42X60 Horizontal Poster
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

World Journal of Pharmaceutical Research Mathur Et Al
World Journal of Pharmaceutical Research Mathur et al . World Journal of Pharmaceutical SJIF ResearchImpact Factor 8.074 Volume 7, Issue 16, 111-124. Review Article ISSN 2277– 7105 ADRS DUE TO ANTIPSYCHOTIC DRUGS: A REVIEW Prashant Mathur*1 and Waseem Yahya2 1,2Department of Pharmacy Practice Shri Guru Ram Rai Institute of Technology and Science, Patel Nagar (248001), Dehradun, Uttarakhand. INTRODUCTION Article Received on 28 June 2018, WHO defines an ADR as ―any response to a drug which is noxious and Revised on 18 July 2018, unintended, and which occurs at doses normally used in man for Accepted on 08 August 2018, DOI: 10.20959/wjpr201816-12706 prophylaxis, diagnosis, or therapy of disease, or for the modification of physiological function‖.[1] The antipsychotic drugs are chemically *Corresponding Author diverse but have the common property of alleviating the symptoms of [2] Prashant Mathur organic as well as functional psychosis. Antipsychotics are among Department of Pharmacy the most effective drugs used in psychiatry in the maintenance therapy Practice Shri Guru Ram Rai of schizophrenia, mania, or in acute psychotic reactions.[3] These drugs Institute of Technology and are also capable of causing a wide range of potential adverse drug Science, Patel Nagar (248001), Dehradun, reactions that can lead to non-compliance that can impair quality of Uttarakhand. life, may cause stigma and physical morbidity which may lead to discontinuation of medication and in extreme cases may be fatal.[4] Antipsychotic drugs have a high therapeutic -

Strategies for Managing Sexual Dysfunction Induced by Antidepressant Medication
King’s Research Portal DOI: 10.1002/14651858.CD003382.pub3 Document Version Publisher's PDF, also known as Version of record Link to publication record in King's Research Portal Citation for published version (APA): Taylor, M. J., Rudkin, L., Bullemor-Day, P., Lubin, J., Chukwujekwu, C., & Hawton, K. (2013). Strategies for managing sexual dysfunction induced by antidepressant medication. Cochrane Database of Systematic Reviews, (5). https://doi.org/10.1002/14651858.CD003382.pub3 Citing this paper Please note that where the full-text provided on King's Research Portal is the Author Accepted Manuscript or Post-Print version this may differ from the final Published version. If citing, it is advised that you check and use the publisher's definitive version for pagination, volume/issue, and date of publication details. And where the final published version is provided on the Research Portal, if citing you are again advised to check the publisher's website for any subsequent corrections. General rights Copyright and moral rights for the publications made accessible in the Research Portal are retained by the authors and/or other copyright owners and it is a condition of accessing publications that users recognize and abide by the legal requirements associated with these rights. •Users may download and print one copy of any publication from the Research Portal for the purpose of private study or research. •You may not further distribute the material or use it for any profit-making activity or commercial gain •You may freely distribute the URL identifying the publication in the Research Portal Take down policy If you believe that this document breaches copyright please contact [email protected] providing details, and we will remove access to the work immediately and investigate your claim. -

