Introduction to Pancreatic Disease
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Acute Pancreatitis Associated with Rotavirus Infection and Review Of
Case Report/Olgu Sunumu İstanbul Med J 2020; 21(1): 78-81 DO I: 10.4274/imj.galenos.2020.88319 Acute Pancreatitis Associated with Rotavirus Infection and Review of The Literature Rotavirüs Enfeksiyonuna Bağlı Akut Pankreatit Olguları ve Literatürün Gözden Geçirilmesi Kamil Şahin, Güzide Doğan University of Health Sciences, Haseki Training and Research Hospital, Department of Pediatrics, İstanbul, Turkey ABSTRACT ÖZ Agents causing acute gastroenteritis are not common causes of Çocuklarda pankreatit etiyolojisinde akut gastroenterit etkenleri pancreatitis etiology in children. Pancreatitis associated with sık görülen sebeplerden değildir. Rotavirüs enfeksiyonuna rotavirus infection is very rare. Cases with acute pancreatitis bağlı görülen pankreatit ise oldukça nadirdir. Rotavirüs during rotavirus gastroenteritis are reported due to rare gastroenteriti sırasında akut pankreatit gelişen olgular, associations. In this article, the causes of acute pancreatitis rotavirüs enfeksiyonuna bağlı akut pankreatitin nadir olması and cases of acute pancreatitis due to rotavirus infection were nedeniyle sunulmuştur. Bu yazıda, akut pankreatit sebepleri ve investigated. Clinical findings were mild, and complications rotavirüse bağlı gelişen akut pankreatit olguları incelenmiştir. were not observed in both of our patients, including a two- İki yaş kız ve üç yaşındaki erkek iki olgumuzda ve literatürde year-old female and a three-year-old male, and other cases değerlendirilen diğer olgularda klinik bulgular hafif seyretmiş, evaluated in the literature. The -

Chronic Pancreatitis. 2
Module "Fundamentals of diagnostics, treatment and prevention of major diseases of the digestive system" Practical training: "Chronic pancreatitis (CP)" Topicality The incidence of chronic pancreatitis is 4.8 new cases per 100 000 of population per year. Prevalence is 25 to 30 cases per 100 000 of population. Total number of patients with CP increased in the world by 2 times for the last 30 years. In Ukraine, the prevalence of diseases of the pancreas (CP) increased by 10.3%, and the incidence increased by 5.9%. True prevalence rate of CP is difficult to establish, because diagnosis is difficult, especially in initial stages. The average time of CP diagnosis ranges from 30 to 60 months depending on the etiology of the disease. Learning objectives: to teach students to recognize the main symptoms and syndromes of CP; to familiarize students with physical examination methods of CP; to familiarize students with study methods used for the diagnosis of CP, the determination of incretory and excretory pancreatic insufficiency, indications and contraindications for their use, methods of their execution, the diagnostic value of each of them; to teach students to interpret the results of conducted study; to teach students how to recognize and diagnose complications of CP; to teach students how to prescribe treatment for CP. What should a student know? Frequency of CP; Etiological factors of CP; Pathogenesis of CP; Main clinical syndromes of CP, CP classification; General and alarm symptoms of CP; Physical symptoms of CP; Methods of -

An Osteopathic Approach to Gastrointestinal Disease
REVIEW An Osteopathic Approach to Gastrointestinal Disease: Somatic Clues for Diagnosis and Clinical Challenges Associated With Helicobacter pylori Antibiotic Resistance Alicia Smilowicz, DO From HealthCalls LLC The estimated prevalence of gastritis in the general US population is approxi- in Portland, Maine, and mately 50%. Patients with gastrointestinal disease often present to the primary the University of New England College of care practitioner with dyspepsia and abdominal pain. Osteopathic palpatory Osteopathic Medicine in evaluation suggests that there is an association among gastrointestinal dis- Biddeford, Maine. ease, the presence of posterior midthoracic pain, and chronic headache. On Financial Disclosures: the basis of findings from a review of the literature, the author assesses the po- None reported. tential etiologic mechanisms of this clinical association. Possible mechanisms Address correspondence to include the physiologic function of the vagus nerve, a neural convergence Alicia Smilowicz, DO, 466 Ocean Ave, Portland, model, and the inherent properties of Helicobacter pylori. To demonstrate the ME 04103-5718. clinical significance of these mechanisms, the author presents the case of a E-mail: docsmilo 30-year-old woman with headache, thoracic discomfort, and gastritis associ- @yahoo.com ated with H pylori infection. The author suggests that successful treatment of Received August 2, 2012; patients with gastrointestinal disease includes osteopathic manipulative treat- revision received November 21, 2012; ment, behavioral modification, and pharmacotherapy, even when challenged accepted by antibiotic resistance. January 6, 2013. J Am Osteopath Assoc. 2013;113(5):404-416 n the practice of clinical medicine, we commonly associate dyspepsia, abdominal pain, nausea, and anorexia with the possible existence of pathologic mechanisms for gastro- Iintestinal disease. -

