Digestive Diseases and Diabetes
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

An Osteopathic Approach to Gastrointestinal Disease
REVIEW An Osteopathic Approach to Gastrointestinal Disease: Somatic Clues for Diagnosis and Clinical Challenges Associated With Helicobacter pylori Antibiotic Resistance Alicia Smilowicz, DO From HealthCalls LLC The estimated prevalence of gastritis in the general US population is approxi- in Portland, Maine, and mately 50%. Patients with gastrointestinal disease often present to the primary the University of New England College of care practitioner with dyspepsia and abdominal pain. Osteopathic palpatory Osteopathic Medicine in evaluation suggests that there is an association among gastrointestinal dis- Biddeford, Maine. ease, the presence of posterior midthoracic pain, and chronic headache. On Financial Disclosures: the basis of findings from a review of the literature, the author assesses the po- None reported. tential etiologic mechanisms of this clinical association. Possible mechanisms Address correspondence to include the physiologic function of the vagus nerve, a neural convergence Alicia Smilowicz, DO, 466 Ocean Ave, Portland, model, and the inherent properties of Helicobacter pylori. To demonstrate the ME 04103-5718. clinical significance of these mechanisms, the author presents the case of a E-mail: docsmilo 30-year-old woman with headache, thoracic discomfort, and gastritis associ- @yahoo.com ated with H pylori infection. The author suggests that successful treatment of Received August 2, 2012; patients with gastrointestinal disease includes osteopathic manipulative treat- revision received November 21, 2012; ment, behavioral modification, and pharmacotherapy, even when challenged accepted by antibiotic resistance. January 6, 2013. J Am Osteopath Assoc. 2013;113(5):404-416 n the practice of clinical medicine, we commonly associate dyspepsia, abdominal pain, nausea, and anorexia with the possible existence of pathologic mechanisms for gastro- Iintestinal disease. -

Epstein–Barr Virus and Helicobacter Pylori Co-Infection in Non-Malignant Gastroduodenal Disorders
pathogens Review Epstein–Barr Virus and Helicobacter Pylori Co-Infection in Non-Malignant Gastroduodenal Disorders Ramsés Dávila-Collado 1, Oscar Jarquín-Durán 1, Le Thanh Dong 2 and J. Luis Espinoza 3,* 1 Faculty of Medicine, UNIDES University, Managua 11001, Nicaragua; [email protected] (R.D.-C.); [email protected] (O.J.-D.) 2 Faculty of Medical Technology, Hanoi Medical University, Hanoi 116001, Vietnam; [email protected] 3 Faculty of Health Sciences, Kanazawa University, Kodatsuno 5-11-80, Kanazawa 920-0942, Ishikawa, Japan * Correspondence: luis@staff.kanazawa-u.ac.jp Received: 20 January 2020; Accepted: 5 February 2020; Published: 6 February 2020 Abstract: Epstein–Barr virus (EBV) and Helicobacter pylori (H. pylori) are two pathogens associated with the development of various human cancers. The coexistence of both microorganisms in gastric cancer specimens has been increasingly reported, suggesting that crosstalk of both pathogens may be implicated in the carcinogenesis process. Considering that chronic inflammation is an initial step in the development of several cancers, including gastric cancer, we conducted a systematic review to comprehensively evaluate publications in which EBV and H. pylori co-infection has been documented in patients with non-malignant gastroduodenal disorders (NMGDs), including gastritis, peptic ulcer disease (PUD), and dyspepsia. We searched the PubMed database up to August 2019, as well as publication references and, among the nine studies that met the inclusion criteria, we identified six studies assessing EBV infection directly in gastric tissues (total 949 patients) and three studies in which EBV infection status was determined by serological methods (total 662 patients). -

