Primary Cutaneous Anaplastic Large Cell Lymphoma / Lymphomatoid
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Lymphomatoid Papulosis and Recurrent Transitional Cell Carcinoma
Volume 20 Number 4 April 2014 Letter Lymphomatoid papulosis and recurrent transitional cell carcinoma of the bladder: a paraneoplastic association WMS Leong1, CWD Aw1, KB Tan2 Dermatology Online Journal 20 (4): 17 1Division of Dermatology, National University Hospital, Singapore 2Department of Pathology, National University Hospital, Singapore Correspondence: Wai Mun Sean Leong, M.B.B.S. University Medicine Cluster National University Hospital 5 Lower Kent Ridge Road Singapore 119074 Phone: 67795555 Email: [email protected] Abstract Lymphomatoid papulosis is a rare, papulonodular skin eruption with histologic features of a CD30+ T cell lymphoma. We present a 79-year-old man with lymphomatoid papulosis and transitional cell carcinoma of the bladder. Introduction Lymphomatoid papulosis (LyP) is a rare, recurrent, self-healing papulonodular skin eruption with histologic features of a CD30+ malignant T cell lymphoma [1]. It belongs to a group of cutaneous CD30+ lymphoproliferative disorders, which includes cutaneous T cell lymphoma [2]. Patients with LyP are at risk of developing a second cutaneous or nodal lymphoma [3,4]. However, an association with transitional cell carcinoma (TCC) of the bladder has not been reported in the literature. This case illustrates a possible association between these two conditions. Case synopsis A 79-year-old man complained of a slightly itchy rash on the arms, neck, and shoulders for one year. Betamethasone- gentamicin cream previously afforded partial improvement. Approximately 9 months prior to presentation at the dermatology clinic, he was diagnosed to have TCC of the bladder (T1G3) and had undergone a trans-urethral resection of bladder cancer (TURBT) in December 2006 and January 2007. -

Comorbidities in Mycosis Fungoides and Racial Differences In
medicines Article Comorbidities in Mycosis Fungoides and Racial Differences in Co-Existent Lymphomatoid Papulosis: A Cross-Sectional Study of 580 Patients in an Urban Tertiary Care Center Subuhi Kaul 1,*, Micah Belzberg 2, John-Douglas Matthew Hughes 3, Varun Mahadevan 2 , Raveena Khanna 2, Pegah R. Bakhshi 2, Michael S. Hong 2, Kyle A. Williams 2, 2 2, 2, Annie L. Grossberg , Shawn G. Kwatra y and Ronald J. Sweren y 1 Department of Medicine, John H. Stroger Hospital of Cook County, Chicago, IL 60612, USA 2 Department of Dermatology, Johns Hopkins University School of Medicine, Baltimore, MD 21287, USA; [email protected] (M.B.); [email protected] (V.M.); [email protected] (R.K.); [email protected] (P.R.B.); [email protected] (M.S.H.); [email protected] (K.A.W.); [email protected] (A.L.G.); [email protected] (S.G.K.); [email protected] (R.J.S.) 3 Section of Dermatology, University of Calgary, Alberta, AB T2N 1N4, Canada; [email protected] * Correspondence: [email protected]; Tel.: +1-312-864-7000 Considered co-senior authors. y Received: 26 October 2019; Accepted: 24 December 2019; Published: 26 December 2019 Abstract: Background: Mycosis fungoides (MF) is a cutaneous T-cell lymphoma. Previous reports have suggested MF is associated with inflammatory conditions such as psoriasis, increased cardiovascular risk factors as well as secondary neoplasms. Methods: A cross-sectional study of MF patients seen from 2013 to 2019 was performed. Comorbidities were selected based on the 2015 Medicare report highlighting the most common chronic medical illnesses in the United States. -

