Management of Vith Nerve Palsy-Avoiding Unnecessary Surgery
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Management of Microtropia
Br J Ophthalmol: first published as 10.1136/bjo.58.3.281 on 1 March 1974. Downloaded from Brit. J. Ophthal. (I974) 58, 28 I Management of microtropia J. LANG Zirich, Switzerland Microtropia or microstrabismus may be briefly described as a manifest strabismus of less than 50 with harmonious anomalous correspondence. Three forms can be distinguished: primary constant, primary decompensating, and secondary. There are three situations in which the ophthalmologist may be confronted with micro- tropia: (i) Amblyopia without strabismus; (2) Hereditary and familial strabismus; (3) Residual strabismus after surgery. This may be called secondary microtropia, for everyone will admit that in most cases of convergent strabismus perfect parallelism and bifoveal fixation are not achieved even after expert treatment. Microtropia and similar conditions were not mentioned by such well-known early copyright. practitioners as Javal, Worth, Duane, and Bielschowsky. The views of Maddox (i898), that very small angles were extremely rare, and that the natural tendency to fusion was much too strong to allow small angles to exist, appear to be typical. The first to mention small residual angles was Pugh (I936), who wrote: "A patient with monocular squint who has been trained to have equal vision in each eye and full stereoscopic vision with good amplitude of fusion may in 3 months relapse into a slight deviation http://bjo.bmj.com/ in the weaker eye and the vision retrogresses". Similar observations of small residual angles have been made by Swan, Kirschberg, Jampolsky, Gittoes-Davis, Cashell, Lyle, Broadman, and Gortz. There has been much discussion in both the British Orthoptic Journal and the American Orthoptic journal on the cause of this condition and ways of avoiding it. -
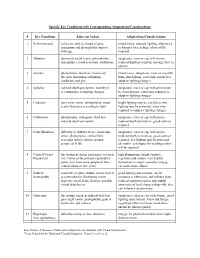
Specific Eye Conditions with Corresponding Adaptations/Considerations
Specific Eye Conditions with Corresponding Adaptations/Considerations # Eye Condition Effect on Vision Adaptations/Considerations 1 Achromotopsia colors are seen as shades of grey, tinted lenses, reduced lighting, alternative nystagmus and photophobia improve techniques for teaching colors will be with age required 2 Albinism decreased visual acuity, photophobia, sunglasses, visor or cap with a brim, nystagmus, central scotomas, strabismus reduced depth perception, moving close to objects 3 Aniridia photophobia, field loss, vision may tinted lenses, sunglasses, visor or cap with fluctuate depending on lighting brim, dim lighting, extra time required to conditions and glare adapt to lighting changes 4 Aphakia reduced depth perception, inability to sunglasses, visor or cap with a brim may accommodate to lighting changes be worn indoors, extra time required to adapt to lighting changes 5 Cataracts poor color vision, photophobia, visual bright lighting may be a problem, low acuity fluctuates according to light lighting may be preferred, extra time required to adapt to lighting changes 6 Colobomas photophobia, nystagmus, field loss, sunglasses, visor or cap with a brim, reduced depth perception reduced depth perception, good contrast required 7 Color Blindness difficulty or inability to see colors and sunglasses, visor or cap with a brim, detail, photophobia, central field reduced depth perception, good contrast scotomas (spotty vision), normal required, low lighting may be preferred, peripheral fields alternative techniques for teaching colors -

