A Clinician's Guide to Positional Plagiocephaly
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
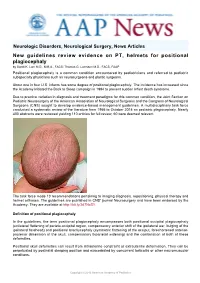
New Guidelines Review Evidence on PT, Helmets for Positional Plagiocephaly by Sandi K
Neurologic Disorders, Neurological Surgery, News Articles New guidelines review evidence on PT, helmets for positional plagiocephaly by Sandi K. Lam M.D., M.B.A., FACS; Thomas G. Luerssen M.D., FACS, FAAP Positional plagiocephaly is a common condition encountered by pediatricians and referred to pediatric subspecialty physicians such as neurosurgeons and plastic surgeons. About one in four U.S. infants has some degree of positional plagiocephaly. The incidence has increased since the Academy initiated the Back to Sleep campaign in 1994 to prevent sudden infant death syndrome. Due to practice variation in diagnosis and treatment paradigms for this common condition, the Joint Section on Pediatric Neurosurgery of the American Association of Neurological Surgeons and the Congress of Neurological Surgeons (CNS) sought to develop evidence-based management guidelines. A multidisciplinary task force conducted a systematic review of the literature from 1966 to October 2014 on pediatric plagiocephaly. Nearly 400 abstracts were reviewed yielding 110 articles for full review; 60 were deemed relevant. The task force made 10 recommendations pertaining to imaging diagnosis, repositioning, physical therapy and helmet orthoses. The guidelines are published in CNS' journal Neurosurgery and have been endorsed by the Academy. They are available at http://bit.ly/2d7NzS1. Definition of positional plagiocephaly In the guidelines, the term positional plagiocephaly encompasses both positional occipital plagiocephaly (unilateral flattening of parieto-occipital region, compensatory anterior shift of the ipsilateral ear, bulging of the ipsilateral forehead) and positional brachycephaly (symmetric flattening of the occiput, foreshortened anterior- posterior dimension of the skull, compensatory biparietal widening) and the combination of both of these deformities. -

West Texas Craniofacial Center of Excellence
TEAM MEMBERS Tammy Camp, M.D. PAID PERMIT #68 LUBBOCK, TX LUBBOCK, U.S. POSTAGE POSTAGE U.S. NONPROFIT ORG Pediatrician, Texas Tech Physicians Desiree Pendergrass, M.D. Pediatrician Dr. Camp Dr. Camp and Dr. Pendergrass will screen infants and children for cardiac, renal, feeding or airway problems often associated with syndromic craniofacial deformities. Alan Eisenbaum, M.D. Pediatric ophthalmologist, Dr. Pendergrass Texas Tech Physicians Curt Cockings, M.D. Pediatric ophthalmologist Dr. Eisenbaum and Dr. Cockings will screen infants and children with abnormal head shapes for any evidence of optic disc swelling of papilledema Dr. Eisenbaum suggestive of elevated intracranial pressure. They will also screen for any visual loss secondary to optic neuropathy, amblyopia or exposure keratopathy as a results of small orbital volume in syndromic synostoses. APPOINTMENTS Dr. Demke sees patients at the Texas Tech Physicians Medical Pavilion in the Surgery Clinic. His clinic days are Tuesday and Thursday, 8 a.m. – 5 p.m. Please call (806)743-2373 for a referral. SURGERY Dr. Nagy sees patients at Covenant Women’s and Children’s Hospital on Tuesdays and Wednesdays 9am – 5pm weekly. For this clinic location, Lubbock, 79430 Texas please call (806) 743-7700 for a referral. He also sees patients at Texas Department Surgery of Tech Physicians Medical Pavilion, 3rd floor, on Mondays from 9am – 5pm 8312 – MS Street 4th 3601 weekly. For this clinic location, please call (806) 743-7335 for a referral. If a patient needs to see both Dr. Demke and Dr. Nagy, arrangements SURGERY will be made to see the patient on the same day. -

