Bone and Soft Tissue Pathology (37-109)
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

A Rare Bone Tumor
OPEN ACCESS L E T T E R T O T H E E D I T O R Periosteal Desmoplastic Fibroma of Radius: A Rare Bone Tumor Aniqua Saleem1,* Hira Saleem2 1 Radiology Department, District Head Quarters Hospital, Rawalpindi Medical University, Rawalpindi 2 Department of Surgery, Shifa International Hospital, Islamabad. Correspondence*: Dr. Aniqua Saleem, Radiology Department, District Head Quarters Hospital, Rawalpindi Medical University, Rawalpindi E-mail: [email protected] © 2019, Saleem et al, Submitted: 05-04-2019 Accepted: 09-06-2019 Conflict of Interest: None Source of Support: Nil This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. DEAR SIR Desmoplastic fibroma is an extremely rare tumor of enhancement on post contrast images and with adjacent bone with a reported incidence of 0.11 % of all primary bone involvement as was evident by focal cortical inter- bone tumors. The most common site of involvement is ruption, mild endosteal thickening and irregularity and mandible (reported incidence 22% of all Desmoplastic also mild ulnar shaft remodeling (Fig. 3a, 3b). To further fibroma cases) followed by metaphysis of long bones. characterize the lesion, Tc99 MDP (methylene diphos- Involvement of forearm especially involving periosteum phonate) bone scan was also performed which showed is seldom reported. Prompt diagnosis and adequate active bone involvement in left distal radial shaft. management is important for limb salvage and restora- tion of limb function. [1-3] An 11-year-old boy presented with painful mild swelling of left forearm for a month, with no significant past med- ical history or any history of trauma. -

A Rare Presentation of Benign Brenner Tumor of Ovary: a Case Report
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Periasamy S et al. Int J Reprod Contracept Obstet Gynecol. 2018 Jul;7(7):2971-2974 www.ijrcog.org pISSN 2320-1770 | eISSN 2320-1789 DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20182920 Case Report A rare presentation of benign Brenner tumor of ovary: a case report Sumathi Periasamy1, Subha Sivagami Sengodan2*, Devipriya1, Anbarasi Pandian2 1Department of Surgery, 2Department of Obstetrics and Gynaecology, Government Mohan Kumaramangalam Medical College, Salem, Tamil Nadu, India Received: 17 April 2018 Accepted: 23 May 2018 *Correspondence: Dr. Subha Sivagami Sengodan, E-mail: [email protected] Copyright: © the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Brenner tumors are rare ovarian tumors accounting for 2-3% of all ovarian neoplasms and about 2% of these tumors are borderline (proliferating) or malignant. These tumors are commonly seen in 4th-8th decades of life with a peak in late 40s and early 50s. Benign Brenner tumors are usually small, <2cm in diameter and often detected incidentally during surgery or on pathological examination. Authors report a case of a large, calcified benign Brenner tumor in a 55-year-old postmenopausal woman who presented with complaint of abdominal pain and mass in abdomen. Imaging revealed large complex solid cystic pelvic mass -peritoneal fibrosarcoma. She underwent laparotomy which revealed huge Brenner tumor weighing 9kg arising from left uterine cornual end extending up to epigastric region. -

A Case Report1 양측 흉막에 발생한 결합조직형성 소원형세포종양의 증례 보고1
Case Report pISSN 1738-2637 / eISSN 2288-2928 J Korean Soc Radiol 2015;72(4):295-299 http://dx.doi.org/10.3348/jksr.2015.72.4.295 Bilateral Presentation of Pleural Desmoplastic Small Round Cell Tumors: A Case Report1 양측 흉막에 발생한 결합조직형성 소원형세포종양의 증례 보고1 You Sun Won, MD1, Jai Soung Park, MD1, Sun Hye Jeong, MD1, Sang Hyun Paik, MD1, Heon Lee, MD1, Jang Gyu Cha, MD1, Eun Suk Koh, MD2 Departments of 1Radiology, 2Pathology, Soonchunhyang University College of Medicine, Bucheon Hospital, Bucheon, Korea Desmoplastic small round cell tumor (DSRCT) is a highly aggressive malignant small cell neoplasm occurring mainly in the abdominal cavity, but it is extremely rare in Received October 13, 2014; Accepted December 21, the pleura. In this case, a 15-year-old male presented with a 1-month history of left 2014 chest pain. Chest radiographs revealed pleural thickening in the left hemithorax and Corresponding author: Jai Soung Park, MD Department of Radiology, Soonchunhyang University chest computed tomography showed multifocal pleural thickening with enhance- College of Medicine, Bucheon Hospital, 170 Jomaru-ro, ment in both hemithoraces. A needle biopsy of the left pleural lesion was performed Wonmi-gu, Bucheon 420-767, Korea. and the final diagnosis was DSRCT of the pleura. We report this unusual case aris- Tel. 82-32-621-5851 Fax. 82-32-621-5874 E-mail: [email protected] ing from the pleura bilaterally. The pleural involvement of this tumor supports the hypothesis that it typically occurs in mesothelial-lined surfaces. This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0) Index terms which permits unrestricted non-commercial use, distri- Pleura bution, and reproduction in any medium, provided the Thickened Pleura original work is properly cited. -

