Empiric Antibiotic Guidelines
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Ceftazidime for Injection) PHARMACY BULK PACKAGE – NOT for DIRECT INFUSION
PRESCRIBING INFORMATION FORTAZ® (ceftazidime for injection) PHARMACY BULK PACKAGE – NOT FOR DIRECT INFUSION To reduce the development of drug-resistant bacteria and maintain the effectiveness of FORTAZ and other antibacterial drugs, FORTAZ should be used only to treat or prevent infections that are proven or strongly suspected to be caused by bacteria. DESCRIPTION Ceftazidime is a semisynthetic, broad-spectrum, beta-lactam antibacterial drug for parenteral administration. It is the pentahydrate of pyridinium, 1-[[7-[[(2-amino-4 thiazolyl)[(1-carboxy-1-methylethoxy)imino]acetyl]amino]-2-carboxy-8-oxo-5-thia-1 azabicyclo[4.2.0]oct-2-en-3-yl]methyl]-, hydroxide, inner salt, [6R-[6α,7β(Z)]]. It has the following structure: The molecular formula is C22H32N6O12S2, representing a molecular weight of 636.6. FORTAZ is a sterile, dry-powdered mixture of ceftazidime pentahydrate and sodium carbonate. The sodium carbonate at a concentration of 118 mg/g of ceftazidime activity has been admixed to facilitate dissolution. The total sodium content of the mixture is approximately 54 mg (2.3 mEq)/g of ceftazidime activity. The Pharmacy Bulk Package vial contains 709 mg of sodium carbonate. The sodium content is approximately 54 mg (2.3mEq) per gram of ceftazidime. FORTAZ in sterile crystalline form is supplied in Pharmacy Bulk Packages equivalent to 6g of anhydrous ceftazidime. The Pharmacy Bulk Package bottle is a container of sterile preparation for parenteral use that contains many single doses. The contents are intended for use in a pharmacy admixture program and are restricted to the preparation of admixtures for intravenous use. THE PHARMACY BULK PACKAGE IS NOT FOR DIRECT INFUSION, FURTHER DILUTION IS REQUIRED BEFORE USE. -

Severe Sepsis and Septic Shock Antibiotic Guide
Stanford Health Issue Date: 05/2017 Stanford Antimicrobial Safety and Sustainability Program Severe Sepsis and Septic Shock Antibiotic Guide Table 1: Antibiotic selection options for healthcare associated and/or immunocompromised patients • Healthcare associated: intravenous therapy, wound care, or intravenous chemotherapy within the prior 30 days, residence in a nursing home or other long-term care facility, hospitalization in an acute care hospital for two or more days within the prior 90 days, attendance at a hospital or hemodialysis clinic within the prior 30 days • Immunocompromised: Receiving chemotherapy, known systemic cancer not in remission, ANC <500, severe cell-mediated immune deficiency Table 2: Antibiotic selection options for community acquired, immunocompetent patients Table 3: Antibiotic selection options for patients with simple sepsis, community acquired, immunocompetent patients requiring hospitalization. Risk Factors for Select Organisms P. aeruginosa MRSA Invasive Candidiasis VRE (and other resistant GNR) Community acquired: • Known colonization with MDROs • Central venous catheter • Liver transplant • Prior IV antibiotics within 90 day • Recent MRSA infection • Broad-spectrum antibiotics • Known colonization • Known colonization with MDROs • Known MRSA colonization • + 1 of the following risk factors: • Prolonged broad antibacterial • Skin & Skin Structure and/or IV access site: ♦ Parenteral nutrition therapy Hospital acquired: ♦ Purulence ♦ Dialysis • Prolonged profound • Prior IV antibiotics within 90 days ♦ Abscess -

