Blood-Based Molecular Biomarker Signatures in Alzheimer's
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Retrocopy Contributions to the Evolution of the Human Genome Robert Baertsch*1, Mark Diekhans1, W James Kent1, David Haussler1 and Jürgen Brosius2
BMC Genomics BioMed Central Research article Open Access Retrocopy contributions to the evolution of the human genome Robert Baertsch*1, Mark Diekhans1, W James Kent1, David Haussler1 and Jürgen Brosius2 Address: 1Center for Biomolecular Science and Engineering, University of California Santa Cruz, Santa Cruz, California 95064, USA and 2Institute of Experimental Pathology, ZMBE, University of Münster, Von-Esmarch-Str. 56, D-48149, Münster, Germany Email: Robert Baertsch* - [email protected]; Mark Diekhans - [email protected]; W James Kent - [email protected]; David Haussler - [email protected]; Jürgen Brosius - [email protected] * Corresponding author Published: 8 October 2008 Received: 17 March 2008 Accepted: 8 October 2008 BMC Genomics 2008, 9:466 doi:10.1186/1471-2164-9-466 This article is available from: http://www.biomedcentral.com/1471-2164/9/466 © 2008 Baertsch et al; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Abstract Background: Evolution via point mutations is a relatively slow process and is unlikely to completely explain the differences between primates and other mammals. By contrast, 45% of the human genome is composed of retroposed elements, many of which were inserted in the primate lineage. A subset of retroposed mRNAs (retrocopies) shows strong evidence of expression in primates, often yielding functional retrogenes. Results: To identify and analyze the relatively recently evolved retrogenes, we carried out BLASTZ alignments of all human mRNAs against the human genome and scored a set of features indicative of retroposition. -

Proteomics Provides Insights Into the Inhibition of Chinese Hamster V79
www.nature.com/scientificreports OPEN Proteomics provides insights into the inhibition of Chinese hamster V79 cell proliferation in the deep underground environment Jifeng Liu1,2, Tengfei Ma1,2, Mingzhong Gao3, Yilin Liu4, Jun Liu1, Shichao Wang2, Yike Xie2, Ling Wang2, Juan Cheng2, Shixi Liu1*, Jian Zou1,2*, Jiang Wu2, Weimin Li2 & Heping Xie2,3,5 As resources in the shallow depths of the earth exhausted, people will spend extended periods of time in the deep underground space. However, little is known about the deep underground environment afecting the health of organisms. Hence, we established both deep underground laboratory (DUGL) and above ground laboratory (AGL) to investigate the efect of environmental factors on organisms. Six environmental parameters were monitored in the DUGL and AGL. Growth curves were recorded and tandem mass tag (TMT) proteomics analysis were performed to explore the proliferative ability and diferentially abundant proteins (DAPs) in V79 cells (a cell line widely used in biological study in DUGLs) cultured in the DUGL and AGL. Parallel Reaction Monitoring was conducted to verify the TMT results. γ ray dose rate showed the most detectable diference between the two laboratories, whereby γ ray dose rate was signifcantly lower in the DUGL compared to the AGL. V79 cell proliferation was slower in the DUGL. Quantitative proteomics detected 980 DAPs (absolute fold change ≥ 1.2, p < 0.05) between V79 cells cultured in the DUGL and AGL. Of these, 576 proteins were up-regulated and 404 proteins were down-regulated in V79 cells cultured in the DUGL. KEGG pathway analysis revealed that seven pathways (e.g. -

Essential Genes and Their Role in Autism Spectrum Disorder
