Study Protocol);
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

A Novel Mechanism of Crizotinib Resistance in a ROS1+ NSCLC Patient 11 April 2016
A novel mechanism of crizotinib resistance in a ROS1+ NSCLC patient 11 April 2016 Molecular analysis of a tumor biopsy from a proto- fusion gene in the crizotinib resistant tumor samples oncogene 1 receptor tyrosine kinase positive compared to the pretreatment tumor samples by (ROS1+) patient with acquired crizotinib resistance DNA sequencing or FISH analysis. SNaPshot revealed a novel mutation in the v-kit Hardy analysis of the crizotinib resistant tumor identified a Zuckerman 4 feline sarcoma viral oncogene novel mutation in the KIT gene encoding the amino homolog receptor tyrosine kinase (KIT) that can acid substitution, pD816G. The drug ponatinib, a potentially be targeted by KIT inhibitors. KIT tyrosine kinase inhibitor, demonstrated inhibition of KITD816G kinase activity. Further, in Chromosomal rearrangements of the gene ROS1+ cells expressing KITD816G the addition of encoding ROS1 in approximately 1-2% of non- ponatinib resensitized cells to crizotinib. small cell lung cancers (NSCLC). Treatment of ROS1+ patients with crizotinib, a small-molecule The authors comment that, "Although our results tyrosine kinase inhibitor, often results in durable demonstrate that ponatinib can overcome KIT- tumor regression. However, despite initial mediated resistance in vitro, it remains unknown treatment success patients typically develop whether ponatinib can overcome this or other KIT resistance to crizotinib and disease progression activating mutations in patients. Detection of KIT inevitably ensues. Understanding the mechanism mutations may allow enrollment of patients with of resistance to crizotinib and identifying new ROS1+ cancer (or other oncogenes), onto clinical targets for therapy will help guide patient trials of KIT inhibitors, however it is likely that dual treatment. -

Predicting Cardiac Risk of Anti-Cancer Drugs
PREDICTING CARDIAC RISK OF ANTI-CANCER DRUGS: A ROLE FOR HUMAN INDUCED PLURIPOTENT STEM CELL-DERIVED CARDIOMYOCYTES Andrew Bruening-Wright, Leslie Ellison, James Kramer, Carlos A. Obejero-Paz Charles River, Cleveland 1 ABSTRACT 3 METHODS 1) The Field Potential and Impedance signals Cardiotoxicity is a major complication of many anti-cancer drugs. Acute effects on cardiac ion channels alter cardiac excitability and induce arrhythmias and ultimately heart failure can develop during chronic treatment. Current in vitro strategies for detecting these risks are minimal and often ineffective, particularly for effects that occur over the course of days or weeks. We aimed to validate a human We used the xCELLigence RTCA CardioECR instrument (ACEA Biosciences) to record impedance and extracellular field A B C cell-based assay that is fast, robust, and predictive of both acute and chronic clinical outcomes. Currently marketed chemotherapeutic agents were tested on the CDI-CardioECR system (CDI/Fujifilm- 2 a b ACEA Biosciences). Cardiomyocytes were exposed for eight days to doxorubicin and various tyrosine kinase inhibitors (erlotinib, lapatinib, nilotinib, sunitinib, and crizotinib) at concentrations comparable potentials. iCell cardiomyocytes , from Cellular Dynamics International/FUJIFILM. Spontaneous twitch activity was recorded for to clinical plasma values. Recordings were made at multiple time points each day and data was analyzed using proprietary algorithms written in VSA and Matlab. Drugs with hERG channel block liability two 48 well plates. Analysis was performed using Origin, Matlab and macros written in VBA. The output of the instrument is the (lapatinib, nilotinib, sunitinib and crizotinib) showed a dose dependent delay in repolarization and an increase in dysrhythmic markers. -

The Effects of Combination Treatments on Drug Resistance in Chronic Myeloid Leukaemia: an Evaluation of the Tyrosine Kinase Inhibitors Axitinib and Asciminib H
Lindström and Friedman BMC Cancer (2020) 20:397 https://doi.org/10.1186/s12885-020-06782-9 RESEARCH ARTICLE Open Access The effects of combination treatments on drug resistance in chronic myeloid leukaemia: an evaluation of the tyrosine kinase inhibitors axitinib and asciminib H. Jonathan G. Lindström and Ran Friedman* Abstract Background: Chronic myeloid leukaemia is in principle a treatable malignancy but drug resistance is lowering survival. Recent drug discoveries have opened up new options for drug combinations, which is a concept used in other areas for preventing drug resistance. Two of these are (I) Axitinib, which inhibits the T315I mutation of BCR-ABL1, a main source of drug resistance, and (II) Asciminib, which has been developed as an allosteric BCR-ABL1 inhibitor, targeting an entirely different binding site, and as such does not compete for binding with other drugs. These drugs offer new treatment options. Methods: We measured the proliferation of KCL-22 cells exposed to imatinib–dasatinib, imatinib–asciminib and dasatinib–asciminib combinations and calculated combination index graphs for each case. Moreover, using the median–effect equation we calculated how much axitinib can reduce the growth advantage of T315I mutant clones in combination with available drugs. In addition, we calculated how much the total drug burden could be reduced by combinations using asciminib and other drugs, and evaluated which mutations such combinations might be sensitive to. Results: Asciminib had synergistic interactions with imatinib or dasatinib in KCL-22 cells at high degrees of inhibition. Interestingly, some antagonism between asciminib and the other drugs was present at lower degrees on inhibition. -

