Autonomic Nervous System 2 & 3
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Communication Center
2/16/2012 Communication Center Nervous System Regulation •The Neural System is only 3% of your body weight, but is the most complex organ system. •Nervous impulses are fast acting (milliseconds) Neural vs. Hormonal but short lived. Overview •The nervous system includes all neural tissue in the body. Basic units are: Two Anatomical Divisions of The Nervous System a. Neurons (individual nerve cells) 1. CNS: Central Nervous System b. Neuroglia • supporting cells • Brain & Spinal Cord • separate & protect the neurons • Responsible for integrating, processing, & • provide supporting framework coordinatinggy sensory data and motor commands. i.e.- stumble example • act as phagocytes • regulate composition of interstitial fluid • The brain is also the organ responsible for • a.k.a. glial cells intelligence, memory, learning, & emotion • outnumber neurons 1 2/16/2012 2. PNS: Peripheral Nervous System PNS has 2 functional divisions • All nervous tissue outside CNS Afferent Division (Sensory) • Carries sensory data to CNS, carries motor •Bring sensory information to CNS from receptors in commands from the CNS. peripheral nervous tissue & organs. • Bundles of nerve fibers carry impulses in the PNS are known as per ip hera l nerves or jus t “nerves”. Efferent Division (Motor) •Carries motor commands from CNS to muscles & • Nerves attached to the brain are called cranial glands, these target organs are called effectors. nerves. Nerves attached to the spinal cord are called spinal nerves. The Efferent Division is broken into Somatic & The ANS has a: Autonomic Components (SNS) Somatic System: controls skeletal muscle contractions these can be voluntary (conscious) or sympathetic division involuntary (unconscious) {reflexes}. } antagonistic effects parasympathetic (ANS) Au tonom ic Sys tem: * a.k.a. -

Muscarinic Acetylcholine Receptor
mAChR Muscarinic acetylcholine receptor mAChRs (muscarinic acetylcholine receptors) are acetylcholine receptors that form G protein-receptor complexes in the cell membranes of certainneurons and other cells. They play several roles, including acting as the main end-receptor stimulated by acetylcholine released from postganglionic fibersin the parasympathetic nervous system. mAChRs are named as such because they are more sensitive to muscarine than to nicotine. Their counterparts are nicotinic acetylcholine receptors (nAChRs), receptor ion channels that are also important in the autonomic nervous system. Many drugs and other substances (for example pilocarpineand scopolamine) manipulate these two distinct receptors by acting as selective agonists or antagonists. Acetylcholine (ACh) is a neurotransmitter found extensively in the brain and the autonomic ganglia. www.MedChemExpress.com 1 mAChR Inhibitors & Modulators (+)-Cevimeline hydrochloride hemihydrate (-)-Cevimeline hydrochloride hemihydrate Cat. No.: HY-76772A Cat. No.: HY-76772B Bioactivity: Cevimeline hydrochloride hemihydrate, a novel muscarinic Bioactivity: Cevimeline hydrochloride hemihydrate, a novel muscarinic receptor agonist, is a candidate therapeutic drug for receptor agonist, is a candidate therapeutic drug for xerostomia in Sjogren's syndrome. IC50 value: Target: mAChR xerostomia in Sjogren's syndrome. IC50 value: Target: mAChR The general pharmacol. properties of this drug on the The general pharmacol. properties of this drug on the gastrointestinal, urinary, and reproductive systems and other… gastrointestinal, urinary, and reproductive systems and other… Purity: >98% Purity: >98% Clinical Data: No Development Reported Clinical Data: No Development Reported Size: 10mM x 1mL in DMSO, Size: 10mM x 1mL in DMSO, 1 mg, 5 mg 1 mg, 5 mg AC260584 Aclidinium Bromide Cat. No.: HY-100336 (LAS 34273; LAS-W 330) Cat. -