University of Pennsylvania ScholarlyCommons Publicly Accessible Penn Dissertations 2017 Essential Genes And Their Role In Autism Spectrum Disorder Xiao Ji University of Pennsylvania, [email protected] Follow this and additional works at: https://repository.upenn.edu/edissertations Part of the Bioinformatics Commons, and the Genetics Commons Recommended Citation Ji, Xiao, "Essential Genes And Their Role In Autism Spectrum Disorder" (2017). Publicly Accessible Penn Dissertations. 2369. https://repository.upenn.edu/edissertations/2369 This paper is posted at ScholarlyCommons. https://repository.upenn.edu/edissertations/2369 For more information, please contact [email protected]. Essential Genes And Their Role In Autism Spectrum Disorder Abstract Essential genes (EGs) play central roles in fundamental cellular processes and are required for the survival of an organism. EGs are enriched for human disease genes and are under strong purifying selection. This intolerance to deleterious mutations, commonly observed haploinsufficiency and the importance of EGs in pre- and postnatal development suggests a possible cumulative effect of deleterious variants in EGs on complex neurodevelopmental disorders. Autism spectrum disorder (ASD) is a heterogeneous, highly heritable neurodevelopmental syndrome characterized by impaired social interaction, communication and repetitive behavior. More and more genetic evidence points to a polygenic model of ASD and it is estimated that hundreds of genes contribute to ASD. The central question addressed in this dissertation is whether genes with a strong effect on survival and fitness (i.e. EGs) play a specific oler in ASD risk. I compiled a comprehensive catalog of 3,915 mammalian EGs by combining human orthologs of lethal genes in knockout mice and genes responsible for cell-based essentiality. -

CD29 Identifies IFN-Γ–Producing Human CD8+ T Cells With
+ CD29 identifies IFN-γ–producing human CD8 T cells with an increased cytotoxic potential Benoît P. Nicoleta,b, Aurélie Guislaina,b, Floris P. J. van Alphenc, Raquel Gomez-Eerlandd, Ton N. M. Schumacherd, Maartje van den Biggelaarc,e, and Monika C. Wolkersa,b,1 aDepartment of Hematopoiesis, Sanquin Research, 1066 CX Amsterdam, The Netherlands; bLandsteiner Laboratory, Oncode Institute, Amsterdam University Medical Center, University of Amsterdam, 1105 AZ Amsterdam, The Netherlands; cDepartment of Research Facilities, Sanquin Research, 1066 CX Amsterdam, The Netherlands; dDivision of Molecular Oncology and Immunology, Oncode Institute, The Netherlands Cancer Institute, 1066 CX Amsterdam, The Netherlands; and eDepartment of Molecular and Cellular Haemostasis, Sanquin Research, 1066 CX Amsterdam, The Netherlands Edited by Anjana Rao, La Jolla Institute for Allergy and Immunology, La Jolla, CA, and approved February 12, 2020 (received for review August 12, 2019) Cytotoxic CD8+ T cells can effectively kill target cells by producing therefore developed a protocol that allowed for efficient iso- cytokines, chemokines, and granzymes. Expression of these effector lation of RNA and protein from fluorescence-activated cell molecules is however highly divergent, and tools that identify and sorting (FACS)-sorted fixed T cells after intracellular cytokine + preselect CD8 T cells with a cytotoxic expression profile are lacking. staining. With this top-down approach, we performed an un- + Human CD8 T cells can be divided into IFN-γ– and IL-2–producing biased RNA-sequencing (RNA-seq) and mass spectrometry cells. Unbiased transcriptomics and proteomics analysis on cytokine- γ– – + + (MS) analyses on IFN- and IL-2 producing primary human producing fixed CD8 T cells revealed that IL-2 cells produce helper + + + CD8 Tcells. -

The Ire1a-XBP1 Pathway Promotes T Helper Cell Differentiation by Resolving Secretory Stress and Accelerating Proliferation
