Systems Biology Understanding of the Effects of Lithium on Cancer
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

CXCR4 Pathway Retards Muscle Atrophy During Cancer Cachexia
Oncogene (2016) 35, 6212–6222 © 2016 Macmillan Publishers Limited, part of Springer Nature. All rights reserved 0950-9232/16 www.nature.com/onc ORIGINAL ARTICLE Activation of the SDF1/CXCR4 pathway retards muscle atrophy during cancer cachexia GB Martinelli1, D Olivari1, AD Re Cecconi1, L Talamini1, L Ottoboni2, SH Lecker3, C Stretch4, VE Baracos4, OF Bathe5, A Resovi6, R Giavazzi1, L Cervo7 and R Piccirillo1 Cancer cachexia is a life-threatening syndrome that affects most patients with advanced cancers and causes severe body weight loss, with rapid depletion of skeletal muscle. No treatment is available. We analyzed microarray data sets to identify a subset of genes whose expression is specifically altered in cachectic muscles of Yoshida hepatoma-bearing rodents but not in those with diabetes, disuse, uremia or fasting. Ingenuity Pathways Analysis indicated that three genes belonging to the C-X-C motif chemokine receptor 4 (CXCR4) pathway were downregulated only in muscles atrophying because of cancer: stromal cell-derived factor 1 (SDF1), adenylate cyclase 7 (ADCY7), and p21 protein-activated kinase 1 (PAK1). Notably, we found that, in the Rectus Abdominis muscle of cancer patients, the expression of SDF1 and CXCR4 was inversely correlated with that of two ubiquitin ligases induced in muscle wasting, atrogin-1 and MuRF1, suggesting a possible clinical relevance of this pathway. The expression of all main SDF1 isoforms (α, β, γ) also declined in Tibialis Anterior muscle from cachectic mice bearing murine colon adenocarcinoma or human renal cancer and drugs with anticachexia properties restored their expression. Overexpressing genes of this pathway (that is, SDF1 or CXCR4) in cachectic muscles increased the fiber area by 20%, protecting them from wasting. -

Genome-Wide Association and Transcriptome Studies Identify Candidate Genes and Pathways for Feed Conversion Ratio in Pigs
Miao et al. BMC Genomics (2021) 22:294 https://doi.org/10.1186/s12864-021-07570-w RESEARCH ARTICLE Open Access Genome-wide association and transcriptome studies identify candidate genes and pathways for feed conversion ratio in pigs Yuanxin Miao1,2,3, Quanshun Mei1,2, Chuanke Fu1,2, Mingxing Liao1,2,4, Yan Liu1,2, Xuewen Xu1,2, Xinyun Li1,2, Shuhong Zhao1,2 and Tao Xiang1,2* Abstract Background: The feed conversion ratio (FCR) is an important productive trait that greatly affects profits in the pig industry. Elucidating the genetic mechanisms underpinning FCR may promote more efficient improvement of FCR through artificial selection. In this study, we integrated a genome-wide association study (GWAS) with transcriptome analyses of different tissues in Yorkshire pigs (YY) with the aim of identifying key genes and signalling pathways associated with FCR. Results: A total of 61 significant single nucleotide polymorphisms (SNPs) were detected by GWAS in YY. All of these SNPs were located on porcine chromosome (SSC) 5, and the covered region was considered a quantitative trait locus (QTL) region for FCR. Some genes distributed around these significant SNPs were considered as candidates for regulating FCR, including TPH2, FAR2, IRAK3, YARS2, GRIP1, FRS2, CNOT2 and TRHDE. According to transcriptome analyses in the hypothalamus, TPH2 exhibits the potential to regulate intestinal motility through serotonergic synapse and oxytocin signalling pathways. In addition, GRIP1 may be involved in glutamatergic and GABAergic signalling pathways, which regulate FCR by affecting appetite in pigs. Moreover, GRIP1, FRS2, CNOT2,andTRHDE may regulate metabolism in various tissues through a thyroid hormone signalling pathway. -

