Genomic Alterations in Fatal Forms of Non-Anaplastic Thyroid Cancer: Identification Of
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

S1 Supplemental Materials Supplemental Methods Supplemental Figure 1. Immune Phenotype of Mcd19 Targeted CAR T and Dose Titratio
Supplemental Materials Supplemental Methods Supplemental Figure 1. Immune phenotype of mCD19 targeted CAR T and dose titration of in vivo efficacy. Supplemental Figure 2. Gene expression of fluorescent-protein tagged CAR T cells. Supplemental Figure 3. Fluorescent protein tagged CAR T cells function similarly to non-tagged counterparts. Supplemental Figure 4. Transduction efficiency and immune phenotype of mCD19 targeted CAR T cells for survival study (Figure 2D). Supplemental Figure 5. Transduction efficiency and immune phenotype of CAR T cells used in irradiated CAR T study (Fig. 3B-C). Supplemental Figure 6. Differential gene expression of CD4+ m19-humBBz CAR T cells. Supplemental Figure 7. CAR expression and CD4/CD8 subsets of human CD19 targeted CAR T cells for Figure 5E-G. Supplemental Figure 8. Transduction efficiency and immune phenotype of mCD19 targeted wild type (WT) and TRAF1-/- CAR T cells used for in vivo study (Figure 6D). Supplemental Figure 9. Mutated m19-musBBz CAR T cells have increased NF-κB signaling, improved cytokine production, anti-apoptosis, and in vivo function. Supplemental Figure 10. TRAF and CAR co-expression in human CD19-targeted CAR T cells. Supplemental Figure 11. TRAF2 over-expressed h19BBz CAR T cells show similar in vivo efficacy to h19BBz CAR T cells in an aggressive leukemia model. S1 Supplemental Table 1. Probesets increased in m19z and m1928z vs m19-musBBz CAR T cells. Supplemental Table 2. Probesets increased in m19-musBBz vs m19z and m1928z CAR T cells. Supplemental Table 3. Probesets differentially expressed in m19z vs m19-musBBz CAR T cells. Supplemental Table 4. Probesets differentially expressed in m1928z vs m19-musBBz CAR T cells. -

Variation in Protein Coding Genes Identifies Information
bioRxiv preprint doi: https://doi.org/10.1101/679456; this version posted June 21, 2019. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC-ND 4.0 International license. Animal complexity and information flow 1 1 2 3 4 5 Variation in protein coding genes identifies information flow as a contributor to 6 animal complexity 7 8 Jack Dean, Daniela Lopes Cardoso and Colin Sharpe* 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 Institute of Biological and Biomedical Sciences 25 School of Biological Science 26 University of Portsmouth, 27 Portsmouth, UK 28 PO16 7YH 29 30 * Author for correspondence 31 [email protected] 32 33 Orcid numbers: 34 DLC: 0000-0003-2683-1745 35 CS: 0000-0002-5022-0840 36 37 38 39 40 41 42 43 44 45 46 47 48 49 Abstract bioRxiv preprint doi: https://doi.org/10.1101/679456; this version posted June 21, 2019. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC-ND 4.0 International license. Animal complexity and information flow 2 1 Across the metazoans there is a trend towards greater organismal complexity. How 2 complexity is generated, however, is uncertain. Since C.elegans and humans have 3 approximately the same number of genes, the explanation will depend on how genes are 4 used, rather than their absolute number. -

Distinct Gene Expression Patterns in a Tamoxifen-Sensitive Human Mammary Carcinoma Xenograft and Its Tamoxifen-Resistant Subline Maca 3366/TAM
