Immune Defense at the Ocular Surface
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
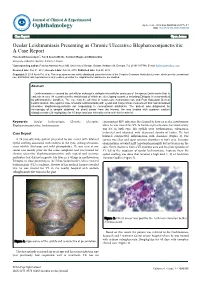
Ocular Leishmaniasis Presenting As Chronic
perim Ex en l & ta a l ic O p in l h t C h f Journal of Clinical & Experimental a o l m l a o n l r o g u Ayele et al., J Clin Exp Ophthalmol 2015, 6:1 y o J Ophthalmology ISSN: 2155-9570 DOI: 10.4172/2155-9570.1000395 Case Report Open Access Ocular Leishmaniasis Presenting as Chronic Ulcerative Blepharoconjunctivitis: A Case Report Fisseha Admassu Ayele*, Yared Assefa Wolde, Tesfalem Hagos and Ermias Diro University of Gondar, Gondar, Amhara, Ethiopia *Corresponding author: Fisseha Admassu Ayele MD, University of Gondar, Gondar, Amhara 196, Ethiopia, Tel: 251911197786; E-mail: [email protected] Received date: Dec 01, 2014, Accepted date: Feb 02, 2015, Published date: Feb 05, 2015 Copyright: © 2015 Ayele FH, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Leishmaniasis is caused by unicellular eukaryotic obligate intracellular protozoa of the genus Leishmania that is endemic in over 98 countries in the world-most of which are developing countries including Ethiopia. It is transmitted by phlebotomine sandflies. The eye may be affected in cutaneous, mucocutaneous and Post Kala-Azar Dermal Leishmaniasis. We report a case of ocular leishmaniasis with eyelid and conjunctival involvement that had simulated ulcerative blepharoconjunctivitis not responding to conventional antibiotics. The patient was diagnosed by microscopy of a sample obtained via direct smear from the lesions. He was treated with systemic sodium stibogluconate (20 mg/kg/day) for 45 days and was clinically cured with this treatment. -

Differentiate Red Eye Disorders
Introduction DIFFERENTIATE RED EYE DISORDERS • Needs immediate treatment • Needs treatment within a few days • Does not require treatment Introduction SUBJECTIVE EYE COMPLAINTS • Decreased vision • Pain • Redness Characterize the complaint through history and exam. Introduction TYPES OF RED EYE DISORDERS • Mechanical trauma • Chemical trauma • Inflammation/infection Introduction ETIOLOGIES OF RED EYE 1. Chemical injury 2. Angle-closure glaucoma 3. Ocular foreign body 4. Corneal abrasion 5. Uveitis 6. Conjunctivitis 7. Ocular surface disease 8. Subconjunctival hemorrhage Evaluation RED EYE: POSSIBLE CAUSES • Trauma • Chemicals • Infection • Allergy • Systemic conditions Evaluation RED EYE: CAUSE AND EFFECT Symptom Cause Itching Allergy Burning Lid disorders, dry eye Foreign body sensation Foreign body, corneal abrasion Localized lid tenderness Hordeolum, chalazion Evaluation RED EYE: CAUSE AND EFFECT (Continued) Symptom Cause Deep, intense pain Corneal abrasions, scleritis, iritis, acute glaucoma, sinusitis, etc. Photophobia Corneal abrasions, iritis, acute glaucoma Halo vision Corneal edema (acute glaucoma, uveitis) Evaluation Equipment needed to evaluate red eye Evaluation Refer red eye with vision loss to ophthalmologist for evaluation Evaluation RED EYE DISORDERS: AN ANATOMIC APPROACH • Face • Adnexa – Orbital area – Lids – Ocular movements • Globe – Conjunctiva, sclera – Anterior chamber (using slit lamp if possible) – Intraocular pressure Disorders of the Ocular Adnexa Disorders of the Ocular Adnexa Hordeolum Disorders of the Ocular -

