Multiple Unilateral Variations in Medial and Lateral Cords of Brachial Plexus and Their Branches
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Anatomical Variants of the Musculocutaneous Nerve- Report of Two Cases
Open Access CRIMSON PUBLISHERS C Wings to the Research Research in Anatomy ISSN: 2577-1922 Case Report Anatomical Variants of the Musculocutaneous Nerve- Report of Two Cases Fernando Martinez1,2 and Guzmán Ripoll1* 1Anatomy Department, Facultad de Medicina Universidad Claeh, Uruguay 2Neurosurgery Department, Universidad de la República, Uruguay *Corresponding author: Guzmán Ripoll, AnatomyDepartment, Facultad de Medicina Universidad Claeh, Maldonado, Uruguay, Email: Submission: February 22, 2018; Published: April 19, 2018 Abstract Introduction: The muscle-cutaneous nerve (MCN) is a mixed nerve, which is mainly responsible for shoulder flexion, elbow flexion and supinationMaterial of theand hand. method: The anatomical variations in this nerve are relatively frequent, fact with clinical and surgical implications. Results: Two variants were A retrospective found in the review 20 cases of 20studied patients (10% operated of the cases): on with anastomosis the Oberlin betweentechnique MCN was and made. median nerve, and absence of the MCN.Discussion: MCN variants are frequently described by the different authors. This has an embryological and phylogenetic explanation: the lateralConclusion: and medial cords form the flexor plane of the muscles of the upper limb. We present 2 cases: an unusual one of median nerve-MCN, and another absence of it. We emphasize that the knowledge of these variants have clinical, surgical and neuro-physiological applications. Introduction The musclecutaneous nerve (MCN) is a mixed nerve, which from basically the use of fascicles of the median nerve to reinforce the ulnar nerve (Figure 1). The modifications of this technique are the motor point of view is mainly responsible for shoulder flexion, brachial plexus injuries with involvement of the upper trunk (C5- the muscles that innervate: coracobrachial, biceps brachialis and anterior brachial muscle (Figure 2). -

Anatomical Variations of the Brachial Plexus Terminal Branches in Ethiopian Cadavers
ORIGINAL COMMUNICATION Anatomy Journal of Africa. 2017. Vol 6 (1): 896 – 905. ANATOMICAL VARIATIONS OF THE BRACHIAL PLEXUS TERMINAL BRANCHES IN ETHIOPIAN CADAVERS Edengenet Guday Demis*, Asegedeche Bekele* Corresponding Author: Edengenet Guday Demis, 196, University of Gondar, Gondar, Ethiopia. Email: [email protected] ABSTRACT Anatomical variations are clinically significant, but many are inadequately described or quantified. Variations in anatomy of the brachial plexus are important to surgeons and anesthesiologists performing surgical procedures in the neck, axilla and upper limb regions. It is also important for radiologists who interpret plain and computerized imaging and anatomists to teach anatomy. This study aimed to describe the anatomical variations of the terminal branches of brachial plexus on 20 Ethiopian cadavers. The cadavers were examined bilaterally for the terminal branches of brachial plexus. From the 40 sides studied for the terminal branches of the brachial plexus; 28 sides were found without variation, 10 sides were found with median nerve variation, 2 sides were found with musculocutaneous nerve variation and 2 sides were found with axillary nerve variation. We conclude that variation in the median nerve was more common than variations in other terminal branches. Key words: INTRODUCTION The brachial plexus is usually formed by the may occur (Moore and Dalley, 1992, Standring fusion of the anterior primary rami of the C5-8 et al., 2005). and T1 spinal nerves. It supplies the muscles of the back and the upper limb. The C5 and C6 fuse Most nerves in the upper limb arise from the to form the upper trunk, the C7 continues as the brachial plexus; it begins in the neck and extends middle trunk and the C8 and T1 join to form the into the axilla. -