Immunohistochemical and Electron Microscopic Findings in Benign Fibroepithelial Vaginal Polyps J Clin Pathol: First Published As 10.1136/Jcp.43.3.224 on 1 March 1990
224 J Clin Pathol 1990;43:224-229 Immunohistochemical and electron microscopic findings in benign fibroepithelial vaginal polyps J Clin Pathol: first published as 10.1136/jcp.43.3.224 on 1 March 1990. Downloaded from T P Rollason, P Byrne, A Williams Abstract LIGHT MICROSCOPY Eleven classic benign "fibroepithelial Sections were cut from routinely processed, polyps" of the vagina were examined paraffin wax embedded blocks at 4 gm and using a panel of immunocytochemical immunocytochemical techniques were agents. Two were also examined electron performed using a standard peroxidase- microscopically. In all cases the stellate antiperoxidase method.7 The antibodies used and multinucleate stromal cells were as follows: polyclonal rabbit characteristic of these lesions stained antimyoglobin (batch A324, Dako Ltd, High strongly for desmin, indicating muscle Wycombe, Buckinghamshire), monoclonal intermediate filament production. In anti-desmin (batch M724, Dako Ltd), mono- common with uterine fibroleiomyomata, clonal anti-epithelial membrane antigen (batch numerous mast cells were also often M613, Dako Ltd), monoclonal anti-vimentin seen. Myoglobin staining was negative. (batch M725, Dako Ltd), polyclonal rabbit Electron microscopical examination anti-cytokeratin (Bio-nuclear services, Read- confirmed that the stromal cells con- ing) and monoclonal anti cytokeratin NCL tained abundant thin filaments with focal 5D3 (batch M503, Bio-nuclear services). densities and also showed the ultrastruc- Mast cells were shown by a standard tural features usually associated with chloroacetate esterase method using pararo- myofibroblasts. saniline,8 which gave an intense red cyto- It is concluded that these tumours plasmic colouration, and by the routine would be better designated polypoid toluidine blue method. myofibroblastomas in view of the above An attempt was made to assess semiquan- findings. -

Pnas.201413825SI.Pdf
Supporting Information Impens et al. 10.1073/pnas.1413825111 13 15 13 15 SI Methods beling) (Silantes Gmbh), or C6 N2 L-lysine HCl and C6 N4 L- Plasmids. pSG5-His6-SUMO1 plasmid encodes the N-terminal arginine HCl (heavy labeling) (Silantes Gmbh). L-Lysine HCl was His6-tagged mature Small ubiquitin modifier 1 (SUMO1) isoform added at its normal concentration in DMEM (146 mg/L), but the (kind gift of A. Dejean, Institut Pasteur, Paris). The pSG5-His6- concentration of L-arginine HCl was reduced to 25 mg/L (30% of SUMO1 T95R mutat was derived from this plasmid using PCR the normal concentration in DMEM) to prevent metabolic con- mutagenesis. pSG5-His6-SUMO2 was obtained by inserting the version of arginine to proline (4). Cells were kept for at least six cDNA corresponding to the human mature SUMO2 isoform population doublings to ensure complete incorporation of the la- with an N-terminal His6 tag in the pSG5 vector (Stratagene). beled lysine and arginine. 2 The pSG5-His6-SUMO2 T91R mutant was derived from this For transfections, cells were seeded in 75-cm flasks or in 6- or plasmid by PCR mutagenesis. N-terminally HA-tagged human 24-well plates at a density of 2.7 × 106 cells per flask or 3 × 105 or cDNA of ZBTB20 (Zinc finger and BTB domain containing 0.5 × 105 cells per well, respectively. The next day cells were 20) isoform 2 (UniProt identifier Q9HC78-2), HMBOX1 (Ho- transfected with Lipofectamine LTX reagents (Invitrogen) (20 μg meobox containing protein 1) isoform 1 (HMBOX1A) (UniProt of DNA per flask, 3.5 μg per well in the six-well plates, or 0.75 μg identifier Q6NT76-1), NACC1 (Nucleus accumbens-associated per well in the 24-well plates) for 48 h. -