Keratoconjunctivitis Sicca (“Dry Eye”) Stephanie Shrader, DVM and John Robertson, VMD, Phd
Keratoconjunctivitis sicca (“Dry Eye”) Stephanie Shrader, DVM and John Robertson, VMD, PhD Introduction and Overview How Tears Are Produced Keratoconjunctivitis sicca (KCS) is a disease of the eyes, The tear film that covers the eyes is made up of three distinct characterized by inflammation of the cornea and conjunctiva. layers. The outermost layer is made up of oils, which are This condition occurs secondary to a deficiency in formation secreted by the Meibomian glands. This lipid layer provides of the tear film that normally protects the cornea (Best et al, protection against evaporation, binds the tear film to the 2014), which leads to dry, irritated eyes. As a result, KCS is cornea, and prevents tears from simply pouring out over the commonly known as “dry eye” or in veterinary terminology, lower eyelid onto the face. The middle layer of the tear film is xerophthalmia. This disease occurs often in West Highland the aqueous layer, which is produced by the lacrimal glands. As White Terriers, but is also common in many other breeds, its name would suggest, the aqueous layer consists primarily including Lhasa Apso, English Bulldog, American Cocker of water, along with important proteins and enzymes that help Spaniel, English Springer Spaniel, Pekingese, Pug, Chinese Shar remove bacteria and cellular waste material, and lubricate the Pei, Yorkshire Terrier, Shih Tzu, Miniature Schnauzer, German surface of the cornea. The innermost layer of the tear film is the Shepherd, Doberman Pinscher, and Boston Terrier. While the mucin layer, which is is produced by tiny secretory cells in the reported incidence of KCS across all dog breeds ranges from conjunctiva known as goblet cells. -

Diagnostic Code Descriptions (ICD9)
INFECTIONS AND PARASITIC DISEASES INTESTINAL AND INFECTIOUS DISEASES (001 – 009.3) 001 CHOLERA 001.0 DUE TO VIBRIO CHOLERAE 001.1 DUE TO VIBRIO CHOLERAE EL TOR 001.9 UNSPECIFIED 002 TYPHOID AND PARATYPHOID FEVERS 002.0 TYPHOID FEVER 002.1 PARATYPHOID FEVER 'A' 002.2 PARATYPHOID FEVER 'B' 002.3 PARATYPHOID FEVER 'C' 002.9 PARATYPHOID FEVER, UNSPECIFIED 003 OTHER SALMONELLA INFECTIONS 003.0 SALMONELLA GASTROENTERITIS 003.1 SALMONELLA SEPTICAEMIA 003.2 LOCALIZED SALMONELLA INFECTIONS 003.8 OTHER 003.9 UNSPECIFIED 004 SHIGELLOSIS 004.0 SHIGELLA DYSENTERIAE 004.1 SHIGELLA FLEXNERI 004.2 SHIGELLA BOYDII 004.3 SHIGELLA SONNEI 004.8 OTHER 004.9 UNSPECIFIED 005 OTHER FOOD POISONING (BACTERIAL) 005.0 STAPHYLOCOCCAL FOOD POISONING 005.1 BOTULISM 005.2 FOOD POISONING DUE TO CLOSTRIDIUM PERFRINGENS (CL.WELCHII) 005.3 FOOD POISONING DUE TO OTHER CLOSTRIDIA 005.4 FOOD POISONING DUE TO VIBRIO PARAHAEMOLYTICUS 005.8 OTHER BACTERIAL FOOD POISONING 005.9 FOOD POISONING, UNSPECIFIED 006 AMOEBIASIS 006.0 ACUTE AMOEBIC DYSENTERY WITHOUT MENTION OF ABSCESS 006.1 CHRONIC INTESTINAL AMOEBIASIS WITHOUT MENTION OF ABSCESS 006.2 AMOEBIC NONDYSENTERIC COLITIS 006.3 AMOEBIC LIVER ABSCESS 006.4 AMOEBIC LUNG ABSCESS 006.5 AMOEBIC BRAIN ABSCESS 006.6 AMOEBIC SKIN ULCERATION 006.8 AMOEBIC INFECTION OF OTHER SITES 006.9 AMOEBIASIS, UNSPECIFIED 007 OTHER PROTOZOAL INTESTINAL DISEASES 007.0 BALANTIDIASIS 007.1 GIARDIASIS 007.2 COCCIDIOSIS 007.3 INTESTINAL TRICHOMONIASIS 007.8 OTHER PROTOZOAL INTESTINAL DISEASES 007.9 UNSPECIFIED 008 INTESTINAL INFECTIONS DUE TO OTHER ORGANISMS -