Tyrosine Kinase Inhibitors Or ALK Inhibitors for the First Line Treatment of Non-Small Cell Lung Cancer
Tyrosine kinase inhibitors or ALK inhibitors for the first line treatment of Non-small cell lung cancer This application seeks the addition of tyrosine kinase inhibitor erlotinib (representative of class) and gefitinib and afatinib (alternatives) as well as ALK-inhibitor crizotinib to the list of the Essential Medicines List for the treatment of non-small cell lung cancer. Introduction In 2013, there were approximately 1.8 million incident lung cancer cases diagnosed worldwide and approximately 1.6 million deaths from the disease (1). Lung cancer had the second highest absolute incidence globally after breast cancer, and in 93 countries was the leading cause of death from malignant disease, accounting for one fifth of the total global burden of disability- adjusted life years from cancer. Men were more likely to develop lung cancer than women, with 1 in 18 men and 1 in 51 women being diagnosed between birth and age 79 years (1). Non-small cell lung cancer (NSCLC) is the most common form of the disease, accounting for 85–90% of all lung cancers (2)(43). For patients with resectable disease, adjuvant chemotherapy improves the absolute 5-year survival rates in Stage II and III NSCLC (9,13,65,44-47). Acceptable adjuvant chemotherapy options include etoposide/cisplatin, docetaxel/cisplatin, gemcitabine/cisplatin, pemetrexed/cisplatin, and carboplatin/paclitaxel for patients with comorbidities or unable to tolerate cisplatin. In patients with non-metastatic but inoperable NSCLC or Stage III disease, concurrent chemoradiotherapy has been shown to improve overall survival (OS) and median survival (47-53). However, most patients with NSCLC present with advanced stage disease – stage IV in particular – and half of all patients treated initially for potentially curable early-stage disease will experience recurrences with metastatic disease (3). -
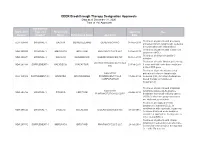
CDER Breakthrough Therapy Designation Approvals Data As of December 31, 2020 Total of 190 Approvals
CDER Breakthrough Therapy Designation Approvals Data as of December 31, 2020 Total of 190 Approvals Submission Application Type and Proprietary Approval Use Number Number Name Established Name Applicant Date Treatment of patients with previously BLA 125486 ORIGINAL-1 GAZYVA OBINUTUZUMAB GENENTECH INC 01-Nov-2013 untreated chronic lymphocytic leukemia in combination with chlorambucil Treatment of patients with mantle cell NDA 205552 ORIGINAL-1 IMBRUVICA IBRUTINIB PHARMACYCLICS LLC 13-Nov-2013 lymphoma (MCL) Treatment of chronic hepatitis C NDA 204671 ORIGINAL-1 SOVALDI SOFOSBUVIR GILEAD SCIENCES INC 06-Dec-2013 infection Treatment of cystic fibrosis patients age VERTEX PHARMACEUTICALS NDA 203188 SUPPLEMENT-4 KALYDECO IVACAFTOR 21-Feb-2014 6 years and older who have mutations INC in the CFTR gene Treatment of previously untreated NOVARTIS patients with chronic lymphocytic BLA 125326 SUPPLEMENT-60 ARZERRA OFATUMUMAB PHARMACEUTICALS 17-Apr-2014 leukemia (CLL) for whom fludarabine- CORPORATION based therapy is considered inappropriate Treatment of patients with anaplastic NOVARTIS lymphoma kinase (ALK)-positive NDA 205755 ORIGINAL-1 ZYKADIA CERITINIB 29-Apr-2014 PHARMACEUTICALS CORP metastatic non-small cell lung cancer (NSCLC) who have progressed on or are intolerant to crizotinib Treatment of relapsed chronic lymphocytic leukemia (CLL), in combination with rituximab, in patients NDA 206545 ORIGINAL-1 ZYDELIG IDELALISIB GILEAD SCIENCES INC 23-Jul-2014 for whom rituximab alone would be considered appropriate therapy due to other co-morbidities -