Diagnostic Immunohistochemistry for Canine Cutaneous Round Cell Tumours — Retrospective Analysis of 60 Cases
FOLIA HISTOCHEMICA ORIGINAL PAPER ET CYTOBIOLOGICA Vol. 57, No. 3, 2019 pp. 146–154 Diagnostic immunohistochemistry for canine cutaneous round cell tumours — retrospective analysis of 60 cases Katarzyna Pazdzior-Czapula, Mateusz Mikiewicz, Michal Gesek, Cezary Zwolinski, Iwona Otrocka-Domagala Department of Pathological Anatomy, Faculty of Veterinary Medicine, University of Warmia and Mazury in Olsztyn, Olsztyn, Poland Abstract Introduction. Canine cutaneous round cell tumours (CCRCTs) include various benign and malignant neoplastic processes. Due to their similar morphology, the diagnosis of CCRCTs based on histopathological examination alone can be challenging, often necessitating ancillary immunohistochemical (IHC) analysis. This study presents a retrospective analysis of CCRCTs. Materials and methods. This study includes 60 cases of CCRCTs, including 55 solitary and 5 multiple tumours, evaluated immunohistochemically using a basic antibody panel (MHCII, CD18, Iba1, CD3, CD79a, CD20 and mast cell tryptase) and, when appropriate, extended antibody panel (vimentin, desmin, a-SMA, S-100, melan-A and pan-keratin). Additionally, histochemical stainings (May-Grünwald-Giemsa and methyl green pyronine) were performed. Results. IHC analysis using a basic antibody panel revealed 27 cases of histiocytoma, one case of histiocytic sarcoma, 18 cases of cutaneous lymphoma of either T-cell (CD3+) or B-cell (CD79a+) origin, 5 cases of plas- macytoma, and 4 cases of mast cell tumours. The extended antibody panel revealed 2 cases of alveolar rhabdo- myosarcoma, 2 cases of amelanotic melanoma, and one case of glomus tumour. Conclusions. Both canine cutaneous histiocytoma and cutaneous lymphoma should be considered at the beginning of differential diagnosis for CCRCTs. While most poorly differentiated CCRCTs can be diagnosed immunohis- tochemically using 1–4 basic antibodies, some require a broad antibody panel, including mesenchymal, epithelial, myogenic, and melanocytic markers. -

Advances in Immune Checkpoint Inhibitors for Bone Sarcoma Therapy T Pichaya Thanindratarna,B, Dylan C
Journal of Bone Oncology 15 (2019) 100221 Contents lists available at ScienceDirect Journal of Bone Oncology journal homepage: www.elsevier.com/locate/jbo Review Article Advances in immune checkpoint inhibitors for bone sarcoma therapy T Pichaya Thanindratarna,b, Dylan C. Deana, Scott D. Nelsonc, Francis J. Horniceka, ⁎ Zhenfeng Duana, a Department of Orthopedic Surgery, Sarcoma Biology Laboratory, David Geffen School of Medicine, University of California, 615 Charles E. Young. Dr. South, Los Angeles, CA 90095, USA b Department of Orthopedic Surgery, Chulabhorn hospital, HRH Princess Chulabhorn College of Medical Science, Bangkok, Thailand c Department of Pathology, University of California, Los Angeles, CA, USA ARTICLE INFO ABSTRACT Keywords: Bone sarcomas are a collection of sporadic malignancies of mesenchymal origin. The most common subtypes Immune checkpoint include osteosarcoma, Ewing sarcoma, chondrosarcoma, and chordoma. Despite the use of aggressive treatment Immunotherapy protocols consisting of extensive surgical resection, chemotherapy, and radiotherapy, outcomes have not sig- Bone sarcoma nificantly improved over the past few decades for osteosarcoma or Ewing sarcoma patients. In addition, chon- Anti-PD-1/PD-L1 drosarcoma and chordoma are resistant to both chemotherapy and radiation therapy. There is, therefore, an Anti-CTLA-4 urgent need to elucidate which novel new therapies may affect bone sarcomas. Emerging checkpoint inhibitors have generated considerable attention for their clinical success in a variety of human cancers, which has led to works assessing their potential in bone sarcoma management. Here, we review the recent advances of anti-PD-1/ PD-L1 and anti-CTLA-4 blockade as well as other promising new immune checkpoint targets for their use in bone sarcoma therapy. -

