A Patient & Parent Guide to Strabismus Surgery
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
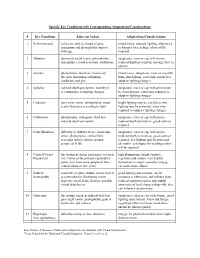
Specific Eye Conditions with Corresponding Adaptations/Considerations
Specific Eye Conditions with Corresponding Adaptations/Considerations # Eye Condition Effect on Vision Adaptations/Considerations 1 Achromotopsia colors are seen as shades of grey, tinted lenses, reduced lighting, alternative nystagmus and photophobia improve techniques for teaching colors will be with age required 2 Albinism decreased visual acuity, photophobia, sunglasses, visor or cap with a brim, nystagmus, central scotomas, strabismus reduced depth perception, moving close to objects 3 Aniridia photophobia, field loss, vision may tinted lenses, sunglasses, visor or cap with fluctuate depending on lighting brim, dim lighting, extra time required to conditions and glare adapt to lighting changes 4 Aphakia reduced depth perception, inability to sunglasses, visor or cap with a brim may accommodate to lighting changes be worn indoors, extra time required to adapt to lighting changes 5 Cataracts poor color vision, photophobia, visual bright lighting may be a problem, low acuity fluctuates according to light lighting may be preferred, extra time required to adapt to lighting changes 6 Colobomas photophobia, nystagmus, field loss, sunglasses, visor or cap with a brim, reduced depth perception reduced depth perception, good contrast required 7 Color Blindness difficulty or inability to see colors and sunglasses, visor or cap with a brim, detail, photophobia, central field reduced depth perception, good contrast scotomas (spotty vision), normal required, low lighting may be preferred, peripheral fields alternative techniques for teaching colors -

Answer Set Companion Answers to Questions
Case Based Pediatrics For Medical Students and Residents Questions and Answers Editors: Loren G. Yamamoto, MD, MPH, MBA Alson S. Inaba, MD Jeffrey K. Okamoto, MD Mary Elaine Patrinos, MD Vince K. Yamashiroya, MD Department of Pediatrics University of Hawaii John A. Burns School of Medicine Kapiolani Medical Center For Women And Children Honolulu, Hawaii Copyright 2004, Loren G. Yamamoto Department of Pediatrics, University of Hawaii John A. Burns School of Medicine Answer Set Companion Answers to Questions Section I. Office Primary Care Chapter I.1. Pediatric Primary Care 1. False. Proximity to the patient is also an important factor. A general surgeon practicing in a small town might be the best person to handle a suspected case of appendicitis, for example. 2. False. Although some third party payors have standards written into their contracts with physicians, and the American Academy of Pediatrics has created a standard, not all pediatricians adhere to these standards. 3. True. Many factors are involved, including the training of the primary care pediatrician and past experience with similar cases. 4.d 5.e Chapter I.2. Growth Monitoring 1. BMI (kg/m 2) = weight in kilograms divided by the square of the height in meters. 2. First 18 months of life. 3. a) If the child's weight is below the 5th percentile, or b) if weight drops more than two major percentile lines. 4. 85th percentile. 5. 30 grams, or 1 oz per day. 6. At 5 years of age. Those who rebound before 5 years have a higher risk of obesity in childhood and adulthood. -

