Second Line Therapy with Axitinib After
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Antitumor Reactivity in Vitro Sorafenib Differentially Affect NK Cell The
The Kinase Inhibitors Sunitinib and Sorafenib Differentially Affect NK Cell Antitumor Reactivity In Vitro This information is current as Matthias Krusch, Julia Salih, Manuela Schlicke, Tina of September 24, 2021. Baessler, Kerstin Maria Kampa, Frank Mayer and Helmut Rainer Salih J Immunol 2009; 183:8286-8294; ; doi: 10.4049/jimmunol.0902404 http://www.jimmunol.org/content/183/12/8286 Downloaded from References This article cites 44 articles, 21 of which you can access for free at: http://www.jimmunol.org/content/183/12/8286.full#ref-list-1 http://www.jimmunol.org/ Why The JI? Submit online. • Rapid Reviews! 30 days* from submission to initial decision • No Triage! Every submission reviewed by practicing scientists • Fast Publication! 4 weeks from acceptance to publication by guest on September 24, 2021 *average Subscription Information about subscribing to The Journal of Immunology is online at: http://jimmunol.org/subscription Permissions Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html Email Alerts Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts The Journal of Immunology is published twice each month by The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 Copyright © 2009 by The American Association of Immunologists, Inc. All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. The Journal of Immunology The Kinase Inhibitors Sunitinib and Sorafenib Differentially Affect NK Cell Antitumor Reactivity In Vitro1 Matthias Krusch,2 Julia Salih,2 Manuela Schlicke,2 Tina Baessler, Kerstin Maria Kampa, Frank Mayer,3 and Helmut Rainer Salih3,4 Sunitinib and Sorafenib are protein kinase inhibitors (PKI) approved for treatment of patients with advanced renal cell cancer (RCC). -

Imatinib-Induced Interstitial Lung Disease and Sunitinib-Associated
CASE Imatinib-induced interstitial lung disease and REPORT sunitinib-associated intra-tumour haemorrhage Herbert H Loong 龍浩鋒 Winnie Yeo 楊明明 An ethnically Chinese patient with newly diagnosed metastatic gastro-intestinal stromal tumour initially treated with imatinib mesylate developed severe interstitial lung disease. As his condition improved after cessation of imatinib mesylate and treatment with corticosteroids, he was started on sunitinib malate. His clinical course was then unfortunately complicated with intra-tumour bleeding. This case report illustrates the dilemmas and complexities associated with treating patients with gastro-intestinal stromal tumours with the new tyrosine kinase inhibitors. Case report A 63-year-old man was referred to our department in January 2007 after being diagnosed with a recurrent gastro-intestinal stromal tumour (GIST). He was initially diagnosed with a duodenal GIST in January 2000 on presenting with symptoms of anaemia. A workup, including upper endoscopy, revealed an ulcerative growth over the third and fourth part of the duodenum. A computed tomographic (CT) scan showed a 4.5 x 5.5 cm soft tissue mass over the same area. A duodenectomy and duodeno-jejunostomy were performed and a pathological examination of tissue removed at surgery confirmed a low-grade GIST (S-100 positive; 4.5 cm in size, mitosis 6/10 high-power field, c-KIT positive). The resection margins were clear so he was managed with routine follow-up and observation. An abdominal ultrasound performed in 2003 showed no evidence of metastases. He remained well until January 2007 when hepatomegaly was found during a physical examination. An abdominal CT scan showed multiple hypervascular tumour foci with cystic changes in both liver lobes. -

The Effects of Combination Treatments on Drug Resistance in Chronic Myeloid Leukaemia: an Evaluation of the Tyrosine Kinase Inhibitors Axitinib and Asciminib H
