Pulse Wave Propagation in the Arterial Tree
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Evaluation of Artery Visualizations for Heart Disease Diagnosis
Evaluation of Artery Visualizations for Heart Disease Diagnosis Michelle A. Borkin, Student Member, IEEE, Krzysztof Z. Gajos, Amanda Peters, Dimitrios Mitsouras, Simone Melchionna, Frank J. Rybicki, Charles L. Feldman, and Hanspeter Pfister, Senior Member, IEEE Fig. 1. Left: Traditional 2D projection (A) of a single artery, and 3D representation (C) of a right coronary artery tree with a rainbow color map. Right: 2D tree diagram representation (B) and equivalent 3D representation (D) of a left coronary artery tree with a diverging color map. Abstract—Heart disease is the number one killer in the United States, and finding indicators of the disease at an early stage is critical for treatment and prevention. In this paper we evaluate visualization techniques that enable the diagnosis of coronary artery disease. A key physical quantity of medical interest is endothelial shear stress (ESS). Low ESS has been associated with sites of lesion formation and rapid progression of disease in the coronary arteries. Having effective visualizations of a patient’s ESS data is vital for the quick and thorough non-invasive evaluation by a cardiologist. We present a task taxonomy for hemodynamics based on a formative user study with domain experts. Based on the results of this study we developed HemoVis, an interactive visualization application for heart disease diagnosis that uses a novel 2D tree diagram representation of coronary artery trees. We present the results of a formal quantitative user study with domain experts that evaluates the effect of 2D versus 3D artery representations and of color maps on identifying regions of low ESS. We show statistically significant results demonstrating that our 2D visualizations are more accurate and efficient than 3D representations, and that a perceptually appropriate color map leads to fewer diagnostic mistakes than a rainbow color map. -

Disruption of Vascular Ca2+-Activated Chloride Currents Lowers Blood Pressure Christoph Heinze,1 Anika Seniuk,2 Maxim V
Research article Disruption of vascular Ca2+-activated chloride currents lowers blood pressure Christoph Heinze,1 Anika Seniuk,2 Maxim V. Sokolov,3 Antje K. Huebner,1 Agnieszka E. Klementowicz,3 István A. Szijártó,4,5 Johanna Schleifenbaum,4 Helga Vitzthum,2 Maik Gollasch,4 Heimo Ehmke,2 Björn C. Schroeder,3 and Christian A. Hübner1 1Institut für Humangenetik, Universitätsklinikum Jena, Friedrich-Schiller Universität Jena, Jena, Germany. 2Institut für Zelluläre und Integrative Physiologie, Universitätsklinikum Hamburg Eppendorf, Hamburg, Germany. 3Max-Delbrück Centrum für Molekulare Medizin (MDC) and NeuroCure, Berlin, Germany. 4Medizinische Klinik mit Schwerpunkt Nephrologie und Internistische Intensivmedizin, Charité – Universitätsmedizin Berlin, Experimental and Clinical Research Center (ECRC), Berlin, Germany. 5Interdisziplinäres Stoffwechsel-Centrum, Charité – Universitätsmedizin Berlin, Berlin, Germany. High blood pressure is the leading risk factor for death worldwide. One of the hallmarks is a rise of periph- eral vascular resistance, which largely depends on arteriole tone. Ca2+-activated chloride currents (CaCCs) in vascular smooth muscle cells (VSMCs) are candidates for increasing vascular contractility. We analyzed the vascular tree and identified substantial CaCCs in VSMCs of the aorta and carotid arteries. CaCCs were small or absent in VSMCs of medium-sized vessels such as mesenteric arteries and larger retinal arterioles. In small vessels of the retina, brain, and skeletal muscle, where contractile intermediate cells or pericytes gradually replace VSMCs, CaCCs were particularly large. Targeted disruption of the calcium-activated chloride channel TMEM16A, also known as ANO1, in VSMCs, intermediate cells, and pericytes eliminated CaCCs in all ves- sels studied. Mice lacking vascular TMEM16A had lower systemic blood pressure and a decreased hyperten- sive response following vasoconstrictor treatment. -

