Unwarranted Administration of Acetylcholinesterase Inhibitors Can
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

The Role of Serotonin in Memory: Interactions with Neurotransmitters and Downstream Signaling
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Bushehr University of Medical Sciences Repository Exp Brain Res (2014) 232:723–738 DOI 10.1007/s00221-013-3818-4 REVIEW The role of serotonin in memory: interactions with neurotransmitters and downstream signaling Mohammad Seyedabadi · Gohar Fakhfouri · Vahid Ramezani · Shahram Ejtemaei Mehr · Reza Rahimian Received: 28 April 2013 / Accepted: 20 December 2013 / Published online: 16 January 2014 © Springer-Verlag Berlin Heidelberg 2014 Abstract Serotonin, or 5-hydroxytryptamine (5-HT), is there has been an alteration in the density of serotonergic found to be involved in many physiological or pathophysi- receptors in aging and Alzheimer’s disease, and serotonin ological processes including cognitive function. Seven dis- modulators are found to alter the process of amyloidogen- tinct receptors (5-HT1–7), each with several subpopulations, esis and exert cognitive-enhancing properties. Here, we dis- have been identified for serotonin, which are different in cuss the serotonin-induced modulation of various systems terms of localization and downstream signaling. Because involved in mnesic function including cholinergic, dopa- of the development of selective agonists and antagonists minergic, GABAergic, glutamatergic transmissions as well for these receptors as well as transgenic animal models as amyloidogenesis and intracellular pathways. of cognitive disorders, our understanding of the role of serotonergic transmission in learning and memory has Keywords Serotonin · Memory · Signaling pathways improved in recent years. A large body of evidence indi- cates the interplay between serotonergic transmission and Abbreviations other neurotransmitters including acetylcholine, dopamine, 2PSDT Two-platform spatial discrimination task γ-aminobutyric acid (GABA) and glutamate, in the neu- 3xTg-AD Triple-transgenic mouse model of Alzheimer’s robiological control of learning and memory. -

Neuronal Nicotinic Receptors
NEURONAL NICOTINIC RECEPTORS Dr Christopher G V Sharples and preparations lend themselves to physiological and pharmacological investigations, and there followed a Professor Susan Wonnacott period of intense study of the properties of nAChR- mediating transmission at these sites. nAChRs at the Department of Biology and Biochemistry, muscle endplate and in sympathetic ganglia could be University of Bath, Bath BA2 7AY, UK distinguished by their respective preferences for C10 and C6 polymethylene bistrimethylammonium Susan Wonnacott is Professor of compounds, notably decamethonium and Neuroscience and Christopher Sharples is a hexamethonium,5 providing the first hint of diversity post-doctoral research officer within the among nAChRs. Department of Biology and Biochemistry at Biochemical approaches to elucidate the structure the University of Bath. Their research and function of the nAChR protein in the 1970’s were focuses on understanding the molecular and facilitated by the abundance of nicotinic synapses cellular events underlying the effects of akin to the muscle endplate, in electric organs of the acute and chronic nicotinic receptor electric ray,Torpedo , and eel, Electrophorus . High stimulation. This is with the goal of affinity snakea -toxins, principallyaa -bungarotoxin ( - Bgt), enabled the nAChR protein to be purified, and elucidating the structure, function and subsequently resolved into 4 different subunits regulation of neuronal nicotinic receptors. designateda ,bg , and d .6 An additional subunit, e , was subsequently identified in adult muscle. In the early 1980’s, these subunits were cloned and sequenced, The nicotinic acetylcholine receptor (nAChR) arguably and the era of the molecular analysis of the nAChR has the longest history of experimental study of any commenced. -

