VHA Handbook 1173.13, Home Oxygen Respiratory Care Program
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

2018 Full Line Catalog Products to Support Dive Shop Operations Table of Contents
2018 FULL LINE CATALOG PRODUCTS TO SUPPORT DIVE SHOP OPERATIONS TABLE OF CONTENTS 3 6 8 TEST EQUIPMENT REGULATOR SERVICE & Flowbenches, ACCESSORIES MAINTENANCE workstations, test Regulator, BC and Tools, O-rings, chambers and other console hoses, chemicals and products used in swivels, adapters and equipment used testing regulators, dive related items. for the service and computers and other maintenance of dive related items. regulators, tanks and other dive equipment. 15 17 19 AIR FILTRATION COMPRESSORS TANK FILLING Filters, towers, bulk Small to medium Whips, fill filter chemicals sized breathing attachments and and related control air compressors, adapters for filling hardware for compressor oils and SCUBA, DIN, SCBA breathing air filtration related accessories. and many other tank/ systems. valve styles. 22 28 30 COMPRESSED GAS PAINTBALL MIXED GAS / HARDWARE Whips, adapters and NITROX / OXYGEN Air station hardware, accessories for filling Hardware, chemicals regulators, valves and servicing paint and tools used and fittings for ball tanks and related for the creation, the storage and equipment. handling and analysis distributions of High of mixed gas, Nitrox Pressure Air. and Oxygen. SALES INFORMATION [email protected] 512.240.6644 • 800.558.1811 voice • 512.240.6645 fax MAILING ADDRESS 4674 Priem Lane, Suite 402 • Pflugerville, TX 78660 ANY AND ALL INFORMATION SUBJECT TO CHANGE WITHOUT NOTICE. ALL RIGHTS RESERVED. www.global-mfg.com 2 | TABLE OF CONTENTS TEST EQUIPMENT and stability, and systemic air rubber cup adapter which 48250 Compact Deluxe FLOWBENCHES tightness. Air flow rates through replaces the mouthpiece. First Flowbench with Double tank valves or gas manifolds stage intermediate pressure is Magnehelic Our top-of-the-line analyzer is can also be determined. -

Frequently Asked Questions (Faqs)
Frequently Asked Questions (FAQs) What is hyperbaric oxygen therapy? Commonly referred to as HBOT, hyperbaric oxygen therapy enhances the body’s natural healing process by delivering oxygen under pressure, which increases the oxygen content in the blood, plasma, cerebral spinal fluid, and other body tissues. There are two basic types of HBOT—hard HBOT and mild HBOT. With hard HBOT, treatments are delivered in a hard-sided chamber typically at pressures greater than 1.5 ATA and using 100% oxygen. 100% oxygen is extremely flammable; therefore, hard HBOT involves managing the risk of explosion. Another concern with hard HBOT is oxygen toxicity. While hard HBOT with 100% oxygen results in greater oxygen saturation in the tissues, many conditions respond better to mild HBOT. In clinical trials to date, there has been virtually no difference in clinical outcome between mild HBOT and hard HBOT. Mild HBOT refers to hyperbaric oxygen therapy at lower pressures, typically 1.5 ATA or below, and the use of an oxygen concentrator delivering 90-95% oxygen inside a portable soft-sided chamber. Mild HBOT has no known safety risks with fire or toxicity, and it is substantially less expensive. Our facility provides concentrated oxygen (90-95%) at 1.3 ATA—(Mild HBOT)a highly effective combination clinically, and without the risk of oxygen toxicity or explosion, as 100% oxygen is avoided. How should I expect mild HBOT to feel? You will be seated or lying down inside the chamber, relaxing comfortably in your own clothing, as you breathe concentrated oxygen (90-95% O2) through a facemask. -

Stratus 5 Oxygen Concentrator User Manual
USER MANUAL OXYGEN CONCENTRATOR CE 0123 v2.1 STR1005 User Manual Symbol Key MARK DEFINITION II Power on Power off Follow Instruction for Use No smoking Caution, consult accompanying documents. Class Ⅱ (Double Insulated) Type BF Applied Part CE certification mark 0123 AC Power Stacking Limit by Number This Way Up Fragile, handle with care Keep dry Temperature limit No open flames IIPP2211 IP21 Drip Proof Equipment Consult instructions for use Stand-by Warning, electricity 2 v2.1 STR1005 User Manual 3 v2.1 STR1005 User Manual SPECIAL NOTES • Please read this manual carefully before using this product and save it for future reference. • If you need assistance with this manual, Please contact your local DME or home health provider • The Stratus 5 is a prescription device. Use only the liter setting prescribed for you. • It is always recommended for critically ill patients to have a backup oxygen source in case of malfunction. • If patient experiences an adverse reaction contact physician or call 911 immediately. • In case of machine malfunction, contact the home medical equipment provider; do not attempt to disassemble the Stratus 5. • The Stratus 5 is not intended as life support, it is for supplemental oxygen use only. Patients with special needs may be unable to understand the alarm features and should be well supervised while using an oxygen concentrator. • The Stratus 5 is for single patient use. • Do not adjust the flowmeter float beyond the red line position. Long-term use out of range will reduce the efficiency of the oxygen generator. SAFETY NOTICE Please read the following information carefully before Operating the oxygen concentrator Warning Special attention should be paid to reducing the risk of fire when using oxygen therapy. -

