Rare Germline Variant Contributions to Myeloid Malignancy Susceptibility
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
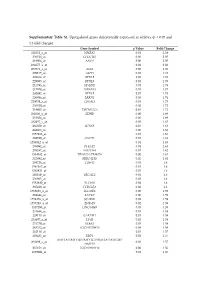
Supplementary Table S1. Upregulated Genes Differentially
Supplementary Table S1. Upregulated genes differentially expressed in athletes (p < 0.05 and 1.3-fold change) Gene Symbol p Value Fold Change 221051_s_at NMRK2 0.01 2.38 236518_at CCDC183 0.00 2.05 218804_at ANO1 0.00 2.05 234675_x_at 0.01 2.02 207076_s_at ASS1 0.00 1.85 209135_at ASPH 0.02 1.81 228434_at BTNL9 0.03 1.81 229985_at BTNL9 0.01 1.79 215795_at MYH7B 0.01 1.78 217979_at TSPAN13 0.01 1.77 230992_at BTNL9 0.01 1.75 226884_at LRRN1 0.03 1.74 220039_s_at CDKAL1 0.01 1.73 236520_at 0.02 1.72 219895_at TMEM255A 0.04 1.72 201030_x_at LDHB 0.00 1.69 233824_at 0.00 1.69 232257_s_at 0.05 1.67 236359_at SCN4B 0.04 1.64 242868_at 0.00 1.63 1557286_at 0.01 1.63 202780_at OXCT1 0.01 1.63 1556542_a_at 0.04 1.63 209992_at PFKFB2 0.04 1.63 205247_at NOTCH4 0.01 1.62 1554182_at TRIM73///TRIM74 0.00 1.61 232892_at MIR1-1HG 0.02 1.61 204726_at CDH13 0.01 1.6 1561167_at 0.01 1.6 1565821_at 0.01 1.6 210169_at SEC14L5 0.01 1.6 236963_at 0.02 1.6 1552880_at SEC16B 0.02 1.6 235228_at CCDC85A 0.02 1.6 1568623_a_at SLC35E4 0.00 1.59 204844_at ENPEP 0.00 1.59 1552256_a_at SCARB1 0.02 1.59 1557283_a_at ZNF519 0.02 1.59 1557293_at LINC00969 0.03 1.59 231644_at 0.01 1.58 228115_at GAREM1 0.01 1.58 223687_s_at LY6K 0.02 1.58 231779_at IRAK2 0.03 1.58 243332_at LOC105379610 0.04 1.58 232118_at 0.01 1.57 203423_at RBP1 0.02 1.57 AMY1A///AMY1B///AMY1C///AMY2A///AMY2B// 208498_s_at 0.03 1.57 /AMYP1 237154_at LOC101930114 0.00 1.56 1559691_at 0.01 1.56 243481_at RHOJ 0.03 1.56 238834_at MYLK3 0.01 1.55 213438_at NFASC 0.02 1.55 242290_at TACC1 0.04 1.55 ANKRD20A1///ANKRD20A12P///ANKRD20A2/// -