Lindström and Friedman BMC Cancer (2020) 20:397 https://doi.org/10.1186/s12885-020-06782-9 RESEARCH ARTICLE Open Access The effects of combination treatments on drug resistance in chronic myeloid leukaemia: an evaluation of the tyrosine kinase inhibitors axitinib and asciminib H. Jonathan G. Lindström and Ran Friedman* Abstract Background: Chronic myeloid leukaemia is in principle a treatable malignancy but drug resistance is lowering survival. Recent drug discoveries have opened up new options for drug combinations, which is a concept used in other areas for preventing drug resistance. Two of these are (I) Axitinib, which inhibits the T315I mutation of BCR-ABL1, a main source of drug resistance, and (II) Asciminib, which has been developed as an allosteric BCR-ABL1 inhibitor, targeting an entirely different binding site, and as such does not compete for binding with other drugs. These drugs offer new treatment options. Methods: We measured the proliferation of KCL-22 cells exposed to imatinib–dasatinib, imatinib–asciminib and dasatinib–asciminib combinations and calculated combination index graphs for each case. Moreover, using the median–effect equation we calculated how much axitinib can reduce the growth advantage of T315I mutant clones in combination with available drugs. In addition, we calculated how much the total drug burden could be reduced by combinations using asciminib and other drugs, and evaluated which mutations such combinations might be sensitive to. Results: Asciminib had synergistic interactions with imatinib or dasatinib in KCL-22 cells at high degrees of inhibition. Interestingly, some antagonism between asciminib and the other drugs was present at lower degrees on inhibition. -

The Tyrosine-Kinase Inhibitor Sunitinib Targets Vascular Endothelial (VE)-Cadherin: a Marker of Response to Antitumoural Treatment in Metastatic Renal Cell Carcinoma
www.nature.com/bjc ARTICLE Translational Therapeutics The tyrosine-kinase inhibitor sunitinib targets vascular endothelial (VE)-cadherin: a marker of response to antitumoural treatment in metastatic renal cell carcinoma Helena Polena1, Julie Creuzet1, Maeva Dufies2, Adama Sidibé1, Abir Khalil-Mgharbel1, Aude Salomon1, Alban Deroux3, Jean-Louis Quesada4, Caroline Roelants1, Odile Filhol1, Claude Cochet1, Ellen Blanc5, Céline Ferlay-Segura5, Delphine Borchiellini6, Jean-Marc Ferrero6, Bernard Escudier7, Sylvie Négrier5, Gilles Pages8 and Isabelle Vilgrain1 BACKGROUND: Vascular endothelial (VE)-cadherin is an endothelial cell-specific protein responsible for endothelium integrity. Its adhesive properties are regulated by post-translational processing, such as tyrosine phosphorylation at site Y685 in its cytoplasmic domain, and cleavage of its extracellular domain (sVE). In hormone-refractory metastatic breast cancer, we recently demonstrated that sVE levels correlate to poor survival. In the present study, we determine whether kidney cancer therapies had an effect on VE- cadherin structural modifications and their clinical interest to monitor patient outcome. METHODS: The effects of kidney cancer biotherapies were tested on an endothelial monolayer model mimicking the endothelium lining blood vessels and on a homotypic and heterotypic 3D cell model mimicking tumour growth. sVE was quantified by ELISA in renal cell carcinoma patients initiating sunitinib (48 patients) or bevacizumab (83 patients) in the first-line metastatic setting (SUVEGIL and TORAVA trials). RESULTS: Human VE-cadherin is a direct target for sunitinib which inhibits its VEGF-induced phosphorylation and cleavage on endothelial monolayer and endothelial cell migration in the 3D model. The tumour cell environment modulates VE-cadherin functions through MMPs and VEGF. We demonstrate the presence of soluble VE-cadherin in the sera of mRCC patients (n = 131) which level at baseline, is higher than in a healthy donor group (n = 96). -