A Patient & Parent Guide to Strabismus Surgery
A Patient & Parent Guide to Strabismus Surgery By George R. Beauchamp, M.D. Paul R. Mitchell, M.D. Table of Contents: Part I: Background Information 1. Basic Anatomy and Functions of the Extra-ocular Muscles 2. What is Strabismus? 3. What Causes Strabismus? 4. What are the Signs and Symptoms of Strabismus? 5. Why is Strabismus Surgery Performed? Part II: Making a Decision 6. What are the Options in Strabismus Treatment? 7. The Preoperative Consultation 8. Choosing Your Surgeon 9. Risks, Benefits, Limitations and Alternatives to Surgery 10. How is Strabismus Surgery Performed? 11. Timing of Surgery Part III: What to Expect Around the Time of Surgery 12. Before Surgery 13. During Surgery 14. After Surgery 15. What are the Potential Complications? 16. Myths About Strabismus Surgery Part IV: Additional Matters to Consider 17. About Children and Strabismus Surgery 18. About Adults and Strabismus Surgery 19. Why if May be Important to a Person to Have Strabismus Surgery (and How Much) Part V: A Parent’s Perspective on Strabismus Surgery 20. My Son’s Diagnosis and Treatment 21. Growing Up with Strabismus 22. Increasing Signs that Surgery Was Needed 23. Making the Decision to Proceed with Surgery 24. Explaining Eye Surgery to My Son 25. After Surgery Appendix Part I: Background Information Chapter 1: Basic Anatomy and Actions of the Extra-ocular Muscles The muscles that move the eye are called the extra-ocular muscles. There are six of them on each eye. They work together in pairs—complementary (or yoke) muscles pulling the eyes in the same direction(s), and opposites (or antagonists) pulling the eyes in opposite directions. -

Hyperopia Hyperopia
Hyperopia Hyperopia hyperopia hyperopia • Farsightedness, or hyperopia, • Farsightedness occurs if your eyeball is too as it is medically termed, is a short or the cornea has too little curvature, so vision condition in which distant objects are usually light entering your eye is not focused correctly. seen clearly, but close ones do • Its effect varies greatly, depending on the not come into proper focus. magnitude of hyperopia, the age of the individual, • Approximately 25% of the the status of the accommodative and general population is hyperopic (a person having hyperopia). convergence system, and the demands placed on the visual system. By Judith Lee and Gretchyn Bailey; reviewed by Dr. Vance Thompson; Flash illustration by Stephen Bagi 1. Cornea is too flap. hyperopia • In theory, hyperopia is the inability to focus and see the close objects clearly, but in practice many young hyperopics can compensate the weakness of their focusing ability by excessive use of the accommodation functions of their eyes. Hyperopia is a refractive error in • But older hyperopics are not as lucky as them. By which parallel rays of light aging, accommodation range diminishes and for 2. Axial is too short. entering the eye reach a focal older hyperopics seeing close objects becomes point behind the plane of the retina, while accommodation an impossible mission. is maintained in a state of relaxation. 1 Amplitude of Accommodation hyperopia Maximum Amplitude= 25-0.4(age) • An emmetropic eye for reading and other near Probable Amplitude= 18.5-.3(age) work, at distance of 16 in (40cm), the required amount of acc. -

Complex Strabismus and Syndromes
Complex Strabismus & Syndromes Some patients exhibit complex combinations of vertical, horizontal, and torsional strabismus. Dr. Shin treats patients with complex strabismus arising from, but not limited to, thyroid-related eye disease, stroke, or brain tumors as well as strabismic disorders following severe orbital and head trauma. The following paragraphs describe specific ocular conditions marked by complex strabismus. Duane Syndrome Duane syndrome represents a constellation of eye findings present at birth that results from an absent 6th cranial nerve nucleus and an aberrant branch of the 3rd cranial nerve that innervates the lateral rectus muscle. Duane syndrome most commonly affects the left eye of otherwise healthy females. Duane syndrome includes several variants of eye movement abnormalities. In the most common variant, Type I, the eye is unable to turn outward to varying degrees from the normal straight ahead position. In addition, when the patient tries to look straight ahead, the eyes may cross. This may lead a person with Duane syndrome to turn his/her head toward one side while viewing objects in front of them in order to better align the eyes. When the involved eye moves toward the nose, the eye retracts slightly back into the eye socket causing a narrowing of the opening between the eyelids. In Type II, the affected eye possesses limited ability to turn inward and is generally outwardly turning. In Type III, the eye has limited inward and outward movement. All three types are characterized by anomalous co-contraction of the medial and lateral rectus muscles, so when the involved eye moves towards the nose, the globe pulls back into the orbit and the vertical space between the eyelids narrows. -