Antimicrobial Stewardship Guidance
Antimicrobial Stewardship Guidance Federal Bureau of Prisons Clinical Practice Guidelines March 2013 Clinical guidelines are made available to the public for informational purposes only. The Federal Bureau of Prisons (BOP) does not warrant these guidelines for any other purpose, and assumes no responsibility for any injury or damage resulting from the reliance thereof. Proper medical practice necessitates that all cases are evaluated on an individual basis and that treatment decisions are patient-specific. Consult the BOP Clinical Practice Guidelines Web page to determine the date of the most recent update to this document: http://www.bop.gov/news/medresources.jsp Federal Bureau of Prisons Antimicrobial Stewardship Guidance Clinical Practice Guidelines March 2013 Table of Contents 1. Purpose ............................................................................................................................................. 3 2. Introduction ...................................................................................................................................... 3 3. Antimicrobial Stewardship in the BOP............................................................................................ 4 4. General Guidance for Diagnosis and Identifying Infection ............................................................. 5 Diagnosis of Specific Infections ........................................................................................................ 6 Upper Respiratory Infections (not otherwise specified) .............................................................................. -
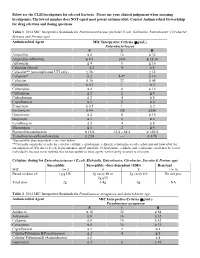
Below Are the CLSI Breakpoints for Selected Bacteria. Please Use Your Clinical Judgement When Assessing Breakpoints
Below are the CLSI breakpoints for selected bacteria. Please use your clinical judgement when assessing breakpoints. The lowest number does NOT equal most potent antimicrobial. Contact Antimicrobial Stewardship for drug selection and dosing questions. Table 1: 2014 MIC Interpretive Standards for Enterobacteriaceae (includes E.coli, Klebsiella, Enterobacter, Citrobacter, Serratia and Proteus spp) Antimicrobial Agent MIC Interpretive Criteria (g/mL) Enterobacteriaceae S I R Ampicillin ≤ 8 16 ≥ 32 Ampicillin-sulbactam ≤ 8/4 16/8 ≥ 32/16 Aztreonam ≤ 4 8 ≥ 16 Cefazolin (blood) ≤ 2 4 ≥ 8 Cefazolin** (uncomplicated UTI only) ≤ 16 ≥ 32 Cefepime* ≤ 2 4-8* ≥ 16 Cefotetan ≤ 16 32 ≥ 64 Ceftaroline ≤ 0.5 1 ≥ 2 Ceftazidime ≤ 4 8 ≥ 16 Ceftriaxone ≤ 1 2 ≥ 4 Cefpodoxime ≤ 2 4 ≥ 8 Ciprofloxacin ≤ 1 2 ≥ 4 Ertapenem ≤ 0.5 1 ≥ 2 Fosfomycin ≤ 64 128 ≥256 Gentamicin ≤ 4 8 ≥ 16 Imipenem ≤ 1 2 ≥ 4 Levofloxacin ≤ 2 4 ≥ 8 Meropenem ≤ 1 2 ≥ 4 Piperacillin-tazobactam ≤ 16/4 32/4 – 64/4 ≥ 128/4 Trimethoprim-sulfamethoxazole ≤ 2/38 --- ≥ 4/76 *Susceptibile dose-dependent – see chart below **Cefazolin can predict results for cefaclor, cefdinir, cefpodoxime, cefprozil, cefuroxime axetil, cephalexin and loracarbef for uncomplicated UTIs due to E.coli, K.pneumoniae, and P.mirabilis. Cefpodoxime, cefinidir, and cefuroxime axetil may be tested individually because some isolated may be susceptible to these agents while testing resistant to cefazolin. Cefepime dosing for Enterobacteriaceae ( E.coli, Klebsiella, Enterobacter, Citrobacter, Serratia & Proteus spp) Susceptible Susceptible –dose-dependent (SDD) Resistant MIC </= 2 4 8 >/= 16 Based on dose of: 1g q12h 1g every 8h or 2g every 8 h Do not give 2g q12 Total dose 2g 3-4g 6g NA Table 2: 2014 MIC Interpretive Standards for Pseudomonas aeruginosa and Acinetobacter spp. -

Which Antibiotic Prophylaxis Guidelines for Infective Endocarditis Should Canadian Dentists Follow?
Debate & O P I N I O N Which Antibiotic Prophylaxis Guidelines for Infective Endocarditis Should Canadian Dentists Follow? Contact Author Herve Y. Sroussi, DMD, PhD; Ashwin R. Prabhu, BDS; Dr. Epstein Joel B. Epstein, DMD, MSD, FRCD(C) Email: [email protected] For citation purposes, the electronic version is the definitive version of this article: www.cda-adc.ca/jcda/vol-73/issue-5/401.html ental providers must keep up to date 2 weeks following a procedure, dental proced- with antibiotic prophylaxis guidelines ures conducted even months earlier may be Dfor infectious endocarditis (IE) as these questioned as causative of IE.4 Furthermore, guidelines represent standards of care and periodontal and dental disease increase the determine medicolegal standards. A survey risk of bacteremia with activities of daily of Canadian dentists revealed that practi- living and may more commonly cause bac- tioners tend to employ antibiotic prophylaxis teremia; therefore, good oral care is of para- according to the guidelines in place at the mount importance in patients with conditions time of their graduation from dental school that place them at risk for IE. — guidelines that often do not meet the cur- To reduce the risk of IE following dental rent standards,1 as both the American Heart procedures, prophylactic measures have Association (AHA)2 and the British Society been developed by experts in the fields of for Antimicrobial Chemotherapy (BSAC)3 have microbiology, epidemiology, cardiology and currently updated their recommendations. dentistry. The principle preventive measure Host factors that increase the risk of IE recommended is the use of prophylactic anti- include specific cardiac abnormalities, a biotics before certain dental procedures in pa- previous episode of IE and the extent of the tients identified as at risk. -

