Upper Extremity Function in Persons with Tetraplegia: Relationships
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Myelopathy—Paresis and Paralysis in Cats
Myelopathy—Paresis and Paralysis in Cats (Disorder of the Spinal Cord Leading to Weakness and Paralysis in Cats) Basics OVERVIEW • “Myelopathy”—any disorder or disease affecting the spinal cord; a myelopathy can cause weakness or partial paralysis (known as “paresis”) or complete loss of voluntary movements (known as “paralysis”) • Paresis or paralysis may affect all four limbs (known as “tetraparesis” or “tetraplegia,” respectively), may affect only the rear legs (known as “paraparesis” or “paraplegia,” respectively), the front and rear leg on the same side (known as “hemiparesis” or “hemiplegia,” respectively) or only one limb (known as “monoparesis” or “monoplegia,” respectively) • Paresis and paralysis also can be caused by disorders of the nerves and/or muscles to the legs (known as “peripheral neuromuscular disorders”) • The spine is composed of multiple bones with disks (intervertebral disks) located in between adjacent bones (vertebrae); the disks act as shock absorbers and allow movement of the spine; the vertebrae are named according to their location—cervical vertebrae are located in the neck and are numbered as cervical vertebrae one through seven or C1–C7; thoracic vertebrae are located from the area of the shoulders to the end of the ribs and are numbered as thoracic vertebrae one through thirteen or T1–T13; lumbar vertebrae start at the end of the ribs and continue to the pelvis and are numbered as lumbar vertebrae one through seven or L1–L7; the remaining vertebrae are the sacral and coccygeal (tail) vertebrae • The brain -

Non-Ketotic Hyperglycaemia and the Hemichorea- Hemiballismus
This open-access article is distributed under ARTICLE Creative Commons licence CC-BY-NC 4.0. Non-ketotic hyperglycaemia and the hemichorea- hemiballismus syndrome – a rare paediatric presentation M P K Hauptfleisch, MB BCh, MMed Paeds, FCPaed (SA), Cert Paed Neuro (SA); J L Rodda, MB BCh, FCPaed (SA) Department of Paediatrics, Faculty of Health Sciences, University of the Witwatersrand, Johannesburg, South Africa and Chris Hani Baragwanath Academic Hospital, Johannesburg, Africa Corresponding author: M P K Hauptfleisch ([email protected]) Hemichorea-hemiballismus may be due to non-ketotic hyperglycaemia, but this condition has rarely been described in paediatrics. We describe the case of a 13-year-old girl with newly diagnosed type 1 diabetes and acute onset of left-sided choreoathetoid movements. Neuroimaging revealed an area of hyperintensity in the right basal ganglia. Her blood glucose level at the time was 19 mmol/L, and there was no ketonuria. The hemiballismus improved with risperidone and glycaemic control. Repeat neuroimaging 4 months later showed complete resolution of the hyperintensities seen. S Afr J Child Health 2018;12(4):134-136. DOI:10.7196/SAJCH.2018.v12i4.1535 Non-ketotic hyperglycaemic hemichorea-hemiballismus (NKHHC) is a rare, reversible condition, with the clinical and radiological signs usually resolving within 6 months, following correction of hyperglycaemia.[1] The condition has previously been described as specifically affecting the elderly, with very few cases described in children and adolescents.[2] We describe a paediatric patient presenting with the classic clinical and radiological findings of NKHHC. Case A 13-year-old female presented to hospital with severe cramps in her left hand. -