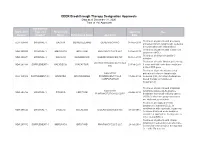
CDER Breakthrough Therapy Designation Approvals Data As of December 31, 2020 Total of 190 Approvals
CDER Breakthrough Therapy Designation Approvals Data as of December 31, 2020 Total of 190 Approvals Submission Application Type and Proprietary Approval Use Number Number Name Established Name Applicant Date Treatment of patients with previously BLA 125486 ORIGINAL-1 GAZYVA OBINUTUZUMAB GENENTECH INC 01-Nov-2013 untreated chronic lymphocytic leukemia in combination with chlorambucil Treatment of patients with mantle cell NDA 205552 ORIGINAL-1 IMBRUVICA IBRUTINIB PHARMACYCLICS LLC 13-Nov-2013 lymphoma (MCL) Treatment of chronic hepatitis C NDA 204671 ORIGINAL-1 SOVALDI SOFOSBUVIR GILEAD SCIENCES INC 06-Dec-2013 infection Treatment of cystic fibrosis patients age VERTEX PHARMACEUTICALS NDA 203188 SUPPLEMENT-4 KALYDECO IVACAFTOR 21-Feb-2014 6 years and older who have mutations INC in the CFTR gene Treatment of previously untreated NOVARTIS patients with chronic lymphocytic BLA 125326 SUPPLEMENT-60 ARZERRA OFATUMUMAB PHARMACEUTICALS 17-Apr-2014 leukemia (CLL) for whom fludarabine- CORPORATION based therapy is considered inappropriate Treatment of patients with anaplastic NOVARTIS lymphoma kinase (ALK)-positive NDA 205755 ORIGINAL-1 ZYKADIA CERITINIB 29-Apr-2014 PHARMACEUTICALS CORP metastatic non-small cell lung cancer (NSCLC) who have progressed on or are intolerant to crizotinib Treatment of relapsed chronic lymphocytic leukemia (CLL), in combination with rituximab, in patients NDA 206545 ORIGINAL-1 ZYDELIG IDELALISIB GILEAD SCIENCES INC 23-Jul-2014 for whom rituximab alone would be considered appropriate therapy due to other co-morbidities -

Nonclinical Antiangiogenesis And
Cancer Therapy: Preclinical Nonclinical Antiangiogenesis and Antitumor Activities of Axitinib (AG-013736), an Oral, Potent, and Selective Inhibitor of Vascular Endothelial Growth Factor Receptor Tyrosine Kinases 1, 2, 3 Dana D. Hu-Lowe, Helen Y.Zou, Maren L. Grazzini, Max E. Hallin, Grant R. Wickman, Karin Amundson, JeffreyH.Chen,DavidA.Rewolinski,ShinjiYamazaki,EllenY.Wu,MicheleA.McTigue,BrionW.Murray, Robert S. Kania, Patrick O’Connor, David R. Shalinsky, and Steve L. Bender Abstract Purpose: Axitinib (AG-013736) is a potent and selective inhibitor of vascular endothelial growth factor (VEGF) receptor tyrosine kinases 1to 3 that is in clinical development for the treatment of solid tumors. We provide a comprehensive description of its in vitro characteristics and activities, in vivo antiangiogenesis, and antitumor efficacy and translational pharmacology data. Experimental Design: The potency, kinase selectivity, pharmacologic activity, and antitumor efficacy of axitinib were assessed in various nonclinical models. Results: Axitinib inhibitscellular autophosphorylation of VEGF receptors(VEGFR) with picomo- lar IC50 values. Counterscreening across multiple kinase and protein panels shows it is selective for VEGFRs. Axitinib blocks VEGF-mediated endothelial cell survival, tube formation, and down- stream signaling through endothelial nitric oxide synthase, Akt and extracellular signal-regulated kinase. Following twice daily oral administration, axitinib produces consistent and dose-depen- dent antitumor efficacy that is associated with blocking VEGFR-2 phosphorylation, vascular per- meability, angiogenesis, and concomitant induction of tumor cell apoptosis. Axitinib in combination with chemotherapeutic or targeted agentsenhancesantitumor efficacy in many tu- mor models compared with single agent alone. Dose scheduling studies in a human pancreatic tumor xenograft model show that simultaneous administration of axitinib and gemcitabine with- out prolonged dose interruption or truncation of axitinib produces the greatest antitumor efficacy. -