Molecular Cancer Therapeutics 151 Distinct gene expression patterns in a tamoxifen-sensitive human mammary carcinoma xenograft and its tamoxifen-resistant subline MaCa 3366/TAM Michael Becker,1 Anette Sommer,2 of acquired tamoxifen resistance. Finally, genes whose Jo¨rn R. Kra¨tzschmar,2 Henrik Seidel,2 expression profiles are distinctly changed between the Hans-Dieter Pohlenz,2 and Iduna Fichtner1 two xenograft lines will be further evaluated as potential targets for diagnostic or therapeutic approaches of 1 Max-Delbrueck-Center for Molecular Medicine, Experimental tamoxifen-resistant breast cancer. [Mol Cancer Ther Pharmacology, and 2Research Laboratories, Schering AG, Berlin, Germany 2005;4(1):151–68] Abstract Introduction The reasons why human mammary tumors become Breast cancer is the most common type of cancer in women resistant to tamoxifen therapy are mainly unknown. of the Western world. Due to advances in early detection Changes in gene expression may occur as cells acquire and treatment, breast cancer survival rates have increased resistance to antiestrogens. We therefore undertook a com- markedly over the past decades. After surgery, estrogen parative gene expression analysis of tamoxifen-sensitive receptor a (ERa)–positive breast cancer is usually treated and tamoxifen-resistant human breast cancer in vivo with endocrine therapy. Tamoxifen, a nonsteroidal anti- models using Affymetrix oligonucleotide arrays to analyze estrogen, also termed selective estrogen receptor modula- differential gene expression. Total RNAs from the tamox- tor, is the first-line therapy for premenopausal and, until ifen-sensitive patient-derived mammary carcinoma xeno- recently, also for postmenopausal hormone receptor– graft MaCa 3366 and the tamoxifen-resistant model MaCa positive women (1). -

The Orchestra of Lipid-Transfer Proteins at the Crossroads Between Metabolism and Signaling
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Elsevier - Publisher Connector Progress in Lipid Research 61 (2016) 30–39 Contents lists available at ScienceDirect Progress in Lipid Research journal homepage: www.elsevier.com/locate/plipres Review The orchestra of lipid-transfer proteins at the crossroads between metabolism and signaling Antonella Chiapparino a, Kenji Maeda a,1, Denes Turei a,b, Julio Saez-Rodriguez b,2,Anne-ClaudeGavina,c,⁎ a European Molecular Biology Laboratory (EMBL), Structural and Computational Biology Unit, Meyerhofstrasse 1, D-69117 Heidelberg, Germany b European Molecular Biology Laboratory (EMBL), European Bioinformatics Institute (EBI), Cambridge CB10 1SD, UK c European Molecular Biology Laboratory (EMBL), Molecular Medicine Partnership Unit (MMPU), Meyerhofstrasse 1, D-69117 Heidelberg, Germany article info abstract Article history: Within the eukaryotic cell, more than 1000 species of lipids define a series of membranes essential for cell func- Received 29 September 2015 tion. Tightly controlled systems of lipid transport underlie the proper spatiotemporal distribution of membrane Accepted 15 October 2015 lipids, the coordination of spatially separated lipid metabolic pathways, and lipid signaling mediated by soluble Available online 1 December 2015 proteins that may be localized some distance away from membranes. Alongside the well-established vesicular transport of lipids, non-vesicular transport mediated by a group of proteins referred to as lipid-transfer proteins Keywords: (LTPs) is emerging as a key mechanism of lipid transport in a broad range of biological processes. More than a Signaling lipid Biological membranes hundred LTPs exist in humans and these can be divided into at least ten protein families. -

Goat Anti-ORP1 Antibody Peptide-Affinity Purified Goat Antibody Catalog # Af1758a