Treatment Recommendations for Feline Pancreatitis
Treatment recommendations for feline pancreatitis Background is recommended. Fentanyl transdermal patches have become Pancreatitis is an elusive disease in cats and consequently has popular for pain relief because they provide a longer duration of been underdiagnosed. This is owing to several factors. Cats with analgesia. It takes at least 6 hours to achieve adequate fentanyl pancreatitis present with vague signs of illness, including lethargy, levels for pain control; therefore, one recommended protocol is to decreased appetite, dehydration, and weight loss. Physical administer another analgesic, such as intravenous buprenorphine, examination and routine laboratory findings are nonspecific, and at the time the fentanyl patch is placed. The cat is then monitored until recently, there have been limited diagnostic tools available closely to see if additional pain medication is required. Cats with to the practitioner for noninvasively diagnosing pancreatitis. As a chronic pancreatitis may also benefit from pain management, and consequence of the difficulty in diagnosing the disease, therapy options for outpatient treatment include a fentanyl patch, sublingual options are not well understood. buprenorphine, oral butorphanol, or tramadol. Now available, the SNAP® fPL™ and Spec fPL® tests can help rule Antiemetic therapy in or rule out pancreatitis in cats presenting with nonspecific signs Vomiting, a hallmark of pancreatitis in dogs, may be absent or of illness. As our understanding of this disease improves, new intermittent in cats. When present, vomiting should be controlled; specific treatment modalities may emerge. For now, the focus is and if absent, treatment with an antiemetic should still be on managing cats with this disease, and we now have the tools considered to treat nausea. -
Pancreatic Disorders in Inflammatory Bowel Disease
Submit a Manuscript: http://www.wjgnet.com/esps/ World J Gastrointest Pathophysiol 2016 August 15; 7(3): 276-282 Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx ISSN 2150-5330 (online) DOI: 10.4291/wjgp.v7.i3.276 © 2016 Baishideng Publishing Group Inc. All rights reserved. MINIREVIEWS Pancreatic disorders in inflammatory bowel disease Filippo Antonini, Raffaele Pezzilli, Lucia Angelelli, Giampiero Macarri Filippo Antonini, Giampiero Macarri, Department of Gastro- acute pancreatitis or chronic pancreatitis has been rec enterology, A.Murri Hospital, Polytechnic University of Marche, orded in patients with inflammatory bowel disease (IBD) 63900 Fermo, Italy compared to the general population. Although most of the pancreatitis in patients with IBD seem to be related to Raffaele Pezzilli, Department of Digestive Diseases and Internal biliary lithiasis or drug induced, in some cases pancreatitis Medicine, Sant’Orsola-Malpighi Hospital, 40138 Bologna, Italy were defined as idiopathic, suggesting a direct pancreatic Lucia Angelelli, Medical Oncology, Mazzoni Hospital, 63100 damage in IBD. Pancreatitis and IBD may have similar Ascoli Piceno, Italy presentation therefore a pancreatic disease could not be recognized in patients with Crohn’s disease and ulcerative Author contributions: Antonini F designed the research; Antonini colitis. This review will discuss the most common F and Pezzilli R did the data collection and analyzed the data; pancreatic diseases seen in patients with IBD. Antonini F, Pezzilli R and Angelelli L wrote the paper; Macarri G revised the paper and granted the final approval. Key words: Pancreas; Pancreatitis; Extraintestinal mani festations; Exocrine pancreatic insufficiency; Ulcerative Conflictofinterest statement: The authors declare no conflict colitis; Crohn’s disease; Inflammatory bowel disease of interest. -
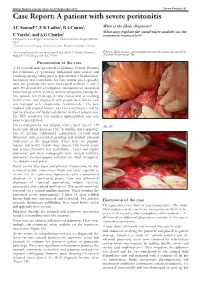
Case Report: a Patient with Severe Peritonitis
Malawi Medical Journal; 25(3): 86-87 September 2013 Severe Peritonitis 86 Case Report: A patient with severe peritonitis J C Samuel1*, E K Ludzu2, B A Cairns1, What is the likely diagnosis? 2 1 What may explain the small white nodules on the C Varela , and A G Charles transverse mesocolon? 1 Department of Surgery, University of North Carolina, Chapel Hill NC USA 2 Department of Surgery, Kamuzu Central Hospital, Lilongwe Malawi Corresponding author: [email protected] 4011 Burnett Womack Figure1. Intraoperative photograph showing the transverse mesolon Bldg CB 7228, Chapel Hill NC 27599 (1a) and the pancreas (1b). Presentation of the case A 42 year-old male presented to Kamuzu Central Hospital for evaluation of worsening abdominal pain, nausea and vomiting starting 3 days prior to presentation. On admission, his history was remarkable for four similar prior episodes over the previous five years that lasted between 3 and 5 days. He denied any constipation, obstipation or associated hematemesis, fevers, chills or urinary symptoms. During the first episode five years ago, he was evaluated at an outlying health centre and diagnosed with peptic ulcer disease and was managed with omeprazole intermittently . His past medical and surgical history was non contributory and he had no allergies and he denied alcohol intake or tobacco use. His HIV serostatus was negative approximately one year prior to presentation. On examination he was afebrile, with a heart rate of 120 (Fig 1B) beats/min, blood pressure 135/78 mmHg and respiratory rate of 22/min. Abdominal examination revealed mild distension with generalized guarding and marked rebound tenderness in the epigastrium. -