Cytokine Profiles of Tear Fluid from Patients with Pediatric Lacrimal
Immunology and Microbiology Cytokine Profiles of Tear Fluid From Patients With Pediatric Lacrimal Duct Obstruction Nozomi Matsumura,1 Satoshi Goto,2 Eiichi Uchio,3 Kyoko Nakajima,4 Takeshi Fujita,1 and Kazuaki Kadonosono5 1Department of Ophthalmology, Kanagawa Children’s Medical Center, Yokohama, Japan 2Department of Ophthalmology, The Jikei University School of Medicine, Tokyo, Japan 3Department of Ophthalmology, Faculty of Medicine, Fukuoka University, Fukuoka, Japan 4Department of Joint Laboratory for Frontier Medical Science, Faculty of Medicine, Fukuoka University, Fukuoka, Japan 5Department of Ophthalmology and Micro-technology, Yokohama City University, Yokohama, Japan Correspondence: Nozomi Matsu- PURPOSE. This study evaluated the cytokine levels in unilateral tear samples from both sides in mura, Department of Ophthalmolo- patients with pediatric lacrimal duct obstruction. gy, Kanagawa Children’s Medical Center, 2-138-4 Mutsukawa, Minami- METHODS. Fifteen cases of unilateral lacrimal duct obstruction (mean, 26.9 6 28.7 months old) ku, Yokohama 232-8555, Japan; were enrolled in this study. Tear samples were collected separately from the obstructed side [email protected]. and the intact side in each case before surgery, which was performed under general Submitted: September 8, 2016 anesthesia or sedation. The levels of IL-2, IL-4, IL-6, IL-10, TNF, IFN-c, and IL-17A then were Accepted: December 2, 2016 measured in each tear sample. A receiver operating characteristic (ROC) curve was constructed for the IL-6 levels in the tears. We also measured the postoperative tear fluid Citation: Matsumura N, Goto S, Uchio levels of IL-6 in those cases from which tear fluid samples could be collected after the surgery. -

Onchocerciasis
11 ONCHOCERCIASIS ADRIAN HOPKINS AND BOAKYE A. BOATIN 11.1 INTRODUCTION the infection is actually much reduced and elimination of transmission in some areas has been achieved. Differences Onchocerciasis (or river blindness) is a parasitic disease in the vectors in different regions of Africa, and differences in cause by the filarial worm, Onchocerca volvulus. Man is the the parasite between its savannah and forest forms led to only known animal reservoir. The vector is a small black fly different presentations of the disease in different areas. of the Simulium species. The black fly breeds in well- It is probable that the disease in the Americas was brought oxygenated water and is therefore mostly associated with across from Africa by infected people during the slave trade rivers where there is fast-flowing water, broken up by catar- and found different Simulium flies, but ones still able to acts or vegetation. All populations are exposed if they live transmit the disease (3). Around 500,000 people were at risk near the breeding sites and the clinical signs of the disease in the Americas in 13 different foci, although the disease has are related to the amount of exposure and the length of time recently been eliminated from some of these foci, and there is the population is exposed. In areas of high prevalence first an ambitious target of eliminating the transmission of the signs are in the skin, with chronic itching leading to infection disease in the Americas by 2012. and chronic skin changes. Blindness begins slowly with Host factors may also play a major role in the severe skin increasingly impaired vision often leading to total loss of form of the disease called Sowda, which is found mostly in vision in young adults, in their early thirties, when they northern Sudan and in Yemen. -

2012 Case Definitions Infectious Disease
Arizona Department of Health Services Case Definitions for Reportable Communicable Morbidities 2012 TABLE OF CONTENTS Definition of Terms Used in Case Classification .......................................................................................................... 6 Definition of Bi-national Case ............................................................................................................................................. 7 ------------------------------------------------------------------------------------------------------- ............................................... 7 AMEBIASIS ............................................................................................................................................................................. 8 ANTHRAX (β) ......................................................................................................................................................................... 9 ASEPTIC MENINGITIS (viral) ......................................................................................................................................... 11 BASIDIOBOLOMYCOSIS ................................................................................................................................................. 12 BOTULISM, FOODBORNE (β) ....................................................................................................................................... 13 BOTULISM, INFANT (β) ................................................................................................................................................... -

