(Or a Ringworm Infection)? What Causes Tinea?
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Estimated Burden of Serious Fungal Infections in Ghana
Journal of Fungi Article Estimated Burden of Serious Fungal Infections in Ghana Bright K. Ocansey 1, George A. Pesewu 2,*, Francis S. Codjoe 2, Samuel Osei-Djarbeng 3, Patrick K. Feglo 4 and David W. Denning 5 1 Laboratory Unit, New Hope Specialist Hospital, Aflao 00233, Ghana; [email protected] 2 Department of Medical Laboratory Sciences, School of Biomedical and Allied Health Sciences, College of Health Sciences, University of Ghana, P.O. Box KB-143, Korle-Bu, Accra 00233, Ghana; [email protected] 3 Department of Pharmaceutical Sciences, Faculty of Health Sciences, Kumasi Technical University, P.O. Box 854, Kumasi 00233, Ghana; [email protected] 4 Department of Clinical Microbiology, School of Medical Sciences, Kwame Nkrumah University of Science and Technology, Kumasi 00233, Ghana; [email protected] 5 National Aspergillosis Centre, Wythenshawe Hospital and the University of Manchester, Manchester M23 9LT, UK; [email protected] * Correspondence: [email protected] or [email protected] or [email protected]; Tel.: +233-277-301-300; Fax: +233-240-190-737 Received: 5 March 2019; Accepted: 14 April 2019; Published: 11 May 2019 Abstract: Fungal infections are increasingly becoming common and yet often neglected in developing countries. Information on the burden of these infections is important for improved patient outcomes. The burden of serious fungal infections in Ghana is unknown. We aimed to estimate this burden. Using local, regional, or global data and estimates of population and at-risk groups, deterministic modelling was employed to estimate national incidence or prevalence. Our study revealed that about 4% of Ghanaians suffer from serious fungal infections yearly, with over 35,000 affected by life-threatening invasive fungal infections. -
Fungal Infection
The Pocket Guide to Fungal Infection Second Edition Malcolm D. Richardson PhD, FIBiol, FRCPath Mycology Unit Department of Bacteriology and Immunology University of Helsinki Helsinki, Finland Elizabeth M. Johnson PhD Mycology Reference Laboratory Health Protection Agency Bristol, United Kingdom The Pocket Guide to Fungal Infection Second Edition To families and friends The Pocket Guide to Fungal Infection Second Edition Malcolm D. Richardson PhD, FIBiol, FRCPath Mycology Unit Department of Bacteriology and Immunology University of Helsinki Helsinki, Finland Elizabeth M. Johnson PhD Mycology Reference Laboratory Health Protection Agency Bristol, United Kingdom © 2005 Malcolm D. Richardson, Elizabeth M. Johnson Published by Blackwell Publishing Ltd Blackwell Publishing, Inc., 350 Main Street, Malden, Massachusetts 02148-5020, USA Blackwell Publishing Ltd, 9600 Garsington Road, Oxford OX4 2DQ, UK Blackwell Publishing Asia Pty Ltd, 550 Swanston Street, Carlton, Victoria 3053, Australia The right of the Authors to be identified as the Authors of this Work has been asserted in accordance with the Copyright, Designs and Patents Act 1988. All rights reserved. No part of this publication may be reproduced, stored in a retrieval system, or transmitted, in any form or by any means, electronic, mechanical, photocopying, recording or otherwise, except as permitted by the UK Copyright, Designs and Patents Act 1988, without the prior permission of the publisher. First edition published 2000 Reprinted 2000, 2002 Second Edition 2005 Library of Congress Cataloging-in-Publication Data Richardson, M. D. The pocket guide to fungal infection / Malcolm D. Richardson, Elizabeth M. Johnson. — 2nd ed. p. ; cm. Includes bibliographical references and index. ISBN-13: 978-1-4051-2218-4 ISBN-10: 1-4051-2218-8 1. -

Fungal Infections from Human and Animal Contact