Rebreathers Open Inspiration Fully Closed Rebreather What Is It Like? Text & Photos by Peter Symes Diving Rebreathers Why Bother?
WWW.AQUALUNG.COM Dräger Ray semiclosed rebreather. Behind, an Rebreathers open Inspiration fully closed rebreather What is it like? WWW.AMBIENTPRESSUREDIVING.COM Text & photos by Peter Symes Diving Rebreathers Why bother? Rebreathers look cool, glitzy, tech- they provide for a much differ- nical and heralded as the future of ent and richer diving experience, which, in the first place, is why we go in diving, right? We read a lot about the water ourselves rather than watch- their impressive performances con- ing dive movies on Animal Planet from cerning duration of dives, gas econ- the comfort of our reclining chair at home. omy, extended no deco limits and However, as we all know, there is no such thing as a free lunch in diving either. There is what not. But isn’t it a bit like watch- a trade-off, and you will have to consider if it the underwater realm so you can have an ing Jeremy Clarkson from BBC’s car is still worth your while despite this. enriching experience by witnessing, first program, Top Gear, whiz around in It is not merely a matter of comparing hand, this magic realm. So, as far as I am fancy Ferraris and Aston Martins with technical matters, performance and param- concerned, if someone invented human eters when pitting rebreathers against the gills and a thin hide to cover and keep me a goofy, happy grin on his face and open circuits (regulators and tanks). It is warm, my twin-set would surely be left to rust reeling off a string of excited super- easy to be blinded by dazzling numbers and in the attic for good. -
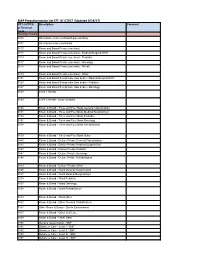
MAP Preauthorization List EFF: 8/1/2017 (Updated 8/24/17)
MAP Preauthorization List EFF: 8/1/2017 (Updated 8/24/17) CPT, HCPCS Description Comment or Revenue Code Revenue Codes 0100 All inclusive room and board plus ancillary 0101 All inclusive room and board 0110 Room and Board Private (one bed) 0111 Room and Board Private (one bed) - Medical/Surgical/GYN 0113 Room and Board Private (one bed) - Pediatric 0117 Room and Board Private (one bed) - Oncology 0118 Room and Board Private (one bed) - Rehab 0119 Room and Board Private (one bed) - Other 0121 Room and Board Semiprivate (two beds) - Medical/Surgical/GYN 0123 Room and Board Semiprivate (two beds) - Pediatric 0127 Room and Board Semiprivate (two beds) - Oncology 0128 Level 1 Rehab 0129 Level 2 Rehab - acute complex 0130 Room & Board - Three and Four Beds General Classification 0131 Room & Board - Three and Four Beds Medical/Surgical/Gyn 0133 Room & Board - Three and Four Beds Pediatric 0137 Room & Board - Three and Four Beds Oncology 0138 Room & Board - Three and Four Beds Rehabilitation 0139 Room & Board - Three and Four Beds Other 0140 Room & Board - Deluxe Private General Classification 0141 Room & Board - Deluxe Private Medical/Surgical/Gyn 0143 Room & Board - Deluxe Private Pediatric 0147 Room & Board - Deluxe Private Oncology 0148 Room & Board - Deluxe Private Rehabilitation 0149 Room & Board - Deluxe Private Other 0150 Room & Board - Ward General Classification 0151 Room & Board - Ward Medical/Surgical/Gyn 0153 Room & Board - Ward Pediatric 0157 Room & Board - Ward Oncology 0158 Room & Board - Ward Rehabilitation 0159 Room & Board - -