A Computational Approach for Defining a Signature of Β-Cell Golgi Stress in Diabetes Mellitus
Page 1 of 781 Diabetes A Computational Approach for Defining a Signature of β-Cell Golgi Stress in Diabetes Mellitus Robert N. Bone1,6,7, Olufunmilola Oyebamiji2, Sayali Talware2, Sharmila Selvaraj2, Preethi Krishnan3,6, Farooq Syed1,6,7, Huanmei Wu2, Carmella Evans-Molina 1,3,4,5,6,7,8* Departments of 1Pediatrics, 3Medicine, 4Anatomy, Cell Biology & Physiology, 5Biochemistry & Molecular Biology, the 6Center for Diabetes & Metabolic Diseases, and the 7Herman B. Wells Center for Pediatric Research, Indiana University School of Medicine, Indianapolis, IN 46202; 2Department of BioHealth Informatics, Indiana University-Purdue University Indianapolis, Indianapolis, IN, 46202; 8Roudebush VA Medical Center, Indianapolis, IN 46202. *Corresponding Author(s): Carmella Evans-Molina, MD, PhD ([email protected]) Indiana University School of Medicine, 635 Barnhill Drive, MS 2031A, Indianapolis, IN 46202, Telephone: (317) 274-4145, Fax (317) 274-4107 Running Title: Golgi Stress Response in Diabetes Word Count: 4358 Number of Figures: 6 Keywords: Golgi apparatus stress, Islets, β cell, Type 1 diabetes, Type 2 diabetes 1 Diabetes Publish Ahead of Print, published online August 20, 2020 Diabetes Page 2 of 781 ABSTRACT The Golgi apparatus (GA) is an important site of insulin processing and granule maturation, but whether GA organelle dysfunction and GA stress are present in the diabetic β-cell has not been tested. We utilized an informatics-based approach to develop a transcriptional signature of β-cell GA stress using existing RNA sequencing and microarray datasets generated using human islets from donors with diabetes and islets where type 1(T1D) and type 2 diabetes (T2D) had been modeled ex vivo. To narrow our results to GA-specific genes, we applied a filter set of 1,030 genes accepted as GA associated. -

The Health-Related Quality of Life of Sarcoma Patients and Survivors In
Cancers 2020, 12 S1 of S7 Supplementary Materials The Health-Related Quality of Life of Sarcoma Patients and Survivors in Germany—Cross-Sectional Results of A Nationwide Observational Study (PROSa) Martin Eichler, Leopold Hentschel, Stephan Richter, Peter Hohenberger, Bernd Kasper, Dimosthenis Andreou, Daniel Pink, Jens Jakob, Susanne Singer, Robert Grützmann, Stephen Fung, Eva Wardelmann, Karin Arndt, Vitali Heidt, Christine Hofbauer, Marius Fried, Verena I. Gaidzik, Karl Verpoort, Marit Ahrens, Jürgen Weitz, Klaus-Dieter Schaser, Martin Bornhäuser, Jochen Schmitt, Markus K. Schuler and the PROSa study group Includes Entities We included sarcomas according to the following WHO classification. - Fletcher CDM, World Health Organization, International Agency for Research on Cancer, editors. WHO classification of tumours of soft tissue and bone. 4th ed. Lyon: IARC Press; 2013. 468 p. (World Health Organization classification of tumours). - Kurman RJ, International Agency for Research on Cancer, World Health Organization, editors. WHO classification of tumours of female reproductive organs. 4th ed. Lyon: International Agency for Research on Cancer; 2014. 307 p. (World Health Organization classification of tumours). - Humphrey PA, Moch H, Cubilla AL, Ulbright TM, Reuter VE. The 2016 WHO Classification of Tumours of the Urinary System and Male Genital Organs—Part B: Prostate and Bladder Tumours. Eur Urol. 2016 Jul;70(1):106–19. - World Health Organization, Swerdlow SH, International Agency for Research on Cancer, editors. WHO classification of tumours of haematopoietic and lymphoid tissues: [... reflects the views of a working group that convened for an Editorial and Consensus Conference at the International Agency for Research on Cancer (IARC), Lyon, October 25 - 27, 2007]. 4. ed. -

