Supplemental Methods and Results
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

A Computational Approach for Defining a Signature of Β-Cell Golgi Stress in Diabetes Mellitus
Page 1 of 781 Diabetes A Computational Approach for Defining a Signature of β-Cell Golgi Stress in Diabetes Mellitus Robert N. Bone1,6,7, Olufunmilola Oyebamiji2, Sayali Talware2, Sharmila Selvaraj2, Preethi Krishnan3,6, Farooq Syed1,6,7, Huanmei Wu2, Carmella Evans-Molina 1,3,4,5,6,7,8* Departments of 1Pediatrics, 3Medicine, 4Anatomy, Cell Biology & Physiology, 5Biochemistry & Molecular Biology, the 6Center for Diabetes & Metabolic Diseases, and the 7Herman B. Wells Center for Pediatric Research, Indiana University School of Medicine, Indianapolis, IN 46202; 2Department of BioHealth Informatics, Indiana University-Purdue University Indianapolis, Indianapolis, IN, 46202; 8Roudebush VA Medical Center, Indianapolis, IN 46202. *Corresponding Author(s): Carmella Evans-Molina, MD, PhD ([email protected]) Indiana University School of Medicine, 635 Barnhill Drive, MS 2031A, Indianapolis, IN 46202, Telephone: (317) 274-4145, Fax (317) 274-4107 Running Title: Golgi Stress Response in Diabetes Word Count: 4358 Number of Figures: 6 Keywords: Golgi apparatus stress, Islets, β cell, Type 1 diabetes, Type 2 diabetes 1 Diabetes Publish Ahead of Print, published online August 20, 2020 Diabetes Page 2 of 781 ABSTRACT The Golgi apparatus (GA) is an important site of insulin processing and granule maturation, but whether GA organelle dysfunction and GA stress are present in the diabetic β-cell has not been tested. We utilized an informatics-based approach to develop a transcriptional signature of β-cell GA stress using existing RNA sequencing and microarray datasets generated using human islets from donors with diabetes and islets where type 1(T1D) and type 2 diabetes (T2D) had been modeled ex vivo. To narrow our results to GA-specific genes, we applied a filter set of 1,030 genes accepted as GA associated. -

4-6 Weeks Old Female C57BL/6 Mice Obtained from Jackson Labs Were Used for Cell Isolation
Methods Mice: 4-6 weeks old female C57BL/6 mice obtained from Jackson labs were used for cell isolation. Female Foxp3-IRES-GFP reporter mice (1), backcrossed to B6/C57 background for 10 generations, were used for the isolation of naïve CD4 and naïve CD8 cells for the RNAseq experiments. The mice were housed in pathogen-free animal facility in the La Jolla Institute for Allergy and Immunology and were used according to protocols approved by the Institutional Animal Care and use Committee. Preparation of cells: Subsets of thymocytes were isolated by cell sorting as previously described (2), after cell surface staining using CD4 (GK1.5), CD8 (53-6.7), CD3ε (145- 2C11), CD24 (M1/69) (all from Biolegend). DP cells: CD4+CD8 int/hi; CD4 SP cells: CD4CD3 hi, CD24 int/lo; CD8 SP cells: CD8 int/hi CD4 CD3 hi, CD24 int/lo (Fig S2). Peripheral subsets were isolated after pooling spleen and lymph nodes. T cells were enriched by negative isolation using Dynabeads (Dynabeads untouched mouse T cells, 11413D, Invitrogen). After surface staining for CD4 (GK1.5), CD8 (53-6.7), CD62L (MEL-14), CD25 (PC61) and CD44 (IM7), naïve CD4+CD62L hiCD25-CD44lo and naïve CD8+CD62L hiCD25-CD44lo were obtained by sorting (BD FACS Aria). Additionally, for the RNAseq experiments, CD4 and CD8 naïve cells were isolated by sorting T cells from the Foxp3- IRES-GFP mice: CD4+CD62LhiCD25–CD44lo GFP(FOXP3)– and CD8+CD62LhiCD25– CD44lo GFP(FOXP3)– (antibodies were from Biolegend). In some cases, naïve CD4 cells were cultured in vitro under Th1 or Th2 polarizing conditions (3, 4). -