18F-FDG Avidity in Lymphoma Readdressed: a Study of 766 Patients
Journal of Nuclear Medicine, published on December 15, 2009 as doi:10.2967/jnumed.109.067892 18F-FDG Avidity in Lymphoma Readdressed: A Study of 766 Patients Michal Weiler-Sagie1, Olga Bushelev2, Ron Epelbaum2,3, Eldad J. Dann2,4,5, Nissim Haim2,3, Irit Avivi2,5, Ayelet Ben-Barak6, Yehudit Ben-Arie2,7, Rachel Bar-Shalom1,2, and Ora Israel1,2 1Department of Nuclear Medicine, Rambam Health Care Campus, Haifa, Israel; 2Ruth and Bruce Rappaport Faculty of Medicine, Technion–Israel Institute of Technology, Haifa, Israel; 3Department of Oncology, Rambam Health Care Campus, Haifa, Israel; 4Blood Bank and Apheresis Unit, Rambam Health Care Campus, Haifa, Israel; 5Department of Hematology and Bone Marrow Transplantation, Rambam Health Care Campus, Haifa, Israel; 6Department of Pediatric Hematology-Oncology, Meyer Children’s Hospital, Rambam Health Care Campus, Haifa, Israel; and 7Department of Pathology, Rambam Health Care Campus, Haifa, Israel PET/CT with 18F-FDG is an important noninvasive diagnostic tool for management of patients with lymphoma, and its use may sur- Lymphoma is a heterogeneous group of diseases rep- pass current guideline recommendations. The aim of the present resenting the fifth most common malignancy in the United study is to enlarge the growing body of evidence concerning 18F- FDG avidity of lymphoma to provide a basis for future guidelines. States, with an estimated 74,340 new cases predicted for Methods: The reports from 18F-FDG PET/CT studies performed 2008 (1). Subtypes of lymphoma differ in molecular char- in a single center for staging of 1,093 patients with newly diag- acteristics and biologic behavior. Based on clinical charac- nosed Hodgkin disease and non-Hodgkin lymphoma between teristics, this entity is divided into aggressive and indolent 2001 and 2008 were reviewed for the presence of 18F-FDG avid- types (2,3). -

Hematopoietic and Lymphoid Neoplasm Coding Manual
Hematopoietic and Lymphoid Neoplasm Coding Manual Effective with Cases Diagnosed 1/1/2010 and Forward Published August 2021 Editors: Jennifer Ruhl, MSHCA, RHIT, CCS, CTR, NCI SEER Margaret (Peggy) Adamo, BS, AAS, RHIT, CTR, NCI SEER Lois Dickie, CTR, NCI SEER Serban Negoita, MD, PhD, CTR, NCI SEER Suggested citation: Ruhl J, Adamo M, Dickie L., Negoita, S. (August 2021). Hematopoietic and Lymphoid Neoplasm Coding Manual. National Cancer Institute, Bethesda, MD, 2021. Hematopoietic and Lymphoid Neoplasm Coding Manual 1 In Appreciation NCI SEER gratefully acknowledges the dedicated work of Drs, Charles Platz and Graca Dores since the inception of the Hematopoietic project. They continue to provide support. We deeply appreciate their willingness to serve as advisors for the rules within this manual. The quality of this Hematopoietic project is directly related to their commitment. NCI SEER would also like to acknowledge the following individuals who provided input on the manual and/or the database. Their contributions are greatly appreciated. • Carolyn Callaghan, CTR (SEER Seattle Registry) • Tiffany Janes, CTR (SEER Seattle Registry) We would also like to give a special thanks to the following individuals at Information Management Services, Inc. (IMS) who provide us with document support and web development. • Suzanne Adams, BS, CTR • Ginger Carter, BA • Sean Brennan, BS • Paul Stephenson, BS • Jacob Tomlinson, BS Hematopoietic and Lymphoid Neoplasm Coding Manual 2 Dedication The Hematopoietic and Lymphoid Neoplasm Coding Manual (Heme manual) and the companion Hematopoietic and Lymphoid Neoplasm Database (Heme DB) are dedicated to the hard-working cancer registrars across the world who meticulously identify, abstract, and code cancer data. -

Landispiwowar.Kristin.Genetics of Select Lymphoproliferative
3/21/16 Objecves Gene+cs of Select • Define tumor suppressor gene and oncogene Lymphoproliferave Neoplasms: • Correlate genotypes Pathophysiology, Prognos+caon, and Therapy with prognosis in lymphoproliferave neoplasms Kris+n Landis-Piwowar PhD, MLS(ASCP)CM • Recognize the targets of lymphoproliferave Clinical Laboratory Hematology, 3/E, McKenzie • Williams neoplasm therapies 2 Leukemia Lymphoma WHO 2008: Mature B-Cell Neoplasms • Chronic lymphocy+c leukemia/small lymphocy+c • Mantle cell lymphoma lymphoma • Diffuse large B-cell lymphoma (DLBCL), NOS • Primarily BM and • Primarily lymph • B-cell prolymphocyc leukemia • T-cell/his+ocyte rich large B-cell lymphoma • Primary DLBCL of the CNS • Splenic marginal zone lymphoma • Primary cutaneous DLBCL, leg type blood involvement node / solid ssue • Hairy cell leukemia • EBV-posi+ve DLBCL of the elderly • Splenic lymphoma/leukemia, unclassifiable • DLBCL associated with chronic inflammaon • Splenic diffuse red pulp small B-cell lymphoma • Lymphomatoid granulomatosis • Hairy cell leukemia variant involvement • Primary medias+nal (thymic) large B-cell lymphoma • Myeloid or • Lymphoplasmacy+c lymphoma • Intravascular large B-cell lymphoma • Waldenström macroglobulinemia • ALK-posi+ve large B-cell lymphoma lymphoid origin • Lymphoid origin • Heavy chain diseases • α Heavy chain disease • Plasmablas+c lymphoma • γ Heavy chain disease • Large B-cell lymphoma arising in HHV8-associated • May secondarily • May secondarily • μ Heavy chain disease mul+centric Castleman disease • Plasma cell myeloma • Primary -