Synermox 500 Mg/125 Mg Tablets
New Zealand Data Sheet 1. PRODUCT NAME Synermox 500 mg/125 mg Tablets 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Synermox 500 mg/125 mg Tablets: Each film‐coated tablet contains amoxicillin trihydrate equivalent to 500 mg amoxicillin, with potassium clavulanate equivalent to 125 mg clavulanic acid. Excipient(s) with known effect For the full list of excipients, see section 6.1. 3. PHARMACEUTICAL FORM Synermox 500 mg/125 mg Tablets: White to off‐white, oval shaped film‐coated tablets, debossed with “RX713” on one side and plain on the other. 4. CLINICAL PARTICULARS 4.1. Therapeutic indications Synermox is indicated in adults and children (see sections 4.2, 4.4 and 5.1) for short term treatment of common bacterial infections such as: Upper Respiratory Tract Infections (including ENT) e.g. Tonsillitis, sinusitis, otitis media. Lower Respiratory Tract Infection e.g. acute exacerbations of chronic bronchitis, lobar and broncho‐pneumonia. Genito‐urinary Tract Infections e.g. Cystitis, urethritis, pyelonephritis, female genital infections. Skin and Soft Tissue Infections. Bone and Joint Infections e.g. Osteomyelitis. Other Infections e.g. septic abortion, puerperal sepsis, intra‐abdominal sepsis, septicaemia, peritonitis, post‐surgical infections. Synermox is indicated for prophylaxis against infection which may be associated with major surgical procedures such as those involving: Gastro‐intestinal tract Pelvic cavity 1 | Page Head and neck Cardiac Renal Joint replacement Biliary tract surgery Infections caused by amoxicillin susceptible organisms are amenable to Synermox treatment due to its amoxicillin content. Mixed infections caused by amoxicillin susceptible organisms in conjunction with Synermox‐susceptible beta‐lactamase‐producing organisms may therefore be treated by Synermox. -

Penicillin Allergy Guidance Document
Penicillin Allergy Guidance Document Key Points Background Careful evaluation of antibiotic allergy and prior tolerance history is essential to providing optimal treatment The true incidence of penicillin hypersensitivity amongst patients in the United States is less than 1% Alterations in antibiotic prescribing due to reported penicillin allergy has been shown to result in higher costs, increased risk of antibiotic resistance, and worse patient outcomes Cross-reactivity between truly penicillin allergic patients and later generation cephalosporins and/or carbapenems is rare Evaluation of Penicillin Allergy Obtain a detailed history of allergic reaction Classify the type and severity of the reaction paying particular attention to any IgE-mediated reactions (e.g., anaphylaxis, hives, angioedema, etc.) (Table 1) Evaluate prior tolerance of beta-lactam antibiotics utilizing patient interview or the electronic medical record Recommendations for Challenging Penicillin Allergic Patients See Figure 1 Follow-Up Document tolerance or intolerance in the patient’s allergy history Consider referring to allergy clinic for skin testing Created July 2017 by Macey Wolfe, PharmD; John Schoen, PharmD, BCPS; Scott Bergman, PharmD, BCPS; Sara May, MD; and Trevor Van Schooneveld, MD, FACP Disclaimer: This resource is intended for non-commercial educational and quality improvement purposes. Outside entities may utilize for these purposes, but must acknowledge the source. The guidance is intended to assist practitioners in managing a clinical situation but is not mandatory. The interprofessional group of authors have made considerable efforts to ensure the information upon which they are based is accurate and up to date. Any treatments have some inherent risk. Recommendations are meant to improve quality of patient care yet should not replace clinical judgment. -

