b, Xin Bianc,d, Jaechul Lima,b, and Ruslan Medzhitova,b,1 aHHMI, Yale University, New Haven, CT 06520; bDepartment of Immunobiology, Yale University School of Medicine, New Haven, CT 06520; cDepartment of Cell Biology, Yale University School of Medicine, New Haven, CT 06520; and dDepartment of Neuroscience, Yale University School of Medicine, New Haven, CT 06520 Contributed by Ruslan Medzhitov, April 14, 2020 (sent for review December 20, 2019; reviewed by Ido Amit and G. William Wong) Adiponectin (Acrp30) is an adipokine associated with protection 5-mers of trimers, respectively referred to as low molecular weight from cardiovascular disease, insulin resistance, and inflammation. (LMW), medium molecular weight (MMW), and high molecular Although its effects are conventionally attributed to binding weight (HMW) complexes. Adiponectin can also be cleaved by Adipor1/2 and T-cadherin, its abundance in circulation, role in serum elastases and thrombin between the globular C1q-like head ceramide metabolism, and homology to C1q suggest an overlooked domain and the collagenous tail domain, forming globular adi- role as a lipid-binding protein, possibly generalizable to other C1q/ ponectin (gAd). While gAd appears to bind AdipoR1/2 and ac- TNF-related proteins (CTRPs) and C1q family members. To investi- tivate AMPK more strongly than full-length protein (19, 20), levels gate this, adiponectin, representative family members, and variants of HMW multimers are more strongly associated with insulin were expressed in Expi293 cells and tested for binding to lipids in sensitivity (21, 22), have a longer half-life in circulation (18), and liposomes using density centrifugation. -
Supplementary Figures and Tables
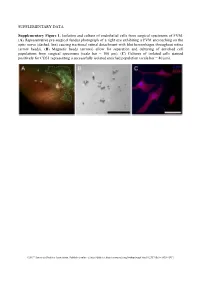
SUPPLEMENTARY DATA Supplementary Figure 1. Isolation and culture of endothelial cells from surgical specimens of FVM. (A) Representative pre-surgical fundus photograph of a right eye exhibiting a FVM encroaching on the optic nerve (dashed line) causing tractional retinal detachment with blot hemorrhages throughout retina (arrow heads). (B) Magnetic beads (arrows) allow for separation and culturing of enriched cell populations from surgical specimens (scale bar = 100 μm). (C) Cultures of isolated cells stained positively for CD31 representing a successfully isolated enriched population (scale bar = 40 μm). ©2017 American Diabetes Association. Published online at http://diabetes.diabetesjournals.org/lookup/suppl/doi:10.2337/db16-1035/-/DC1 SUPPLEMENTARY DATA Supplementary Figure 2. Efficient siRNA knockdown of RUNX1 expression and function demonstrated by qRT-PCR, Western Blot, and scratch assay. (A) RUNX1 siRNA induced a 60% reduction of RUNX1 expression measured by qRT-PCR 48 hrs post-transfection whereas expression of RUNX2 and RUNX3, the two other mammalian RUNX orthologues, showed no significant changes, indicating specificity of our siRNA. Functional inhibition of Runx1 signaling was demonstrated by a 330% increase in insulin-like growth factor binding protein-3 (IGFBP3) RNA expression level, a known target of RUNX1 inhibition. Western blot demonstrated similar reduction in protein levels. (B) siRNA- 2’s effect on RUNX1 was validated by qRT-PCR and western blot, demonstrating a similar reduction in both RNA and protein. Scratch assay demonstrates functional inhibition of RUNX1 by siRNA-2. ns: not significant, * p < 0.05, *** p < 0.001 ©2017 American Diabetes Association. Published online at http://diabetes.diabetesjournals.org/lookup/suppl/doi:10.2337/db16-1035/-/DC1 SUPPLEMENTARY DATA Supplementary Table 1. -

