Second Malignancies Secondary Myelodysplastic Syndrome
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Primary Cutaneous Anaplastic Large Cell Lymphoma / Lymphomatoid
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual patients Clonally related Overlapping clinical and/or histological features Clinical, histologic, and phenotypic characteristics required for diagnosis Types 1. Primary cutaneous anaplastic large cell lymphoma (C-ALCL) 2. Lymphomatoid papulosis 3. Borderline lesions C-ALCL: Definition T-cell lymphoma, presenting in the skin and consisting of anaplastic lymphoid cells, the majority of which are CD30- positive Distinction from: (a) systemic ALCL with cutaneous involvement, and (b) secondary high-grade lymphomas with CD30 expression In nearly all patients disease is limited to the skin at the time of diagnosis Assessed by meticulous staging Patients should not have other subtypes of lymphoma C-ALCL: Synonyms Lukes-Collins: Not listed (T-immunoblastic) Kiel: Anaplastic large cell Working Formulation: Various categories (diffuse large cell; immunoblastic) REAL: Primary cutaneous anaplastic large cell (CD30+) lymphoma Related terms: Regressing atypical histiocytosis; Ki-1 lymphoma C-ALCL: Epidemiology 25% of the T-cell lymphomas arising primarily in the skin. Predominantly in adults/elderly and rare in children. The male to female ratio is 1.5-2.0:1. C-ALCL: Sites of Involvement The disease is nearly always limited to the skin at the time of diagnosis Extracutaneous dissemination may occur Mainly regional lymph nodes Involvement of other organs is rare C-ALCL: Clinical Features Most present solitary or localized skin lesions which may be tumors, nodules or (more rarely) papules Multicentric cutaneous disease occurs in 20% Lesions may show partial or complete spontaneous regression (similar to lymphomatoid papulosis) Cutaneous relapses are frequent Extracutaneous dissemination occurs in approximately 10% of the patients. -

Hematopoietic and Lymphoid Neoplasm Coding Manual
Hematopoietic and Lymphoid Neoplasm Coding Manual Effective with Cases Diagnosed 1/1/2010 and Forward Published August 2021 Editors: Jennifer Ruhl, MSHCA, RHIT, CCS, CTR, NCI SEER Margaret (Peggy) Adamo, BS, AAS, RHIT, CTR, NCI SEER Lois Dickie, CTR, NCI SEER Serban Negoita, MD, PhD, CTR, NCI SEER Suggested citation: Ruhl J, Adamo M, Dickie L., Negoita, S. (August 2021). Hematopoietic and Lymphoid Neoplasm Coding Manual. National Cancer Institute, Bethesda, MD, 2021. Hematopoietic and Lymphoid Neoplasm Coding Manual 1 In Appreciation NCI SEER gratefully acknowledges the dedicated work of Drs, Charles Platz and Graca Dores since the inception of the Hematopoietic project. They continue to provide support. We deeply appreciate their willingness to serve as advisors for the rules within this manual. The quality of this Hematopoietic project is directly related to their commitment. NCI SEER would also like to acknowledge the following individuals who provided input on the manual and/or the database. Their contributions are greatly appreciated. • Carolyn Callaghan, CTR (SEER Seattle Registry) • Tiffany Janes, CTR (SEER Seattle Registry) We would also like to give a special thanks to the following individuals at Information Management Services, Inc. (IMS) who provide us with document support and web development. • Suzanne Adams, BS, CTR • Ginger Carter, BA • Sean Brennan, BS • Paul Stephenson, BS • Jacob Tomlinson, BS Hematopoietic and Lymphoid Neoplasm Coding Manual 2 Dedication The Hematopoietic and Lymphoid Neoplasm Coding Manual (Heme manual) and the companion Hematopoietic and Lymphoid Neoplasm Database (Heme DB) are dedicated to the hard-working cancer registrars across the world who meticulously identify, abstract, and code cancer data. -