Viewed the Existence of Multiple Muscarinic CNS Penetration May Occur When the Blood-Brain Barrier Receptors in the Mammalian Myocardium and Have Is Compromised
BMC Pharmacology BioMed Central Research article Open Access In vivo antimuscarinic actions of the third generation antihistaminergic agent, desloratadine G Howell III†1, L West†1, C Jenkins2, B Lineberry1, D Yokum1 and R Rockhold*1 Address: 1Department of Pharmacology and Toxicology, University of Mississippi Medical Center, Jackson, MS 39216, USA and 2Tougaloo College, Tougaloo, MS, USA Email: G Howell - [email protected]; L West - [email protected]; C Jenkins - [email protected]; B Lineberry - [email protected]; D Yokum - [email protected]; R Rockhold* - [email protected] * Corresponding author †Equal contributors Published: 18 August 2005 Received: 06 October 2004 Accepted: 18 August 2005 BMC Pharmacology 2005, 5:13 doi:10.1186/1471-2210-5-13 This article is available from: http://www.biomedcentral.com/1471-2210/5/13 © 2005 Howell et al; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Abstract Background: Muscarinic receptor mediated adverse effects, such as sedation and xerostomia, significantly hinder the therapeutic usefulness of first generation antihistamines. Therefore, second and third generation antihistamines which effectively antagonize the H1 receptor without significant affinity for muscarinic receptors have been developed. However, both in vitro and in vivo experimentation indicates that the third generation antihistamine, desloratadine, antagonizes muscarinic receptors. To fully examine the in vivo antimuscarinic efficacy of desloratadine, two murine and two rat models were utilized. The murine models sought to determine the efficacy of desloratadine to antagonize muscarinic agonist induced salivation, lacrimation, and tremor. -

P2 Receptor-Mediated Modulation of Neurotransmitter Release—An Update
Purinergic Signalling (2007) 3:269–284 DOI 10.1007/s11302-007-9080-0 ORIGINAL ARTICLE P2 receptor-mediated modulation of neurotransmitter release—an update Beáta Sperlágh & Attila Heinrich & Cecilia Csölle Received: 13 July 2007 /Accepted: 28 August 2007 / Published online: 9 October 2007 # Springer Science + Business Media B.V. 2007 Abstract Presynaptic nerve terminals are equipped with a ENPP ectonucleotide pyrophosphatase number of presynaptic auto- and heteroreceptors, including EJP excitatory junction potential ionotropic P2X and metabotropic P2Y receptors. P2 recep- ENTPDase ectonucleoside triphosphate diphosphohydro- tors serve as modulation sites of transmitter release by ATP lase and other nucleotides released by neuronal activity and EPP end plate potential pathological signals. A wide variety of P2X and P2Y EPSC excitatory postsynaptic current receptors expressed at pre- and postsynaptic sites as well as EPSP excitatory postsynaptic potential in glial cells are involved directly or indirectly in the GABA +-aminobutyric acid modulation of neurotransmitter release. Nucleotides are GPCR G-protein coupled receptor released from synaptic and nonsynaptic sites throughout the IL-1β interleukin-1β nervous system and might reach concentrations high enough IPSC inhibitory postsynaptic current to activate these receptors. By providing a fine-tuning LC locus coeruleus mechanism these receptors also offer attractive sites for LPS lipopolysaccharide pharmacotherapy in nervous system diseases. Here we mEPP miniature EPP review the rapidly emerging data on the modulation of mEPSC miniature EPSC transmitter release by facilitatory and inhibitory P2 receptors NA noradrenaline and the receptor subtypes involved in these interactions. NMJ neuromuscular junction NT neurotransmitter Keywords Neuromodulation . Presynaptic . P2X receptor . NTS nucleus tractus solitarii P2Y receptors . -