Epstein–Barr Virus and Helicobacter Pylori Co-Infection in Non-Malignant Gastroduodenal Disorders
pathogens Review Epstein–Barr Virus and Helicobacter Pylori Co-Infection in Non-Malignant Gastroduodenal Disorders Ramsés Dávila-Collado 1, Oscar Jarquín-Durán 1, Le Thanh Dong 2 and J. Luis Espinoza 3,* 1 Faculty of Medicine, UNIDES University, Managua 11001, Nicaragua; [email protected] (R.D.-C.); [email protected] (O.J.-D.) 2 Faculty of Medical Technology, Hanoi Medical University, Hanoi 116001, Vietnam; [email protected] 3 Faculty of Health Sciences, Kanazawa University, Kodatsuno 5-11-80, Kanazawa 920-0942, Ishikawa, Japan * Correspondence: luis@staff.kanazawa-u.ac.jp Received: 20 January 2020; Accepted: 5 February 2020; Published: 6 February 2020 Abstract: Epstein–Barr virus (EBV) and Helicobacter pylori (H. pylori) are two pathogens associated with the development of various human cancers. The coexistence of both microorganisms in gastric cancer specimens has been increasingly reported, suggesting that crosstalk of both pathogens may be implicated in the carcinogenesis process. Considering that chronic inflammation is an initial step in the development of several cancers, including gastric cancer, we conducted a systematic review to comprehensively evaluate publications in which EBV and H. pylori co-infection has been documented in patients with non-malignant gastroduodenal disorders (NMGDs), including gastritis, peptic ulcer disease (PUD), and dyspepsia. We searched the PubMed database up to August 2019, as well as publication references and, among the nine studies that met the inclusion criteria, we identified six studies assessing EBV infection directly in gastric tissues (total 949 patients) and three studies in which EBV infection status was determined by serological methods (total 662 patients). -