Steffensen Et Al. Supplement 2A
Liver Wild-type Knockout 1 2 4 1 2 4 1 1 1 C C C C C C W W W K K K IMAGE:640919 expressed sequence AA960558 IMAGE:523974 RIKEN cDNA 1810004N01 gene IMAGE:1211217 eukaryotic translation initiation factor 4E binding protein 2 IMAGE:314741 beta-site APP cleaving enzyme IMAGE:1038420 silica-induced gene 41 IMAGE:1229655 soc-2 suppressor of clear homolog C. elegans IMAGE:1150065 Unknown IMAGE:1038486 RIKEN cDNA 2700038M07 gene IMAGE:524351 amyloid beta A4 precursor protein IMAGE:819912 thymus expressed acidic protein IMAGE:779426 RIKEN cDNA 5230400G24 gene IMAGE:945643 ESTs IMAGE:850544 Mpv17 transgene, kidney disease mutant IMAGE:537568 expressed sequence AA675315 IMAGE:1107584 yes-associated protein, 65 kDa IMAGE:961363 expressed sequence AU015422 IMAGE:775218 expressed sequence AI265322 IMAGE:792656 protein phosphatase 1B, magnesium dependent, beta isoform IMAGE:1038592 ESTs, Weakly similar to A43932 mucin 2 precursor, intestinal [H.sapiens] IMAGE:1224917 huntingtin interacting protein 2 IMAGE:751186 ESTs IMAGE:865151 Trk-fused gene IMAGE:523016 SWI/SNF related, matrix associated, actin dependent regulator of chromatin, subfamily a, member 5 IMAGE:765039 FBJ osteosarcoma oncogene B IMAGE:1003995 expressed sequence AI844632 IMAGE:903863 RIKEN cDNA 1300006L01 gene IMAGE:934094 ESTs IMAGE:988962 expressed sequence C77245 IMAGE:1023308 ESTs, Weakly similar to S71512 hypothetical protein T2 - mouse [M.musculus] IMAGE:865317 eukaryotic translation initiation factor 3 IMAGE:720445 ribosomal protein S6 IMAGE:1005417 expressed sequence AU024550 -

Complement Component 2 Deficiency
Complement component 2 deficiency Description Complement component 2 deficiency is a disorder that causes the immune system to malfunction, resulting in a form of immunodeficiency. Immunodeficiencies are conditions in which the immune system is not able to protect the body effectively from foreign invaders such as bacteria and viruses. People with complement component 2 deficiency have a significantly increased risk of recurrent bacterial infections, specifically of the lungs (pneumonia), the membrane covering the brain and spinal cord (meningitis), and the blood (sepsis), which may be life-threatening. These infections most commonly occur in infancy and childhood and become less frequent in adolescence and adulthood. Complement component 2 deficiency is also associated with an increased risk of developing autoimmune disorders such as systemic lupus erythematosus (SLE) or vasculitis. Autoimmune disorders occur when the immune system malfunctions and attacks the body's tissues and organs. Between 10 and 20 percent of individuals with complement component 2 deficiency develop SLE. Females with complement component 2 deficiency are more likely to have SLE than affected males, but this is also true of SLE in the general population. The severity of complement component 2 deficiency varies widely. While some affected individuals experience recurrent infections and other immune system difficulties, others do not have any health problems related to the disorder. Frequency In Western countries, complement component 2 deficiency is estimated to affect 1 in 20, 000 individuals; its prevalence in other areas of the world is unknown. Causes Complement component 2 deficiency is caused by mutations in the C2 gene. This gene provides instructions for making the complement component 2 protein, which helps regulate a part of the body's immune response known as the complement system. -

In Kidney Injury
antioxidants Review Regulation of Complement Activation by Heme Oxygenase-1 (HO-1) in Kidney Injury Maria G. Detsika 1,* and Elias A. Lianos 2,3 1 First Department of Critical Care Medicine & Pulmonary Services, GP Livanos and M. Simou Laboratories, National & Kapodistrian University of Athens, Medical School, Evangelismos Hospital, 10675 Athens, Greece 2 Thorax Foundation, Research Center of Intensive Care and Emergency Thoracic Medicine, 10675 Athens, Greece; [email protected] 3 Veterans Affairs Medical Center and Virginia Tech, Carilion School of Medicine, 1970 Roanoke Blvd, Salem, VA 24153, USA * Correspondence: [email protected]; Tel.: +30-210-723552; Fax: +30-210-7239127 Abstract: Heme oxygenase is a cytoprotective enzyme with strong antioxidant and anti-apoptotic properties. Its cytoprotective role is mainly attributed to its enzymatic activity, which involves the degradation of heme to biliverdin with simultaneous release of carbon monoxide (CO). Recent studies uncovered a new cytoprotective role for heme oxygenase-1 (HO-1) by identifying a regulatory role on the complement control protein decay-accelerating factor. This is a key complement regulatory protein preventing dysregulation or overactivation of complement cascades that can cause kidney injury. Cell-specific targeting of HO-1 induction may, therefore, be a novel approach to attenuate complement-dependent forms of kidney disease. Keywords: heme; heme oxygenase-1 (HO-1); complement; kidney injury 1. Introduction Citation: Detsika, M.G.; Lianos, E.A. Although the role of heme, in various cellular processes, such as gene transcription Regulation of Complement and translation and cellular differentiation, proliferation, and apoptosis, has been known Activation by Heme Oxygenase-1 for decades, the role of the heme-degrading enzyme heme oxygenase-1 (HO-1) only gained (HO-1) in Kidney Injury. -