Nutrition Care for Persons Infected with the Hepatitis C Virus
HHeeppaattiittiiss CC:: NNuuttrriittiioonn CCaarree QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ QQ CCaannaaddiiaann GGuuiiddeelliinneess ffoorr HHeeaalltthh CCaarree PPrroovviiddeerrss Endorsed by: ♦ Canadian Association for the Study of the Liver ♦ Canadian Association of Hepatology Nurses ♦ Canadian Hemophilia Society ♦ Canadian Liver Foundation ♦ Hepatitis C Society of Canada Funding for the development and Copyright 2003, Dietitians of Canada. dissemination of these guidelines was All rights reserved. provided by Health Canada, Community Acquired Infections Division: This document, as well as an online <www.healthcanada.ca/hepc>. professional education program and patient education handouts, are available from the These guidelines are designed to serve as a Dietitians of Canada website at general framework to assist decision <www.dieteticsatwork.com>. making for nutritional management of Permission is granted to download and patients infected with the hepatitis C virus reproduce the documents in their entirety. and are based on the best information available at the time of publication. The particular needs of individuals infected with Également disponible en français sous le the hepatitis C virus will determine how titre, Hépatite C : Soins nutritionnels – these guidelines are used. The skill and Lignes directrices canadiennes pour les judgement of the health care provider is intervenants de la santé. important in making health care decisions. The opinions expressed in this document do not -

Helicobacter Pylori: Types of Diseases, Diagnosis, Treatment and Causes Of
Journal of Mind and Medical Sciences Volume 3 | Issue 2 Article 7 2016 Helicobacter pylori: types of diseases, diagnosis, treatment and causes of therapeutic failure Cosmin Vasile Obleaga Craiova University of Medicine and Pharmacy, Department of Surgery, [email protected] Cristin Constantin Vere Craiova University of Medicine and Pharmacy, Department of Gastroenterology Ionica Daniel Valcea Craiova University of Medicine and Pharmacy, Department of Surgery Mihai Calin Ciorbagiu Craiova University of Medicine and Pharmacy, Department of Surgery Emil Moraru Craiova University of Medicine and Pharmacy, Department of Surgery See next page for additional authors Follow this and additional works at: http://scholar.valpo.edu/jmms Part of the Digestive System Diseases Commons, Gastroenterology Commons, and the Surgery Commons Recommended Citation Obleaga, Cosmin Vasile; Vere, Cristin Constantin; Valcea, Ionica Daniel; Ciorbagiu, Mihai Calin; Moraru, Emil; and Mirea, Cecil Sorin (2016) "Helicobacter pylori: types of diseases, diagnosis, treatment and causes of therapeutic failure," Journal of Mind and Medical Sciences: Vol. 3 : Iss. 2 , Article 7. Available at: http://scholar.valpo.edu/jmms/vol3/iss2/7 This Review Article is brought to you for free and open access by ValpoScholar. It has been accepted for inclusion in Journal of Mind and Medical Sciences by an authorized administrator of ValpoScholar. For more information, please contact a ValpoScholar staff member at [email protected]. Helicobacter pylori: types of diseases, diagnosis, treatment and causes of therapeutic failure Cover Page Footnote This study was financially supported by the project: "The or le of Helicobacter pylori infection in upper gastrointestinalnon-variceal bleedings. A clinical, endoscopic, serological and histopathological study" sponsored by "The eM dical Center Amaradia"(Contract No. -

A Practical Approach to Management of Acute Pancreatitis: Similarities and Dissimilarities of Disease in Children and Adults
Journal of Clinical Medicine Review A Practical Approach to Management of Acute Pancreatitis: Similarities and Dissimilarities of Disease in Children and Adults Zachary M. Sellers 1 , Monique T. Barakat 1,2 and Maisam Abu-El-Haija 3,4,* 1 Department of Pediatrics, Division of Pediatric Gastroenterology, Hepatology, and Nutrition, Stanford University, Palo Alto, CA 94304, USA; [email protected] (Z.M.S.); [email protected] (M.T.B.) 2 Department of Medicine, Division of Gastroenterology and Hepatology, Stanford University, Palo Alto, CA 94304, USA 3 Division of Pediatric Gastroenterology, Hepatology and Nutrition, Cincinnati Children’s Hospital Medical Center, Cincinnati, OH 45229, USA 4 Department of Pediatrics, College of Medicine, University of Cincinnati, Cincinnati, OH 45221, USA * Correspondence: [email protected]; Tel.: +1-(513)-803-2123; Fax: +1-(513)-487-5528 Abstract: Acute pancreatitis (AP) is associated with significant morbidity and mortality, and it substantially contributes to the healthcare burden of gastrointestinal disease and quality of life in children and adults. AP across the lifespan is characterized by similarities and differences in epidemiology, diagnostic modality, etiologies, management, adverse events, long-term outcomes, and areas in greatest need of research. In this review, we touch on each of these shared and distinctive features of AP in children and adults, with an emphasis on recent advances in the conceptualization Citation: Sellers, Z.M.; Barakat, M.T.; and management of AP. Abu-El-Haija, M. A Practical Approach to Management of Acute Keywords: acute pancreatitis; management; outcomes; gastrointestinal disease Pancreatitis: Similarities and Dissimilarities of Disease in Children and Adults. J. Clin. Med. 2021, 10, 2545. -