Pancreatic Resection: Nutritional Implications and Long Term Follow Up
NUTRITION ISSUES IN GASTROENTEROLOGY, SERIES #150 NUTRITION ISSUES IN GASTROENTEROLOGY, SERIES #150 Carol Rees Parrish, M.S., R.D., Series Editor Pancreatic Resection: Nutritional Implications and Long Term Follow Up Mary E. Phillips Pancreatic resection is carried out for benign and malignant diseases of the pancreas, duodenum and distal common bile duct. These operations contribute significantly to both macro-nutrient and micro-nutrient malabsorption. Pancreatic enzyme supplements are underused and should be administered routinely to all patients who have had a pancreatic head resection. Patients suffer both short term and long term deficiencies and are prone to other gastro-intestinal conditions with similar symptoms. Thus, identifying the cause of their symptoms is challenging and requires careful follow up in a multi-professional setting. Vitamin and mineral deficiencies are common and weight loss, abdominal symptoms and diabetes have a significant impact on quality of life and survival. Patients should have access to specialist dietetic support and endocrine function should be assessed routinely following all pancreatic resection. Assessment of vitamin and mineral status should be carried out in patients who have undergone curative resection or who have benign disease. INTRODUCTION ypes of pancreatic resections vary considerably; poor, but some pancreatic resections are carried out each having a different impact on the digestive for benign disease, and long term implications must Tsystem and therefore on the patient’s nutritional be considered in all patients with benign disease, and status. Poor nutritional status is associated with poor those who have had surgery with curative intent. quality of life,1 and reduced survival.2 Pancreatic Fat, carbohydrate and protein malabsorption all exocrine insufficiency (PEI) is common and occur in PEI;5-7 yet historical treatment has focused on fat undertreated3 and there is a lack of funding for dietetic malabsorption. -

Download PDF the Differential Diagnosis of Chronic Pancreatitis
Current Health Sciences Journal Vol. 35, No. 3, 2009 Original Paper The Differential Diagnosis of Chronic Pancreatitis (1) (1) (1) (1) D.I. GHEONEA , P. VILMANN , A SĂFTOIU , T. CIUREA , D. (1) (1) PÎRVU , MIHNEA IONESCU (1) Department of Gastroenterology, University of Medicine and Pharmacy Craiova, România; (1) Department of Surgical Gastroenterology, Gentofte University Hospital, Hellerup, Denmark ABSTRACT BACKGROUND Chronic pancreatitis is an inflammatory disease of the pancreas with a physiopathology that is yet to be fully understood, with a multifactorial etiology, of which alcohol abuse causes the majority of cases. PATIENTS AND METHOD We included 80 patients diagnosed with chronic pancreatitis, admitted in the Gastroenterology Clinic of the University of Medicine and Pharmacy Craiova. In each patient, demographic parameters, family and personal history were recorded. All patients were initially evaluated by transabdominal ultrasound. In selected cases other imagistic methods were used: computed tomography, endoscopic ultrasound with fine needle aspiration, endoscopic retrograde cholangiopancreatography. RESULTS The mean age in the studied group ranged between 26 and 76 years with a mean age of 52.9 years. The male to female ratio was 3.6:1. The most frequent presenting symptom was abdominal pain (93.75%), followed by fatigue (70%), anorexia (50%); fewer patients presented with emesis, loss of weight, diarrhea, meteorism and flatulence. The most frequent etiologic factor of chronic pancreatitis in the studied group was alcohol abuse. Using imaging methods the following complications of chronic pancreatitis were diagnosed in the studied group: complicated or uncomplicated pseudocysts (31.57%), pancreatic cancer (18.75%), obstructive jaundice (10%), segmental portal hypertension (2.5%), and pseudoaneurysm (1.25%).CONCLUSSIONS Transabdominal ultrasound is quite accurate in diagnosing chronic pancreatitis and its morbidities and its non-invasiveness makes it the method of choice in the initial assessment of the disease. -

ESPEN Guideline on Clinical Nutrition in Acute and Chronic Pancreatitis
Clinical Nutrition 39 (2020) 612e631 Contents lists available at ScienceDirect Clinical Nutrition journal homepage: http://www.elsevier.com/locate/clnu ESPEN Guideline ESPEN guideline on clinical nutrition in acute and chronic pancreatitis * Marianna Arvanitakis a, , Johann Ockenga b, Mihailo Bezmarevic c, Luca Gianotti d, , Zeljko Krznaric e, Dileep N. Lobo f g, Christian Loser€ h, Christian Madl i, Remy Meier j, Mary Phillips k, Henrik Højgaard Rasmussen l, Jeanin E. Van Hooft m, Stephan C. Bischoff n a Department of Gastroenterology, Erasme University Hospital ULB, Brussels, Belgium b Department of Gastroenterology, Endocrinology and Clinical Nutrition, Klinikum Bremen Mitte, Bremen, Germany c Department of Hepatobiliary and Pancreatic Surgery, Clinic for General Surgery, Military Medical Academy, University of Defense, Belgrade, Serbia d School of Medicine and Surgery, University of Milano-Bicocca and Department of Surgery, San Gerardo Hospital, Monza, Italy e Department of Gastroenterology, Hepatology and Nutrition, Clinical Hospital Centre & School of Medicine, Zagreb, Croatia f Gastrointestinal Surgery, Nottingham Digestive Diseases Centre, National Institute for Health Research. (NIHR) Nottingham Biomedical Research Centre, Nottingham University Hospitals NHS Trust, University of Nottingham, Queen's Medical Centre, Nottingham, NG7 2UH, UK g MRC Versus Arthritis Centre for Musculoskeletal Ageing Research, School of Life Sciences, University of Nottingham, Queen's Medical Centre, Nottingham NG7 2UH, UK h Medical Clinic, DRK-Kliniken -

