Detailed Review Paper on Rotavirus Vaccines
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

(ACIP) General Best Guidance for Immunization
8. Altered Immunocompetence Updates This section incorporates general content from the Infectious Diseases Society of America policy statement, 2013 IDSA Clinical Practice Guideline for Vaccination of the Immunocompromised Host (1), to which CDC provided input in November 2011. The evidence supporting this guidance is based on expert opinion and arrived at by consensus. General Principles Altered immunocompetence, a term often used synonymously with immunosuppression, immunodeficiency, and immunocompromise, can be classified as primary or secondary. Primary immunodeficiencies generally are inherited and include conditions defined by an inherent absence or quantitative deficiency of cellular, humoral, or both components that provide immunity. Examples include congenital immunodeficiency diseases such as X- linked agammaglobulinemia, SCID, and chronic granulomatous disease. Secondary immunodeficiency is acquired and is defined by loss or qualitative deficiency in cellular or humoral immune components that occurs as a result of a disease process or its therapy. Examples of secondary immunodeficiency include HIV infection, hematopoietic malignancies, treatment with radiation, and treatment with immunosuppressive drugs. The degree to which immunosuppressive drugs cause clinically significant immunodeficiency generally is dose related and varies by drug. Primary and secondary immunodeficiencies might include a combination of deficits in both cellular and humoral immunity. Certain conditions like asplenia and chronic renal disease also can cause altered immunocompetence. Determination of altered immunocompetence is important to the vaccine provider because incidence or severity of some vaccine-preventable diseases is higher in persons with altered immunocompetence; therefore, certain vaccines (e.g., inactivated influenza vaccine, pneumococcal vaccines) are recommended specifically for persons with these diseases (2,3). Administration of live vaccines might need to be deferred until immune function has improved. -

Candidate Rotavirus Vaccine Recommendations for Consideration by the WHO Strategic Advisory Group of Experts (SAGE) on Immunization
Candidate rotavirus vaccine recommendations for consideration by the WHO Strategic Advisory Group of Experts (SAGE) on Immunization 1. Overall recommendation WHO strongly recommends the inclusion of rotavirus vaccination into the national immunization programmes of all regions of the world. In particular, countries where deaths among children due to diarrhoeal diseases account for ≥10% of under-5 mortality rate should prioritize the introduction of rotavirus vaccination. Countries where deaths among children due to diarrhoeal diseases account for <10% of under-5 mortality rate should also consider the introduction of rotavirus vaccination based on anticipated reduction in mortality and morbidity from diarrhoea, savings in health care costs, and the cost-effectiveness of vaccination. Justification: Rotavirus is a major cause of mortality in countries with high diarrhoeal disease mortality among children under five years of age. Every year, rotavirus gastroenteritis is estimated to cause approximately 527,000 (475,000-580,000) deaths globally among children <5 years old. Most of these deaths occur in developing countries and 90% of the rotavirus- associated fatalities occur in Africa and Asia alone. Globally, >2 million children are hospitalized each year for rotavirus infections. In a recent report of sentinel hospital-based rotavirus surveillance from 35 nations representing each of the six WHO regions between 2001 and 2008, an average of 40% (range= 34%-45%) of hospitalizations for diarrhea among children < 5 years old were attributable to rotavirus infection. 2. Detailed recommendation: Extrapolating efficacy data from a rotavirus vaccine study performed in one population to use of same rotavirus vaccine in other populations Efficacy/effectiveness data from a rotavirus vaccine study performed in a population from one of three under-5 mortality rate categories* can be extrapolated for use in populations in the same under-5 mortality rate category. -