Chapter 15 Hydrocephalus: New Theories and New Shunts?
Chapter 15 Hydrocephalus: New Theories and New Shunts? Marvin Bergsneider, M.D. Introduction The optimal and ideal management for any given clinical disorder should be fundamentally aimed at reversing or preventing the pathobiological mechanism underlying the disorder. For hydrocephalus, our current incomplete understanding of the pathophysiology is, in part, responsible for significant inadequacies of the current mainstay of treatment: the cerebrospinal fluid (CSF) shunt. The management of shunt-related problems and disorders has become a de facto subspecialty within neurosurgery. Although it is clear that the treatment of hydrocephalus was vastly improved with the introduction of the differential pressure valve by Nulsen and Spitz (25) half a century ago, it can be argued that little further improvement has occurred in the interim. A randomized, multicenter trial failed to show a benefit from “technologically advanced” valve designs compared with a standard differential pressure valve (7) similar to the one designed by John Holter. Probably one of the most refractory problems of CSF shunt diversion has been that of over-drainage. In children, excessive CSF drainage by the shunt is an important cause of shunt failure caused by ventricular catheter obstruction resulting from ventricular collapse. Over time, shunted hydrocephalic children can develop the slit-ventricle syndrome—one of the most challenging conditions to treat in neurosurgery. In older adults, shunt over-drainage can result in the devastating complication of subdural hematoma. A similar degree of ventricular reduction occurs despite the implementation of valve designs touted to prevent it, including flow-limiting valves and antisiphon devices (31). Why have efforts failed to prevent excessive CSF drainage by shunts? Although the answer is likely multifactorial, we argue that the fundamental problem lies in our incomplete and overly simplistic understanding of the hydrodynamics of hydrocephalus and in vivo shunt physiology. -

Ingeniería Cardiovascular - Del Laboratorio a La Clínica
INGENIERÍA CARDIOVASCULAR - DEL LABORATORIO A LA CLÍNICA INGENIERÍA CARDIOVASCULAR DEL LABORATORIO A LA CLÍNICA RICARDO L. ARMENTANO Departamento de Ingeniería Biológica, CENUR LITOTAL NORTE, URUGUAY Facultad de Ingeniería, UNIVERSIDAD DE LA REPÚBLICA, URUGUAY. Introducción La Ingeniería Cardiovascular integra elementos de la biología, la ingeniería eléctrica, la ingeniería mecánica, la matemática y la física con el fin de describir y comprender al sistema cardiovascular. Su objetivo es desarrollar, comprobar y validar una interpretación predictiva y cuantitativa del sistema cardiovascular en un adecuado nivel de detalle, y aplicar conceptos resultantes hacia la solución de diversas patologías. La dinámica del sistema cardiovascular caracteriza al corazón y al sistema vascular como un todo, y comprende la física del sistema circulatorio incluyendo el continente (las paredes arteriales) y el contenido (sangre), así como la interrelación entre ambos. La pared arterial y la sangre contienen la información esencial sobre el estado fisiológico del sistema circulatorio completo, en tanto que la interdependencia de estos componentes está relacionada con procesos complejos que podrían explicar la formación de lesiones en la pared vascular, tales como las placas de ateroma, o el aumento en la rigidez de la pared como está descripto en la hipertensión arterial. Los incipientes cambios morfológicos de la pared arterial inducidos por procesos patológicos pueden ser considerados marcadores precoces de futuras alteraciones circulatorias. La modelización matemática de la pared arterial, a partir de la estimación de los coeficientes de la ecuación del modelo, obtenida a través de estudios en animales conscientes, constituye una herramienta de gran valor e indispensable para una mejor comprensión de la génesis de las enfermedades cardiovasculares. -

Simple Models of the Cardiovascular System for Educational and Research Purposes
56 ORIGINAL ARTICLE SIMPLE MODELS OF THE CARDIOVASCULAR SYSTEM FOR EDUCATIONAL AND RESEARCH PURPOSES Tomáš Kulhánek*, Martin Tribula, Jiří Kofránek, Marek Mateják Institute of Pathological Physiology, 1st Faculty of Medicine, Charles University in Prague, Prague, Czech Republic * Corresponding author: [email protected] Article history AbstrAct — Modeling the cardiovascular system as an analogy of an electri- Received 14 September 2014 cal circuit composed of resistors, capacitors and inductors is introduced in many Revised 30 October 2014 research papers. This contribution uses an object oriented and acausal approach, Accepted 4 November 2014 which was recently introduced by several other authors, for educational and re- Available online 24 November 2014 search purpose. Examples of several hydraulic systems and whole system model- ing hemodynamics of a pulsatile cardiovascular system are presented in Modelica Keywords language using Physiolibrary. Modelica modeling physiology cardiovascular system Physiolibrary INTRODUCTION grown technology from the scientific community, such as SBML [10], JSIM [11] or CellML [1,12] or industrial The mathematical formalization of the cardiovas- standard technology implemented by several vendors, cular system (CVS), i.e. the models, can be divided such as the Modelica language [8,9]. into two main approaches. The first approach builds This article introduces a modeling method which 3D models with geometrical, mechanical properties follows the second approach for modeling CVS as and the time-dependence -

