Incessant Bilobed Thymus in an Old Male Cadaver Case Report
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-
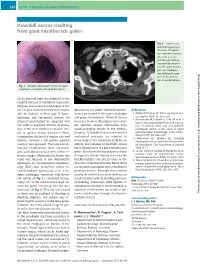
Downhill Varices Resulting from Giant Intrathoracic Goiter
E40 UCTN – Unusual cases and technical notes Downhill varices resulting from giant intrathoracic goiter Fig. 2 Sagittal com- puted tomography of the chest. The goiter was immense, reaching the aortic arch, sur- rounding the trachea and partially compres- sing the upper esopha- gus. The esophagus was additionally com- pressed by anterior spinal spondylophytes. Fig. 1 Multiple submucosal veins in the upper esophagus, consistent with downhill varices. An 82-year-old man was admitted to the hospital because of substernal chest pain, dyspnea, and occasional dysphagia to sol- ids. His past medical history was remark- geal varices are called “downhill varices”, References able for diabetes mellitus type II, hyper- as they are located in the upper esophagus 1 Kotfila R, Trudeau W. Extraesophageal vari- – lipidemia, and Parkinson’s disease. On and project downwards. Downhill varices ces. Dig Dis 1998; 16: 232 241 2 Basaranoglu M, Ozdemir S, Celik AF et al. A occur as a result of shunting in cases of up- physical examination he appeared frail case of fibrosing mediastinitis with obstruc- but with no apparent distress. Examina- per systemic venous obstruction from tion of superior vena cava and downhill tion of the neck showed no masses, stri- space-occupying lesions in the medias- esophageal varices: a rare cause of upper dor or jugular venous distension. Heart tinum [2,3]. Downhill varices as a result of gastrointestinal hemorrhage. J Clin Gastro- – examination disclosed a regular rate and mediastinal processes are reported to enterol 1999; 28: 268 270 3 Calderwood AH, Mishkin DS. Downhill rhythm; however a 2/6 systolic ejection occur in up to 50% of patients [3,4]. -

Selective Venous Sampling for Primary Hyperparathyroidism: How to Perform an Examination and Interpret the Results with Reference to Thyroid Vein Anatomy
Jpn J Radiol DOI 10.1007/s11604-017-0658-3 INVITED REVIEW Selective venous sampling for primary hyperparathyroidism: how to perform an examination and interpret the results with reference to thyroid vein anatomy Takayuki Yamada1 · Masaya Ikuno1 · Yasumoto Shinjo1 · Atsushi Hiroishi1 · Shoichiro Matsushita1 · Tsuyoshi Morimoto1 · Reiko Kumano1 · Kunihiro Yagihashi1 · Takuyuki Katabami2 Received: 11 April 2017 / Accepted: 28 May 2017 © Japan Radiological Society 2017 Abstract Primary hyperparathyroidism (pHPT) causes and brachiocephalic veins for catheterization of the thyroid hypercalcemia. The treatment for pHPT is surgical dis- veins and venous anastomoses. section of the hyperfunctioning parathyroid gland. Lower rates of hypocalcemia and recurrent laryngeal nerve injury Keywords Primary hyperparathyroidism · Localization · imply that minimally invasive parathyroidectomy (MIP) is Thyroid vein · Venous sampling safer than bilateral neck resection. Current trends in MIP use can be inferred only by reference to preoperative locali- zation studies. Noninvasive imaging studies (typically pre- Introduction operative localization studies) show good detection rates of hyperfunctioning glands; however, there have also been Primary hyperparathyroidism (pHPT) is a common endocrine cases of nonlocalization or discordant results. Selective disease. Most patients have one adenoma, but double adeno- venous sampling (SVS) is an invasive localization method mas have been reported in up to 15% of cases [1]. Approxi- for detecting elevated intact parathyroid -