Piperacillin/Tazobactam Drug Class1 Antibiotic – Penicillin with Β-Lactamase Inhibitor
Monographs for Commonly Administered Intravenous Medications in Home and Community Care Piperacillin/Tazobactam Drug Class1 Antibiotic – penicillin with β-lactamase inhibitor Spectrum1 Refer to product monograph for complete spectrum For β-lactamase producing bacteria strains (e.g., Haemophilus influenza, Escherichia coli, and Staphylococcus aureus). Also to susceptible Acinetobacter species, Klebsiella pneumonia, Pseudomonas aeruginosa often combined with aminoglycoside). Cross Sensitivities / Allergies1 Cross sensitivities with penicillin and possibly cephalosporin and/or beta-lactam inhibitors Indications1,2 Intra-abdominal Respiratory tract Skin and skin structure Septicemia Gynecological Urinary tract Other conditions based on culture and sensitivity results Outpatient Considerations1 For patients with a documented allergy to penicillin, cephalosporin or beta-lactam inhibitor, the first dose should be administered in a hospital or clinic setting. Must be able to access laboratory monitoring (either at outpatient laboratory or by arranging in-home lab) if using an interacting oral medication (see Potential Drug Interactions section) Prescribing Considerations At time of ordering please provide the following to the pharmacist: and Dosage in Adults1,2 Height, weight Most recent serum creatinine with date obtained Indication (infection being treated) Usually dosed every 6 to 8 hours. Available as 2 g/0.25 g, 3 g/0.375 g, 4 g/0.5 g piperacillin/tazobactam (dose selected based on indication) Maximum 18 g/ 2.25 g piperacillin/tazobactam daily Dose and administration interval require adjustment for renal impairment Errors have occurred due to unusual ordering as combined dose of piperacillin and tazobactam. Order may be expressed only as piperacillin component or as a total of piperacillin + tazobactam (8:1 ratio). -

Antibiotic Prophylaxis for Surgical Procedures
Summary and Conclusions Antibiotic Prophylaxis for Surgical Procedures A Systematic Review Swedish Council on Health Technology Assessment SBU Board of Directors and Scientific Advisory Committee Secretariat MÅNS ROSÉN Executive Director, SBU Board of Directors NINA REHNQVIST BJÖRN KLINGE MARGARETA TROEIN Karolinska Institute, Solna Karolinska Institute, TÖLLBORN (Chair) Solna The Swedish Society of Medicine EVA NILSSON BÅGENHOLM MÅNS ROSÉN The Swedish Medical SBU MATS ULFENDAHL Association The Swedish Research KARIN STRANDBERG NÖJD Council HÅKAN CEDER The Swedish Association The National Board of Local Authorities and SABINA WIKGREN ORSTAM of Health and Welfare Regions The Swedish Association ANNA-KARIN EKLUND HÅKAN SÖRMAN of Local Authorities and Swedish Association The Swedish Association Regions of Health Professionals of Local Authorities and Regions Scientific Advisory Committee DAVID BERGQVIST MATS G HANSSON ULF NÄSLUND Uppsala University Uppsala University Norrland University Hospital (Chair) Hospital, Umeå MIKAEL HELLSTRÖM BJÖRN BEERMANN Sahlgrenska Hospital, JOAKIM RAMSBERG Medical Products Agency, Gothenburg i3 Innovus, Stockholm Uppsala MARGARETA MÖLLER BO RUNESON CHRISTINA BERGH University Hospital, Karolinska Institute, Sahlgrenska Hospital, Örebro Solna Gothenburg JÖRGEN NORDENSTRÖM GUNNEL SVENSÄTER CECILIA BJÖRKELUND Karolinska University Malmö University Gothenburg University Hospital, Solna ANIA WILLMAN 2 SBU'S SUMMARY AND CONCLUSIONS SÖLVE ELMSTÅHL OLOF NYRÉN Blekinge Institute of University Hospital, Karolinska Institute, -