E-Cigarette Use in Patients Receiving Home Oxygen Therapy
FOCUSED REVIEW E-cigarette use in patients receiving home oxygen therapy Yves Lacasse MD MSc FRCP1,2, Martin Légaré MD FRCP3, François Maltais MD FRCP1,2 Y Lacasse, M Légaré, F Maltais. E-cigarette use in patients receiving La cigarette électronique chez les patients sous home oxygen therapy. Can Respir J 2015;22(2):83-85. oxygénothérapie à domicile Current smokers who are prescribed home oxygen may not benefit from the therapy. In addition to being an obvious fire hazard, there is some evi- Il se peut que les fumeurs qui se font prescrire une oxygénothérapie à domi- dence that the physiological mechanisms by which home oxygen is cile ne profitent pas de ce traitement. Sans compter que le tabagisme pose believed to operate are inhibited by smoking. Although their effectiveness un risque d’incendie évident, certaines données probantes indiquent qu’il is yet to be demonstrated, electronic cigarettes (e-cigarettes) are often inhibe les mécanismes physiologiques par lesquels l’oxygénothérapie à regarded as an aid to smoking cessation. However, several burn accidents domicile fonctionnerait. Même si son efficacité reste à démontrer, la ciga- in e-cigarette smokers receiving home oxygen therapy have also been rette électronique (vapoteuse) est souvent perçue comme une aide au reported, leading Health Canada to release a warning of fire risk to oxygen sevrage du tabagisme. Cependant, plusieurs incidents de brûlure chez des therapy patients from e-cigarettes. It is the authors’ position that patients vapoteurs sous oxygénothérapie à domicile ont été déclarés, ce qui a incité receiving oxygen should definitely not use e-cigarettes. -

Florida Special Needs Registry Registration Information - Osceola County
Florida Special Needs Registry Registration Information - Osceola County Instructions: Complete this form and fax or mail it to Osceola County to register an individual for the Florida Special Needs Registry. This form is not required if you have already registered on line. Required fields are indicated with an asterisk (*). Mail: Osceola County Special Needs Registry Fax: (407) 742-9022 2586 Partin Settlement Road Kissimmee, FL 34744 PERSONAL INFORMATION ABOUT THE REGISTRANT *First Name Middle Name *Last Name Suffix *Birth Date *Gender (select only one) Male Female Transgender Non-Binary Prefer Not To Provide *Height Feet: Inches: *Weight (pounds) Living Situation (select only one) Live alone Live with relative or Other living situation caregiver *Primary Language Secondary Language Veteran Yes No Last 4 digits of SSN Email Address Are you completing this form on behalf of the Family Member Caregiver Neighbor Friend registrant? If so, please indicate your relationship to the registrant (select only Home Health Care County Emergency County Health DOH State Staff one) Provider Management Staff Department Staff ADDRESS FOR THE REGISTRANT (physical address is required) *Physical Address (cannot be a PO Box) *Physical City *Physical State FL *Physical Zip Code Name of Complex, Subdivision or Mobile Home Park Is the home at this address a mobile home? Yes No Is the home at this address a highrise or Yes No multi-story home? Does this home have stairs? Yes No Is there a gate that requires a code to enter? Yes No Do you live at this address -

Emblemhealth's Pre-Authorization List
EmblemHealth's Pre-authorization List This is a complete list of all services requiring a Prior Approval for HIP members or a Pre-Certification for GHI members* (jointly referred to as "pre-authorization") subject to their benefit plan's coverage for all places of service, including Office (POS 11). The list accounts for EmblemHealth's medical policies, medical technology database, provider manual, and special utilization management programs. Pre-authorization is not a guarantee of payment. Payment is subject to a member's eligibility for benefits on the date of service. Emergency services do not require a pre-authorization. *GHI PPO City of New York employees and non-Medicare eligible retirees with GHI PPO benefits will be managed by Empire BCBS for inpatient and outpatient services. To see what needs authorization, use their look-up tool: https://www.empireblue.com/wps/portal/ehpprovider. CPT/ HCPCS Description Code 0008M Oncology (breast), mRNA analysis of 58 genes using hybrid capture, on formalin-fixed paraffin- embedded (FFPE) tissue, prognostic algorithm reported as a risk score 00640 Anesthesia for manipulation of the spine or for closed procedures on the cervical, thoracic or lumbar spine 0085T Breath test for heart transplant rejection 0100T Placement of a subconjunctival retinal prosthesis receiver and pulse generator, and implantation of intra-ocular retinal electrode array, with vitrectomy 0195T Arthrodesis, pre-sacral interbody technique, disc space preparation, discectomy, without instrumentation, with image guidance, includes -

