Joubert Syndrome and Related Disorders
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

A 10-Year-Old Girl with Joubert Syndrome and Chronic Kidney Disease and Its Related Complications
4226 Letter to the Editor A 10-year-old girl with Joubert syndrome and chronic kidney disease and its related complications Chong Tian1#, Jiaxiang Chen1,2#, Xing Ming1, Xianchun Zeng1, Rongpin Wang1 1Department of Medical Imaging, Guizhou Provincial People’s Hospital, Guiyang, China; 2Guizhou University School of Medicine, Guiyang, China #These authors contributed equally to this work. Correspondence to: Rongpin Wang. Department of Medical Imaging, Guizhou Provincial People’s Hospital, Zhongshan East Road 83, Guiyang 550002, China. Email: [email protected]. Submitted Aug 05, 2020. Accepted for publication Apr 01, 2021. doi: 10.21037/qims-20-943 View this article at: http://dx.doi.org/10.21037/qims-20-943 Introduction and ankles was tolerated without redness, swelling, fistula, or sinus tract surrounding the skin. She had been healthy in Joubert syndrome (JS) is a rare genetic disorder of recessive the past, and her academic performance was moderate. She neurodevelopmental disorder characterized by distinctive was a picky eater and had a mild short stature but showed cerebellar vermis and mid-hindbrain hypoplasia/dysplasia no other development dysplasia. Nystagmus, oculomotor called the “molar tooth sign” (MTS) (1). Patients present apraxia, hypotonia, and abnormal breathing patterns were with symptoms characteristic of hypotonia in infancy not observed. Concerning the patient’s family history, her and later develop ataxia, ocular motor apraxia, and may mother and father appeared normal, but their first child died also present with developmental delays or intellectual retardation. Defined by the central nervous system features, of renal failure at the age of 4, their second-born twin sons JS also affects many other organs, such as the kidneys, liver, died in the perinatal period (causes unknown), and a third and bones. -

Molar Tooth Sign of the Midbrain-Hindbrain Junction
American Journal of Medical Genetics 125A:125–134 (2004) Molar Tooth Sign of the Midbrain–Hindbrain Junction: Occurrence in Multiple Distinct Syndromes Joseph G. Gleeson,1* Lesley C. Keeler,1 Melissa A. Parisi,2 Sarah E. Marsh,1 Phillip F. Chance,2 Ian A. Glass,2 John M. Graham Jr,3 Bernard L. Maria,4 A. James Barkovich,5 and William B. Dobyns6** 1Division of Pediatric Neurology, Department of Neurosciences, University of California, San Diego, California 2Division of Genetics and Development, Children’s Hospital and Regional Medical Center, University of Washington, Washington 3Medical Genetics Birth Defects Center, Ahmanson Department of Pediatrics, Cedars-Sinai Medical Center, UCLA School of Medicine, Los Angeles, California 4Department of Child Health, University of Missouri, Missouri 5Departments of Radiology, Pediatrics, Neurology, Neurosurgery, University of California, San Francisco, California 6Department of Human Genetics, University of Chicago, Illinois The Molar Tooth Sign (MTS) is defined by patients with these variants of the MTS will an abnormally deep interpeduncular fossa; be essential for localization and identifica- elongated, thick, and mal-oriented superior tion of mutant genes. ß 2003 Wiley-Liss, Inc. cerebellar peduncles; and absent or hypo- plastic cerebellar vermis that together give KEY WORDS: Joubert; molar tooth; Va´ r- the appearance of a ‘‘molar tooth’’ on axial adi–Papp; OFD-VI; COACH; brain MRI through the junction of the mid- Senior–Lo¨ ken; Dekaban– brain and hindbrain (isthmus region). It was Arima; cerebellar vermis; first described in Joubert syndrome (JS) hypotonia; ataxia; oculomo- where it is present in the vast majority of tor apraxia; kidney cysts; patients with this diagnosis. -