(Rituxan®), Rituximab-Abbs (Truxima®), Rituximab-Pvvr (Ruxience®) Prior Authorization Drug Coverage Policy
1 Rituximab Products: Rituximab (Rituxan®), Rituximab-abbs (Truxima®), Rituximab-pvvr (Ruxience®) Prior Authorization Drug Coverage Policy Effective Date: 2/1/2021 Revision Date: n/a Review Date: 7/2/20 Lines of Business: Commercial Policy type: Prior Authorization This Drug Coverage Policy provides parameters for the coverage of rituximab (Rituxan®), rituximab-abbs (Truxima®), and rituximab-pvvr (Ruxience®). Consideration of medically necessary indications are based upon U.S. Food and Drug Administration (FDA) indications, recommended uses within the Centers of Medicare & Medicaid Services (CMS) five recognized compendia, including the National Comprehensive Cancer Network (NCCN) Drugs & Biologics Compendium (Category 1 or 2A recommendations), and peer-reviewed scientific literature eligible for coverage according to the CMS, Medicare Benefit Policy Manual, Chapter 15, section 50.4.5 titled, “Off- Label Use of Anti-Cancer Drugs and Biologics.” This policy evaluates whether the drug therapy is proven to be effective based on published evidence-based medicine. Drug Description1-3 Rituximab (Rituxan®), rituximab-abbs (Truxima®), and rituximab-pvvr (Ruxience®) are monoclonal antibodies that target the CD20 antigen expressed on the surface of pre-B and mature B- lymphocytes. Upon binding to cluster of differentiation (CD) 20, rituximab mediates B-cell lysis. Possible mechanisms of cell lysis include complement dependent cytotoxicity (CDC) and antibody dependent cell mediated cytotoxicity (ADCC). B cells are believed to play a role in the pathogenesis of rheumatoid arthritis (RA) and associated chronic synovitis. In this setting, B cells may be acting at multiple sites in the autoimmune/inflammatory process, including through production of rheumatoid factor (RF) and other autoantibodies, antigen presentation, T-cell activation, and/or proinflammatory cytokine production. -

Indolent Non-Hodgkin's Lymphomas
Follicular and Low-Grade Non-Hodgkin Lymphomas (Indolent Lymphomas) Stefan K Barta, M.D., M.S. Associate Professor of Medicine Leader, T Cell Lymphoma Program Perelman Center for Advanced Medicine Facts and Figures: Non-Hodgkin Lymphomas • Most common blood cancer • 7th most common cancer in the US3 • 71,850 new cases in the US in 20151 • 19,790 died of NHL in 20151 • About 549,625 people are living with a history of NHL (2012)1 • 85% of all NHLs are B-cell lymphomas2 • Follicular lymphoma = 2nd most common type, ~25% of all NHLs4 1 http://seer.cancer.gov/statfacts/html/nhl.html. 2 ACS. Detailed Guide (revised January 21, 2000): Non-Hodgkin’s Lymphoma. 3 http://www.cancer.gov/cancertopics/types/commoncancers 4 Blood 89: 3909, 1997 The Immune System T- CELLS B- CELLS Cellular immunity: Humoral immunity: helper + cytotoxic T-cells antibodies Lymphatic System Lymph Node Anatomy Lymph Node: Microscopic View germinal center Lymphocyte: Microscopic View Causes Possible cause(s): • chemical exposures (pesticides, fertilizers or solvents) • individuals with compromised immune systems • heredity • infections (e.g. H. pylori, Hep C, chlamydia trachomatis) • most patients have no clear risk factors • IN MOST CASES, THE EXACT CAUSE IS UNKNOWN Cellular Origins of Lymphomas & Leukemias PLEURIPOTENT STEM CELL ACUTE LEUKEMIAS LYMPHOID STEM CELL ACUTE LYMPHOBLASTIC LEUKEMIAS PRECURSOR T - CELL PRECURSOR B - CELL LYMPHOBLASTIC LYMPHOMAS / LEUKEMIAS MATURE T - CELL MATURE B - CELL NON-HODGKIN LYMPHOMAS / CHRONIC LYMPHOCYTIC LEUKEMIA LYMPH NODES, EXTRANODAL -
Localized AL Amyloidosis in a Patient with Diffuse Large B-Cell Lymphoma of the Breast
Included in the theme issue: 284 Letters to the Editor ACNE, RETINOIDS AND LYMPHOMAS Acta Derm Venereol 2012; 92: 284–285 Localized AL Amyloidosis in a Patient with Diffuse Large B-cell Lymphoma of the Breast Hsien-Yi Chiu, Chia-Yu Chu and Tsen-Fang Tsai* Department of Dermatology, National Taiwan University Hospital, 7 Chung-Shan South Road, Taipei 100, Taiwan. *E-mail: [email protected] Accepted July 11, 2011. Amyloidosis refers to a variety of conditions in which a protein polysaccharide complex, amyloid protein, is accumulated locally or systemically in tissues or organs. Amyloid in the skin may be derived directly from kerati- nocytes, or secondarily from immunoglobulin light chain fragments (AL type), fragments of the acute-phase reac- tant serum amyloid A (AA type), etc. Nodular amyloido- sis (NA) is a rare type of localized AL amyloidosis, with most reported cases being of the lambda light chains (1) and is often histopathologically indistinguishable from systemic amyloidosis. Its association with lymphoma has been observed infrequently. CASE REPORT An 88-year-old woman initially noticed a 5×3 cm mass in her right breast in 1990. She was diagnosed with non-Hodgkin’s lymphoma (NHL) (diffuse large immunoblastic B-cell type, sta- ge IE) after the excision of the mass in a tertiary referral centre. Bone marrow biopsy revealed no evidence of lymphoma invol- vement. She achieved complete remission after chemotherapy. Six years after the diagnosis of lymphoma she developed multiple enlarging nodules on her legs. On examination, there were coalescing, waxy, skin-coloured, nodules with some foci of haemorrhage, central ulceration and crusts on the legs (Fig. -

