Compartment Syndromes
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Conventional Explosions and Blast Injuries 7
Chapter 7: CONVENTIONAL EXPLOSIONS AND BLAST INJURIES David J. Dries, MSE, MD, FCCM David Bracco, MD, EDIC, FCCM Tarek Razek, MD Norma Smalls-Mantey, MD, FACS, FCCM Dennis Amundson, DO, MS, FCCM Objectives ■ Describe the mechanisms of injury associated with conventional explosions. ■ Outline triage strategies and markers of severe injury in patients wounded in conventional explosions. ■ Explain the general principles of critical care and procedural support in mass casualty incidents caused by conventional explosions. ■ Discuss organ-specific support for victims of conventional explosions. Case Study Construction workers are using an acetylene/oxygen mixture to do some welding work in a crowded nearby shopping mall. Suddenly, an explosion occurs, shattering windows in the mall and on the road. The acetylene tank seems to be at the origin of the explosion. The first casualties arrive at the emergency department in private cars and cabs. They state that at the scene, blood and injured people are everywhere. - What types of patients do you expect? - How many patients do you expect? - When will the most severely injured patients arrive? - What is your triage strategy, and how will you triage these patients? - How do you initiate care in victims of conventional explosions? Fundamental Disaster Management I . I N T R O D U C T I O N Detonation of small-volume, high-intensity explosives is a growing threat to civilian as well as military populations. Understanding circumstances surrounding conventional explosions helps with rapid triage and recognition of factors that contribute to poor outcomes. Rapid evacuation of salvageable victims and swift identification of life-threatening injuries allows for optimal resource utilization and patient management. -

Characterizing Explosive Effects on Underground Structures.” Electronic Scientific Notebook 1160E
NUREG/CR-7201 Characterizing Explosive Effects on Underground Structures Office of Nuclear Security and Incident Response AVAILABILITY OF REFERENCE MATERIALS IN NRC PUBLICATIONS NRC Reference Material Non-NRC Reference Material As of November 1999, you may electronically access Documents available from public and special technical NUREG-series publications and other NRC records at libraries include all open literature items, such as books, NRC’s Library at www.nrc.gov/reading-rm.html. Publicly journal articles, transactions, Federal Register notices, released records include, to name a few, NUREG-series Federal and State legislation, and congressional reports. publications; Federal Register notices; applicant, Such documents as theses, dissertations, foreign reports licensee, and vendor documents and correspondence; and translations, and non-NRC conference proceedings NRC correspondence and internal memoranda; bulletins may be purchased from their sponsoring organization. and information notices; inspection and investigative reports; licensee event reports; and Commission papers Copies of industry codes and standards used in a and their attachments. substantive manner in the NRC regulatory process are maintained at— NRC publications in the NUREG series, NRC regulations, The NRC Technical Library and Title 10, “Energy,” in the Code of Federal Regulations Two White Flint North may also be purchased from one of these two sources. 11545 Rockville Pike Rockville, MD 20852-2738 1. The Superintendent of Documents U.S. Government Publishing Office These standards are available in the library for reference Mail Stop IDCC use by the public. Codes and standards are usually Washington, DC 20402-0001 copyrighted and may be purchased from the originating Internet: bookstore.gpo.gov organization or, if they are American National Standards, Telephone: (202) 512-1800 from— Fax: (202) 512-2104 American National Standards Institute 11 West 42nd Street 2. -

Case Report Forearm Compartment Syndrome Following Thrombolytic Therapy for Massive Pulmonary Embolism: a Case Report and Review of Literature
Hindawi Publishing Corporation Case Reports in Orthopedics Volume 2011, Article ID 678525, 4 pages doi:10.1155/2011/678525 Case Report Forearm Compartment Syndrome following Thrombolytic Therapy for Massive Pulmonary Embolism: A Case Report and Review of Literature Ravi Badge and Mukesh Hemmady Department of Trauma and Orthopaedics Surgery, Wrightington, Wigan and Leigh NHS Trust, Wigan WN1 2NN, UK Correspondence should be addressed to Ravi Badge, [email protected] Received 2 November 2011; Accepted 6 December 2011 Academic Editor: M. K. Lyons Copyright © 2011 R. Badge and M. Hemmady. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Use of thrombolytic therapy in pulmonary embolism is restricted in cases of massive embolism. It achieves faster lysis of the thrombus than the conventional heparin therapy thus reducing the morbidity and mortality associated with PE. The compartment syndrome is a well-documented, potentially lethal complication of thrombolytic therapy and known to occur in the limbs involved for vascular lines or venepunctures. The compartment syndrome in a conscious and well-oriented patient is mainly diagnosed on clinical ground with its classical signs and symptoms like disproportionate pain, tense swollen limb and pain on passive stretch. However these findings may not be appropriately assessed in an unconscious patient and therefore the clinicians should have high index of suspicion in a patient with an acutely swollen tense limb. In such scenarios a prompt orthopaedic opinion should be considered. In this report, we present a case of acute compartment syndrome of the right forearm in a 78 years old male patient following repeated attempts to secure an arterial line for initiating the thrombolytic therapy for the management of massive pulmonary embolism. -