Four Effective and Feasible Interventions for Hemi-Inattention
University of Puget Sound Sound Ideas School of Occupational Master's Capstone Projects Occupational Therapy, School of 5-2016 Four Effective and Feasible Interventions for Hemi- inattention Post CVA: Systematic Review and Collaboration for Knowledge Translation in an Inpatient Rehab Setting. Elizabeth Armbrust University of Puget Sound Domonique Herrin University of Puget Sound Christi Lewallen University of Puget Sound Karin Van Duzer University of Puget Sound Follow this and additional works at: http://soundideas.pugetsound.edu/ot_capstone Part of the Occupational Therapy Commons Recommended Citation Armbrust, Elizabeth; Herrin, Domonique; Lewallen, Christi; and Van Duzer, Karin, "Four Effective and Feasible Interventions for Hemi-inattention Post CVA: Systematic Review and Collaboration for Knowledge Translation in an Inpatient Rehab Setting." (2016). School of Occupational Master's Capstone Projects. 4. http://soundideas.pugetsound.edu/ot_capstone/4 This Article is brought to you for free and open access by the Occupational Therapy, School of at Sound Ideas. It has been accepted for inclusion in School of Occupational Master's Capstone Projects by an authorized administrator of Sound Ideas. For more information, please contact [email protected]. INTERVENTIONS FOR HEMI-INATTENTION IN INPATIENT REHAB Four Effective and Feasible Interventions for Hemi-inattention Post CVA: Systematic Review and Collaboration for Knowledge Translation in an Inpatient Rehab Setting. May 2016 This evidence project, submitted by Elizabeth Armbrust, -
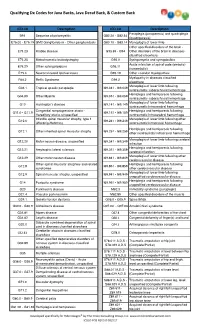
ICD-10 Backs
Qualifying Dx Codes for Java Backs, Java Decaf Back, & Custom Back ICD-10 Description ICD-10 Description Paraplegia (paraparesis) and quadriplegia B91 Sequelae of poliomyelitis G82.20 - G82.54 (quadriparesis) E75.00 - E75.19 GM2 Gangliosidosis - Other gangliosidosis G83.10 - G83.14 Monoplegia of lower limb Other specified disorders of the brain - E75.23 Krabbe disease G93.89 - G94 Other disorders of the brain in diseases classified elsewhere E75.25 Metachromatic leukodystrophy G95.0 Syringomyelia and syringobulbia Acute infarction of spinal code (embolic) E75.29 Other sphingolipidosis G95.11 (nonembolic) E75.4 Neuronal ceroid lipofuscinosis G95.19 Other vascular myelopathies Myelopathy in diseases classified F84.2 Rett's Syndrome G99.2 elsewhere Monoplegia of lower limb following G04.1 Tropical spastic paraplegia I69.041 - I69.049 nontraumatic subarachnoid hemorrhage Hemiplegia and hemiparesis following G04.89 Other Myelitis I69.051 - I69.059 nontraumatic subarachnoid hemorrhage Monoplegia of lower limb following G10 Huntington's disease I69.141 - I69.149 nontraumatic intracerebral hemorrhage Congenital nonprogressive ataxia - Hemiplegia and hemiparesis following G11.0 - G11.9 I69.151 - I69.159 Hereditary ataxia, unspecified nontraumatic intracerebral hemorrhage Infantile spinal muscular atrophy, type 1 Monoplegia of lower limb following other G12.0 I69.241 - I69.249 (Werdnig-Hoffman) nontraumatic intracranial hemorrhage Hemiplegia and hemiparesis following G12.1 Other inherited spinal muscular atrophy I69.251 - I69.259 other nontraumatic -

Traumatic Hemiparesis Associated with Type III Klippel-Feil Syndrome
online ML Comm www.jkns.or.kr J Korean Neurosurg Soc 42 : 145-148, 2007 Case Report Traumatic Hemiparesis Associated with Jin-Kyu Park, M.D. Type III Klippel-Feil Syndrome Han-Yong Huh, M.D. Kyeong-Sik Ryu, M.D. Chun-Kun Park, M.D. Klippel-Feil Syndrome (KFS) is a complex congenital syndrome of osseous and visceral anomalies. It is mainly associated with multi-level cervical spine fusion with hypermobile normal segments. Therefore, a patient with KFS can be at risk of severe neurological symptoms even after a minor trauma. We report a patient with type III KFS who developed a hemiparesis after a minor trauma and was successfully managed with operation. KEY WORDS : Hemiparesis·Klippel-Feil Syndrome·Trauma. INTRODUCTION Department of Neurosurgery In 1912, Klippel and Feil first described a syndrome that consisted of a clinical triad of short Kangnam St. Mary’s Hospital The Catholic University of Korea neck, limitation in head and neck movements and low posterior hairline. Currently, this Seoul, Korea syndrome called Klippel-Feil syndrome (KFS) is referred to a congenital fusion of two or more vertebrae7). Multi-level fused cervical vertebrae may become symptomatic during the rapid growth of adolescence or in adult life by the entrapment of the brain and/or the spinal cord. The classification of KFS is based on the site and extent of the cervical fusion9). Type I is applied to patients with an extensive cervical and upper thoracic spinal fusion. Type II refers to patients with one or two interspace fusions, often associated with hemivertebrae and occipitio- atlantal fusions. -