Rotavirus Vaccine: Questions and Answers for Health Care Providers
Rotavirus Vaccine Questions and Answers for Health Care Providers In April 2014, Manitoba Health, Seniors and Active Living launched a publicly-funded Rotavirus Immunization Program for infants born on or after March 1, 2014. In 2018, Manitoba, along with the rest of Canada, switched from RotarixTM to RotaTeq®. As of May 15, 2021, Manitoba has switched back to Rotarix®, for use in its publicly-funded Rotavirus Immunization Program, for infants born on or after April 1, 2021. This document includes an updated list of questions and answers for your reference. 1. Why is there a Rotavirus Immunization Program in Manitoba? 2. Who qualifies for publicly-funded rotavirus vaccine? 3. Which rotavirus vaccine does Manitoba use? 4. Why does the vaccine series need to be completed before eight months of age? 5. How is Rotarix® packaged? 6. How are the oral tube and cap disposed of after use? 7. Should a spit-up dose of vaccine be repeated? 8. Are there any precautions that health care providers should take when administering the oral rotavirus vaccine? 9. Oral rotavirus vaccine contains sucrose in an amount expected to have an effect on immunization injection pain. When should Rotarix® be given in relation to other vaccines to elicit a reduction in pain? 10. How do I administer Rotarix®? 11. Is additional screening for potential contraindications required prior to administering rotavirus vaccine? 12. Can infants born to mothers on immunosuppressive medication be immunized? 13. Are there any issues related to circulating maternal antibodies interfering with the response to the live attenuated vaccine? 14. Are the two rotavirus vaccines, RotaTeq® and Rotarix™, interchangeable? 15. -

Case Studies Controversies in Vaccination
European Review, Vol. 21, No. S1, S56–S61 r 2013 Academia Europæa. The online version of this article is published within an Open Access environment subject to the conditions of the Creative Commons Attribution license ,http://creativecommons.org/licenses/by/3.0/.. doi:10.1017/S1062798713000227 Session 3 – Case Studies Controversies in Vaccination ROMAN PRYMULA University Hospital Hradec Kralove, Sokolska 581, 500 05 Hradec Kralove, Czech Republic. E-mail: [email protected] Infectious diseases still jeopardize human health and even lives. In spite of the variety of advanced treatment methods, prevention is considered to be the most effective way to fight infections, and vaccination, no doubt, is one of the most effective preventive measures in the history of mankind. The vaccine controversy is based on a dispute over morality, ethics, effectiveness, and/or safety. There is no 100% safe or effective vaccine; however, benefits clearly overweigh risks. Ironically, as the numbers of cases of vaccine- preventable infectious diseases are falling, the controversies relating to vaccine safety are growing. Vaccines are generally victims of their own success. Controversies can afflict the positive acceptance of immunization, decrease the coverage and uptake and finally threaten the health of children and adults. The advent of vaccination has proven to be one of the most effective preventive measures in the history of medicine. Vaccines play a significant role in the prevention of debili- tating and, in many cases, life-threatening infectious diseases. Vaccines also provide important benefits in terms of reducing or avoiding costs associated with illness, both direct and indirect. In spite of the absence of any kind of ideal global healthcare system and lack of resources, the World Health Organisation (WHO) and the United Nations Children’s Fund (UNICEF) were able, in 1974, to establish a major global project called the Expanded Programme on Immunization (EPI). -

NSP4)-Induced Intrinsic Apoptosis
viruses Article Viperin, an IFN-Stimulated Protein, Delays Rotavirus Release by Inhibiting Non-Structural Protein 4 (NSP4)-Induced Intrinsic Apoptosis Rakesh Sarkar †, Satabdi Nandi †, Mahadeb Lo, Animesh Gope and Mamta Chawla-Sarkar * Division of Virology, National Institute of Cholera and Enteric Diseases, P-33, C.I.T. Road Scheme-XM, Beliaghata, Kolkata 700010, India; [email protected] (R.S.); [email protected] (S.N.); [email protected] (M.L.); [email protected] (A.G.) * Correspondence: [email protected]; Tel.: +91-33-2353-7470; Fax: +91-33-2370-5066 † These authors contributed equally to this work. Abstract: Viral infections lead to expeditious activation of the host’s innate immune responses, most importantly the interferon (IFN) response, which manifests a network of interferon-stimulated genes (ISGs) that constrain escalating virus replication by fashioning an ill-disposed environment. Interestingly, most viruses, including rotavirus, have evolved numerous strategies to evade or subvert host immune responses to establish successful infection. Several studies have documented the induction of ISGs during rotavirus infection. In this study, we evaluated the induction and antiviral potential of viperin, an ISG, during rotavirus infection. We observed that rotavirus infection, in a stain independent manner, resulted in progressive upregulation of viperin at increasing time points post-infection. Knockdown of viperin had no significant consequence on the production of total Citation: Sarkar, R.; Nandi, S.; Lo, infectious virus particles. Interestingly, substantial escalation in progeny virus release was observed M.; Gope, A.; Chawla-Sarkar, M. upon viperin knockdown, suggesting the antagonistic role of viperin in rotavirus release. Subsequent Viperin, an IFN-Stimulated Protein, studies unveiled that RV-NSP4 triggered relocalization of viperin from the ER, the normal residence Delays Rotavirus Release by Inhibiting of viperin, to mitochondria during infection. -

