Medicines and Falls in Hospital
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
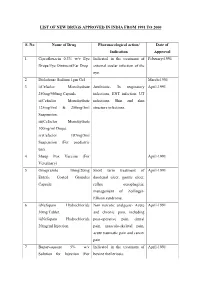
List of New Drugs Approved in India from 1991 to 2000
LIST OF NEW DRUGS APPROVED IN INDIA FROM 1991 TO 2000 S. No Name of Drug Pharmacological action/ Date of Indication Approval 1 Ciprofloxacin 0.3% w/v Eye Indicated in the treatment of February-1991 Drops/Eye Ointment/Ear Drop external ocular infection of the eye. 2 Diclofenac Sodium 1gm Gel March-1991 3 i)Cefaclor Monohydrate Antibiotic- In respiratory April-1991 250mg/500mg Capsule. infections, ENT infection, UT ii)Cefaclor Monohydrate infections, Skin and skin 125mg/5ml & 250mg/5ml structure infections. Suspension. iii)Cefaclor Monohydrate 100mg/ml Drops. iv)Cefaclor 187mg/5ml Suspension (For paediatric use). 4 Sheep Pox Vaccine (For April-1991 Veterinary) 5 Omeprazole 10mg/20mg Short term treatment of April-1991 Enteric Coated Granules duodenal ulcer, gastric ulcer, Capsule reflux oesophagitis, management of Zollinger- Ellison syndrome. 6 i)Nefopam Hydrochloride Non narcotic analgesic- Acute April-1991 30mg Tablet. and chronic pain, including ii)Nefopam Hydrochloride post-operative pain, dental 20mg/ml Injection. pain, musculo-skeletal pain, acute traumatic pain and cancer pain. 7 Buparvaquone 5% w/v Indicated in the treatment of April-1991 Solution for Injection (For bovine theileriosis. Veterinary) 8 i)Kitotifen Fumerate 1mg Anti asthmatic drug- Indicated May-1991 Tablet in prophylactic treatment of ii)Kitotifen Fumerate Syrup bronchial asthma, symptomatic iii)Ketotifen Fumerate Nasal improvement of allergic Drops conditions including rhinitis and conjunctivitis. 9 i)Pefloxacin Mesylate Antibacterial- In the treatment May-1991 Dihydrate 400mg Film Coated of severe infection in adults Tablet caused by sensitive ii)Pefloxacin Mesylate microorganism (gram -ve Dihydrate 400mg/5ml Injection pathogens and staphylococci). iii)Pefloxacin Mesylate Dihydrate 400mg I.V Bottles of 100ml/200ml 10 Ofloxacin 100mg/50ml & Indicated in RTI, UTI, May-1991 200mg/100ml vial Infusion gynaecological infection, skin/soft lesion infection. -

Comparison of the Antiischaemic and Antianginal Effects of Nicorandil and Amlodipine in Patients with Symptomatic Stable Angina Pectoris: the SWAN Study
Journal of Clinical and Basic Cardiology An Independent International Scientific Journal Journal of Clinical and Basic Cardiology 1999; 2 (2), 213-217 Comparison of the antiischaemic and antianginal effects of nicorandil and amlodipine in patients with symptomatic stable angina pectoris: the SWAN study The SWAN Study Group Homepage: www.kup.at/jcbc Online Data Base Search for Authors and Keywords Indexed in Chemical Abstracts EMBASE/Excerpta Medica Krause & Pachernegg GmbH · VERLAG für MEDIZIN und WIRTSCHAFT · A-3003 Gablitz/Austria ORIGINAL PAPERS, CLINICAL The SWAN study J Clin Basic Cardiol 1999; 2: 213 Comparison of the antiischaemic and antianginal effects of nicorandil and amlodipine in patients with symptomatic stable angina pectoris: the SWAN study The SWAN Study Group1 This multicentre, double-blind, randomised study compared the antiischaemic and antianginal effects of nicorandil and amlodipine in patients with symptomatic stable angina pectoris. Nicorandil is a new coronary and balanced peripheral vasodilating agent that operates through two mechanisms of action: activation of ATP-dependent K-channels and stimulation of guanylate cyclase. A total of 121 patients with symptomatic stable angina pectoris were randomised to receive nicorandil 10 mg twice daily (bd) or amlodipine 5 mg once daily (od) for 8 weeks (optional dosage increase after 2-4 weeks to 20 mg bd and 10 mg od, respec- tively). Symptom-limited exercise tolerance tests were performed at baseline, and after 2 and 8 weeks treatment, respectively. In addition, the number of anginal attacks, nitroglycerin (NTG) usage, blood pressure (BP), heart rate (HR) and adverse events were recorded, and a subjective assessment of quality of life performed. -

