University of Cincinnati
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Linaclotide: a Novel Therapy for Chronic Constipation and Constipation- Predominant Irritable Bowel Syndrome Brian E
Linaclotide: A Novel Therapy for Chronic Constipation and Constipation- Predominant Irritable Bowel Syndrome Brian E. Lacy, PhD, MD, John M. Levenick, MD, and Michael D. Crowell, PhD, FACG Dr. Lacy is Section Chief of Gastroenter- Abstract: Chronic constipation and irritable bowel syndrome ology and Hepatology and Dr. Levenick (IBS) are functional gastrointestinal disorders that significantly is a Gastroenterology Fellow in the affect patients’ quality of life. Chronic constipation and IBS are Division of Gastroenterology and prevalent—12% of the US population meet the diagnostic crite- Hepatology at Dartmouth-Hitchcock Medical Center in Lebanon, New ria for IBS, and 15% meet the criteria for chronic constipation— Hampshire. Dr. Crowell is a Professor and these conditions negatively impact the healthcare system of Medicine in the Division of from an economic perspective. Despite attempts at dietary Gastroenterology and Hepatology at modification, exercise, or use of over-the-counter medications, Mayo Clinic in Scottsdale, Arizona. many patients have persistent symptoms. Alternative treatment options are limited. This article describes linaclotide (Linzess, Address correspondence to: Dr. Brian E. Lacy Ironwood Pharmaceuticals/Forest Pharmaceuticals), a new, first- Division of Gastroenterology and in-class medication for the treatment of chronic constipation Hepatology, Area 4C and constipation-predominant IBS. Dartmouth-Hitchcock Medical Center 1 Medical Center Drive Lebanon, NH 03756; Tel: 603-650-5215; Fax: 603-650-5225; onstipation is -

A Novel Role for Uroguanylin in the Regulation of Sodium Balance
A novel role for uroguanylin in the regulation of sodium balance Leonard R. Forte J Clin Invest. 2003;112(8):1138-1141. https://doi.org/10.1172/JCI20057. Commentary Uroguanylin is a peptide hormone that regulates sodium excretion by the kidney when excess NaCl is consumed. A new study demonstrates that mice deficient in uroguanylin have blunted urinary sodium excretion responses to oral sodium loads in addition to elevated blood pressure (see related article beginning on page 1244). A physiological role for uroguanylin is discussed, linking the intestine and kidney in an endocrine axis for the maintenance of sodium balance. Find the latest version: https://jci.me/20057/pdf A novel role for uroguanylin in the interest in uroguanylin as a novel play- er in the complex physiological scheme regulation of sodium balance that has evolved to regulate the urinary excretion of sodium chloride and thus Leonard R. Forte to influence sodium balance and blood pressure in the body (7). Medical Research Service, Truman Memorial Veterans Administration Hospital and Radiopharmaceutical Sciences Institute and Department of Medical Pharmacology and Uroguanylin deficiency impairs Physiology, School of Medicine, University of Missouri, Columbia, Missouri, USA sodium excretion Inactivation of uroguanylin genes in Uroguanylin is a peptide hormone that regulates sodium excretion by mice produces an animal model with the kidney when excess NaCl is consumed. A new study demonstrates an impaired capacity to excrete NaCl that mice deficient in uroguanylin have blunted urinary sodium excre- in urine when salt loads are adminis- tion responses to oral sodium loads in addition to elevated blood pres- tered orally (7). -

Role of Phytochemicals in Colon Cancer Prevention: a Nutrigenomics Approach