REVIEW Anti-CD20-Based Therapy of B Cell Lymphoma: State of The
Leukemia (2002) 16, 2004–2015 2002 Nature Publishing Group All rights reserved 0887-6924/02 $25.00 www.nature.com/leu REVIEW Anti-CD20-based therapy of B cell lymphoma: state of the art C Kosmas1, K Stamatopoulos2, N Stavroyianni2, N Tsavaris3 and T Papadaki4 1Department of Medicine, 2nd Division of Medical Oncology, ‘Metaxa’ Cancer Hospital, Piraeus, Greece; 2Department of Hematology, G Papanicolaou General Hospital, Thessaloniki, Greece; 3Oncology Unit, Department of Pathophysiology, Athens University School of Medicine, Laikon General Hospital, Athens, Greece; and 4Hemopathology Department, Evangelismos Hospital, Athens, Greece Over the last 5 years, studies applying the chimeric anti-CD20 ficulties in identifying a completely tumor-specific target; (2) MAb have renewed enthusiasm and triggered world-wide appli- the impracticality of constructing a unique antibody for each cation of anti-CD20 MAb-based therapies in B cell non-Hodg- kin’s lymphoma (NHL). Native chimeric anti-CD20 and isotope- patient; (3) the development of an immune response to murine 6 labeled murine anti-CD20 MAbs are currently employed with immunoglobulins (human anti-mouse antibodies, HAMA). By encouraging results as monotherapy or in combination with the end of the 1980s enthusiasm for therapeutic MAbs was conventional chemotherapy and in consolidation of remission waning; murine native (unconjugated), radioactively labeled after treatments with curative intent (ie after/ in combination or toxin-conjugated MAbs failed to yield significant clinical with high-dose chemotherapy and hematopoietic stem cell responses; moreover, they were not uncommonly associated rescue). On the available experience, anti-CD20 MAb-based therapeutic strategies will be increasingly integrated in the with toxicities, predominantly in the form of serum sickness treatment of B cell NHL and related malignancies. -

Delivering Novel Targeted Therapies to Cancer Patients
NEXT-GENERATION RADIOIMMUNOTHERAPIES FOR NON-HODGKIN’S LYMPHOMA PATIENTS SEPTEMBER 2019 Nordic Nanovector ASA Kjelsåsveien 168 B, 0884 Oslo, Norway www.nordicnanovector.com IR contact: [email protected] Forward-looking statements This slide presentation contains certain forward-looking statements. These statements are based on management's current expectations and are subject to uncertainty and changes in circumstances, since they relate to events and depend on circumstances that will occur in the future and which, by their nature, will have an impact on Nordic Nanovector's business, financial condition and results of operations. The terms "anticipates", "assumes", "believes", "can", "could", "estimates", "expects", "forecasts", "intends", "may", "might", "plans", "should", "projects", "targets", "will", "would" or, in each case, their negative, or other variations or comparable terminology are used to identify forward looking statements. These forward-looking statements are not historic facts. There are a number of factors that could cause actual results and developments to differ materially from those expressed or implied in the forward-looking statements. Factors that could cause these differences include, but are not limited to, risks associated with implementation of Nordic Nanovector's strategy, risks and uncertainties associated with the development and/or approval of Nordic Nanovector's product candidates, ongoing and future clinical trials and expected trial results, the ability to commercialise Betalutin®, technology changes and new products in Nordic Nanovector's potential market and industry, Nordic Nanovector's freedom to operate (competitors patents) in respect of the products it develops, the ability to develop new products and enhance existing products, the impact of competition, changes in general economy and industry conditions, and legislative, regulatory and political factors. -

