Metatarsal Stress Fracture
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
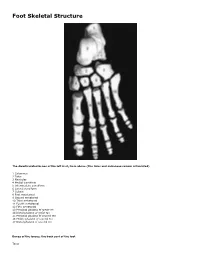
Skeletal Foot Structure
Foot Skeletal Structure The disarticulated bones of the left foot, from above (The talus and calcaneus remain articulated) 1 Calcaneus 2 Talus 3 Navicular 4 Medial cuneiform 5 Intermediate cuneiform 6 Lateral cuneiform 7 Cuboid 8 First metatarsal 9 Second metatarsal 10 Third metatarsal 11 Fourth metatarsal 12 Fifth metatarsal 13 Proximal phalanx of great toe 14 Distal phalanx of great toe 15 Proximal phalanx of second toe 16 Middle phalanx of second toe 17 Distal phalanx of second toe Bones of the tarsus, the back part of the foot Talus Calcaneus Navicular bone Cuboid bone Medial, intermediate and lateral cuneiform bones Bones of the metatarsus, the forepart of the foot First to fifth metatarsal bones (numbered from the medial side) Bones of the toes or digits Phalanges -- a proximal and a distal phalanx for the great toe; proximal, middle and distal phalanges for the second to fifth toes Sesamoid bones Two always present in the tendons of flexor hallucis brevis Origin and meaning of some terms associated with the foot Tibia: Latin for a flute or pipe; the shin bone has a fanciful resemblance to this wind instrument. Fibula: Latin for a pin or skewer; the long thin bone of the leg. Adjective fibular or peroneal, which is from the Greek for pin. Tarsus: Greek for a wicker frame; the basic framework for the back of the foot. Metatarsus: Greek for beyond the tarsus; the forepart of the foot. Talus (astragalus): Latin (Greek) for one of a set of dice; viewed from above the main part of the talus has a rather square appearance. -

Fibular Stress Fractures in Runners
Fibular Stress Fractures in Runners Robert C. Dugan, MS, and Robert D'Ambrosia, MD New Orleans, Louisiana The incidence of stress fractures of the fibula and tibia is in creasing with the growing emphasis on and participation in jog ging and aerobic exercise. The diagnosis requires a high level of suspicion on the part of the clinician. A thorough history and physical examination with appropriate x-ray examination and often technetium 99 methylene diphosphonate scan are re quired for the diagnosis. With the advent of the scan, earlier diagnosis is possible and earlier return to activity is realized. The treatment is complete rest from the precipitating activity and a gradual return only after there is no longer any pain on deep palpation at the fracture site. X-ray findings may persist 4 to 6 months after the initial injury. A stress fracture is best described as a dynamic tigue fracture, spontaneous fracture, pseudofrac clinical syndrome characterized by typical symp ture, and march fracture. The condition was first toms, physical signs, and findings on plain x-ray described in the early 1900s, mostly by military film and bone scan.1 It is a partial or incomplete physicians.5 The first report from the private set fracture resulting from an inability to withstand ting was in 1940, by Weaver and Francisco,6 who nonviolent stress that is applied in a rhythmic, re proposed the term pseudofracture to describe a peated, subthreshold manner.2 The tibiofibular lesion that always occurred in the upper third of joint is the most frequent site.3 Almost invariably one or both tibiae and was characterized on roent the fracture is found in the distal third of the fibula, genograms by a localized area of periosteal thick although isolated cases of proximal fibular frac ening and new bone formation over what appeared tures have also been reported.4 The symptoms are to be an incomplete V-shaped fracture in the cor exacerbated by stress and relieved by inactivity. -

