No Pain, No Gain: a Case of Exercise-Induced Rhabdomyolysis
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

(12) Patent Application Publication (10) Pub. No.: US 2002/0152483 A1 Reue Et Al
US 2002O1524.83A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2002/0152483 A1 Reue et al. (43) Pub. Date: Oct. 17, 2002 (54) NOVEL GENE ASSOCATED WITH Publication Classification REGULATION OF ADPOSITY AND INSULIN RESPONSE (51) Int. Cl." ............................ A01K 67/00; C12O 1/68; C12P 19/34 (75) Inventors: Karen Reue, Torrance, CA (US); (52) U.S. Cl. .................................. 800/9; 435/6; 435/91.2 Miklos Peterfy, Los Angeles, CA (US) (57) ABSTRACT Correspondence Address: This invention pertains to the identification and isolation of LAW OFFICES OF JONATHAN ALAN QUINE a gene implicated in the fatty liver dystrophy (fld) pheno PO BOX 458 type. Mouse and human forms of the novel gene, designated ALAMEDA, CA 94501 herein as Lpin1/LPIN1 (mouse and human genes, respec tively), are identified. This invention additionally provides (73) Assignee: The Regents of the University of Cali methods of Screening for agents that alter adipose tissue fornia development. The methods involve contacting a cell con taining a Lpin1 gene With a test agent, and detecting a (21) Appl. No.: 10/028,056 change in the expression or activity of a Lpin1 gene product, (22) Filed: Dec. 19, 2001 where a difference in the expression or activity of Lpin1 in the contacted cell indicates that the agent alters or is likely Related U.S. Application Data to alter adipose tissue development. Also provided are methods of identifying Lpin1 mutations, and methods of (60) Provisional application No. 60/257,772, filed on Dec. mitigating Symptoms of lipodystrophy, obesity, diabetes, 22, 2000. atherOSclerosis and related pathologies. -

1 First Presentation of LPIN1 Acute Rhabdomyolysis in Adolescence and Adulthood
Manuscript File Click here to view linked References 1 First presentation of LPIN1 acute rhabdomyolysis in adolescence and adulthood 2 3 Chiara Pizzamiglioa, Nayana Lahirib, Niranjanan Nirmalananthanc, Bhrigu Soodd, Subash 4 Somalankad, Philip Ostrowskie, Rahul Phadkef, Dominic Gerard O’Donovang, Francesco 5 Muntonih, Rosaline Quinlivana 6 7 a. MRC Centre for Neuromuscular Diseases, UCL Institute of Neurology and National Hospital for 8 Neurology and Neurosurgery, Queen Square, London, United Kingdom 9 10 b. Clinical Genetics Department, St George's University Hospitals NHS Foundation Trust, London, 11 United Kingdom 12 13 c. Departments of Neurology and Neuroradiology, Atkinson Morley Regional Neurosciences 14 Centre, St George's Hospital, London, United Kingdom 15 16 d. South West Thames Renal & Transplantation Unit and South West Thames Institute for Renal 17 Research, Saint Helier Hospital, Carshalton, Surrey, United Kingdom 18 19 e. South West Thames Regional Genetics Service, St George's University NHS Foundation Trust, 20 London, United Kingdom 21 22 f. Division of Neuropathology, Dubowitz Neuromuscular Centre, UCL Great Ormond Street 23 Hospital for Children, United Kingdom; Division of Neuropathology, National Hospital for 24 Neurology and Neurosurgery, Queen Square, London, United Kingdom 25 1 26 g. Neuropathology, Department of Histopathology, Addenbrooke’s Hospital, Cambridge University 27 Hospitals NHS Foundation Trust, Cambridge, United Kingdom 28 29 h. Paediatric Neurology, Dubowitz Neuromuscular Centre, UCL Institute of Child Health and Great 30 Ormond Street Hospital for Children, London, United Kingdom 31 32 Corresponding author: Chiara Pizzamiglio ([email protected]) 33 34 Abstract: LPIN1 mutations are a known common cause of autosomal recessive, recurrent and life- 35 threatening acute rhabdomyolysis of childhood-onset. -