Anatomy & Embryology of Thyroid & Parathyroid
ANATOMY & EMBRYOLOGY OF THYROID & PARATHYROID By Prof . Saeed Abuel Makarem & Associate Prof. Sanaa Alshaarawy 1 OBJECTIVES Ò By the end of the lecture, the student should be able to: Ò Describe the shape, position, relations and structure of the thyroid gland. Ò List the blood supply & lymphatic drainage of the thyroid gland. Ò List the nerves endanger with thyroidectomy operation. Ò Describe the shape, position, blood supply & lymphatic drainage of the parathyroid glands. Ò Describe the development of the thyroid & parathyroid glands. Ò Describe the most common congenital anomalies of the thyroid gland. 2 Before we go to the thyroid What are the parts of the deep fascia or deep cervical fascia of the neck? It is divided mainly into 3 layers: 1- Investing layer. 2- Pretracheal layer. 3- Prevertebral layer. 3 Ò Endocrine, butterfly Thyroid gland shaped gland. Ò Consists of right & left lobes. Ò The 2 lobes are connected to each other by a narrow isthmus, which overlies the 2nd ,3rd & 4th tracheal rings. Ò It is surrounded by a facial sheath derived from the pretracheal layer of the deep cervical fascia. 4 Thyroid gland Ò Each lobe is pear- shaped, with its apex reaches up to the oblique line of thyroid cartilage. Ò Its base lies at the level of 4th or 5th tracheal rings. Ò Inside the pretracheal facial capsule, there is another C.T capsule. Ò So, it s surrounded by 2 membranes. 5 Each lobe is pear shape, with its apex directed upward as far as the Anterior oblique line of the thyroid cartilage; its base lies at the 4th or 5th tracheal ring. -

SŁOWNIK ANATOMICZNY (ANGIELSKO–Łacinsłownik Anatomiczny (Angielsko-Łacińsko-Polski)´ SKO–POLSKI)
ANATOMY WORDS (ENGLISH–LATIN–POLISH) SŁOWNIK ANATOMICZNY (ANGIELSKO–ŁACINSłownik anatomiczny (angielsko-łacińsko-polski)´ SKO–POLSKI) English – Je˛zyk angielski Latin – Łacina Polish – Je˛zyk polski Arteries – Te˛tnice accessory obturator artery arteria obturatoria accessoria tętnica zasłonowa dodatkowa acetabular branch ramus acetabularis gałąź panewkowa anterior basal segmental artery arteria segmentalis basalis anterior pulmonis tętnica segmentowa podstawna przednia (dextri et sinistri) płuca (prawego i lewego) anterior cecal artery arteria caecalis anterior tętnica kątnicza przednia anterior cerebral artery arteria cerebri anterior tętnica przednia mózgu anterior choroidal artery arteria choroidea anterior tętnica naczyniówkowa przednia anterior ciliary arteries arteriae ciliares anteriores tętnice rzęskowe przednie anterior circumflex humeral artery arteria circumflexa humeri anterior tętnica okalająca ramię przednia anterior communicating artery arteria communicans anterior tętnica łącząca przednia anterior conjunctival artery arteria conjunctivalis anterior tętnica spojówkowa przednia anterior ethmoidal artery arteria ethmoidalis anterior tętnica sitowa przednia anterior inferior cerebellar artery arteria anterior inferior cerebelli tętnica dolna przednia móżdżku anterior interosseous artery arteria interossea anterior tętnica międzykostna przednia anterior labial branches of deep external rami labiales anteriores arteriae pudendae gałęzie wargowe przednie tętnicy sromowej pudendal artery externae profundae zewnętrznej głębokiej -

An Unusual Origin and Course of the Thyroidea Ima Artery, with Absence of Inferior Thyroid Artery Bilaterally
Surgical and Radiologic Anatomy (2019) 41:235–237 https://doi.org/10.1007/s00276-018-2122-1 ANATOMIC VARIATIONS An unusual origin and course of the thyroidea ima artery, with absence of inferior thyroid artery bilaterally Doris George Yohannan1 · Rajeev Rajan1 · Akhil Bhuvanendran Chandran1 · Renuka Krishnapillai1 Received: 31 May 2018 / Accepted: 21 October 2018 / Published online: 25 October 2018 © Springer-Verlag France SAS, part of Springer Nature 2018 Abstract We report an unusual origin and course of the thyroidea ima artery in a male cadaver. The ima artery originated from the right subclavian artery very close to origin of the right vertebral artery. The artery coursed anteriorly between the common carotid artery medially and internal jugular vein laterally. It then coursed obliquely, from below upwards, from lateral to medial superficial to common carotid artery, to reach the inferior pole of the right lobe of thyroid and branched repeatedly to supply the anteroinferior and posteroinferior aspects of both the thyroid lobes and isthmus. The superior thyroid arteries were normal. Both the inferior thyroid arteries were absent. The unusual feature of this thyroidea ima artery is its origin from the subclavian artery close to vertebral artery origin, the location being remarkably far-off from the usual near midline position, and the oblique and relatively superficial course. This report is a caveat to neck surgeons to consider such a superficially running vessel to be a thyroidea ima artery. Keywords Thyroid vascular anatomy · Thyroidea ima artery · Artery of Neubauer · Blood supply of thyroid · Variations Introduction (1.1%), transverse scapular (1.1%), or pericardiophrenic or thyrocervical trunk [8, 10]. -