Rotavirus Fact Sheet
ROTAVIRUS FACT SHEET What is Rotavirus? commonly spreads in families, hospitals, and childcare Rotavirus is a virus that commonly causes inflammation centers. A person with rotavirus disease is most likely to of the stomach and intestines (acute gastroenteritis). spread the virus from the time they are sick through the first 3 days after they recover. Who can get Rotavirus disease? Anyone. However, it is most common in infants and Is there a vaccine for Rotavirus? young children. A person may be infected more than Yes. The vaccine is highly effective at preventing severe once. Nearly every child who is not vaccinated as an rotavirus disease in infants and young children. The infant is expected to be infected within the first years of vaccine is given orally starting at age 2 months as a life. series of 2 doses or 3 doses, depending on the specific type. What are the symptoms of Rotavirus disease? Children with rotavirus disease may have severe watery How can the spread of Rotavirus be prevented? diarrhea, vomiting, fever, abdominal pain, and loss of The virus spreads so easily that frequent handwashing appetite. Vomiting and diarrhea can lead to dehydration. with soap and water is important, but not sufficient for Signs of dehydration include decreased urination, dry controlling the spread of the disease. Rotavirus mouth and throat, and feeling dizzy when standing up. A vaccination is the best way to protect children against child who is dehydrated may have few or no tears when rotavirus disease. crying and be unusually sleepy or fussy. Usually a person’s first infection with rotavirus tends to cause the How is Rotavirus disease treated? most severe symptoms. -

Pink Book Webinar Series: Rotavirus and Hepatitis a Slides
Centers for Disease Control and Prevention National Center for Immunization and Respiratory Diseases Rotavirus and Hepatitis A Pink Book Webinar Series 2018 Mark Freedman, DVM, MPH Veterinary Medical Officer Photographs and images included in this presentation are licensed solely for CDC/NCIRD online and presentation use. No rights are implied or extended for use in printing or any use by other CDC CIOs or any external audiences. Rotavirus: Disease and Vaccine Rotavirus . First identified as a cause of diarrhea in 1973 . Most common cause of severe gastroenteritis in infants and young children . Nearly universal infection by age 5 years . Responsible for up to 500,000 diarrheal deaths each year worldwide Rotavirus . Two important outer shell proteins—VP7, or G-protein, and VP4, or P-protein define the serotype of the virus . From 1996–2005, five predominate strains in the U.S. (G1–G4, G9) accounted for 90% of the isolates . G1 strain accounts for 75% of infections . Very stable and may remain viable for weeks or months if not disinfected Rotavirus Immunity . Antibody against VP7 and VP4 probably important for protection • Cell-mediated immunity probably plays a role in recovery and immunity . First infection usually does not lead to permanent immunity . Reinfection can occur at any age . Subsequent infections generally less severe Rotavirus Clinical Features . Short incubation period . First infection after 3 months of age generally most severe . May be asymptomatic or result in severe, dehydrating diarrhea with fever and vomiting . Gastrointestinal symptoms generally resolve in 3–7 days Rotavirus Complications . Infection can lead to severe diarrhea, dehydration, electrolyte imbalance, and metabolic acidosis . -