Idiopathic Interstitial Keratitis in a Child 35
Summer 2021 • Vol 16 | No 1 Case report SA Ophthalmology Journal Idiopathic interstitial keratitis in a child 35 Idiopathic interstitial keratitis in a child DA Erasmus MBBCh, MMed, Dip Ophth (SA); Registrar, Department of Neurosciences, Division of Ophthalmology, University of the Witwatersrand, Johannesburg, South Africa ORCID: https://orcid.org/0000-0002-8395-7080 R Höllhumer MBChB, MMed, FC Ophth(SA); Consultant ophthalmologist, Department of Neurosciences, Division of Ophthalmology, University of the Witwatersrand, Johannesburg, South Africa ORCID: https://orcid.org/0000-0002-4375-2224 Corresponding author: Dr DA Erasmus, 40 2nd Avenue, Parktown North, 2193; tel.: +27 76 462 3355; email: [email protected] Abstract Interstitial keratitis represents inflammation and new vessel investigations can help to establish the underlying cause of formation in the middle layers of the cornea without tissue interstitial keratitis. loss. The most important infective aetiologies include herpes viruses, tuberculosis and syphilis. Keywords: interstitial, keratitis, inflammation, cornea, stroma Non-infectious causes such as Cogan’s syndrome should be considered in those cases with associated neurosensory Funding: No external funding was received. hearing loss. The pattern and laterality of inflammation together with the Conflict of interest: The authors have no conflicts of interest presence or absence of systemic features as well as relevant to declare. Severe Mild Moderate Moderate/Mild A * Dry Eye range like NEVER BEFORE Introduction systemic features provides a clue to the a tuberculosis (TB) endemic area such as Interstitial keratitis is a non-ulcerative underlying cause of interstitial keratitis. South Africa. Parasitic infections causing inflammation and subsequent Interstitial keratitis can be broadly interstitial keratitis are very uncommonly vascularisation of the corneal stroma divided into infectious and non-infectious encountered in South Africa but imported which does not primarily involve the aetiologies. -

Treatment of Interface Keratitis with Oral Corticosteroids
Treatment of interface keratitis with oral corticosteroids Scott M. MacRae, MD, Larry F. Rich, MD, Damien C. Macaluso, MD ABSTRACT Purpose: To describe the results of treating interface keratitis using a combination of intensive topical and oral corticosteroids. Setting: Casey Eye Institute, Portland, Oregon, USA. Methods: Thirteen eyes treated for grade 2 to 3 interface keratitis using an oral cortico- steroid (prednisone 60 to 80 mg) as well as an hourly topical corticosteroid were retrospectively reviewed. The best corrected visual acuity (BCVA) was used as an objective guide of whether to treat with intense topical and oral corticosteroids, flap irrigation, or both. Predisposing factors such as intraoperative epithelial defects or a history of severe allergies or atopy were also looked for. Results: All 13 eyes responded favorably to the combination of intensive topical and oral corticosteroids and had a BCVA of 20/20 after the keratitis resolved. In 6 eyes (46%), the patients had a history of severe seasonal allergies. One day postoperatively, 3 eyes (23%) had an epithelial defect and 2 eyes (15%), lint particles or debris embedded in the interface. With oral corticosteroid use, 3 patients (23%) noted mild stomach irritation and 2 (15%) noted nervousness. All 5 side effects resolved without sequelae. No patient developed a serious side effect. Conclusion: A short, intense course of an oral corticosteroid was an effective treatment in patients with grade 2 or higher interface keratitis when combined with a topical corti- costeroid administered hourly. The BCVA is a helpful objective measure of the severity of interface keratitis and can be used to guide the clinician in the therapeutic strategy. -

Frequency and Risk Factors of Symptomatic Dry Eye Disease at Tertiary Care Eye Hospital, Karachi
Biostatistics and Biometrics Open Access Journal ISSN: 2573-2633 Research Article Biostat Biometrics Open Acc J Faisal’s Issue - January 2018 Copyright © All rights are reserved by Muhammad Faisal Fahim DOI: 10.19080/BBOAJ.2018.04.555639 Frequency and Risk Factors of Symptomatic Dry Eye Disease at Tertiary Care Eye Hospital, Karachi Shaheerah Gul1, Adil Salim Jafri1, Muhammad Faisal Fahim2* 1Department of Ophthalmology, Al-Ibrahim Eye Hospital, Pakistan 2Department of Research & Development, Al-Ibrahim Eye Hospital, Pakistan Submission: November 27, 2017; Published: January 19, 2018 *Corresponding author: Muhammad Faisal Fahim, M.Sc (Statistics), Statistician, Research & Development Department, Al-Ibrahim Eye Hospital, Isra postgraduate Institute of Ophthalmology, Karachi, Pakistan, Tel: ; Email: Abstract Objective: To determine frequency and risk factors of symptomatic dry eye disease at tertiary care eye hospital, Karachi. Material & Methods: This was a descriptive cross sectional study carried out at Al-Ibrahim Eye Hospital, Isra postgraduate Institute of Oph- thalmology, Karachi from March to October 2016. Non-Probability purposive sampling technique was used for data collection. Inclusion criteria give consent. Symptoms of dry eye were assessed using Tear breakup test (TBUT) test. SPSS version 20.0 was used to analyze data. were patients aged ≥ 21 years and on the basis of dry eye symptoms. Exclusion criteria were other systemic eye disease and those who did not Results: A total of 100 patients 65 female and 35 male were diagnosed with dry eye syndrome. The age group of 21-30 years having the high- est frequency of 34 patients, whereas after the 50 years of age the frequency of patients decreases to 21. -