Study Protocol);
AG-013736, PF-02341066 A4061068 Final Protocol Amendment 2, 27 January 2016 CLINICAL PROTOCOL A PHASE 1B, OPEN LABEL, DOSE ESCALATION STUDY TO EVALUATE SAFETY, PHARMACOKINETICS AND PHARMACODYNAMICS OF AXITINIB (AG-013736) IN COMBINATION WITH CRIZOTINIB (PF-02341066) IN PATIENTS WITH ADVANCED SOLID TUMORS Compounds: AG-013736, PF-02341066 Compound Names: axitinib, crizotinib United States (US) Investigational New IND 63,662 Drug (IND) Numbers: IND 73,544 European Clinical Trials Database 2015-001724-31 (EudraCT) Number Protocol Number: A4061068 Phase: 1b Page 1 AG-013736, PF-02341066 A4061068 Final Protocol Amendment 2, 27 January 2016 Document History Document Version Date Summary of Changes and Rationale Amendment 2 26 January 2016 Added EudraCT number. SCHEDULE OF ACTIVITIES: - Contraception check added to align with the Sponsor’s most recent protocol template. - Registration and Study Treatment: updated to clarify which patient subgroup will receive axitinib single agent during a 7-day Lead-In period and which subgroup will start with the combination without the Lead-In period. - Archival Tumor Tissue, De Novo Tumor Biopsy: footnotes updated to align with Patient Selection Section, Inclusion Criterion #1. Section 1. Introduction: literature updated; axitinib and crizotinib safety data updated according to the last version of the Investigator’s Brochure. Section 4. Patient Selection: - Inclusion Criterion #1, Dose Expansion Phase: language updated: 1. to make the selected patient population more in line with the actual 2nd and 3rd line advanced RCC population; 2. to include alternative option for the collection of biopsy in the Dose Expansion Cohort 2 patients. - Exclusion Criterion #8: language updated to align with the current standard language of crizotinib clinical protocols. -

Sunitinib Malate)
Prescribing Information Update for SUTENT® (sunitinib malate) July 12, 2010 Dear Health Care Provider: Pfizer Oncology is committed to providing you with up-to-date information about SUTENT® (sunitinib malate) capsules. This letter is to inform you of an important update to the SUTENT prescribing information (PI). The following boxed warning and safety information has been added to the PI for SUTENT: WARNING: HEPATOTOXICITY Hepatotoxicity has been observed in clinical trials and post-marketing experience. This hepatotoxicity may be severe and deaths have been reported. WARNINGS and PRECAUTIONS Hepatotoxicity SUTENT has been associated with hepatotoxicity, which may result in liver failure or death. Liver failure has been observed in clinical trials (7/2281 [0.3%]) and post-marketing experience. Liver failure signs include jaundice, elevated transaminases and/or hyperbilirubinemia in conjunction with encephalopathy, coagulopathy, and/or renal failure. Monitor liver function tests (ALT, AST, bilirubin) before initiation of treatment, during each cycle of treatment, and as clinically indicated. SUTENT should be interrupted for Grade 3 or 4 drug-related hepatic adverse events and discontinued if there is no resolution. Do not restart SUTENT if patients subsequently experience severe changes in liver function tests or have other signs and symptoms of liver failure. Safety in patients with ALT or AST >2.5 × ULN or, if due to liver metastases, >5.0 × ULN has not been established. In addition, the labeling includes a new Medication Guide that your patients will receive when SUTENT is dispensed. Pfizer maintains a global safety database, monitoring all clinical trials and reports of spontaneous adverse events. The incidence of liver failure referenced above is consistent with the very low rate of hepatic failure described in the clinical trials of sunitinib used to support original FDA registration in 2006. -