Acknowledgement to Reviewers 2014
Osteoarthritis and Cartilage 23 (2015) iiieviii Acknowledgement to Reviewers 2014 Stefan Lohmander Editor in Chief We are fortunate to have an outstanding group of reviewers who kindly volunteer their time and effort to review manuscripts for Osteoarthritis and Cartilage. They are critical team players in the continued success of the journal, ensuring a peer review process of the highest integrity and quality. I wish to thank those reviewers who provided their expertise in evaluating manuscripts for Osteoarthritis and Cartilage in 2014. Roy Aaron, Providence, United States Frank Beier, London, Canada Steven Abramson, New York, United States Kim Bennell, Parkville, Australia Ilana Ackerman, Parkville, Australia John Bertram, Calgary, Canada Douglas Adams, Farmington, United States Bruce Beynnon, Burlington, United States Michael Adams, Bristol, United Kingdom Sita Bierma-Zeinstra, Rotterdam, Netherlands Adetola Adesida, Edmonton, Canada Johannes Bijlsma, Utrecht, Netherlands Isaac Afara, Kuopio, Finland Trevor Birmingham, London, Canada Sudha Agarwal, Columbus, United States Sandip Biswal, Stanford, United States Bharat Aggarwal, Houston, United States Bernd Bittersohl, Düsseldorf, Germany Thomas Aigner, Coburg, Germany Jan Bjordal, Bergen, Norway Dawn Aitken, Hobart, Australia Francisco Blanco, A Coruna,~ Spain Michael Albro, New York, United States Esmeralda Blaney Davidson, Nijmegen, Netherlands Hamza Alizai, Valley Strean, United States Katerina Blazek, Stanford, United States Kelli Allen, Durham, United States Henning Bliddal, Frederiksberg, -
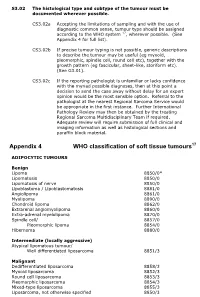

Appendix 4 WHO Classification of Soft Tissue Tumours17
S3.02 The histological type and subtype of the tumour must be documented wherever possible. CS3.02a Accepting the limitations of sampling and with the use of diagnostic common sense, tumour type should be assigned according to the WHO system 17, wherever possible. (See Appendix 4 for full list). CS3.02b If precise tumour typing is not possible, generic descriptions to describe the tumour may be useful (eg myxoid, pleomorphic, spindle cell, round cell etc), together with the growth pattern (eg fascicular, sheet-like, storiform etc). (See G3.01). CS3.02c If the reporting pathologist is unfamiliar or lacks confidence with the myriad possible diagnoses, then at this point a decision to send the case away without delay for an expert opinion would be the most sensible option. Referral to the pathologist at the nearest Regional Sarcoma Service would be appropriate in the first instance. Further International Pathology Review may then be obtained by the treating Regional Sarcoma Multidisciplinary Team if required. Adequate review will require submission of full clinical and imaging information as well as histological sections and paraffin block material. Appendix 4 WHO classification of soft tissue tumours17 ADIPOCYTIC TUMOURS Benign Lipoma 8850/0* Lipomatosis 8850/0 Lipomatosis of nerve 8850/0 Lipoblastoma / Lipoblastomatosis 8881/0 Angiolipoma 8861/0 Myolipoma 8890/0 Chondroid lipoma 8862/0 Extrarenal angiomyolipoma 8860/0 Extra-adrenal myelolipoma 8870/0 Spindle cell/ 8857/0 Pleomorphic lipoma 8854/0 Hibernoma 8880/0 Intermediate (locally -

THE AMERICAN JOURNAL of CANCER a Continuation of the Journal of Cancer Research
THE AMERICAN JOURNAL OF CANCER A Continuation of The Journal of Cancer Research ~ VOLUMEXXXIV DECEMBER,1938 NUMBER4 SYNOVIAL SARCOMAS IN SEROUS BURSAE AND TENDON SHEATHS PROF. LOUIS BERGER, M.D. (From the Pathological Department, HBpital de I'Enfant-Jdsus, and the Anti-Cancer Center of Lava1 University, Quebec) Progress in the knowledge of malignant tumors arising from synovial tissue has been slow. In spite of some recent and valuable contributions, this chapter is far from complete. The reasons for this are threefold: first, the want of knowledge concerning the normal features and nature of synovial tissue, which was long studied in articulations only, although it is common, also, to serous bursae and tendon sheaths; second, the relative-perhaps only apparent-rarity of cases; finally, the lack of precision and even vagueness of the reports in the literature., Most of the older authors, and even some contemporary ones, interested primarily in the clinical or surgical aspects of the question, have been satisfied with a purely topographical diagnosis and have either neglected the histologic aspects of their tumors or described them only briefly and superficially. We have had the opportunity of studying five cases of synovial sarcoma, differing more or less from one another but all originating outside of articu- lations, that is in serous bursae or tendon sheaths, where these tumors are less known, but perhaps easier to study than in the more intricate tissues of the joints. THENORMAL SYNOVIAL TISSUE The prototype of synovial tissue is encountered in the synovial membranes of the joints, but all histologists admit that the lining tissue of the serous bursae and tendon sheaths is homologous with articular synovialis.