Human Induced Pluripotent Stem Cell–Derived Podocytes Mature Into Vascularized Glomeruli Upon Experimental Transplantation
BASIC RESEARCH www.jasn.org Human Induced Pluripotent Stem Cell–Derived Podocytes Mature into Vascularized Glomeruli upon Experimental Transplantation † Sazia Sharmin,* Atsuhiro Taguchi,* Yusuke Kaku,* Yasuhiro Yoshimura,* Tomoko Ohmori,* ‡ † ‡ Tetsushi Sakuma, Masashi Mukoyama, Takashi Yamamoto, Hidetake Kurihara,§ and | Ryuichi Nishinakamura* *Department of Kidney Development, Institute of Molecular Embryology and Genetics, and †Department of Nephrology, Faculty of Life Sciences, Kumamoto University, Kumamoto, Japan; ‡Department of Mathematical and Life Sciences, Graduate School of Science, Hiroshima University, Hiroshima, Japan; §Division of Anatomy, Juntendo University School of Medicine, Tokyo, Japan; and |Japan Science and Technology Agency, CREST, Kumamoto, Japan ABSTRACT Glomerular podocytes express proteins, such as nephrin, that constitute the slit diaphragm, thereby contributing to the filtration process in the kidney. Glomerular development has been analyzed mainly in mice, whereas analysis of human kidney development has been minimal because of limited access to embryonic kidneys. We previously reported the induction of three-dimensional primordial glomeruli from human induced pluripotent stem (iPS) cells. Here, using transcription activator–like effector nuclease-mediated homologous recombination, we generated human iPS cell lines that express green fluorescent protein (GFP) in the NPHS1 locus, which encodes nephrin, and we show that GFP expression facilitated accurate visualization of nephrin-positive podocyte formation in -

Comprehensive Genetic Analysis of Complement and Coagulation Genes in Atypical Hemolytic Uremic Syndrome
BASIC RESEARCH www.jasn.org Comprehensive Genetic Analysis of Complement and Coagulation Genes in Atypical Hemolytic Uremic Syndrome † † † ‡ † Fengxiao Bu,* Tara Maga,* Nicole C. Meyer, Kai Wang, Christie P. Thomas, § † † Carla M. Nester, § and Richard J. H. Smith* § *Interdisciplinary PhD Program in Genetics, †Molecular Otolaryngology and Renal Research Laboratories, ‡Department of Biostatistics, College of Public Health, and §Rare Renal Disease Clinic, Departments of Pediatrics and Internal Medicine, Carver College of Medicine, University of Iowa, Iowa City, Iowa ABSTRACT Atypical hemolytic uremic syndrome (aHUS) is a thrombotic microangiopathy caused by uncontrolled activation of the alternative pathway of complement at the cell surface level that leads to microangiopathic hemolytic anemia, thrombocytopenia, and acute kidney failure. In approximately one half of affected patients, pathogenic loss-of-function variants in regulators of complement or gain-of-function variants in effectors of complement are identified, clearly implicating complement in aHUS. However, there are strong lines of evidence supporting the presence of additional genetic contributions to this disease. To identify novel aHUS-associated genes, we completed a comprehensive screen of the complement and coagulation pathways in 36 patients with sporadic aHUS using targeted genomic enrichment and mas- sively parallel sequencing. After variant calling, quality control, and hard filtering, we identified 84 reported or novel nonsynonymous variants, 22 of which have been previously associated with disease. Using computational prediction methods, 20 of the remaining 62 variants were predicted to be dele- terious. Consistent with published data, nearly one half of these 42 variants (19; 45%) were found in genes implicated in the pathogenesis of aHUS. Several genes in the coagulation pathway were also identified as important in the pathogenesis of aHUS.