Orthopedic Trauma Postoperative Care and Rehab
Orthopedic Trauma Postoperative Care and Rehab Serge Charles Kaska, MD Name that Beach 100$ Still 100$ 75$ 50$ 1$ Omaha • June 6th 1941 • !st Infantry Division • 2000 KIA LIFE OR LIMB THREAT 1. Compartment Syndrome 2. Fat Emboli Syndrome 3. Pulmonary Embolism 4. Shock Compartment syndrome case A 16 year old male was retrieving a tire from his truck bed on the side of the highway in the pouring rain when a car careens off of the road and sandwiches the patients legs between the bumpers at freeway speed. Acute compartment syndrome Compartment syndrome DEFINED Definition: Elevated tissue pressure within a closed fascial space • Pathogenesis – Too much in-flow: results in edema or hemorrhage – Decreased outflow: results in venous obstruction caused by tight dressing and/or cast. • Reduces tissue perfusion • Results in cell death Compartment syndrome tissue survival • Muscle – 3-4 hours: reversible changes – 6 hours: variable damage – 8 hours: irreversible changes • Nerve – 2 hours: looses nerve conduction – 4 hours: neuropraxia – 8 hours: irreversible changes Physical exam 1. Pain 2. Pain 3. Pain Physical exam • Inspection – Swelling, skin is tight and shiny • Motion – Active motion will be refused or unable. Must see dorsiflexion • Palpation – Severe pain with palpation • Alarming pain with passive stretch Physical exam • Dorsiflexion Physical Exam • Palpation – Severe pain with palpation • Alarming pain with passive stretch Physical exam • Evaluations from nurses, therapists, and orthotech’s are CRITICAL • If you call a doctor and say that -
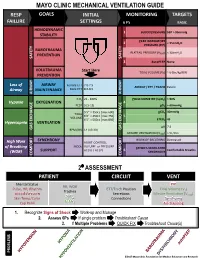
Mechanical Ventilation Guide
MAYO CLINIC MECHANICAL VENTILATION GUIDE RESP GOALS INITIAL MONITORING TARGETS FAILURE SETTINGS 6 P’s BASIC HEMODYNAMIC 1 BLOOD PRESSURE SBP > 90mmHg STABILITY PEAK INSPIRATORY 2 < 35cmH O PRESSURE (PIP) 2 BAROTRAUMA PLATEAU PRESSURE (P ) < 30cmH O PREVENTION PLAT 2 SAFETY SAFETY 3 AutoPEEP None VOLUTRAUMA Start Here TIDAL VOLUME (V ) ~ 6-8cc/kg IBW PREVENTION T Loss of AIRWAY Female ETT 7.0-7.5 AIRWAY / ETT / TRACH Patent Airway MAINTENANCE Male ETT 8.0-8.5 AIRWAY AIRWAY FiO2 21 - 100% PULSE OXIMETRY (SpO2) > 90% Hypoxia OXYGENATION 4 PEEP 5 [5-15] pO2 > 60mmHg 5’5” = 350cc [max 600] pCO2 40mmHg TIDAL 6’0” = 450cc [max 750] 5 VOLUME 6’5” = 500cc [max 850] ETCO2 45 Hypercapnia VENTILATION pH 7.4 GAS GAS EXCHANGE BPM (RR) 14 [10-30] GAS EXCHANGE MINUTE VENTILATION (VMIN) > 5L/min SYNCHRONY WORK OF BREATHING Decreased High Work ASSIST CONTROL MODE VOLUME or PRESSURE of Breathing PATIENT-VENTILATOR AC (V) / AC (P) 6 Comfortable Breaths (WOB) SUPPORT SYNCHRONY COMFORT COMFORT 2⁰ ASSESSMENT PATIENT CIRCUIT VENT Mental Status PIP RR, WOB Pulse, HR, Rhythm ETT/Trach Position Tidal Volume (V ) Trachea T Blood Pressure Secretions Minute Ventilation (V ) SpO MIN Skin Temp/Color 2 Connections Synchrony ETCO Cap Refill 2 Air-Trapping 1. Recognize Signs of Shock Work-up and Manage 2. Assess 6Ps If single problem Troubleshoot Cause 3. If Multiple Problems QUICK FIX Troubleshoot Cause(s) PROBLEMS ©2017 Mayo Clinic Foundation for Medical Education and Research CAUSES QUICK FIX MANAGEMENT Bleeding Hemostasis, Transfuse, Treat cause, Temperature control HYPOVOLEMIA Dehydration Fluid Resuscitation (End points = hypoxia, ↑StO2, ↓PVI) 3rd Spacing Treat cause, Beware of hypoxia (3rd spacing in lungs) Pneumothorax Needle D, Chest tube Abdominal Compartment Syndrome FLUID Treat Cause, Paralyze, Surgery (Open Abdomen) OBSTRUCTED BLOOD RETURN Air-Trapping (AutoPEEP) (if not hypoxic) Pop off vent & SEE SEPARATE CHART PEEP Reduce PEEP Cardiac Tamponade Pericardiocentesis, Drain. -