Genetic Effects of LPIN1 Polymorphisms on Milk Production Traits in Dairy Cattle
G C A T T A C G G C A T genes Article Genetic Effects of LPIN1 Polymorphisms on Milk Production Traits in Dairy Cattle Bo Han 1, Yuwei Yuan 1, Ruobing Liang 1, Yanhua Li 2, Lin Liu 2 and Dongxiao Sun 1,* 1 Department of Animal Genetics, Breeding and Reproduction, College of Animal Science and Technology, Key Laboratory of Animal Genetics, Breeding and Reproduction of Ministry of Agriculture and Rural Affairs, National Engineering Laboratory for Animal Breeding, China Agricultural University, Beijing 100193, China; [email protected] (B.H.); [email protected] (Y.Y.); [email protected] (R.L.) 2 Beijing Dairy Cattle Center, Qinghe’nanzhen Deshengmenwai Street, Chaoyang District, Beijing 100192, China; [email protected] (Y.L.); [email protected] (L.L.) * Correspondence: [email protected] Received: 12 March 2019; Accepted: 28 March 2019; Published: 2 April 2019 Abstract: Our initial RNA sequencing work identified that lipin 1 (LPIN1) was differentially expressed during dry period, early lactation, and peak of lactation in dairy cows, and it was enriched into the fat metabolic Gene Ontology (GO) terms and pathways, thus we considered LPIN1 as the candidate gene for milk production traits. In this study, we detected the polymorphisms of LPIN1 and verified their genetic effects on milk yield and composition in a Chinese Holstein cow population. We found seven SNPs by re-sequencing the entire coding region and partial flanking region of LPIN1, including one in 50 flanking region, four in exons, and two in 30 flanking region. Of these, four SNPs, c.637T > C, c.708A > G, c.1521C > T, and c.1555A > C, in the exons were predicted to result in the amino acid replacements. -

Low-Fat Clues to Obesity More
RESEARCH HIGHLIGHTS WEB WATCH OBESITY LocusLink — is there life after death? By the time you read this, NCBI’s LocusLink will be no Low-fat clues to obesity more. As of 1 March 2005, it will have been replaced by NCBI’s Entrez Gene. A new insight into the pathways expression predisposed the mice to Born in 1999, LocusLink involved in obesity has come from obesity. However, whereas the has served the genetic community well. It was a surprising source — studies of skeletal-muscle transgenics created to help manage and extremely skinny mice. became obese even on a stan- access increasing amounts Mice that lack a functional Lpin1 dard diet, mice that overex- of sequence data and web gene develop a condition that is pressed Lpin1 in adipose resources. The first known as lipodystrophy, which tissue only put on excess 1 publication to describe it is characterized by a severe lack of weight when they were refers to it as a “web directory” that “provides a adipose tissue. The lipin protein that fed a high-fat diet, indi- single point-of-access to a is encoded by this gene is expressed in cating an important envi- variety of gene-specific adipose tissue and skeletal muscle, ronmental contribution, information sources including and the lack of fatty tissue in lipin- which is reminiscent of web resources and RefSeq”. deficient mice is caused by a failure of human obesity. Throughout its life, adipocytes to differentiate. Jack Phan The authors then LocusLink was continuously updated to inform us not only and Karen Reue had previously shown showed that the causes of about the sequence and that lipin deficiency prevents mice excessive weight gain associ- function of an increasing from becoming obese, and that this ated with increased lipin levels number of species but also works both for mice that are overfed were mediated by different path- about the correct gene and those that are genetically predis- ways in the two types of transgenic nomenclature. -
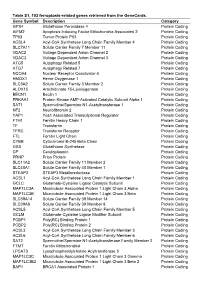
Table S1. 103 Ferroptosis-Related Genes Retrieved from the Genecards
Table S1. 103 ferroptosis-related genes retrieved from the GeneCards. Gene Symbol Description Category GPX4 Glutathione Peroxidase 4 Protein Coding AIFM2 Apoptosis Inducing Factor Mitochondria Associated 2 Protein Coding TP53 Tumor Protein P53 Protein Coding ACSL4 Acyl-CoA Synthetase Long Chain Family Member 4 Protein Coding SLC7A11 Solute Carrier Family 7 Member 11 Protein Coding VDAC2 Voltage Dependent Anion Channel 2 Protein Coding VDAC3 Voltage Dependent Anion Channel 3 Protein Coding ATG5 Autophagy Related 5 Protein Coding ATG7 Autophagy Related 7 Protein Coding NCOA4 Nuclear Receptor Coactivator 4 Protein Coding HMOX1 Heme Oxygenase 1 Protein Coding SLC3A2 Solute Carrier Family 3 Member 2 Protein Coding ALOX15 Arachidonate 15-Lipoxygenase Protein Coding BECN1 Beclin 1 Protein Coding PRKAA1 Protein Kinase AMP-Activated Catalytic Subunit Alpha 1 Protein Coding SAT1 Spermidine/Spermine N1-Acetyltransferase 1 Protein Coding NF2 Neurofibromin 2 Protein Coding YAP1 Yes1 Associated Transcriptional Regulator Protein Coding FTH1 Ferritin Heavy Chain 1 Protein Coding TF Transferrin Protein Coding TFRC Transferrin Receptor Protein Coding FTL Ferritin Light Chain Protein Coding CYBB Cytochrome B-245 Beta Chain Protein Coding GSS Glutathione Synthetase Protein Coding CP Ceruloplasmin Protein Coding PRNP Prion Protein Protein Coding SLC11A2 Solute Carrier Family 11 Member 2 Protein Coding SLC40A1 Solute Carrier Family 40 Member 1 Protein Coding STEAP3 STEAP3 Metalloreductase Protein Coding ACSL1 Acyl-CoA Synthetase Long Chain Family Member 1 Protein -