Imaging of Osteomyelitis: the Key Is in the Combination
Special RepoRt Special RepoRt Imaging of osteomyelitis: the key is in the combination An accurate diagnosis of osteomyelitis requires the combination of anatomical and functional imaging techniques. Conventional radiography is the first imaging modality to begin with, as it provides an overview of both the anatomy and the pathologic conditions of the bone. Sonography is most useful in the diagnosis of fluid collections, periosteal involvement and soft tissue abnormalities, and may provide guidance for diagnostic or therapeutic interventions. MRI highlights sites with tissue edema and increased regional perfusion, and provides accurate information of the extent of the infectious process and the tissues involved. To detect osteomyelitis before anatomical changes are present, functional imaging could have some advantages over anatomical imaging. Fluorine-18 fluorodeoxyglucose-PET has the highest diagnostic accuracy for confirming or excluding the diagnosis of chronic osteomyelitis. For both SPECT and PET, specificity improves considerably when the scintigraphic images are fused with computed tomography. Close cooperation between clinicians and imagers remains the key to early and adequate diagnosis when osteomyelitis is suspected or evaluated. †1 KEYWORDS: computed tomography n hybrid systems n imaging n MRI n nuclear Carlos Pineda , medicine n osteomyelitis n ultrasonography Angelica Pena2, Rolando Espinosa2 & Cristina Osteomyelitis is inflammation of the bone that osteomyelitis. The ideal imaging technique Hernández-Díaz1 is usually due to infection. There are different should have a high sensitivity and specificity; 1Musculoskeletal Ultrasound Department, Instituto Nacional de classification systems to categorize osteomyeli- numerous studies have been published con- Rehabilitacion, Avenida tis. Traditionally, it has been labeled as acute, cerning the accuracy of the various modali- Mexico‑Xochimilco No. -

Establishment of a Dental Effects of Hypophosphatasia Registry Thesis
Establishment of a Dental Effects of Hypophosphatasia Registry Thesis Presented in Partial Fulfillment of the Requirements for the Degree Master of Science in the Graduate School of The Ohio State University By Jennifer Laura Winslow, DMD Graduate Program in Dentistry The Ohio State University 2018 Thesis Committee Ann Griffen, DDS, MS, Advisor Sasigarn Bowden, MD Brian Foster, PhD Copyrighted by Jennifer Laura Winslow, D.M.D. 2018 Abstract Purpose: Hypophosphatasia (HPP) is a metabolic disease that affects development of mineralized tissues including the dentition. Early loss of primary teeth is a nearly universal finding, and although problems in the permanent dentition have been reported, findings have not been described in detail. In addition, enzyme replacement therapy is now available, but very little is known about its effects on the dentition. HPP is rare and few dental providers see many cases, so a registry is needed to collect an adequate sample to represent the range of manifestations and the dental effects of enzyme replacement therapy. Devising a way to recruit patients nationally while still meeting the IRB requirements for human subjects research presented multiple challenges. Methods: A way to recruit patients nationally while still meeting the local IRB requirements for human subjects research was devised in collaboration with our Office of Human Research. The solution included pathways for obtaining consent and transferring protected information, and required that the clinician providing the clinical data refer the patient to the study and interact with study personnel only after the patient has given permission. Data forms and a custom database application were developed. Results: The registry is established and has been successfully piloted with 2 participants, and we are now initiating wider recruitment. -

Multiplanar CT Analysis of Fifth Metatarsal Morphology
FAIXXX10.1177/1071100715623041Foot & Ankle InternationalDeSandis et al 623041research-article2015 Article Foot & Ankle International® 2016, Vol. 37(5) 528 –536 Multiplanar CT Analysis of Fifth Metatarsal © The Author(s) 2015 Reprints and permissions: sagepub.com/journalsPermissions.nav Morphology: Implications for Operative DOI: 10.1177/1071100715623041 Management of Zone II Fractures fai.sagepub.com Bridget DeSandis, BA1, Conor Murphy, MD2, Andrew Rosenbaum, MD1, Matthew Levitsky, BA1, Quinn O’Malley1, Gabrielle Konin, MD1, and Mark Drakos, MD1 Abstract Background: Percutaneous internal fixation is currently the method of choice treating proximal zone II fifth metatarsal fractures. Complications have been reported due to poor screw placement and inadequate screw sizing. The purpose of this study was to define the morphology of the fifth metatarsal to help guide surgeons in selecting the appropriate screw size preoperatively. Methods: Multiplanar analysis of fifth metatarsal morphology was completed using computed tomographic (CT) scans from 241 patients. Specific parameters were analyzed and defined in anteroposterior (AP), lateral, and oblique views including metatarsal length, distance from the base to apex of curvature, apex medullary canal width, apex height, and fifth metatarsal angle. Results: The average metatarsal length in the AP view was 71.4 ± 6.1 mm and in the lateral view 70.4 ± 6.0 mm, with 95% of patients having lengths between 59.3 and 83.5 mm and 58.4 and 82.4 mm, respectively. The average canal width at the apex of curvature was 4.1 ± 0.9 mm in the AP view and 5.3 ± 1.1 mm in the lateral view, with 95% of patients having widths between 2.2 and 5.9 mm and 3.2 and 7.5 mm, respectively. -