Strabismus Surgery Kenneth W
11 Strabismus Surgery Kenneth W. Wright and Pauline Hong his chapter discusses various strabismus surgery procedures Tand how they work. When a muscle contracts, it produces a force that rotates the globe. The rotational force that moves an eye is directly proportional to the length of the moment arm (m) (Fig. 11-1A) and the force of the muscle contraction (F) (Fig. 11-1B). Rotational force ϭ m ϫ F where m ϭ moment arm and F ϭ muscle force. Strabismus surgery corrects ocular misalignment by at least four different mechanisms: slackening a muscle (i.e., recession), tightening a muscle (i.e., resection or plication), reducing the length of the moment arm (i.e., Faden), or changing the vector of the muscle force by moving the muscle’s insertion site (i.e., transposition). MUSCLE RECESSION A muscle recession moves the muscle insertion closer to the muscle’s origin (Fig. 11-2), creating muscle slack. This muscle slack reduces muscle strength per Starling’s length–tension curve but does not significantly change the moment arm when the eye is in primary position (Fig. 11-3). The arc of contact of the rectus muscles wrapping around the globe to insert anterior to the equator of the eye allows for large recessions of the rectus muscles without significantly changing the moment arm. Figure 11-3 shows a 7.0-mm recession of the medial and lateral rectus muscles. Note there is no change in the moment arm with these large recessions. Thus, the effect of a recession on eye position is determined by the amount of muscle slack created.1a The 388 chapter 11: strabismus surgery 389 FIGURE 11-1A,B. -

EPOS 2021 Vision 2020 - EPOS 2021
EPOS 2021 Vision 2020 - EPOS 2021 Final programme & Abstract book EPOS 2021 Virtual Conference 18 - 19 June 2021 www.epos2021.dk EPOS 2021 Vision 2020 - EPOS 2021 2 Contents Final programme . 3 Invited speaker abstracts . 5 Free paper presentations . 33 Rapid fire presentations . 60 Poster presentations . 70 Local organizing Committee: Conference chair: Lotte Welinder Dept. of Ophthalmology, Aalborg University Hospital Members: Dorte Ancher Larsen Dept. of Ophthalmology, Aarhus University Hospital Else Gade Dept. of Ophthalmology, University Hospital Odense Lisbeth Sandfeld Dept. of Ophthalmology, Zealand University Hospital, Roskilde Kamilla Rothe Nissen Dept. of Ophthalmology, Rigshospitalet, University Hospital of Copenhagen Line Kessel Dept. of Ophthalmology, Rigshospitalet (Glostrup), University Hospital of Copenhagen Helena Buch Heesgaard Copenhagen Eye and Strabismus Clinic, CFR Hospitals EPOS Board Members: Darius Hildebrand President Eva Larsson Secretary Christina Gehrt-Kahlert Treasurer Catherine Cassiman Anne Cees Houtman Matthieu Robert Sandra Valeina EPOS 2021 Programme 3 Friday 18 June 8.50-9.00 Opening, welcome remarks 9.00-10.15 Around ROP and prematurity - Part 1 Moderators: Eva Larsson (SE) and Lotte Welinder (DK) 9.00-9.10 L1 Visual impairment. National Danish Registry of visual Kamilla Rothe Nissen (DK) impairment and blindness? 9.10-9.20 L2 Epidemiology of ROP Gerd Holmström (SE) 9.20-9.40 L3 The premature child. Ethical issues in neonatal care Gorm Greisen (DK) 9.40-9.50 L4 Ocular development and visual functioning -

Hyperopia Hyperopia
Hyperopia Hyperopia hyperopia hyperopia • Farsightedness, or hyperopia, • Farsightedness occurs if your eyeball is too as it is medically termed, is a short or the cornea has too little curvature, so vision condition in which distant objects are usually light entering your eye is not focused correctly. seen clearly, but close ones do • Its effect varies greatly, depending on the not come into proper focus. magnitude of hyperopia, the age of the individual, • Approximately 25% of the the status of the accommodative and general population is hyperopic (a person having hyperopia). convergence system, and the demands placed on the visual system. By Judith Lee and Gretchyn Bailey; reviewed by Dr. Vance Thompson; Flash illustration by Stephen Bagi 1. Cornea is too flap. hyperopia • In theory, hyperopia is the inability to focus and see the close objects clearly, but in practice many young hyperopics can compensate the weakness of their focusing ability by excessive use of the accommodation functions of their eyes. Hyperopia is a refractive error in • But older hyperopics are not as lucky as them. By which parallel rays of light aging, accommodation range diminishes and for 2. Axial is too short. entering the eye reach a focal older hyperopics seeing close objects becomes point behind the plane of the retina, while accommodation an impossible mission. is maintained in a state of relaxation. 1 Amplitude of Accommodation hyperopia Maximum Amplitude= 25-0.4(age) • An emmetropic eye for reading and other near Probable Amplitude= 18.5-.3(age) work, at distance of 16 in (40cm), the required amount of acc. -