Prochlorperazine 5Mg Tablets
Package leaflet: Information for the patient Prochlorperazine 5mg tablets Read all of this leaflet carefully before you start taking this • the person is a child. This is because children may develop unusual face and body medicine, because it contains important information for you. movements (dystonic reactions) • Keep this leaflet. You may need to read it again. • you are diabetic or have high levels of sugar in your blood (hyperglycaemia). Your doctor • If you have any further questions, ask your doctor or pharmacist. may want to monitor you more closely. • This medicine has been prescribed for you only. Do not pass it on to If you are not sure if any of the above apply to you, talk to your doctor or pharmacist before others. It may harm them, even if their signs of illness are the same taking Prochlorperazine Tablets. as yours. Other medicines and Prochlorperazine tablets • If you get any side effects, talk to your doctor or pharmacist. Tell your doctor or pharmacist if you are taking, have recently taken or might take any This includes any possible side effects not listed in this leaflet. other medicines. This includes medicines you buy without a prescription, including herbal See section 4. medicines. This is because Prochlorperazine Tablets can affect the way some other medicines work. What is in this leaflet: Also some medicines can affect the way Prochlorperazine Tablets work. 1 What Prochlorperazine tablets are and what they In particular, tell your doctor if you are taking any of the following: • medicines to help you sleep -

Investigating the Influence of Polymers on Supersaturated
Page 1 of 45 Molecular Pharmaceutics 1 2 3 4 5 6 7 Investigating the Influence of Polymers on 8 9 10 11 12 Supersaturated Flufenamic Acid Cocrystal Solutions 13 14 15 16 1 1 2 2 1 17 Minshan Guo , Ke Wang , Noel Hamill , Keith Lorimer and Mingzhong Li * 18 19 20 1School of pharmacy, De Montfort University, Leicester, UK 21 22 23 2Almac Science, Seagoe Industrial Estate, Craigavon, UK 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 55 56 57 58 59 60 ACS Paragon Plus Environment 1 Molecular Pharmaceutics Page 2 of 45 1 2 3 4 5 6 7 Table of contents graphic 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 55 56 57 58 59 60 ACS Paragon Plus Environment 2 Page 3 of 45 Molecular Pharmaceutics 1 2 3 Abstract 4 5 6 7 The development of enabling formulations is a key stage when demonstrating the effectiveness 8 9 10 of pharmaceutical cocrystals to maximize the oral bioavailability for poorly water soluble drugs. 11 12 Inhibition of drug crystallization from a supersaturated cocrystal solution through a fundamental 13 14 understanding of the nucleation and crystal growth is important. In this study, the influence of 15 16 17 the three polymers of polyethylene glycol (PEG), polyvinylpyrrolidone (PVP) and a copolymer 18 19 of N-vinly-2-pyrrodidone (60%) and vinyl acetate (40%) (PVP-VA) on the flufenamic acid 20 21 22 (FFA) crystallization from three different supersaturated solutions of the pure FFA and two 23 24 cocrystals of FFA-NIC CO and FFA-TP CO has been investigated by measuring nucleation 25 26 induction times and desupersaturation rates in the presence and absence of seed crystals. -