Supplementary Table S4. FGA Co-Expressed Gene List in LUAD
Supplementary Table S4. FGA co-expressed gene list in LUAD tumors Symbol R Locus Description FGG 0.919 4q28 fibrinogen gamma chain FGL1 0.635 8p22 fibrinogen-like 1 SLC7A2 0.536 8p22 solute carrier family 7 (cationic amino acid transporter, y+ system), member 2 DUSP4 0.521 8p12-p11 dual specificity phosphatase 4 HAL 0.51 12q22-q24.1histidine ammonia-lyase PDE4D 0.499 5q12 phosphodiesterase 4D, cAMP-specific FURIN 0.497 15q26.1 furin (paired basic amino acid cleaving enzyme) CPS1 0.49 2q35 carbamoyl-phosphate synthase 1, mitochondrial TESC 0.478 12q24.22 tescalcin INHA 0.465 2q35 inhibin, alpha S100P 0.461 4p16 S100 calcium binding protein P VPS37A 0.447 8p22 vacuolar protein sorting 37 homolog A (S. cerevisiae) SLC16A14 0.447 2q36.3 solute carrier family 16, member 14 PPARGC1A 0.443 4p15.1 peroxisome proliferator-activated receptor gamma, coactivator 1 alpha SIK1 0.435 21q22.3 salt-inducible kinase 1 IRS2 0.434 13q34 insulin receptor substrate 2 RND1 0.433 12q12 Rho family GTPase 1 HGD 0.433 3q13.33 homogentisate 1,2-dioxygenase PTP4A1 0.432 6q12 protein tyrosine phosphatase type IVA, member 1 C8orf4 0.428 8p11.2 chromosome 8 open reading frame 4 DDC 0.427 7p12.2 dopa decarboxylase (aromatic L-amino acid decarboxylase) TACC2 0.427 10q26 transforming, acidic coiled-coil containing protein 2 MUC13 0.422 3q21.2 mucin 13, cell surface associated C5 0.412 9q33-q34 complement component 5 NR4A2 0.412 2q22-q23 nuclear receptor subfamily 4, group A, member 2 EYS 0.411 6q12 eyes shut homolog (Drosophila) GPX2 0.406 14q24.1 glutathione peroxidase -