Portable Oxygen Concentrator Therapy Guide Guidance for Patients Requiring Long-Term, Supplemental Oxygen Solutions
Portable Oxygen Concentrator Therapy Guide Guidance for patients requiring long-term, supplemental oxygen solutions. Table of Contents Part One: Oxygen Therapy 101 Part Two: Oxygen Concentrators Part Three: Portable Oxygen Concentrators Part Four: Which Oxygen Concentrator is Right For You? Confused or overwhelmed? Let us help you! Our Product Specialists are standing by to answer questions and offer tips.(800) 515-8049 INTRODUCTION 3 Welcome! OxygenDirect is pleased to provide this educational guide for current and potential patients to understand the benefits of oxygen therapy—and specifically portable oxygen concentrators. We intend to expand patients’ knowledge and appreciation of advancements in technology that are now available. This document is designed to complement the information provided by a doctor or healthcare provider when discussing oxygen therapy options. Who is OxygenDirect? OxygenDirect is dedicated to helping oxygen therapy patients breathe easier without interfering with lifestyles and daily activities. We offer a wide selection of portable and home oxygen products and accessories, plus a diverse range of CPAP machines and accessories. Our OxygenDirect Product Specialists can help evaluate patients’ oxygen needs and varying product features to ultimately arrive at a product that perfectly fits a wide range of lifestyles and budgets. Disclaimer: The information contained in this document is general in nature and is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health providers with any questions you may have regarding a breathing/medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this document. -

Oxygen Safety
Oxygen Safety Table of Contents Page In your Home 1. Prepare your Home ..................................................................... 3 2. Fire Safety Guidelines................................................................. 4 3. Oxygen Storage and Handling ................................................... 6 4. Concentrator Safety .................................................................... 6 5. Liquid Oxygen Safety .................................................................. 6 On the Go 6. Tips for Traveling with Oxygen .................................................. 7 7. Automobile Travel with Oxygen ................................................. 7 8. Cruise Line Travel with Oxygen ................................................. 8 9. Bus Travel with Oxygen .............................................................. 8 10. Train Travel with Oxygen ............................................................ 9 11. Airline Travel with Oxygen ......................................................... 9 References .................................................................................................. 11 Contact Us .................................................................................................. 11 Printable No Smoking Sign ....................................................................... 12 Printable Oxygen in Use Sign ................................................................... 13 This booklet provides general safety information for oxygen concentrators, compressed -

COVID-19 Basic Manual on Oxygen Supply Systems in Emts and AMCS
Emergency Medical Teams Operational Support COVID-19 Basic Manual on oxygen supply systems in EMTs and AMCS Preliminary Document - Version 2.1, 18 February 2021 PAN AMERICAN HEALTH ORGANIZATION (PAHO/WHO) | www.paho.org Contents 1. Introduction.....................................................................................3 2. Basic concepts ..................................................................................4 2.1 Medical gases .............................................................................4 2.2 Medical parameters of O2 ..................................................................4 2.3 Regulation.................................................................................5 3. Sources of oxygen for medical use...............................................................6 4. Oxygen systems for medical use.................................................................9 4.1 Individual O2 systems .....................................................................11 4.1.1 Individual cylinders...............................................................11 4.1.2 Individual concentrators ..........................................................12 4.2 Centralized O2 systems ...................................................................12 4.3 Components .............................................................................13 4.3.1 Pipes and fittings..................................................................13 4.3.2 Sockets and connectors...........................................................15 -

Oxygen Therapy Orders
Welcome to the Specialized Medical Services Respiratory training webinar series! SMS is your Long Term Care (LTC) facility single source for oxygen, medical equipment, respiratory care services and supplies nationwide. This respiratory module is for reference purposes and designed to provide a basic understanding of Oxygen Equipment commonly used in Long Term Care. It is still important to consult your local respiratory professional and follow physician orders when applying respiratory treatment. At the completion of each training module, a short post test will be offered, and with successful completion, a training certificate recognizing your participation for your records. Oxygen Equipment Webinar Training Session Training Objectives • Recognize the different types of oxygen equipment • Understand how to operate each piece of equipment • Select the right system for your patients’ needs • Learn common troubleshooting techniques 3 Primary System Types 1. Compressed gas (cylinder/tank) 2. Oxygen concentrators 3. Liquid oxygen Compressed Gas Cylinders • Compressed Oxygen • Stored under pressure in a vessel or tank • Variety of tank sizes Oxygen Concentrators • Electrically operated devices • Draw in air from the surrounding room • Filter out the nitrogen • Compress the remaining oxygen for patient use • Deliver medical grade oxygen Liquid Oxygen • Compressed and cooled • Converts oxygen to a liquid state • Much larger storage ratio of oxygen Types of Compressed Gas Cylinders “Walk O2 About” Aluminum E Standard Aluminum E With Integrated