Properties and Units in Clinical Pharmacology and Toxicology
Pure Appl. Chem., Vol. 72, No. 3, pp. 479–552, 2000. © 2000 IUPAC INTERNATIONAL FEDERATION OF CLINICAL CHEMISTRY AND LABORATORY MEDICINE SCIENTIFIC DIVISION COMMITTEE ON NOMENCLATURE, PROPERTIES, AND UNITS (C-NPU)# and INTERNATIONAL UNION OF PURE AND APPLIED CHEMISTRY CHEMISTRY AND HUMAN HEALTH DIVISION CLINICAL CHEMISTRY SECTION COMMISSION ON NOMENCLATURE, PROPERTIES, AND UNITS (C-NPU)§ PROPERTIES AND UNITS IN THE CLINICAL LABORATORY SCIENCES PART XII. PROPERTIES AND UNITS IN CLINICAL PHARMACOLOGY AND TOXICOLOGY (Technical Report) (IFCC–IUPAC 1999) Prepared for publication by HENRIK OLESEN1, DAVID COWAN2, RAFAEL DE LA TORRE3 , IVAN BRUUNSHUUS1, MORTEN ROHDE1, and DESMOND KENNY4 1Office of Laboratory Informatics, Copenhagen University Hospital (Rigshospitalet), Copenhagen, Denmark; 2Drug Control Centre, London University, King’s College, London, UK; 3IMIM, Dr. Aiguader 80, Barcelona, Spain; 4Dept. of Clinical Biochemistry, Our Lady’s Hospital for Sick Children, Crumlin, Dublin 12, Ireland #§The combined Memberships of the Committee and the Commission (C-NPU) during the preparation of this report (1994–1996) were as follows: Chairman: H. Olesen (Denmark, 1989–1995); D. Kenny (Ireland, 1996); Members: X. Fuentes-Arderiu (Spain, 1991–1997); J. G. Hill (Canada, 1987–1997); D. Kenny (Ireland, 1994–1997); H. Olesen (Denmark, 1985–1995); P. L. Storring (UK, 1989–1995); P. Soares de Araujo (Brazil, 1994–1997); R. Dybkær (Denmark, 1996–1997); C. McDonald (USA, 1996–1997). Please forward comments to: H. Olesen, Office of Laboratory Informatics 76-6-1, Copenhagen University Hospital (Rigshospitalet), 9 Blegdamsvej, DK-2100 Copenhagen, Denmark. E-mail: [email protected] Republication or reproduction of this report or its storage and/or dissemination by electronic means is permitted without the need for formal IUPAC permission on condition that an acknowledgment, with full reference to the source, along with use of the copyright symbol ©, the name IUPAC, and the year of publication, are prominently visible. -

<I>Iguana Iguana</I>
Journal of the American Association for Laboratory Animal Science Vol 58, No 6 Copyright 2019 November 2019 by the American Association for Laboratory Animal Science Pages 810–816 Use of Rodent Sedation Tests to Evaluate Midazolam and Flumazenil in Green Iguanas (Iguana iguana) Thais F Bressan, Thayanee Sobreira, and Adriano B Carregaro* This study aimed to evaluate the applicability of rodent behavioral tests to assess the effects of midazolam and flumazenil in green iguanas. Four tests commonly used to assess sedation in rodents—the open field test, forced swim test, behavioral scale, and traction test—were conducted in 10 juveniles iguanas. The animals received midazolam (2 mg/kg IM) or 0.9% NaCl (0.4 mL/kg IM), and the tests were conducted between 0 and 300 min thereafter. To verify the effects of midazolam and flumazenil, the most informative tests from the evaluation stage and the limb withdrawal latency time (LWLT) were used. All 10 iguanas were tested under 4 conditions, as follows: MS, midazolam (2 mg/kg IM), followed 30 min later by 0.9% NaCl (0.4 mL/kg IM); FS, flumazenil (0.05 mg/kg IM), followed by 0.9% NaCl (0.4 mL/kg IM) 30 min later; MF, midazolam (2 mg/ kg IM), followed by flumazenil (0.05 mg/kg IM) 30 min later; and CON, 0.9% NaCl (0.4 mL/kg IM). The behavioral scale and the forced swim test showed the best detection of the onset, peak effect, and the differences between the sedated and con- trol iguanas, with testing done between 15 and 240 min after drug administration. -