Journal of Patient-Centered Research and Reviews Volume 4 Issue 2 Article 4 4-25-2017 Fungal Infections From Human and Animal Contact Dennis J. Baumgardner Follow this and additional works at: https://aurora.org/jpcrr Part of the Bacterial Infections and Mycoses Commons, Infectious Disease Commons, and the Skin and Connective Tissue Diseases Commons Recommended Citation Baumgardner DJ. Fungal infections from human and animal contact. J Patient Cent Res Rev. 2017;4:78-89. doi: 10.17294/2330-0698.1418 Published quarterly by Midwest-based health system Advocate Aurora Health and indexed in PubMed Central, the Journal of Patient-Centered Research and Reviews (JPCRR) is an open access, peer-reviewed medical journal focused on disseminating scholarly works devoted to improving patient-centered care practices, health outcomes, and the patient experience. REVIEW Fungal Infections From Human and Animal Contact Dennis J. Baumgardner, MD Aurora University of Wisconsin Medical Group, Aurora Health Care, Milwaukee, WI; Department of Family Medicine and Community Health, University of Wisconsin School of Medicine and Public Health, Madison, WI; Center for Urban Population Health, Milwaukee, WI Abstract Fungal infections in humans resulting from human or animal contact are relatively uncommon, but they include a significant proportion of dermatophyte infections. Some of the most commonly encountered diseases of the integument are dermatomycoses. Human or animal contact may be the source of all types of tinea infections, occasional candidal infections, and some other types of superficial or deep fungal infections. This narrative review focuses on the epidemiology, clinical features, diagnosis and treatment of anthropophilic dermatophyte infections primarily found in North America. -

Tinea Capitis
TPGC01.qxd 1/5/06 1:15 PM Page 4 Dermatophytosis Tinea capitis Tinea capitis due to Trichophyton tonsurans. Kerion due to Trichophyton verrucosum. Definition Tinea capitis describes infection of the scalp and hair with a dermatophyte. Geographical distribution World-wide, but more common in Africa, Asia and southern and eastern Europe, occurring mainly in prepubescent children. Increasing incidence. 4 TPGC01.qxd 1/5/06 1:15 PM Page 5 Dermatophytosis Hair infected by Microsporum gyseum showing large-spored ecothrix invasion. Macroconidia of Microsporum canis. Causal organisms and habitat • Several Trichophyton spp. and Microsporum spp. • Zoophilic M. canis (cats and dogs) is common in western Europe. • Anthropophilic T. violaceum is predominant in eastern and southern Europe and north Africa. • Anthropophilic T. tonsurans is increasing in prevalence, especially in North America. 5 TPGC01.qxd 1/5/06 1:15 PM Page 6 Dermatophytosis Microsporum canis in culture. • Anthropophilic species can be contagious and endemic. • T. schoenleinii causes favus. Clinical manifestations • Mild scaling lesions to widespread alopecia. • Kerion: highly inflammatory, suppurating lesion caused by zoophilic dermatophytes. • Black dot appearance seen with ectothrix hair invasion. • Favus is a distinctive infection with grey, crusting lesions. • Asymptomatic carrier state recognized, may promote spread of infection. • T. tonsurans and T. violaceum – most commonly implicated in the carrier state. • Minimal inflammatory response. • Low spore numbers. • Topical treatment -

Tinea Capitis 2014 L.C
BJD GUIDELINES British Journal of Dermatology British Association of Dermatologists’ guidelines for the management of tinea capitis 2014 L.C. Fuller,1 R.C. Barton,2 M.F. Mohd Mustapa,3 L.E. Proudfoot,4 S.P. Punjabi5 and E.M. Higgins6 1Department of Dermatology, Chelsea & Westminster Hospital, Fulham Road, London SW10 9NH, U.K. 2Department of Microbiology, Leeds General Infirmary, Leeds LS1 3EX, U.K. 3British Association of Dermatologists, Willan House, 4 Fitzroy Square, London W1T 5HQ, U.K. 4St John’s Institute of Dermatology, Guy’s and St Thomas’ NHS Foundation Trust, St Thomas’ Hospital, Westminster Bridge Road, London SE1 7EH, U.K. 5Department of Dermatology, Hammersmith Hospital, 150 Du Cane Road, London W12 0HS, U.K. 6Department of Dermatology, King’s College Hospital, Denmark Hill, London SE5 9RS, U.K. 1.0 Purpose and scope Correspondence Claire Fuller. The overall objective of this guideline is to provide up-to- E-mail: [email protected] date, evidence-based recommendations for the management of tinea capitis. This document aims to update and expand Accepted for publication on the previous guidelines by (i) offering an appraisal of 8 June 2014 all relevant literature since January 1999, focusing on any key developments; (ii) addressing important, practical clini- Funding sources cal questions relating to the primary guideline objective, i.e. None. accurate diagnosis and identification of cases; suitable treat- ment to minimize duration of disease, discomfort and scar- Conflicts of interest ring; and limiting spread among other members of the L.C.F. has received sponsorship to attend conferences from Almirall, Janssen and LEO Pharma (nonspecific); has acted as a consultant for Alliance Pharma (nonspe- community; (iii) providing guideline recommendations and, cific); and has legal representation for L’Oreal U.K. -