Surgical Options in Managing Convergent Strabismus Fixus Related to High Myopia
Ophthalmol Ina 2015;41(2):107-115 107 Case Report Surgical Options in Managing Convergent Strabismus Fixus Related to High Myopia Jessica Zarwan, Gusti G Suardana, Anna P Bani Department of Ophthalmology, Faculty of Medicine, Indonesia University Cipto Mangunkusumo Hospital, Jakarta ABSTRACT Background: Convergent strabismus fixus is a condition in which one or both eyes are anchored in extreme adduction. This condition is caused by superotemporal herniation of the enlarged globe from the muscle cone through the space between the superior and lateral rectus muscle. It is commonly related to high myopia. Recently, transposition type procedure which unite the superior and lateral rectus muscles were proposed as the treatment of choice in this condition. However, there is no clear consensus regarding the best surgical procedure in convergent strabismus fixus. This case series reported three rare cases of convergent strabismus fixus related to high myopia and highlight the option of surgical procedure that can be done in these cases. Case Illustration: Three patients presented with convergent strabismus fixus of both eyes with history of bilateral high myopia since childhood. All patients showed Krimsky tests of >95∆ET preoperatively, with medial displacement of superior rectus and inferior displacement of lateral rectus of both eyes in all patients on orbital imaging. The bilateral Yokoma procedure both resulted in an orthophoric postoperative result with marked improvement in abduction and elevation. The hemi-Jensen also showed a significant improvement of over than 60∆ on the operated eye, resorting it to a central position during primary gaze. Conclusion: Convergent strabismus fixus is a rare condition and frequently associated with high myopia. -

Strabismus, Amblyopia & Leukocoria
Strabismus, Amblyopia & Leukocoria [ Color index: Important | Notes: F1, F2 | Extra ] EDITING FILE Objectives: ➢ Not given. Done by: Jwaher Alharbi, Farrah Mendoza. Revised by: Rawan Aldhuwayhi Resources: Slides + Notes + 434 team. NOTE: F1& F2 doctors are different, the doctor who gave F2 said she is in the exam committee so focus on her notes Amblyopia ● Definition Decrease in visual acuity of one eye without the presence of an organic cause that explains that decrease in visual acuity. He never complaints of anything and his family never noticed any abnormalities ● Incidence The most common cause of visual loss under 20 years of life (2-4% of the general population) ● How? Cortical ignorance of one eye. This will end up having a lazy eye ● binocular vision It is achieved by the use of the two eyes together so that separate and slightly dissimilar images arising in each eye are appreciated as a single image by the process of fusion. It’s importance 1. Stereopsis 2. Larger field If there is no coordination between the two eyes the person will have double vision and confusion so as a compensatory mechanism for double vision the brain will cause suppression. The visual pathway is a plastic system that continues to develop during childhood until around 6-9 years of age. During this time, the wiring between the retina and visual cortex is still developing. Any visual problem during this critical period, such as a refractive error or strabismus can mess up this developmental wiring, resulting in permanent visual loss that can't be fixed by any corrective means when they are older Why fusion may fail ? 1. -