Anatomy of the Woodchuck (Marmota Monax)
QL737 .R68B49 2005 Anatomy of the Woodchuck (Marmota monax) A. J. Bezuidenhout and H. E. Evans SPECIAL PUBLICATION NO. 13 AMERICAN SOCIETY OF MAMMALOGISTS LIBRARY OF THE /XT FOR THE ^> ^ PEOPLE ^ ^* <£ FOR _ EDVCATION O <£ FOR ^J O, SCIENCE j< Anatomy of the Woodchuck (Marmota monax) by A. J. Bezuidenhout and H. E. Evans SPECIAL PUBLICATION NO. 13 American Society of Mammalogists Published 21 February 2005 Price $45.00 includes postage and handling. American Society of Mammalogists P.O. Box 7060 Lawrence, KS 66044-1897 ISBN: 1-891276-43-3 Library of Congress Control Number: 2005921107 Printed at Allen Press, Inc., Lawrence, Kansas 66044 Issued: 21 February 2005 Copyright © by the American Society of Mammalogists 2005 SPECIAL PUBLICATIONS American Society of Mammalogists This series, published by the American Society of Mammalogists in association with Allen Press, Inc., has been established for peer-reviewed papers of monographic scope concerned with any aspect of the biology of mammals. Copies of Special Publications by the Society may be ordered from: American Society of Mammalogists, % Allen Marketing and Management, P.O. Box 7060, Lawrence, KS 66044-8897, or at www. mammalogy.org. Dr. Joseph F. Merritt Editor for Special Publications Department of Biology United States Air Force Academy 2355 Faculty Drive US Air Force Academy, CO 80840 Dr. David M. Leslie, Jr. Chair, ASM Publications Committee Oklahoma Cooperative Fish and Wildlife Research Unit United States Geological Survey 404 Life Sciences West Oklahoma State University Stillwater, OK 74078-3051 Anatomy of the Woodchuck (Marmota MONAX) A. J. Bezuidenhout and H. E. Evans Published by the American Society of Mammalogists Contents Page Acknowledgments vii Foreword ix Chapter 1. -

Superior and Posterior Mediastina Reading: 1. Gray's Anatomy For
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray’s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior mediastinum Clinical Correlate: 1. Aortic aneurysms Superior Mediastinum (pp.181-199) 27 Review of the Subdivisions of the Mediastinum Superior mediastinum Comprises area within superior thoracic aperture and transverse thoracic plane -Transverse thoracic plane – arbitrary line from the sternal angle anteriorly to the IV disk or T4 and T5 posteriorly Inferior mediastinum Extends from transverse thoracic plane to diaphragm; 3 subdivisions Anterior mediastinum – smallest subdivision of mediastinum -Lies between the body of sternum and transversus thoracis muscles anteriorly and the pericardium posteriorly -Continuous with superior mediastinum at the sternal angle and limited inferiorly by the diaphragm -Consists of sternopericardial ligaments, fat, lymphatic vessels, and branches of internal thoracic vessels. Contains inferior part of thymus in children Middle mediastinum – contains heart Posterior mediastinum Superior Mediastinum Thymus – lies posterior to manubrium and extends into the anterior mediastinum -Important in development of immune system through puberty -Replaced by adipose tissue in adult Arterial blood supply -Anterior intercostals and mediastinal branches of internal thoracic artery Venous blood supply -Veins drain into left brachiocephalic, internal thoracic, and thymic veins 28 Brachiocephalic Veins - Formed by the -