American Board of Psychiatry and Neurology, Inc
AMERICAN BOARD OF PSYCHIATRY AND NEUROLOGY, INC. CERTIFICATION EXAMINATION IN NEUROLOGY 2015 Content Blueprint (January 13, 2015) Part A Basic neuroscience Number of questions: 120 01. Neuroanatomy 3-5% 02. Neuropathology 3-5% 03. Neurochemistry 2-4% 04. Neurophysiology 5-7% 05. Neuroimmunology/neuroinfectious disease 2-4% 06. Neurogenetics/molecular neurology, neuroepidemiology 2-4% 07. Neuroendocrinology 1-2% 08. Neuropharmacology 4-6% Part B Behavioral neurology, cognition, and psychiatry Number of questions: 80 01. Development through the life cycle 3-5% 02. Psychiatric and psychological principles 1-3% 03. Diagnostic procedures 1-3% 04. Clinical and therapeutic aspects of psychiatric disorders 5-7% 05. Clinical and therapeutic aspects of behavioral neurology 5-7% Part C Clinical neurology (adult and child) The clinical neurology section of the Neurology Certification Examination is comprised of 60% adult neurology questions and 40% child neurology questions. Number of questions: 200 01. Headache disorders 1-3% 02. Pain disorders 1-3% 03. Epilepsy and episodic disorders 1-3% 04. Sleep disorders 1-3% 05. Genetic disorders 1-3% 2015 ABPN Content Specifications Page 1 of 22 Posted: Certification in Neurology AMERICAN BOARD OF PSYCHIATRY AND NEUROLOGY, INC. 06. Congenital disorders 1-3% 07. Cerebrovascular disease 1-3% 08. Neuromuscular diseases 2-4% 09. Cranial nerve palsies 1-3% 10. Spinal cord diseases 1-3% 11. Movement disorders 1-3% 12. Demyelinating diseases 1-3% 13. Neuroinfectious diseases 1-3% 14. Critical care 1-3% 15. Trauma 1-3% 16. Neuro-ophthalmology 1-3% 17. Neuro-otology 1-3% 18. Neurologic complications of systemic diseases 2-4% 19. -

Joubert Syndrome Genereview
Title: Joubert Syndrome GeneReview — Molecular Genetics: Less Common Genetic Causes Authors: Parisi M, Glass I Updated: June 2017 Note: The following information is provided by the authors listed above and has not been reviewed by GeneReviews staff. Joubert Syndrome: Less Common Genetic Causes ARL13B B9D1 B9D2 CEP41 IFT172 KIF7 OFD1 (CXORF5) PDE6D POC1B TCTN1 TCTN3 TMEM138 TMEM231 TMEM237 (ALS2CR4) TTC21B ARL13B Gene structure. ARL13B is a ten-exon gene that encodes a 428-amino acid protein. Pathogenic variants. Two families with a phenotype typical of classic Joubert syndrome had missense and/or nonsense variants in this gene; one of these individuals also had evidence of a retinopathy [Cantagrel et al 2008]. Normal gene product. ARL13B encodes ADP-ribosylation factor-like protein 13B, a member of the ADP-ribosylation factor-like family. Multiple transcript variants result from alternate splicing; two protein isoforms are known. The AR13B protein is a small GTPase in the Ras superfamily that contains both N-terminal and C-terminal guanine nucleotide-binding motifs. It is localized to the cilia and plays a role in cilia formation and maintenance as well as sonic hedgehog signaling. Abnormal gene product. In C elegans, pathogenic variants in the homolog arl13 exhibit defective cilium morphology, localization, and anterograde intraflagellar transport [Cevik et al 2010]. Mice with defects in the murine ortholog have neural tube defects and polydactyly, as well as an embryonic-lethal phenotype [Cantagrel et al 2008, Doherty 2009]. B9D1. See Tables A and B. B9D2. See Tables A and B. CEP41 Gene structure. The gene consists of 11 exons and spans approximately 50 kb. -