Identification of Differentially Expressed Genes in Human Bladder Cancer Through Genome-Wide Gene Expression Profiling
521-531 24/7/06 18:28 Page 521 ONCOLOGY REPORTS 16: 521-531, 2006 521 Identification of differentially expressed genes in human bladder cancer through genome-wide gene expression profiling KAZUMORI KAWAKAMI1,3, HIDEKI ENOKIDA1, TOKUSHI TACHIWADA1, TAKENARI GOTANDA1, KENGO TSUNEYOSHI1, HIROYUKI KUBO1, KENRYU NISHIYAMA1, MASAKI TAKIGUCHI2, MASAYUKI NAKAGAWA1 and NAOHIKO SEKI3 1Department of Urology, Graduate School of Medical and Dental Sciences, Kagoshima University, 8-35-1 Sakuragaoka, Kagoshima 890-8520; Departments of 2Biochemistry and Genetics, and 3Functional Genomics, Graduate School of Medicine, Chiba University, 1-8-1 Inohana, Chuo-ku, Chiba 260-8670, Japan Received February 15, 2006; Accepted April 27, 2006 Abstract. Large-scale gene expression profiling is an effective CKS2 gene not only as a potential biomarker for diagnosing, strategy for understanding the progression of bladder cancer but also for staging human BC. This is the first report (BC). The aim of this study was to identify genes that are demonstrating that CKS2 expression is strongly correlated expressed differently in the course of BC progression and to with the progression of human BC. establish new biomarkers for BC. Specimens from 21 patients with pathologically confirmed superficial (n=10) or Introduction invasive (n=11) BC and 4 normal bladder samples were studied; samples from 14 of the 21 BC samples were subjected Bladder cancer (BC) is among the 5 most common to microarray analysis. The validity of the microarray results malignancies worldwide, and the 2nd most common tumor of was verified by real-time RT-PCR. Of the 136 up-regulated the genitourinary tract and the 2nd most common cause of genes we detected, 21 were present in all 14 BCs examined death in patients with cancer of the urinary tract (1-7). -

Blood-Derived Mitochondrial DNA Copy Number Is Associated with Gene Expression Across Multiple
bioRxiv preprint doi: https://doi.org/10.1101/2020.07.17.209023; this version posted July 18, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. 1 Blood-derived mitochondrial DNA copy number is associated with gene expression across multiple 2 tissues and is predictive for incident neurodegenerative disease 3 4 Stephanie Y. Yang1, Christina A. Castellani1, Ryan J. Longchamps1, Vamsee K. Pillalamarri1, Brian 5 O’Rourke2, Eliseo Guallar3, Dan E. Arking1,2 6 7 8 1McKusick-Nathans Department of Genetic Medicine, Johns Hopkins University School of Medicine, 9 Baltimore, MD 10 2Division of Cardiology, Department of Medicine, Johns Hopkins University School of Medicine, 11 Baltimore, MD 12 3Departments of Epidemiology and Medicine, and Welch Center for Prevention, Epidemiology, and 13 Clinical Research, Johns Hopkins University Bloomberg School of Public Health, Baltimore, MD 14 15 Email addresses: 16 [email protected] 17 [email protected] 18 [email protected] 19 [email protected] 20 [email protected] 21 [email protected] 22 [email protected] 23 24 25 26 27 28 29 30 31 32 33 34 35 *Correspondence and address for reprints to: 36 Dan E. Arking, Ph.D. 37 Johns Hopkins University School of Medicine 38 733 N Broadway Ave 39 Miller Research Building Room 459 40 Baltimore, MD 21205 41 (410) 502-4867 (ph) 42 [email protected] 1 bioRxiv preprint doi: https://doi.org/10.1101/2020.07.17.209023; this version posted July 18, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. -