The Effects of Antipsychotic Treatment on Metabolic Function: a Systematic Review and Network Meta-Analysis
The effects of antipsychotic treatment on metabolic function: a systematic review and network meta-analysis Toby Pillinger, Robert McCutcheon, Luke Vano, Katherine Beck, Guy Hindley, Atheeshaan Arumuham, Yuya Mizuno, Sridhar Natesan, Orestis Efthimiou, Andrea Cipriani, Oliver Howes ****PROTOCOL**** Review questions 1. What is the magnitude of metabolic dysregulation (defined as alterations in fasting glucose, total cholesterol, low density lipoprotein (LDL) cholesterol, high density lipoprotein (HDL) cholesterol, and triglyceride levels) and alterations in body weight and body mass index associated with short-term (‘acute’) antipsychotic treatment in individuals with schizophrenia? 2. Does baseline physiology (e.g. body weight) and demographics (e.g. age) of patients predict magnitude of antipsychotic-associated metabolic dysregulation? 3. Are alterations in metabolic parameters over time associated with alterations in degree of psychopathology? 1 Searches We plan to search EMBASE, PsycINFO, and MEDLINE from inception using the following terms: 1 (Acepromazine or Acetophenazine or Amisulpride or Aripiprazole or Asenapine or Benperidol or Blonanserin or Bromperidol or Butaperazine or Carpipramine or Chlorproethazine or Chlorpromazine or Chlorprothixene or Clocapramine or Clopenthixol or Clopentixol or Clothiapine or Clotiapine or Clozapine or Cyamemazine or Cyamepromazine or Dixyrazine or Droperidol or Fluanisone or Flupehenazine or Flupenthixol or Flupentixol or Fluphenazine or Fluspirilen or Fluspirilene or Haloperidol or Iloperidone -

Maternal Use of Psychiatric Medications During Pregnancy And
MATERNAL USE OF PSYCHIATRIC MEDICATIONS DURING PREGNANCY AND ADVERSE BIRTH OUTCOMES AND NEURODEVELOPMENTAL PROBLEMS IN OFFSPRING Ayesha C. Sujan Submitted to the faculty of the University Graduate School in partial fulfillment of the requirements for the degree Doctor of Philosophy in the Department of Psychological and Brain Sciences, Indiana University July 2021 ii Accepted by the Graduate Faculty, Indiana University, in partial fulfillment of the requirements for the degree of Doctor of Philosophy. Doctoral Committee _______________________________________________ Brian M. D’Onofrio, PhD _______________________________________________ Richard Viken, PhD _______________________________________________ Patrick D. Quinn, PhD _______________________________________________ Christina Ludema, PhD _______________________________________________ A. Sara Oberg, PhD, MD April 22nd, 2020 iii © 2021 Ayesha C. Sujan iv Ayesha Sujan MATERNAL USE OF PSYCHIATRIC MEDICATIONS DURING PREGNANCY AND ADVERSE BIRTH OUTCOMES AND NEURODEVELOPMENTAL PROBLEMS IN OFFSPRING Understanding consequences of prenatal exposure to psychiatric and analgesic medications is important because use of these medications among pregnant women is relatively common and increasing. Rodent experiments have shown effects of perinatal exposure to specific medications; however, these findings might not apply to humans. Human observational studies have been used to study prenatal exposure to psychiatric and analgesic medications rather than randomiZed control trials due to ethical concerns -