Renal Cystic Disorders Infosheet 6-14-19
Next Generation Sequencing Panel for Renal Cystic Disorders Clinical Features: Renal cystic diseases are a genetically heterogeneous group of conditions characterized By isolated renal disease or renal cysts in conjunction with extrarenal features (1). Age of onset of renal cystic disease ranges from neonatal to adult onset. Common features of renal cystic diseases include renal insufficiency and progression to end stage renal disease (ESRD). Identification of the genetic etiology of renal cystic disease can aid in appropriate clinical management of the affected patient. Our Renal Cystic Disorders Panel includes sequence and deletion/duplicaton analysis of all 79 genes listed below. Renal Cystic Disorders Sequencing Panel AHI1 BMPER HNF1B NEK8 TCTN3 WDPCP ANKS6 C5orf42 IFT27 NOTCH2 TFAP2A WDR19 ARL13B CC2D2A IFT140 NPHP1 TMEM107 XPNPEP3 ARL6 CDC73 IFT172 NPHP3 TMEM138 ZNF423 B9D1 CEP104 INPP5E NPHP4 TMEM216 B9D2 CEP120 INVS OFD1 TMEM231 BBIP1 CEP164 IQCB1 PDE6D TMEM237 BBS1 CEP290 JAG1 PKD2 TMEM67 BBS10 CEP41 KIAA0556 PKHD1 TRIM32 BBS12 CEP83 KIAA0586 REN TSC1 BBS2 CRB2 KIF14 RPGRIP1L TSC2 BBS4 CSPP1 KIF7 SALL1 TTC21B BBS5 DCDC2 LZTFL1 SDCCAG8 TTC8 BBS7 GLIS2 MKKS TCTN1 UMOD BBS9 GLIS3 MKS1 TCTN2 VHL Disorder Genes Inheritance Clinical features/molecular genetics Bardet Biedl ARL6 AR Bardet-Biedl syndrome (BBS) is an autosomal syndrome BBS1 recessive multi-systemic ciliopathy characterized By BBS10 retinal dystrophy, oBesity, postaxial polydactyly, BBS12 leaning difficulties, renal involvement and BBS2 genitourinary abnormalities (2). Visual prognosis is BBS4 poor, and the mean age of legal Blindness is 15.5 BBS5 years. Birth weight is typically normal But significant BBS7 weight gain Begins within the first year. Renal BBS9 disease is a major cause of morBidity and mortality. -

Autism Spectrum Disorders—A Genetics Review Judith H
GENETEST REVIEW Genetics in Medicine Autism spectrum disorders—A genetics review Judith H. Miles, MD, PhD TABLE OF CONTENTS Prevalence .........................................................................................................279 Adenylosuccinate lyase deficiency ............................................................285 Clinical features................................................................................................279 Creatine deficiency syndromes..................................................................285 Core autism symptoms...................................................................................279 Smith-Lemli-Opitz syndrome.....................................................................285 Diagnostic criteria and tools..........................................................................280 Other single-gene disorders.......................................................................285 Neurologic and medical symptoms .............................................................281 Developmental syndromes of undetermined etiology..............................286 Genetics of autism...........................................................................................281 Moebius syndrome or sequence...............................................................286 Chromosomal disorders and CNVS..............................................................282 Landau-Kleffner syndrome .........................................................................286 Single-gene -
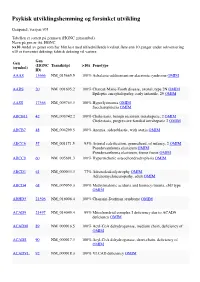

Psykisk Utviklingshemming Og Forsinket Utvikling
Psykisk utviklingshemming og forsinket utvikling Genpanel, versjon v03 Tabellen er sortert på gennavn (HGNC gensymbol) Navn på gen er iht. HGNC >x10 Andel av genet som har blitt lest med tilfredstillende kvalitet flere enn 10 ganger under sekvensering x10 er forventet dekning; faktisk dekning vil variere. Gen Gen (HGNC Transkript >10x Fenotype (symbol) ID) AAAS 13666 NM_015665.5 100% Achalasia-addisonianism-alacrimia syndrome OMIM AARS 20 NM_001605.2 100% Charcot-Marie-Tooth disease, axonal, type 2N OMIM Epileptic encephalopathy, early infantile, 29 OMIM AASS 17366 NM_005763.3 100% Hyperlysinemia OMIM Saccharopinuria OMIM ABCB11 42 NM_003742.2 100% Cholestasis, benign recurrent intrahepatic, 2 OMIM Cholestasis, progressive familial intrahepatic 2 OMIM ABCB7 48 NM_004299.5 100% Anemia, sideroblastic, with ataxia OMIM ABCC6 57 NM_001171.5 93% Arterial calcification, generalized, of infancy, 2 OMIM Pseudoxanthoma elasticum OMIM Pseudoxanthoma elasticum, forme fruste OMIM ABCC9 60 NM_005691.3 100% Hypertrichotic osteochondrodysplasia OMIM ABCD1 61 NM_000033.3 77% Adrenoleukodystrophy OMIM Adrenomyeloneuropathy, adult OMIM ABCD4 68 NM_005050.3 100% Methylmalonic aciduria and homocystinuria, cblJ type OMIM ABHD5 21396 NM_016006.4 100% Chanarin-Dorfman syndrome OMIM ACAD9 21497 NM_014049.4 99% Mitochondrial complex I deficiency due to ACAD9 deficiency OMIM ACADM 89 NM_000016.5 100% Acyl-CoA dehydrogenase, medium chain, deficiency of OMIM ACADS 90 NM_000017.3 100% Acyl-CoA dehydrogenase, short-chain, deficiency of OMIM ACADVL 92 NM_000018.3 100% VLCAD -