Pediatric Ophthalmology/Strabismus 2017-2019
Academy MOC Essentials® Practicing Ophthalmologists Curriculum 2017–2019 Pediatric Ophthalmology/Strabismus *** Pediatric Ophthalmology/Strabismus 2 © AAO 2017-2019 Practicing Ophthalmologists Curriculum Disclaimer and Limitation of Liability As a service to its members and American Board of Ophthalmology (ABO) diplomates, the American Academy of Ophthalmology has developed the Practicing Ophthalmologists Curriculum (POC) as a tool for members to prepare for the Maintenance of Certification (MOC) -related examinations. The Academy provides this material for educational purposes only. The POC should not be deemed inclusive of all proper methods of care or exclusive of other methods of care reasonably directed at obtaining the best results. The physician must make the ultimate judgment about the propriety of the care of a particular patient in light of all the circumstances presented by that patient. The Academy specifically disclaims any and all liability for injury or other damages of any kind, from negligence or otherwise, for any and all claims that may arise out of the use of any information contained herein. References to certain drugs, instruments, and other products in the POC are made for illustrative purposes only and are not intended to constitute an endorsement of such. Such material may include information on applications that are not considered community standard, that reflect indications not included in approved FDA labeling, or that are approved for use only in restricted research settings. The FDA has stated that it is the responsibility of the physician to determine the FDA status of each drug or device he or she wishes to use, and to use them with appropriate patient consent in compliance with applicable law. -

Surgical Options in Managing Convergent Strabismus Fixus Related to High Myopia
Ophthalmol Ina 2015;41(2):107-115 107 Case Report Surgical Options in Managing Convergent Strabismus Fixus Related to High Myopia Jessica Zarwan, Gusti G Suardana, Anna P Bani Department of Ophthalmology, Faculty of Medicine, Indonesia University Cipto Mangunkusumo Hospital, Jakarta ABSTRACT Background: Convergent strabismus fixus is a condition in which one or both eyes are anchored in extreme adduction. This condition is caused by superotemporal herniation of the enlarged globe from the muscle cone through the space between the superior and lateral rectus muscle. It is commonly related to high myopia. Recently, transposition type procedure which unite the superior and lateral rectus muscles were proposed as the treatment of choice in this condition. However, there is no clear consensus regarding the best surgical procedure in convergent strabismus fixus. This case series reported three rare cases of convergent strabismus fixus related to high myopia and highlight the option of surgical procedure that can be done in these cases. Case Illustration: Three patients presented with convergent strabismus fixus of both eyes with history of bilateral high myopia since childhood. All patients showed Krimsky tests of >95∆ET preoperatively, with medial displacement of superior rectus and inferior displacement of lateral rectus of both eyes in all patients on orbital imaging. The bilateral Yokoma procedure both resulted in an orthophoric postoperative result with marked improvement in abduction and elevation. The hemi-Jensen also showed a significant improvement of over than 60∆ on the operated eye, resorting it to a central position during primary gaze. Conclusion: Convergent strabismus fixus is a rare condition and frequently associated with high myopia. -