A Syllabus of Core Surgical Anatomy
A Syllabus of Core Surgical Anatomy Background In February 2010, it was agreed that the Anatomy Committee would undertake to develop a new generic examination for implementation in 2012 to assess anatomy for surgical trainees. Content Anatomical questions relate to: • clinical examination – surface anatomy, inspection, palpation, percussion, auscultation, pelvic examination, testing for peripheral nerve injuries, potential sites of spread of tumours (as determined by anatomy e.g. lymphatic drainage of the breast) • urethral catheterization • vascular access (arterial and venous, peripheral and central) • the airway: maintenance, access • chest drainage • imaging (plain radiographs, CT, MRI, US, contrast studies) • surgical access – open and minimally invasive • endoscopy (GI, arthroscopy etc) • peripheral nerve blocks • percutaneous liver biopsy • trauma (aligned to anatomy in EMST) • common anatomical complications of routine surgical procedures • principles of anatomy: terminology, anatomical position, planes, relationships in regional anatomy, movements, tissues, systems, and anatomical variation. Syllabus Essential (+++) • What an early SET 1 trainee (PGY 2-3 with general experience) should know. • Must recognise, understand and be able to explain. • These structures comprise core basic surgical anatomy and are essential in inter-specialty communication. • Lack of knowledge could jeapordise patient safety. • Includes all common and important anatomical characteristics of the structure: location, constituent parts, relations, blood supply and lymphatic drainage, innervation, course and distribution, when the structure is at risk, effects of injury, and common variants of clinical importance. Desirable (++) • Should be able to describe the basic anatomy/location of the structure, its function, major nerve and blood supply ± lymphatic drainage, and general relations. Non-core (+) • Not considered core knowledge but may be appropriate for specialty-specific anatomy. -

Transcervical Thymectomy
Original Article Page 1 of 5 Transcervical thymectomy Marcin Zieliński1, Mariusz Rybak1*, Katarzyna Solarczyk-Bombik1, Michal Wilkojc1, Wojciech Czajkowski1, Sylweriusz Kosinski2, Edward Fryzlewicz2, Tomasz Nabialek2, Malgorzata Szolkowska3, Juliusz Pankowski4 1Department of the Thoracic Surgery, 2Department the Anesthesiology and Intensive Care, Pulmonary Hospital, Zakopane, Poland; 3Department of Pathology of the Tuberculosis Institute, Warsaw, Poland; 4Department of Pathology, Pulmonary Hospital, Zakopane, Poland Contributions: (I) Conception and design: M Zieliński; (II) Administrative support: None; (III) Provision of study materials or patients: None; (IV) Collection and assembly of data: All authors; (V) Data analysis and interpretation: None; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Marcin Zieliński, MD, PhD. Department of Thoracic Surgery, Pulmonary Hospital, Ul. Gładkie 1, 34 500 Zakopane, Poland. Email: [email protected]. Background: The aim of this article is to describe the technique of minimally invasive extended thymectomy performed through the transcervical video-thoracoscopic (VATS) approach with elevation of the sternum for the thymic tumors with/without myasthenia gravis (MG). Methods: The operation is done through the collar incision in the neck of a length of 4–8 cm. To facilitate an access to the mediastinum a one-tooth hook connected to the Zakopane bar (Aesculap-Chifa, Nowy Tomysl, Poland) is inserted under the sternal notch for elevation of the sternum. Careful anatomical dissection of the structures of the lower neck region is done with preservation from injury of the thyroid gland, the parathyroid glands and both laryngeal recurrent nerves. The thymus gland is resected en-bloc with the surrounding fatty tissue of the lower neck and the anterior superior mediastinum. -

Endocrine Block اي كالم باللون الذهبي مأخوذ من التيم وورك فايل )الي يقال انه اكسترا( EDITING FLIE Anatomy of Pituitary Gland
PRACTICAL ANATOMY Endocrine Block اي كﻻم باللون الذهبي مأخوذ من التيم وورك فايل )الي يقال انه اكسترا( EDITING FLIE Anatomy Of Pituitary Gland 2 Identify the Pointed areas: 1 1- hypophyseal fossa(Sella turcica). 2-anterior & posterior clinoidal process. The pituitary gland: located in middle cranial fossa and protected in sella turcica (hypophyseal fossa) of body of sphenoid. Relations Of Pituitary Gland Identify the Pointed areas: 1- mamillary bodies (posteriorly). 2 2-optic chiasma (anteriorly). 1 3-Sphenoidal air sinuses (inferior) . 3 4-body of the sphenoid. If Pituitary gland became enlarged (e.g 4 adenoma ) it will cause pressure on optic chiasma and lead to Bilateral temporal eye field blindness Relations Of Pituitary Gland 1 2 Identify the Pointed area : 1- Pituitary gland. 2- Diaphragma sellae (superior). 3-Sphenoidal air sinuses(inferior) . 4-Cavernous sinuses (lateral) . 4 3 Identify the Pointed area : 2 1- Anterior lobe(Adenohypophysis) . 2- optic chiasma 3- infundibulum . 4- Posterior lobe (Neurohypophysis) 3 SUBDIVISIONS OF PITUITARY GLAND 1 Anterior Posterior 4 Lobe(Adenohyp Lobe(Neurohyp ophysis) ophysis) The true gland connected to hypothalamus through hypothalamo- hypophyseal tract synthesizes & Secretes hormones Stores hormones secreted by hypothalamicnuclei receives a nerve supply from some of the hypothalamic nuclei (supraoptic & Hormone-releasing & inhibiting factors paraventricular) The axons of these produced by hypothalamus use nuclei convey their neurosecretion to Hypophyseal Portal System to reach the the Posterior lobe of pituitary gland Anterior lobe of pituitary gland through Hypothalamo-Hypophyseal tract from where it passes into the blood stream. Blood Supply Of Pituitary Gland Identify the Pointed area : 1- Superior hypophyseal artery: supplies infundibulum & forms a capillary network from which vessels pass downward & form sinusoids into the anterior lobe of pituitary gland (hypophyseal portal system). -