Molar Tooth Sign with Deranged Liver Function Tests: an Indian Case with COACH Syndrome
Hindawi Publishing Corporation Case Reports in Pediatrics Volume 2015, Article ID 385910, 3 pages http://dx.doi.org/10.1155/2015/385910 Case Report Molar Tooth Sign with Deranged Liver Function Tests: An Indian Case with COACH Syndrome Rama Krishna Sanjeev,1 Seema Kapoor,2 Manisha Goyal,3 Rajiv Kapur,4 and Joseph Gerard Gleeson5,6,7 1 Department of Pediatrics, ACMS, India 2DivisionofGenetics,LokNayak&MaulanaAzadMedicalCollege,NewDelhi,India 3Department of Paediatrics, Maulana Azad Medical College, New Delhi, India 4Department of Radiology, ACMS, New Delhi, India 5Neurogenetics Laboratory, Department of Neurosciences and Paediatrics, USA 6Rady Children’s Hospital, USA 7Howard Hughes Medical Institute, CA, USA Correspondence should be addressed to Rama Krishna Sanjeev; [email protected] Received 18 October 2014; Revised 18 March 2015; Accepted 30 March 2015 Academic Editor: Ozgur Cogulu Copyright © 2015 Rama Krishna Sanjeev et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. We report the first genetically proven case of COACH syndrome from the Indian subcontinent in a 6-year-old girl who presented with typical features of Joubert syndrome along with hepatic involvement. Mutation analysis revealed compound heterozygous missense mutation in the known gene TMEM67 (also called MKS3). 1. Introduction born to nonconsanguineous couple at term after LSCS with birth weight of 3.5 kg. Her motor developmental milestones COACH syndrome (cerebellar vermis hypo/aplasia, oligo- and speech were grossly delayed. phrenia, congenital ataxia, coloboma, and hepatic fibrosis; On examination, her weight was 18.2 kg (50th centile), OMIM# 216360) is a rare autosomal recessive multisystemic height 107 cm (50th centile), and head circumference 53 cm disorder first proposed by Verloes and Lambotte [1]. -
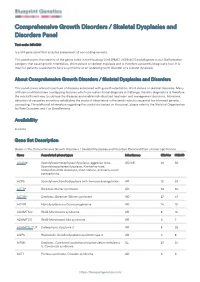
Blueprint Genetics Comprehensive Growth Disorders / Skeletal
Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders Panel Test code: MA4301 Is a 374 gene panel that includes assessment of non-coding variants. This panel covers the majority of the genes listed in the Nosology 2015 (PMID: 26394607) and all genes in our Malformation category that cause growth retardation, short stature or skeletal dysplasia and is therefore a powerful diagnostic tool. It is ideal for patients suspected to have a syndromic or an isolated growth disorder or a skeletal dysplasia. About Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders This panel covers a broad spectrum of diseases associated with growth retardation, short stature or skeletal dysplasia. Many of these conditions have overlapping features which can make clinical diagnosis a challenge. Genetic diagnostics is therefore the most efficient way to subtype the diseases and enable individualized treatment and management decisions. Moreover, detection of causative mutations establishes the mode of inheritance in the family which is essential for informed genetic counseling. For additional information regarding the conditions tested on this panel, please refer to the National Organization for Rare Disorders and / or GeneReviews. Availability 4 weeks Gene Set Description Genes in the Comprehensive Growth Disorders / Skeletal Dysplasias and Disorders Panel and their clinical significance Gene Associated phenotypes Inheritance ClinVar HGMD ACAN# Spondyloepimetaphyseal dysplasia, aggrecan type, AD/AR 20 56 Spondyloepiphyseal dysplasia, Kimberley -