bioRxiv preprint doi: https://doi.org/10.1101/235010; this version posted December 15, 2017. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC-ND 4.0 International license. The IRE1a-XBP1 pathway promotes T helper cell differentiation by resolving secretory stress and accelerating proliferation Jhuma Pramanik1, Xi Chen1, Gozde Kar1,2, Tomás Gomes1, Johan Henriksson1, Zhichao Miao1,2, Kedar Natarajan1, Andrew N. J. McKenzie3, Bidesh Mahata1,2*, Sarah A. Teichmann1,2,4* 1. Wellcome Trust Sanger Institute, Wellcome Genome Campus, Hinxton, Cambridge, CB10 1SA, United Kingdom 2. EMBL-European Bioinformatics Institute, Wellcome Genome Campus, Hinxton, Cambridge, CB10 1SD, United Kingdom 3. MRC Laboratory of Molecular Biology, Cambridge Biomedical Campus, Francis Crick Avenue, Cambridge CB2 OQH, United Kingdom 4. Theory of Condensed Matter, Cavendish Laboratory, 19 JJ Thomson Ave, Cambridge CB3 0HE, United Kingdom. *To whom correspondence should be addressed: [email protected] and [email protected] Keywords: Th2 lymphocyte, XBP1, Genome wide XBP1 occupancy, Th2 lymphocyte proliferation, ChIP-seq, RNA-seq, Th2 transcriptome Summary The IRE1a-XBP1 pathway, a conserved adaptive mediator of the unfolded protein response, is indispensable for the development of secretory cells. It maintains endoplasmic reticulum homeostasis by facilitating protein folding and enhancing secretory capacity of the cells. Its role in immune cells is emerging. It is involved in dendritic cell, plasma cell and eosinophil development and differentiation. Using genome-wide approaches, integrating ChIPmentation and mRNA-sequencing data, we have elucidated the regulatory circuitry governed by the IRE1a-XBP1 pathway in type-2 T helper cells (Th2). -

SND1, a Component of RNA-Induced Silencing Complex, Is Up-Regulated in Human Colon Cancers and Implicated in Early Stage Colon Carcinogenesis
Research Article SND1, a Component of RNA-Induced Silencing Complex, Is Up-regulated in Human Colon Cancers and Implicated in Early Stage Colon Carcinogenesis Naoto Tsuchiya, Masako Ochiai, Katsuhiko Nakashima, Tsuneyuki Ubagai, Takashi Sugimura, and Hitoshi Nakagama Biochemistry Division, National Cancer Center Research Institute, 5-1-1 Tsukiji, Chuo-ku, Tokyo, Japan Abstract transcription factors is well known to be a causative event involved Colon cancers have been shown to develop after accumulation in malignant transformation, for example, with functional inacti- vation or intragenic mutation of p53 (3), and gene amplification or of multiple genetic and epigenetic alterations with changes in global gene expression profiles, contributing to the establish- overexpression of c-myc (4). ment of widely diverse phenotypes. Transcriptional and Recently, posttranscriptional regulation, especially translational posttranscriptional regulation of gene expression by small control, of gene expression has become a major interest in the field of cancer research, because accumulating evidence strongly RNA species, such as the small interfering RNA and microRNA suggests its biological relevance for cancer development and and the RNA-induced silencing complex (RISC), is currently drawing major interest with regard to cancer development. progression (5). Some oncogenes and tumor suppressor genes, including c-myc (6), Mdm-2(7), and p53 (8), have been shown to be SND1, also called Tudor-SN and p100 and recently reported to regulated at the translational level. Overexpression of the transla- be a component of RISC, is among the list of highly expressed tion initiation factor eIF4E promotes malignant transformation of genes in human colon cancers. In the present study, we normal fibroblasts (9) and cooperates with c-Myc to drive B-cell showed remarkable up-regulation of SND1 mRNA in human lymphomatogenesis in eIF4E transgenic mice (10). -

Investigating the Molecular Mechanisms of Splicing-Perturbing Small Molecules with Massively Parallel Sequencing in a Myotonic Dystrophy 1 Model