G:\All Users\Sally\COVD Journal\COVD 37 #3\Maples
Essay Treating the Trinity of Infantile Vision Development: Infantile Esotropia, Amblyopia, Anisometropia W.C. Maples,OD, FCOVD 1 Michele Bither, OD, FCOVD2 Southern College of Optometry,1 Northeastern State University College of Optometry2 ABSTRACT INTRODUCTION The optometric literature has begun to emphasize One of the most troublesome and long recognized pediatric vision and vision development with the advent groups of conditions facing the ophthalmic practitioner and prominence of the InfantSEE™ program and recently is that of esotropia, amblyopia, and high refractive published research articles on amblyopia, strabismus, error/anisometropia.1-7 The recent institution of the emmetropization and the development of refractive errors. InfantSEE™ program is highlighting the need for early There are three conditions with which clinicians should be vision examinations in order to diagnose and treat familiar. These three conditions include: esotropia, high amblyopia. Conditions that make up this trinity of refractive error/anisometropia and amblyopia. They are infantile vision development anomalies include: serious health and vision threats for the infant. It is fitting amblyopia, anisometropia (predominantly high that this trinity of early visual developmental conditions hyperopia in the amblyopic eye), and early onset, be addressed by optometric physicians specializing in constant strabismus, especially esotropia. The vision development. The treatment of these conditions is techniques we are proposing to treat infantile esotropia improving, but still leaves many children handicapped are also clinically linked to amblyopia and throughout life. The healing arts should always consider anisometropia. alternatives and improvements to what is presently The majority of this paper is devoted to the treatment considered the customary treatment for these conditions. -

Strabismus, Amblyopia & Leukocoria
Strabismus, Amblyopia & Leukocoria [ Color index: Important | Notes: F1, F2 | Extra ] EDITING FILE Objectives: ➢ Not given. Done by: Jwaher Alharbi, Farrah Mendoza. Revised by: Rawan Aldhuwayhi Resources: Slides + Notes + 434 team. NOTE: F1& F2 doctors are different, the doctor who gave F2 said she is in the exam committee so focus on her notes Amblyopia ● Definition Decrease in visual acuity of one eye without the presence of an organic cause that explains that decrease in visual acuity. He never complaints of anything and his family never noticed any abnormalities ● Incidence The most common cause of visual loss under 20 years of life (2-4% of the general population) ● How? Cortical ignorance of one eye. This will end up having a lazy eye ● binocular vision It is achieved by the use of the two eyes together so that separate and slightly dissimilar images arising in each eye are appreciated as a single image by the process of fusion. It’s importance 1. Stereopsis 2. Larger field If there is no coordination between the two eyes the person will have double vision and confusion so as a compensatory mechanism for double vision the brain will cause suppression. The visual pathway is a plastic system that continues to develop during childhood until around 6-9 years of age. During this time, the wiring between the retina and visual cortex is still developing. Any visual problem during this critical period, such as a refractive error or strabismus can mess up this developmental wiring, resulting in permanent visual loss that can't be fixed by any corrective means when they are older Why fusion may fail ? 1. -

Management of Vith Nerve Palsy-Avoiding Unnecessary Surgery
MANAGEMENT OF VITH NERVE PALSY-AVOIDING UNNECESSARY SURGERY P. RIORDAN-E VA and J. P. LEE London SUMMARY for unrecovered VIth nerve palsy must involve a trans Unresolved Vlth nerve palsy that is not adequately con position procedure3.4. The availability of botulinum toxin trolled by an abnormal head posture or prisms can be to overcome the contracture of the ipsilateral medial rectus 5 very suitably treated by surgery. It is however essential to now allows for full tendon transplantation techniques -7, differentiate partially recovered palsies, which are with the potential for greatly increased improvements in amenable to horizontal rectus surgery, from unrecovered final fields of binocular single vision, and deferment of palsies, which must be treated initially by a vertical any necessary surgery to the medial recti, which is also muscle transposition procedure. Botulinum toxin is a likely to improve the final outcome. valuable tool in making this distinction. It also facilitates This study provides definite evidence, from a large full tendon transposition in unrecovered palsies, which series of patients, of the potential functional outcome from appears to produce the best functional outcome of all the the surgical treatment of unresolved VIth nerve palsy, transposition procedures, with a reduction in the need for together with clear guidance as to the forms of surgery that further surgery. A study of the surgical management of 12 should be undertaken in specific cases. The fundamental patients with partially recovered Vlth nerve palsy and 59 role of botulinum toxin in establishing the degree of lateral patients with unrecovered palsy provides clear guidelines rectus function and hence the correct choice of initial sur on how to attain a successful functional outcome with the gery, and as an adjunct to transposition surgery for unre minimum amount of surgery. -