PACKAGE LEAFLET: INFORMATION for the USER Lercanidipine
PACKAGE LEAFLET: INFORMATION FOR THE USER Lercanidipine Hydrochloride 10 mg Film-coated Tablets Lercanidipine Hydrochloride 20 mg Film-coated Tablets lercanidipine hydrochloride Read all of this leaflet carefully before you start using this medicine because it contains important information for you. - Keep this leaflet. You may need to read it again. - If you have any further questions, ask your doctor or pharmacist. - This medicine has been prescribed for you only. Do not pass it on to others. It may harm them, even if their signs of illness are the same as yours. - If you get any of the side effects talk to your doctor or pharmacist. This includes any possible side effects not listed in this leaflet. See section 4. What is in this leaflet: 1. What Lercanidipine Hydrochloride Film-coated Tablets is and what it is used for 2. What you need to know before you take Lercanidipine Hydrochloride Film-coated Tablets 3. How to take Lercanidipine Hydrochloride Film-coated Tablets 4. Possible side effects 5. How to store Lercanidipine Hydrochloride Film-coated Tablets 6. Contents of the pack and other information 1. WHAT LERCANIDIPINE HYDROCHLORIDE FILM-COATED TABLETS IS AND WHAT IT IS USED FOR Lercanidipine belongs to a group of medicines called calcium channel blockers (dihydropyridine derivatives) that lower blood pressure.. Lercanidipine is used to treat high blood pressure also known as hypertension in adults over the age of 18 years (it is not recommended for children under 18 years old). 2. WHAT YOU NEED TO KNOW BEFORE YOU TAKE LERCANIDIPINE -

Optum Essential Health Benefits Enhanced Formulary PDL January
PENICILLINS ketorolac tromethamineQL GENERIC mefenamic acid amoxicillin/clavulanate potassium nabumetone amoxicillin/clavulanate potassium ER naproxen January 2016 ampicillin naproxen sodium ampicillin sodium naproxen sodium CR ESSENTIAL HEALTH BENEFITS ampicillin-sulbactam naproxen sodium ER ENHANCED PREFERRED DRUG LIST nafcillin sodium naproxen DR The Optum Preferred Drug List is a guide identifying oxacillin sodium oxaprozin preferred brand-name medicines within select penicillin G potassium piroxicam therapeutic categories. The Preferred Drug List may piperacillin sodium/ tazobactam sulindac not include all drugs covered by your prescription sodium tolmetin sodium drug benefit. Generic medicines are available within many of the therapeutic categories listed, in addition piperacillin sodium/tazobactam Fenoprofen Calcium sodium to categories not listed, and should be considered Meclofenamate Sodium piperacillin/tazobactam as the first line of prescribing. Tolmetin Sodium Amoxicillin/Clavulanate Potassium LOW COST GENERIC PREFERRED For benefit coverage or restrictions please check indomethacin your benefit plan document(s). This listing is revised Augmentin meloxicam periodically as new drugs and new prescribing LOW COST GENERIC naproxen kit information becomes available. It is recommended amoxicillin that you bring this list of medications when you or a dicloxacillin sodium CARDIOVASCULAR covered family member sees a physician or other penicillin v potassium ACE-INHIBITORS healthcare provider. GENERIC QUINOLONES captopril ANTI-INFECTIVES -

Effect of Felodipine Against Pilocarpine Induced Seizures in Rats
Int. J. Pharm. Sci. Rev. Res., 52(1), September - October 2018; Article No. 10, Pages: 54-60 ISSN 0976 – 044X Research Article Effect of Felodipine against Pilocarpine induced Seizures in Rats Osama Q. Fadheel 1, Faruk H. AL-Jawad 1, Waleed K. Abdulsahib 2, Haider F. Ghazi 3 1Pharmacology Department, College of Medicine, Al-Nahrain University, Baghdad, Iraq. 2Pharmacy department, Al- Farahidi University College, Baghdad, Iraq. 3Microbiology Department, College of Medicine, Al-Nahrain University, Iraq. *Corresponding author’s E-mail: [email protected] Received: 25-07-2018; Revised: 22-08-2018; Accepted: 05-09-2018. ABSTRACT Epilepsy is a standout amongst the most well-known genuine cerebrum issue, can happen at all ages. The examination was performed to investigate the conceivable antiepileptic impact of Felodipine against pilocarpine prompted seizure in male rats. The investigation did on forty male Wister rats similarly assigned to four gathering: (1) typical gathering (not got any medication). Gathering (2) negative control gathering (got just pilocarpine amid acceptance of seizure. Gathering (3) positive control gathering (Valproic corrosive gathering got 20 mg/kg orally twice every day). Gathering (4) Felodipine gathering (1 mg/kg got orally once every day). Rats of each gathering (aside from typical gathering) were infused intraperitoneal with pilocarpine hydrochloride (400 mg/kg) following 21 long stretches of tried medications organization orally. The mean beginning and term of seizure were resolved to assess the viability of tried medications and to contrast these impact and that of typical gathering and Valproic corrosive gathering. Additionally, neuroprotective impact (Neu N), NMDA receptor, Sodium diverts were estimated in all gatherings. -