Cerebellar Disease in the Dog and Cat
CEREBELLAR DISEASE IN THE DOG AND CAT: A LITERATURE REVIEW AND CLINICAL CASE STUDY (1996-1998) b y Diane Dali-An Lu BVetMed A thesis submitted for the degree of Master of Veterinary Medicine (M.V.M.) In the Faculty of Veterinary Medicine University of Glasgow Department of Veterinary Clinical Studies Division of Small Animal Clinical Studies University of Glasgow Veterinary School A p ril 1 9 9 9 © Diane Dali-An Lu 1999 ProQuest Number: 13815577 All rights reserved INFORMATION TO ALL USERS The quality of this reproduction is dependent upon the quality of the copy submitted. In the unlikely event that the author did not send a com plete manuscript and there are missing pages, these will be noted. Also, if material had to be removed, a note will indicate the deletion. uest ProQuest 13815577 Published by ProQuest LLC(2018). Copyright of the Dissertation is held by the Author. All rights reserved. This work is protected against unauthorized copying under Title 17, United States C ode Microform Edition © ProQuest LLC. ProQuest LLC. 789 East Eisenhower Parkway P.O. Box 1346 Ann Arbor, Ml 48106- 1346 GLASGOW UNIVERSITY lib ra ry ll5X C C ^ Summary SUMMARY________________________________ The aim of this thesis is to detail the history, clinical findings, ancillary investigations and, in some cases, pathological findings in 25 cases of cerebellar disease in dogs and cats which were presented to Glasgow University Veterinary School and Hospital during the period October 1996 to June 1998. Clinical findings were usually characteristic, although the signs could range from mild tremor and ataxia to severe generalised ataxia causing frequent falling over and difficulty in locomotion. -

Reach and Palmar Grasp in Tetraplegics with Neuromuscular Electrical Stimulation
REACH AND PALMAR GRASP IN TETRAPLEGICS WITH NEUROMUSCULAR ELECTRICAL STIMULATION ALCANCE E PREENSÃO PALMAR EM TETRAPLÉGICOS COM ESTIMULAÇÃO ELÉTRICA NEUROMUSCULAR ORIGINAL ARTICLE ARTIGO ORIGINAL ALCANCE Y PRENSIÓN PALMAR EN TETRAPLÉJICOS CON ESTIMULACIÓN ELÉCTRICA NEUROMUSCULAR ARTÍCULO ORIGINAL Enio Walker Azevedo Cacho1 ABSTRACT (Physiotherapist) Roberta de Oliveira Cacho1 Objective: To evaluate the movement strategies of quadriplegics, assisted by neuromuscular electrical stimulation, (Physiotherapist) on reach and palmar grasp using objects of different weights. Methods: It was a prospective clinical trial. Four chronic Rodrigo Lício Ortolan2 quadriplegics (C5-C6), with injuries of traumatic origin, were recruited and all of them had their reach and palmar grasp (Electrical Engineer) movement captured by four infrared cameras and six retro-reflective markers attached to the trunk and right arm, as- 1 Núbia Maria Freire Vieira Lima sisted or not by neuromuscular electrical stimulation to the triceps, extensor carpi radialis longus, extensor digitorum (Physiotherapist) communis, flexor digitorum superficialis, opponens pollicis and lumbricals. It was measured by a Neurological and Edson Meneses da Silva Filho1 (Physiotherapist) Functional Classification of Spinal Cord Injuries of the American Spinal Injury Association, Functional Independence Alberto Cliquet Jr3,4 Measure and kinematic variables. Results: The patients were able to reach and execute palmar grasp in all cylinders (Electronics Engineer) using the stimulation sequences assisted by neuromuscular electrical stimulation. The quadriplegics produced lower peak velocity, a shorter time of movement and reduction in movement segmentation, when assisted by neuromuscular 1. Universidade Federal do Rio electrical stimulation. Conclusion: This study showed that reach and palmar grasp movement assisted by neuromuscular Grande do Norte, Faculdade de Ciências de Saúde do Trairi, electrical stimulation was able to produce motor patterns more similar to healthy subjects. -