Redalyc.Tissue Depletion of Azaperone and Its Metabolite
Revista de Toxicología ISSN: 0212-7113 [email protected] Asociación Española de Toxicología España Mestorino, N.; Marchetti, M. L.; Daniele, M.; Martínez, M. A.; Martínez-Larrañaga, M. R.; Anadón, A. Tissue depletion of azaperone and its metabolite azaperol after oral administration of azaperone in food-producing pigs Revista de Toxicología, vol. 30, núm. 2, julio-diciembre, 2013, pp. 209-214 Asociación Española de Toxicología Pamplona, España Available in: http://www.redalyc.org/articulo.oa?id=91931189013 How to cite Complete issue Scientific Information System More information about this article Network of Scientific Journals from Latin America, the Caribbean, Spain and Portugal Journal's homepage in redalyc.org Non-profit academic project, developed under the open access initiative Rev. Toxicol. (2013) 30: 209-214 Tissue depletion of azaperone and its metabolite azaperol after oral administration of azaperone in food-producing pigs Mestorino N1* , Marchetti M L1 , Daniele M1 , Martínez M A2 , Martínez-Larrañaga M R2 , Anadón A2 . 1Laboratorio de Estudios Farmacológicos y Toxicológicos (LEFyT), Facultad de Ciencias Veterinarias, Universidad Nacional de La Plata, 1900- La Plata, Buenos Aires, Argentina. 2Departamento de Toxicología y Farmacología, Facultad de Veterinaria, Universidad Complutense de Madrid, 28040-Madrid, España. Recibido 5 de noviembre de 2013 / Aceptado 20 de diciembre de 2013 Abstract: Azaperone is a butyrophenone tranquilizer for swine. establecidos por la Unión Europea (100 mg / kg en el músculo, el Food producing pigs are particularly sensitive to stress during hígado, los riñones y la piel + grasa) en ningún momento del handling and transport to the abattoir. In vivo, azaperone is partially muestreo. Como consecuencia, según los resultados obtenidos en el metabolised to azaperol, a metabolite with pharmacological activity. -

When Taking Medication May Be a Sin: Dietary Requirements and Food Laws
BJPsych Advances (2015), vol. 21, 425–432 doi: 10.1192/apt.bp.114.012534 When taking medication may be a ARTICLE sin: dietary requirements and food laws in psychotropic prescribing Waqqas A. Khokhar, Simon L. Dein, Mohammed S. Qureshi, Imran Hameed, Mohammed M. Ali, Yasir Abbasi, Hasan Aman & Ruchit Sood In psychiatric practice, it is not uncommon to Waqqas A. Khokhar is a SUMMARY come across patients who refuse any psychiatric consultant psychiatrist with Leicestershire Partnership NHS Religious laws do not usually forbid the use of intervention, placing their faith in a spiritual psychotropic medication, but many do forbid the Trust and an honorary lecturer in recovery enabled by their religious beliefs (Campion the Centre for Ageing and Mental consumption of animal-based derivatives of bovine 1997; Koenig 2001). Although religious laws do Health at Staffordshire University. and/or porcine origin (e.g. gelatin and stearic not usually restrict the taking of psychotropic Simon L. Dein is a senior lecturer acid) such as are found in many medications. at University College London, an Demonstrating awareness of this, combined with medication, many do forbid consumption of the Honorary Clinical Professor at a genuine concern about how it affects the patient, animal derivatives, particularly gelatin and stearic the University of Durham and a may strengthen the doctor–patient relationship acid, that many psychotropics contain. This has consultant psychiatrist with the and avoid non-adherence. In this article, we major implications, for example, for patients who North Essex Partnership University NHS Foundation Trust. Mohammed outline dietary requirements of key religions and follow Judaism, Islam, Hinduism, Buddhism and S. -
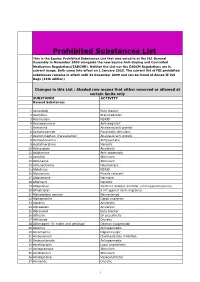
Prohibited Substances List
Prohibited Substances List This is the Equine Prohibited Substances List that was voted in at the FEI General Assembly in November 2009 alongside the new Equine Anti-Doping and Controlled Medication Regulations(EADCMR). Neither the List nor the EADCM Regulations are in current usage. Both come into effect on 1 January 2010. The current list of FEI prohibited substances remains in effect until 31 December 2009 and can be found at Annex II Vet Regs (11th edition) Changes in this List : Shaded row means that either removed or allowed at certain limits only SUBSTANCE ACTIVITY Banned Substances 1 Acebutolol Beta blocker 2 Acefylline Bronchodilator 3 Acemetacin NSAID 4 Acenocoumarol Anticoagulant 5 Acetanilid Analgesic/anti-pyretic 6 Acetohexamide Pancreatic stimulant 7 Acetominophen (Paracetamol) Analgesic/anti-pyretic 8 Acetophenazine Antipsychotic 9 Acetylmorphine Narcotic 10 Adinazolam Anxiolytic 11 Adiphenine Anti-spasmodic 12 Adrafinil Stimulant 13 Adrenaline Stimulant 14 Adrenochrome Haemostatic 15 Alclofenac NSAID 16 Alcuronium Muscle relaxant 17 Aldosterone Hormone 18 Alfentanil Narcotic 19 Allopurinol Xanthine oxidase inhibitor (anti-hyperuricaemia) 20 Almotriptan 5 HT agonist (anti-migraine) 21 Alphadolone acetate Neurosteriod 22 Alphaprodine Opiod analgesic 23 Alpidem Anxiolytic 24 Alprazolam Anxiolytic 25 Alprenolol Beta blocker 26 Althesin IV anaesthetic 27 Althiazide Diuretic 28 Altrenogest (in males and gelidngs) Oestrus suppression 29 Alverine Antispasmodic 30 Amantadine Dopaminergic 31 Ambenonium Cholinesterase inhibition 32 Ambucetamide Antispasmodic 33 Amethocaine Local anaesthetic 34 Amfepramone Stimulant 35 Amfetaminil Stimulant 36 Amidephrine Vasoconstrictor 37 Amiloride Diuretic 1 Prohibited Substances List This is the Equine Prohibited Substances List that was voted in at the FEI General Assembly in November 2009 alongside the new Equine Anti-Doping and Controlled Medication Regulations(EADCMR). -