In a Child with Myositis Ossificans Progressiva
Pediatr Radiol (1993) 23:45%462 Pediatric Radiology Springer-Verlag 1993 Chronic intoxication by ethane-l-hydroxy-l,l-diphosphonate (EHDP) in a child with myositis ossificans progressiva U. E. Pazzaglia 1, G. Beluffi 2, A. Ravelli 3, G. Zatti 1, A. Martini 3 1 Clinica Ortopedica, Ospedale F. Del Ponte, Varese, Italy 2 Servizio di Radiodiagnostica, Sezione Radiologia Pediatrica, Pavia, Italy 3 Clinica Pediatrica dell'Universit~ di Pavia, IRCCS Policlinico S. Matteo, Pavia, Italy Received: 4 February 1993/Accepted: 25 March 1993 Abstract. A child with myositis ossificans progressiva was opsy performed elsewhere did not show any relevant pathological treated for 8 years with ethane-l-hydroxy-l,l-diphospho- change. Treatment with steroid was started and continued for sev- eral months. nate (EHDP) 30-40 mg/kg per day. Latterly he com- One and half years later a large soft tissue swelling appeared in plained of severe, progressive bone and joint pain which the shoulder girdle and followed a course similar to the lesion in the made standing and walking almost impossible. A radio- sternodeidomastoid muscle. The child was admitted to another hos- graphic skeletal survey showed diffuse ricket-like lesions. pital 1 month later. Laboratory tests showed that inflammatory pa- Withdrawal of EHDP therapy produced substantial im- rameters, serum calcium and phosphate, alkaline phosphatase and provement in his general condition as well as in the radio- muscle enzymes were normal. Electromyography was also normal. graphic appearance of the bones. Multiple exostoses were A muscle biopsy was consistent with myositis ossificans progressiva. Therapy was started with ethane-l-hydroxyd,l-diphosphonate observed in this case and, particularly those around the (EHDP) 30 mg/kg per day. -

Rethinking the Evolution of the Human Foot: Insights from Experimental Research Nicholas B
© 2018. Published by The Company of Biologists Ltd | Journal of Experimental Biology (2018) 221, jeb174425. doi:10.1242/jeb.174425 REVIEW Rethinking the evolution of the human foot: insights from experimental research Nicholas B. Holowka* and Daniel E. Lieberman* ABSTRACT presumably owing to their lack of arches and mobile midfoot joints Adaptive explanations for modern human foot anatomy have long for enhanced prehensility in arboreal locomotion (see Glossary; fascinated evolutionary biologists because of the dramatic differences Fig. 1B) (DeSilva, 2010; Elftman and Manter, 1935a). Other studies between our feet and those of our closest living relatives, the great have documented how great apes use their long toes, opposable apes. Morphological features, including hallucal opposability, toe halluces and mobile ankles for grasping arboreal supports (DeSilva, length and the longitudinal arch, have traditionally been used to 2009; Holowka et al., 2017a; Morton, 1924). These observations dichotomize human and great ape feet as being adapted for bipedal underlie what has become a consensus model of human foot walking and arboreal locomotion, respectively. However, recent evolution: that selection for bipedal walking came at the expense of biomechanical models of human foot function and experimental arboreal locomotor capabilities, resulting in a dichotomy between investigations of great ape locomotion have undermined this simple human and great ape foot anatomy and function. According to this dichotomy. Here, we review this research, focusing on the way of thinking, anatomical features of the foot characteristic of biomechanics of foot strike, push-off and elastic energy storage in great apes are assumed to represent adaptations for arboreal the foot, and show that humans and great apes share some behavior, and those unique to humans are assumed to be related underappreciated, surprising similarities in foot function, such as to bipedal walking. -