Sixth Nerve Palsy
COMPREHENSIVE OPHTHALMOLOGY UPDATE VOLUME 7, NUMBER 5 SEPTEMBER-OCTOBER 2006 CLINICAL PRACTICE Sixth Nerve Palsy THOMAS J. O’DONNELL, MD, AND EDWARD G. BUCKLEY, MD Abstract. The diagnosis and etiologies of sixth cranial nerve palsies are reviewed along with non- surgical and surgical treatment approaches. Surgical options depend on the function of the paretic muscle, the field of greatest symptoms, and the likelihood of inducing diplopia in additional fields by a given procedure. (Comp Ophthalmol Update 7: xx-xx, 2006) Key words. botulinum toxin (Botox®) • etiology • sixth nerve palsy (paresis) Introduction of the cases, the patients had hypertension and/or, less frequently, Sixth cranial nerve (abducens) palsy diabetes; 26% were undetermined, is a common cause of acquired 5% had a neoplasm, and 2% had an horizontal diplopia. Signs pointing aneurysm. It was noted that patients toward the diagnosis are an who had an aneurysm or neoplasm abduction deficit and an esotropia had additional neurologic signs or increasing with gaze toward the side symptoms or were known to have a of the deficit (Figure 1). The diplopia cancer.2 is typically worse at distance. Measurements are made with the Anatomical Considerations uninvolved eye fixing (primary deviation), and will be larger with the The sixth cranial nerve nuclei are involved eye fixing (secondary located in the lower pons beneath the deviation). A small vertical deficit may fourth ventricle. The nerve on each accompany a sixth nerve palsy, but a side exits from the ventral surface of deviation over 4 prism diopters the pons. It passes from the posterior Dr. O’Donnell is affiliated with the should raise the question of cranial fossa to the middle cranial University of Tennessee Health Sci- additional pathology, such as a fourth fossa, ascends the clivus, and passes ence Center, Memphis, TN. -

Iris Mammillations: Significance and Associations
IRIS MAMMILLATIONS: SIGNIFICANCE AND ASSOCIATIONS 2 l NICOLA K. RAGGEL2, 1. ACHESON and A. LINN MURPHREE Los Angeles and London SUMMARY mammiform (nipple- or teat-like) protuberances. Iris mammillations are rarely described, distinctive Iris mammillations are an occasional finding with few previous reports. They are most commonly villiform protuberances that can cover the iris. In the l--6 majority of reported cases they are unilateral and found in association with melanosis oculi, with or sporadic, and are seen in association with oculodermal without periocular skin involvement in a naevus of melanosis. In past literature and current clinical Ota. They are thus often less precisely referred to as practice they are frequently confused with tbe iris iris melanosis, a term which should best be reserved nodules seen in neurofibromatosis type 1. Their clinical for increased pigmentation of the iris, irrespective of significance is not established, although it has been the presence of iris elevations overlying the pigmen 7 suggested that iris mammillations may be an external ted areas. This is supported by the rare descriptions sign of ocular hypertension or intraocular malignancy. of iris elevations in the absence of any increased iris We report a series of 9 patients between the ages of 3 pigmentation?,8 and 28 years with iris mammillations. The mammilla Iris mammillations are usually unilateral, often tions appear as regularly spaced, deep brown, smooth, presenting as heterochromia iridis. Occasional bilat 7 conical elevations on the iris, of uniform height or eral cases have been described. ,8 Iris mammillations increasing in height as the pupil margin is approached. -

A Review of Neuro-Ophthalmologic Emergencies Type of Article: Review
A Review of Neuro-ophthalmologic Emergencies Type of Article: Review Bassey Fiebai Department of Ophthalmology, University of Port Harcourt Teaching Hospital, Port Harcourt, Nigeria The emphasis of this review are the emergencies where ABSTRACT failure to recognize the early stages of these diseases result Background 2,3,4 in adverse prognosis . These emergencies can be grouped Neuro-ophthalmic emergencies are relatively uncommon, 1 into four major categories for ease of diagnosis (Table 1) . however their outcome cause severe morbidity and even The first 3 groups are based on initial symptoms and the last mortality. The ocular manifestations of these disorders are group accommodates other disease conditions that pointers to a more dangerous central nervous system or constitute a neuro-ophthalmic emergency but do not systemic pathology. The review aims to highlight the major strictly fall under the other 3 groups. The review aims to ocular disorders that constitute neuro-ophthalmologic highlight the major ocular disorders that constitute neuro- emergencies with a view to increasing the index of ophthalmologic emergencies with a view to increasing the suspicion of these visual/life threatening disorders among index of suspicion of these visual/life threatening primary care physicians, neurologists and disorders among primary care physicians, neurologists and ophthalmologists. ophthalmologists by providing relevant information on the clinical presentation and management of these Method emergencies. The available literature on neuro-ophthalmologic -

