Ototoxic Medications (Mustargen)
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Rheumatoid Arthritis (1 of 23)
Rheumatoid Arthritis (1 of 23) 1 Patient presents w/ signs & symptoms of rheumatoid arthritis (RA) 2 4 DIAGNOSIS No Is RA confi rmed? ALTERNATIVE DIAGNOSIS Yes A Pharmacological therapy • Conventional synthetic disease-modifying anti-rheumatic drug (DMARD) (csDMARD) monotherapy [Methotrexate (preferred), Lefl unomide or Sulfasalazine] • Adjunctive therapy [corticosteroids, nonsteroidal anti-infl ammatory drugs (NSAIDs)] B Non-pharmacological therapy 3 CONTINUE TREATMENT Symptoms improved Yes • at 3 mth & treatment goal Consider decreasing achieved at 6 mth? dose if in sustained remission No A Pharmacological therapy A Add any one of the Pharmacological following: therapy 3 • TNF inhibitor1 or • Change to or add a No Yes • Non-TNF second csDMARD Are poor prognostic factors 1 B present? biological or Non-pharmacological • Jak-inhibitor therapy MIMS B Non- pharmacological therapy TREATMENT © See next page 1In patients who cannot use csDMARDs as comedication, interleukin-6 receptor antagonists & targeted synthetic DMARDs (tsDMARDs) have some advantages over other biological DMARDs (bDMARDs) Not all products are available or approved for above use in all countries. Specifi c prescribing information may be found in the latest MIMS. B105 © MIMS 2020 Rheumatoid Arthritis (2 of 23) TREATMENT OF PATIENTS W/ POOR PROGNOSTIC FACTORS CONT’D CONTINUE 3 TREATMENT RHEUMATOID ARTHRITIS RHEUMATOID Symptoms improved • Yes Consider decreasing at 3 mth & treatment goal dose or increasing achieved at 6 mth? interval if in sustained remission No A Pharmacological therapy • Switch to another TNF inhibitor or non-TNF biological1 or • Jak-inhibitor B Non-pharmacological therapy 3 Symptoms improved Yes at 3 mth & treatment goal achieved at 6 mth? No 1In patients who failed one TNF inhibitor therapy, considerMIMS giving a second TNF inhibitor or changing to an agent from a diff erent class © Not all products are available or approved for above use in all countries. -
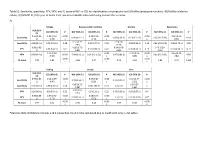

Table S1: Sensitivity, Specificity, PPV, NPV, and F1 Score of NLP Vs. ICD for Identification of Symptoms for (A) Biome Developm
Table S1: Sensitivity, specificity, PPV, NPV, and F1 score of NLP vs. ICD for identification of symptoms for (A) BioMe development cohort; (B) BioMe validation cohort; (C) MIMIC-III; (D) 1 year of notes from patients in BioMe calculated using manual chart review. A) Fatigue Nausea and/or vomiting Anxiety Depression NLP (95% ICD (95% CI) P NLP (95% CI) ICD (95% CI) P NLP (95% CI) ICD (95% CI) P NLP (95% CI) ICD (95% CI) P CI) 0.99 (0.93- 0.59 (0.43- <0.00 0.25 (0.12- <0.00 <0.00 0.54 (0.33- Sensitivity 0.99 (0.9 – 1) 0.98 (0.88 -1) 0.3 (0.15-0.5) 0.85 (0.65-96) 0.02 1) 0.73) 1 0.42) 1 1 0.73) 0.57 (0.29- 0.9 (0.68- Specificity 0.89 (0.4-1) 0.75 (0.19-1) 0.68 0.97 (0.77-1) 0.03 0.98 (0.83-1) 0.22 0.81 (0.53-0.9) 0.96 (0.79-1) 0.06 0.82) 0.99) 0.99 (0.92- 0.86 (0.71- 0.94 (0.79- 0.79 (0.59- PPV 0.96 (0.82-1) 0.3 0.95 (0.66-1) 0.02 0.95 (0.66-1) 0.16 0.93 (0.68-1) 0.12 1) 0.95) 0.99) 0.92) 0.13 (0.03- <0.00 0.49 (0.33- <0.00 0.66 (0.48- NPV 0.89 (0.4-1) 0.007 0.94 (0.63-1) 0.34 (0.2-0.51) 0.97 (0.81-1) 0.86 (0.6-0.95) 0.04 0.35) 1 0.65) 1 0.81) <0.00 <0.00 <0.00 F1 Score 0.99 0.83 0.88 0.57 0.95 0.63 0.82 0.79 0.002 1 1 1 Itching Cramp Pain NLP (95% ICD (95% CI) P NLP (95% CI) ICD (95% CI) P NLP (95% CI) ICD (95% CI) P CI) 0.98 (0.86- 0.24 (0.09- <0.00 0.09 (0.01- <0.00 0.52 (0.37- <0.00 Sensitivity 0.98 (0.85-1) 0.99 (0.93-1) 1) 0.45) 1 0.29) 1 0.66) 1 0.89 (0.72- 0.5 (0.37- Specificity 0.96 (0.8-1) 0.98 (0.86-1) 0.68 0.98 (0.88-1) 0.18 0.5 (0-1) 1 0.98) 0.66) 0.88 (0.69- PPV 0.96 (0.8-1) 0.8 (0.54-1) 0.32 0.8 (0.16-1) 0.22 0.99 (0.93-1) 0.98 (0.87-1) NA* 0.97) 0.98 (0.85- 0.57 (0.41- <0.00 0.58 (0.43- <0.00 NPV 0.98 (0.86-1) 0.5 (0-1) 0.02 (0-0.08) NA* 1) 0.72) 1 0.72) 1 <0.00 <0.00 <0.00 F1 Score 0.97 0.56 0.91 0.28 0.99 0.68 1 1 1 *Denotes 95% confidence intervals and P values that could not be calculated due to insufficient cells in 2x2 tables. -

Profile Profile Profile Profile
127 4. Berl et al. Mechanism of allergic contact dermatitis from Piroxin; Fr. : Brexin; Cycladol; Feldene; Geldene; Inflacedt; 3-(4-[2-(1-p-Chlorobenzoyl-5-methoxy,2-methylindol-3-yia V, Proxalyoc; Zofora; Ger.: Brexidolt; Flexaset; Pirobeta; Piroflam; propacetamol: sensitization to activated N,N-diethylglycine. Contad cetoxy)eth)'i}piperazln-1-yl)propyt '4cbenzamldo-N,N,dipro 38: Pirox; Gr. : Bleduran; Brexin; Calmopyrol; Conzila; Feldene; Dermatitis I998; 185-8. pylglutaramate dimaieate. 5. Hersch M, et al. Effect of intravenous propacetamol on blood pressure in Fidinor; Flodeneu; Grecotens; Inflamase�N; Neo Axedil; Nilvo; febrile critically patients. Pharmacotherapy 2008; 28: I205-IO. Oximezin; Painrelipt�D; Pedifan; Propanol; Pyrcost; Reumaplus; 076.6 ill C�,HsaCIN50s,2C;H,04� 1 Ruvamed; Sinartrol; Valopon; Zerospasm; Zitumex; Hong Kong: Porphyria. The Drug Database for Acute Porphyria, com cinc� s ·-,57,�32�53�3 {,orogh:meracin); 59209-40-4 (.orogturn'eta CP-Pirox; Feldene; Mobilist; Piram-Dt; Piroxicat; Sefdene; piled by the Norwegian Porphyria Centre (NAPOS) and Synoxicamt; Vidapirocamt; Hung. : Brexin; Feldene; Flamexin; maleate). the Porphyria Centre Sweden, classifies propacetamol as Hotemin; Pirorheumt; India: Amida; Brexic; Camrox; Camsun; ATC - MOIA814. probably not porphyrinogenic; it may be used as a drug of Cycladol; Dolocare; Dolocip; Dolodil; Dolokam; Dololup; Dolo� ATC vet - 0MO/A8l4. first choice and no precautions are needed.1 nex; Dolopir; Doloswift; Dupox; Estcom; Felcam; Feldex; Flex� UN!/ - F2PUN24B8C ar; Kemonex; Lincitrax; Medicam; Meloxi; Micropec; Mobicam; I. The Drug Database for Acute Porphyria. Available at: http:l/www. drugs-porphyria.org (accessed II !10/11) Mobidin; Movon; Noxicam-MD; Pam; Panorox; Pirox; Suganril; ; Profile Indon.: Faxident; Felcam; Feldene; Infeld; Kifadene; Lanareu Proglumetacin maleate, an indoleacetic add derivative P epa at ons ma; Licofel; Maxicamt; Pirocam; Pirodenet; Pirofel; Rexicam; .........r r .......i ............... -

)&F1y3x PHARMACEUTICAL APPENDIX to THE