Arterial Variations of the Subclavian-Axillary Arterial Tree: Its Association with the Supply of the Rotator Cuff Muscles
Int. J. Morphol., 32(4):1436-1443, 2014. Arterial Variations of the Subclavian-Axillary Arterial Tree: Its Association with the Supply of the Rotator Cuff Muscles Variaciones Arteriales del Árbol Arterial Subclavio-Axilar. Su Asociación con la Irrigación del Manguito de los Rotadores N. Naidoo*; L. Lazarus*; B. Z. De Gama*; N. O. Ajayi* & K. S. Satyapal* NAIDOO, N.; LAZARUS, L.; DE GAMA, B. Z.; AJAYI, N. O. & SATYAPAL, K. S. Arterial variations of the subclavian-axillary arterial tree: Its association with the supply of the rotator cuff muscles. Int. J. Morphol., 32(4):1436-1443, 2014. SUMMARY: The subclavian-axillary arterial tree is responsible for the arterial supply to the rotator cuff muscles as well as other shoulder muscles. This study comprised the bilateral dissection of the shoulder and upper arm region in thirty-one adult and nineteen fetal cadaveric specimens. The variable origins and branching patterns of the axillary, subscapular, circumflex scapular, thoracodorsal, posterior circumflex humeral and suprascapular arteries identified in this study corroborated the findings of previous studies. In addition, unique variations that are unreported in the literature were also observed. The precise anatomy of the arterial distribution to the rotator cuff muscles is important to the surgeon and radiologist. It will aid proper interpretation of radiographic images and avoid injury to this area during surgical procedures. KEY WORDS: Subclavian-axillary arterial tree; Variations; Supply; Rotator cuff muscles. INTRODUCTION Standard anatomical textbooks divide the axillary identified by Saralaya et al. (2008) to arise as a large artery into three parts using its relation to the pectoralis minor collateral branch from the first part of the axillary artery muscle (Salopek et al., 2007). -

Journal of Neurology Research Review & Reports
Journal of Neurology Research Review & Reports Case Report Open Access Bilateral Tortuous Upper Limb Arterial Tree and Their Clinical Significance Alka Bhingardeo Department of Anatomy, All India Institute of Medical Sciences, Bibinagar ABSTRACT The detailed knowledge about the possible anatomical variations of upper limb arteries is vital for the reparative surgery of the region. Brachial artery is the main artery of upper limb; it is a continuation of axillary artery from the lower border of teres major muscle. During routine cadaveric dissection, we found bilateral tortuous brachial artery which was superficial as well as tortuous throughout its course. It is called superficial as it was superficial to the median nerve. At the neck of radius, it was divided into two terminal branches radial and ulnar arteries which were also tortuous. Tortuosity of the radial artery was more near the flexor retinaculum. When observed, the continuation of ulnar artery as superficial palmar arch also showed tortuosity throughout, including its branches. Being superficial such brachial artery can be more prone to trauma. Tortuous radial artery is one of the causes of access failure in trans-radial approach of coronary interventions. To the best of our knowledge, this is the first case where entire post axillary upper limb arterial system is tortuous bilaterally. So knowledge of such tortuous upper limb arterial tree is important for cardiologist, radiologist, plastic surgeons and orthopedic surgeons. *Corresponding author Alka Bhingardeo, Assistant Professor, Department of Anatomy, All India Institute of Medical Sciences, Bibinagar, Telangana, India, Mob: 8080096151, Email: [email protected] Received: November 08, 2020; Accepted: November 16, 2020; Published: November 21, 2020 Keywords: Radial Artery, Superficial Brachial Artery, Tortuous, Brachial Artery Ulnar Artery, Upper Limb The brachial artery commenced from the axillary artery at the lower border of teres major muscle. -