Common Stress Fractures BRENT W
COVER ARTICLE PRACTICAL THERAPEUTICS Common Stress Fractures BRENT W. SANDERLIN, LCDR, MC, USNR, Naval Branch Medical Clinic, Fort Worth, Texas ROBERT F. RASPA, CAPT, MC, USN, Naval Hospital Jacksonville, Jacksonville, Florida Lower extremity stress fractures are common injuries most often associated with partic- ipation in sports involving running, jumping, or repetitive stress. The initial diagnosis can be made by identifying localized bone pain that increases with weight bearing or repet- itive use. Plain film radiographs are frequently unrevealing. Confirmation of a stress frac- ture is best made using triple phase nuclear medicine bone scan or magnetic resonance imaging. Prevention of stress fractures is most effectively accomplished by increasing the level of exercise slowly, adequately warming up and stretching before exercise, and using cushioned insoles and appropriate footwear. Treatment involves rest of the injured bone, followed by a gradual return to the sport once free of pain. Recent evidence sup- ports the use of air splinting to reduce pain and decrease the time until return to full par- ticipation or intensity of exercise. (Am Fam Physician 2003;68:1527-32. Copyright© 2003 American Academy of Family Physicians) tress fractures are among the involving repetitive use of the arms, such most common sports injuries as baseball or tennis. Stress fractures of and are frequently managed the ribs occur in sports such as rowing. by family physicians. A stress Upper extremity and rib stress fractures fracture should be suspected in are far less common than lower extremity Sany patient presenting with localized stress fractures.1 bone or periosteal pain, especially if he or she recently started an exercise program Etiology and Pathophysiology or increased the intensity of exercise. -

Overuse Injuries in Sport: a Comprehensive Overview R
Aicale et al. Journal of Orthopaedic Surgery and Research (2018) 13:309 https://doi.org/10.1186/s13018-018-1017-5 REVIEW Open Access Overuse injuries in sport: a comprehensive overview R. Aicale1*, D. Tarantino1 and N. Maffulli1,2 Abstract Background: The absence of a single, identifiable traumatic cause has been traditionally used as a definition for a causative factor of overuse injury. Excessive loading, insufficient recovery, and underpreparedness can increase injury risk by exposing athletes to relatively large changes in load. The musculoskeletal system, if subjected to excessive stress, can suffer from various types of overuse injuries which may affect the bone, muscles, tendons, and ligaments. Methods: We performed a search (up to March 2018) in the PubMed and Scopus electronic databases to identify the available scientific articles about the pathophysiology and the incidence of overuse sport injuries. For the purposes of our review, we used several combinations of the following keywords: overuse, injury, tendon, tendinopathy, stress fracture, stress reaction, and juvenile osteochondritis dissecans. Results: Overuse tendinopathy induces in the tendon pain and swelling with associated decreased tolerance to exercise and various types of tendon degeneration. Poor training technique and a variety of risk factors may predispose athletes to stress reactions that may be interpreted as possible precursors of stress fractures. A frequent cause of pain in adolescents is juvenile osteochondritis dissecans (JOCD), which is characterized by delamination and localized necrosis of the subchondral bone, with or without the involvement of articular cartilage. The purpose of this compressive review is to give an overview of overuse injuries in sport by describing the theoretical foundations of these conditions that may predispose to the development of tendinopathy, stress fractures, stress reactions, and juvenile osteochondritis dissecans and the implication that these pathologies may have in their management. -

Metric and Non Metric Characteristics of Human Forefoot: a Radiological Study in Egyptian Population
Australian Journal of Basic and Applied Sciences 2019 February; 13(2): pages 46-54 DOI: 10.22587/ajbas.2019.13.2.6 Original paper AENSI Publications Journal home page: www.ajbasweb.com Metric and Non metric characteristics of human forefoot: A radiological study in Egyptian population Samah Mohammed, Mahmoud Abozaid and Fatma Elzahraa, Fouad Abd Elbaky Department of Anatomy, Faculty of medicine, Minia University, Minia, Egypt. Correspondence Author: Samah Mohammed, Department of Anatomy, Faculty of medicine, Minia University, Minia, Egypt. Received date: 1 January 2019, Accepted date: 15 January 2018, Online date: 28 February 2019 Copyright: © 2019 Samah Mohammed et al, This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Human forefoot is composed of metatarsal bones and phalanges. Their morphology and dimensions are important for proper bipedal locomotor function. Structural defects affecting forefoot bones result in foot dysfunction. The aim of the present study is to describe the morphology of the bones of forefoot and to measure their lengths and widths. A digital radiographic study was conducted on right and left feet of 100 healthy individuals (50 males and 50 females) above 21 years old. Inspection of the forefoot bones using radiographs was done to describe general shapes of bones. The lengths and widths of metatarsal bone and phalanges were measured using Digital Imaging and Communications in Medicine (DICOM) format. Mean and standard deviations were obtained for all measurements of each side of both sexes. -