Summary of Product Characteristics, Labelling and Package Leaflet
SUMMARY OF PRODUCT CHARACTERISTICS, LABELLING AND PACKAGE LEAFLET 1 SUMMARY OF PRODUCT CHARACTERISTICS 2 1. NAME OF THE MEDICINAL PRODUCT /.../ 10 mg film-coated tablet /.../ 20 mg film-coated tablet 2. QUALITATIVE AND QUANTITATIVE COMPOSITION One film-coated tablet contains 10 mg lercanidipine hydrochloride, equivalent to 9.4 mg lercanidipine. One film-coated tablet contains 20 mg lercanidipine hydrochloride, equivalent to 18.8 mg lercanidipine. Excipient with known effect: /.../ 10 mg film-coated tablet: Lactose monohydrate 30 mg Excipient with known effect: /.../ 20 mg film-coated tablet: Lactose monohydrate 60 mg For the full list of excipients, see section 6.1. 3. PHARMACEUTICAL FORM Film--coated tablet /.../ 10 mg film-coated tablet: Yellow, round, biconvex 6.5 mm film-coated tablets, scored on one side, marked 'L' on the other side. /.../ 20 mg film-coated tablet: Pink, round, biconvex 8.5 mm film-coated tablets, scored on one side, marked 'L' on the other side. The score line is only to facilitate breaking for ease of swallowing and not to divide into equal doses. 4. CLINICAL PARTICULARS 4.1 Therapeutic indications /.../ is indicated for the treatment of mild to moderate essential hypertension. 4.2 Posology and method of administration Posology Route of administration: For oral use. The recommended dosage is 10 mg orally once a day at least 15 minutes before meals; the dose may be increased to 20 mg depending on the individual patient's response. Dose titration should be gradual, because it may take about 2 weeks before the maximal antihypertensive effect is apparent. Some individuals, not adequately controlled on a single antihypertensive agent, may benefit from the addition of lercandipine to therapy with a beta-adrenoreceptor blocking drug, a diuretic (hydrochlorothiazide) or an angiotensin converting enzyme inhibitor. -

Tall Man Lettering List REPORT DECEMBER 2013 1
Tall Man Lettering List REPORT DECEMBER 2013 1 TALL MAN LETTERING LIST REPORT WWW.HQSC.GOVT.NZ Published in December 2013 by the Health Quality & Safety Commission. This document is available on the Health Quality & Safety Commission website, www.hqsc.govt.nz ISBN: 978-0-478-38555-7 (online) Citation: Health Quality & Safety Commission. 2013. Tall Man Lettering List Report. Wellington: Health Quality & Safety Commission. Crown copyright ©. This copyright work is licensed under the Creative Commons Attribution-No Derivative Works 3.0 New Zealand licence. In essence, you are free to copy and distribute the work (including other media and formats), as long as you attribute the work to the Health Quality & Safety Commission. The work must not be adapted and other licence terms must be abided. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nd/3.0/nz/ Copyright enquiries If you are in doubt as to whether a proposed use is covered by this licence, please contact: National Medication Safety Programme Team Health Quality & Safety Commission PO Box 25496 Wellington 6146 ACKNOWLEDGEMENTS The Health Quality & Safety Commission acknowledges the following for their assistance in producing the New Zealand Tall Man lettering list: • The Australian Commission on Safety and Quality in Health Care for advice and support in allowing its original work to be either reproduced in whole or altered in part for New Zealand as per its copyright1 • The Medication Safety and Quality Program of Clinical Excellence Commission, New South -