A High-Throughput Approach to Uncover Novel Roles of APOBEC2, a Functional Orphan of the AID/APOBEC Family
Rockefeller University Digital Commons @ RU Student Theses and Dissertations 2018 A High-Throughput Approach to Uncover Novel Roles of APOBEC2, a Functional Orphan of the AID/APOBEC Family Linda Molla Follow this and additional works at: https://digitalcommons.rockefeller.edu/ student_theses_and_dissertations Part of the Life Sciences Commons A HIGH-THROUGHPUT APPROACH TO UNCOVER NOVEL ROLES OF APOBEC2, A FUNCTIONAL ORPHAN OF THE AID/APOBEC FAMILY A Thesis Presented to the Faculty of The Rockefeller University in Partial Fulfillment of the Requirements for the degree of Doctor of Philosophy by Linda Molla June 2018 © Copyright by Linda Molla 2018 A HIGH-THROUGHPUT APPROACH TO UNCOVER NOVEL ROLES OF APOBEC2, A FUNCTIONAL ORPHAN OF THE AID/APOBEC FAMILY Linda Molla, Ph.D. The Rockefeller University 2018 APOBEC2 is a member of the AID/APOBEC cytidine deaminase family of proteins. Unlike most of AID/APOBEC, however, APOBEC2’s function remains elusive. Previous research has implicated APOBEC2 in diverse organisms and cellular processes such as muscle biology (in Mus musculus), regeneration (in Danio rerio), and development (in Xenopus laevis). APOBEC2 has also been implicated in cancer. However the enzymatic activity, substrate or physiological target(s) of APOBEC2 are unknown. For this thesis, I have combined Next Generation Sequencing (NGS) techniques with state-of-the-art molecular biology to determine the physiological targets of APOBEC2. Using a cell culture muscle differentiation system, and RNA sequencing (RNA-Seq) by polyA capture, I demonstrated that unlike the AID/APOBEC family member APOBEC1, APOBEC2 is not an RNA editor. Using the same system combined with enhanced Reduced Representation Bisulfite Sequencing (eRRBS) analyses I showed that, unlike the AID/APOBEC family member AID, APOBEC2 does not act as a 5-methyl-C deaminase. -

Proteomic Shifts in Embryonic Stem Cells with Gene Dose Modifications Suggest the Presence of Balancer Proteins in Protein Regulatory Networks
Proteomic shifts in embryonic stem cells with gene dose modifications suggest the presence of balancer proteins in protein regulatory networks. Lei Mao, Claus Zabel, Marion Herrmann, Tobias Nolden, Florian Mertes, Laetitia Magnol, Caroline Chabert, Daniela Hartl, Yann Herault, Jean Maurice Delabar, et al. To cite this version: Lei Mao, Claus Zabel, Marion Herrmann, Tobias Nolden, Florian Mertes, et al.. Proteomic shifts in embryonic stem cells with gene dose modifications suggest the presence of balancer proteins in protein regulatory networks.. PLoS ONE, Public Library of Science, 2007, 2 (11), pp.e1218. 10.1371/jour- nal.pone.0001218. hal-00408296 HAL Id: hal-00408296 https://hal.archives-ouvertes.fr/hal-00408296 Submitted on 31 May 2020 HAL is a multi-disciplinary open access L’archive ouverte pluridisciplinaire HAL, est archive for the deposit and dissemination of sci- destinée au dépôt et à la diffusion de documents entific research documents, whether they are pub- scientifiques de niveau recherche, publiés ou non, lished or not. The documents may come from émanant des établissements d’enseignement et de teaching and research institutions in France or recherche français ou étrangers, des laboratoires abroad, or from public or private research centers. publics ou privés. Proteomic Shifts in Embryonic Stem Cells with Gene Dose Modifications Suggest the Presence of Balancer Proteins in Protein Regulatory Networks Lei Mao1,2*, Claus Zabel1, Marion Herrmann1, Tobias Nolden2, Florian Mertes2, Laetitia Magnol3, Caroline Chabert4, Daniela -