10320 Camino Santa Fe, Suite G San Diego, CA 92121 Tel: 858.875.1900 Fax: 858.622.0609 Goat Anti-ORP1 Antibody Peptide-affinity purified goat antibody Catalog # AF1758a Specification Goat Anti-ORP1 Antibody - Product Information Application WB Primary Accession Q9BXW6 Other Accession NP_542164, 114876, 64291 (mouse), 259221 (rat) Reactivity Human Predicted Mouse, Rat, Dog, Cow Host Goat Clonality Polyclonal Concentration 100ug/200ul Isotype IgG Calculated MW 108470 AF1758a staining (0.5 µg/ml) of Human Goat Anti-ORP1 Antibody - Additional Information Muscle lysate (RIPA buffer, 35 µg total protein per lane). Primary incubated for 1 hour. Gene ID 114876 Detected by western blot using chemiluminescence. Other Names Oxysterol-binding protein-related protein 1, ORP-1, OSBP-related protein 1, OSBPL1A, Goat Anti-ORP1 Antibody - Background ORP1, OSBP8, OSBPL1, OSBPL1B This gene encodes a member of the Format oxysterol-binding protein (OSBP) family, a 0.5 mg IgG/ml in Tris saline (20mM Tris group of intracellular lipid receptors. Most pH7.3, 150mM NaCl), 0.02% sodium azide, members contain an N-terminal pleckstrin with 0.5% bovine serum albumin homology domain and a highly conserved Storage C-terminal OSBP-like sterol-binding domain, Maintain refrigerated at 2-8°C for up to 6 although some members contain only the months. For long term storage store at sterol-binding domain. Transcript variants -20°C in small aliquots to prevent derived from alternative promoter usage freeze-thaw cycles. and/or alternative splicing exist; they encode different isoforms. Precautions Goat Anti-ORP1 Antibody is for research use Goat Anti-ORP1 Antibody - References only and not for use in diagnostic or therapeutic procedures. -

Genomic Landscape of Paediatric Adrenocortical Tumours
ARTICLE Received 5 Aug 2014 | Accepted 16 Jan 2015 | Published 6 Mar 2015 DOI: 10.1038/ncomms7302 Genomic landscape of paediatric adrenocortical tumours Emilia M. Pinto1,*, Xiang Chen2,*, John Easton2, David Finkelstein2, Zhifa Liu3, Stanley Pounds3, Carlos Rodriguez-Galindo4, Troy C. Lund5, Elaine R. Mardis6,7,8, Richard K. Wilson6,7,9, Kristy Boggs2, Donald Yergeau2, Jinjun Cheng2, Heather L. Mulder2, Jayanthi Manne2, Jesse Jenkins10, Maria J. Mastellaro11, Bonald C. Figueiredo12, Michael A. Dyer13, Alberto Pappo14, Jinghui Zhang2, James R. Downing10, Raul C. Ribeiro14,* & Gerard P. Zambetti1,* Paediatric adrenocortical carcinoma is a rare malignancy with poor prognosis. Here we analyse 37 adrenocortical tumours (ACTs) by whole-genome, whole-exome and/or transcriptome sequencing. Most cases (91%) show loss of heterozygosity (LOH) of chromosome 11p, with uniform selection against the maternal chromosome. IGF2 on chromosome 11p is overexpressed in 100% of the tumours. TP53 mutations and chromosome 17 LOH with selection against wild-type TP53 are observed in 28 ACTs (76%). Chromosomes 11p and 17 undergo copy-neutral LOH early during tumorigenesis, suggesting tumour-driver events. Additional genetic alterations include recurrent somatic mutations in ATRX and CTNNB1 and integration of human herpesvirus-6 in chromosome 11p. A dismal outcome is predicted by concomitant TP53 and ATRX mutations and associated genomic abnormalities, including massive structural variations and frequent background mutations. Collectively, these findings demonstrate the nature, timing and potential prognostic significance of key genetic alterations in paediatric ACT and outline a hypothetical model of paediatric adrenocortical tumorigenesis. 1 Department of Biochemistry, St Jude Children’s Research Hospital, Memphis, Tennessee 38105, USA. 2 Department of Computational Biology and Bioinformatics, St Jude Children’s Research Hospital, Memphis, Tennessee 38105, USA. -