Hemiballismus: /Etiology and Surgical Treatment by Russell Meyers, Donald B
J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.13.2.115 on 1 May 1950. Downloaded from J. Neurol. Neurosurg. Psychiat., 1950, 13, 115. HEMIBALLISMUS: /ETIOLOGY AND SURGICAL TREATMENT BY RUSSELL MEYERS, DONALD B. SWEENEY, and JESS T. SCHWIDDE From the Division of Neurosurgery, State University of Iowa, College ofMedicine, Iowa City, Iowa Hemiballismus is a relatively uncommon hyper- 1949; Whittier). A few instances are on record in kinesia characterized by vigorous, extensive, and which the disorder has run an extended chronic rapidly executed, non-patterned, seemingly pur- course (Touche, 1901 ; Marcus and Sjogren, 1938), poseless movements involving one side of the body. while in one case reported by Lea-Plaza and Uiberall The movements are almost unceasing during the (1945) the abnormal movements are said to have waking state and, as with other hyperkinesias con- ceased spontaneously after seven weeks. Hemi- sidered to be of extrapyramidal origin, they cease ballismus has also been known to cease following during sleep. the supervention of a haemorrhagic ictus. Clinical Aspects Terminology.-There appears to be among writers on this subject no agreement regarding the precise Cases are on record (Whittier, 1947) in which the Protected by copyright. abnormal movements have been confined to a single features of the clinical phenomena to which the limb (" monoballismus ") or to both limbs of both term hemiballismus may properly be applied. sides (" biballismus ") (Martin and Alcock, 1934; Various authors have credited Kussmaul and Fischer von Santha, 1932). In a majority of recorded (1911) with introducing the term hemiballismus to instances, however, the face, neck, and trunk as well signify the flinging or flipping character of the limb as the limbs appear to have been involved. -

PREVENTING SECONDARY MEDICAL COMPLICATIONS: a Guide for Personal Assistants to People with Spinal Cord Injury
PREVENTING SECONDARY MEDICAL COMPLICATIONS: A Guide for Personal Assistants to People with Spinal Cord Injury Medical Rehabilitation Research and Training Center in Secondary Complications in Spinal Cord Injury SPAIN REHABILITATION CENTER University of Alabama at Birmingham Preventing Secondary Medical Complications: A Guide For Personal Assistants to People With Spinal Cord Injury Developed by: Medical Rehabilitation Research and Training Center in Secondary Complications in Spinal Cord Injury Training Office Department of Physical Medicine and Rehabilitation Spain Rehabilitation Center University of Alabama at Birmingham Acknowledgment Our thanks to the following individuals who helped us in the development of this booklet: Lorraine Arrington Judy Matthews Brenda Bass Margaret A. Nosek, PhD Betty Bass Scott and Donna Sartain Cathy Crawford, RD Drenda Scroggin Charles Cowan Anna Smith Allan Drake Brenda Smith David Felton Susan Smith, RN,BSN Peg Hale, RN,BSN Nita Straiton Bobbie Kent Donna Thornton Phillip Klebine Frank Wilkinson C.J. and Cindy Luster Larrie Waters c 1992, Revised 1996, The Board of Trustees of the University of Alabama This publication is supported in part by a grant (#H133B30025) from the National Institute on Disability and Rehabilitation Research, Department of Education, Washington, D.C. 20202. Opinions expressed in this document are not necessarily those of the granting agency. The University of Alabama at Birmingham administers its educational programs and activities, including admissions, without regard to race, color, religion, sex, national origin, handicap or Vietnam era or disabled veteran status. (Title IX of the Education Amendments of 1972 specifically prohibits discrimination on the basis of sex.) Direct inquires to Academic Affirmative Action Officer, The University of Alabama at Birmingham, UAB Station, Birmingham, Alabama, 35294. -

When Normal Multi-Joint Movement Synergies Become Pathologic Marco Santello Arizona State University at the Tempe Campus
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2015 Are movement disorders and sensorimotor injuries pathologic synergies? When normal multi-joint movement synergies become pathologic Marco Santello Arizona State University at the Tempe Campus Catherine E. Lang Washington University School of Medicine in St. Louis Follow this and additional works at: https://digitalcommons.wustl.edu/open_access_pubs Recommended Citation Santello, Marco and Lang, Catherine E., ,"Are movement disorders and sensorimotor injuries pathologic synergies? When normal multi-joint movement synergies become pathologic." Frontiers in Human Neuroscience.8,. 1050. (2015). https://digitalcommons.wustl.edu/open_access_pubs/3648 This Open Access Publication is brought to you for free and open access by Digital Commons@Becker. It has been accepted for inclusion in Open Access Publications by an authorized administrator of Digital Commons@Becker. For more information, please contact [email protected]. REVIEW ARTICLE published: 06 January 2015 HUMAN NEUROSCIENCE doi: 10.3389/fnhum.2014.01050 Are movement disorders and sensorimotor injuries pathologic synergies? When normal multi-joint movement synergies become pathologic Marco Santello1* and Catherine E. Lang 2 1 Neural Control of Movement Laboratory, School of Biological and Health Systems Engineering, Arizona State University, Tempe, AZ, USA 2 Program in Physical Therapy, Program in Occupational Therapy, Department of Neurology, Washington University School of Medicine in St. Louis, St. Louis, MO, USA Edited by: The intact nervous system has an exquisite ability to modulate the activity of multiple mus- Ana Bengoetxea, Universidad del País cles acting at one or more joints to produce an enormous range of actions. Seemingly Vasco-Euskal Herriko Unibertsitatea, Spain simple tasks, such as reaching for an object or walking, in fact rely on very complex spatial Reviewed by: and temporal patterns of muscle activations. -