Osteoblastic Heparan Sulfate Regulates Osteoprotegerin Function and Bone Mass
Osteoblastic heparan sulfate regulates osteoprotegerin function and bone mass Satoshi Nozawa, … , Haruhiko Akiyama, Yu Yamaguchi JCI Insight. 2018;3(3):e89624. https://doi.org/10.1172/jci.insight.89624. Research Article Bone biology Bone remodeling is a highly coordinated process involving bone formation and resorption, and imbalance of this process results in osteoporosis. It has long been recognized that long-term heparin therapy often causes osteoporosis, suggesting that heparan sulfate (HS), the physiological counterpart of heparin, is somehow involved in bone mass regulation. The role of endogenous HS in adult bone, however, remains unclear. To determine the role of HS in bone homeostasis, we conditionally ablated Ext1, which encodes an essential glycosyltransferase for HS biosynthesis, in osteoblasts. Resultant conditional mutant mice developed severe osteopenia. Surprisingly, this phenotype is not due to impairment in bone formation but to enhancement of bone resorption. We show that osteoprotegerin (OPG), which is known as a soluble decoy receptor for RANKL, needs to be associated with the osteoblast surface in order to efficiently inhibit RANKL/RANK signaling and that HS serves as a cell surface binding partner for OPG in this context. We also show that bone mineral density is reduced in patients with multiple hereditary exostoses, a genetic bone disorder caused by heterozygous mutations of Ext1, suggesting that the mechanism revealed in this study may be relevant to low bone mass conditions in humans. Find the latest version: https://jci.me/89624/pdf RESEARCH ARTICLE Osteoblastic heparan sulfate regulates osteoprotegerin function and bone mass Satoshi Nozawa,1,2 Toshihiro Inubushi,1 Fumitoshi Irie,1 Iori Takigami,2 Kazu Matsumoto,2 Katsuji Shimizu,2 Haruhiko Akiyama,2 and Yu Yamaguchi1 1Human Genetics Program, Sanford Burnham Prebys Medical Discovery Institute, La Jolla, California, USA. -

Long Term Treatment of Recurring Pathological Fractures Due to Mccune Albright Syndrome: Case Report and Literature Review
Vol.2, No.9, 562-567 (2013) Case Reports in Clinical Medicine http://dx.doi.org/10.4236/crcm.2013.29142 Long term treatment of recurring pathological fractures due to Mccune Albright Syndrome: Case report and literature review Yoshvin Sunnassee, Yuhui Shen, Rong Wan, Jianqiang Xu, Weibin Zhang* Department of Orthopedics, Shanghai Ruijin Hospital, Shanghai Jiao Tong University School of Medicine, Shanghai Institute of Traumatology and Orthopedics, Shanghai, China; *Corresponding Author: [email protected] Received 17 June 2013; revised 15 July 2013; accepted 10 August 2013 Copyright © 2013 Yoshvin Sunnassee et al. This is an open access article distributed under the Creative Commons Attribution Li- cense, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. In accordance of the Creative Commons Attribution License all Copyrights © 2013 are reserved for SCIRP and the owner of the intel- lectual property Yoshvin Sunnassee et al. All Copyright © 2013 are guarded by law and by SCIRP as a guardian. ABSTRACT mentation, precocious puberty and polyostotic fibrous dysplasia (PFD) [1,2]. Patients with PFD have poor bone McCune Albright syndrome is a rare genetic quality and are liable to pathological fractures. We here- disorder which is characterized by café au lait by report the case of a male patient who is treated for 7 skin pigmentation, precocious puberty and poly- years in our center for recurring pathological fractures of ostotic fibrous dysplasia. Treating recurring pa- the femur due to MAS. When the patient was first seen, thological fractures due to Albright syndrome is he presented with a shepherd’s crook deformity of the a very challenging endeavor, and more so when proximal femur.