Monoamine Oxidase Inhibitors: Promising Therapeutic Agents for Alzheimer's Disease (Review)
MOLECULAR MEDICINE REPORTS 9: 1533-1541, 2014 Monoamine oxidase inhibitors: Promising therapeutic agents for Alzheimer's disease (Review) ZHIYOU CAI Department of Neurology, The Lu'an Affiliated Hospital of Anhui Medical University, Lu'an People's Hospital, Lu'an, Anhui 237005, P.R. China Received July 2, 2013; Accepted February 10, 2014 DOI: 10.3892/mmr.2014.2040 Abstract. Activated monoamine oxidase (MAO) has a critical 6. MAO activation contributes to cognitive impairment in role in the pathogenesis of Alzheimer's disease (AD), including patients with AD the formation of amyloid plaques from amyloid β peptide (Aβ) 7. Activated MAO contributes to the formation of amyloid production and accumulation, formation of neurofibrillary plaques tangles, and cognitive impairment via the destruction of cholin- 8. Is activated MAO associated with the formation of ergic neurons and disorder of the cholinergic system. Several neurofibrillary tangles? studies have indicated that MAO inhibitors improve cognitive 9. Evidence for the neuroprotective effect of MAO inhibitors deficits and reverse Aβ pathology by modulating proteolytic in AD cleavage of amyloid precursor protein and decreasing Aβ 10. Conclusions and outlook protein fragments. Thus, MAO inhibitors may be considered as promising therapeutic agents for AD. 1. Introduction Monoamine oxidase (MAO) catalyzes the oxidative deamina- Contents tion of biogenic and xenobiotic amines and has an important role in the metabolism of neuroactive and vasoactive amines in 1. Introduction the central nervous system (CNS) and peripheral tissues. The 2. Monoamine oxidase (MAO) enzyme preferentially degrades benzylamine and phenylethyl- 3. Involvement of MAO in neurodegeneration amine and targets a wide variety of specific neurotransmitters 4. -

Alzheimer Dementia: Starting, Stopping Drug Therapy
REVIEW CME CREDIT LUKE D. KIM, MD, FACP, CMD RONAN M. FACTORA, MD, FACP, AGSF Assistant Professor of Medicine, Cleveland Clinic Lerner Assistant Professor of Medicine, Cleveland Clinic Lerner College of Medicine of Case Western Reserve University, College of Medicine of Case Western Reserve University, Cleveland, OH; Center for Geriatric Medicine, Medicine Cleveland, OH; Center for Geriatric Medicine, Medicine Institute, Cleveland Clinic Institute, Cleveland Clinic Alzheimer dementia: Starting, stopping drug therapy ABSTRACT lzheimer disease is the most common A form of dementia. In 2016, an estimated Alzheimer disease is the most common type of dementia. 5.2 million Americans age 65 and older had Two classes of cognition-enhancing drugs are approved Alzheimer disease. The prevalence is project- to treat the symptoms, and both have provided modest ed to increase to 13.8 million by 2050, includ- benefi t in clinical trials. Psychotropic drugs are sometimes ing 7 million people age 85 and older.1 used off-label to treat behavioral symptoms of Alzheimer Although no cure for dementia exists, sev- disease. All these medications should be continuously eral cognition-enhancing drugs have been ap- evaluated for clinical effi cacy and, when appropriate, proved by the US Food and Drug Administra- discontinued if the primary benefi t—preservation of cog- tion (FDA) to treat the symptoms of Alzheimer nitive and functional status and a reduction in behaviors dementia. The purpose of these drugs is to associated with dementia—is no longer being achieved. stabilize cognitive and functional status, with a secondary benefi t of potentially reducing be- KEY POINTS havioral problems associated with dementia. -

Cholinergic Treatments with Emphasis on M1 Muscarinic Agonists As Potential Disease-Modifying Agents for Alzheimer’S Disease
Neurotherapeutics: The Journal of the American Society for Experimental NeuroTherapeutics Cholinergic Treatments with Emphasis on M1 Muscarinic Agonists as Potential Disease-Modifying Agents for Alzheimer’s Disease Abraham Fisher Israel Institute for Biological Research, P. O. Box 19, Ness-Ziona 74100, Israel Summary: The only prescribed drugs for treatment of Alzhei- formation of -amyloid plaques, and tangles containing hyper- mer’s disease (AD) are acetylcholinesterase inhibitors (e.g., phosphorylated tau proteins) are apparently linked. Such link- donepezil, rivastigmine, galantamine, and tacrine) and meman- ages may have therapeutic implications, and this review is an tine, an NMDA antagonist. These drugs ameliorate mainly the attempt to analyze these versus the advantages and drawbacks symptoms of AD, such as cognitive impairments, rather than of some cholinergic compounds, such as acetylcholinesterase halting or preventing the causal neuropathology. There is cur- inhibitors, M1 muscarinic agonists, M2 antagonists, and nico- rently no cure for AD and there is no way to stop its progres- tinic agonists. Among the reviewed treatments, M1 selective sion, yet there are numerous therapeutic approaches directed agonists emerge, in particular, as potential disease modifiers. against various pathological hallmarks of AD that are exten- Key Words: Alzheimer’s, cholinergic, -amyloid, tau, acetyl- sively being pursued. In this context, the three major hallmark cholinesterase inhibitors, M1 muscarinic, nicotinic, agonists, characteristics of AD (i.e., the CNS cholinergic hypofunction, M2 muscarinic antagonists. INTRODUCTION (␣-APPs) that is neurotrophic and neuroprotective. In an alternate pathway, -secretase (BACE1) cleaves APP Alzheimer’s disease (AD) is a progressive, neurode- releasing a large secreted derivative sAPP andaC- generative disease that is a major health problem in terminal fragment C99 that can be further cleaved by modern societies. -