INVESTIGATING THE MOLECULAR MECHANISMS OF SPLICING-PERTURBING SMALL MOLECULES WITH MASSIVELY PARALLEL SEQUENCING IN A MYOTONIC DYSTROPHY 1 MODEL by MATTHEW TANNER A THESIS Presented to the Department of Chemistry and Biochemistry and the Robert D. Clark Honors College in partial fulfillment of the requirements for the degree of Bachelor of Science June, 2014 An Abstract of the Thesis of Matthew Tanner for the degree of Bachelor of Science in the Department of Chemistry and Biochemistry to be taken June, 2014 Title: Investigating the Molecular Mechanisms of Splicing-Perturbing Small Molecules with Massively Parallel Sequencing in a Myotonic Dystrophy 1 Model Approved: 4 fhh 73cJ-i J. Andrew Berglund Myotonic dystrophy is the most common form of adult-onset muscular dystrophy and appears in two forms: myotonic dystrophy 1 (OM 1) and 2 (DM2). Both diseases arc characterized by progressive muscle degeneration, myotonia. iridescent cataracts, and in severe cases neurodcgcncration and cardiac dysfunction. Both fonns of myotonic dystrophy arc caused by an expansion of repeat DNA in distinct loci in the genome. In DM 1, a CTG repeat is expanded from less than 50 repeats in nonnal individuals to up to several thousand repeats in DM 1 patients. The molecular basis of this disease relics on the transcription of these repeats from DNA into RNA. Small molecules that can specifically target the repeats at the DNA level and inhibit their transcription - and thus alleviate the disease symptoms - represent a prime target for the development of therapeutics. This study investigates the capacity of two small molecules, pentamidine and actinomycin D, to reverse the molecular symptoms of DM I through transcriptional inhibition and provides insight into their DNA target specificity and potential mechanisms of action. -

Aneuploidy: Using Genetic Instability to Preserve a Haploid Genome?
Health Science Campus FINAL APPROVAL OF DISSERTATION Doctor of Philosophy in Biomedical Science (Cancer Biology) Aneuploidy: Using genetic instability to preserve a haploid genome? Submitted by: Ramona Ramdath In partial fulfillment of the requirements for the degree of Doctor of Philosophy in Biomedical Science Examination Committee Signature/Date Major Advisor: David Allison, M.D., Ph.D. Academic James Trempe, Ph.D. Advisory Committee: David Giovanucci, Ph.D. Randall Ruch, Ph.D. Ronald Mellgren, Ph.D. Senior Associate Dean College of Graduate Studies Michael S. Bisesi, Ph.D. Date of Defense: April 10, 2009 Aneuploidy: Using genetic instability to preserve a haploid genome? Ramona Ramdath University of Toledo, Health Science Campus 2009 Dedication I dedicate this dissertation to my grandfather who died of lung cancer two years ago, but who always instilled in us the value and importance of education. And to my mom and sister, both of whom have been pillars of support and stimulating conversations. To my sister, Rehanna, especially- I hope this inspires you to achieve all that you want to in life, academically and otherwise. ii Acknowledgements As we go through these academic journeys, there are so many along the way that make an impact not only on our work, but on our lives as well, and I would like to say a heartfelt thank you to all of those people: My Committee members- Dr. James Trempe, Dr. David Giovanucchi, Dr. Ronald Mellgren and Dr. Randall Ruch for their guidance, suggestions, support and confidence in me. My major advisor- Dr. David Allison, for his constructive criticism and positive reinforcement. -

Insights Into SND1 Oncogene Promoter Regulation