Muscarinic Cholinergic Receptors in Developing Rat Lung
1136 WHITSETT AND HOLLINGER Am J Obstet Gynecol 126:956 Michaelis LL 1978 The effects of arterial COztension on regional myocardial 2. Belik J, Wagerle LC, Tzimas M, Egler JM, Delivoria-Papadopoulos M 1983 and renal blood flow: an experimental study. J Surg Res 25:312 Cerebral blood flow and metabolism following pancuronium paralysis in 18. Leahy FAN. Cates D. MacCallum M. Rigatto H 1980 Effect of COz and 100% newborn lambs. Pediatr Res 17: 146A (abstr) O2 on cerebral blood flow in preterm infants. J Appl Physiol48:468 3. Berne RM, Winn HR, Rubio R 1981 The local regulation of cerebral blood 19. Norman J, MacIntyre J, Shearer JR, Craigen IM, Smith G 1970 Effect of flow. Prog Cardiovasc Dis 24:243 carbon dioxide on renal blood flow. Am J Physiol 219:672 4. Brann AW Jr, Meyers RE 1975 Central nervous system findings in the newborn 20. Nowicki PT, Stonestreet BS, Hansen NB, Yao AC, Oh W 1983 Gastrointestinal monkey following severe in utero partial asphyxia. Neurology 25327 blood flow and oxygen in awake newborn piglets: the effect of feeding. Am 5. Bucciarelli RL, Eitzman DV 1979 Cerebral blood flow during acute acidosis J Physiol245:G697 in perinatal goats. Pediatr Res 13: 178 21. Paulson OB, Olesen J, Christensen MS 1972 Restoration of auto-regulation of 6. Dobbing J, Sands J 1979 Comparative aspects of the brain growth spurt. Early cerebral blood flow by hypocapnia. Neurology 22:286 Hum Dev 3:79 22. Peckham GJ. Fox WW 1978 Physiological factors affecting pulmonary artery 7. Fox WW 1982 Arterial blood gas evaluation and mechanical ventilation in the pressure in infants with persistent pulmonary hypertension.J Pediatr 93: 1005 management of persistent pulmonary hypertension of the neonate. -

Palliative Care
World Health Organisation Essential Medicines List for Children (EMLc); Palliative Care CONSULTATION DOCUMENT Prepared by Anita Aindow Medicines Information Pharmacist Alder Hey Children’s Hospital, Liverpool, UK Dr Lynda Brook Macmillan Consultant in Paediatric Palliative Care Alder Hey Children’s Hospital, Liverpool, UK Acknowledgements Professor Tim Eden Professor of Paediatric Oncology, Royal Manchester Children’s Hospital, Manchester, UK Mr Anthony Nunn, Clinical Director of Pharmacy, Alder Hey Children’s Hospital, Liverpool, UK Dr Suzanne Hill Scientist, Policy, Access and Rational Use: Medicines Policy and Standards World health Authority, Geneva For their help and guidance in the preparation of this document Correspondence to Dr Lynda Brook, Macmillan Consultant in Paediatric Palliative Care Department of Paediatric Oncology, Royal Liverpool Children’s Hospital, Eaton Road, Liverpool, L12 2AP Tel: 0151 252 5187 Fax: 0151 252 5676 E-mail: [email protected] DECLARATION OF CONFLICT OF INTERESTS : None June 2008 WHO EMLc: Palliative Care – June 2008 CONTENTS Abstract 3 Summary of recommendations 5 Background 15 Methods 17 Identification of priorities for pharmacological management in palliative 17 care for children Pharmacological management of identified symptoms 17 Results 19 PRIORITIES FOR PHARMACOLOGICAL MANAGEMENT IN PALLIATIVE CARE FOR 19 CHILDREN ESSENTIAL MEDICINES FOR PHARMACOLOGICAL MANAGEMENT IN PALLIATIVE 23 CARE FOR CHILDREN Fatigue and weakness 24 Pain 29 Anorexia and weight loss 52 Delirium and agitation 55 Breathlessness 61 Nausea and vomiting 68 Constipation 89 Depression 95 Excess respiratory tract secretions 106 Anxiety 113 Appendix 116 2 WHO EMLc: Palliative Care – June 2008 ABSTRACT Background The World Health Organization (WHO) Essential Medicines List for Children (EMLc) aims to promote worldwide equity of access to essential medicines for children and is based on the criteria of safety, efficacy and cost effectiveness. -