Brachial-Plexopathy.Pdf
Brachial Plexopathy, an overview Learning Objectives: The brachial plexus is the network of nerves that originate from cervical and upper thoracic nerve roots and eventually terminate as the named nerves that innervate the muscles and skin of the arm. Brachial plexopathies are not common in most practices, but a detailed knowledge of this plexus is important for distinguishing between brachial plexopathies, radiculopathies and mononeuropathies. It is impossible to write a paper on brachial plexopathies without addressing cervical radiculopathies and root avulsions as well. In this paper will review brachial plexus anatomy, clinical features of brachial plexopathies, differential diagnosis, specific nerve conduction techniques, appropriate protocols and case studies. The reader will gain insight to this uncommon nerve problem as well as the importance of the nerve conduction studies used to confirm the diagnosis of plexopathies. Anatomy of the Brachial Plexus: To assess the brachial plexus by localizing the lesion at the correct level, as well as the severity of the injury requires knowledge of the anatomy. An injury involves any condition that impairs the function of the brachial plexus. The plexus is derived of five roots, three trunks, two divisions, three cords, and five branches/nerves. Spinal roots join to form the spinal nerve. There are dorsal and ventral roots that emerge and carry motor and sensory fibers. Motor (efferent) carries messages from the brain and spinal cord to the peripheral nerves. This Dorsal Root Sensory (afferent) carries messages from the peripheral to the Ganglion is why spinal cord or both. A small ganglion containing cell bodies of sensory NCS’s sensory fibers lies on each posterior root. -

Anastomotic Branch from the Median Nerve to the Musculocutaneous Nerve: a Case Report
Case Report www.anatomy.org.tr Recieved: February 10, 2008; Accepted: April 22, 2008; Published online: October 31, 2008 doi:10.2399/ana.08.063 Anastomotic branch from the median nerve to the musculocutaneous nerve: a case report Feray Güleç Uyaro¤lu1, Gülgün Kayal›o¤lu2, Mete Ertürk2 1Department of Neurology, Ege University Faculty of Medicine, Izmir, Turkey 2Department of Anatomy, Ege University Faculty of Medicine, Izmir, Turkey Abstract Anomalies of the brachial plexus and its terminal branches are not uncommon. Communicating branch arising from the mus- culocutaneous nerve to the median nerve is a frequent variation, whereas the presence of an anastomotic branch arising from the median nerve and joining the musculocutaneous nerve is very rare. During routine dissection of cadaver upper limbs, we observed an anastomotic branch arising from the median nerve running distally to join with the branches of the musculocutaneous nerve in a left upper extremity. The anastomotic branch originated from the median nerve 11.23 cm prox- imal to the interepicondylar line. After running distally and coursing between the biceps brachii and the brachialis muscles, this anastomotic branch communicated with two branches of the musculocutaneous nerve separately. The presence of the communicating branches between these nerves should be considered during surgical interventions and clinical investigations of the arm. Key words: anatomy; brachial plexus; communicating branch; upper limb; variation Anatomy 2008; 2: 63-66, © 2008 TSACA Introduction neous nerve (C5, C6, and C7) connects with the median nerve in the arm.2,3 The musculocutaneous nerve is the Variations of the brachial plexus and its terminal continuation of the lateral cord of the brachial plexus. -

Bilateral Anatomical Variation in the Formation of Trunks of the Brachial Plexus - a Case Report
THIEME Case Report 9 Bilateral Anatomical Variation in the Formation of Trunks of the Brachial Plexus - A Case Report E.F. Lasch1 M.B. Nazer1 L.M. Bartholdy1 1 Laboratório de Anatomia Humana, Departamento de Biologia e Address for correspondence E. F. Lasch, Laboratório de Anatomia Farmácia, Universidade Santa Cruz do Sul – UNISC, Santa Cruz do Sul, Humana, Departamento de Biologia e Farmácia, Universidade Santa RioGrandedoSul,Brazil Cruz do Sul – UNISC, Av Independência, 2293, CEP 96815-900, Santa Cruz do Sul, RS, Brazil (e-mail: [email protected]). J Morphol Sci 2018;35:9–13. Abstract This study presents a bilateral variation in the formation of trunks of brachial plexus in a male cadaver. The right brachial plexus was composed of six roots (C4-T1) and the left brachial plexus of five roots (C5-T1). Both formed four trunks thus changing the contributions of the anterior divisions of the cervical nerves involved in the formation Keywords of the cords and the five main somatic motor nerves for the upper limb. There are very ► brachial plexus few case reports in the scientific literature on this topic; thus making the present study ► trunks very relevant. Introduction medial and lateral pectoral nerve, arise from the cords and innervate the shoulder muscles. The long infraclavicular Most of the upper limb nerves arise from by the brachial branches, which extend longitudinally to the upper limb, plexus (BP), which has a complex anatomical structure that are: the radial nerve, the ulnar nerve, and the median begins in the root of the neck and extends to the axilla nerve.4,5 (armpit region). -
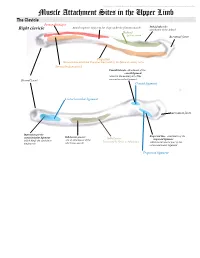
Muscle Attachment Sites in the Upper Limb
This document was created by Alex Yartsev ([email protected]); if I have used your data or images and forgot to reference you, please email me. Muscle Attachment Sites in the Upper Limb The Clavicle Pectoralis major Smooth superior surface of the shaft, under the platysma muscle Deltoid tubercle: Right clavicle attachment of the deltoid Deltoid Axillary nerve Acromial facet Trapezius Sternocleidomastoid and Trapezius innervated by the Spinal Accessory nerve Sternocleidomastoid Conoid tubercle, attachment of the conoid ligament which is the medial part of the Sternal facet coracoclavicular ligament Conoid ligament Costoclavicular ligament Acromial facet Impression for the Trapezoid line, attachment of the costoclavicular ligament Subclavian groove: Subclavius trapezoid ligament which binds the clavicle to site of attachment of the Innervated by Nerve to Subclavius which is the lateral part of the the first rib subclavius muscle coracoclavicular ligament Trapezoid ligament This document was created by Alex Yartsev ([email protected]); if I have used your data or images and forgot to reference you, please email me. The Scapula Trapezius Right scapula: posterior Levator scapulae Supraspinatus Deltoid Deltoid and Teres Minor are innervated by the Axillary nerve Rhomboid minor Levator Scapulae, Rhomboid minor and Rhomboid Major are innervated by the Dorsal Scapular Nerve Supraspinatus and Infraspinatus innervated by the Suprascapular nerve Infraspinatus Long head of triceps Rhomboid major Teres Minor Teres Major Teres Major -