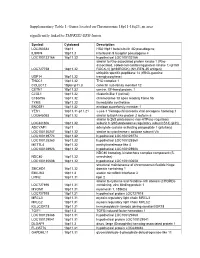
Supplementary Table 1: Genes Located on Chromosome 18P11-18Q23, an Area Significantly Linked to TMPRSS2-ERG Fusion
Supplementary Table 1: Genes located on Chromosome 18p11-18q23, an area significantly linked to TMPRSS2-ERG fusion Symbol Cytoband Description LOC260334 18p11 HSA18p11 beta-tubulin 4Q pseudogene IL9RP4 18p11.3 interleukin 9 receptor pseudogene 4 LOC100132166 18p11.32 hypothetical LOC100132166 similar to Rho-associated protein kinase 1 (Rho- associated, coiled-coil-containing protein kinase 1) (p160 LOC727758 18p11.32 ROCK-1) (p160ROCK) (NY-REN-35 antigen) ubiquitin specific peptidase 14 (tRNA-guanine USP14 18p11.32 transglycosylase) THOC1 18p11.32 THO complex 1 COLEC12 18pter-p11.3 collectin sub-family member 12 CETN1 18p11.32 centrin, EF-hand protein, 1 CLUL1 18p11.32 clusterin-like 1 (retinal) C18orf56 18p11.32 chromosome 18 open reading frame 56 TYMS 18p11.32 thymidylate synthetase ENOSF1 18p11.32 enolase superfamily member 1 YES1 18p11.31-p11.21 v-yes-1 Yamaguchi sarcoma viral oncogene homolog 1 LOC645053 18p11.32 similar to BolA-like protein 2 isoform a similar to 26S proteasome non-ATPase regulatory LOC441806 18p11.32 subunit 8 (26S proteasome regulatory subunit S14) (p31) ADCYAP1 18p11 adenylate cyclase activating polypeptide 1 (pituitary) LOC100130247 18p11.32 similar to cytochrome c oxidase subunit VIc LOC100129774 18p11.32 hypothetical LOC100129774 LOC100128360 18p11.32 hypothetical LOC100128360 METTL4 18p11.32 methyltransferase like 4 LOC100128926 18p11.32 hypothetical LOC100128926 NDC80 homolog, kinetochore complex component (S. NDC80 18p11.32 cerevisiae) LOC100130608 18p11.32 hypothetical LOC100130608 structural maintenance -
Imbalanced Mitochondrial Function Provokes Heterotaxy Via Aberrant Ciliogenesis
Imbalanced mitochondrial function provokes heterotaxy via aberrant ciliogenesis Martin D. Burkhalter, … , Stephanie M. Ware, Melanie Philipp J Clin Invest. 2019;129(7):2841-2855. https://doi.org/10.1172/JCI98890. Research Article Cardiology Development Graphical abstract Find the latest version: https://jci.me/98890/pdf The Journal of Clinical Investigation RESEARCH ARTICLE Imbalanced mitochondrial function provokes heterotaxy via aberrant ciliogenesis Martin D. Burkhalter,1,2 Arthi Sridhar,3 Pedro Sampaio,4 Raquel Jacinto,4 Martina S. Burczyk,2 Cornelia Donow,2 Max Angenendt,2 Competence Network for Congenital Heart Defects Investigators,5 Maja Hempel,6 Paul Walther,7 Petra Pennekamp,8 Heymut Omran,8 Susana S. Lopes,4 Stephanie M. Ware,3 and Melanie Philipp1,2 1 Department of Experimental and Clinical Pharmacology and Pharmacogenomics, University of Tübingen, Tübingen, Germany. 2Institute of Biochemistry and Molecular Biology, Ulm University, Ulm, Germany. 3Department of Pediatrics, Indiana University School of Medicine, Indianapolis, Indiana, USA. 4CEDOC Chronic Diseases Research Center, NOVA Medical School, Faculdade de Ciências Médicas, Universidade Nova de Lisboa, Lisboa, Portugal. 5Competence Network for Congenital Heart Defects, National Register for Congenital Heart Defects, Deutsches Zentrum für Herz-Kreislaufforschung (DZHK), Berlin, Germany. 6Institute of Human Genetics, University Medical Center Hamburg-Eppendorf, Hamburg, Germany. 7Central Facility for Electron Microscopy, Ulm University, Ulm, Germany. 8Department of General Pediatrics, University Hospital Muenster, Muenster, Germany. About 1% of all newborns are affected by congenital heart disease (CHD). Recent findings identify aberrantly functioning cilia as a possible source for CHD. Faulty cilia also prevent the development of proper left-right asymmetry and cause heterotaxy, the incorrect placement of visceral organs. -