A Computational Approach for Defining a Signature of Β-Cell Golgi Stress in Diabetes Mellitus
Page 1 of 781 Diabetes A Computational Approach for Defining a Signature of β-Cell Golgi Stress in Diabetes Mellitus Robert N. Bone1,6,7, Olufunmilola Oyebamiji2, Sayali Talware2, Sharmila Selvaraj2, Preethi Krishnan3,6, Farooq Syed1,6,7, Huanmei Wu2, Carmella Evans-Molina 1,3,4,5,6,7,8* Departments of 1Pediatrics, 3Medicine, 4Anatomy, Cell Biology & Physiology, 5Biochemistry & Molecular Biology, the 6Center for Diabetes & Metabolic Diseases, and the 7Herman B. Wells Center for Pediatric Research, Indiana University School of Medicine, Indianapolis, IN 46202; 2Department of BioHealth Informatics, Indiana University-Purdue University Indianapolis, Indianapolis, IN, 46202; 8Roudebush VA Medical Center, Indianapolis, IN 46202. *Corresponding Author(s): Carmella Evans-Molina, MD, PhD ([email protected]) Indiana University School of Medicine, 635 Barnhill Drive, MS 2031A, Indianapolis, IN 46202, Telephone: (317) 274-4145, Fax (317) 274-4107 Running Title: Golgi Stress Response in Diabetes Word Count: 4358 Number of Figures: 6 Keywords: Golgi apparatus stress, Islets, β cell, Type 1 diabetes, Type 2 diabetes 1 Diabetes Publish Ahead of Print, published online August 20, 2020 Diabetes Page 2 of 781 ABSTRACT The Golgi apparatus (GA) is an important site of insulin processing and granule maturation, but whether GA organelle dysfunction and GA stress are present in the diabetic β-cell has not been tested. We utilized an informatics-based approach to develop a transcriptional signature of β-cell GA stress using existing RNA sequencing and microarray datasets generated using human islets from donors with diabetes and islets where type 1(T1D) and type 2 diabetes (T2D) had been modeled ex vivo. To narrow our results to GA-specific genes, we applied a filter set of 1,030 genes accepted as GA associated. -

2020 Program Book
PROGRAM BOOK Note that TAGC was cancelled and held online with a different schedule and program. This document serves as a record of the original program designed for the in-person meeting. April 22–26, 2020 Gaylord National Resort & Convention Center Metro Washington, DC TABLE OF CONTENTS About the GSA ........................................................................................................................................................ 3 Conference Organizers ...........................................................................................................................................4 General Information ...............................................................................................................................................7 Mobile App ....................................................................................................................................................7 Registration, Badges, and Pre-ordered T-shirts .............................................................................................7 Oral Presenters: Speaker Ready Room - Camellia 4.......................................................................................7 Poster Sessions and Exhibits - Prince George’s Exhibition Hall ......................................................................7 GSA Central - Booth 520 ................................................................................................................................8 Internet Access ..............................................................................................................................................8 -

DEAD-Box RNA Helicases in Cell Cycle Control and Clinical Therapy
cells Review DEAD-Box RNA Helicases in Cell Cycle Control and Clinical Therapy Lu Zhang 1,2 and Xiaogang Li 2,3,* 1 Department of Nephrology, Renmin Hospital of Wuhan University, Wuhan 430060, China; [email protected] 2 Department of Internal Medicine, Mayo Clinic, 200 1st Street, SW, Rochester, MN 55905, USA 3 Department of Biochemistry and Molecular Biology, Mayo Clinic, 200 1st Street, SW, Rochester, MN 55905, USA * Correspondence: [email protected]; Tel.: +1-507-266-0110 Abstract: Cell cycle is regulated through numerous signaling pathways that determine whether cells will proliferate, remain quiescent, arrest, or undergo apoptosis. Abnormal cell cycle regula- tion has been linked to many diseases. Thus, there is an urgent need to understand the diverse molecular mechanisms of how the cell cycle is controlled. RNA helicases constitute a large family of proteins with functions in all aspects of RNA metabolism, including unwinding or annealing of RNA molecules to regulate pre-mRNA, rRNA and miRNA processing, clamping protein complexes on RNA, or remodeling ribonucleoprotein complexes, to regulate gene expression. RNA helicases also regulate the activity of specific proteins through direct interaction. Abnormal expression of RNA helicases has been associated with different diseases, including cancer, neurological disorders, aging, and autosomal dominant polycystic kidney disease (ADPKD) via regulation of a diverse range of cellular processes such as cell proliferation, cell cycle arrest, and apoptosis. Recent studies showed that RNA helicases participate in the regulation of the cell cycle progression at each cell cycle phase, including G1-S transition, S phase, G2-M transition, mitosis, and cytokinesis. -