Role of phytochemicals in colon cancer prevention: a nutrigenomics approach Marjan J van Erk Promotor: Prof. Dr. P.J. van Bladeren Hoogleraar in de Toxicokinetiek en Biotransformatie Wageningen Universiteit Co-promotoren: Dr. Ir. J.M.M.J.G. Aarts Universitair Docent, Sectie Toxicologie Wageningen Universiteit Dr. Ir. B. van Ommen Senior Research Fellow Nutritional Systems Biology TNO Voeding, Zeist Promotiecommissie: Prof. Dr. P. Dolara University of Florence, Italy Prof. Dr. J.A.M. Leunissen Wageningen Universiteit Prof. Dr. J.C. Mathers University of Newcastle, United Kingdom Prof. Dr. M. Müller Wageningen Universiteit Dit onderzoek is uitgevoerd binnen de onderzoekschool VLAG Role of phytochemicals in colon cancer prevention: a nutrigenomics approach Marjan Jolanda van Erk Proefschrift ter verkrijging van graad van doctor op gezag van de rector magnificus van Wageningen Universiteit, Prof.Dr.Ir. L. Speelman, in het openbaar te verdedigen op vrijdag 1 oktober 2004 des namiddags te vier uur in de Aula Title Role of phytochemicals in colon cancer prevention: a nutrigenomics approach Author Marjan Jolanda van Erk Thesis Wageningen University, Wageningen, the Netherlands (2004) with abstract, with references, with summary in Dutch ISBN 90-8504-085-X ABSTRACT Role of phytochemicals in colon cancer prevention: a nutrigenomics approach Specific food compounds, especially from fruits and vegetables, may protect against development of colon cancer. In this thesis effects and mechanisms of various phytochemicals in relation to colon cancer prevention were studied through application of large-scale gene expression profiling. Expression measurement of thousands of genes can yield a more complete and in-depth insight into the mode of action of the compounds. -

Human Genome Center Laboratory of Genome Database Laboratory of Sequence Analysis ゲノムデータベース分野 シークエンスデータ情報処理分野
136 Human Genome Center Laboratory of Genome Database Laboratory of Sequence Analysis ゲノムデータベース分野 シークエンスデータ情報処理分野 Professor Minoru Kanehisa, Ph.D. 教授(委嘱) 理学博士 金 久 實 Research Associate Toshiaki Katayama, M.Sc. 助 手 理学修士 片山俊明 Research Associate Shuichi Kawashima, M.Sc. 助 手 理学修士 川島秀一 Lecturer Tetsuo Shibuya, Ph.D. 講 師 理学博士 渋谷哲朗 Research Associate Michihiro Araki, Ph.D. 助 手 薬学博士 荒木通啓 Owing to continuous developments of high-throughput experimental technologies, ever-increasing amounts of data are being generated in functional genomics and proteomics. We are developing a new generation of databases and computational technologies, beyond the traditional genome databases and sequence analysis tools, for making full use of such large-scale data in biomedical applications, espe- cially for elucidating cellular functions as behaviors of complex interaction systems. 1. Comprehensive repository for community We have been developing the server based on genome annotation open source software including BioRuby, BioPerl, BioDAS and GMOD/GBrowse to make Toshiaki Katayama, Mari Watanabe and Mi- the system consistent with the existing open noru Kanehisa standards. The contents of the KEGG DAS data- base can be accessed graphically in a web KEGG DAS is an advanced genome database browser using GBrowse GUI (graphical user in- system providing DAS (Distributed Annotation terface) and also programatically by the DAS System) service for all organisms in the protocol. The DAS, which is an XML over HTTP GENOME and GENES databases in KEGG data retrieving protocol, enables the user to (Kyoto Encyclopedia of Genes and Genomes). write various kinds of automated programs for Currently, KEGG DAS contains 6,943,951 anno- analyzing genome sequences and annotations. -

Therapeutically Targeting Guanylate