Brachial Plexus Injury Investigation , Localization and Treatment
BRACHIAL PLEXUS INJURY INVESTIGATION , LOCALIZATION AND TREATMENT EMBRYOLOGY § Brachial plexus (BP) is developed at 5 weeks of gestation § Afferent fibers develop from neuroblast located alongside neural tube § Efferent fibers originate from neuroblast in the basal plate of tube from where they grow outside § Afferent and efferent fibers join to form the nerve § Nerves divide into anterior and posterior divisions § There are connections between these nerves in the brachial plexus commons.wikimedia.org/wiki/File:Brachial_plexus.jpg ANATOMY lFormed by ventral primary rami of lower four cervical and first thoracic nerve root. l Frequently have contributions from C4(pre-fixed) or T2 (post-fixed). PREFIXED BRACHIAL PLEXUS http://www.msdlatinamerica.com/ebooks/HandSurgery/sid744608.html Post-fixed plexus http://www.msdlatinamerica.com/ebooks/HandSurgery/sid744608.html RELATIONS OF BRACHIAL PLEXUS Fig. 4. The reIationship of the axillary artery to the cords is an important anatomic relationship. The cords surround the axiIIary artery and are named for their position with respect to the axillary artery. L.C. lateral cord MC. Medial cord: PC . posterior Cord. Levels § Roots § Real § Trunks § Texans § Divisions § Drink § Cords § Cold § Branches § Beer § C5 and C6 roots form upper trunk § C8 and T1 roots the lower trunk § C7 forms the middle trunk § Joining point of C5-C6 roots is ERB”S POINT § Each trunk divides into an anterior and a posterior division and passes beneath the clavicle § All 3 posterior divisions merge to form the posterior cord § Anterior division of the upper and middle trunk merge to form the lateral cord § Anterior division of lower trunk forms the medial cord § Lateral cord splits into 2 terminal branches: a) Musculocutaneous nerve b) Lateral cord contribution to median nerve (sensory) § Posterior cord splits into a)axillary nerve and b)radial nerve § Medial cord gives off a) medial cord contribution to the median nerve(motor) and b)ulnar nerve § There are few terminal branches of the roots trunks and cords. -