Results of Penetrating Keratoplasty in Syphilitic Interstitial Keratitis
RESULTS OF PENETRATING KERATOPLASTY IN SYPHILITIC INTERSTITIAL KERATITIS GOEGEBUER A.*, ***, AJAY LOHIYA**, ***, CLAERHOUT I.*, KESTELYN PH.* ABSTRACT ratite interstitielle (KI) syphilitique avec ceux dé- crits dans la litérature. Purpose: To compare the results in our patient se- Méthode: Analyse rétrospective des cas, avec acui- ries after penetrating keratoplasty (PKP) for syphi- té visuelle, clarté du greffon, épisodes de rejet, pres- litic interstitial keratitis (IK) with those described in sion intraoculaire et comptage postopératoire des the literature. cellules endothéliales. Methods: Retrospective case series in which visual Résultats: L’acuité visuelle s’est améliorée dans tous acuity (VA), graft clarity,rejection episodes, intraocu- les cas. Il n’y avait pas de signes de déhiscence du lar pressure and endothelial cell density (ECD) were greffon, ni d’ occurrence d’une membrane rétrocor- examined postoperatively. néenne. L’inflammation postopératoire n’était pas Results: Postoperative VA improved in all cases. plus prononcée chez nos patients avec une kératite There was no evidence of wound dehiscense or oc- interstitielle comparée aux patients opérés pour currence of retrocorneal membrane formation in any d’autres raisons. Un déclin normal du comptage des case. Postoperative inflammation was not more se- cellules endothéliales prouvait qu’il n’y avait pas d’in- vere in our patients with syphilitic IK compared to flammation infraclinique. patients undergoing PKP for other reasons. A nor- Conclusion: Une kératoplastie transfixiante pour KI mal decline in ECD proved that there was no sub- syphilitique a un bon pronostic en ce qui concerne clinical inflammation as well. la clarté du greffon. Tous les patients bénéficiaient Conclusion: PKP for syphilitic IK has a good prog- d’ une amélioration de l’acuité visuelle, bien que par- nosis in our case series as far as graft survival is con- fois limitée. -

Microbial Keratitis After Corneal Collagen Crosslinking
CASE REPORT Microbial keratitis after corneal collagen crosslinking Juan J. Pe´rez-Santonja, MD, Alberto Artola, MD, Jaime Javaloy, MD, Jorge L. Alio´, MD, PhD, Jose´L. Abad, PhD Several infiltrates appeared in the upper midperipheral cornea of a 29-year-old woman who had had uneventful corneal collagen crosslinking (CXL) with riboflavin and ultraviolet-A light (UVA) for the treatment of keratoconus in the right eye. Staphylococcus epidermidis keratitis was con- firmed by microbiological studies, which guided treatment with topical fortified antibiotic agents. Before CXL, the best spectacle-corrected visual acuity (BSCVA) in the right eye was 20/25, the manifest refraction was À0.25 À0.25 Â 125, and the anterior segment was normal under biomi- croscopy. Five months after the procedure, the BSCVA was 20/22, the manifest refraction was C1.00 À2.50 Â 40, and slitlamp examination revealed a mild residual haze in the upper midper- ipheral cornea. Collagen crosslinking with riboflavin–UVA is a minimally invasive method but tra- ditionally requires epithelial removal, which could be a predisposing factor to bacterial keratitis. J Cataract Refract Surg 2009; 35:1138–1140 Q 2009 ASCRS and ESCRS Keratoconus is a noninflammatory ectasia of the cor- light (UVA) has been developed.3 This technique in- nea that is usually bilateral. The condition typically creases the corneal rigidity of treated corneas, and pre- starts at puberty, progressing in approximately 20% liminary clinical studies have shown improvement of cases to the extent that keratoplasty is necessary.1 and stabilization of keratectasia with few, if any, com- Hard contact lenses and corneal grafting have been plications in patients with keratoconus.4,5 the major treatment modalities for keratoconus, We report a case of microbial keratitis that devel- although some patients can now benefit from intracor- oped after CXL with riboflavin and UVA for the treat- neal ring segment implantation.1,2 None of these tech- ment of keratoconus.