Treating Dementia with Cholinesterase Inhibitors Patient Information - Older Persons Mental Health
Treating Dementia with Cholinesterase Inhibitors Patient information - Older Persons Mental Health www.cdhb.health.nz/patientinfo Dementia is a progressive disease of the brain in which brain cells die and are not replaced. It results in impaired memory, thinking and behaviour. In recent years a number of medications for dementia have become available in New Zealand, includ- ing cholinesterase inhibitors, which are discussed below. For more information, please contact your GP or specialist. Other useful sources of information are Alzhei- mer’s Canterbury (314 Worcester St, Christchurch, phone (03) 379 2590) and the website www.alzheimers.org.nz click on “your Alzheimer’s organisation” to take you to Canterbury. Cholinesterase Cholinesterase Treating Dementia with with Dementia Treating Inhibitors Older Older Persons Mental Health How do cholinesterase inhibitors work? Cholinesterase inhibitors are designed to enhance memory and other brain functions by influencing chemical activity in the brain. Acetylcholine is a chemical messenger in the brain that is thought to be important for the function of brain cells involved in memory, thought and judgement. Acetylcholine is released by one brain cell to transmit a message to another. Once a message is received, various enzymes, including some called cholinesterases, break down the chemical messenger for reuse. In the brain affected by dementia, the cells that produce acetylcholine are damaged or destroyed, resulting in lower levels of the chemical messenger. A cholinesterase inhibitor is designed to reduce the activity of the cholinesterases, thereby slowing down the breakdown of acetylcholine. By maintaining levels of acetylcholine, the drug may help compensate for the loss of functioning brain cells. -

Drug Treatments for Alzheimer's Disease
Factsheet 407LP Drug treatments December 2014 for Alzheimer’s disease There are no drug treatments that can cure Alzheimer’s disease or any other common type of dementia. However, medicines have been developed for Alzheimer’s disease that can temporarily alleviate symptoms, or slow down their progression, in some people. This factsheet explains how the main drug treatments for Alzheimer’s disease work, how to access them, and when they can be prescribed and used effectively. For more information about Alzheimer’s disease see factsheet 401, What is Alzheimer’s disease? Contents n What are the main drugs used? n How do they work? n Are these drugs effective for everyone with Alzheimer’s disease? n Are there any side effects? n How are these drugs prescribed? n Are these drugs effective for other types of dementia? n Taking the drugs n Questions to ask the doctor when starting the drugs n Stopping treatment n NICE guidance: a summary n Research into new treatments n Other useful organisations. 2 Drug treatments for Alzheimer’s disease Drug treatments for Alzheimer’s disease Drug treatment for Alzheimer’s disease is important, but the benefits are small, and drugs should only be one part of a person’s overall care. Non- drug treatments, activities and support are just as important in helping someone to live well with Alzheimer’s disease. Many drugs have at least two names. The generic name identifies the substance. The brand name varies depending on the company that manufactures it. For example, a familiar painkiller has the generic name paracetamol and is manufactured under brand names such as Panadol and Calpol, among others. -
Neuromuscular Blocking Agents
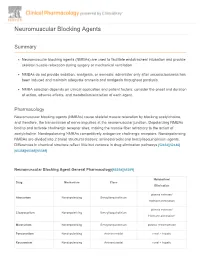
Neuromuscular Blocking Agents Summary Neuromuscular blocking agents (NMBAs) are used to facilitate endotracheal intubation and provide skeletal muscle relaxation during surgery or mechanical ventilation. NMBAs do not provide sedation, analgesia, or amnesia; administer only after unconsciousness has been induced and maintain adequate amnesia and analgesia throughout paralysis. NMBA selection depends on clinical application and patient factors; consider the onset and duration of action, adverse effects, and metabolism/excretion of each agent. Pharmacology Neuromuscular blocking agents (NMBAs) cause skeletal muscle relaxation by blocking acetylcholine, and therefore, the transmission of nerve impulses at the neuromuscular junction. Depolarizing NMBAs bind to and activate cholinergic receptor sites, making the muscle fiber refractory to the action of acetylcholine. Nondepolarizing NMBAs competitively antagonize cholinergic receptors. Nondepolarizing NMBAs are divided into 2 broad structural classes: aminosteroidal and benzylisoquinolinium agents. Differences in chemical structure reflect little but variance in drug elimination pathways.[52452][52486] [65358][65369][65389] Neuromuscular Blocking Agent General Pharmacology[65358][65369] Metabolism/ Drug Mechanism Class Elimination plasma esterase/ Atracurium Nondepolarizing Benzylisoquinolinium Hofmann elimination plasma esterase/ Cisatracurium Nondepolarizing Benzylisoquinolinium Hofmann elimination* Mivacurium Nondepolarizing Benzylisoquinolinium plasma cholinesterase Pancuronium Nondepolarizing -