Clinical Utility Gene Card For: Joubert Syndrome - Update 2013
European Journal of Human Genetics (2013) 21, doi:10.1038/ejhg.2013.10 & 2013 Macmillan Publishers Limited All rights reserved 1018-4813/13 www.nature.com/ejhg CLINICAL UTILITY GENE CARD UPDATE Clinical utility gene card for: Joubert syndrome - update 2013 Enza Maria Valente*,1,2, Francesco Brancati1, Eugen Boltshauser3 and Bruno Dallapiccola4 European Journal of Human Genetics (2013) 21, doi:10.1038/ejhg.2013.10; published online 13 February 2013 Update to: European Journal of Human Genetics (2011) 19, doi:10.1038/ejhg.2011.49; published online 30 March 2011 1. DISEASE CHARACTERISTICS 1.6 Analytical methods 1.1 Name of the disease (synonyms) Direct sequencing of coding genomic regions and splice site junctions; Joubert syndrome (JS); Joubert-Boltshauser syndrome; Joubert syn- multiplex microsatellite analysis for detection of NPHP1 homozygous drome-related disorders (JSRD), including cerebellar vermis hypo/ deletion. Possibly, qPCR or targeted array-CGH for detection of aplasia, oligophrenia, congenital ataxia, ocular coloboma, and hepatic genomic rearrangements in other genes. fibrosis (COACH) syndrome; cerebellooculorenal, or cerebello-oculo- renal (COR) syndrome; Dekaban-Arima syndrome; Va´radi-Papp 1.7 Analytical validation syndrome or Orofaciodigital type VI (OFDVI) syndrome; Malta Direct sequencing of both DNA strands; verification of sequence and syndrome. qPCR results in an independent experiment. 1.2 OMIM# of the disease 1.8 Estimated frequency of the disease 213300, 243910, 216360, 277170. (incidence at birth-‘birth prevalence’-or population prevalence) No good population-based data on JSRD prevalence have been published. A likely underestimated frequency between 1/80 000 and 1.3 Name of the analysed genes or DNA/chromosome segments 1/100 000 live births is based on unpublished data. -

Blueprint Genetics Comprehensive Skeletal Dysplasias and Disorders
Comprehensive Skeletal Dysplasias and Disorders Panel Test code: MA3301 Is a 251 gene panel that includes assessment of non-coding variants. Is ideal for patients with a clinical suspicion of disorders involving the skeletal system. About Comprehensive Skeletal Dysplasias and Disorders This panel covers a broad spectrum of skeletal disorders including common and rare skeletal dysplasias (eg. achondroplasia, COL2A1 related dysplasias, diastrophic dysplasia, various types of spondylo-metaphyseal dysplasias), various ciliopathies with skeletal involvement (eg. short rib-polydactylies, asphyxiating thoracic dysplasia dysplasias and Ellis-van Creveld syndrome), various subtypes of osteogenesis imperfecta, campomelic dysplasia, slender bone dysplasias, dysplasias with multiple joint dislocations, chondrodysplasia punctata group of disorders, neonatal osteosclerotic dysplasias, osteopetrosis and related disorders, abnormal mineralization group of disorders (eg hypopohosphatasia), osteolysis group of disorders, disorders with disorganized development of skeletal components, overgrowth syndromes with skeletal involvement, craniosynostosis syndromes, dysostoses with predominant craniofacial involvement, dysostoses with predominant vertebral involvement, patellar dysostoses, brachydactylies, some disorders with limb hypoplasia-reduction defects, ectrodactyly with and without other manifestations, polydactyly-syndactyly-triphalangism group of disorders, and disorders with defects in joint formation and synostoses. Availability 4 weeks Gene Set Description -

Irish Rare Kidney Disease Network (IRKDN)
Irish Rare kidney Disease Network (IRKDN) Others Cork University Mater, Waterford University Dr Liam Plant Hospital Galway Dr Abernathy University Hospital Renal imaging Dr M Morrin Prof Griffin Temple St and Crumlin Beaumont Hospital CHILDRENS Hospital Tallaght St Vincents Dr Atiff Awann Rare Kidney Disease Clinic Hospital University Hospital Prof Peter Conlon Dr Lavin Prof Dr Holian Little Renal pathology Lab Limerick University Dr Dorman and Hospital Dr Doyle Dr Casserly Patient Renal Council Genetics St James Laboratory Hospital RCSI Dr Griffin Prof Cavaller MISION Provision of care to patients with Rare Kidney Disease based on best available medical evidence through collaboration within Ireland and Europe Making available clinical trials for rare kidney disease to Irish patients where available Collaboration with other centres in Europe treating rare kidney disease Education of Irish nephrologists on rare Kidney Disease. Ensuring a seamless transition of children from children’s hospital with rare kidney disease to adult centres with sharing of knowledge of rare paediatric kidney disease with adult centres The provision of precise molecular diagnosis of patients with rare kidney disease The provision of therapeutic plan based on understanding of molecular diagnosis where available Development of rare disease specific registries within national renal It platform ( Emed) Structure Beaumont Hospital will act as National rare Kidney Disease Coordinating centre working in conjunction with a network of Renal unit across the country