Dominant Mutations in Mtdna Maintenance Gene SSBP1 Cause Optic Atrophy and Foveopathy
Dominant mutations in mtDNA maintenance gene SSBP1 cause optic atrophy and foveopathy Camille Piro-Mégy, … , Maria Sola, Cécile Delettre J Clin Invest. 2020;130(1):143-156. https://doi.org/10.1172/JCI128513. Research Article Genetics Ophthalmology Graphical abstract Find the latest version: https://jci.me/128513/pdf The Journal of Clinical Investigation RESEARCH ARTICLE Dominant mutations in mtDNA maintenance gene SSBP1 cause optic atrophy and foveopathy Camille Piro-Mégy,1 Emmanuelle Sarzi,1 Aleix Tarrés-Solé,2 Marie Péquignot,1 Fenna Hensen,3 Mélanie Quilès,1 Gaël Manes,1 Arka Chakraborty,2 Audrey Sénéchal,1 Béatrice Bocquet,1,4 Chantal Cazevieille,1 Agathe Roubertie,1,4 Agnès Müller,1,5 Majida Charif,6 David Goudenège,6 Guy Lenaers,6 Helmut Wilhelm,7 Ulrich Kellner,8 Nicole Weisschuh,9 Bernd Wissinger,9 Xavier Zanlonghi,10 Christian Hamel,1,4 Johannes N. Spelbrink,3 Maria Sola,2 and Cécile Delettre1 1Institute of Neurosciences of Montpellier, INSERM, University of Montpellier, Montpellier, France. 2Structural MitoLab, Department of Structural Biology, “Maria de Maeztu” Unit of Excellence, Molecular Biology Institute Barcelona (IBMB-CSIC), Barcelona, Spain. 3Radboud Center for Mitochondrial Medicine, Department of Paediatrics, Radboudumc, Nijmegen, Netherlands. 4CHU Montpellier, Centre of Reference for Genetic Sensory Diseases, Gui de Chauliac Hospital, Montpellier, France. 5Faculté de Pharmacie, Université de Montpellier, Montpellier, France. 6UMR CNRS 6015-INSERM U1083, MitoVasc Institute, Angers University, Angers, France. 7University Eye Hospital, Centre for Ophthalmology, University of Tübingen, Tübingen, Germany. 8Rare Retinal Disease Center, AugenZentrum Siegburg, MVZ Augenärztliches Diagnostik- und Therapiecentrum Siegburg GmbH, Siegburg, Germany. 9Institute for Ophthalmic Research, Centre for Ophthalmology, University of Tübingen, Tübingen, Germany. -

The Genome-Wide Dynamics of the Binding of Ldb1 Complexes During Erythroid Differentiation
Downloaded from genesdev.cshlp.org on September 28, 2021 - Published by Cold Spring Harbor Laboratory Press The genome-wide dynamics of the binding of Ldb1 complexes during erythroid differentiation Eric Soler,1,7,9 Charlotte Andrieu-Soler,1,7 Ernie de Boer,1,7 Jan Christian Bryne,2,8 Supat Thongjuea,2,8 Ralph Stadhouders,1 Robert-Jan Palstra,1 Mary Stevens,1 Christel Kockx,3 Wilfred van IJcken,3 Jun Hou,1 Christine Steinhoff,4 Erikjan Rijkers,5 Boris Lenhard,2,11 and Frank Grosveld1,6,10 1Department of Cell Biology, Erasmus Medical Center, 3015GE Rotterdam, The Netherlands; 2Computational Biology Unit- Bergen Center for Computational Science and Sars Centre for Marine Molecular Biology, University of Bergen, N-5008 Bergen, Norway; 3Biomics Department, Erasmus Medical Center, 3015GE Rotterdam, The Netherlands; 4Department of Computational Biology, Max Planck Institute for Molecular Genetics, 14195 Berlin, Germany; 5Department of Biochemistry, Erasmus Medical Center, 3015GE Rotterdam, The Netherlands; 6Center for Biomedical Genetics and Cancer Genomics Center, Erasmus Medical Center, 3015GE Rotterdam, The Netherlands One of the complexes formed by the hematopoietic transcription factor Gata1 is a complex with the Ldb1 (LIM domain-binding protein 1) and Tal1 proteins. It is known to be important for the development and differentiation of the erythroid cell lineage and is thought to be implicated in long-range interactions. Here, the dynamics of the composition of the complex—in particular, the binding of the negative regulators Eto2 and Mtgr1—are studied, in the context of their genome-wide targets. This shows that the complex acts almost exclusively as an activator, binding a very specific combination of sequences, with a positioning relative to transcription start site, depending on the type of the core promoter. -