Original Article E€Ects of Serotonin 1A Agonist on Acute Spinal Cord Injury
Spinal Cord (2002) 40, 519 ± 523 ã 2002 International Spinal Cord Society All rights reserved 1362 ± 4393/02 $25.00 www.nature.com/sc Original Article Eects of serotonin 1A agonist on acute spinal cord injury Y Saruhashi*,1, Y Matsusue1 and S Hukuda2 1Department of Orthopedic Surgery, Shiga University of Medical Science, Otsu, Japan; 2Tane-daini Hospital, Osaka, Japan Study design: We evaluated the eects of serotonin (5-HT) agonists on in vitro models of spinal cord compressive injury. Evoked potentials in injured rat spinal cords (n=24) were recorded during perfusion with 5-HT agonists. Objectives: To evaluate the therapeutic eects of 5-HT agonists on the recovery of compound action potentials in injured spinal cords. Methods: Rat dorsal columns were isolated, placed in a chamber, and injured by extradural compression with a clip. Conducting action potentials were activated by supramaximal constant current electrical stimuli and recorded during perfusion with 5-HT agonists and antagonists. Results: After inducing compression injuries, mean action potential amplitudes were reduced to 33.9+5.4% of the pre-injury level. After 120 min of perfusion with Ringer's solution, the mean amplitudes recovered to 62.8+8.4% of the pre-injury level. At a concentration of 100 mM, perfusion with tandospirone (a 5-HT1A agonist) resulted in a signi®cantly greater recovery of mean action potential amplitudes at 2 h after the injury (86.2+6.9% of pre-injury value) as compared with the control Ringer's solution (62.8+8.4% of pre-injury value, P50.05). In contrast, quipazine (a 5-HT2A agonist) accelerated the decrease of amplitude (54.5+11.7% of pre-injury value). -