)&f1y3X PHARMACEUTICAL APPENDIX TO THE HARMONIZED TARIFF SCHEDULE )&f1y3X PHARMACEUTICAL APPENDIX TO THE TARIFF SCHEDULE 3 Table 1. This table enumerates products described by International Non-proprietary Names (INN) which shall be entered free of duty under general note 13 to the tariff schedule. The Chemical Abstracts Service (CAS) registry numbers also set forth in this table are included to assist in the identification of the products concerned. For purposes of the tariff schedule, any references to a product enumerated in this table includes such product by whatever name known. Product CAS No. Product CAS No. ABAMECTIN 65195-55-3 ACTODIGIN 36983-69-4 ABANOQUIL 90402-40-7 ADAFENOXATE 82168-26-1 ABCIXIMAB 143653-53-6 ADAMEXINE 54785-02-3 ABECARNIL 111841-85-1 ADAPALENE 106685-40-9 ABITESARTAN 137882-98-5 ADAPROLOL 101479-70-3 ABLUKAST 96566-25-5 ADATANSERIN 127266-56-2 ABUNIDAZOLE 91017-58-2 ADEFOVIR 106941-25-7 ACADESINE 2627-69-2 ADELMIDROL 1675-66-7 ACAMPROSATE 77337-76-9 ADEMETIONINE 17176-17-9 ACAPRAZINE 55485-20-6 ADENOSINE PHOSPHATE 61-19-8 ACARBOSE 56180-94-0 ADIBENDAN 100510-33-6 ACEBROCHOL 514-50-1 ADICILLIN 525-94-0 ACEBURIC ACID 26976-72-7 ADIMOLOL 78459-19-5 ACEBUTOLOL 37517-30-9 ADINAZOLAM 37115-32-5 ACECAINIDE 32795-44-1 ADIPHENINE 64-95-9 ACECARBROMAL 77-66-7 ADIPIODONE 606-17-7 ACECLIDINE 827-61-2 ADITEREN 56066-19-4 ACECLOFENAC 89796-99-6 ADITOPRIM 56066-63-8 ACEDAPSONE 77-46-3 ADOSOPINE 88124-26-9 ACEDIASULFONE SODIUM 127-60-6 ADOZELESIN 110314-48-2 ACEDOBEN 556-08-1 ADRAFINIL 63547-13-7 ACEFLURANOL 80595-73-9 ADRENALONE -

Objective Measures of Ototoxicity
The following article appeared in the September 2005 issue (Vol. 9, No. 1, pp. 10-16) of the Division 6 publication Perspectives on Hearing and Hearing Disorders: Research and Diagnostics. To learn more about Division 6, contact the ASHA Action Center at 1-800-498-2071 or visit the division’s Web page at www.asha.org/about/membership-certification/divs/div_6.htm. Objective Measures of Ototoxicity Elizabeth Leigh-Paffenroth Veterans Affairs Rehabilitation Research and Development Service, National Center for Rehabilitative Auditory Research, VA Medical Center Portland, OR Department of Otolaryngology, Oregon Health & Science University Portland, OR Kelly M. Reavis, Jane S. Gordon, Kathleen T. Dunckley Veterans Affairs Rehabilitation Research and Development Service, National Center for Rehabilitative Auditory Research, VA Medical Center Portland, OR Stephen A. Fausti and Dawn Konrad-Martin Veterans Affairs Rehabilitation Research and Development Service, National Center for Rehabilitative Auditory Research, VA Medical Center Portland, OR Department of Otolaryngology, Oregon Health & Science University, Portland, OR A leading cause of preventable sensorineural hear- of patients who are unable to provide reliable re- ing loss is therapeutic treatment with medications that sponses; subsequently, many of these patients do not are toxic to inner ear tissues, including certain drugs receive monitoring for ototoxic-induced changes in used to fight cancer and life-threatening infectious dis- their hearing. The development of objective measures eases. Ototoxic-induced hearing loss typically begins that do not require patient cooperation is necessary to in the high frequencies and progresses to lower fre- monitor all patients receiving ototoxic drugs. quencies as drug administration continues (Campbell Two objective measures offer promise in their abil- & Durrant, 1993; Campbell et al., 2003; Macdonald, ity to detect and to monitor hearing changes caused by Harrison, Wake, Bliss, & Macdonald, 1994). -