Properties of the Venous and Arterial Innervation in the Mesentery
J. Smooth Muscle Res. (2003) 39 (6): 269–279 269 Invited Review Properties of the Venous and Arterial Innervation in the Mesentery David L. KREULEN1 1Department of Physiology, Michigan State University, East Lansing, MI 48824-3320, USA Introduction The neural control of arteries and veins involves interactions between several vasoactive neurotransmitters released from the postganglionic sympathetic nerves and spinal sensory nerves. Sympathetic nerves are primarily vasoconstrictor in their action while the sensory nerves are vasodilatory; a result of the neurotransmitters released by these nerves. Thus, the nervous regulation of the vascular component of systemic blood pressure and of regional blood flow is the summation of vasoconstrictor and vasodilatory influences. Also, although the influence of arterial diameter on systemic blood pressure has received the most attention, venous diameter and compliance also are important in the regulation of blood pressure. The nervous regulation of blood flow and blood pressure depends upon the organization of sensory and sympathetic pathways to the vasculature as well as the events at the neuro-effector junctions in artery and vein. The sympathetic and sensory innervation of the mesenteric circulation consists of prevertebral sympathetic ganglion and dorsal root ganglion neurons, respectively. The axons of the neurons travel to the mesenteric arteries and veins in the paravascular nerves, which divide in the adventitia of the blood vessels to form the perivascular nerve plexus. Ultimately these axons divide into terminal axons, lose their Schwann cell sheath, and form neuroeffector junctions with vascular smooth muscle cells (Klemm et al., 1993). Although we know that arteries and veins are innervated by separate sympathetic neurons, all the mechanisms whereby these separate innervations regulate systemic blood pressure are not known. -

Role of Muscarinic Acetylcholine Receptors in Adult Neurogenesis and Cholinergic Seizures
Role of Muscarinic Acetylcholine Receptors in Adult Neurogenesis and Cholinergic Seizures Rebecca L. Kow A dissertation submitted in partial fulfillment of the requirements for the degree of Doctor of Philosophy University of Washington 2014 Reding Committee: Neil Nathanson, Chair Sandra Bajjalieh Joseph Beavo Program Authorized to Offer Degree: Pharmacology ©Copyright 2014 Rebecca L. Kow University of Washington Abstract Role of Muscarinic Acetylcholine Receptors in Adult Neurogenesis and Cholinergic Seizures Rebecca L. Kow Chair of the Supervisory Committee: Professor Neil M. Nathanson Department of Pharmacology Muscarinic acetylcholine receptors (mAChRs) are G protein-coupled receptors (GPCRs) that mediate important functions in the periphery and in the central nervous systems. In the brain these receptors modulate many processes including learning, locomotion, pain, and reward behaviors. In this work we investigated the role of mAChRs in adult neurogenesis and further clarified the regulation of muscarinic agonist-induced seizures. We first investigated the role of mAChRs in adult neurogenesis in the subventricular zone (SVZ) and the subgranular zone (SGZ). We were unable to detect any modulation of adult neurogenesis by mAChRs. Administration of muscarinic agonists or antagonists did not alter proliferation or viability of adult neural progenitor cells (aNPCs) in vitro. Similarly, muscarinic agonists did not alter proliferation or survival of new adult cells in vivo. Loss of the predominant mAChR subtype in the forebrain, the M1 receptor, also caused no alterations in adult neurogenesis in vitro or in vivo, indicating that the M1 receptor does not mediate the actions of endogenous acetylcholine on adult neurogenesis. We also investigated the interaction between mAChRs and cannabinoid receptor 1 (CB1) in muscarinic agonist pilocarpine-induced seizures. -