Monoamine Oxidase B Is Elevated in Alzheimer Disease Neurons, Is Associated with Γ-Secretase and Regulates Neuronal Amyloid Β
Schedin-Weiss et al. Alzheimer's Research & Therapy (2017) 9:57 DOI 10.1186/s13195-017-0279-1 RESEARCH Open Access Monoamine oxidase B is elevated in Alzheimer disease neurons, is associated with γ-secretase and regulates neuronal amyloid β-peptide levels Sophia Schedin-Weiss1*, Mitsuhiro Inoue1,2, Lenka Hromadkova3,4, Yasuhiro Teranishi1,2, Natsuko Goto Yamamoto1,2, Birgitta Wiehager1, Nenad Bogdanovic5, Bengt Winblad1, Anna Sandebring-Matton1, Susanne Frykman1 and Lars O. Tjernberg1 Abstract Background: Increased levels of the pathogenic amyloid β-peptide (Aβ), released from its precursor by the transmembrane protease γ-secretase, are found in Alzheimer disease (AD) brains. Interestingly, monoamine oxidase B (MAO-B) activity is also increased in AD brain, but its role in AD pathogenesis is not known. Recent neuroimaging studies have shown that the increased MAO-B expression in AD brain starts several years before the onset of the disease. Here, we show a potential connection between MAO-B, γ-secretase and Aβ in neurons. Methods: MAO-B immunohistochemistry was performed on postmortem human brain. Affinity purification of γ- secretase followed by mass spectrometry was used for unbiased identification of γ-secretase-associated proteins. The association of MAO-B with γ-secretase was studied by coimmunoprecipitation from brain homogenate, and by in-situ proximity ligation assay (PLA) in neurons as well as mouse and human brain sections. The effect of MAO-B on Aβ production and Notch processing in cell cultures was analyzed by siRNA silencing or overexpression experiments followed by ELISA, western blot or FRET analysis. Methodology for measuring relative intraneuronal MAO-B and Aβ42 levels in single cells was developed by combining immunocytochemistry and confocal microscopy with quantitative image analysis. -

Norepinephrine May Oppose Other Neuromodulators to Impact Alzheimer’S Disease
International Journal of Molecular Sciences Hypothesis Norepinephrine May Oppose Other Neuromodulators to Impact Alzheimer’s Disease Paul J. Fitzgerald Department of Psychiatry, University of Michigan, Ann Arbor, MI 48109, USA; pfi[email protected] Abstract: While much of biomedical research since the middle of the twentieth century has focused on molecular pathways inside the cell, there is increasing evidence that extracellular signaling pathways are also critically important in health and disease. The neuromodulators norepinephrine (NE), serotonin (5-hydroxytryptamine, 5HT), dopamine (DA), acetylcholine (ACH), and melatonin (MT) are extracellular signaling molecules that are distributed throughout the brain and modulate many disease processes. The effects of these five neuromodulators on Alzheimer’s disease (AD) are briefly examined in this paper, and it is hypothesized that each of the five molecules has a u- shaped (or Janus-faced) dose-response curve, wherein too little or too much signaling is pathological in AD and possibly other diseases. In particular it is suggested that NE is largely functionally opposed to 5HT, ACH, MT, and possibly DA in AD. In this scenario, physiological “balance” between the noradrenergic tone and that of the other three or four modulators is most healthy. If NE is largely functionally opposed to other prominent neuromodulators in AD, this may suggest novel combinations of pharmacological agents to counteract this disease. It is also suggested that the majority of cases of AD and possibly other diseases involve an excess of noradrenergic tone and a collective deficit of the other four modulators. Keywords: neurodegeneration; dementia; cognitive impairment; noradrenaline; locus coeruleus; Citation: Fitzgerald, P.J. clonidine; guanfacine; propranolol; prazosin; terazosin; cholinesterase inhibitors Norepinephrine May Oppose Other Neuromodulators to Impact Alzheimer’s Disease. -