Rapidly Progressive Tetraplegia and Cognitive Deterioration During Rehabilitation: a Case of Neurodegenerative Disease
J Surg Med. 2019;3(1):100-102. Case report DOI: 10.28982/josam.454181 Olgu sunumu Rapidly progressive tetraplegia and cognitive deterioration during rehabilitation: A case of neurodegenerative disease Rehabilitasyon sırasında hızlı ilerleyen tetrapleji ve bilişsel bozulma: Bir nörodejeneratif hastalık olgusu Sevgi İkbali Afşar 1, Oya Ümit Yemişçi 1 1 Department of Physical Medicine and Abstract Rehabilitation, Baskent University, Human prion diseases are fatal, progressive neurodegenerative disorders caused by neurolytic pathogen proteins, called Faculty of Medicine, Ankara, Turkey prions. The most common human prion disease is sporadic Creutzfeldt-Jakob disease, with an approximate annual prevalence of 0.5-1 per million. The symptoms and signs include rapidly progressive dementia, ataxia, myoclonic ORCID ID of the authors SİA: 0000-0002-4003-3646 seizures, akinetic mutism and other neurological and neurobehavioral disorders. The clinical spectrum of Creutzfeldt- OÜY: 0000-0002-0501-5127 Jakob disease is highly variable; therefore it can be difficult to diagnose premortem. This article describes a 78-year- old woman who initially presented with difficulty walking and balance disorder. As a result of the evaluation, the patient was transferred to rehabilitation clinic, with a diagnosis of cervical spinal stenosis. During hospitalization, she showed progressive decline in gait and balance and deteriorated rapidly. The patient was considered to be probable sporadic Creutzfeldt-Jakob disease after further investigations. Keywords: Neurodegenerative disease, Creutzfeldt-Jakob disease, Rehabilitation Öz Corresponding author / Sorumlu yazar: İnsan prion hastalıkları, prionlar olarak adlandırılan nörolitik patojen proteinlerin neden olduğu ilerleyici Sevgi İkbali Afşar Address / Adres: Fevzi Cakmak Cad. 5. Sokak nörodejeneratif hastalıklardır. En yaygın insan prion hastalığı sporadik Creutzfeldt-Jakob hastalığı olup, yıllık No: 48, 06490, Ankara, Türkiye prevalansı yaklaşık milyonda 0.5-1'dir. -

Mechanisms of Injury in Dyskinetic Cerebral Palsy
Mechanisms of Injury in Dyskinetic Cerebral Palsy Alec Hoon, MD Associate Professor of Pediatrics Johns Hopkins University School of Medicine Director, Phelps Center for Cerebral Palsy Kennedy Krieger Institute Neurodevelopmental Evaluation Structure‐Function Genetic, Epigenetic, Clinical Phenotype Abnormalities Environmental Risk Factors CP Diagnosis Etiologic Diagnosis Child‐Family Rehabilitative Characteristics Management Medical Surgical Measurement CAM Cell‐Based therapy Techniques Outcome Key Concepts in Cerebral Palsy • Motor control‐ tone, posture, movement • 2‐3/1000 children • Risk factors include infection, inflammation, low birth weight, prematurity, genetic • Secondary to brain dysgenesis or injury • “Non‐progressive”‐ manifestations can change • Unilateral and bilateral phenotypes • A range of associated disorders • Etiology links to phenotype links to treatment 1 Cerebral Palsy‐ Clinical Phenotypes CEREBRAL PALSY Spastic Dyskinetic Ataxic Hypotonia Bilateral Unilateral Hypertonic Hyperkinetic Spastic Diplegia Hemiplegia Dystonic Rigid Dystonic Tetraplegia Quadriplegia Athetosis Chorea Hemiballismus Cascade of events in brain injury 1. Prenatal antecedents may be suspected‐(Freud) 2. Final common pathways often involve hypoxia‐ ischemia and infection‐inflammation 3. Injury may have a protracted time course 4. Injury may lead to myelin abnormalities, reduced plasticity and decreased cell number 5. Injury changes both developmental trajectory and may sensitive brain to later injury The Evolving Nature of Injury TIME