RIDA®QUICK Rota/Adeno/Noro Combi Quick Detection of the Three Main Viral Gastroenteritis Agents
R-Biopharm – dedicated to food safety RIDA®QUICK Rota/Adeno/Noro Combi Quick detection of the three main viral gastroenteritis agents • Distinction between Noroviruses of genogroup I and genogroup II • Quick detection of outbreaks and mixed infections • Kit includes ready-to-use stool extraction vials • Simple test execution R-Biopharm – dedicated to food safety The three main viral gastroenteritis agents Despite the introduction of a vaccine, rotavirus is associated gastroenteritis and the third most still the most common cause of severe diarrhea common causal agent of viral gastroenteritis in in children under the age of five. In high-risk children. groups (children, immunosuppressed and elderly One in five cases of acute gastroenteritis worldwide patients) severe forms of disease can occur, making is caused by the norovirus. In developing countries, rotaviruses particularly significant in nosocomial norovirus causes the death of an estimated 50,000 infections in nursery and pediatric wards and children. Norovirus incurs a cost of 60 billion USD intensive care and oncology units. In 2013, an every year in medical care and productivity losses. estimated 215,000 children worldwide died from a rotavirus infection. The use of the RIDA®QUICK Rota/Adeno/Noro Combi, available as a double cassette, allows for Adenoviruses can cause infections of the eyes, quick and sensitive detection of the most significant respiratory or gastrointestinal tract. Types 40/41 of viral gastroenteritis agents. the adenovirus are the major cause of adenovirus- Perspective – Mixed infections In practice, mixed infections involving two or more gastroenteritis agents are often observed. RIDA®QUICK Rota/Adeno/Noro Combi enables rapid detection of single and mixed infections within 15 minutes. -

(Pneumococcal Conjugate Vaccine) Schedule
Changes to the infant pneumococcal conjugate vaccine schedule Information for healthcare practitioners Changes to the infant pneumococcal conjugate vaccine schedule About Public Health England Public Health England exists to protect and improve the nation’s health and wellbeing, and reduce health inequalities. We do this through world-leading science, research, knowledge and intelligence, advocacy, partnerships and the delivery of specialist public health services. We are an executive agency of the Department of Health and Social Care, and a distinct delivery organisation with operational autonomy. We provide government, local government, the NHS, Parliament, industry and the public with evidence-based professional, scientific and delivery expertise and support. Public Health England Wellington House 133-155 Waterloo Road London SE1 8UG Tel: 020 7654 8000 www.gov.uk/phe Twitter: @PHE_uk Facebook: www.facebook.com/PublicHealthEngland For queries relating to this document, please contact: [email protected] © Crown copyright 2019 You may re-use this information (excluding logos) free of charge in any format or medium, under the terms of the Open Government Licence v3.0. To view this licence, visit OGL. Where we have identified any third party copyright information you will need to obtain permission from the copyright holders concerned. Published December 2019 PHE publications PHE supports the UN gateway number: 2019204 Sustainable Development Goals 2 Changes to the infant pneumococcal conjugate vaccine schedule Contents About -
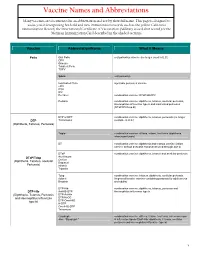
Vaccine Names and Abbreviations Vaccine Names and Abbreviations Many Vaccines Are Documented in an Abbreviation and Not by Their Full Name
Vaccine Names and Abbreviations Vaccine Names and Abbreviations Many vaccines are documented in an abbreviation and not by their full name. This page is designed to assist you in interpreting both old and new immunization records such as the yellow California Immunization Record, the International Certificate of Vaccination (Military issued shot record) or the Mexican Immunization Card described in the shaded sections. Vaccine Abbreviation/Name What it Means Polio Oral Polio oral poliovirus vaccine (no longer used in U.S.) OPV Orimune Trivalent Polio TOPV Sabin oral poliovirus Inactivated Polio injectable poliovirus vaccine eIPV IPOL IPV Pentacel combination vaccine: DTaP/Hib/IPV Pediarix combination vaccine: diphtheria, tetanus, acellular pertussis, Haemophilus influenzae type b and inactivated poliovirus (DTaP/IPV/Hep B) DTP or DPT combination vaccine: diphtheria, tetanus, pertussis (no longer DTP Tri-Immunol available in U.S.) (Diphtheria, Tetanus, Pertussis) Triple combination vaccine: difteria, tétano, tos ferina (diphtheria, tetanus pertussis) DT combination vaccine: diphtheria and tetanus vaccine (infant vaccine without pertussis component used through age 6) DTaP combination vaccine: diphtheria, tetanus and acellular pertussis DTaP/Tdap Acel-Imune Certiva (Diphtheria, Tetanus, acellular Daptacel Pertussis) Infanrix Tripedia Tdap combination vaccine: tetanus, diphtheria, acellular pertussis Adacel (improved booster vaccine containing pertussis for adolescents Boostrix and adults) DTP-Hib combination vaccine: diphtheria, tetanus, -