Deciphering Genetic Associations Using Genome-Wide Epigenomics Approaches
Deciphering genetic associations using genome-wide epigenomics approaches by Xinchen Wang B.Sc. Biochemistry University of Toronto, 2011 Submitted to the Department of Biology in Partial Fulfillment of the Requirements for the Degree of DOCTOR OF PHILOSOPHY at the MASSACHUSETTS INSTITUTE OF TECHNOLOGY June 2017 © Massachusetts Institute of Technology 2017. All rights reserved Signature of Author ......................................................................................................................... Xinchen Wang Department of Biology May 26, 2017 Certified by ........................................................................................................................................ Manolis Kellis Professor of Computer Science Thesis Advisor Certified by ........................................................................................................................................ Laurie A. Boyer Associate Professor of Biology Thesis Advisor Accepted by ....................................................................................................................................... Amy E. Keating Professor of Biology Co-Chair, Biology Graduate Committee 2 Deciphering genetic associations using genome-wide epigenomics approaches . by . Xinchen Wang Submitted to the Department of Biology on May 26, 2017 in Partial Fulfillment of the Requirements for the Degree of Doctor of Philosophy in Biology Abstract Genetic mapping of the drivers of complex human phenotypes and disease through the genome-wide -

A Genetic Investigation of the Muscle and Neuronal Channelopathies: from Sanger to Next – Generation Sequencing
A Genetic Investigation of the Muscle and Neuronal Channelopathies: From Sanger to Next – Generation Sequencing Alice Gardiner MRC Centre for Neuromuscular Diseases and UCL Institute of Neurology Supervised by Professor Henry Houlden and Professor Mike Hanna 1 Declaration I, Alice Gardiner, confirm that the work presented in this thesis is my own. Where information has been derived from other sources, I confirm that this has been indicated in the thesis. Signature A~~~ . Date ~.'t..J.q~ l.?,.q.l.~ . 2 Abstract The neurological channelopathies are a group of hereditary, episodic and frequently debilitating diseases often caused by dysfunction of voltage-gated ion channels. This thesis reports genetic studies of carefully clinically characterised patient cohorts with different episodic neurological and neuromuscular disorders including paroxysmal dyskinesias, episodic ataxia, periodic paralysis and episodic rhabdomyolysis. Genetic and clinical heterogeneity has in the past, using traditional Sanger sequencing methods, made genetic diagnosis difficult and time consuming. This has led to many patients and families being undiagnosed. Here, different sequencing technologies were employed to define the genetic architecture in the paroxysmal disorders. Initially, Sanger sequencing was employed to screen the three known paroxysmal dyskinesia genes in a large cohort of paroxysmal movement disorder patients and smaller mixed episodic phenotype cohort. A genetic diagnosis was achieved in 39% and 13% of the cohorts respectively, and the genetic and phenotypic overlap was highlighted. Subsequently, next-generation sequencing panels were developed, for the first time in our laboratory. Small custom-designed amplicon-based panels were used for the skeletal muscle and neuronal channelopathies. They offered considerable clinical and practical benefit over traditional Sanger sequencing and revealed further phenotypic overlap, however there were still problems to overcome with incomplete coverage. -