Management of Major Depressive Disorder Clinical Practice Guidelines May 2014
Federal Bureau of Prisons Management of Major Depressive Disorder Clinical Practice Guidelines May 2014 Table of Contents 1. Purpose ............................................................................................................................................. 1 2. Introduction ...................................................................................................................................... 1 Natural History ................................................................................................................................. 2 Special Considerations ...................................................................................................................... 2 3. Screening ........................................................................................................................................... 3 Screening Questions .......................................................................................................................... 3 Further Screening Methods................................................................................................................ 4 4. Diagnosis ........................................................................................................................................... 4 Depression: Three Levels of Severity ............................................................................................... 4 Clinical Interview and Documentation of Risk Assessment............................................................... -

Solifenacin Succinate Tablets PI
465mm (18.31”) 32mm (1.26”) HIGHLIGHTS OF PRESCRIBING • Gastrointestinal Disorders: Use with 3 DOSAGE FORMS AND STRENGTHS Table 1. Percentages of Patients With Identified Adverse Reactions, Derived From Multiple dose studies of solifenacin succinate in elderly volunteers (65 to 80 years) FDA Approved Patient Labeling FDA Approved Patient Labeling INFORMATION caution in patients with decreased Solifenacin succinate tablets are available as follows: All Adverse Events Exceeding Placebo Rate and Reported by 1% or More Patients showed that Cmax, AUC and t1/2 values were 20 to 25% higher as compared to the These highlights do not include gastrointestinal motility (5.3) 5 mg – white, round, standard, normal convex, film-coated, unscored tablets, debossed for Combined Pivotal Studies younger volunteers (18 to 55 years). Solifenacin Succinate Tablets Solifenacin Succinate Tablets all the information needed to • Central Nervous System Effects: with “TV” on one side of the tablet and with “2N” on the other side of the tablet. Placebo Solifenacin Succinate Solifenacin Succinate 8.6 Renal Impairment Read the Patient Information that comes with Read the Patient Information that comes with use SOLIFENACIN SUCCINATE Somnolence has been reported with 10 mg – light-pink to pink, round, standard, normal convex, film-coated, unscored (%) 5 mg (%) 10 mg (%) Solifenacin succinate should be used with caution in patients with renal impairment. TABLETS safely and effectively. solifenacin succinate tablets before you start solifenacin succinate tablets before you start solifenacin succinate. Advise patients not tablets, debossed with “TV” on one side of the tablet and with “3N” on the other side Number of Patients 1216 578 1233 There is a 2.1 fold increase in AUC and 1.6 fold increase in t1/2 of solifenacin in patients See full prescribing information for to drive or operate heavy machinery until of the tablet. -

Package Leaflet: Information for the User Hydroxyzine Bluefish 25 Mg
Package leaflet: Information for the user Hydroxyzine Bluefish 25 mg film-coated tablets hydroxyzine hydrochloride Read all of this leaflet carefully before you start using this medicine because it contains important information for you. - Keep this leaflet. You may need to read it again. - If you have any further questions, ask your doctor or pharmacist. - This medicine has been prescribed for you only. Do not pass it on to others. It may harm them, even if their signs of illness are the same as yours. - If you get any side effects, talk to your doctor or pharmacist. This includes any possible side effects not listed in this leaflet. See section 4. What is in this leaflet 1. What Hydroxyzine Bluefish is and what it is used for 2. What you need to know before you use Hydroxyzine Bluefish 3. How to use Hydroxyzine Bluefish 4. Possible side effects 5. How to store Hydroxyzine Bluefish 6. Contents of the pack and other information 1. What Hydroxyzine Bluefish is and what it is used for Hydroxyzine Bluefish blocks histamine, a substance found in body tissues. It is effective against anxiety, itching and urticaria. Hydroxyzine Bluefish is used to treat anxiety in adults itching (pruritus) associated with hives (urticaria) in adults adolescents and children of 5 years and above 2. What you need to know before you take Hydroxyzine Bluefish Do not take Hydroxyzine Bluefish - if you are allergic to hydroxyzine hydrochloride or any of the other ingredients of this medicine (listed in section 6) - if you are allergic (hypersensitive) to cetirizine, aminophylline, ethylenediamine or piperazine derivatives (closely related active substances of other medicines).