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Archivo Digital para la Docencia y la Investigación REVIEW published: 11 December 2018 doi: 10.3389/fonc.2018.00606 Insights Into SND1 Oncogene Promoter Regulation Begoña Ochoa, Yolanda Chico and María José Martínez* Department of Physiology, Faculty of Medicine and Nursing, University of the Basque Country UPV/EHU, Leioa, Spain The staphylococcal nuclease and Tudor domain containing 1 gene (SND1), also known as Tudor-SN, TSN or p100, encodes an evolutionarily conserved protein with invariant domain composition. SND1 contains four repeated staphylococcal nuclease domains and a single Tudor domain, which confer it endonuclease activity and extraordinary capacity for interacting with nucleic acids, individual proteins and protein complexes. Originally described as a transcriptional coactivator, SND1 plays fundamental roles in the regulation of gene expression, including RNA splicing, interference, stability, and editing, as well as in the regulation of protein and lipid homeostasis. Recently, SND1 has gained attention as a potential disease biomarker due to its positive correlation with cancer progression and metastatic spread. Such functional diversity of SND1 marks this gene as interesting for further analysis in relation with the multiple levels of regulation of SND1 protein production. In this review, we summarize the SND1 genomic region Edited by: and promoter architecture, the set of transcription factors that can bind the proximal Markus A. N. Hartl, promoter, and the evidence supporting transactivation of SND1 promoter by a number of University of Innsbruck, Austria signal transduction pathways operating in different cell types and conditions. Unraveling Reviewed by: John Strouboulis, the mechanisms responsible for SND1 promoter regulation is of utmost interest to King’s College London, decipher the SND1 contribution in the realm of both normal and abnormal physiology. -

Blood-Based Molecular Biomarker Signatures in Alzheimer's
bioRxiv preprint doi: https://doi.org/10.1101/481879; this version posted December 31, 2018. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. Article Blood-based molecular biomarker signatures in Alzheimer’s disease: insights from systems biomedicine perspective Tania Islam 1,#, Md. Rezanur Rahman 2,#,*, Md. Shahjaman3, Toyfiquz Zaman2, Md. Rezaul Karim2, Julian M.W. Quinn4, R.M. Damian Holsinger5,6, and Mohammad Ali Moni 6,* 1Department of Biotechnology and Genetic Engineering, Islamic University, Kushtia, Bangladesh; [email protected](T.I.). 2 Department of Biochemistry and Biotechnology, School of Biomedical Science, Khwaja Yunus Ali University, Sirajgonj, Bangladesh; [email protected](M.R.R.). 3 Department of Statistics, Begum Rokeya University, Rangpur, Bangladesh; [email protected] (M.S.). 4 Bone Biology Division, Garvan Institute of Medical Research, Darlinghurst, NSW, Australia;[email protected](J.W.W.Q.). 5 Laboratory of Molecular Neuroscience and Dementia, Brain and Mind Centre, The University of Sydney, Camperdown, NSW, Australia; [email protected] (R.M.D.H.). 6 Discipline of Biomedical Science, School of Medical Sciences, The University of Sydney, Sydney, NSW, Australia; [email protected] (M.A.M.). #These two authors have made an equal contribution and hold joint first authorship for this work. * Correspondence: [email protected] (M.R.R.) or [email protected] (M.A.M.). Abstract: Background and objectives: Alzheimer’s disease (AD) is the progressive neurodegenerative disease characterized by dementia, but no peripheral biomarkers available yet that can detect the AD. -
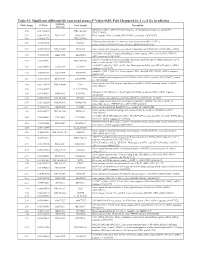
(P -Value<0.05, Fold Change≥1.4), 4 Vs. 0 Gy Irradiation