Mechanism of Myeloid-Derived Suppressor Cell
MECHANISM OF MYELOID-DERIVED SUPPRESSOR CELL ACCUMULATION IN CANCER AND SUSCEPTIBILITY TO REVERSAL BY SUNITINIB by JENNIFER SUSAN KO, M.D. Submitted in partial fulfillment of the requirements For the degree of Doctor of Philosophy Thesis Adviser: Dr. James H. Finke Department of Pathology CASE WESTERN RESERVE UNIVERSITY January, 2010 CASE WESTERN RESERVE UNIVERSITY SCHOOL OF GRADUATE STUDIES We hereby approve the thesis of Jennifer Susan Ko candidate for the Doctor of Philosophy degree*. (signed) Alan Levine Ph.D. David Kaplan M.D., Ph.D. Clark Distelhorst M.D. James Finke Ph.D. Charles Tannenbaum Ph.D. (date) October 12th, 2009 *We also certify that written approval has been obtained for any proprietary material contained therein. 2 TABLE OF CONTENTS Title Page 1 Signature Sheet 2 Table of Contents 3 List of Tables 6 List of Figures 7 Acknowledgements 9 List of Abbreviations 10 Abstract 14 Chapter 1: Introduction 16 Overview: Myeloid-derived suppressor cells in cancer: a novel therapeutic target. 16 Immunotherapy in cancer 16 Myeloid-derived suppressor cells limit immunotherapy 22 Myeloid-derived suppressor cells limit anti-angiogenic therapy 28 Multiple factors are implicated in MDSC formation 30 Vascular Endothelial Growth Factor 30 Stem Cell Factor 32 Granulocyte- and Granulocyte/Monocyte Colony Stimulating Factors 33 S100A9 and Inflammation 34 Intracellular signaling implicated in MDSC programming 36 3 Chapter 2: Sunitinib Mediates Reversal of Myeloid-Derived Suppressor Cell Accumulation in Renal Cell Carcinoma Patients 44 Statement -

In Vitro Kinetic Characterization of Axitinib Metabolism S
Supplemental material to this article can be found at: http://dmd.aspetjournals.org/content/suppl/2015/10/28/dmd.115.065615.DC1 1521-009X/44/1/102–114$25.00 http://dx.doi.org/10.1124/dmd.115.065615 DRUG METABOLISM AND DISPOSITION Drug Metab Dispos 44:102–114, January 2016 Copyright ª 2015 by The American Society for Pharmacology and Experimental Therapeutics In Vitro Kinetic Characterization of Axitinib Metabolism s Michael A. Zientek, Theunis C. Goosen, Elaine Tseng, Jian Lin, Jonathan N. Bauman, Gregory S. Walker, Ping Kang, Ying Jiang, Sascha Freiwald, David Neul, and Bill J. Smith Pharmacokinetics, Pharmacodynamics, and Drug Metabolism, Pfizer Inc., San Diego, California (M.A.Z, P.K., Y.J, S.F., D.N, B.J.S.); and Pharmacokinetics, Pharmacodynamics, and Drug Metabolism, Pfizer Inc., Groton, Connecticut (T.C.G., E.T., J.L., J.N.B, G.S.W.) Received May 26, 2015; accepted October 27, 2015 ABSTRACT N-Methyl-2-[3-((E)-2-pyridin-2-yl-vinyl)-1H-indazol-6-ylsulfanyl]- predominately metabolized by CYP3A4/5, with minor contributions benzamide (axitinib) is an oral inhibitor of vascular endothelial from CYP2C19 and CYP1A2. The apparent substrate concentration at growth factor receptors 1–3, which is approved for the treatment half-maximal velocity (Km)andVmax values for the formation of axitinib Downloaded from of advanced renal cell cancer. Human [14C]-labeled clinical studies sulfoxide by CYP3A4 or CYP3A5 were 4.0 or 1.9 mMand9.6or indicate axitinib’s primary route of clearance is metabolism. The 1.4 pmol·min21·pmol21, respectively. Using a CYP3A4-specific inhibitor aims of the in vitro experiments presented herein were to identify (Cyp3cide) in liver microsomes expressing CYP3A5, 66% of the and characterize the enzymes involved in axitinib metabolic clear- axitinib intrinsic clearance was attributable to CYP3A4 and 15% to ance. -

(ALK) Rearrangement in Adult Renal Cell Carcinoma with Lung Metastasis: a Case Report and Literature Review