MECHANISMS in ENDOCRINOLOGY: Novel Genetic Causes of Short Stature
J M Wit and others Genetics of short stature 174:4 R145–R173 Review MECHANISMS IN ENDOCRINOLOGY Novel genetic causes of short stature 1 1 2 2 Jan M Wit , Wilma Oostdijk , Monique Losekoot , Hermine A van Duyvenvoorde , Correspondence Claudia A L Ruivenkamp2 and Sarina G Kant2 should be addressed to J M Wit Departments of 1Paediatrics and 2Clinical Genetics, Leiden University Medical Center, PO Box 9600, 2300 RC Leiden, Email The Netherlands [email protected] Abstract The fast technological development, particularly single nucleotide polymorphism array, array-comparative genomic hybridization, and whole exome sequencing, has led to the discovery of many novel genetic causes of growth failure. In this review we discuss a selection of these, according to a diagnostic classification centred on the epiphyseal growth plate. We successively discuss disorders in hormone signalling, paracrine factors, matrix molecules, intracellular pathways, and fundamental cellular processes, followed by chromosomal aberrations including copy number variants (CNVs) and imprinting disorders associated with short stature. Many novel causes of GH deficiency (GHD) as part of combined pituitary hormone deficiency have been uncovered. The most frequent genetic causes of isolated GHD are GH1 and GHRHR defects, but several novel causes have recently been found, such as GHSR, RNPC3, and IFT172 mutations. Besides well-defined causes of GH insensitivity (GHR, STAT5B, IGFALS, IGF1 defects), disorders of NFkB signalling, STAT3 and IGF2 have recently been discovered. Heterozygous IGF1R defects are a relatively frequent cause of prenatal and postnatal growth retardation. TRHA mutations cause a syndromic form of short stature with elevated T3/T4 ratio. Disorders of signalling of various paracrine factors (FGFs, BMPs, WNTs, PTHrP/IHH, and CNP/NPR2) or genetic defects affecting cartilage extracellular matrix usually cause disproportionate short stature. -

Prenatal Ultrasonography of Craniofacial Abnormalities
Prenatal ultrasonography of craniofacial abnormalities Annisa Shui Lam Mak, Kwok Yin Leung Department of Obstetrics and Gynaecology, Queen Elizabeth Hospital, Hong Kong SAR, China REVIEW ARTICLE https://doi.org/10.14366/usg.18031 pISSN: 2288-5919 • eISSN: 2288-5943 Ultrasonography 2019;38:13-24 Craniofacial abnormalities are common. It is important to examine the fetal face and skull during prenatal ultrasound examinations because abnormalities of these structures may indicate the presence of other, more subtle anomalies, syndromes, chromosomal abnormalities, or even rarer conditions, such as infections or metabolic disorders. The prenatal diagnosis of craniofacial abnormalities remains difficult, especially in the first trimester. A systematic approach to the fetal Received: May 29, 2018 skull and face can increase the detection rate. When an abnormality is found, it is important Revised: June 30, 2018 to perform a detailed scan to determine its severity and search for additional abnormalities. Accepted: July 3, 2018 Correspondence to: The use of 3-/4-dimensional ultrasound may be useful in the assessment of cleft palate and Kwok Yin Leung, MBBS, MD, FRCOG, craniosynostosis. Fetal magnetic resonance imaging can facilitate the evaluation of the palate, Cert HKCOG (MFM), Department of micrognathia, cranial sutures, brain, and other fetal structures. Invasive prenatal diagnostic Obstetrics and Gynaecology, Queen Elizabeth Hospital, Gascoigne Road, techniques are indicated to exclude chromosomal abnormalities. Molecular analysis for some Kowloon, Hong Kong SAR, China syndromes is feasible if the family history is suggestive. Tel. +852-3506 6398 Fax. +852-2384 5834 E-mail: [email protected] Keywords: Craniofacial; Prenatal; Ultrasound; Three-dimensional ultrasonography; Fetal structural abnormalities This is an Open Access article distributed under the Introduction terms of the Creative Commons Attribution Non- Commercial License (http://creativecommons.org/ licenses/by-nc/3.0/) which permits unrestricted non- Craniofacial abnormalities are common. -