R-Loop Proximity Proteomics Identifies a Role of DDX41 in Transcription- 2 Associated Genomic Instability
R-loop proximity proteomics identies a role of DDX41 in transcription-associated genomic instability Thorsten Mosler Institute of Molecular Biology (IMB) Francesca Conte Institute of Molecular Biology (IMB) Ivan Mikicic Institute of Molecular Biology (IMB) https://orcid.org/0000-0003-3393-0688 Nastasja Kreim Institute of Molecular Biology Martin Möckel Institute of Molecular Biology (IMB) Johanna Flach Medical Faculty Mannheim of the Heidelberg University Brian Luke Johannes Gutenberg University of Mainz https://orcid.org/0000-0002-1648-5511 Petra Beli ( [email protected] ) Institute of Molecular Biology (IMB) https://orcid.org/0000-0001-9507-9820 Article Keywords: DDX41, genomic instability, proximity proteomics, R-loops, transcription Posted Date: April 26th, 2021 DOI: https://doi.org/10.21203/rs.3.rs-337351/v1 License: This work is licensed under a Creative Commons Attribution 4.0 International License. Read Full License 1 R-loop proximity proteomics identifies a role of DDX41 in transcription- 2 associated genomic instability 1 1 1 1 1 3 Thorsten Mosler , Francesca Conte , Ivan Mikicic , Nastasja Kreim , Martin M. Möckel , 4 Johanna Flach2, Brian Luke1,3, Petra Beli1,3,# 5 6 1Institute of Molecular Biology (IMB), Mainz, Germany 7 2Department of Hematology and Oncology, Medical Faculty Mannheim of the Heidelberg 8 University, Mannheim, Germany 9 3Institute of Developmental Biology and Neurobiology (IDN), Johannes Gutenberg-Universität, 10 Mainz, Germany. 11 #Correspondence should be addressed to [email protected] 12 13 14 15 16 17 18 19 20 21 22 Keywords: DDX41, genomic instability, proximity proteomics, R-loops, transcription 23 1 24 Abstract 25 Transcription can pose a threat to genomic stability through the formation of R-loops that 26 obstruct the progression of replication forks. -

Expression of the POTE Gene Family in Human Ovarian Cancer Carter J Barger1,2, Wa Zhang1,2, Ashok Sharma 1,2, Linda Chee1,2, Smitha R
www.nature.com/scientificreports OPEN Expression of the POTE gene family in human ovarian cancer Carter J Barger1,2, Wa Zhang1,2, Ashok Sharma 1,2, Linda Chee1,2, Smitha R. James3, Christina N. Kufel3, Austin Miller 4, Jane Meza5, Ronny Drapkin 6, Kunle Odunsi7,8,9, 2,10 1,2,3 Received: 5 July 2018 David Klinkebiel & Adam R. Karpf Accepted: 7 November 2018 The POTE family includes 14 genes in three phylogenetic groups. We determined POTE mRNA Published: xx xx xxxx expression in normal tissues, epithelial ovarian and high-grade serous ovarian cancer (EOC, HGSC), and pan-cancer, and determined the relationship of POTE expression to ovarian cancer clinicopathology. Groups 1 & 2 POTEs showed testis-specifc expression in normal tissues, consistent with assignment as cancer-testis antigens (CTAs), while Group 3 POTEs were expressed in several normal tissues, indicating they are not CTAs. Pan-POTE and individual POTEs showed signifcantly elevated expression in EOC and HGSC compared to normal controls. Pan-POTE correlated with increased stage, grade, and the HGSC subtype. Select individual POTEs showed increased expression in recurrent HGSC, and POTEE specifcally associated with reduced HGSC OS. Consistent with tumors, EOC cell lines had signifcantly elevated Pan-POTE compared to OSE and FTE cells. Notably, Group 1 & 2 POTEs (POTEs A/B/B2/C/D), Group 3 POTE-actin genes (POTEs E/F/I/J/KP), and other Group 3 POTEs (POTEs G/H/M) show within-group correlated expression, and pan-cancer analyses of tumors and cell lines confrmed this relationship. Based on their restricted expression in normal tissues and increased expression and association with poor prognosis in ovarian cancer, POTEs are potential oncogenes and therapeutic targets in this malignancy. -