Molecular and Immunological Dissection of Diffuse Large
Leukemia (1999) 13, 1441–1447 1999 Stockton Press All rights reserved 0887-6924/99 $15.00 http://www.stockton-press.co.uk/leu ,Molecular and immunological dissection of diffuse large B cell lymphoma: CD5؉ and CD5؊ with CD10؉ groups may constitute clinically relevant subtypes S Harada1,2, R Suzuki1, K Uehira3, Y Yatabe4, Y Kagami3, M Ogura3, H Suzuki5, A Oyama6, Y Kodera7, R Ueda2, Y Morishima3, S Nakamura4 and M Seto1 1Laboratory of Chemotherapy, Aichi Cancer Center Research Institute; 3Department of Hematology and Chemotherapy, 4Department of Pathology and Clinical Laboratories, Aichi Cancer Center Hospital; 2Second Department of Internal Medicine, Nagoya City University School of Medicine; 5Department of Internal Medicine, Okazaki Municipal Hospital; 6Department of Internal Medicine, Aichi Prefectural Hospital; 7Department of Internal Medicine, Japanese Red Cross, Nagoya First Hospital, Japan Diffuse large B cell lymphoma (DLBL) constitutes the greatest genotypic parameters were found not to be helpful for deline- percentage of adult non-Hodgkin’s lymphomas and represents ating distinctive morphologic subgroups). DLBL accounts for a diverse spectrum of lymphoid neoplasms. Clinicopathologic, the greatest percentage (48%) of adult non-Hodgkin’s lym- phenotypic and genotypic findings were correlated and com- 4 pared for 63 DLBL cases to investigate whether they represent phoma (NHL) among Japanese patients and for about 40% clinically relevant subtypes. They were all cyclin D1 negative of initial NHL diagnoses in the United States.5 Among DLBL, and were phenotypically divided into three groups, ie group I only a few entities, eg primary mediastinal large B cell lym- + − + (CD5 type, n = 11), group II (CD5 CD10 type, n = 19), and phoma characterized by the fact that it has a peculiar disease − − = group III (CD5 CD10 type, n 33). -

Unitedhealthcare Cancer Therapy Pathways Program Regimens
UnitedHealthcare Cancer Therapy Pathways Program Overview 2 Breast Cancer 3 Pancreatic Cancer 15 Melanoma 19 Colon/Rectal Cancer 23 Hepatobiliary Cancers 30 Lung Cancer, Small Cell 35 Lung Cancer, Non-Small Cell 40 Ovarian, Fallopian and Primary Peritoneal Cancer 56 Head and Neck Cancer 67 Multiple Myeloma 74 Lymphoma, Diffuse Large B-Cell 86 Lymphoma, Follicular 92 Lymphoma, Marginal Zone 97 Lymphoma, Mantle Cell 101 Change control 1 OVERVIEW Cancer Therapy Pathways Program With the rapid approval of new therapies, along with the rising cost of cancer care, pathways serve a critical role in the delivery of high-quality and high-value cancer treatments while reducing an unwarranted variation in care. The UnitedHealthcare Cancer Therapy Pathways Program aims to improve quality and value in cancer care by identifying anti-cancer regimens supported by evidence-based guidelines to help reduce total cost of care and improve outcomes. The program’s regimens are selected on the basis of clinical benefit (efficacy) and side-effect profile (toxicity). Among regimens with comparable efficacy and toxicity, additional consideration is given to the frequency of hospitalizations during therapy, duration of therapy, drug costs and total cost of care. Care decisions are between the physician and the patient The Cancer Therapy Pathways Program is not a substitute for the experience and judgment of a physician or other health care professional. Any clinician participating in the program must use independent medical judgment in the context of individual -