Bioinformatics Analysis Based on Gene Expression Omnibus
ANTICANCER RESEARCH 39 : 1689-1698 (2019) doi:10.21873/anticanres.13274 Chemo-resistant Gastric Cancer Associated Gene Expression Signature: Bioinformatics Analysis Based on Gene Expression Omnibus JUN-BAO LIU 1* , TUNYU JIAN 2* , CHAO YUE 3, DAN CHEN 4, WEI CHEN 5, TING-TING BAO 6, HAI-XIA LIU 7, YUN CAO 8, WEI-BING LI 6, ZHIJIAN YANG 9, ROBERT M. HOFFMAN 9 and CHEN YU 6 1Traditional Chinese Medicine Department, People's Hospital of Henan Province, People's Hospital of Zhengzhou University, Zhengzhou, P.R. China; 2Institute of Botany, Jiangsu Province and Chinese Academy of Sciences, Nanjing, P.R. China; 3Department of general surgery, Jiangsu Cancer Hospital & Jiangsu Institute of Cancer Research & The Affiliated Cancer Hospital of Nanjing Medical University, Nanjing, P.R. China; 4Research Center of Clinical Oncology, Jiangsu Cancer Hospital & Jiangsu Institute of Cancer Research & The Affiliated Cancer Hospital of Nanjing Medical University, Nanjing, P.R. China; 5Department of Head and Neck Surgery, Jiangsu Cancer Hospital & Jiangsu Institute of Cancer Research & The Affiliated Cancer Hospital of Nanjing Medical University, Nanjing, P.R. China; 6Department of Integrated TCM & Western Medicine, Jiangsu Cancer Hospital & Jiangsu Institute of Cancer Research & The Affiliated Cancer Hospital of Nanjing Medical University, Nanjing, P.R. China; 7Emergency Department, The Second Affiliated Hospital of Nanjing University of Chinese Medicine, Nanjing, P.R. China; 8Master candidate of Oncology, Nanjing University of Chinese Medicine, Nanjing, P.R. China; 9AntiCancer, Inc., San Diego, CA, U.S.A. Abstract. Background/Aim: This study aimed to identify identified, including 13 up-regulated and 1,473 down-regulated biomarkers for predicting the prognosis of advanced gastric genes. -
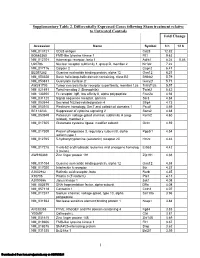
Supplementary Table 2
Supplementary Table 2. Differentially Expressed Genes following Sham treatment relative to Untreated Controls Fold Change Accession Name Symbol 3 h 12 h NM_013121 CD28 antigen Cd28 12.82 BG665360 FMS-like tyrosine kinase 1 Flt1 9.63 NM_012701 Adrenergic receptor, beta 1 Adrb1 8.24 0.46 U20796 Nuclear receptor subfamily 1, group D, member 2 Nr1d2 7.22 NM_017116 Calpain 2 Capn2 6.41 BE097282 Guanine nucleotide binding protein, alpha 12 Gna12 6.21 NM_053328 Basic helix-loop-helix domain containing, class B2 Bhlhb2 5.79 NM_053831 Guanylate cyclase 2f Gucy2f 5.71 AW251703 Tumor necrosis factor receptor superfamily, member 12a Tnfrsf12a 5.57 NM_021691 Twist homolog 2 (Drosophila) Twist2 5.42 NM_133550 Fc receptor, IgE, low affinity II, alpha polypeptide Fcer2a 4.93 NM_031120 Signal sequence receptor, gamma Ssr3 4.84 NM_053544 Secreted frizzled-related protein 4 Sfrp4 4.73 NM_053910 Pleckstrin homology, Sec7 and coiled/coil domains 1 Pscd1 4.69 BE113233 Suppressor of cytokine signaling 2 Socs2 4.68 NM_053949 Potassium voltage-gated channel, subfamily H (eag- Kcnh2 4.60 related), member 2 NM_017305 Glutamate cysteine ligase, modifier subunit Gclm 4.59 NM_017309 Protein phospatase 3, regulatory subunit B, alpha Ppp3r1 4.54 isoform,type 1 NM_012765 5-hydroxytryptamine (serotonin) receptor 2C Htr2c 4.46 NM_017218 V-erb-b2 erythroblastic leukemia viral oncogene homolog Erbb3 4.42 3 (avian) AW918369 Zinc finger protein 191 Zfp191 4.38 NM_031034 Guanine nucleotide binding protein, alpha 12 Gna12 4.38 NM_017020 Interleukin 6 receptor Il6r 4.37 AJ002942 -

Epigenetic Modifications to Cytosine and Alzheimer's Disease
University of Kentucky UKnowledge Theses and Dissertations--Chemistry Chemistry 2017 EPIGENETIC MODIFICATIONS TO CYTOSINE AND ALZHEIMER’S DISEASE: A QUANTITATIVE ANALYSIS OF POST-MORTEM TISSUE Elizabeth M. Ellison University of Kentucky, [email protected] Digital Object Identifier: https://doi.org/10.13023/ETD.2017.398 Right click to open a feedback form in a new tab to let us know how this document benefits ou.y Recommended Citation Ellison, Elizabeth M., "EPIGENETIC MODIFICATIONS TO CYTOSINE AND ALZHEIMER’S DISEASE: A QUANTITATIVE ANALYSIS OF POST-MORTEM TISSUE" (2017). Theses and Dissertations--Chemistry. 86. https://uknowledge.uky.edu/chemistry_etds/86 This Doctoral Dissertation is brought to you for free and open access by the Chemistry at UKnowledge. It has been accepted for inclusion in Theses and Dissertations--Chemistry by an authorized administrator of UKnowledge. For more information, please contact [email protected]. STUDENT AGREEMENT: I represent that my thesis or dissertation and abstract are my original work. Proper attribution has been given to all outside sources. I understand that I am solely responsible for obtaining any needed copyright permissions. I have obtained needed written permission statement(s) from the owner(s) of each third-party copyrighted matter to be included in my work, allowing electronic distribution (if such use is not permitted by the fair use doctrine) which will be submitted to UKnowledge as Additional File. I hereby grant to The University of Kentucky and its agents the irrevocable, non-exclusive, and royalty-free license to archive and make accessible my work in whole or in part in all forms of media, now or hereafter known. -