ORIGINAL ARTICLE Therapeutically targeting guanylate cyclase-C: computational modeling of plecanatide, a uroguanylin analog Andrea Brancale1 , Kunwar Shailubhai2, Salvatore Ferla1, Antonio Ricci1, Marcella Bassetto1 & Gary S Jacob2 1School of Pharmacy and Pharmaceutical Sciences, Cardiff University, Cardiff, United Kingdom 2Synergy Pharmaceuticals, New York, New York Keywords Abstract guanylate Cyclase-C, linaclotide, molecular dynamics, plecanatide, uroguanylin Plecanatide is a recently developed guanylate cyclase-C (GC-C) agonist and the first uroguanylin analog designed to treat chronic idiopathic constipation (CIC) Correspondence and irritable bowel syndrome with constipation (IBS-C). GC-C receptors are Andrea Brancale, Cardiff School of Pharmacy found across the length of the intestines and are thought to play a key role in and Pharmaceutical Sciences, Cardiff fluid regulation and electrolyte balance. Ligands of the GC-C receptor include University, Redwood Building, King Edward endogenous agonists, uroguanylin and guanylin, as well as diarrheagenic, VII Avenue, Cardiff, CF10 3NB. Escherichia coli heat-stable enterotoxins (ST). Plecanatide mimics uroguanylin Tel: +44 (0)29 2087 4485; Fax: +44(29) 2087 4149; in its 2 disulfide-bond structure and in its ability to activate GC-Cs in a pH- E-mail: [email protected] dependent manner, a feature associated with the presence of acid-sensing resi- dues (Asp2 and Glu3). Linaclotide, a synthetic analog of STh (a 19 amino acid Funding Information member of ST family), contains the enterotoxin’s key structural elements, Financial Support for this study provided by including the presence of three disulfide bonds. Linaclotide, like STh, activates Synergy Pharmaceuticals Inc. We also GC-Cs in a pH-independent manner due to the absence of pH-sensing residues. -
Supplementary Data
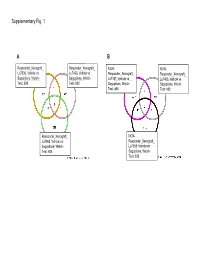
Supplementary Fig. 1 A B Responder_Xenograft_ Responder_Xenograft_ NON- NON- Lu7336, Vehicle vs Lu7466, Vehicle vs Responder_Xenograft_ Responder_Xenograft_ Sagopilone, Welch- Sagopilone, Welch- Lu7187, Vehicle vs Lu7406, Vehicle vs Test: 638 Test: 600 Sagopilone, Welch- Sagopilone, Welch- Test: 468 Test: 482 Responder_Xenograft_ NON- Lu7860, Vehicle vs Responder_Xenograft_ Sagopilone, Welch - Lu7558, Vehicle vs Test: 605 Sagopilone, Welch- Test: 333 Supplementary Fig. 2 Supplementary Fig. 3 Supplementary Figure S1. Venn diagrams comparing probe sets regulated by Sagopilone treatment (10mg/kg for 24h) between individual models (Welsh Test ellipse p-value<0.001 or 5-fold change). A Sagopilone responder models, B Sagopilone non-responder models. Supplementary Figure S2. Pathway analysis of genes regulated by Sagopilone treatment in responder xenograft models 24h after Sagopilone treatment by GeneGo Metacore; the most significant pathway map representing cell cycle/spindle assembly and chromosome separation is shown, genes upregulated by Sagopilone treatment are marked with red thermometers. Supplementary Figure S3. GeneGo Metacore pathway analysis of genes differentially expressed between Sagopilone Responder and Non-Responder models displaying –log(p-Values) of most significant pathway maps. Supplementary Tables Supplementary Table 1. Response and activity in 22 non-small-cell lung cancer (NSCLC) xenograft models after treatment with Sagopilone and other cytotoxic agents commonly used in the management of NSCLC Tumor Model Response type -

From Escherichia Coli Heat-Stable Enterotoxin to Mammalian Endogenous Guanylin Hormones