COVID-19 Vaccine: Critical Questions with Complicated Answers
Review Biomol Ther 29(1), 1-10 (2021) COVID-19 Vaccine: Critical Questions with Complicated Answers Mohammad Faisal Haidere1,†, Zubair Ahmed Ratan2,3,†, Senjuti Nowroz4, Sojib Bin Zaman5, You-Jung Jung6, Hassan Hosseinzadeh2,* and Jae Youl Cho7,* 1Department of Soil, Water and Environment, University of Dhaka, Dhaka 1000, Bangladesh 2School of Health & Society, University of Wollongong, NSW 2500, Australia 3Department of Biomedical Engineering, Khulna University of Engineering and Technology, Khulna 9203, Bangladesh 4Department of Chemistry, University of Dhaka, Dhaka 1000, Bangladesh 5Department of Medicine, School of Clinical Sciences, Monash University, Victoria 3800, Australia 6Biological Resources Utilization Department, National Institute of Biological Resources, Incheon 22689, Republic of Korea 7Department of Integrative Biotechnology, and Biomedical Institute for Convergence at SKKU (BICS), Sungkyunkwan University, Suwon 16419, Republic of Korea Abstract COVID-19 has caused extensive human casualties with significant economic impacts around the globe, and has imposed new challenges on health systems worldwide. Over the past decade, SARS, Ebola, and Zika also led to significant concerns among the scientific community. Interestingly, the SARS and Zika epidemics ended before vaccine development; however, the scholarly com- munity and the pharmaceutical companies responded very quickly at that time. Similarly, when the genetic sequence of SARS- CoV-2 was revealed, global vaccine companies and scientists have stepped forward to develop a vaccine, triggering a race toward vaccine development that the whole world is relying on. Similarly, an effective and safe vaccine could play a pivotal role in eradi- cating COVID-19. However, few important questions regarding SARS-CoV-2 vaccine development are explored in this review. Key Words: COVID-19, Vaccine, Vaccine backfires, Vaccine safety INTRODUCTION vember 2002 in the Guangdong province of China. -

HUMAN ADENOVIRUS Credibility of Association with Recreational Water: Strongly Associated
6 Viruses This chapter summarises the evidence for viral illnesses acquired through ingestion or inhalation of water or contact with water during water-based recreation. The organisms that will be described are: adenovirus; coxsackievirus; echovirus; hepatitis A virus; and hepatitis E virus. The following information for each organism is presented: general description, health aspects, evidence for association with recreational waters and a conclusion summarising the weight of evidence. © World Health Organization (WHO). Water Recreation and Disease. Plausibility of Associated Infections: Acute Effects, Sequelae and Mortality by Kathy Pond. Published by IWA Publishing, London, UK. ISBN: 1843390663 192 Water Recreation and Disease HUMAN ADENOVIRUS Credibility of association with recreational water: Strongly associated I Organism Pathogen Human adenovirus Taxonomy Adenoviruses belong to the family Adenoviridae. There are four genera: Mastadenovirus, Aviadenovirus, Atadenovirus and Siadenovirus. At present 51 antigenic types of human adenoviruses have been described. Human adenoviruses have been classified into six groups (A–F) on the basis of their physical, chemical and biological properties (WHO 2004). Reservoir Humans. Adenoviruses are ubiquitous in the environment where contamination by human faeces or sewage has occurred. Distribution Adenoviruses have worldwide distribution. Characteristics An important feature of the adenovirus is that it has a DNA rather than an RNA genome. Portions of this viral DNA persist in host cells after viral replication has stopped as either a circular extra chromosome or by integration into the host DNA (Hogg 2000). This persistence may be important in the pathogenesis of the known sequelae of adenoviral infection that include Swyer-James syndrome, permanent airways obstruction, bronchiectasis, bronchiolitis obliterans, and steroid-resistant asthma (Becroft 1971; Tan et al.