Characterization of a Novel Signal Transducer Element Intrinsic To
Characterization of a Novel Signal Transducer Element Intrinsic to Class IIIa/b Adenylate Cyclases and Guanylate Cyclases Miriam Ziegler1, Jens Bassler2, Stephanie Beltz1, Anita Schultz1, Andrei N. Lupas2, Joachim E. Schultz1* 1 Pharmazeutisches Institut der Universität Tübingen, Auf der Morgenstelle 8, 72076 Tübingen, Germany 2 Max-Planck-Institut für Entwicklungsbiologie, Abt. Proteinevolution, Spemannstr. 35, 72076 Tübingen, Germany Article Running title Novel Cylase-Transducer-Element in Adenylate Cyclases Article type : Regular Paper Correspondence J. E. Schultz, Pharmazeutisches Institut der Universität Tübingen, Auf der Morgenstelle 8, D- 72076 Tübingen, Germany, FAX: +49 7071 292476 Tel: +49 7071 2972475; E-mail: [email protected] Keywords adenylate cyclase, cyclic AMP (cAMP), receptor regulation, quorum-sensing, signal transduction, Legionella This article has been accepted for publication and undergone full peer review but has not Accepted been through the copyediting, typesetting, pagination and proofreading process, which may lead to differences between this version and the Version of Record. Please cite this article as doi: 10.1111/febs.14047 This article is protected by copyright. All rights reserved. Abbreviations AC, adenylate cyclase; GC, guanylate cyclase; CTE, cyclase-transducer-element; LAI-1, Legionella autoinducer-1; CAI-1, Legionella autoinducer-1; QS, quorum-sensing; CLANS, CLuster ANalysis of Sequences. Cholera Abstract Adenylate cyclases (ACs) are signalling proteins that produce the second messenger cAMP. Class III ACs comprises four groups (class IIIa-d); of these, class IIIa and IIIb ACs have been identified in bacteria and eukaryotes. Many class IIIa ACs are anchored to membranes via hexahelical domains. In eukaryotic ACs, membrane anchors are well conserved, suggesting that this region possesses important functional characteristics that are as yet Article unknown. -

Protective Potential of Mir-146A-5P and Its Underlying Molecular
Li et al. Cancer Cell Int (2019) 19:167 https://doi.org/10.1186/s12935-019-0886-y Cancer Cell International PRIMARY RESEARCH Open Access Protective potential of miR-146a-5p and its underlying molecular mechanism in diverse cancers: a comprehensive meta-analysis and bioinformatics analysis Mei‑wei Li†, Li Gao†, Yi‑wu Dang, Ping Li, Zu‑yun Li*, Gang Chen* and Dian‑zhong Luo Abstract Background/aims: Studies have shown that miR‑146a‑5p was diferentially expressed in diverse cancers, but the associations between miR‑146a‑5p expression and prognosis across multiple types of cancer as well its potential targets and downstream pathways have not been comprehensively analyzed. In this study, we performed the frst meta‑analysis of the prognostic value of miR‑146a‑5p expression in diverse malignancies and explored prospective targets of miR‑146a‑5p and related signaling pathways. Methods: A thorough search for articles related to miR‑146a‑5p was performed, and RNA‑seq data from The Cancer Genome Atlas (TCGA) and microarray data from gene expression omnibus profles were used to collect information about the prognostic value of miR‑146a‑5p. A comprehensive meta‑analysis was conducted. Twelve platforms in miRWalk 2.0 were applied to predict targets of miR‑146a‑5p. TCGA RNA‑seq data were used to validate the inverse relationships between miR‑146a‑5p and its likely targets. Subsequently, gene ontology and pathway analyses were conducted using Funrich version 3.1.3. Potential protein–protein interaction (PPI) networks were constructed. Poten‑ tial target genes of miR‑146a‑5p in lung cancer were validated by RT‑qPCR. -