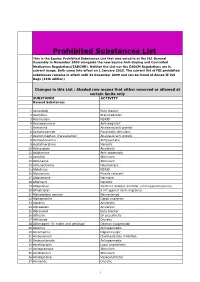
Prohibited Substances List
Prohibited Substances List This is the Equine Prohibited Substances List that was voted in at the FEI General Assembly in November 2009 alongside the new Equine Anti-Doping and Controlled Medication Regulations(EADCMR). Neither the List nor the EADCM Regulations are in current usage. Both come into effect on 1 January 2010. The current list of FEI prohibited substances remains in effect until 31 December 2009 and can be found at Annex II Vet Regs (11th edition) Changes in this List : Shaded row means that either removed or allowed at certain limits only SUBSTANCE ACTIVITY Banned Substances 1 Acebutolol Beta blocker 2 Acefylline Bronchodilator 3 Acemetacin NSAID 4 Acenocoumarol Anticoagulant 5 Acetanilid Analgesic/anti-pyretic 6 Acetohexamide Pancreatic stimulant 7 Acetominophen (Paracetamol) Analgesic/anti-pyretic 8 Acetophenazine Antipsychotic 9 Acetylmorphine Narcotic 10 Adinazolam Anxiolytic 11 Adiphenine Anti-spasmodic 12 Adrafinil Stimulant 13 Adrenaline Stimulant 14 Adrenochrome Haemostatic 15 Alclofenac NSAID 16 Alcuronium Muscle relaxant 17 Aldosterone Hormone 18 Alfentanil Narcotic 19 Allopurinol Xanthine oxidase inhibitor (anti-hyperuricaemia) 20 Almotriptan 5 HT agonist (anti-migraine) 21 Alphadolone acetate Neurosteriod 22 Alphaprodine Opiod analgesic 23 Alpidem Anxiolytic 24 Alprazolam Anxiolytic 25 Alprenolol Beta blocker 26 Althesin IV anaesthetic 27 Althiazide Diuretic 28 Altrenogest (in males and gelidngs) Oestrus suppression 29 Alverine Antispasmodic 30 Amantadine Dopaminergic 31 Ambenonium Cholinesterase inhibition 32 Ambucetamide Antispasmodic 33 Amethocaine Local anaesthetic 34 Amfepramone Stimulant 35 Amfetaminil Stimulant 36 Amidephrine Vasoconstrictor 37 Amiloride Diuretic 1 Prohibited Substances List This is the Equine Prohibited Substances List that was voted in at the FEI General Assembly in November 2009 alongside the new Equine Anti-Doping and Controlled Medication Regulations(EADCMR). -

S1 Table. List of Medications Analyzed in Present Study Drug
S1 Table. List of medications analyzed in present study Drug class Drugs Propofol, ketamine, etomidate, Barbiturate (1) (thiopental) Benzodiazepines (28) (midazolam, lorazepam, clonazepam, diazepam, chlordiazepoxide, oxazepam, potassium Sedatives clorazepate, bromazepam, clobazam, alprazolam, pinazepam, (32 drugs) nordazepam, fludiazepam, ethyl loflazepate, etizolam, clotiazepam, tofisopam, flurazepam, flunitrazepam, estazolam, triazolam, lormetazepam, temazepam, brotizolam, quazepam, loprazolam, zopiclone, zolpidem) Fentanyl, alfentanil, sufentanil, remifentanil, morphine, Opioid analgesics hydromorphone, nicomorphine, oxycodone, tramadol, (10 drugs) pethidine Acetaminophen, Non-steroidal anti-inflammatory drugs (36) (celecoxib, polmacoxib, etoricoxib, nimesulide, aceclofenac, acemetacin, amfenac, cinnoxicam, dexibuprofen, diclofenac, emorfazone, Non-opioid analgesics etodolac, fenoprofen, flufenamic acid, flurbiprofen, ibuprofen, (44 drugs) ketoprofen, ketorolac, lornoxicam, loxoprofen, mefenamiate, meloxicam, nabumetone, naproxen, oxaprozin, piroxicam, pranoprofen, proglumetacin, sulindac, talniflumate, tenoxicam, tiaprofenic acid, zaltoprofen, morniflumate, pelubiprofen, indomethacin), Anticonvulsants (7) (gabapentin, pregabalin, lamotrigine, levetiracetam, carbamazepine, valproic acid, lacosamide) Vecuronium, rocuronium bromide, cisatracurium, atracurium, Neuromuscular hexafluronium, pipecuronium bromide, doxacurium chloride, blocking agents fazadinium bromide, mivacurium chloride, (12 drugs) pancuronium, gallamine, succinylcholine -

Preventing Hearing Loss Caused by Chemical (Ototoxicity) and Noise Exposure
Preventing Hearing Loss Caused by Chemical (Ototoxicity) and Noise Exposure Safety and Health Information Bulletin SHIB 03-08-2018 DHHS (NIOSH) Publication No. 2018-124 Introduction Millions of workers are exposed to noise in the workplace every day and when uncontrolled, noise exposure may cause permanent hearing loss. Research demonstrates exposure to certain chemicals, called ototoxicants, may cause hearing loss or balance problems, regardless of noise exposure. Substances including certain pesticides, solvents, and pharmaceuticals that contain ototoxicants can negatively affect how the ear functions, causing hearing loss, and/or affect balance. Source/Copyright: OSHA The risk of hearing loss is increased when workers are exposed to these chemicals while working around elevated noise levels. This combination often results in hearing loss that can be temporary or permanent, depending on the level of noise, the dose of the chemical, and the duration of the exposure. This hearing impairment affects many occupations and industries, from machinists to firefighters. Effects on Hearing Harmful exposure to ototoxicants may occur through inhalation, ingestion, or skin absorption. Health effects caused by ototoxic chemicals vary based on exposure frequency, intensity, duration, workplace exposure to other hazards, and individual factors such as age. Effects may be temporary or permanent, can affect hearing sensitivity and result in a standard threshold shift. Since chemicals can affect central portions of the auditory system (e.g., nerves or nuclei in the central nervous system, the pathways to the brain or in the brain itself), not only do sounds need to be louder to be detected, but also they lose clarity. Specifically, speech discrimination dysfunction, the ability to hear voices separately from background noise, may occur and involve: . -

(19) 11 Patent Number: 6165500