The SPA Arrangement of the Branches of the Upper Trunk of the Brachial Plexus: a Correction of a Longstanding Misconception and a New Diagram of the Brachial Plexus
LABORATORY INVESTIGATION J Neurosurg 125:350–354, 2016 The SPA arrangement of the branches of the upper trunk of the brachial plexus: a correction of a longstanding misconception and a new diagram of the brachial plexus Amgad Hanna, MD Department of Neurological Surgery, University of Wisconsin, Madison, Wisconsin OBJECTIVE Brachial plexus (BP) diagrams in most textbooks and papers represent the branches and divisions of the upper trunk (UT) in the following sequence from cranial to caudal: suprascapular nerve, anterior division, and then posterior division. This concept contradicts what is seen in the operating room and is noticed by most peripheral nerve surgeons. This cadaveric study was conducted to look specifically at the exact pattern of branching of the upper trunk of the BP. METHODS Ten cadavers (20 BPs) were dissected. Both supra- and infraclavicular exposures were performed. The clavicle was retracted or resected to identify the divisions of the BP. A posterior approach was used in 2 cases. RESULTS In all dissections the origin of the posterior division was in a more cranial and dorsal plane in relation to the anterior division. In most dissections the supra scapular nerve branched off distally from the UT, giving it the appearance of a trifurcation, taking off just cranial and dorsal to the posterior division. The branching pattern of the UT consistently had the following sequential arrangement from cranial and posterior to caudal and anterior: suprascapular nerve (S), posterior division (P), and anterior division (A), hence the acronym SPA. CONCLUSIONS Supraclavicular exposure of the BP exposes only the trunks and divisions. Recognizing the “SPA” arrangement of the branches helps in identifying the correct targets for neurotization, especially given that these 3 branches are the most common targets for BP repair. -

Pectoral Nerves – a Third Nerve and Clinical Implications Kleehammer, A.C., Davidson, K.B., and Thompson, B.J
Pectoral Nerves – A Third Nerve and Clinical Implications Kleehammer, A.C., Davidson, K.B., and Thompson, B.J. Department of Anatomy, DeBusk College of Osteopathic Medicine, Lincoln Memorial University Introduction Summary Table 1. Initial Dataset and Observations The textbook description of the pectoral nerves A describes a medial and lateral pectoral nerve arising A from the medial and lateral cords, respectively, to innervate the pectoralis major and minor muscles. Studies have described variations in the origins and branching of the pectoral nerves and even in the muscles they innervate (Porzionato et al., 2011, Larionov et al., 2020). There have also been reports of three pectoral nerves with distinct origins (Aszmann et Table 1: Initial Dataset and Observations Our initial dataset consisted of 31 anatomical donors, dissected bilaterally, Each side was considered an al., 2000) and variability of the spinal nerve fibers Independent observation. Of the 62 brachial plexuses, 50 met our inclusion criteria. contributing to these nerves (Lee, 2007). Given the Table 2. Branching Patterns of Pectoral Nerves frequency of reported variation from the textbook description, reexamining the origin, course and B branching of the pectoral nerves could prove useful for B students and clinicians alike. The pectoral nerves are implicated in a variety of cases including surgeries of the breast, pectoral, and axillary region (David et al., 2012). Additionally, the lateral pectoral nerve has recently gained attention for potential use as a nerve graft for other damaged nerves such as the spinal accessory nerve (Maldonado, et al., 2017). The objective of this study was to assess the frequency and patterns of pectoral nerve branching in order to more accurately describe their orientation and implications in clinical cases. -