Soluble Adenylyl Cyclase Inhibition Prevents Human Sperm Functions Essential for Fertilization
bioRxiv preprint doi: https://doi.org/10.1101/2021.04.27.441671; this version posted April 28, 2021. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. Soluble adenylyl cyclase inhibition prevents human sperm functions essential for fertilization Melanie Balbach1, Lubna Ghanem1, Thomas Rossetti1, Navpreet Kaur1, Carla Ritagliati1,3, Jacob Ferreira1, Dario Krapf3, Lis C Puga Molina4, Celia Maria Santi4, Jan Niklas Hansen5, Dagmar Wachten5, Makoto Fushimi2, Peter T. Meinke1,2, Jochen Buck1 & Lonny R. Levin1 1Department of Pharmacology, Weill Cornell Medicine, New York City, NY 2Tri-Institutional Therapeutics Discovery Institute, New York City, NY 3Laboratory of Cell Signal Transduction Networks, Instituto de Biología Molecular y Celular de Rosario, Rosario, Argentina 4Department of OB/GYN, Washington University School of Medicine, Saint Louis, Missouri 5Institute of Innate Immunity, Biophysical Imaging, Medical Faculty, University of Bonn, Bonn, Germany To whom correspondence should be addressed: Dr. Lonny R. Levin, Department of Pharmacology, Weill Cornell Medicine, 1300 York Avenue, New York City, NY, 10065; phone: +1 212 746 6752, email: [email protected] bioRxiv preprint doi: https://doi.org/10.1101/2021.04.27.441671; this version posted April 28, 2021. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. 1 Abstract 2 Soluble adenylyl cyclase (sAC: ADCY10) is essential for activating dormant sperm. Studies of 3 freshly dissected mouse sperm identified sAC as needed for initiating capacitation and activating 4 motility. -

Anti-ADCY5 Antibody (ARG10771)
Product datasheet [email protected] ARG10771 Package: 50 μg anti-ADCY5 antibody Store at: -20°C Summary Product Description Rabbit Polyclonal antibody recognizes ADCY5 Tested Reactivity Hu, Ms, Rat Tested Application Confocal, Dot, ELISA, ICC/IF, IHC, IP, WB Host Rabbit Clonality Polyclonal Isotype IgG Target Name ADCY5 Antigen Species Rat Immunogen Synthetic peptide from Rat ADCY5. Conjugation Un-conjugated Alternate Names FDFM; ATP pyrophosphate-lyase 5; AC5; Adenylate cyclase type V; Adenylate cyclase type 5; EC 4.6.1.1; Adenylyl cyclase 5 Application Instructions Application table Application Dilution Confocal 1:200 - 1:1000 Dot 1:10000 ELISA 1:10000 ICC/IF 1:200 - 1:1000 IHC 1:200 - 1:1000 IP 1:200 WB 1:500 Application Note * The dilutions indicate recommended starting dilutions and the optimal dilutions or concentrations should be determined by the scientist. Calculated Mw 139 kDa Properties Form Liquid Purification Affinity purified. Buffer Tris-Glycine Buffer (pH 7.4 - 7.8), Hepes, 0.02% Sodium azide, 30% Glycerol and 0.5% BSA. Preservative 0.02% Sodium azide www.arigobio.com 1/2 Stabilizer 30% Glycerol and 0.5% BSA Concentration 0.5 mg/ml Storage instruction For continuous use, store undiluted antibody at 2-8°C for up to a week. For long-term storage, aliquot and store at -20°C. Storage in frost free freezers is not recommended. Avoid repeated freeze/thaw cycles. Suggest spin the vial prior to opening. The antibody solution should be gently mixed before use. Note For laboratory research only, not for drug, diagnostic or other use. Bioinformation Gene Symbol Adcy5 Gene Full Name adenylate cyclase 5 Background This gene encodes a member of the membrane-bound adenylyl cyclase enzymes. -