New Insights Into the Runt Domain of RUNX2 in Melanoma Cell Proliferation and Migration
cells Article New Insights into the Runt Domain of RUNX2 in Melanoma Cell Proliferation and Migration Michela Deiana 1,2 , Luca Dalle Carbonare 2 , Michela Serena 1 , Samuele Cheri 1,2 , Francesca Parolini 1 , Alberto Gandini 3, Giulia Marchetto 2, Giulio Innamorati 3, Marcello Manfredi 4, Emilio Marengo 4, Jessica Brandi 5, Daniela Cecconi 5, Antonio Mori 1, Maria Mihaela Mina 2, Franco Antoniazzi 3, Monica Mottes 1 , Natascia Tiso 6 , Giovanni Malerba 1, Donato Zipeto 1 and Maria Teresa Valenti 2,* 1 Department of Neurosciences, Biomedicine and Movement Sciences, University of Verona, I-37134 Verona, Italy; [email protected] (M.D.); [email protected] (M.S.); [email protected] (S.C.); [email protected] (F.P.); [email protected] (A.M.); [email protected] (M.M.); [email protected] (G.M.); [email protected] (D.Z.) 2 Department of Medicine, University of Verona, I-37134 Verona, Italy; [email protected] (L.D.C.); [email protected] (G.M.); [email protected] (M.M.M.) 3 Department of Surgery, Dentistry, Pediatrics and Gynecology, University of Verona, I-37134 Verona, Italy; [email protected] (A.G.); [email protected] (G.I.); [email protected] (F.A.) 4 Department of Sciences and Technological Innovation, University of Piemonte Orientale, I-15121 Alessandria, Italy; [email protected] (M.M.); [email protected] (E.M.) 5 Proteomics and Mass Spectrometry Laboratory, Department of Biotechnology, University of Verona, I-37134 Verona, Italy; [email protected] (J.B.); [email protected] (D.C.) 6 Department of Biology, University of Padova, I-35131 Padova, Italy; [email protected] * Correspondence: [email protected]; Tel.: +39-045-8128450 Received: 5 October 2018; Accepted: 16 November 2018; Published: 20 November 2018 Abstract: The mortality rate for malignant melanoma (MM) is very high, since it is highly invasive and resistant to chemotherapeutic treatments. -
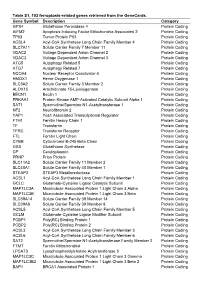
Table S1. 103 Ferroptosis-Related Genes Retrieved from the Genecards
Table S1. 103 ferroptosis-related genes retrieved from the GeneCards. Gene Symbol Description Category GPX4 Glutathione Peroxidase 4 Protein Coding AIFM2 Apoptosis Inducing Factor Mitochondria Associated 2 Protein Coding TP53 Tumor Protein P53 Protein Coding ACSL4 Acyl-CoA Synthetase Long Chain Family Member 4 Protein Coding SLC7A11 Solute Carrier Family 7 Member 11 Protein Coding VDAC2 Voltage Dependent Anion Channel 2 Protein Coding VDAC3 Voltage Dependent Anion Channel 3 Protein Coding ATG5 Autophagy Related 5 Protein Coding ATG7 Autophagy Related 7 Protein Coding NCOA4 Nuclear Receptor Coactivator 4 Protein Coding HMOX1 Heme Oxygenase 1 Protein Coding SLC3A2 Solute Carrier Family 3 Member 2 Protein Coding ALOX15 Arachidonate 15-Lipoxygenase Protein Coding BECN1 Beclin 1 Protein Coding PRKAA1 Protein Kinase AMP-Activated Catalytic Subunit Alpha 1 Protein Coding SAT1 Spermidine/Spermine N1-Acetyltransferase 1 Protein Coding NF2 Neurofibromin 2 Protein Coding YAP1 Yes1 Associated Transcriptional Regulator Protein Coding FTH1 Ferritin Heavy Chain 1 Protein Coding TF Transferrin Protein Coding TFRC Transferrin Receptor Protein Coding FTL Ferritin Light Chain Protein Coding CYBB Cytochrome B-245 Beta Chain Protein Coding GSS Glutathione Synthetase Protein Coding CP Ceruloplasmin Protein Coding PRNP Prion Protein Protein Coding SLC11A2 Solute Carrier Family 11 Member 2 Protein Coding SLC40A1 Solute Carrier Family 40 Member 1 Protein Coding STEAP3 STEAP3 Metalloreductase Protein Coding ACSL1 Acyl-CoA Synthetase Long Chain Family Member 1 Protein -