Occipital Plagiocephaly: a Critical Review of the Literature
Occipital plagiocephaly: a critical review of the literature Harold L. Rekate, M.D. Pediatric Neurosurgery, Barrow Neurologic Institute, Phoenix, Arizona The objective of this review was to determine what information is available on the incidence, pathophysiology, late complications, and treatment paradigms for occipital plagiocephaly based on a critical review of the literature obtained from recognized databases in peer-reviewed scientific publications. The content of this article is based on a critical review of the literature, and when discussing treatment options, classification of those articles with respect to the strength of the recommendations they contain. Using standard computerized search techniques, databases containing medical literature were queried for key words related to occipital plagiocephaly beginning in 1966. Key words used for this search were: lambdoid, craniosynostosis, cranial sutures, facial asymmetry, torticollis, and plagiocephaly. Titles of all articles were scanned for relevance. Copies of all potentially relevant articles published in the English language were obtained and received at least a cursory review. Several articles not captured by these methods were found to be important when referenced in the articles obtained. Articles discussing treatment were divided into Class I, Class II, and Class III data for the purpose of deciding on their applicability to the development of a potential consensus for the treatment of this controversial condition. Using the aforementioned key words, there were 4308 articles identified with potential relevance: scanning by title excluded all but 89. Of the 89, those with on-line abstracts were scanned, the remainder were obtained via interlibrary loan when needed for scanning of the article itself. The actual incidence of occipital plagiocephaly is unknown and there are no population-based studies of its incidence or prevalence. -

Cell Lines Or Lymphocytes Collected from Blood Via Trizol HDAC4 in Each of These Cases Revealed De Novo Mutations
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Elsevier - Publisher Connector ARTICLE Haploinsufficiency of HDAC4 Causes Brachydactyly Mental Retardation Syndrome, with Brachydactyly Type E, Developmental Delays, and Behavioral Problems Stephen R. Williams,1 Micheala A. Aldred,3 Vazken M. Der Kaloustian,4,6 Fahed Halal,5 Gordon Gowans,7 D. Ross McLeod,8 Sara Zondag,9 Helga V. Toriello,9 R. Ellen Magenis,10 and Sarah H. Elsea1,2,* Brachydactyly mental retardation syndrome (BDMR) is associated with a deletion involving chromosome 2q37. BDMR presents with a range of features, including intellectual disabilities, developmental delays, behavioral abnormalities, sleep disturbance, craniofacial and skeletal abnormalities (including brachydactyly type E), and autism spectrum disorder. To date, only large deletions of 2q37 have been reported, making delineation of a critical region and subsequent identification of candidate genes difficult. We present clinical and molecular analysis of six individuals with overlapping deletions involving 2q37.3 that refine the critical region, reducing the candi- date genes from >20 to a single gene, histone deacetylase 4 (HDAC4). Driven by the distinct hand and foot anomalies and similar cognitive features, we identified other cases with clinical findings consistent with BDMR but without a 2q37 deletion, and sequencing of HDAC4 identified de novo mutations, including one intragenic deletion probably disrupting normal splicing and one intragenic insertion that results in a frameshift and premature stop codon. HDAC4 is a histone deacetylase that regulates genes important in bone, muscle, À/À neurological, and cardiac development. Reportedly, Hdac4 mice have severe bone malformations resulting from premature ossifica- tion of developing bones. -

Occipital Plagiocephaly: a Critical Review of the Literature
Occipital plagiocephaly: a critical review of the literature Harold L. Rekate, M.D. Pediatric Neurosurgery, Barrow Neurologic Institute, Phoenix, Arizona The objective of this review was to determine what information is available on the incidence, pathophysiology, late complications, and treatment paradigms for occipital plagiocephaly based on a critical review of the literature obtained from recognized databases in peer-reviewed scientific publications. The content of this article is based on a critical review of the literature, and when discussing treatment options, classification of those articles with respect to the strength of the recommendations they contain. Using standard computerized search techniques, databases containing medical literature were queried for key words related to occipital plagiocephaly beginning in 1966. Key words used for this search were: lambdoid, craniosynostosis, cranial sutures, facial asymmetry, torticollis, and plagiocephaly. Titles of all articles were scanned for relevance. Copies of all potentially relevant articles published in the English language were obtained and received at least a cursory review. Several articles not captured by these methods were found to be important when referenced in the articles obtained. Articles discussing treatment were divided into Class I, Class II, and Class III data for the purpose of deciding on their applicability to the development of a potential consensus for the treatment of this controversial condition. Using the aforementioned key words, there were 4308 articles identified with potential relevance: scanning by title excluded all but 89. Of the 89, those with on-line abstracts were scanned, the remainder were obtained via interlibrary loan when needed for scanning of the article itself. The actual incidence of occipital plagiocephaly is unknown and there are no population-based studies of its incidence or prevalence. -