2861 Case Report Anaplastic lymphoma kinase (ALK) rearrangement in adult renal cell carcinoma with lung metastasis: a case report and literature review Shengyu Zhou1, Guanxing Sun2, Jianwei Wang1, Hongtu Zhang1 1Department of Medical Oncology, National Cancer Center/National Clinical Research Center for Cancer/Cancer Hospital, Chinese Academy of Medical Sciences (CAMS) and Peking Union Medical College (PUMC), Beijing, China; 2Department of Medical Oncology, Zaozhuang Municipal Hospital, Zaozhuang, China Correspondence to: Shengyu Zhou. Department of Medical Oncology, National Cancer Center/National Clinical Research Center for Cancer/Cancer Hospital, Chinese Academy of Medical Sciences (CAMS) and Peking Union Medical College (PUMC), Beijing 100021, China. Email: [email protected]. Abstract: Renal cell carcinoma (RCC) with anaplastic lymphoma kinase (ALK) rearrangement is rare, and the genetic profiles of the tumor have not been elucidated. Here, we report a case with recurrent papillary RCC and lung metastasis after nephrectomy for nearly 7 years. The patient first received sunitinib, whereas the drug toxicity was intolerable. Combined Immunohistology (IHC) and fluorescence in situ hybridization (FISH) revealed the patient has an ALK rearrangement, and the patient then was treated with crizotinib. The patient had good tolerance, and a partial response in the target lesions was achieved. In order to further understand the benefit of crizotinib in ALK-rearranged RCC, the patient was detected with whole exome sequencing (WES) to study her genetic profiles. Compared those of RCC cases without ALK rearrangement (nALK-RCC), the patient and nine RCC cases with ALK rearrangement (ALK-RCC) revealed unique genetic characteristics: 1) The common mutations that occurred in RCC were not found in ALK-RCC.; 2) A total of 11 co-existing mutations in ALK-RCC were found, and they occurred in nALK-RCC at a relatively low frequency. -

Tyrosine Kinase Inhibitors Significantly Improved Survival Outcomes in Patients with Metastatic Gastrointestinal Stromal Tumour: a Multi-Institutional Cohort Study
ORIGINAL ARTICLE Tyrosine kinase inhibitors significantly improved survival outcomes in patients with metastatic gastrointestinal stromal tumour: a multi-institutional cohort study † ‡ A. Deruchie Tan BSc,* K. Willemsma BSc,* A. MacNeill MD, K. DeVries MSc, A. Srikanthan MD MHSc,* ‡ † § C. McGahan MSc, T. Hamilton MD, H. Li BSc,* C.D. Blanke MD, and C.E. Simmons MD MSc* ABSTRACT Background The real-world impact of tyrosine kinase inhibitors (TKIs) in clinical practice for gastrointestinal stromal tumour (GIST) has not been extensively reported. We sought to assess how outcomes have changed over the eras and to evaluate the effect of access to imatinib and sunitinib on survival in patients with unresectable or metastatic GIST in British Columbia. Methods Patients with metastatic or unresectable GIST were allocated to one of three eras: pre-2002, 2002–2007, and post-2007 based on treatment availability (pre-imatinib, post-imatinib, and post-sunitinib). Overall survival (OS) and progression-free survival (PFS) were compared between eras. Univariate and multivariate analyses were performed to determine the effects of tumour, patient, and treatment characteristics on survival outcomes. Results Of 657 patients diagnosed with GIST throughout British Columbia during 1996–2016, 196 had metastatic disease: 23 in the pre-imatinib era, 67 in the post-imatinib era, and 106 in the post-sunitinib era. A significant increase in OS, by 53.6 months (p = 0.0007), and PFS, by 29.1 months (p = 0.044), was observed after the introduction of imatinib. The introduction of sunitinib did not significantly affect OS or PFS. Conclusions Implementation of TKIs has drastically improved survival outcomes for patients with metastatic GIST by up to 4.55 years in the real-world setting.