Evaluating the Role of LPIN1 Variation in Insulin Resistance, Body Weight, and Human Lipodystrophy in U.K
ORIGINAL ARTICLE Evaluating the Role of LPIN1 Variation in Insulin Resistance, Body Weight, and Human Lipodystrophy in U.K. Populations Katherine A. Fawcett,1 Neil Grimsey,2 Ruth J.F. Loos,3 Eleanor Wheeler,1 Allan Daly,1 Maria Soos,4 Robert Semple,4 Holly Syddall,5 Cyrus Cooper,5 Symeon Siniossoglou,2 Stephen O’Rahilly,4 Nicholas J. Wareham,3 and Ineˆs Barroso1 OBJECTIVE—Loss of lipin 1 activity causes lipodystrophy and insulin resistance in the fld mouse, and LPIN1 expression and common genetic variation were recently suggested to influence ipin 1, a multifunctional protein highly expressed adiposity and insulin sensitivity in humans. We aimed to conduct in mouse and human adipose tissue, has been a comprehensive association study to clarify the influence of shown to influence adipose tissue development common LPIN1 variation on adiposity and insulin sensitivity in Land function. Null mutations in the murine lipin 1 U.K. populations and to examine the role of LPIN1 mutations in gene (Lpin1) result in impaired adipocyte differentiation insulin resistance syndromes. leading to a severe reduction in adipose tissue mass, RESEARCH DESIGN AND METHOD—Twenty-two single nu- insulin resistance, and progressive peripheral neuropathy 2J cleotide polymorphisms tagging common LPIN1 variation were in the fld and fld mouse models (1). In contrast, trans- genotyped in Medical Research Council (MRC) Ely (n ϭ 1,709) genic mice with adipose tissue–specific overexpression of and Hertfordshire (n ϭ 2,901) population-based cohorts. LPIN1 Lpin1 exhibit diet-induced obesity and enhanced insulin exons, exon/intron boundaries, and 3Ј untranslated region were sensitivity compared with those seen in wild-type litter- sequenced in 158 patients with idiopathic severe insulin resis- mates (2). -

Citgenedb: a Comprehensive Database of Human and Mouse
bioRxiv preprint doi: https://doi.org/10.1101/250514; this version posted February 4, 2018. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. CITGeneDB: A comprehensive database of human and mouse genes enhancing or suppressing cold-induced thermogenesis validated by perturbation experiments in mice Jin Li1,2, Su-Ping Deng1,2, Gang Wei3, Peng Yu1,2,* 1Department of Electrical and Computer Engineering & 2TEES-AgriLife Center for Bioinformatics and Genomic Systems Engineering, Texas A&M University, College Station, TX 77843, USA. 3Shanghai Key Laboratory of Diabetes, Shanghai Institute for Diabetes, Shanghai Clinical Medical Centre of Diabetes, Shanghai Key Clinical Centre of Metabolic Diseases, Department of Endocrinology and Metabolism, Shanghai Jiao-Tong University Affiliated Sixth People’s Hospital, Shanghai 200233, China. *Corresponding author. E-mail: [email protected] Abstract Cold-induced thermogenesis increases energy expenditure and can reduce body weight in mammals, so the genes involved in it are thought to be potential therapeutic targets for treating obesity and diabetes. In the quest for more effective therapies, a great deal of research has been conducted to elucidate the regulatory mechanism of cold-induced thermogenesis. Over the last decade, a large number of genes that can enhance or suppress cold-induced thermogenesis have been discovered, but a comprehensive list of these genes is lacking. To fill this gap, we examined all of the annotated human and mouse genes and curated those demonstrated to enhance or suppress cold-induced thermogenesis by in vivo or ex vivo experiments in mice. -

Essential Amino Acid Ratios and Mtor Affect Lipogenic Gene Networks And
Li et al. Journal of Animal Science and Biotechnology (2016) 7:44 DOI 10.1186/s40104-016-0104-x RESEARCH Open Access Essential amino acid ratios and mTOR affect lipogenic gene networks and miRNA expression in bovine mammary epithelial cells Shanshan Li1, Afshin Hosseini2, Marina Danes3, Carolina Jacometo4, Jianxin Liu1* and Juan J. Loor2* Abstract Background: The objective of this study was to study how changing the ratio of Lys to Thr, Lys to His, and Lys to Val affects the expression of lipogenic genes and microRNA (miRNA) in bovine mammary epithelial cells. Results: Triplicate cultures with the respective “optimal” amino acid (AA) ratio (OPAA = Lys:Met 2.9:1; Thr:Phe 1.05:1; Lys:Thr 1.8:1; Lys:His 2.38:1; Lys:Val 1.23:1) plus rapamycin (OPAARMC; positive control), OPAA, Lys:Thr 2.1:1 (LT2.1), Lys:Thr 1.3:1 (LT1.3), Lys:His 3.05:1 (LH3.0), or Lys:Val 1.62:1 (LV1.6) were incubated in lactogenic medium for 12 h. The expression of 15 lipogenic genes and 7 miRNA were evaluated. Responses to LT2.1, LT1.3, LH3.0, and LV1.6 relative to the control (OPAARMC) included up-regulated expression of ACSS2, FABP3, ACACA, FASN, SCD, LPIN1, INSIG1, SREBF1, PPARD, and NR1H3 (commonly known as LXR-α). Furthermore, LV1.6 up-regulated expression of ACSL1, DGAT1, and RXRA and down-regulated PPARG expression. Although no effect of OPAA on expression of PPARG was observed, compared with the control, OPAA up-regulated expression of the PPAR targets ACSS2, FABP3, ACACA, FASN, SCD, LPIN1, INSIG1, and SREBF1. -