Leaky Gut and Gut-Liver Axis in Liver Cirrhosis: Clinical Studies Update
Gut and Liver https://doi.org/10.5009/gnl20032 pISSN 1976-2283 eISSN 2005-1212 Review Article Leaky Gut and Gut-Liver Axis in Liver Cirrhosis: Clinical Studies Update Hiroshi Fukui Department of Gastroenterology, Nara Medical University, Kashihara, Japan Article Info Portal blood flows into the liver containing the gut microbiome and its products such as endotoxin Received January 15, 2020 and bacterial DNA. The cirrhotic liver acts and detoxifies as the initial site of microbial products. Revised June 9, 2020 In so-called “leaky gut,” the increased intestinal permeability for bacteria and their products con- Accepted June 9, 2020 stitutes an important pathogenetic factor for major complications in patients with liver cirrhosis. Published online October 21, 2020 Prolonged gastric and small intestinal transit may induce intestinal bacterial overgrowth, a condi- tion in which colonic bacteria translocate into the small gut. Cirrhotic patients further show gut Corresponding Author dysbiosis characterized by an overgrowth of potentially pathogenic bacteria and a decrease in Hiroshi Fukui autochthonous nonpathogenic bacteria. Pathological bacterial translocation (BT) is a contributing ORCID https://orcid.org/0000-0003-1832-7338 factor in the development of various severe complications. Bile acids (BAs) undergo extensive E-mail [email protected] enterohepatic circulation and play important roles in the gut-liver axis. BT-induced inflammation prevents synthesis of BAs in the liver through inhibition of BA-synthesizing enzyme CYP7A1. A lower abundance of 7α-dehydroxylating gut bacteria leads to decreased conversion of primary to secondary BAs. Decreases in total and secondary BAs may play an important role in the gut dysbiosis characterized by a proinflammatory and toxic gut microbiome inducing BT and endo- toxemia, as addressed in my previous reviews. -

Diagnosis and Management of Autoimmune Hemolytic Anemia in Patients with Liver and Bowel Disorders
Journal of Clinical Medicine Review Diagnosis and Management of Autoimmune Hemolytic Anemia in Patients with Liver and Bowel Disorders Cristiana Bianco 1 , Elena Coluccio 1, Daniele Prati 1 and Luca Valenti 1,2,* 1 Department of Transfusion Medicine and Hematology, Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico, 20122 Milan, Italy; [email protected] (C.B.); [email protected] (E.C.); [email protected] (D.P.) 2 Department of Pathophysiology and Transplantation, Università degli Studi di Milano, 20122 Milan, Italy * Correspondence: [email protected]; Tel.: +39-02-50320278; Fax: +39-02-50320296 Abstract: Anemia is a common feature of liver and bowel diseases. Although the main causes of anemia in these conditions are represented by gastrointestinal bleeding and iron deficiency, autoimmune hemolytic anemia should be considered in the differential diagnosis. Due to the epidemiological association, autoimmune hemolytic anemia should particularly be suspected in patients affected by inflammatory and autoimmune diseases, such as autoimmune or acute viral hepatitis, primary biliary cholangitis, and inflammatory bowel disease. In the presence of biochemical indices of hemolysis, the direct antiglobulin test can detect the presence of warm or cold reacting antibodies, allowing for a prompt treatment. Drug-induced, immune-mediated hemolytic anemia should be ruled out. On the other hand, the choice of treatment should consider possible adverse events related to the underlying conditions. Given the adverse impact of anemia on clinical outcomes, maintaining a high clinical suspicion to reach a prompt diagnosis is the key to establishing an adequate treatment. Keywords: autoimmune hemolytic anemia; chronic liver disease; inflammatory bowel disease; Citation: Bianco, C.; Coluccio, E.; autoimmune disease; autoimmune hepatitis; primary biliary cholangitis; treatment; diagnosis Prati, D.; Valenti, L. -