Pancreatic Cancer Treatment Using Na+/K+ Atpase
(19) & (11) EP 1 796 688 B1 (12) EUROPEAN PATENT SPECIFICATION (45) Date of publication and mention (51) Int Cl.: of the grant of the patent: A61K 31/704 (2006.01) A61P 35/00 (2006.01) 18.05.2011 Bulletin 2011/20 (86) International application number: (21) Application number: 05794315.1 PCT/US2005/031331 (22) Date of filing: 02.09.2005 (87) International publication number: WO 2006/028969 (16.03.2006 Gazette 2006/11) (54) PANCREATIC CANCER TREATMENT USING NA+/K+ ATPASE INHIBITORS PANKREASKREBSBEHANDLUNG MIT NA+/K+-ATPASE-HEMMERN TRAITEMENT DU CANCER DU PANCREAS AU MOYEN D’INHIBITEURS D’APTASE NA+/K+ (84) Designated Contracting States: • SHARMA, Ajay AT BE BG CH CY CZ DE DK EE ES FI FR GB GR Sudbury , MA 01776 (US) HU IE IS IT LI LT LU LV MC NL PL PT RO SE SI SK TR (74) Representative: Tomkinson, Alexandra et al Bailey Walsh & Co (30) Priority: 02.09.2004 US 606684 P 5 York Place Leeds LS1 2SD (GB) (43) Date of publication of application: 20.06.2007 Bulletin 2007/25 (56) References cited: WO-A-00/45165 WO-A-03/099011 (73) Proprietor: Bionaut Pharmaceuticals Inc WO-A-2005/060951 WO-A-2005/077925 Stoneham, MA 02180 (US) US-A1- 2005 182 105 (72) Inventors: • KHODADOUST, Mehran - c/o BT Intern. Ltd. London EC4M 7SB (GB) Note: Within nine months of the publication of the mention of the grant of the European patent in the European Patent Bulletin, any person may give notice to the European Patent Office of opposition to that patent, in accordance with the Implementing Regulations. -

V1 Madrid 3 Intro.Pdf
Clasificación de la OMS de las neoplasias linfoides is about to begin! Please silence your cellphones, beepers, person sitting next to you….. When Dr. Campo asked me to provide this introduction, I had to think long and hard before agreeing to prepare it for this course & deciding how to do it but….. he is a good friend so …… Clasificación de los linfomas. Evolución conceptual. Please do not be disappointed The remainder of this presentation is in American Style English However, this is an international story not from just one family tree nor one side of the Atlantic So let’s begin! S. Fairey Lymphoma classification over the last half- century: A tale of evolution & revolution The Rappaport classification 1966 1974 Lymphomas are neoplasms of the immune system and should be categorized as such! The “functional” lymphoma classifications Cells of the normal immune system Lukes & Collins, Cancer 34:1488, 1974 Morphology & immunophenotype R. D. Collins - Vanderbilt R. L. Lukes - USC 1974 K. Lennert Signing off on the Kiel classification The 1970’s were very exciting but tumultuous times – not everyone was on the same page! “It was the best of times, it was the worst of times, it was the age of wisdom, it was the age of foolishness….” The 1970’s were very exciting but tumultuous times – not everyone was on the same page! “It was the best of times, it was the worst of times, it was the age of wisdom, it was the age of foolishness….” Lancet 1974 7;2(7880): 586 Lancet 1974 7;2(7880): 586 NCI Working Formulation Cancer 49:2112, 1982 Morphologic classification based in large part on survival data from the late 1970s. -
Diffuse Large B-Cell Lymphoma (Part 1 of 5)
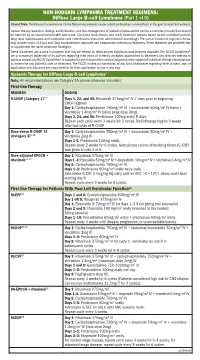
NON-HODGKIN LYMPHOMA TREATMENT REGIMENS: Diffuse Large B-cell Lymphoma (Part 1 of 5) Clinical Trials: The National Comprehensive Cancer Network recommends cancer patient participation in clinical trials as the gold standard for treatment. Cancer therapy selection, dosing, administration, and the management of related adverse events can be a complex process that should be handled by an experienced health care team. Clinicians must choose and verify treatment options based on the individual patient; drug dose modifications and supportive care interventions should be administered accordingly. The cancer treatment regimens below may include both U.S. Food and Drug Administration-approved and unapproved indications/regimens. These regimens are provided only to supplement the latest treatment strategies. These Guidelines are a work in progress that may be refined as often as new significant data become available. The NCCN Guidelines® are a consensus statement of its authors regarding their views of currently accepted approaches to treatment. Any clinician seeking to apply or consult any NCCN Guidelines® is expected to use independent medical judgment in the context of individual clinical circumstances to determine any patient’s care or treatment. The NCCN makes no warranties of any kind whatsoever regarding their content, use, or application and disclaims any responsibility for their application or use in any way. Systemic Therapy for Diffuse Large B-cell Lymphoma1 Note: All recommendations are Category 2A unless otherwise indicated. First-line Therapy REGIMEN DOSING R-CHOP (Category 1)2–7 Days 1, 22, and 43: Rituximab 375mg/m2 IV 7 days prior to beginning CHOP regimen Day 1: Cyclophosphamide 750mg/m2 IV + doxorubicin 50mg/m2 IV bolus + vincristine 1.4mg/m2 IV bolus (max dose 2mg) Days 3, 24, and 45: Prednisone 100mg orally 5 days.