Brazilian Journal of Medical and Biological Research (2014) 47(3): 179-191, http://dx.doi.org/10.1590/1414-431X20133063 ISSN 1414-431X Review From Escherichia coli heat-stable enterotoxin to mammalian endogenous guanylin hormones A.A.M. Lima1 and M.C. Fonteles1,2 1Unidade de Pesquisas Clı´nicas, Instituto de Biomedicina, Departamento de Fisiologia e Farmacologia, Escola de Medicina, Universidade Federal do Ceara´, Fortaleza, CE, Brasil 2Instituto de Cieˆncias Biome´dicas, Universidade Estadual do Ceara´, Fortaleza, CE, Brasil Abstract The isolation of heat-stable enterotoxin (STa) from Escherichia coli and cholera toxin from Vibrio cholerae has increased our knowledge of specific mechanisms of action that could be used as pharmacological tools to understand the guanylyl cyclase-C and the adenylyl cyclase enzymatic systems. These discoveries have also been instrumental in increasing our understanding of the basic mechanisms that control the electrolyte and water balance in the gut, kidney, and urinary tracts under normal conditions and in disease. Herein, we review the evolution of genes of the guanylin family and STa genes from bacteria to fish and mammals. We also describe new developments and perspectives regarding these novel bacterial compounds and peptide hormones that act in electrolyte and water balance. The available data point toward new therapeutic perspectives for pathological features such as functional gastrointestinal disorders associated with constipation, colorectal cancer, cystic fibrosis, asthma, hypertension, gastrointestinal barrier function damage associated with enteropathy, enteric infection, malnutrition, satiety, food preferences, obesity, metabolic syndrome, and effects on behavior and brain disorders such as attention deficit, hyperactivity disorder, and schizophrenia. Key words: Heat-stable enterotoxin; Guanylin; Guanylyl cyclase; Secretory diarrhea; Kidney function; Electrolyte and water balance Introduction The heat-stable enterotoxin (Sta) from Escherichia coli kidney function using pure STa toxin. -

A Uroguanylin-GUCY2C Endocrine Axis Regulates Feeding in Mice
A uroguanylin-GUCY2C endocrine axis regulates feeding in mice Michael A. Valentino, … , Stephanie Schulz, Scott A. Waldman J Clin Invest. 2011;121(9):3578-3588. https://doi.org/10.1172/JCI57925. Research Article Intestinal enteroendocrine cells are critical to central regulation of caloric consumption, since they activate hypothalamic circuits that decrease appetite and thereby restrict meal size by secreting hormones in response to nutrients in the gut. Although guanylyl cyclase and downstream cGMP are essential regulators of centrally regulated feeding behavior in invertebrates, the role of this primordial signaling mechanism in mammalian appetite regulation has eluded definition. In intestinal epithelial cells, guanylyl cyclase 2C (GUCY2C) is a transmembrane receptor that makes cGMP in response to the paracrine hormones guanylin and uroguanylin, which regulate epithelial cell dynamics along the crypt-villus axis. Here, we show that silencing of GUCY2C in mice disrupts satiation, resulting in hyperphagia and subsequent obesity and metabolic syndrome. This defined an appetite-regulating uroguanylin-GUCY2C endocrine axis, which we confirmed by showing that nutrient intake induces intestinal prouroguanylin secretion into the circulation. The prohormone signal is selectively decoded in the hypothalamus by proteolytic liberation of uroguanylin, inducing GUCY2C signaling and consequent activation of downstream anorexigenic pathways. Thus, evolutionary diversification of primitive guanylyl cyclase signaling pathways allows GUCY2C to coordinate endocrine regulation of central food acquisition pathways with paracrine control of intestinal homeostasis. Moreover, the uroguanylin-GUCY2C endocrine axis may provide a therapeutic target to control appetite, obesity, and metabolic syndrome. Find the latest version: https://jci.me/57925/pdf Research article Related Commentary, page 3384 A uroguanylin-GUCY2C endocrine axis regulates feeding in mice Michael A. -