Clinical Biliary Tract and Pancreatic Disease
Clinical Upper Gastrointestinal Disorders in Urgent Care, Part 2: Biliary Tract and Pancreatic Disease Urgent message: Upper abdominal pain is a common presentation in urgent care practice. Narrowing the differential diagnosis is sometimes difficult. Understanding the pathophysiology of each disease is the key to making the correct diagnosis and providing the proper treatment. TRACEY Q. DAVIDOFF, MD art 1 of this series focused on disorders of the stom- Pach—gastritis and peptic ulcer disease—on the left side of the upper abdomen. This article focuses on the right side and center of the upper abdomen: biliary tract dis- ease and pancreatitis (Figure 1). Because these diseases are regularly encountered in the urgent care center, the urgent care provider must have a thorough understand- ing of them. Biliary Tract Disease The gallbladder’s main function is to concentrate bile by the absorption of water and sodium. Fasting retains and concentrates bile, and it is secreted into the duodenum by eating. Impaired gallbladder contraction is seen in pregnancy, obesity, rapid weight loss, diabetes mellitus, and patients receiving total parenteral nutrition (TPN). About 10% to 15% of residents of developed nations will form gallstones in their lifetime.1 In the United States, approximately 6% of men and 9% of women 2 have gallstones. Stones form when there is an imbal- ©Phototake.com ance in the chemical constituents of bile, resulting in precipitation of one or more of the components. It is unclear why this occurs in some patients and not others, Tracey Q. Davidoff, MD, is an urgent care physician at Accelcare Medical Urgent Care in Rochester, New York, is on the Board of Directors of the although risk factors do exist. -

Research Article Nonalcoholic Fatty Liver Disease Aggravated the Severity of Acute Pancreatitis in Patients
Hindawi BioMed Research International Volume 2019, Article ID 9583790, 7 pages https://doi.org/10.1155/2019/9583790 Research Article Nonalcoholic Fatty Liver Disease Aggravated the Severity of Acute Pancreatitis in Patients Dacheng Wu,1 Min Zhang,1 Songxin Xu,1 Keyan Wu,1 Ningzhi Wang,1 Yuanzhi Wang,1 Jian Wu,1 Guotao Lu ,1 Weijuan Gong,1,2 Yanbing Ding ,1 and Weiming Xiao 1 Department of Gastroenterology, Affiliated Hospital of Yangzhou University, Yangzhou University, No. Hanjiang Media Road, Yangzhou ,Jiangsu,China Department of Immunology, School of Medicine, Yangzhou University, Yangzhou, China Correspondence should be addressed to Yanbing Ding; [email protected] and Weiming Xiao; [email protected] Received 17 October 2018; Accepted 3 January 2019; Published 22 January 2019 Guest Editor: Marina Berenguer Copyright © 2019 Dacheng Wu et al. Tis is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Background and Aim. Te incidence of nonalcoholic fatty liver disease (NAFLD) as a metabolic disease is increasing annually. In the present study, we aimed to explore the infuence of NAFLD on the severity of acute pancreatitis (AP). Methods.Teseverity of AP was diagnosed and analyzed according to the 2012 revised Atlanta Classifcation. Outcome variables, including the severity of AP, organ failure (all types of organ failure), and systemic infammatory response syndrome (SIRS), were compared for patients with and without NAFLD. Results. Six hundred and ffy-six patients were enrolled in the study and were divided into two groups according to the presence or absence of NAFLD.