USOO6165500A United States Patent (19) 11 Patent Number: 6,165,500 Cevc (45) Date of Patent: *Dec. 26, 2000 54 PREPARATION FOR THE APPLICATION OF WO 88/07362 10/1988 WIPO. AGENTS IN MINI-DROPLETS OTHER PUBLICATIONS 75 Inventor: Gregor Cevc, Heimstetten, Germany V.M. Knepp et al., “Controlled Drug Release from a Novel Liposomal Delivery System. II. Transdermal Delivery Char 73 Assignee: Idea AG, Munich, Germany acteristics” on Journal of Controlled Release 12(1990) Mar., No. 1, Amsterdam, NL, pp. 25–30. (Exhibit A). * Notice: This patent issued on a continued pros- C.E. Price, “A Review of the Factors Influencing the Pen ecution application filed under 37 CFR etration of Pesticides Through Plant Leaves” on I.C.I. Ltd., 1.53(d), and is subject to the twenty year Plant Protection Division, Jealott's Hill Research Station, patent term provisions of 35 U.S.C. Bracknell, Berkshire RG12 6EY, U.K., pp. 237-252. 154(a)(2). (Exhibit B). K. Karzel and R.K. Liedtke, “Mechanismen Transkutaner This patent is Subject to a terminal dis- Resorption” on Grandlagen/Basics, pp. 1487–1491. (Exhibit claimer. C). Michael Mezei, “Liposomes as a Skin Drug Delivery Sys 21 Appl. No.: 07/844,664 tem” 1985 Elsevier Science Publishers B.V. (Biomedical Division), pp 345-358. (Exhibit E). 22 Filed: Apr. 8, 1992 Adrienn Gesztes and Michael Mazei, “Topical Anesthesia of 30 Foreign Application Priority Data the Skin by Liposome-Encapsulated Tetracaine” on Anesth Analg 1988; 67: pp 1079–81. (Exhibit F). Aug. 24, 1990 DE) Germany ............................... 40 26834 Harish M. Patel, "Liposomes as a Controlled-Release Sys Aug. -

Protocol Synopsis
Risk of Upper Gastrointestinal Complications in Users of Nonsteroidal Anti-inflammatory Drugs Study Protocol—V2.0 (Final) October 19, 2009 Prepared by Jordi Castellsague Susana Perez-Gutthann RTI Health Solutions E-mail: [email protected] Federica Pisa, MD, MStat Fabio Barbone, MD, DrPH Udine University, AOUD Udine Institute of Hygiene and Epidemiology E-mail: [email protected] RTI-HS Project No.: 0301655 PROTOCOL APPROVAL SIGNATURE PAGE Project Title : Risk of Upper Gastrointestinal Complications in Users ofNonsteroidal Anti-inflammatory Drugs RTI-HS Project 0301655 Final Appro val Date: October 22,2009 Authors: Jordi Castellsague, MD, MPH; Susana Perez-Gutthann, MD, PhD (RTI HS) Fede rica Pisa, MD, MStat; Fabio Barbone, MD, DrPH (Udine University, AOUD Udine) Version: Version 2.0 Final Version Date: October 19, 2009 The following people have reviewed the protocol and give their approval: Susana Perez-Gutthann, MD, PhD Date Global Head Epidemiology RTI Health Solutions / Fabio Barbone, MD, D H Signature Date Director, Institute of Hygiene and Epidemiology University of Udine ii TABLE OF CONTENTS 1 STUDY SYNOPSIS ............................................................................................ 1 2 BACKGROUND ................................................................................................. 4 3 KEY ROLES AND RESPONSIBILITIES ............................................................ 5 3.1.1 Financial Sponsorship .................................................................................................... -

Why Is Drug-Induced Ototoxicity Still Not Preventable Nor Is It Treatable in 2019? - a Literature Review of Aminoglycoside and Cisplatin Ototoxicity Cherrabi Kaoutar*