Anesthesia and Analgesia in Laboratory Animals
GUIDELINES ON ANESTHESIA AND ANALGESIA IN LABORATORY ANIMALS University of South Florida provides the following guidelines for use by IACUC-certified faculty and staff. CONTENTS PAGE A. Background……………………………………………………….…………………………… 1 B. Definitions....……………………………………………………..…………………………….. 2 C. General Considerations……………………………………….,…………………………….. 3 D. Controlled Substances……………………………………….……………………………… 3 E. Pre-Anesthetic Treatments………………………………….………………………………. 4 F. General Anesthetics………………………………………….………………………………. 4 G. Neuromuscular Blocking Agents………………………….……………………………….. 5 H. Monitoring Anesthesia…………………………………….…………………………………. 6 I. Analgesics……………………………………………………………………………………… 7 J. Comments regarding Anesthetics and Analgesics……………………………………... 7 REFERENCE TABLES PAGE I. Signs of Pain and Distress in Laboratory Animals………………………………………… 10 II. Commonly Used Anesthetics and Analgesics for Mice….………..…...….………...…… 11 III. Commonly Used Anesthetics and Analgesics for Rats……………………………...…… 12 IV. Commonly Used Anesthetics and Analgesics for Gerbils……….……………..…….. 13 V. Commonly Used Anesthetics and Analgesics for Hamsters…….……………..……. 14 VI. Commonly Used Anesthetics and Analgesics for Guinea Pigs….…………….….……. 15 VII. Commonly Used Anesthetics and Analgesics for Rabbits.……...…………….………… 16 VIII. Commonly Used Anesthetics and Analgesics for Dogs.…………………….…………… 17 IX. Commonly Used Anesthetics and Analgesics for Cats.……………………..…………… 18 X. Commonly Used Anesthetics and Analgesics for Pigs ..……………..….………………..19 XI. Commonly Used Anesthetics and Analgesics -

Antipsychotics
The Fut ure of Antipsychotic Therapy (page 7 in syllabus) Stepp,,hen M. Stahl, MD, PhD Adjunct Professor, Department of Psychiatry Universityyg of California, San Diego School of Medicine Honorary Visiting Senior Fellow, Cambridge University, UK Sppyonsored by the Neuroscience Education Institute Additionally sponsored by the American Society for the Advancement of Pharmacotherapy This activity is supported by an educational grant from Sunovion Pharmaceuticals Inc. Copyright © 2011 Neuroscience Education Institute. All rights reserved. Individual Disclosure Statement Faculty Editor / Presenter Stephen M. Stahl, MD, PhD, is an adjunct professor in the department of psychiatry at the University of California, San Diego School of Medicine, and an honorary visiting senior fellow at the University of Cambridge in the UK. Grant/Research: AstraZeneca, BioMarin, Dainippon Sumitomo, Dey, Forest, Genomind, Lilly, Merck, Pamlab, Pfizer, PGxHealth/Trovis, Schering-Plough, Sepracor/Sunovion, Servier, Shire, Torrent Consultant/Advisor: Advent, Alkermes, Arena, AstraZeneca, AVANIR, BioMarin, Biovail, Boehringer Ingelheim, Bristol-Myers Squibb, CeNeRx, Cypress, Dainippon Sumitomo, Dey, Forest, Genomind, Janssen, Jazz, Labopharm, Lilly, Lundbeck, Merck, Neuronetics, Novartis, Ono, Orexigen, Otsuka, Pamlab, Pfizer, PGxHealth/Trovis, Rexahn, Roche, Royalty, Schering-Plough, Servier, Shire, Solvay/Abbott, Sunovion/Sepracor, Valeant, VIVUS, Speakers Bureau: Dainippon Sumitomo, Forest, Lilly, Merck, Pamlab, Pfizer, Sepracor/Sunovion, Servier, Wyeth Copyright © 2011 Neuroscience Education Institute. All rights reserved. Learninggj Objectives • Differentiate antipsychotic drugs from each other on the basis of their pharmacological mechanisms and their associated therapeutic and side effects • Integrate novel treatment approaches into clinical practice according to best practices guidelines • Identify novel therapeutic options currently being researched for the treatment of schizophrenia Copyright © 2011 Neuroscience Education Institute.