Neuron Types and Neurotransmitters
Neuron types and Neurotransmitters Faisal I. Mohammed. PhD, MD University of Jordan 1 Objectives Understand synaptic transmission List types of sensory neurons Classify neurotransmitters Explain the mechanism of neurotransmission Judge the types of receptors for the neurotrasmitters University of Jordan 2 Functional Unit (Neuron) 3 Transmission of Receptor Information to the Brain ➢The larger the nerve fiber diameter the faster the rate of transmission of the signal ➢Velocity of transmission can be as fast as 120 m/sec or as slow as 0.5 m/sec ➢Nerve fiber classification ➢type A - myelinated fibers of varying sizes, generally fast transmission speed ➢subdivided into a, b, g, d type B- partially myelinated neurons (3-14m/sec speed) ➢type C - unmyelinated fibers, small with slow transmission speed University of Jordan 4 Types of Nerve Fiber -Myelinated fibers – Type A (types I, II and III) - A α - A β - A γ - A δ -Umyelinated Fibers- Type C (type IV) University of Jordan 5 Neuron Classification University of Jordan 6 Structural Classification of Neurons University of Jordan 7 Neurotransmitters ❖Chemical substances that function as synaptic transmitters 1. Small molecules which act as rapidly acting transmitters ❖acetylcholine, norepinephrine, dopamine, serotonin, GABA, glycine, glutamate, NO 2. Neuropeptides (Neuromodulators) ❖more potent than small molecule transmitters, cause more prolonged actions ❖endorphins, enkephalins, VIP, ect. ❖hypothalamic releasing hormones ❖TRH, LHRH, ect. ❖pituitary peptides ❖ACTH, prolactin, vasopressin, -
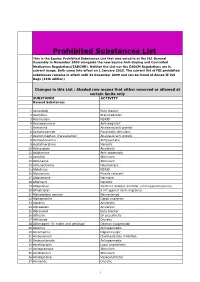
Prohibited Substances List
Prohibited Substances List This is the Equine Prohibited Substances List that was voted in at the FEI General Assembly in November 2009 alongside the new Equine Anti-Doping and Controlled Medication Regulations(EADCMR). Neither the List nor the EADCM Regulations are in current usage. Both come into effect on 1 January 2010. The current list of FEI prohibited substances remains in effect until 31 December 2009 and can be found at Annex II Vet Regs (11th edition) Changes in this List : Shaded row means that either removed or allowed at certain limits only SUBSTANCE ACTIVITY Banned Substances 1 Acebutolol Beta blocker 2 Acefylline Bronchodilator 3 Acemetacin NSAID 4 Acenocoumarol Anticoagulant 5 Acetanilid Analgesic/anti-pyretic 6 Acetohexamide Pancreatic stimulant 7 Acetominophen (Paracetamol) Analgesic/anti-pyretic 8 Acetophenazine Antipsychotic 9 Acetylmorphine Narcotic 10 Adinazolam Anxiolytic 11 Adiphenine Anti-spasmodic 12 Adrafinil Stimulant 13 Adrenaline Stimulant 14 Adrenochrome Haemostatic 15 Alclofenac NSAID 16 Alcuronium Muscle relaxant 17 Aldosterone Hormone 18 Alfentanil Narcotic 19 Allopurinol Xanthine oxidase inhibitor (anti-hyperuricaemia) 20 Almotriptan 5 HT agonist (anti-migraine) 21 Alphadolone acetate Neurosteriod 22 Alphaprodine Opiod analgesic 23 Alpidem Anxiolytic 24 Alprazolam Anxiolytic 25 Alprenolol Beta blocker 26 Althesin IV anaesthetic 27 Althiazide Diuretic 28 Altrenogest (in males and gelidngs) Oestrus suppression 29 Alverine Antispasmodic 30 Amantadine Dopaminergic 31 Ambenonium Cholinesterase inhibition 32 Ambucetamide Antispasmodic 33 Amethocaine Local anaesthetic 34 Amfepramone Stimulant 35 Amfetaminil Stimulant 36 Amidephrine Vasoconstrictor 37 Amiloride Diuretic 1 Prohibited Substances List This is the Equine Prohibited Substances List that was voted in at the FEI General Assembly in November 2009 alongside the new Equine Anti-Doping and Controlled Medication Regulations(EADCMR). -

Drug Repurposing for the Management of Depression: Where Do We Stand Currently?