Identifying the Misshapen Head: Craniosynostosis and Related Disorders Mark S
CLINICAL REPORT Guidance for the Clinician in Rendering Pediatric Care Identifying the Misshapen Head: Craniosynostosis and Related Disorders Mark S. Dias, MD, FAAP, FAANS,a Thomas Samson, MD, FAAP,b Elias B. Rizk, MD, FAAP, FAANS,a Lance S. Governale, MD, FAAP, FAANS,c Joan T. Richtsmeier, PhD,d SECTION ON NEUROLOGIC SURGERY, SECTION ON PLASTIC AND RECONSTRUCTIVE SURGERY Pediatric care providers, pediatricians, pediatric subspecialty physicians, and abstract other health care providers should be able to recognize children with abnormal head shapes that occur as a result of both synostotic and aSection of Pediatric Neurosurgery, Department of Neurosurgery and deformational processes. The purpose of this clinical report is to review the bDivision of Plastic Surgery, Department of Surgery, College of characteristic head shape changes, as well as secondary craniofacial Medicine and dDepartment of Anthropology, College of the Liberal Arts characteristics, that occur in the setting of the various primary and Huck Institutes of the Life Sciences, Pennsylvania State University, State College, Pennsylvania; and cLillian S. Wells Department of craniosynostoses and deformations. As an introduction, the physiology and Neurosurgery, College of Medicine, University of Florida, Gainesville, genetics of skull growth as well as the pathophysiology underlying Florida craniosynostosis are reviewed. This is followed by a description of each type of Clinical reports from the American Academy of Pediatrics benefit from primary craniosynostosis (metopic, unicoronal, bicoronal, sagittal, lambdoid, expertise and resources of liaisons and internal (AAP) and external reviewers. However, clinical reports from the American Academy of and frontosphenoidal) and their resultant head shape changes, with an Pediatrics may not reflect the views of the liaisons or the emphasis on differentiating conditions that require surgical correction from organizations or government agencies that they represent. -

The Genetics of Canine Skull Shape Variation
PERSPECTIVES The Genetics of Canine Skull Shape Variation Jeffrey J. Schoenebeck and Elaine A. Ostrander1 Cancer Genetics Branch, National Human Genome Research Institute, National Institutes of Health, Bethesda, Maryland 20892 ABSTRACT A dog’s craniofacial diversity is the result of continual human intervention in natural selection, a process that began tens of thousands of years ago. To date, we know little of the genetic underpinnings and developmental mechanisms that make dog skulls so morphologically plastic. In this Perspectives, we discuss the origins of dog skull shapes in terms of history and biology and highlight recent advances in understanding the genetics of canine skull shapes. Of particular interest are those molecular genetic changes that are associated with the development of distinct breeds. OMETIME during the Paleolithic, a remarkable transfor- Variation in Skull Shape and Dog Domestication mation occurred. Small numbers of gray wolves adopted S Molecular clock estimates from mitochondrial DNA suggest a new pack master—humans. Through the process of do- domestication started as early as 135,000 years ago (Vilà mestication, the modern dog emerged. Today most dogs et al. 1997). More conservative estimates are based on ar- share little resemblance to their lupine ancestors. As a result chaeological records, which indicate that dog domestication of artificial selection, dogs radiated to fill niches in our lives, began somewhere between 15,000 and 36,000 years ago becoming our herders, guardians, hunters, rescuers, and com- (see summary by Larson et al. 2012). Current archaeologi- panions (Wilcox and Walkowicz 1995). The range of sizes cal estimates depend on carbon dating of bones, whose among dogs extends beyond that of wolves, giving dogs the morphologies appear distinct from that of contemporary distinction of being the most morphologically diverse terres- wolves. -