Therapies for Common Cutaneous Fungal Infections
MedicineToday 2014; 15(6): 35-47 PEER REVIEWED FEATURE 2 CPD POINTS Therapies for common cutaneous fungal infections KENG-EE THAI MB BS(Hons), BMedSci(Hons), FACD Key points A practical approach to the diagnosis and treatment of common fungal • Fungal infection should infections of the skin and hair is provided. Topical antifungal therapies always be in the differential are effective and usually used as first-line therapy, with oral antifungals diagnosis of any scaly rash. being saved for recalcitrant infections. Treatment should be for several • Topical antifungal agents are typically adequate treatment weeks at least. for simple tinea. • Oral antifungal therapy may inea and yeast infections are among the dermatophytoses (tinea) and yeast infections be required for extensive most common diagnoses found in general and their differential diagnoses and treatments disease, fungal folliculitis and practice and dermatology. Although are then discussed (Table). tinea involving the face, hair- antifungal therapies are effective in these bearing areas, palms and T infections, an accurate diagnosis is required to ANTIFUNGAL THERAPIES soles. avoid misuse of these or other topical agents. Topical antifungal preparations are the most • Tinea should be suspected if Furthermore, subsequent active prevention is commonly prescribed agents for dermatomy- there is unilateral hand just as important as the initial treatment of the coses, with systemic agents being used for dermatitis and rash on both fungal infection. complex, widespread tinea or when topical agents feet – ‘one hand and two feet’ This article provides a practical approach fail for tinea or yeast infections. The pharmacol- involvement. to antifungal therapy for common fungal infec- ogy of the systemic agents is discussed first here. -

Tinea Capitis: Unusual Chronic Presentation in an Elderly Woman
ISSN: 2474-3658 Salazar et al. J Infect Dis Epidemiol 2018, 4:048 DOI: 10.23937/2474-3658/1510048 Volume 4 | Issue 1 Journal of Open Access Infectious Diseases and Epidemiology CASE REPORT Tinea Capitis: Unusual Chronic Presentation in an Elderly Woman Elizabeth Salazar1*, Daniel Asz-Sigall2, Diana Vega3 and Roberto Arenas4 1Dermato-Oncologist, Private Practice, Mexico City, Mexico 2 Check for Dermatologist, Dermato-Oncology and Trichology Clinic, National University of Mexico, Mexico City, Mexico updates 3Mycologist, Mycology Section, Hospital General “Dr. Manuel Gea González”, Mexico City, Mexico 4Dermatologist and Mycologist, Mycology Section, General Hospital “Dr. Manuel Gea González”, Mexico City, Mexico *Corresponding authors: Elizabeth Salazar, Dermato-Oncologist, Private Practice, Mexico City, Mexico, E-mail: dra. [email protected] The non-inflammatory clinical presentation can be Abstract found in 90% of affected children. It is more frequent in Tinea capitis is a superficial fungal infection of the scalp tropical regions with low socioeconomic conditions and and hair caused by dermatophytes such as Trichophyton and Microsporum. Tinea capitis is very rare in adults, and affects almost exclusively children (98%). The inflamma- may affect those with immunosuppressive diseases or tory form is observed only in 10% and most commonly menopausal elderly women. Clinical manifestations along seen in prepubescent children. Tinea capitis is caused with trichoscopy and Wood’s light, can help the clinician to by dermatophytes that use keratin as a nutrient source. determine the correct diagnosis, in order to reduce irrevers- Scalp erythema, scaling, and crusting are typical signs of ible sequelae and decrease multiple contagion. KOH direct exam and culture confirm diagnosis and aetiology. -

Geophilic Dermatophytes and Other Keratinophilic Fungi in the Nests of Wetland Birds