Acute Compartment Syndrome Complicating Deep Venous Thrombosis
SMGr up Case Report SM Journal of Acute Compartment Syndrome Case Reports Complicating Deep Venous Thrombosis Senthil Dhayalan1*, David Jardine1*, Tony Goh2 and Nicholas Lash3 1Senior registrar and General Physician, Dept of General Medicine, NZ 2Consultant Radiologist, Dept of Radiology, NZ 3Orthopaediac Surgeon, Dept of Orthopaedics, NZ A 40-yr old, heavily-built man initially presented to his general practitioner 2 days before Article Information admission with recent onset of pain and swelling in his left calf. A duplex ultrasound scan Received date: Nov 21, 2018 demonstrated a popliteal and lower leg deep vein thrombosis [DVT], extending 15 cm above the Accepted date: Nov 26, 2018 knee into the femoral vein. He was started appropriately on enoxaparin 130 mg bd. Despite the Published date: Nov 27, 2018 treatment, the pain got worse, particularly when standing, and he was admitted for symptom control. Five weeks earlier he had undergone anterior cruciate ligament repair of the left knee, *Corresponding author [without heparin prophylaxis] and made a satisfactory recovery (Figure 1). Jardine D, General Medicine On examination he was mildly distressed with a low-normal blood pressure [110/70 mmHg] Department, Christchurch hospital, and a persistent low-grade fever [temperature ranged from 37.0-37.8 oC]. The left leg was moderately Private Bag 4710, Christchurch 8140, diffusely swollen, slightly warm and darker in colour [figure]. The pain was localised to the posterior New Zealand, compartments and was exacerbated by dorsi-flexing the ankle and squeezing the gastrocnemius. Email: [email protected] There were no signs of joint effusion, thrombophlebitis, lymphadenopathy or cellulitis. -

Effect of a Small Dike on Blast Wave Propagation
92 Yuta Sugiyama et al. Research paper Effect of a small dike on blast wave propagation Yu ta S u giyama*†,Kunihiko Wakabayashi*,Tomoharu Matsumura*,andYoshioNakayama* *National Institute of Advanced Industrial Science and Technology (AIST), Central 5, 1-1-1 Higashi, Tsukuba, Ibaraki 305-8565, JAPAN Phone : +81-29-861-0552 †Corresponding author : [email protected] Received : January 6, 2015 Accepted : March 31, 2015 Abstract This paper, by means of numerical simulations and experiments, investigates the effect of a small dike on the propagation of a blast wave so as to extract factors related to the strength of the blast wave on the ground. Three materials were considered in this study : detonation products, steel, and air. A cylindrical charge of pentaerythritol tetranitrate (PETN), with a diameter to height ratio of 1.0, was used in the experiments and numerical simulations. A steel dike surrounded the explosive charge on all sides. Its shape and size were parameters in this study. To elucidate the effect of the dike, we conducted two series of numerical simulations and experiments : one without a dike and one with a dike. Peak overpressures on the ground agreed with the experimental results. The numerical simulations qualitatively showed the effect of the three-dimensional diffraction and reflection of the blast wave at the dike, which affected the propagation behavior of the blast wave. Keywords : numerical simulation, experiment, blast wave, dike effect, directionalcharacteristics 1. Introduction interaction of the blast wave and a dike. We have been High-energetic materials yield powerful energy formulating our own numerical program, and in an early instantly, and are used widely in industrial technologies. -