What Are the Main Gastrointestinal Concerns for People with LDS?
Many individuals with Loeys-Dietz syndrome (LDS) have gastrointestinal issues, often associated with food allergies. Because each person with LDS is different, it is important to talk with your doctor about what care is right for you. What are the main gastrointestinal concerns for people with LDS? • Food allergies - People may be allergic to one food or to many. A person can be allergic to any type of food, but frequent food allergies include milk, eggs, peanuts, tree nuts, fish, shellfish, soy and wheat. People with LDS are more likely to have food allergies than the general popula- tion. Symptoms range from mild to severe, and may include rashes, trouble breathing, abdominal pain, abnormal bowel movements, poor weight gain, reflux, vomiting, esophageal spasm, and decreased appetite. Food allergy responses range from chronic, low-grade symptoms to acute life- threatening reactions. People with food allergies are frequently prescribed injectable epinephrine (Epi-Pen) to use in emergencies. Instructions for epinephrine use are different for people with LDS than for the general population and should be discussed with your doctor. • Eosinophilic Gastrointestinal Disease (EGID) - Eosinophilic esophagitis, gastroenteritis, and/or colitis - In some individuals, food allergies can result in allergic inflammation in the intestinal lining. When there is intestinal inflammation there are extra white blood cells in the lining of the intestine. These specific white blood cells, known as eosinophils, are active in allergies. You do not have to have other symptoms of food allergies to have EGID. People with LDS are more likely to have this kind of inflammation than the general population. -

The Liver in Pediatric Gastrointestinal Disease
INVITED REVIEW The Liver in Pediatric Gastrointestinal Disease Hanh D. Vo, Jiliu Xu, Simon S. Rabinowitz, Stanley E. Fisher, and Steven M. Schwarz ABSTRACT well-known clinicopathologic associations. This monograph high- Hepatic involvement is often encountered in gastrointestinal (GI) dis- lights important aspects of the pathogenesis, diagnosis, and present eases, in part because of the close anatomic and physiologic relations management of hepatobiliary abnormalities associated with 3 com- between the liver and GI tract. Drainage of the mesenteric blood supply to mon GI disorders in the pediatric population: IBD, celiac disease, the portal vein permits absorbed and/or translocated nutrients, toxins, and cystic fibrosis (CF). Less frequently encountered hepatobiliary bacterial elements, cytokines, and immunocytes to gain hepatic access. manifestations of infectious and autoimmune GI disorders are listed Liver problems in digestive disorders may range from nonspecific hepa- in Table 1, but are beyond the scope of this review. tocellular enzyme elevations to significant pathologic processes that may progress to end-stage liver disease. Hepatobiliary manifestations of primary GI diseases in childhood and adolescence are not uncommon HEPATIC MANIFESTATIONS OF IBD and include several well-described associations, such as sclerosing cho- IBD encompasses a group of chronic inflammatory diseases langitis with inflammatory bowel disease. Liver damage may also result of the GI tract that includes Crohn disease (CD), ulcerative colitis from the effects of drugs used to treat GI diseases, for example, the (UC), and indeterminate colitis. Hepatic and biliary tract abnorm- hepatotoxicity of immunomodulatory therapies. This review highlights alities (Table 2) may represent part of the overall disease process in the important features of the hepatic and biliary abnormalities associated these disorders, or may occur as a consequence of medical therapy. -
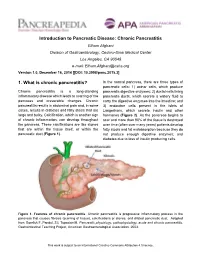
Introduction to Pancreatic Disease
Introduction to Pancreatic Disease: Chronic Pancreatitis Elham Afghani Division of Gastroenterology, Cedars-Sinai Medical Center Los Angeles, CA 90048 e-mail: [email protected] Version 1.0, December 16, 2014 [[DOI: 10.3998/panc.2015.3] 1. What is chronic pancreatitis? In the normal pancreas, there are three types of pancreatic cells: 1) acinar cells, which produce Chronic pancreatitis is a long-standing pancreatic digestive enzymes; 2) ductal cells lining inflammatory disease which leads to scarring of the pancreatic ducts, which secrete a watery fluid to pancreas and irreversible changes. Chronic carry the digestive enzymes into the intestine; and pancreatitis results in abdominal pain and, in some 3) endocrine cells present in the islets of cases, results in diabetes and fatty stools that are Langerhans, which secrete insulin and other large and bulky. Calcification, which is another sign hormones (Figure 2). As the pancreas begins to of chronic inflammation, can develop throughout scar and more than 90% of the tissue is destroyed the pancreas. These calcifications are like stones over time (often over many years) patients develop that are within the tissue itself, or within the fatty stools and fat malabsorption because they do pancreatic duct (Figure 1). not produce enough digestive enzymes; and diabetes due to loss of insulin producing cells. Figure 1. Features of chronic pancreatitis. Chronic pancreatitis is progressive inflammatory process in the pancreas that causes fibrosis (scarring of tissue), calcifications or stones, and dilated pancreatic duct. Adapted from Gorelick F, Pandol, SJ, Topazian M. Pancreatic physiology, pathophysiology, acute and chronic pancreatitis. Gastrointestinal Teaching Project, American Gastroenterological Association. -