Radial and Longitudinal Motion of the Arterial Wall: Their Relation to Pulsatile Pressure and Flow in the Artery Dan Wang Old Dominion University
Old Dominion University ODU Digital Commons Mechanical & Aerospace Engineering Faculty Mechanical & Aerospace Engineering Publications 2018 Radial and Longitudinal Motion of the Arterial Wall: Their Relation to Pulsatile Pressure and Flow in the Artery Dan Wang Old Dominion University Linda Vahala Old Dominion University Zhili Hao Old Dominion University Follow this and additional works at: https://digitalcommons.odu.edu/mae_fac_pubs Part of the Biomechanical Engineering Commons, Cardiovascular System Commons, and the Electrical and Computer Engineering Commons Repository Citation Wang, Dan; Vahala, Linda; and Hao, Zhili, "Radial and Longitudinal Motion of the Arterial Wall: Their Relation to Pulsatile Pressure and Flow in the Artery" (2018). Mechanical & Aerospace Engineering Faculty Publications. 69. https://digitalcommons.odu.edu/mae_fac_pubs/69 Original Publication Citation Wang, D., Vahala, L., & Hao, Z. (2018). Radial and longitudinal motion of the arterial wall: Their er lation to pulsatile pressure and flow in the artery. Physical Review E, 98(3), 032402. doi:10.1103/PhysRevE.98.032402 This Article is brought to you for free and open access by the Mechanical & Aerospace Engineering at ODU Digital Commons. It has been accepted for inclusion in Mechanical & Aerospace Engineering Faculty Publications by an authorized administrator of ODU Digital Commons. For more information, please contact [email protected]. PHYSICAL REVIEW E 98, 032402 (2018) Radial and longitudinal motion of the arterial wall: Their relation to pulsatile pressure -
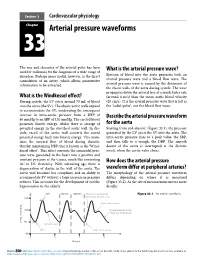
Arterial Pressure Waveforms
Section 3 Cardiovascular physiology Chapter 33 Arterial pressure waveforms The rate and character of the arterial pulse has been What is the arterial pressure wave? used for millennia for the diagnosis of a wide range of disorders. Perhaps more useful, however, is the direct Ejection of blood into the aorta generates both an cannulation of an artery, which allows quantitative arterial pressure wave and a blood flow wave. The information to be extracted. arterial pressure wave is caused by the distension of the elastic walls of the aorta during systole. The wave propagates down the arterial tree at a much faster rate What is the Windkessel effect? (around 4 m/s) than the mean aortic blood velocity During systole, the LV ejects around 70 mL of blood (20 cm/s). It is the arterial pressure wave that is felt as into the aorta (the SV). The elastic aortic walls expand the ‘radial pulse’, not the blood flow wave. to accommodate the SV, moderating the consequent increase in intra-aortic pressure from a DBP of Describethearterialpressurewaveform 80 mmHg to an SBP of 120 mmHg. The ejected blood possesses kinetic energy, whilst there is storage of for the aorta potential energy in the stretched aortic wall. In dia- Starting from end-diastole (Figure 33.1), the pressure stole, recoil of the aortic wall converts the stored generated by the LV ejects the SV into the aorta. The potential energy back into kinetic energy. This main- intra-aortic pressure rises to a peak value, the SBP, tains the onward flow of blood during diastole, and then falls to a trough, the DBP. -

Elastic Fibers and Biomechanics of the Aorta: Insights from Mouse Studies
Review MATBIO-1552; No. of pages: 13; 4C: Elastic fibers and biomechanics of the aorta: Insights from mouse studies Hiromi Yanagisawa a and Jessica Wagenseil b a - Life Science Center for Survival Dynamics, Tsukuba Advanced Research Alliance (TARA), University of Tsukuba, Tsukuba 305-8577, Japan b - Department of Mechanical Engineering and Materials Science, Washington University at St. Louis, St. Louis, MO, USA Correspondence to Hiromi Yanagisawa and Jessica Wagenseil: [email protected], [email protected]. https://doi.org/10.1016/j.matbio.2019.03.001 Abstract Elastic fibers are major components of the extracellular matrix (ECM) in the aorta and support a life-long cycling of stretch and recoil. Elastic fibers are formed from mid-gestation throughout early postnatal development and the synthesis is regulated at multiple steps, including coacervation, deposition, cross- linking, and assembly of insoluble elastin onto microfibril scaffolds. To date, more than 30 molecules have been shown to associate with elastic fibers and some of them play a critical role in the formation and maintenance of elastic fibers in vivo. Because the aorta is subjected to high pressure from the left ventricle, elasticity of the aorta provides the Windkessel effect and maintains stable blood flow to distal organs throughout the cardiac cycle. Disruption of elastic fibers due to congenital defects, inflammation, or aging dramatically reduces aortic elasticity and affects overall vessel mechanics. Another important component in the aorta is the vascular smooth muscle cells (SMCs). Elastic fibers and SMCs alternate to create a highly organized medial layer within the aortic wall. The physical connections between elastic fibers and SMCs form the elastin-contractile units and maintain cytoskeletal organization and proper responses of SMCs to mechanical strain. -