Review Article iMedPub Journals Archives of Medicine 2020 www.imedpub.com Vol.12 No.2:3 ISSN 1989-5216 DOI: 10.36648/1989-5216.12.2.304 Why is Drug-Induced Ototoxicity Still Not Preventable nor is it Treatable in 2019? - A Literature Review of Aminoglycoside and Cisplatin Ototoxicity Cherrabi Kaoutar* Department of Oto-Rhino-Laryngology and Cervico-Facial Studies, Fez, Morocco *Corresponding author: Cherrabi Kaoutar, Resident, Department of Oto-Rhino-Laryngology and Cervico-Facial Studies, Fez, Morocco, Tel: 0679382957; E-mail: [email protected] Received date: October 17, 2019; Accepted date: March 02, 2019; Published date: March 09, 2020 Citation: Cherrabi K (2020) Why is Drug-Induced Ototoxicity Still Not Preventable nor is it Treatable in 2019? - A Literature Review of Aminoglycoside and Cisplatin Ototoxicity. Arch Med Vol: 12 Iss: 2:3 Copyright: ©2020 Cherrabi K. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. The thorough exploration of inner ear proteome, transcriptome, and genome in physiological and Abstract pathological contexts as potential biomarkers of early stages of cell lesions: The clinical application would not Oto-toxicity is defined by cochlear and or vestibular only allow a more specific understanding of different cellular lesions due to the use of drugs. The difference in mechanisms of iatrogenic oto-toxicity, but also allow new specific mechanisms, the great semi logical variability, the insights into targeted protective and post-lesional heterogeneity of incriminated drugs, the inaccessibility to therapies. -

Concomitant Use of Nsaids Or Ssris with Noacs Requires Monitoring for Bleeding
Original Article Yonsei Med J 2020 Sep;61(9):741-749 https://doi.org/10.3349/ymj.2020.61.9.741 pISSN: 0513-5796 · eISSN: 1976-2437 Concomitant Use of NSAIDs or SSRIs with NOACs Requires Monitoring for Bleeding Min-Taek Lee1, Kwang-Yeol Park2, Myo-Song Kim1, Seung-Hun You1, Ye-Jin Kang1, and Sun-Young Jung1 1College of Pharmacy, Chung-Ang University, Seoul; 2Department of Neurology, Chung-Ang University Hospital, Chung-Ang University College of Medicine, Seoul, Korea. Purpose: Non-vitamin K antagonist oral anticoagulants (NOACs) are widely used in patients with atrial fibrillation (AF) because of their effectiveness in preventing stroke and their better safety, compared with warfarin. However, there are concerns for an in- creased risk of bleeding associated with concomitant use of non-steroidal anti-inflammatory drugs (NSAIDs) or selective sero- tonin reuptake inhibitors (SSRIs) with NOACs. In this study, we aimed to evaluate the risk of bleeding events in individuals taking concomitant NSAIDs or SSRIs with NOACs after being diagnosed with AF. Materials and Methods: A nested case-control analysis to assess the safety of NSAIDs and SSRIs among NOAC users with AF was performed using data from Korean National Health Insurance Service from January 2012 to December 2017. Among patients who were newly prescribed NOACs, 1233 cases hospitalized for bleeding events were selected, and 24660 controls were determined. Results: The risk of bleeding events was higher in patients receiving concomitant NSAIDs [adjusted odds ratio (aOR) 1.41; 95% confidence interval (CI) 1.24–1.61] or SSRIs (aOR 1.92; 95% CI 1.52–2.42) with NOACs, compared to no use of either drug, respec- tively.