Table S1: Significant differentially expressed genes (P -Value<0.05, Fold Change≥1.4), 4 vs. 0 Gy irradiation Genbank Fold Change P -Value Gene Symbol Description Accession Q9F8M7_CARHY (Q9F8M7) DTDP-glucose 4,6-dehydratase (Fragment), partial (9%) 6.70 0.017399678 THC2699065 [THC2719287] 5.53 0.003379195 BC013657 BC013657 Homo sapiens cDNA clone IMAGE:4152983, partial cds. [BC013657] 5.10 0.024641735 THC2750781 Ciliary dynein heavy chain 5 (Axonemal beta dynein heavy chain 5) (HL1). 4.07 0.04353262 DNAH5 [Source:Uniprot/SWISSPROT;Acc:Q8TE73] [ENST00000382416] 3.81 0.002855909 NM_145263 SPATA18 Homo sapiens spermatogenesis associated 18 homolog (rat) (SPATA18), mRNA [NM_145263] AA418814 zw01a02.s1 Soares_NhHMPu_S1 Homo sapiens cDNA clone IMAGE:767978 3', 3.69 0.03203913 AA418814 AA418814 mRNA sequence [AA418814] AL356953 leucine-rich repeat-containing G protein-coupled receptor 6 {Homo sapiens} (exp=0; 3.63 0.0277936 THC2705989 wgp=1; cg=0), partial (4%) [THC2752981] AA484677 ne64a07.s1 NCI_CGAP_Alv1 Homo sapiens cDNA clone IMAGE:909012, mRNA 3.63 0.027098073 AA484677 AA484677 sequence [AA484677] oe06h09.s1 NCI_CGAP_Ov2 Homo sapiens cDNA clone IMAGE:1385153, mRNA sequence 3.48 0.04468495 AA837799 AA837799 [AA837799] Homo sapiens hypothetical protein LOC340109, mRNA (cDNA clone IMAGE:5578073), partial 3.27 0.031178378 BC039509 LOC643401 cds. [BC039509] Homo sapiens Fas (TNF receptor superfamily, member 6) (FAS), transcript variant 1, mRNA 3.24 0.022156298 NM_000043 FAS [NM_000043] 3.20 0.021043295 A_32_P125056 BF803942 CM2-CI0135-021100-477-g08 CI0135 Homo sapiens cDNA, mRNA sequence 3.04 0.043389246 BF803942 BF803942 [BF803942] 3.03 0.002430239 NM_015920 RPS27L Homo sapiens ribosomal protein S27-like (RPS27L), mRNA [NM_015920] Homo sapiens tumor necrosis factor receptor superfamily, member 10c, decoy without an 2.98 0.021202829 NM_003841 TNFRSF10C intracellular domain (TNFRSF10C), mRNA [NM_003841] 2.97 0.03243901 AB002384 C6orf32 Homo sapiens mRNA for KIAA0386 gene, partial cds. -

Histone Methyltransferase MMSET/NSD2 Alters EZH2 Binding and Reprograms the Myeloma Epigenome Through Global and Focal Changes in H3K36 and H3K27 Methylation
Histone Methyltransferase MMSET/NSD2 Alters EZH2 Binding and Reprograms the Myeloma Epigenome through Global and Focal Changes in H3K36 and H3K27 Methylation Relja Popovic1., Eva Martinez-Garcia1., Eugenia G. Giannopoulou2,3, Quanwei Zhang4, Qingyang Zhang4, Teresa Ezponda1, Mrinal Y. Shah1, Yupeng Zheng5, Christine M. Will1, Eliza C. Small1, Youjia Hua1, Marinka Bulic1, Yanwen Jiang6, Matteo Carrara7, Raffaele A. Calogero7, William L. Kath8, Neil L. Kelleher5, Ji-Ping Wang4, Olivier Elemento6, Jonathan D. Licht1* 1 Division of Hematology/Oncology, Northwestern University Feinberg School of Medicine, Chicago, Illinois, United States of America, 2 Arthritis and Tissue Degeneration Program and the David Z. Rosensweig Genomics Research Center, Hospital for Special Surgery, New York, New York, United States of America, 3 Biological Sciences Department, New York City College of Technology, City University of New York, Brooklyn, New York, New York, United States of America, 4 Department of Statistics, Northwestern University, Evanston, Illinois, United States of America, 5 Department of Chemistry and Molecular Biosciences, Chemistry of Life Processes Institute, Northwestern University, Evanston, Illinois, United States of America, 6 HRH Prince Alwaleed Bin Talal Bin Abdulaziz Alsaud Institute for Computational Biomedicine and Department of Physiology and Biophysics, Weill Cornell Medical College, New York, New York, United States of America, 7 Molecular Biotechnology Center, Department of Biotechnology and Health Sciences, University of Torino, Torino, Italy, 8 Department of Engineering Sciences and Applied Mathematics, Northwestern University, Evanston, Illinois, United States of America Abstract Overexpression of the histone methyltransferase MMSET in t(4;14)+ multiple myeloma patients is believed to be the driving factor in the pathogenesis of this subtype of myeloma.