Bilateral Atraumatic Compartment Syndrome of the Legs Leading to Rhabdomyolysis and Acute Renal Failure Following Prolonged Kneeling in a Heroin Addict
PAJT 10.5005/jp-journals-10030-1075 CASE REPORTBilateral Atraumatic Compartment Syndrome of the Legs Leading to Rhabdomyolysis and Acute Renal Failure Bilateral Atraumatic Compartment Syndrome of the Legs Leading to Rhabdomyolysis and Acute Renal Failure Following Prolonged Kneeling in a Heroin Addict. A Case Report and Review of Relevant Literature Saptarshi Biswas, Ramya S Rao, April Duckworth, Ravi Kothuru, Lucio Flores, Sunil Abrol ABSTRACT cerrado, que interfiere con la circulación de los componentes mioneurales del compartimento. Síndrome compartimental Introduction: Compartment syndrome is defined as a symptom bilateral de las piernas es una presentación raro que requiere complex caused by increased pressure of tissue fluid in a closed una intervención quirúrgica urgente. En un reporte reciente osseofascial compartment which interferes with circulation (Khan et al 2012), ha habido reportados solo 8 casos de to the myoneural components of the compartment. Bilateral síndrome compartimental bilateral. compartment syndrome of the legs is a rare presentation Se sabe que el abuso de heroína puede causar el síndrome requiring emergent surgical intervention. In a recent case report compartimental y rabdomiólisis traumática y atraumática. El (Khan et al 2012) there have been only eight reported cases hipotiroidismo también puede presentarse independiente con cited with bilateral compartment syndrome. rabdomiólisis. Heroin abuse is known to cause compartment syndrome, traumatic and atraumatic rhabdomyolysis. Hypothyroidism can Presentación del caso: Presentamos un caso de una mujer also independently present with rhabdomyolysis. de 22 años quien presentó con tumefacción bilateral de las piernas asociado con la perdida de la sensación, después Case presentation: We present a case of a 22 years old female de pasar dos días arrodillado contra una pared después de who presented with bilateral swelling of the legs with associated usar heroína intravenosa. -

Assessment, Management and Decision Making in the Treatment of Polytrauma Patients with Head Injuries
Compartment Syndrome Andrew H. Schmidt, M.D. Professor, Dept. of Orthopedic Surgery, Univ. of Minnesota Chief, Department of Orthopaedic Surgery Hennepin County Medical Center April 2016 Disclosure Information Andrew H. Schmidt, M.D. Conflicts of Commitment/ Effort Board of Directors: OTA Critical Issues Committee: AOA Editorial Board: J Knee Surgery, J Orthopaedic Trauma Medical Director, Director Clinical Research: Hennepin County Med Ctr. Disclosure of Financial Relationships Royalties: Thieme, Inc.; Smith & Nephew, Inc. Consultant: Medtronic, Inc.; DGIMed; Acumed; St. Jude Medical (spouse) Stock: Conventus Orthopaedics; Twin Star Medical; Twin Star ECS; Epien; International Spine & Orthopedic Institute, Epix Disclosure of Off-Label and/or investigative Uses I will not discuss off label use and/or investigational use in my presentation. Objectives • Review Pathophysiology of Acute Compartment Syndrome • Review Current Diagnosis and Treatment – Risk Factors – Clinical Findings – Discuss role and technique of compartment pressure monitoring. Pathophysiology of Compartment Syndrome Pressure Inflexible Fascia Injured Muscle Vascular Consequences of Elevated Intracompartment Pressure: A-V Gradient Theory Pa (High) Pv (Low) artery arteriole capillary venule vein Local Blood Pa - Pv Flow = R Matsen, 1980 Increased interstitial pressure Pa (High) Tissue ischemia artery arteriole capillary venule vein Lysis of cell walls Release of osmotically active cellular contents into interstitial fluid Increased interstitial pressure More cellular -
![Arxiv:2103.05710V1 [Physics.Hist-Ph] 9 Mar 2021 Taylor Compared His Solution of the Evolution of the to Solve This Problem – Professor G](https://docslib.b-cdn.net/cover/3896/arxiv-2103-05710v1-physics-hist-ph-9-mar-2021-taylor-compared-his-solution-of-the-evolution-of-the-to-solve-this-problem-professor-g-1033896.webp)
Arxiv:2103.05710V1 [Physics.Hist-Ph] 9 Mar 2021 Taylor Compared His Solution of the Evolution of the to Solve This Problem – Professor G
Submitted to ANS/NT (2021) LA-UR-20-30042 (v3) On the Symmetry of Blast Waves Roy S. Baty (XTD-PRI)*and Scott D. Ramsey (XTD-NTA) Applied Physics Theoretical Design Division Los Alamos National Laboratory Abstract— This article presents a brief historical review of G. I. Taylor’s solution of the point blast wave problem which was applied to the Trinity test of the first atomic bomb. Lie group symmetry techniques are used to derive Taylor’s famous two-fifths law that relates the position of a blast wave to the time after the explosion and the total energy released. The theory of exterior differential systems is combined with the method of characteristics to demonstrate that the solution of the blast wave problem is directly related to the basic relationships that exist between the geometry (or symmetry) and the physics of wave propagation through the equations of motion. The point blast wave model is cast in terms of two exterior differential systems and both systems are shown to be integrable with local solutions for the velocity, pressure, and density along curves in space and time behind the blast wave. Endorsement: Len G. Margolin (XCP-5) I. HISTORICAL INTRODUCTION the Trinity test is 24:8 (±1:98) kilotons, which is pre- In 1950, the Proceedings of the Royal Society of Lon- sented in this issue by Selby, et al. [5]. Given the physical don published two papers by Sir Geoffrey Taylor [1] and complexity of the atomic explosion, the fact that Taylor’s [2]: the main purpose of these papers was to develop, blast wave solution accurately bounded and predicted the solve, and apply the results of a so-called point blast wave Trinity yield is remarkable. -