Collateral Circulation in Spinal Cord Injury: a Comprehensive Review
Published online: 2020-09-29 THIEME Review Article 1 Collateral Circulation in Spinal Cord Injury: A Comprehensive Review Ezequiel Garcia-Ballestas1 B. V. Murlimanju2 Yeider A. Durango-Espinosa1 Andrei F. Joaquim3 Harold E. Vasquez4 Luis Rafael Moscote-Salazar5 Amit Agrawal6 1Faculty of Medicine, Center for Biomedical Research (CIB), Address for correspondence Luis Rafael Moscote-Salazar, MD, University of Cartagena, Cartagena, Colombia Neurosurgeon-Critical Care, Center for Biomedical Research (CIB), 2Department of Anatomy, Kasturba Medical College, Mangalore, Cartagena Neurotrauma Research Group, Faculty of Medicine, Manipal Academy of Higher Education, Manipal, Karnataka, India University of Cartagena, Calle de la Universidad, Cra. 6 #36-100, 3Neurosurgery Division, Cartagena de Indias, Bolivar Department of Cartagena, Bolívar 130001, Columbia Neurology, State University of Campinas, Campinas-Sao Paulo, Brazil (e-mail: [email protected]). 4Universidad del Sinu, Cartagena de Indias, Consejo Latinoamericano de Neurointensivismo (CLaNi), Cartagena de Indias, Colombia 5Neurosurgeon-Critical Care, Center for Biomedical Research (CIB), Cartagena Neurotrauma Research Group, Faculty of Medicine, University of Cartagena, Cartagena, Colombia 6Department of Neurosurgery, All India Institute of Medical Sciences, Bhopal, Madhya Pradesh, India Indian J Neurotrauma:2021;18:1–6 Abstract Surgery is the most common cause of spinal cord ischemia; it is also caused by hemo- dynamic changes, which disrupt the blood flow. Direct ligation of the spinal arteries, especially the Adamkiewicz artery is involved as well. Other causes of spinal cord isch- emia include arteriography procedures, thoracic surgery, epidural and rachianesthesia, foraminal infiltration, arterial dissection, systemic hypotension, emboligenic heart dis- ease, thoracic disc herniation, and compression. Understanding the vascular anatomy of the spinal cord is essential to develop optimal strategies for preventing ischemic injuries to the spinal cord. -

The Suboccipital Cavernous Sinus
The suboccipital cavernous sinus Kenan I. Arnautovic, M.D., Ossama Al-Mefty, M.D., T. Glenn Pait, M.D., Ali F. Krisht, M.D., and Muhammad M. Husain, M.D. Departments of Neurosurgery and Pathology, University of Arkansas for Medical Sciences, and Laboratory Service, Veterans Administration Medical Center, Little Rock, Arkansas The authors studied the microsurgical anatomy of the suboccipital region, concentrating on the third segment (V3) of the vertebral artery (VA), which extends from the transverse foramen of the axis to the dural penetration of the VA, paying particular attention to its loops, branches, supporting fibrous rings, adjacent nerves, and surrounding venous structures. Ten cadaver heads (20 sides) were fixed in formalin, their blood vessels were perfused with colored silicone rubber, and they were dissected under magnification. The authors subdivided the V3 into two parts, the horizontal (V3h) and the vertical (V3v), and studied the anatomical structures topographically, from the superficial to the deep tissues. In two additional specimens, serial histological sections were acquired through the V3 and its encircling elements to elucidate their cross-sectional anatomy. Measurements of surgically and clinically important features were obtained with the aid of an operating microscope. This study reveals an astonishing anatomical resemblance between the suboccipital complex and the cavernous sinus, as follows: venous cushioning; anatomical properties of the V3 and those of the petrouscavernous internal carotid artery (ICA), namely their loops, branches, supporting fibrous rings, and periarterial autonomic neural plexus; adjacent nerves; and skull base locations. Likewise, a review of the literature showed a related embryological development and functional and pathological features, as well as similar transitional patterns in the arterial walls of the V3 and the petrous-cavernous ICA.