BRCC3 Mutations in Myeloid Neoplasms
Myeloid Malignancies SUPPLEMENTARY APPENDIX BRCC3 mutations in myeloid neoplasms Dayong Huang, 1,2 * Yasunobu Nagata, 3* Vera Grossmann, 4 Tomas Radivoyevitch, 5 Yusuke Okuno, 3 Genta Nagae, 6 Naoko Hosono, 2 Susanne Schnittger, 4 Masashi Sanada, 3 Bartlomiej Przychodzen, 2 Ayana Kon, 3 Chantana Polprasert, 2 Wenyi Shen, 2 Michael J. Clemente, 2 James G. Phillips, 2 Tamara Alpermann, 4 Kenichi Yoshida, 3 Niroshan Nadarajah, 4 7 Mikkael A. Sekeres, Kevin Oakley, 8 Nhu Nguyen, 8 Yuichi Shiraishi, 9 Yusuke Shiozawa, 3 Kenichi Chiba, 9 Hiroko Tanaka, 10 H. Phillip Koeffler, 11,12 Hans-Ulrich Klein, 13 Martin Dugas, 13 Hiroyuki Aburatani, 6 Satoru Miyano, 9,10 Claudia Haferlach, 4 Wolfgang Kern, 4 Torsten Haferlach, 4 Yang Du, 8 Seishi Ogawa, 3 and Hideki Makishima 2,3 1Department of Hematology, Beijing Friendship Hospital, Capital Medical University, Beijing, China; 2Department of Translational Hema - tology and Oncology Research, Taussig Cancer Institute, Cleveland Clinic, Cleveland, OH, USA; 3Department of Pathology and Tumor Biol - ogy, Kyoto University, Japan; 4Munich Leukemia Laboratory (MLL), Germany; 5Department of Quantitative Health Sciences, Lerner Research Institute, Cleveland Clinic, OH, USA; 6Genome Science Division, Research Center for Advanced Science and Technology, The University of Tokyo, Japan; 7Leukemia Program, Taussig Cancer Institute, Cleveland Clinic, OH, USA; 8Department of Pediatrics, Uni - formed Services University of the Health Sciences, Bethesda, MD, USA; 9Laboratory of DNA Information Analysis, Human Genome Cen - ter, Institute of Medical Science, The University of Tokyo, Japan; 10 Laboratory of Sequence Analysis, Human Genome Center, Institute of Medical Science, The University of Tokyo, Japan; 11 Department of Hematology/Oncology, Cedars-Sinai Medical Center, Los Angeles, CA, USA; 12 Cancer Science Institute of Singapore, National University of Singapore; and 13 Institute of Medical Informatics, University of Mün - ster, Germany *DH and YN contributed equally to this work. -

Supplementary Table S4. FGA Co-Expressed Gene List in LUAD
Supplementary Table S4. FGA co-expressed gene list in LUAD tumors Symbol R Locus Description FGG 0.919 4q28 fibrinogen gamma chain FGL1 0.635 8p22 fibrinogen-like 1 SLC7A2 0.536 8p22 solute carrier family 7 (cationic amino acid transporter, y+ system), member 2 DUSP4 0.521 8p12-p11 dual specificity phosphatase 4 HAL 0.51 12q22-q24.1histidine ammonia-lyase PDE4D 0.499 5q12 phosphodiesterase 4D, cAMP-specific FURIN 0.497 15q26.1 furin (paired basic amino acid cleaving enzyme) CPS1 0.49 2q35 carbamoyl-phosphate synthase 1, mitochondrial TESC 0.478 12q24.22 tescalcin INHA 0.465 2q35 inhibin, alpha S100P 0.461 4p16 S100 calcium binding protein P VPS37A 0.447 8p22 vacuolar protein sorting 37 homolog A (S. cerevisiae) SLC16A14 0.447 2q36.3 solute carrier family 16, member 14 PPARGC1A 0.443 4p15.1 peroxisome proliferator-activated receptor gamma, coactivator 1 alpha SIK1 0.435 21q22.3 salt-inducible kinase 1 IRS2 0.434 13q34 insulin receptor substrate 2 RND1 0.433 12q12 Rho family GTPase 1 HGD 0.433 3q13.33 homogentisate 1,2-dioxygenase PTP4A1 0.432 6q12 protein tyrosine phosphatase type IVA, member 1 C8orf4 0.428 8p11.2 chromosome 8 open reading frame 4 DDC 0.427 7p12.2 dopa decarboxylase (aromatic L-amino acid decarboxylase) TACC2 0.427 10q26 transforming, acidic coiled-coil containing protein 2 MUC13 0.422 3q21.2 mucin 13, cell surface associated C5 0.412 9q33-q34 complement component 5 NR4A2 0.412 2q22-q23 nuclear receptor subfamily 4, group A, member 2 EYS 0.411 6q12 eyes shut homolog (Drosophila) GPX2 0.406 14q24.1 glutathione peroxidase -