Blast Injuries – Essential Facts
BLAST INJURIES Essential Facts Key Concepts • Bombs and explosions can cause unique patterns of injury seldom seen outside combat • Expect half of all initial casualties to seek medical care over a one-hour period • Most severely injured arrive after the less injured, who bypass EMS triage and go directly to the closest hospitals • Predominant injuries involve multiple penetrating injuries and blunt trauma • Explosions in confined spaces (buildings, large vehicles, mines) and/or structural collapse are associated with greater morbidity and mortality • Primary blast injuries in survivors are predominantly seen in confined space explosions • Repeatedly examine and assess patients exposed to a blast • All bomb events have the potential for chemical and/or radiological contamination • Triage and life saving procedures should never be delayed because of the possibility of radioactive contamination of the victim; the risk of exposure to caregivers is small • Universal precautions effectively protect against radiological secondary contamination of first responders and first receivers • For those with injuries resulting in nonintact skin or mucous membrane exposure, hepatitis B immunization (within 7 days) and age-appropriate tetanus toxoid vaccine (if not current) Blast Injuries Essential Facts • Primary: Injury from over-pressurization force (blast wave) impacting the body surface — TM rupture, pulmonary damage and air embolization, hollow viscus injury • Secondary: Injury from projectiles (bomb fragments, flying debris) — Penetrating trauma, -

Shock Waves in Laser-Induced Plasmas
atoms Review Shock Waves in Laser-Induced Plasmas Beatrice Campanella, Stefano Legnaioli, Stefano Pagnotta , Francesco Poggialini and Vincenzo Palleschi * Applied and Laser Spectroscopy Laboratory, ICCOM-CNR, 56124 Pisa, Italy; [email protected] (B.C.); [email protected] (S.L.); [email protected] (S.P.); [email protected] (F.P.) * Correspondence: [email protected]; Tel.: +39-050-315-2224 Received: 7 May 2019; Accepted: 5 June 2019; Published: 7 June 2019 Abstract: The production of a plasma by a pulsed laser beam in solids, liquids or gas is often associated with the generation of a strong shock wave, which can be studied and interpreted in the framework of the theory of strong explosion. In this review, we will briefly present a theoretical interpretation of the physical mechanisms of laser-generated shock waves. After that, we will discuss how the study of the dynamics of the laser-induced shock wave can be used for obtaining useful information about the laser–target interaction (for example, the energy delivered by the laser on the target material) or on the physical properties of the target itself (hardness). Finally, we will focus the discussion on how the laser-induced shock wave can be exploited in analytical applications of Laser-Induced Plasmas as, for example, in Double-Pulse Laser-Induced Breakdown Spectroscopy experiments. Keywords: shock wave; Laser-Induced Plasmas; strong explosion; LIBS; Double-Pulse LIBS 1. Introduction The sudden release of energy delivered by a pulsed laser beam on a material (solid, liquid or gaseous) may produce a small (but strong) explosion, which is associated, together with other effects (ablation of material, plasma formation and excitation), with a violent displacement of the surrounding material and the production of a shock wave.