Gnomad Lof Supplement
1 gnomAD supplement gnomAD supplement 1 Data processing 4 Alignment and read processing 4 Variant Calling 4 Coverage information 5 Data processing 5 Sample QC 7 Hard filters 7 Supplementary Table 1 | Sample counts before and after hard and release filters 8 Supplementary Table 2 | Counts by data type and hard filter 9 Platform imputation for exomes 9 Supplementary Table 3 | Exome platform assignments 10 Supplementary Table 4 | Confusion matrix for exome samples with Known platform labels 11 Relatedness filters 11 Supplementary Table 5 | Pair counts by degree of relatedness 12 Supplementary Table 6 | Sample counts by relatedness status 13 Population and subpopulation inference 13 Supplementary Figure 1 | Continental ancestry principal components. 14 Supplementary Table 7 | Population and subpopulation counts 16 Population- and platform-specific filters 16 Supplementary Table 8 | Summary of outliers per population and platform grouping 17 Finalizing samples in the gnomAD v2.1 release 18 Supplementary Table 9 | Sample counts by filtering stage 18 Supplementary Table 10 | Sample counts for genomes and exomes in gnomAD subsets 19 Variant QC 20 Hard filters 20 Random Forest model 20 Features 21 Supplementary Table 11 | Features used in final random forest model 21 Training 22 Supplementary Table 12 | Random forest training examples 22 Evaluation and threshold selection 22 Final variant counts 24 Supplementary Table 13 | Variant counts by filtering status 25 Comparison of whole-exome and whole-genome coverage in coding regions 25 Variant annotation 30 Frequency and context annotation 30 2 Functional annotation 31 Supplementary Table 14 | Variants observed by category in 125,748 exomes 32 Supplementary Figure 5 | Percent observed by methylation. -

PCV2 Aggravated SS2 Infection Directly Showed from Differentially 2 Expressed Proteome of PK15 Cells
bioRxiv preprint doi: https://doi.org/10.1101/2020.02.24.962738; this version posted February 26, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-NC-ND 4.0 International license. 1 TITLE: PCV2 aggravated SS2 infection directly showed from differentially 2 expressed proteome of PK15 cells. 3 Tan Jimin1,2, Xiao Qi2,3,4, Li Xingguang5, Fan Hongjie1*, He Kongwang2,3,4* 4 5 6 1College of Veterinary Medicine, Nanjing Agricultural University, Nanjing, China 7 2Jiangsu Key Laboratory for Food Quality and Safety-State Key Laboratory Cultivation 8 Base Ministry of Science and Technology, Nanjing, China 9 3Institute of Veterinary Medicine, Jiangsu Academy of Agricultural Sciences-Key 10 Laboratory of Veterinary Biological Engineering and Technology, Ministry of 11 Agriculture and Rural Affairs, Nanjing, China 12 4Jiangsu Co-Innovation Center for the Prevention and Control of Important Animal 13 Infectious Disease and Zoonose, Yangzhou University, Yangzhou, China 14 5Hubei Engineering Research Center of Viral Vector, Wuhan University of 15 Bioengineering, Wuhan 430415, China. 16 Correspondence: 17 Fan Hongjie ([email protected]) 18 He Kongwang ([email protected]) 19 20 21 Running title: PCV2 and SS2 co-infection proteomic study of Porcine Kidney cell 15 22 23 bioRxiv preprint doi: https://doi.org/10.1101/2020.02.24.962738; this version posted February 26, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. -
Rab Proteins and the Compartmentalization of the Endosomal System