Datasheet Blank Template
SAN TA C RUZ BI OTEC HNOL OG Y, INC . DDX41 (N-13): sc-104868 BACKGROUND RECOMMENDED SECONDARY REAGENTS DDX41 (probable ATP-dependent RNA helicase DDX41, DEAD-box protein To ensure optimal results, the following support (secondary) reagents are abstrakt homolog) is a 622 amino acid protein encoded by the human gene recommended: 1) Western Blotting: use donkey anti-goat IgG-HRP: sc-2020 DDX41. DDX41 belongs to the DEAD-box helicase family (DDX41 subfamily) (dilution range: 1:2000-1:100,000) or Cruz Marker™ compatible donkey and contains one CCHC-type zinc finger, one helicase ATP-binding domain and anti- goat IgG-HRP: sc-2033 (dilution range: 1:2000-1:5000), Cruz Marker™ one helicase C-terminal domain. DDX41 is required during post-transcriptional Molecular Weight Standards: sc-2035, TBS Blotto A Blocking Reagent: gene expression and is thought to be involved in pre-mRNA splicing. DDX41 sc-2333 and Western Blotting Luminol Reagent: sc-2048. 2) Immunoprecip- is believed to be a probable ATP-dependent RNA helicase. RNA helicases are itation: use Protein A/G PLUS-Agarose: sc-2003 (0.5 ml agarose/2.0 ml). highly conserved enzymes that utilize the energy derived from NTP hydrolysis 3) Immunofluorescence: use donkey anti-goat IgG-FITC: sc-2024 (dilution to modulate the structure of RNA. RNA helicases participate in all biological range: 1:100-1:400) or donkey anti-goat IgG-TR: sc-2783 (dilution range: processes that involve RNA, including transcription, splicing and translation. 1:100-1:400) with UltraCruz™ Mounting Medium: sc-24941. REFERENCES DATA 1. Irion, U. -

Fusion Transcripts and Transcribed Retrotransposed Loci Discovered Through Comprehensive Transcriptome Analysis Using Paired-End Ditags (Pets)
Downloaded from genome.cshlp.org on September 24, 2021 - Published by Cold Spring Harbor Laboratory Press Letter Fusion transcripts and transcribed retrotransposed loci discovered through comprehensive transcriptome analysis using Paired-End diTags (PETs) Yijun Ruan,1,6 Hong Sain Ooi,2 Siew Woh Choo,2 Kuo Ping Chiu,2 Xiao Dong Zhao,1 K.G. Srinivasan,1 Fei Yao,1 Chiou Yu Choo,1 Jun Liu,1 Pramila Ariyaratne,2 Wilson G.W. Bin,2 Vladimir A. Kuznetsov,2 Atif Shahab,3 Wing-Kin Sung,2,4 Guillaume Bourque,2 Nallasivam Palanisamy,5 and Chia-Lin Wei1,6 1Genome Technology and Biology Group, Genome Institute of Singapore, Singapore 138672, Singapore; 2Information and Mathematical Science Group, Genome Institute of Singapore, Singapore 138672, Singapore; 3Bioinformatics Institute, Singapore 138671, Singapore; 4School of Computing, National University of Singapore, Singapore 117543, Singapore; 5Cancer Biology Group, Genome Institute of Singapore, Singapore 138672, Singapore Identification of unconventional functional features such as fusion transcripts is a challenging task in the effort to annotate all functional DNA elements in the human genome. Paired-End diTag (PET) analysis possesses a unique capability to accurately and efficiently characterize the two ends of DNA fragments, which may have either normal or unusual compositions. This unique nature of PET analysis makes it an ideal tool for uncovering unconventional features residing in the human genome. Using the PET approach for comprehensive transcriptome analysis, we were able to identify fusion transcripts derived from genome rearrangements and actively expressed retrotransposed pseudogenes, which would be difficult to capture by other means. Here, we demonstrate this unique capability through the analysis of 865,000 individual transcripts in two types of cancer cells. -