ACTA MyCoLoGICA Vol. 46 (1): 83–107 2011 Geophilic dermatophytes and other keratinophilic fungi in the nests of wetland birds Teresa KoRnIŁŁoWICz-Kowalska1, IGnacy KIToWSKI2 and HELEnA IGLIK1 1Department of Environmental Microbiology, Mycological Laboratory University of Life Sciences in Lublin Leszczyńskiego 7, PL-20-069 Lublin, [email protected] 2Department of zoology, University of Life Sciences in Lublin, Akademicka 13 PL-20-950 Lublin, [email protected] Korniłłowicz-Kowalska T., Kitowski I., Iglik H.: Geophilic dermatophytes and other keratinophilic fungi in the nests of wetland birds. Acta Mycol. 46 (1): 83–107, 2011. The frequency and species diversity of keratinophilic fungi in 38 nests of nine species of wetland birds were examined. nine species of geophilic dermatophytes and 13 Chrysosporium species were recorded. Ch. keratinophilum, which together with its teleomorph (Aphanoascus fulvescens) represented 53% of the keratinolytic mycobiota of the nests, was the most frequently observed species. Chrysosporium tropicum, Trichophyton terrestre and Microsporum gypseum populations were less widespread. The distribution of individual populations was not uniform and depended on physical and chemical properties of the nests (humidity, pH). Key words: Ascomycota, mitosporic fungi, Chrysosporium, occurrence, distribution INTRODUCTION Geophilic dermatophytes and species representing the Chrysosporium group (an arbitrary term) related to them are ecologically classified as keratinophilic fungi. Ke- ratinophilic fungi colonise keratin matter (feathers, hair, etc., animal remains) in the soil, on soil surface and in other natural environments. They are keratinolytic fungi physiologically specialised in decomposing native keratin. They fully solubilise na- tive keratin (chicken feathers) used as the only source of carbon and energy in liquid cultures after 70 to 126 days of growth (20°C) (Korniłłowicz-Kowalska 1997). -

Therapies for Common Cutaneous Fungal Infections
MedicineToday 2014; 15(6): 35-47 PEER REVIEWED FEATURE 2 CPD POINTS Therapies for common cutaneous fungal infections KENG-EE THAI MB BS(Hons), BMedSci(Hons), FACD Key points A practical approach to the diagnosis and treatment of common fungal • Fungal infection should infections of the skin and hair is provided. Topical antifungal therapies always be in the differential are effective and usually used as first-line therapy, with oral antifungals diagnosis of any scaly rash. being saved for recalcitrant infections. Treatment should be for several • Topical antifungal agents are typically adequate treatment weeks at least. for simple tinea. • Oral antifungal therapy may inea and yeast infections are among the dermatophytoses (tinea) and yeast infections be required for extensive most common diagnoses found in general and their differential diagnoses and treatments disease, fungal folliculitis and practice and dermatology. Although are then discussed (Table). tinea involving the face, hair- antifungal therapies are effective in these bearing areas, palms and T infections, an accurate diagnosis is required to ANTIFUNGAL THERAPIES soles. avoid misuse of these or other topical agents. Topical antifungal preparations are the most • Tinea should be suspected if Furthermore, subsequent active prevention is commonly prescribed agents for dermatomy- there is unilateral hand just as important as the initial treatment of the coses, with systemic agents being used for dermatitis and rash on both fungal infection. complex, widespread tinea or when topical agents feet – ‘one hand and two feet’ This article provides a practical approach fail for tinea or yeast infections. The pharmacol- involvement. to antifungal therapy for common fungal infec- ogy of the systemic agents is discussed first here. -
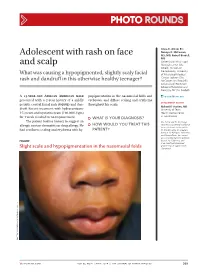
Adolescent with Rash on Face and Scalp
Photo RoUNDS Anna K. Allred, BS; Nancye K. McCowan, Adolescent with rash on face MS, MD; Robert Brodell, MD University of Mississippi and scalp Medical Center (Ms. Allred); Division of Dermatology, University What was causing a hypopigmented, slightly scaly facial of Mississippi Medical Center, Jackson (Drs. rash and dandruff in this otherwise healthy teenager? McCowan and Brodell); University of Rochester School of Medicine and Dentistry, NY (Dr. Brodell) A 13-year-old African American male popigmentation in the nasomesial folds and [email protected] presented with a 2-year history of a mildly eyebrows, and diffuse scaling and erythema DEpartment EDItOR pruritic central facial rash (FIGURE) and dan- throughout his scalp. Richard p. Usatine, MD druff. Recent treatment with hydrocortisone