Axilla & Brachial Plexus
Anatomy Guy Dissection Sheet Axilla & Brachial Plexus Dr. Craig Goodmurphy Anatomy Guy Major Dissection Objectives 1. Review some of the superficial veins and nerves and extrapolate skin incisions down the arm while sparing the cephalic and basilic veins 2. Secure the upper limb in an abducted position and review the borders of the axilla while reflecting pec major and minor. 3. You may need to remove the middle third of the clavicle with bone cutters or oscillating saw 4. Identify and open the axillary sheath to find the axillary vein and separate it away from the arteries and nerves 5. Once it is mobilized remove smaller veins and reflect the axillary vein medially Major Dissection Objectives Arteries 6. Locate and clean the subclavian artery as it becomes the axillary a. at the first rib. 7. Identifying part 1, 2 and 3 of the axillary artery as they relate to pectoralis minor 8. Identify & clean the thoracoacromial trunk and its branches along with the lateral thoracic artery 9. Clean the subscapular artery and follow it to the circumflex scapular and thoracodorsal branches removing the fat of the region and noting variations and lymph nodes that may be present. 10. Locate the posterior and anterior humeral circumflex arteries and the brachial artery Eastern Virginia Medical School 1 Anatomy Guy Dissection Sheet Axilla & Brachial Plexus Major Dissection Objectives Nerves 11. Review the parts of the brachial plexus with roots in the scalene gap, trunks superior to the clavicle, divisions posterior to the clavicle, cords and branches inferior to the clavicle. 12. Locate the musculocutaneous nerve laterally as it pierces the coracobrachialis m. -
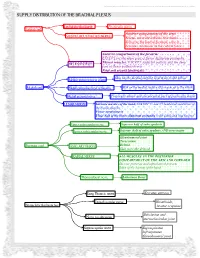
Supply Distribution of the Brachial Plexus
This document was created by Alex Yartsev ([email protected]); if I have used your data or images and forgot to reference you, please email me. SUPPLY DISTRIBUTION OF THE BRACHIAL PLEXUS Lateral pectoral nerve Pectoralis major Lateral cord Anterior compartment of the arm: MUSCULOCUTANEOUS NERVE Biceps, coracobrachialis, brachialis Skin over the lateral forearm, once it becomes cutaneous in the cubital fossa Anterior compartment of the forearm: EXCEPT for the ulnar part of flexor digitorum profundis MEDIAN NERVE Thenar muscles: EXCEPT adductor pollicis and the deep part of flexor pollicis brevis First and second lumbricals Skin on the medial surface of arm up to the elbow MedialLateral cutaneous cord: nerve of arm lateral pectoral nerve Medial cord Skin on the medial surface of forearm up to the elbow Medial cutaneous MUSCULOCUTANEOUS nerve of forearm NERVE lateral root of MEDIAN NERVE Medial pectoral nerve Pectoralis minor and sternocostal part of pectoralis major o Medial cord forms ULNAR NERVE Intrinsic muscles of the hand, EXCEPT 1st and 2nd lumbricals and three of the thenar muscles Flexor carpi ulnaris Ulnar half of the flexor digitorum profundis to the pinky and ring fingers Upper subscapular nerve Superior half of subscapularis medial root of MEDIAN NERVE Lower subscapular nerve Inferior half of subscapularis AND teres major medial pectoral nerve medial cutaneous nerveGlenohumeral of arm joint Teres minor medial cutaneous nerve of forearm Posterior cord AXILLARY NERVE Deltoid ULNAR NERVE Skin over the deltoid RADIAL NERVE ALL MUSCLES IN THE POSTERIOR COMPARTMENT OF THE ARM AND FOREARM Ski over posterior and inferolateral forearm Some of the dorsum of the hand o o Thoracodorsal nerve Latissimus Dorsi o o Posterior cord forms: Long Thoracic nerve Serratus anterior Dorsal scapular nerve Rhomboids; Supraclavicular branches levator scapulae Subclavius and Nerve to subclavius sternoclavicular joint Suprascapular nerve Supraspinatus Infraspinatus Glenohumeral joint. -

Pectoral Region and Axilla Doctors Notes Notes/Extra Explanation Editing File Objectives
Color Code Important Pectoral Region and Axilla Doctors Notes Notes/Extra explanation Editing File Objectives By the end of the lecture the students should be able to : Identify and describe the muscles of the pectoral region. I. Pectoralis major. II. Pectoralis minor. III. Subclavius. IV. Serratus anterior. Describe and demonstrate the boundaries and contents of the axilla. Describe the formation of the brachial plexus and its branches. The movements of the upper limb Note: differentiate between the different regions Flexion & extension of Flexion & extension of Flexion & extension of wrist = hand elbow = forearm shoulder = arm = humerus I. Pectoralis Major Origin 2 heads Clavicular head: From Medial ½ of the front of the clavicle. Sternocostal head: From; Sternum. Upper 6 costal cartilages. Aponeurosis of the external oblique muscle. Insertion Lateral lip of bicipital groove (humerus)* Costal cartilage (hyaline Nerve Supply Medial & lateral pectoral nerves. cartilage that connects the ribs to the sternum) Action Adduction and medial rotation of the arm. Recall what we took in foundation: Only the clavicular head helps in flexion of arm Muscles are attached to bones / (shoulder). ligaments / cartilage by 1) tendons * 3 muscles are attached at the bicipital groove: 2) aponeurosis Latissimus dorsi, pectoral major, teres major 3) raphe Extra Extra picture for understanding II. Pectoralis Minor Origin From 3rd ,4th, & 5th ribs close to their costal cartilages. Insertion Coracoid process (scapula)* 3 Nerve Supply Medial pectoral nerve. 4 Action 1. Depression of the shoulder. 5 2. Draw the ribs upward and outwards during deep inspiration. *Don’t confuse the coracoid process on the scapula with the coronoid process on the ulna Extra III.