Downloaded from http://cshperspectives.cshlp.org/ on September 27, 2021 - Published by Cold Spring Harbor Laboratory Press Rab Proteins and the Compartmentalization of the Endosomal System Angela Wandinger-Ness1 and Marino Zerial2 1Department of Pathology MSC08 4640, University of New Mexico HSC, Albuquerque, New Mexico 87131 2Max Planck Institute of Molecular and Cell Biology and Genetics, 01307 Dresden, Germany Correspondence: [email protected]; [email protected] Of the approximately 70 human Rab GTPases, nearly three-quarters are involved in endo- cytic trafficking. Significant plasticity in endosomal membrane transport pathways is closely coupled to receptor signaling and Rab GTPase-regulated scaffolds. Here we review current literature pertaining to endocytic Rab GTPaselocalizations, functions, and coordination with regulatory proteins and effectors. The roles of Rab GTPasesin (1) compartmentalization of the endocytic pathway into early, recycling, late, and lysosomal routes; (2) coordination of individual transport steps from vesicle budding to fusion; (3) effector interactomes; and (4) integration of GTPase and signaling cascades are discussed. he general working principle of Rab coded by interacting proteins (Wittinghofer TGTPases is that they contribute to the struc- et al. 1993). Guanine-nucleotide exchange fac- tural and functional identity of intracellular or- tors (GEFs) and GTPase-activating proteins ganelles. These functions rely on the versatile (GAPs) catalyze the exchange and hydrolysis GTP/GDP cycle for the assembly of multipro- reactions and, therefore, act as regulators of tein machineries on the cytoplasmic surface of the GTP–GDP cycle (Yoshimura et al. 2010; intracellular membranes. Rab GTPase protein Wu et al. 2011; Barr 2013; Guo et al. 2013; Kot- assemblies are spatially and temporally regulat- ting and Gerwert 2013). -

PRODUCT SPECIFICATION Product Datasheet
Product Datasheet QPrEST PRODUCT SPECIFICATION Product Name QPrEST OSBL1 Mass Spectrometry Protein Standard Product Number QPrEST35597 Protein Name Oxysterol-binding protein-related protein 1 Uniprot ID Q9BXW6 Gene OSBPL1A Product Description Stable isotope-labeled standard for absolute protein quantification of Oxysterol-binding protein-related protein 1. Lys (13C and 15N) and Arg (13C and 15N) metabolically labeled recombinant human protein fragment. Application Absolute protein quantification using mass spectrometry Sequence (excluding VPKNSLQQSREDWLEAIEEHSAYSTHYCSQDQLTDEEEEDTVSAADLKKS fusion tag) LEKAQSCQQRLDREISNFLKMIKECDMAKEMLPSFLQKVEVVSEA Theoretical MW 28807 Da including N-terminal His6ABP fusion tag Fusion Tag A purification and quantification tag (QTag) consisting of a hexahistidine sequence followed by an Albumin Binding Protein (ABP) domain derived from Streptococcal Protein G. Expression Host Escherichia coli LysA ArgA BL21(DE3) Purification IMAC purification Purity >90% as determined by Bioanalyzer Protein 230 Purity Assay Isotopic Incorporation >99% Concentration >5 μM after reconstitution in 100 μl H20 Concentration Concentration determined by LC-MS/MS using a highly pure amino acid analyzed internal Determination reference (QTag), CV ≤10%. Amount >0.5 nmol per vial, two vials supplied. Formulation Lyophilized in 100 mM Tris-HCl 5% Trehalose, pH 8.0 Instructions for Spin vial before opening. Add 100 μL ultrapure H2O to the vial. Vortex thoroughly and spin Reconstitution down. For further dilution, see Application Protocol. Shipping Shipped at ambient temperature Storage Lyophilized product shall be stored at -20°C. See COA for expiry date. Reconstituted product can be stored at -20°C for up to 4 weeks. Avoid repeated freeze-thaw cycles. Notes For research use only Product of Sweden. For research use only. Not intended for pharmaceutical development, diagnostic, therapeutic or any in vivo use.