Peptide Vaccines for Cancers Expressing MPHOSPH1 Or DEPDC1 Polypeptides
(19) & (11) EP 2 476 698 A2 (12) EUROPEAN PATENT APPLICATION (43) Date of publication: (51) Int Cl.: 18.07.2012 Bulletin 2012/29 C07K 14/435 (2006.01) A61K 38/00 (2006.01) A61K 39/00 (2006.01) A61P 35/00 (2006.01) (2006.01) (2006.01) (21) Application number: 12155446.3 C07K 7/00 C12N 15/09 (22) Date of filing: 16.10.2007 (84) Designated Contracting States: • Nakamura, Yusuke AT BE BG CH CY CZ DE DK EE ES FI FR GB GR Tokyo 113-8654 (JP) HU IE IS IT LI LT LU LV MC MT NL PL PT RO SE • Tsunoda, Takuya SI SK TR Tokyo 113-8654 (JP) • Osawa, Ryuji (30) Priority: 17.10.2006 US 852575 P Kawasaki-shi Kanagawa 213-0012 (JP) (62) Document number(s) of the earlier application(s) in • Shida, Midori accordance with Art. 76 EPC: Kawasaki-shi 07827901.5 / 2 091 965 Kanagawa 213-0012 (JP) (71) Applicant: Oncotherapy Science, Inc. (74) Representative: Vossius & Partner Kawasaki-shi Siebertstrasse 4 Kanagawa 213-0012 (JP) 81675 München (DE) (72) Inventors: Remarks: • Fujioka, Tomoaki This application was filed on 14-02-2012 as a Morioka-shi divisional application to the application mentioned Iwate 020-8505 (JP) under INID code 62. (54) Peptide vaccines for cancers expressing MPHOSPH1 or DEPDC1 polypeptides (57) The present invention provides peptides having cytotoxic T cell inducibility. The present invention also an amino acid sequence as set forth in SEQ ID NO: 7, provides drugs for treating or preventing a disease as- 8, 9, 10, 11, 12, 192, 195, 197, 209, 225, 226, 228, 230, sociated with the over- expression of MPHOSPH1 and/or 240, 241, 243, 244, 249, 253, 254 or 255, as well as DEPDC1, e.g. -

TRANSCRIPTOME ANALYSIS in MAMMALIAN CELL CULTURE: APPLICATIONS in PROCESS DEVELOPMENT and CHARACTERIZATION Anne Kantardjieff We
TRANSCRIPTOME ANALYSIS IN MAMMALIAN CELL CULTURE: APPLICATIONS IN PROCESS DEVELOPMENT AND CHARACTERIZATION A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY Anne Kantardjieff IN PARTIAL FULFILLMENT OF THE REQUIREMENTS FOR THE DEGREE OF DOCTOR OF PHILOSOPHY Wei-Shou Hu August, 2009 © Anne Kantardjieff, August 2009 ACKNOWLEDGMENTS First and foremost, I would like to thank my advisor, Prof. Wei-Shou Hu. He is a consummate teacher, who always puts the best interests of his students first. I am eternally grateful for all the opportunities he has given me and all that I have learned from him. I can only hope to prove as inspriring to others as he has been to me. I would like to thank my thesis committee members, Prof. Kevin Dorfman, Prof. Scott Fahrenkrug, and Prof. Friedrich Srienc, for taking the time to serve on my committee. It goes without saying that what makes the Hu lab a wonderful place to work are the people. I consider myself lucky to have joined what could only be described as a family. Thank you to all the Hu group members, past and present: Jongchan Lee, Wei Lian, Mugdha Gadgil, Sarika Mehra, Marcela de Leon Gatti, Ziomara Gerdtzen, Patrick Hossler, Katie Wlaschin, Gargi Seth, Fernando Ulloa, Joon Chong Yee, C.M. Cameron, David Umulis, Karthik Jayapal, Salim Charaniya, Marlene Castro, Nitya Jacob, Bhanu Mulukutla, Siguang Sui, Kartik Subramanian, Cornelia Bengea, Huong Le, Anushree Chatterjee, Jason Owens, Shikha Sharma, Kathryn Johnson, Eyal Epstein, ze Germans, Kirsten Keefe, Kim Coffee, Katherine Mattews and Jessica Raines-Jones. -

Association of Cnvs with Methylation Variation