Binding of the Nicotinic Cholinergic Antagonist, Dihydro-&Erythroidine, to Rat Brain Tissue
0270.6474/84/0412-2906$02,00/O The Journal of Neuroscience Copyright 0 Society for Neuroscience Vol. 4, No. 12, pp. 2906-2911 Printed in U.S.A. December 1964 BINDING OF THE NICOTINIC CHOLINERGIC ANTAGONIST, DIHYDRO-&ERYTHROIDINE, TO RAT BRAIN TISSUE’ MICHAEL WILLIAMS’ AND JANET L. ROBINSON Merck Institute for Therapeutic Research, Merck, Sharp and Dohme Research Laboratories, West Point, Pennsylvania Received November 3, 1983; Revised April 20, 1984; Accepted May 8, 1984 Abstract The nicotinic cholinergic antagonist, dihydro-P-erythroidine, binds to two sites in rat cortical membranes with dissociation constants of 4 and 22 nM and respective apparent B,,, values of 52 and 164 fmol/mg of protein. Binding to the higher affinity site, defined by the use of 2 nM (3H]dihydro-/3-erythroidine, was saturable, reversible, and susceptible to protein denaturation. Binding was highest in the thalamus and lowest in the spinal cord and showed preferential enrichment in a synaptosomal subfraction of rat brain. Nicotine displaced [3H]dihydro-/3-erythroidine in a stereospecitic manner, the (-)-isomer being approximately 6 times more potent than the (+)-isomer. The alkaloid nicotinic agonists, cytisine and lobeline, were potent inhibitors of binding, while acetylcholine in the presence of the cholinesterase inhibitor di-isopropylfluorophosphate was equipotent with (+)-nicotine. Binding was also inhibited by the muscarinic ligands, arecoline, atropine, and oxotremorine. The nicotinic antagonists mecamylamine, hexamethonium, and pempidine were essentially inactive in displacing [3H]dihydro-fi-erythroidine. These findings indicate that dihydro-B-erythroidine binds to a nicotinic recognition site in rat brain which is neuromuscular, rather than ganglionic, in nature and that such binding is similar in several respects to that seen with nicotinic agonists. -

The Pipeline and Future of Drug Development In
Molecular Psychiatry (2007) 12, 904–922 & 2007 Nature Publishing Group All rights reserved 1359-4184/07 $30.00 www.nature.com/mp FEATURE REVIEW The pipeline and future of drug development in schizophrenia JA Gray1 and BL Roth2 1Department of Psychiatry, University of California, San Francisco, CA, USA and 2Department of Pharmacology, University of North Carolina School of Medicine, Chapel Hill, NC, USA While the current antipsychotic medications have profoundly impacted the treatment of schizophrenia over the past 50 years, the newer atypical antipsychotics have not fulfilled initial expectations, and enormous challenges remain in long-term treatment of this debilitating disease. In particular, improved treatment of the negative symptoms and cognitive dysfunction in schizophrenia which greatly impact overall morbidity is needed. In this review we will briefly discuss the current pipeline of drugs for schizophrenia, outlining many of the strategies and targets currently under investigation for the development of new schizophrenia drugs. Many of these compounds have great potential as augmenting agents in the treatment of negative symptoms and cognition. In addition, we will highlight the importance of developing new paradigms for drug discovery in schizophrenia and call for an increased role of academic scientists in discovering and validating novel drug targets. Indeed, recent breakthroughs in genetic studies of schizophrenia are allowing for the development of hypothesis-driven approaches for discovering possible disease-modifying drugs for schizophrenia. Thus, this is an exciting and pivotal time for the development of truly novel approaches to drug development and treatment of complex disorders like schizophrenia. Molecular Psychiatry (2007) 12, 904–922; doi:10.1038/sj.mp.4002062; published online 31 July 2007 Keywords: antipsychotics; cognition; negative symptoms; drug discovery; preclinical models; target validation Introduction antipsychotic drugs.