A Second Hybrid-Binding Domain Modulates the Activity of Drosophila Ribonuclease H1
bioRxiv preprint doi: https://doi.org/10.1101/2020.03.26.010645; this version posted March 28, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY 4.0 International license. A second hybrid-binding domain modulates the activity of Drosophila ribonuclease H1 Jose M. González de Cózar1, Maria Carretero-Junquera1,*, Grzegorz L. Ciesielski1,2, Sini M. Miettinen3, Markku Varjosalo3, Laurie S. Kaguni1,4, Eric Dufour1 & Howard T. Jacobs1,§ 1Faculty of Medicine and Health Technology, FI-33014 Tampere University, Finland 2Department of Chemistry, Auburn University at Montgomery, Montgomery, AL 36117, USA 3Institute of Biotechnology, FI-00014 University of Helsinki, Finland 4Department of Biochemistry and Molecular Biology, Michigan State University, East Lansing, MI 48824, USA *Present address: Department of Cellular and Molecular Medicine, University of Copenhagen, 1165 København, Denmark §Corresponding author: Howard T. Jacobs E-mail: [email protected] Running title: Drosophila RNase H1 Keywords: ribonuclease H, heteroduplex, single-stranded DNA-binding protein, mitochondria, shotgun proteomics, biolayer interferometry, EMSA 1 bioRxiv preprint doi: https://doi.org/10.1101/2020.03.26.010645; this version posted March 28, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY 4.0 International license. ABSTRACT In eukaryotes, ribonuclease H1 (RNase H1) is involved in the processing and removal of RNA/DNA hybrids in both nuclear and mitochondrial DNA. -

View of Untreated Versus DT Treated Glomeruli at 5 Days
BASIC RESEARCH www.jasn.org Proximal Tubules Have the Capacity to Regulate Uptake of Albumin † Mark C. Wagner,* Silvia B. Campos-Bilderback,* Mahboob Chowdhury, Brittany Flores,* ‡ Xianyin Lai, Jered Myslinski,* Sweekar Pandit,* Ruben M. Sandoval,* Sarah E. Wean,* † | Yuan Wei,§ Lisa M. Satlin,§ Roger C. Wiggins, Frank A. Witzmann, and | Bruce A. Molitoris* *Indiana University School of Medicine, The Roudebush Veterans Affair Medical Center, Indiana Center for Biological Microscopy, Indianapolis, Indiana; §Department of Pediatrics, The Icahn School of Medicine at Mount Sinai, New York; †Department of Internal Medicine, University of Michigan, Ann Arbor, Michigan; ‡Department of Biochemistry and Molecular Biology, Indiana University School of Medicine, Indianapolis, Indiana; and |Department of Cellular and Integrative Physiology, Indiana University School of Medicine, Indianapolis, Indiana ABSTRACT Evidence from multiple studies supports the concept that both glomerular filtration and proximal tubule (PT) reclamation affect urinary albumin excretion rate. To better understand these roles of glomerular filtration and PT uptake, we investigated these processes in two distinct animal models. In a rat model of acute exogenous albumin overload, we quantified glomerular sieving coefficients (GSC) and PT uptake of Texas Red-labeled rat serum albumin using two-photon intravital microscopy. No change in GSC was observed, but a significant decrease in PT albumin uptake was quantified. In a second model, loss of endogenous albumin was induced in rats by podocyte-specific transgenic expression of diphtheria toxin receptor. In these albumin-deficient rats, exposure to diphtheria toxin induced an increase in albumin GSC and albumin filtration, resulting in increased exposure of the PTs to endogenous albumin. In this case, PT albumin reabsorption was markedly increased.