Congenital Scoliosis of the Pediatric Cervical Spine
Congenital Scoliosis of the Pediatric Cervical Spine Brandon Toll, Amer Samdani, Joshua Pahys and Steven Hwang Shriners Hospitals for Children-Philadelphia ICEOS Portugal 2018 Introduction Literature on congenital scoliosis predominantly focuses on thoracic and thoracolumbar curves Papers to date include a handful of 1-2 patients and one series of 18 patients of cervicothoracic hemi vertebra (Chen et al, Spine 2018) Purpose: to better define surgical outcomes of patients having undergone spinal fusions for cervical scoliosis with osseous anomalies Methods Retrospective chart and radiographic review of 17 patients was conducted (2009-2016) from a single center (Shriners Hospitals for Children-Philadelphia) All patients treated surgically for cervical congenital scoliosis with adequate clinical and radiographic data available for analysis Analysis was performed with t-tests (paired and independent samples) and binary correlation Concurrent Findings Cohort Total Number (%) VACTERL Syndrome 2 (11.8) 9 boys/8 girls Tethered Cord 2 (11.8) The most prevalent presentations Sprengel’s Deformity 2 (11.8) were torticollis (29%), and Klippel- Torticollis 5 (29.4) Feil syndrome (17.6%) Klippel-Feil Syndrome 3 (17.6) Pierre Robin Syndrome 1 (5.9) Mean age at surgery was 7.07 ± Brown Syndrome 1 (5.9) 3.38 years Bruck Syndrome 1 (5.9) Average follow-up of 3.06 ± 1.78 Poland’s Syndrome 1 (5.9) years Goldenhar Syndrome 1 (5.9) Larsen Syndrome 2 (11.8) 4 cognitively delayed (23.5%) and 3 non-ambulatory (17.6%) Cognitively Delayed 4 (23.5) Non-ambulatory -

Review Article Cleidocranial Dysplasia: Clinical and Molecular Genetics
J Med Genet 1999;36:177–182 177 Review article Cleidocranial dysplasia: clinical and molecular genetics Stefan Mundlos Abstract Chinese named Arnold, was probably de- Cleidocranial dysplasia (CCD) (MIM scribed by Jackson.6 He was able to trace 356 119600) is an autosomal dominant skeletal members of this family of whom 70 were dysplasia characterised by abnormal aVected with the “Arnold Head”. CCD was clavicles, patent sutures and fontanelles, originally thought to involve only bones of supernumerary teeth, short stature, and a membranous origin. More recent and detailed variety of other skeletal changes. The dis- clinical investigations have shown that CCD is ease gene has been mapped to chromo- a generalised skeletal dysplasia aVecting not some 6p21 within a region containing only the clavicles and the skull but the entire CBFA1, a member of the runt family of skeleton. CCD was therefore considered to be transcription factors. Mutations in the a dysplasia rather than a dysostosis.7 Skeletal CBFA1 gene that presumably lead to syn- abnormalities commonly found include cla- thesis of an inactive gene product were vicular aplasia/hypoplasia, bell shaped thorax, identified in patients with CCD. The func- enlarged calvaria with frontal bossing and open tion of CBFA1 during skeletal develop- fontanelles, Wormian bones, brachydactyly ment was further elucidated by the with hypoplastic distal phalanges, hypoplasia of generation of mutated mice in which the the pelvis with widened symphysis pubis, Cbfa1 gene locus was targeted. Loss of one severe dental anomalies, and short stature. The Cbfa1 allele (+/-) leads to a phenotype very changes suggest that the gene responsible is not similar to human CCD, featuring hypo- only active during early development, as plasia of the clavicles and patent fonta- implied by changes in the shape or number of nelles. -

Cranial Sutures & Funny Shaped Heads: Radiological Diagnosis
Objectives • The objectives of this presentation are to: – Review the imaging features of normal cranial sutures – Identify the characteristics of abnormal skull shape on imaging – Review the characteristics of the most common non- syndromic and syndromic causes of craniosynostosis Anatomical Review Anatomical Review • The bony plates of the skull communicate at the cranial sutures • The anterior fontanelle occurs where the coronal & metopic sutures meet • The posterior fontanelle occurs where the sagittal & lambdoid sutures meet Anatomical Review • The main cranial sutures & fontanelles include: Metopic Suture Anterior Fontanelle Coronal Sutures Squamosal Sutures Posterior Fontanelle Sagittal Suture Lambdoid Sutures Anatomical Review • Growth of the skull occurs perpendicular to the cranial suture • This is controlled by a complex signalling system including: – Ephrins (mark the suture boundary) – Fibroblast growth factor receptors (FGFR) – Transcription factor TWIST Anatomical Review • The cranial sutures are important for rapid skull growth in-utero & infancy • The cranial sutures can usually be visualised on imaging into late adulthood Normal Radiological Appearances Normal Radiological Appearances • The cranial sutures can be visualised on plain radiographs • Standard views include: – PA – Lateral – Townes PA Skull radiograph Sagittal Suture Left Coronal Suture Right CoronalRight lambdoidSutureSuture Metopic Suture Left lambdoid Suture Townes View Sagittal Suture Left Coronal Suture Right Coronal Suture Right Lambdoid Suture Left