Gastrointestinal Manifestations of Systemic Sclerosis Isabel M
Cur gy: ren lo t o R t e a s e m McFarlane et al., Rheumatology (Sunnyvale) 2018, a u r c e h h 8:1 R Rheumatology: Current Research DOI: 10.4172/2161-1149.1000235 ISSN: 2161-1149 Review Article Open Access Gastrointestinal Manifestations of Systemic Sclerosis Isabel M. McFarlane*, Manjeet S. Bhamra, Alexandra Kreps, Sadat Iqbal, Firas Al-Ani, Carla Saladini-Aponte, Christon Grant, Soberjot Singh, Khalid Awwal, Kristaq Koci DO, Yair Saperstein, Fray M. Arroyo-Mercado, Derek B. Laskar and Purna Atluri Division of Rheumatology and Gastroenterology, Department of Medicine and Pathology, State University of New York, Hospitals Kings County Hospital Brooklyn, USA *Corresponding author: Isabel M. McFarlane, Clinical Assistant Professor of Medicine Associate Program Director Residency Program, Department of Medicine, Division of Rheumatology SUNY Downstate, Brooklyn, USA, Tel: 718-221-6515; Email: [email protected] Received date: January 26, 2018; Accepted date: March 27, 2018; Published date: March 30, 2018 Copyright: ©2018 McFarlane IM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Systemic sclerosis (SSc) is a rare autoimmune disease characterized by fibroproliferative alterations of the microvasculature leading to fibrosis and loss of function of the skin and internal organs. Gastrointestinal manifestations of SSc are the most commonly encountered complications of the disease affecting nearly 90% of the SSc population. Among these complications, the esophagus and the anorectum are the most commonly affected. However, this devastating disorder does not spare any part of the gastrointestinal tract (GIT), and includes the oral cavity, esophagus, stomach, small and large bowels as well as the liver and pancreas. -

Biliary Pain Work-Up and Management in General Practice Michael Crawford
The right upper quadrant Biliary pain Work-up and management in general practice Michael Crawford Background Pain arising from the gallbladder and biliary tree is a Pain arising from the gallbladder and biliary tree is a common common presentation in general practice. Differentiating clinical presentation. Differentiation from other causes of biliary pain from other causes of abdominal pain can abdominal pain can sometimes be difficult. sometimes be difficult. There is substantial variability in the type, duration and associations of pain arising from the Objective gallbladder. Furthermore, there is overlap with a number This article discusses the work-up, management and after care of of other common abdominal conditions, such as peptic patients with biliary pain. ulcer disease, gastro-oesophageal reflux and irritable Discussion bowel syndrome. It is often not possible to be certain that The role for surgery for gallstones and gallbladder polyps is a particular symptom is related to gallbladder pathology described. Difficulties in the diagnosis and management before cholecystectomy. of gallbladder pain are discussed. Intra- and post-operative complications are described, along with their management. The Clinical presentations of pain issue of post-operative pain in particular is examined, focusing Gallstones on the timing of the pain and the relevant investigations. Gallstones are a common problem, with an estimated prevalence of Keywords 25–30% in Australians over the age of 50 years.1 Risk factors for the general surgery; gastrointestinal disease; gallbladder; biliary development of gallstones include: tract; pain • female gender • increasing age • family history • rapid changes in weight • ethnicity. Most people with gallstones do not experience pain, with only about 6% undergoing a cholecystectomy over a 30 year period in one observational study.2 Confirming that the gallbladder is the source of pain can be challenging.