Pediatric Cataracts: a Retrospective Study of 12 Years (2004
Pediatric Cataracts: A Retrospective Study of 12 Years (2004 - 2016) Cataratas em Idade Pediátrica: Estudo Retrospetivo de 12 ARTIGO ORIGINAL Anos (2004 - 2016) Jorge MOREIRA1, Isabel RIBEIRO1, Ágata MOTA1, Rita GONÇALVES1, Pedro COELHO1, Tiago MAIO1, Paula TENEDÓRIO1 Acta Med Port 2017 Mar;30(3):169-174 ▪ https://doi.org/10.20344/amp.8223 ABSTRACT Introduction: Cataracts are a major cause of preventable childhood blindness. Visual prognosis of these patients depends on a prompt therapeutic approach. Understanding pediatric cataracts epidemiology is of great importance for the implementation of programs of primary prevention and early diagnosis. Material and Methods: We reviewed the clinical cases of pediatric cataracts diagnosed in the last 12 years at Hospital Pedro Hispano, in Porto. Results: We identified 42 cases of pediatric cataracts with an equal gender distribution. The mean age at diagnosis was 6 years and 64.3% of patients had bilateral disease. Decreased visual acuity was the commonest presenting sign (36.8%) followed by leucocoria (26.3%). The etiology was unknown in 59.5% of cases and there was a slight predominance of nuclear type cataract (32.5%). Cataract was associated with systemic diseases in 23.8% of cases and with ocular abnormalities in 33.3% of cases. 47.6% of patients were treated surgically. Postoperative complications occurred in 35% of cases and posterior capsular opacification was the most common (25%). Discussion: The report of 42 cases is probably the result of the low prevalence of cataracts in this age. Although the limitations of our study include small sample size, the profile of children with cataracts in our hospital has characteristics relatively similar to those described in the literature. -

Consecutive Exotropia After Convergent Strabismus Surgery—Surgical Treatment
Open Journal of Ophthalmology, 2016, 6, 103-107 Published Online May 2016 in SciRes. http://www.scirp.org/journal/ojoph http://dx.doi.org/10.4236/ojoph.2016.62014 Consecutive Exotropia after Convergent Strabismus Surgery—Surgical Treatment Ala Paduca State University of Medicine and Pharmacy “Nicolae Testemitanu”, Chișinău, Moldova Received 19 March 2016; accepted 9 May 2016; published 12 May 2016 Copyright © 2016 by author and Scientific Research Publishing Inc. This work is licensed under the Creative Commons Attribution International License (CC BY). http://creativecommons.org/licenses/by/4.0/ Abstract Purpose: In this study the results of consecutive exotropia surgical treatment by using different surgical technics are presented. Methods: This study included 34 patients, aged 21 to 47 years (mean 27.9), who underwent medial rectus muscle advancement alone or in combination with medial rectus resection and/or lateral rectus recession. The mean interval between original sur- gery and surgery for consecutive exotropia was 8.5 years (range: 5.5 years to 14 years). Most of patients had 2 and more prior surgeries (73.5%) sold by an adduction deficit (47.06%). Results: The overall mean preoperative exodeviation was 35.12 ± 10.13 PD. Satisfactory alignment (within 10 PD of orthophoria) was achieved in 20 patients (58.8%) at 10 days after surgery and 24 pa- tients (70.5%) at final 6-month follow-up. The most common surgical procedures were unilateral MR advancement and LR recession—47%. Conclusion: Medial rectus advancement is an effective method of surgical treatment, especially in cases with adduction limitation, but the risk of the eye- lid fissure narrowing in cases of MRM advancement more than 5 mm associated with resection is present.