Successful Treatment of CD30+Lymphomatoid Papulosis
ooggeenneessii iinn ss && rrcc aa MM CC uu tt ff aa Journal ofJournal of oo gg ll ee ee aa aa nn nn nn nn ee ee rr rr ss ss uu uu ii ii Watabe et al., J Carcinog Mutagen 2014, 5:3 ss ss oo oo JJ JJ ISSN: 2157-2518 CarCarcinogenesiscinogenesis & Mutagenesis DOI: 10.4172/2157-2518.1000174 Case Report Open Access Successful Treatment of CD30+Lymphomatoid Papulosis using a 308-nm Excimer Light Akiko Watabe, Taku Fujimura*, Sadanori Furudate and Setsuya Aiba Department of Dermatology, Tohoku University Graduate School of Medicine, Sendai, Japan *Corresponding author: Taku Fujimura, Department of Dermatology, Tohoku University Graduate School of Medicine, Seiryo-machi 1-1, Aoba-ku, Sendai, 980-8574, Japan, Tel:+81 (22) 717-7271; Fax: +81 (22) 717-7361; E-mail: [email protected] Received date: Mar 11, 2014, Accepted date: May 03, 2014, Published date: May 07, 2014 Copyright: © 2013 Watabe A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited Abstract We describe a 61-year-old Japanese patient with Lymphomatoid papulosis (LYP) successfully archived complete remission, using a 308-nm Excimer light. Interestingly, immunohistochemical staining revealed that CD30+ anaplastic tumor cells were surrounded by CD163+ macrophages and CCL18 producing cells, both of which were reported to correlate with the prognosis of CTCL. Our present study sheds light on the possible pathogenesis of LYP and the possibility of a 308-nm Excimer light phototherapy for LYP. -

Indolent Non-Hodgkin's Lymphomas
Follicular and Low-Grade Non-Hodgkin Lymphomas (Indolent Lymphomas) Stefan K Barta, M.D., M.S. Associate Professor of Medicine Leader, T Cell Lymphoma Program Perelman Center for Advanced Medicine Facts and Figures: Non-Hodgkin Lymphomas • Most common blood cancer • 7th most common cancer in the US3 • 71,850 new cases in the US in 20151 • 19,790 died of NHL in 20151 • About 549,625 people are living with a history of NHL (2012)1 • 85% of all NHLs are B-cell lymphomas2 • Follicular lymphoma = 2nd most common type, ~25% of all NHLs4 1 http://seer.cancer.gov/statfacts/html/nhl.html. 2 ACS. Detailed Guide (revised January 21, 2000): Non-Hodgkin’s Lymphoma. 3 http://www.cancer.gov/cancertopics/types/commoncancers 4 Blood 89: 3909, 1997 The Immune System T- CELLS B- CELLS Cellular immunity: Humoral immunity: helper + cytotoxic T-cells antibodies Lymphatic System Lymph Node Anatomy Lymph Node: Microscopic View germinal center Lymphocyte: Microscopic View Causes Possible cause(s): • chemical exposures (pesticides, fertilizers or solvents) • individuals with compromised immune systems • heredity • infections (e.g. H. pylori, Hep C, chlamydia trachomatis) • most patients have no clear risk factors • IN MOST CASES, THE EXACT CAUSE IS UNKNOWN Cellular Origins of Lymphomas & Leukemias PLEURIPOTENT STEM CELL ACUTE LEUKEMIAS LYMPHOID STEM CELL ACUTE LYMPHOBLASTIC LEUKEMIAS PRECURSOR T - CELL PRECURSOR B - CELL LYMPHOBLASTIC LYMPHOMAS / LEUKEMIAS MATURE T - CELL MATURE B - CELL NON-HODGKIN LYMPHOMAS / CHRONIC LYMPHOCYTIC LEUKEMIA LYMPH NODES, EXTRANODAL -