Safety and Efficacy of Ceftaroline Fosamil in the Management of Community-Acquired Bacterial Pneumonia Heather F
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Scholarly Papers 2014 Safety and Efficacy of Ceftaroline Fosamil in the Management of Community-Acquired Bacterial Pneumonia Heather F. DeBellis Kimberly L. Barefield Philadelphia College of Osteopathic Medicine, [email protected] Follow this and additional works at: https://digitalcommons.pcom.edu/scholarly_papers Part of the Medicine and Health Sciences Commons Recommended Citation DeBellis, Heather F. and Barefield, Kimberly L., "Safety and Efficacy of Ceftaroline Fosamil in the Management of Community- Acquired Bacterial Pneumonia" (2014). PCOM Scholarly Papers. 1913. https://digitalcommons.pcom.edu/scholarly_papers/1913 This Article is brought to you for free and open access by DigitalCommons@PCOM. It has been accepted for inclusion in PCOM Scholarly Papers by an authorized administrator of DigitalCommons@PCOM. For more information, please contact [email protected]. Open Access: Full open access to Clinical Medicine Reviews this and thousands of other papers at http://www.la-press.com. in Therapeutics Safety and Efficacy of Ceftaroline Fosamil in the Management of Community- Acquired Bacterial Pneumonia Heather F. DeBellis and Kimberly L. Tackett South University School of Pharmacy, Savannah, GA, USA. ABSTR ACT: Ceftaroline fosamil is a new fifth-generation cephalosporin indicated for the treatment of community-acquired bacterial pneumonia (CABP). It possesses antimicrobial effects against both Gram-positive and Gram-negative bacteria, including methicillin-resistant Staphylococcus aureus (MRSA), but not against anaerobes. Organisms covered by this novel agent that are commonly associated with CABP are Streptococcus pneumoniae, Staphylococcus aureus, Haemophilus influenzae, Moraxella catarrhalis, and Klebsiella pneumoniae; however, ceftaroline fosamil lacks antimicrobial activity against Pseudomonas and Acinetobacter species. -

Guideline on Antibiotic Prophylaxis for Dental Patients at Risk for Infection
american academy of pediatric dentistry Guideline on Antibiotic Prophylaxis for Dental Patients at Risk for Infection Originating Committee clinical affairs committee Review Council council on clinical affairs Adopted 1990 Revised 1991, 1997, 1999, 2002, 2005, 2007, 2008 Purpose may be at increased risk. If a patient reports a syndrome or The American Academy of Pediatric Dentistry (AAPD) recog- medical condition with which the practitioner is not familiar, nizes that numerous medical conditions predispose patients it is appropriate to contact the child’s physician to determine to bacteremia-induced infections. Because it is not possible to susceptibility to bacteremia-induced infections. predict when a susceptible patient will develop an infection, In 2007, the American Heart Association (AHA) released its prophylactic antibiotics are recommended when these patients newly revised guidelines for the prevention of IE and reducing undergo procedures most likely to produce bacteremia. This the risk for producing resistant strains of bacteria.3 The 2007 guideline is intended to help practitioners make appropriate revision was based on relevant literature and studies, in con- decisions regarding antibiotic prophylaxis for dental patients sultation with national and international experts. The AAPD, at risk. acknowledging the AHA’s expertise and efforts to produce evidenced-based recommendations, continues to endorse the Methods AHA guideline for antibiotic prophylaxis, now entitled “Pre- This guideline is based on a review of current dental and medical vention of Infective Endocarditis”. literature pertaining to postprocedural bacteremia-induced The primary reasons for the revision include: infections. A MEDLINE search was performed using the key- • “IE is much more likely to result from frequent exposure words “infective endocarditis” (IE), “bacteremia”, “antibiotic to random bacteremias associated with daily activities than prophylaxis”, and “dental infection”. -

Antibiotic Prophylaxis for GI Endoscopy
GUIDELINE Antibiotic prophylaxis for GI endoscopy This is one of a series of statements discussing the use of procedure. Endoscopy-related bacteremia carries a small GI endoscopy in common clinical situations. The Stan- risk of localization of infection in remote tissues (ie, infec- dards of Practice Committee of the American Society for tive endocarditis [IE]). Endoscopy also may result in local Gastrointestinal Endoscopy (ASGE) prepared this docu- infections in which a typically sterile space or tissue is ment, and it updates a previously issued document on breached and contaminated by an endoscopic accessory this topic.1 In preparing this guideline, MEDLINE and or by contrast material injection. This document is an up- PubMed databases were used to search for publications date of the prior ASGE document on antibiotic prophylaxis between January 1975 and December 2013 pertaining for GI endoscopy,1 discusses infectious adverse events to this topic. The search was supplemented by accessing related to endoscopy, and provides recommendations for the “related articles” feature of PubMed, with articles periprocedural antibiotic therapy. identified on MEDLINE and PubMed as the references. Additional references were obtained from the bibliogra- phies of the identified articles and from recommenda- BACTEREMIA ASSOCIATED WITH tions of expert consultants. When few or no data were ENDOSCOPIC PROCEDURES available from well-designed prospective trials, emphasis was given to results from large series and reports from Bacteremia can occur after endoscopic procedures and has been advocated as a surrogate marker for IE risk. How- recognized experts. Weaker recommendations are indi- fi cated by phrases such as “We suggest.” whereas stronger ever, clinically signi cant infections are extremely rare.