Thyroid and Parathyroid Glands
Thyroid and Parathyroid Glands Lecture (2) . Important . Doctors Notes Please check our Editing File . Notes/Extra explanation هذا العمل مبني بشكل أساسي على عمل دفعة 436 مع المراجعة {ومنْْيتو َ ّكْْع َلْْا ِّْللْفَهُوْْحس بهْ} َ َ َ َ َ َ َ َ َ ُ ُ والتدقيق وإضافة المﻻحظات وﻻ يغني عن المصدر اﻷساسي للمذاكرة . Objectives At the end of the lecture, students should be able to: Describe the shape, position, relations and of the thyroid gland. List the blood supply & lymphatic drainage of the thyroid gland. List the nerves endanger with thyroidectomy operation. Describe the shape, position, blood supply & lymphatic drainage of the parathyroid glands. Parts of the deep cervical fascia of the neck o It is divided mainly into 3 layers (or more) important during surgeries: • Investing layer (covers neck completely) • Pretracheal layer (covers thyroid gland and trachea) • Prevertebral layer (surrounds vertebra & prevretbral muscles). o The carotid sheath is part of the deep cervical fascia of the neck Note: At the 4 the corners of the neck, the investing layer separates to form two layers (anterior and posterior layers) to cover the sternocleidomastoid muscle in the anterolateral corner and trapezius muscle in the posterolateral corner "الغدة الدرقية" Thyroid Gland o Endocrine, butterfly shaped gland, Consists of right & left lobes connected to each other by a narrow isthmus, which overlies the 2nd ,3rd & 4th tracheal rings. o The gland is surrounded by a facial sheath derived from the pretracheal layer of the deep cervical fascia, what is the -

THE VARIATIONS of the INFERIOR THYROID VEIN of the DOMESTIC Clit
AUTHOR'S ABSTRACT OF THIS PAPER ISSCED BY THE BIBLIOGR.4PHIC SERVICE, FEBRUbRY 24 THE VARIATIONS OF THE INFERIOR THYROID VEIN OF THE DOMESTIC CLiT HARRISON R. HUNT West Virginia Universitv SEVEN FIGURES The inferior thyroid veins of man vary considerably. The following observations, made on thirty-three domestic cats selected at random, show that the same is true of this vein in the cat. Each of the accompanying figures represents, some- what diagrammatically, the conditions in a single animal. These seven animals suffice to give a fairly complete idea of the variations in the remaining twenty-six. Figure 1 shows the inferior thyroid vein (I) communicating anteriorly with the left internal jugular, receiving branches from only the left lobe of the thyroid gland (14), then passing ob- liquely backward across the trachea (13) to join the right innominate vein (10). The veins labeled 2 and 3 in this and the following figures were not homologized with certainty with the human superior and middle thyroid veins. Two other dis- sections resembled figure 1 very closely, except that in one of them the inferior thyroid vein joined the external jugular vein at a. Figure 2 resembles figure 1 in some respects. However, the inferior thyroid vein (1) in figure 2 receives a branch (a) from the right lobe of the thyroid gland (14), empties into the right internal jugular vein (a), but in the dissection did not appear to communicate directly with the left internal jugular. The inferior thyroid vein in a second cat joined the jugulars at m 39 40 HARRISON R.