Lymphomatoid Papulosis Development in Acute Lymphoblastic Leukemia
Case Report J Med Cases. 2021;12(8):306-309 Lymphomatoid Papulosis Development in Acute Lymphoblastic Leukemia Kazumi Ouraa, Tomonobu Satoa, d , Akihiro Iguchib, Naohisa Toriumic, Takeo Sarashinac Abstract LyP is a rare disease with an incidence of 1.2 - 1.9 per million [1] and accounts for 16.0-47.0% of pediatric cutaneous lym- Lymphomatoid papulosis (LyP) is a chronic, recurrent benign skin phoproliferative disorders [2]. It has been reported that LyP disease characterized by histological features of a CD 30-positive cu- often disappears spontaneously and has a benign course [3, taneous T-cell lymphoproliferative disorder. It is rare, with an annual, 4]. However, a relationship between LyP and certain hemato- worldwide incidence of 1.2 - 1.9 per million, and accounts for 16-47% logical malignancies has also been reported [5-7]. Herein, we of pediatric cutaneous lymphoproliferative disorders. It often occurs describe a case in which tumors appeared in the left scrotum on the extremities or the trunk and rarely affects the face or genitals. and under the left lip during maintenance therapy for pre- Its onset may be triggered by irradiation therapy, immunomodulating cursor B-cell acute lymphoblastic leukemia (BCP-ALL). We agents, infection or atopic dermatitis. It has a benign course but is as- needed to distinguish the tumor from extramedullary recur- sociated with certain hematological malignancies. Mycosis fungoides rence of ALL or de novo other cutaneous lymphoma; how- and primary cutaneous anaplastic large cell lymphoma are the most ever, the histological findings of a tumor biopsy resulted in a commonly associated hematological malignancies. -

Co-Occurrence of Lymphomatoid Papulosis and Mycosis Fungoides in a Young Female: a Case Report Natalie Steinhoff, DO,* Brian Wanner,** Matthew H
Co-Occurrence of Lymphomatoid Papulosis and Mycosis Fungoides in a Young Female: A Case Report Natalie Steinhoff, DO,* Brian Wanner,** Matthew H. Mahoney, MD*** *Dermatology Resident, PGY-3, Nova Southeastern University College of Osteopathic Medicine, Largo Medical Center, Largo, FL **Osteopathic Medical Student, 4th year, Des Moines University College of Osteopathic Medicine, Des Moines, IA ***Dermatologist and Clinical Faculty, Nova Southeastern University College of Osteopathic Medicine, Largo Medical Center, Largo, FL Disclosures: None Correspondence: Natalie Steinhoff, DO; NSUCOM/Largo Medical Center; 201 14th St. SW, Largo, FL 33770; [email protected] Abstract There have been reports of lymphomatoid papulosis (LyP) and mycosis fungoides (MF) presenting separately, simultaneously, and consecutively. LyP is a CD30+ lymphoproliferative disorder, and MF is the most common cutaneous T-cell lymphoma (CTCL). LyP most often presents with self-regressing, erythematous-to-brown papules or small nodules. Mycosis fungoides has a variety of clinical manifestations, but in early stages it commonly presents as an erythematous patch or plaque. Recognizing LyP is important due to its association with development of secondary malignancies, most commonly MF, Hodgkin’s disease, and anaplastic large-cell lymphoma (ALCL). We report a case of a 35-year-old woman with recurrent LyP lesions since childhood who went on to develop concurrent LyP and MF. We discuss the need to evaluate LyP patients for secondary lymphomas and provide a concise review of the literature focusing on clinical presentation, diagnosis, disease associations, and management. microabscesses (mycosis cells in the epidermis), Spontaneous self-regression of lesions is required Introduction 3 19 Lymphomatoid papulosis (LyP) is one of two and a band-like dermal infiltrate of lymphocytes. -