LPIN2 Is Associated with Type 2 Diabetes, Glucose Metabolism and Body Composition
Diabetes Publish Ahead of Print, published online September 5, 2007 LPIN2 is associated with type 2 diabetes, glucose metabolism and body composition Yurii S. Aulchenko,1,* Jan Pullen,2 Wigard P. Kloosterman,3 Mojgan Yazdanpanah,1 Albert Hofman,1 Norbert Vaessen,1 Pieter J. L. M. Snijders,1 Dmitry Zubakov,1 Ian Mackay,2,* Mark Olavesen,2 Balbinder Sidhu,2 Vicki E. Smith,2 Alisoun Carey,2 Eugene Berezikov,3 André G. Uittenlinden,4 Ronald H. A. Plasterk,3 Ben A. Oostra1, and Cornelia M. van Duijn1 1Genetic Epidemiology Unit, Department of Epidemiology & Biostatistics, Clinical Genetics, and Forensic Molecular Biology, Erasmus MC Rotterdam, 3000 CA, The Netherlands, 2Oxagen Limited, Abingdon, Oxfordshire, OX14 4RY, United Kingdom, 3Hubrecht Laboratory, Netherlands Institute for Developmental Biology, 3584 CT Utrecht, The Netherlands and 4Department of Internal Medicine, Erasmus MC Rotterdam, 3000 CA, The Netherlands *Present address: National Institute of Agricultural Botany, Cambridge CB3 0LE, UK *To whom correspondence should be addressed: Yurii S. Aulchenko Department of Epidemiology & Biostatistics, Erasmus MC Rotterdam, Postbus 2040, 3000 CA Rotterdam, The Netherlands e-mail: [email protected] Received for publication 11 March 2007 and accepted in revised form 26 August 2007. Additional information for this article can be found in an online appendix at http://diabetes.diabetesjournals.org. Copyright American Diabetes Association, Inc., 2007 ABSTRACT Objective: To identify type 2 diabetes (T2D) gene located at the chromosome 18p11. Research design and methods: We investigated the region in a young genetically isolated population by genotyping 34 single-nucleotide polymorphisms (SNPs) in 78 cases and 101 controls. Two SNPs were selected and followed up in two cohorts. -

Wasin Vol. 9 N. 4 2558.Pmd
Asian Biomedicine Vol. 9 No. 4 August 2015; 455 - 471 DOI: 10.5372/1905-7415.0904.415 Original article Antiaging phenotype in skeletal muscle after endurance exercise is associated with the oxidative phosphorylation pathway Wasin Laohavinija, Apiwat Mutirangurab,c aFaculty of Medicine, Chulalongkorn University, Bangkok 10330, Thailand bDepartment of Anatomy, Faculty of Medicine, Chulalongkorn University, Bangkok 10330, Thailand cCenter of Excellence in Molecular Genetics of Cancer and Human Diseases, Chulalongkorn University, Bangkok 10330, Thailand Background: Performing regular exercise may be beneficial to delay aging. During aging, numerous biochemical and molecular changes occur in cells, including increased DNA instability, epigenetic alterations, cell-signaling disruptions, decreased protein synthesis, reduced adenosine triphosphate (ATP) production capacity, and diminished oxidative phosphorylation. Objectives: To identify the types of exercise and the molecular mechanisms associated with antiaging phenotypes by comparing the profiles of gene expression in skeletal muscle after various types of exercise and aging. Methods: We used bioinformatics data from skeletal muscles reported in the Gene Expression Omnibus repository and used Connection Up- and Down-Regulation Expression Analysis of Microarrays to identify genes significant in antiaging. The significant genes were mapped to molecular pathways and reviewed for their molecular functions, and their associations with molecular and cellular phenotypes using the Database for Annotation,