Suppression and Retinal Correspondence in Intermittent Exotropia
Downloaded from bjo.bmj.com on May 23, 2012 - Published by group.bmj.com British Journal of Ophthalmology, 1986, 70, 673-676 Suppression and retinal correspondence in intermittent exotropia JEFFREY COOPER AND CAROL DIBBLE RECORD From the Institute of Vision Research, SUNYIState College of Optometry, 100 East 24th Street, New York, New York 10010, USA SUMMARY Suppression scotomas and retinal projection (retinal correspondence) were measured in six intermittent exotropes during deviation. Measurements used red-green anaglyph stimuli presented on a black background which could be varied from 3-4 minutes of arc to 3024'. Results showed non-suppression of all points between the fovea and the diplopia point. Harmonious anomalous retinal correspondence was usually observed. Two subjects had spontaneous changes from anomalous retinal correspondence to normal retinal correspondence without a concurrent change in ocular position. Conventional testing resulted in more variable results in regard to retinal correspondence and suppression, suggesting that non-suppression and anomalous retinal corres- pondence occur when black backgrounds are used for testing. Patients with intermittent exotropia of the diverg- image and anomalous retinal correspondence (ARC) ence excess type (DE) or basic exotropia usually do in the deviated position and normal retinal corres- not complain of diplopia when their eyes are deviat- pondence (NRC) in the aligned position on the ing.' Parks2 believes that the absence of diplopia is Hering-Bielschowsky afterimage test.' due to a dense temporal hemiretinal suppression. We therefore attempted to qualify the depth of Using a technique employing Risley prisms, suppression in deviating intermittent exotropes while Jampolsky3 demonstrated that DE patients have a monitoring ocular position. -

Sixth Nerve Palsy
Sixth Nerve Palsy WHAT IS CRANIAL NERVE VI PALSY? Sixth cranial nerve palsy is weakness of the nerve that innervates the lateral rectus muscle. The lateral rectus muscle rotates the eye away from the nose and when the lateral rectus muscle is weak, the eye crosses inward toward the nose (esotropia). The esotropia is larger when looking at a distant target and looking to same side as the affected lateral rectus muscle. WHAT CAUSES CRANIAL NERVE VI PALSY? The most common causes of sixth cranial nerve palsy are stroke, trauma, viral illness, brain tumor, inflammation, infection, migraine headache and elevated pressure inside the brain. The condition can be present at birth; however, the most common cause in children is trauma. In older persons, a small stroke is the most common cause. Sometimes the cause of the palsy is never determined despite extensive investigation. The sixth cranial nerve has a long course from the brainstem to the lateral rectus muscle and depending on the location of the abnormality, other neurologic structures may be involved. Hearing loss, facial weakness, decreased facial sensation, droopy eyelid and/or abnormal eye movement can be associated, depending on the location of the lesion. DOES SIXTH CRANIAL NERVE PALSY IMPROVE WITH TIME? It is possible for palsies to resolve with time, and the amount of resolution primarily depends on the underlying cause. Palsy caused by viral illness generally resolves completely; whereas palsy caused by trauma is typically associated with incomplete resolution. Maximum improvement usually occurs during the first six months after onset. WHAT ARE THE SYMPTOMS OF SIXTH NERVE PALSY? Double vision (2 images seen side by side) is the most common symptom.