Whole-Genome DNA Methylation and Hydroxymethylation Profiling for HBV-Related Hepatocellular Carcinoma
INTERNATIONAL JOURNAL OF ONCOLOGY 49: 589-602, 2016 Whole-genome DNA methylation and hydroxymethylation profiling for HBV-related hepatocellular carcinoma CHAO YE*, RAN TAO*, QINGYI CAO, DANHUA ZHU, YINI WANG, JIE WANG, JUAN LU, ERMEI CHEN and LANJUAN LI State Key Laboratory for Diagnosis and Treatment of Infectious Diseases, Collaborative Innovation Center for Diagnosis and Treatment of Infectious Diseases, The First Affiliated Hospital, College of Medicine, Zhejiang University, Hangzhou, Zhejiang 310000, P.R. China Received March 18, 2016; Accepted May 13, 2016 DOI: 10.3892/ijo.2016.3535 Abstract. Hepatocellular carcinoma (HCC) is a common tions between them. Taken together, in the present study we solid tumor worldwide with a poor prognosis. Accumulating conducted the first genome-wide mapping of DNA methyla- evidence has implicated important regulatory roles of epigen- tion combined with hydroxymethylation in HBV-related HCC etic modifications in the occurrence and progression of HCC. and provided a series of potential novel epigenetic biomarkers In the present study, we analyzed 5-methylcytosine (5-mC) for HCC. and 5-hydroxymethylcytosine (5-hmC) levels in the tumor tissues and paired adjacent peritumor tissues (APTs) from Introduction four individual HCC patients using a (hydroxy)methylated DNA immunoprecipitation approach combined with deep Hepatocellular carcinoma (HCC), a common solid tumor, is sequencing [(h)MeDIP-Seq]. Bioinformatics analysis revealed the third most frequent cause of cancer-related death in the that the 5-mC levels in the promoter regions of 2796 genes and world. Hepatitis B virus (HBV) infection is the main cause of the 5-hmC levels in 507 genes differed significantly between HCC in China (1). -

Research Article Complex and Multidimensional Lipid Raft Alterations in a Murine Model of Alzheimer’S Disease
SAGE-Hindawi Access to Research International Journal of Alzheimer’s Disease Volume 2010, Article ID 604792, 56 pages doi:10.4061/2010/604792 Research Article Complex and Multidimensional Lipid Raft Alterations in a Murine Model of Alzheimer’s Disease Wayne Chadwick, 1 Randall Brenneman,1, 2 Bronwen Martin,3 and Stuart Maudsley1 1 Receptor Pharmacology Unit, National Institute on Aging, National Institutes of Health, 251 Bayview Boulevard, Suite 100, Baltimore, MD 21224, USA 2 Miller School of Medicine, University of Miami, Miami, FL 33124, USA 3 Metabolism Unit, National Institute on Aging, National Institutes of Health, 251 Bayview Boulevard, Suite 100, Baltimore, MD 21224, USA Correspondence should be addressed to Stuart Maudsley, [email protected] Received 17 May 2010; Accepted 27 July 2010 Academic Editor: Gemma Casadesus Copyright © 2010 Wayne Chadwick et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Various animal models of Alzheimer’s disease (AD) have been created to assist our appreciation of AD pathophysiology, as well as aid development of novel therapeutic strategies. Despite the discovery of mutated proteins that predict the development of AD, there are likely to be many other proteins also involved in this disorder. Complex physiological processes are mediated by coherent interactions of clusters of functionally related proteins. Synaptic dysfunction is one of the hallmarks of AD. Synaptic proteins are organized into multiprotein complexes in high-density membrane structures, known as lipid rafts. These microdomains enable coherent clustering of synergistic signaling proteins.