University of Texas 1% cream and nystatin cream (100,000 U/gm) Health Science Center at San Antonio for 1 week resulted in no improvement. ● What is youR diAgnosis? The patient had no history to suggest an Ms. Allred and Dr. McCowan allergic contact dermatitis or drug allergy. He ● HoW Would you TReAT THIS reported no potential conflict of interest relevant to this article. had confluent scaling and erythema with hy- pATIENT? Dr. Brodell serves on speaker’s bureaus for Allergan, Galderma, and PharmaDerm, has served as a consultant and on advisory Figure boards for Galderma, and is an investigator/received grant/research support from Slight scale and hypopigmentation in the nasomesial folds Genentech. PHO T o COU RT ESY OF : R o B e RT BR ODELL , MD jfponline.com Vol 63, no 4 | ApRIL 2014 | The jouRnAl of Family PracTice 209 PHOTO RoUNDS Diagnosis: the Malassezia yeast and topical steroids are Seborrheic dermatitis used to suppress inflammation. -

Fungal Infections (Mycoses): Dermatophytoses (Tinea, Ringworm)
Editorial | Journal of Gandaki Medical College-Nepal Fungal Infections (Mycoses): Dermatophytoses (Tinea, Ringworm) Reddy KR Professor & Head Microbiology Department Gandaki Medical College & Teaching Hospital, Pokhara, Nepal Medical Mycology, a study of fungal epidemiology, ecology, pathogenesis, diagnosis, prevention and treatment in human beings, is a newly recognized discipline of biomedical sciences, advancing rapidly. Earlier, the fungi were believed to be mere contaminants, commensals or nonpathogenic agents but now these are commonly recognized as medically relevant organisms causing potentially fatal diseases. The discipline of medical mycology attained recognition as an independent medical speciality in the world sciences in 1910 when French dermatologist Journal of Raymond Jacques Adrien Sabouraud (1864 - 1936) published his seminal treatise Les Teignes. This monumental work was a comprehensive account of most of then GANDAKI known dermatophytes, which is still being referred by the mycologists. Thus he MEDICAL referred as the “Father of Medical Mycology”. COLLEGE- has laid down the foundation of the field of Medical Mycology. He has been aptly There are significant developments in treatment modalities of fungal infections NEPAL antifungal agent available. Nystatin was discovered in 1951 and subsequently and we have achieved new prospects. However, till 1950s there was no specific (J-GMC-N) amphotericin B was introduced in 1957 and was sanctioned for treatment of human beings. In the 1970s, the field was dominated by the azole derivatives. J-GMC-N | Volume 10 | Issue 01 developed to treat fungal infections. By the end of the 20th century, the fungi have Now this is the most active field of interest, where potential drugs are being January-June 2017 been reported to be developing drug resistance, especially among yeasts. -
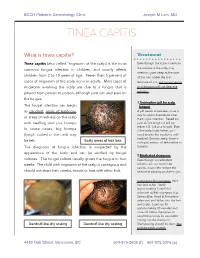
Tinea Capitis
BCCH Pediatric Dermatology Clinic Joseph M Lam, MD TINEA CAPITIS What is tinea capitis? Treatment Tinea capitis (also called “ringworm of the scalp) is the most Even though the scale is seen on common fungus infection in children, and usually affects the surface of the scalp, the infection goes deep to the root children from 2 to 10 years of age. Fewer than 5 percent of of the hair, under the skin. cases of ringworm of the scalp occur in adults. Most cases of Because of this, just using creams ringworm involving the scalp are due to a fungus that is or shampoos will not clear the passed from person to person, although pets can also pass on infection. the fungus. 1.Terbinafine (pill for scalp The fungal infection can begin fungus) as dandruff, areas of baldness, A pill needs to be taken once a day for about 4 weeks to clear or areas of redness on the scalp the fungus infection. Based on with swelling and pus bumps. your child’s weight, it will be either 1/2, 3/4 or a full pill. Even In some cases, big bumps if the scalp looks better, you (lymph nodes) in the neck may need to take the medicine until Scaly areas of hair loss finished. Unfortunately, there is be felt. no liquid version of terbinafine in The diagnosis of fungus infection is suspected by the Canada. appearance of the scalp and can be verified by fungal 2.Medicated shampoos cultures. The fungal culture usually grows the fungus in four Even though a medicated weeks.