life Review Drug Repurposing for the Management of Depression: Where Do We Stand Currently? Hosna Mohammad Sadeghi 1,†, Ida Adeli 1,† , Taraneh Mousavi 1,2, Marzieh Daniali 1,2, Shekoufeh Nikfar 3,4,5 and Mohammad Abdollahi 1,2,* 1 Toxicology and Diseases Group (TDG), Pharmaceutical Sciences Research Center (PSRC), The Institute of Pharmaceutical Sciences (TIPS), Tehran University of Medical Sciences, Tehran 1417614411, Iran; [email protected] (H.M.S.); [email protected] (I.A.); [email protected] (T.M.); [email protected] (M.D.) 2 Department of Toxicology and Pharmacology, School of Pharmacy, Tehran University of Medical Sciences, Tehran 1417614411, Iran 3 Personalized Medicine Research Center, Endocrinology and Metabolism Research Institute, Tehran University of Medical Sciences, Tehran 1417614411, Iran; [email protected] 4 Pharmaceutical Sciences Research Center (PSRC) and the Pharmaceutical Management and Economics Research Center (PMERC), Evidence-Based Evaluation of Cost-Effectiveness and Clinical Outcomes Group, The Institute of Pharmaceutical Sciences (TIPS), Tehran University of Medical Sciences, Tehran 1417614411, Iran 5 Department of Pharmacoeconomics and Pharmaceutical Administration, School of Pharmacy, Tehran University of Medical Sciences, Tehran 1417614411, Iran * Correspondence: [email protected] † Equally contributed as first authors. Citation: Mohammad Sadeghi, H.; Abstract: A slow rate of new drug discovery and higher costs of new drug development attracted Adeli, I.; Mousavi, T.; Daniali, M.; the attention of scientists and physicians for the repurposing and repositioning of old medications. Nikfar, S.; Abdollahi, M. Drug Experimental studies and off-label use of drugs have helped drive data for further studies of ap- Repurposing for the Management of proving these medications. -
![[3H]Acetylcholine to Muscarinic Cholinergic Receptors’](https://docslib.b-cdn.net/cover/7448/3h-acetylcholine-to-muscarinic-cholinergic-receptors-1087448.webp)
[3H]Acetylcholine to Muscarinic Cholinergic Receptors’
0270.6474/85/0506-1577$02.00/O The Journal of Neuroscience CopyrIght 0 Smety for Neurosmnce Vol. 5, No. 6, pp. 1577-1582 Prrnted rn U S.A. June 1985 High-affinity Binding of [3H]Acetylcholine to Muscarinic Cholinergic Receptors’ KENNETH J. KELLAR,2 ANDREA M. MARTINO, DONALD P. HALL, Jr., ROCHELLE D. SCHWARTZ,3 AND RICHARD L. TAYLOR Department of Pharmacology, Georgetown University, Schools of Medicine and Dentistry, Washington, DC 20007 Abstract affinities (Birdsall et al., 1978). Evidence for this was obtained using the agonist ligand [3H]oxotremorine-M (Birdsall et al., 1978). High-affinity binding of [3H]acetylcholine to muscarinic Studies of the actions of muscarinic agonists and detailed analy- cholinergic sites in rat CNS and peripheral tissues was meas- ses of binding competition curves between muscarinic agonists and ured in the presence of cytisin, which occupies nicotinic [3H]antagonists have led to the concept of muscarinic receptor cholinergic receptors. The muscarinic sites were character- subtypes (Rattan and Goyal, 1974; Goyal and Rattan, 1978; Birdsall ized with regard to binding kinetics, pharmacology, anatom- et al., 1978). This concept was reinforced by the discovery of the ical distribution, and regulation by guanyl nucleotides. These selective actions and binding properties of the antagonist pirenze- binding sites have characteristics of high-affinity muscarinic pine (Hammer et al., 1980; Hammer and Giachetti, 1982; Watson et cholinergic receptors with a Kd of approximately 30 nM. Most al., 1983; Luthin and Wolfe, 1984). An evolving classification scheme of the muscarinic agonist and antagonist drugs tested have for these muscarinic receptors divides them into M-l and M-2 high affinity for the [3H]acetylcholine binding site, but piren- subtypes (Goyal and Rattan, 1978; for reviews, see Hirschowitz et zepine, an antagonist which is selective for M-l receptors, al., 1984).