The Impact of the Ubiquitin System in the Pathogenesis of Squamous Cell Carcinomas
cancers Review The Impact of the Ubiquitin System in the Pathogenesis of Squamous Cell Carcinomas Veronica Gatti 1, Francesca Bernassola 2, Claudio Talora 3, Gerry Melino 2 and Angelo Peschiaroli 1,* 1 National Research Council of Italy, Institute of Translational Pharmacology, 00133 Rome, Italy; [email protected] 2 Department of Experimental Medicine, TOR, University of Rome Tor Vergata, 00133 Rome, Italy; [email protected] (F.B.); [email protected] (G.M.) 3 Department of Molecular Medicine, Sapienza University of Rome, 00185 Rome, Italy; [email protected] * Correspondence: [email protected] Received: 20 May 2020; Accepted: 13 June 2020; Published: 16 June 2020 Abstract: The ubiquitin system is a dynamic regulatory pathway controlling the activity, subcellular localization and stability of a myriad of cellular proteins, which in turn affects cellular homeostasis through the regulation of a variety of signaling cascades. Aberrant activity of key components of the ubiquitin system has been functionally linked with numerous human diseases including the initiation and progression of human tumors. In this review, we will contextualize the importance of the two main components of the ubiquitin system, the E3 ubiquitin ligases (E3s) and deubiquitinating enzymes (DUBs), in the etiology of squamous cell carcinomas (SCCs). We will discuss the signaling pathways regulated by these enzymes, emphasizing the genetic and molecular determinants underlying their deregulation in SCCs. Keywords: squamous cell carcinoma; E3 ubiquitin ligase; deubiquitinating enzymes; oncogenes; tumor suppressor 1. Introduction 1.1. Molecular Landscape of SCCs Squamous cell carcinomas (SCCs) are highly common and malignant solid cancers that arise from stratified and pseudo-stratified epithelia of the skin, and the aerodigestive and genitourinary tracts. -

Mouse Brcc3 Knockout Project (CRISPR/Cas9)
https://www.alphaknockout.com Mouse Brcc3 Knockout Project (CRISPR/Cas9) Objective: To create a Brcc3 knockout Mouse model (C57BL/6N) by CRISPR/Cas-mediated genome engineering. Strategy summary: The Brcc3 gene (NCBI Reference Sequence: NM_001166457 ; Ensembl: ENSMUSG00000031201 ) is located on Mouse chromosome X. 11 exons are identified, with the ATG start codon in exon 1 and the TAA stop codon in exon 10 (Transcript: ENSMUST00000033544). Exon 5~7 will be selected as target site. Cas9 and gRNA will be co-injected into fertilized eggs for KO Mouse production. The pups will be genotyped by PCR followed by sequencing analysis. Note: Exon 5 starts from about 36.2% of the coding region. Exon 5~7 covers 26.69% of the coding region. The size of effective KO region: ~2527 bp. The KO region does not have any other known gene. Page 1 of 9 https://www.alphaknockout.com Overview of the Targeting Strategy Wildtype allele 5' gRNA region gRNA region 3' 1 5 6 7 11 Legends Exon of mouse Brcc3 Knockout region Page 2 of 9 https://www.alphaknockout.com Overview of the Dot Plot (up) Window size: 15 bp Forward Reverse Complement Sequence 12 Note: The 2000 bp section upstream of Exon 5 is aligned with itself to determine if there are tandem repeats. No significant tandem repeat is found in the dot plot matrix. So this region is suitable for PCR screening or sequencing analysis. Overview of the Dot Plot (down) Window size: 15 bp Forward Reverse Complement Sequence 12 Note: The 2000 bp section downstream of Exon 7 is aligned with itself to determine if there are tandem repeats.