Lymphomatoid Papulosis in Children a Retrospective Cohort Study of 35 Cases
STUDY Lymphomatoid Papulosis in Children A Retrospective Cohort Study of 35 Cases Tamar Nijsten, MD; Clara Curiel-Lewandrowski, MD; Marshall E. Kadin, MD Background: Lymphomatoid papulosis (LyP) is a rare of follow-up was 9.0 years. All included patients were con- entity, considered to be part of the spectrum of the CD30+ firmed by histologic examination. cutaneous lymphoproliferative disorders. About 10% to 20% of the adult LyP patients will develop an associated Results: The age distribution was significantly differ- lymphoid malignancy. Only a few cases of LyP have been ent, with boys having an earlier onset of LyP (P=.03). described in children, and the risk of associated lym- Of the 35 LyP patients, 3 (9%) developed a malignant phoid malignancies in these patients is not known. lymphoma; all were diagnosed as having non-Hodgkin lymphoma. Compared with the general population, pa- Objectives: To study the association between child- tients with childhood-onset LyP have a significantly in- hood onset of LyP and other malignancies and to deter- creased risk of developing non-Hodgkin lymphoma (rela- mine the clinical characteristics in this subgroup of pa- tive risk, 226.2; 95% confidence interval, 73.4-697.0). tients. More than two thirds of the patients reported being atopic, which is significantly more than the expected preva- Design: Retrospective cohort study. lence of atopy (relative risk, 3.1; 95% confidence inter- val, 2.2-4.3). Setting: Referral center at a university hospital. Retro- spective registry for patients with LyP of childhood on- Conclusions: Lymphomatoid papulosis presents simi- set (Յ18 years). -
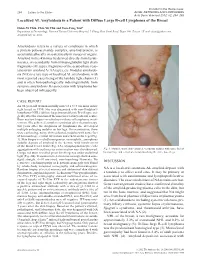
Localized AL Amyloidosis in a Patient with Diffuse Large B-Cell Lymphoma of the Breast
Included in the theme issue: 284 Letters to the Editor ACNE, RETINOIDS AND LYMPHOMAS Acta Derm Venereol 2012; 92: 284–285 Localized AL Amyloidosis in a Patient with Diffuse Large B-cell Lymphoma of the Breast Hsien-Yi Chiu, Chia-Yu Chu and Tsen-Fang Tsai* Department of Dermatology, National Taiwan University Hospital, 7 Chung-Shan South Road, Taipei 100, Taiwan. *E-mail: [email protected] Accepted July 11, 2011. Amyloidosis refers to a variety of conditions in which a protein polysaccharide complex, amyloid protein, is accumulated locally or systemically in tissues or organs. Amyloid in the skin may be derived directly from kerati- nocytes, or secondarily from immunoglobulin light chain fragments (AL type), fragments of the acute-phase reac- tant serum amyloid A (AA type), etc. Nodular amyloido- sis (NA) is a rare type of localized AL amyloidosis, with most reported cases being of the lambda light chains (1) and is often histopathologically indistinguishable from systemic amyloidosis. Its association with lymphoma has been observed infrequently. CASE REPORT An 88-year-old woman initially noticed a 5×3 cm mass in her right breast in 1990. She was diagnosed with non-Hodgkin’s lymphoma (NHL) (diffuse large immunoblastic B-cell type, sta- ge IE) after the excision of the mass in a tertiary referral centre. Bone marrow biopsy revealed no evidence of lymphoma invol- vement. She achieved complete remission after chemotherapy. Six years after the diagnosis of lymphoma she developed multiple enlarging nodules on her legs. On examination, there were coalescing, waxy, skin-coloured, nodules with some foci of haemorrhage, central ulceration and crusts on the legs (Fig. -

Primary Cutaneous Lymphoma: ESMO Clinical Recommendations for Diagnosis, Treatment and Follow-Up R
Annals of Oncology 19 (Supplement 2): ii72–ii76, 2008 clinical recommendations doi:10.1093/annonc/mdn095 Primary cutaneous lymphoma: ESMO Clinical Recommendations for diagnosis, treatment and follow-up R. Dummer1 & M. Dreyling2 On behalf of the ESMO Guidelines Working Group* 1Department of Dermatology, University Hospital, Zu¨rich, Switzerland; 2Department of Medicine III, University Hospital Grosshadern, Munich, Germany introduction the quality of life due to their impact on skin appearance and annoying symptoms such as pruritus. In some cases they can Cutaneous lymphomas (CL) are the second most common already be disfiguring in early disease stages. In advanced stages, extranodal non-Hodgkin’s lymphomas. Their incidence is local skin problems are accompanied by systemic immune estimated at 1/100 000 yearly. Primary CL develop by definition suppression which results in an increased risk of infections and in the skin and remain confined to the skin for a long period of secondary malignancies. Some of the late-stage problems in time, while secondary CL reflect cutaneous spread from MF/SS patients might have been aggravated by earlier disseminated primary nodal or extranodal lymphomas. Primary therapeutic interventions, e.g. radiotherapy or phototherapy CL include a wide spectrum of clinically and histologically may contribute to mutations that increase the proliferative heterogeneous lymphoproliferative neoplasms: 75% of CL are and invasive capacity of the tumor cell populations. Cytotoxic cutaneous T-cell lymphomas (CTCL); 25% cutaneous B-cell drugs favor infectious complications. Most patients with lymphomas (CBCL); and a few percent other uncommon advanced disease may die due to secondary problems such as forms. CL and nodal or extracutaneous lymphomas with the infections.