www.nature.com/npjgenmed ARTICLE OPEN Association of CNVs with methylation variation Xinghua Shi1,8, Saranya Radhakrishnan2, Jia Wen1, Jin Yun Chen2, Junjie Chen1,8, Brianna Ashlyn Lam1, Ryan E. Mills 3, ✉ ✉ Barbara E. Stranger4, Charles Lee5,6,7 and Sunita R. Setlur 2 Germline copy number variants (CNVs) and single-nucleotide polymorphisms (SNPs) form the basis of inter-individual genetic variation. Although the phenotypic effects of SNPs have been extensively investigated, the effects of CNVs is relatively less understood. To better characterize mechanisms by which CNVs affect cellular phenotype, we tested their association with variable CpG methylation in a genome-wide manner. Using paired CNV and methylation data from the 1000 genomes and HapMap projects, we identified genome-wide associations by methylation quantitative trait locus (mQTL) analysis. We found individual CNVs being associated with methylation of multiple CpGs and vice versa. CNV-associated methylation changes were correlated with gene expression. CNV-mQTLs were enriched for regulatory regions, transcription factor-binding sites (TFBSs), and were involved in long- range physical interactions with associated CpGs. Some CNV-mQTLs were associated with methylation of imprinted genes. Several CNV-mQTLs and/or associated genes were among those previously reported by genome-wide association studies (GWASs). We demonstrate that germline CNVs in the genome are associated with CpG methylation. Our findings suggest that structural variation together with methylation may affect cellular phenotype. npj Genomic Medicine (2020) 5:41 ; https://doi.org/10.1038/s41525-020-00145-w 1234567890():,; INTRODUCTION influence transcript regulation is DNA methylation, which involves The extent of genetic variation that exists in the human addition of a methyl group to cytosine residues within a CpG population is continually being characterized in efforts to identify dinucleotide. -

Human Genome Center Laboratory of Genome Database Laboratory of Sequence Analysis ゲノムデータベース分野 シークエンスデータ情報処理分野
104 Human Genome Center Laboratory of Genome Database Laboratory of Sequence Analysis ゲノムデータベース分野 シークエンスデータ情報処理分野 Professor Minoru Kanehisa, Ph.D. 教 授 理学博士 金 久 實 Assistant Professor Toshiaki Katayama, M.Sc. 助 教 理学修士 片山俊明 Assistant Professor Shuichi Kawashima, M.Sc. 助 教 理学修士 川島秀一 Lecturer Tetsuo Shibuya, Ph.D. 講 師 理学博士 渋谷哲朗 Assistant Professor Michihiro Araki, Ph.D. 助 教 薬学博士 荒木通啓 DNA, RNA, and proteins are the basic molecular building blocks of life, but the liv- ing cell contains additional molecules, including water, ions, small chemical com- pounds, glycans, lipids, and other biochemical molecules, without which the cell would not function. We are developing bioinformatics methods to integrate differ- ent types of data and knowledge on various aspects of the biological systems to- wards basic understanding of life as a molecular interaction/reaction system and also for practical applications in medical and pharmaceutical sciences. 1. KEGG DRUG and KEGG DISEASE KEGG DISEASE (http://www.genome.jp/kegg/ disease/) as a new addition to the KEGG suite Minoru Kanehisa and Michihiro Araki of databases. Each disease entry consists of a list of diseases genes and other lists of molecules KEGG is a database of biological systems that such as environmental factors, markers, drugs, integrates genomic, chemical, and systemic func- etc. Both DRUG and DISEASE are highly inte- tional information. It is widely used as a refer- grated with other KEGG databases including ence knowledge base for understanding higher- PATHWAY, BRITE, GENES, and COMPOUND, order functions and utilities of the cell or the or- and also with other Internet resources.