Newer-Generation EGFR Inhibitors in Lung Cancer: How Are They Best Used?
cancers Review Newer-Generation EGFR Inhibitors in Lung Cancer: How Are They Best Used? Tri Le 1 and David E. Gerber 1,2,3,* 1 Department of Internal Medicine, University of Texas Southwestern Medical Center, Dallas, TX 75390-8852, USA; [email protected] 2 Department of Clinical Sciences, University of Texas Southwestern Medical Center, Dallas, TX 75390-8852, USA 3 Division of Hematology-Oncology, Harold C. Simmons Comprehensive Cancer Center, University of Texas Southwestern Medical Center, Dallas, TX 75390-8852, USA * Correspondence: [email protected]; Tel.: +1-214-648-4180; Fax: +1-214-648-1955 Received: 15 January 2019; Accepted: 4 March 2019; Published: 15 March 2019 Abstract: The FLAURA trial established osimertinib, a third-generation epidermal growth factor receptor (EGFR) tyrosine kinase inhibitor (TKI), as a viable first-line therapy in non-small cell lung cancer (NSCLC) with sensitizing EGFR mutations, namely exon 19 deletion and L858R. In this phase 3 randomized, controlled, double-blind trial of treatment-naïve patients with EGFR mutant NSCLC, osimertinib was compared to standard-of-care EGFR TKIs (i.e., erlotinib or gefinitib) in the first-line setting. Osimertinib demonstrated improvement in median progression-free survival (18.9 months vs. 10.2 months; hazard ratio 0.46; 95% CI, 0.37 to 0.57; p < 0.001) and a more favorable toxicity profile due to its lower affinity for wild-type EGFR. Furthermore, similar to later-generation anaplastic lymphoma kinase (ALK) inhibitors, osimertinib has improved efficacy against brain metastases. Despite this impressive effect, the optimal sequencing of osimertinib, whether in the first line or as subsequent therapy after the failure of earlier-generation EGFR TKIs, is not clear. -

ALK Tyrosine Kinase Inhibitors, 5.01.538
PHARMACY POLICY – 5.01.538 ALK Tyrosine Kinase Inhibitors Effective Date: June 1, 2021 RELATED MEDICAL POLICIES: Last Revised: May 20, 2021 None Replaces: N/A Select a hyperlink below to be directed to that section. POLICY CRITERIA | CODING | RELATED INFORMATION EVIDENCE REVIEW | REFERENCES | HISTORY ∞ Clicking this icon returns you to the hyperlinks menu above. Introduction The anaplastic lymphoma kinase (ALK) gene provides instructions for making a specific kind of protein called ALK receptor tyrosine kinase. This protein helps cells communicate. When this gene is damaged, cell growth can get stuck in the “on” position and cells grow uncontrollably. Changes to the ALK gene can lead to non-small-cell lung cancer. Tyrosine kinase inhibitors block specific enzymes, essentially working to turn the cell growth to the “off” position. ALK tyrosine kinase inhibitors specifically targets cancers caused by changes to the ALK gene. This policy describes when this specific form of chemotherapy may be considered medically necessary. Note: The Introduction section is for your general knowledge and is not to be taken as policy coverage criteria. The rest of the policy uses specific words and concepts familiar to medical professionals. It is intended for providers. A provider can be a person, such as a doctor, nurse, psychologist, or dentist. A provider also can be a place where medical care is given, like a hospital, clinic, or lab. This policy informs them about when a service may be covered. Policy Coverage Criteria Drug Medical Necessity Alecensa® (alectinib) Alecensa® (alectinib) may be considered medically necessary for the treatment of adult patients with advanced or Drug Medical Necessity metastatic non-small cell lung cancer (NSCLC) that is anaplastic lymphoma kinase (ALK)-positive. -

Nonclinical Antiangiogenesis And
Cancer Therapy: Preclinical Nonclinical Antiangiogenesis and Antitumor Activities of Axitinib (AG-013736), an Oral, Potent, and Selective Inhibitor of Vascular Endothelial Growth Factor Receptor Tyrosine Kinases 1, 2, 3 Dana D. Hu-Lowe, Helen Y.Zou, Maren L. Grazzini, Max E. Hallin, Grant R. Wickman, Karin Amundson, JeffreyH.Chen,DavidA.Rewolinski,ShinjiYamazaki,EllenY.Wu,MicheleA.McTigue,BrionW.Murray, Robert S. Kania, Patrick O’Connor, David R. Shalinsky, and Steve L. Bender Abstract Purpose: Axitinib (AG-013736) is a potent and selective inhibitor of vascular endothelial growth factor (VEGF) receptor tyrosine kinases 1to 3 that is in clinical development for the treatment of solid tumors. We provide a comprehensive description of its in vitro characteristics and activities, in vivo antiangiogenesis, and antitumor efficacy and translational pharmacology data. Experimental Design: The potency, kinase selectivity, pharmacologic activity, and antitumor efficacy of axitinib were assessed in various nonclinical models. Results: Axitinib inhibitscellular autophosphorylation of VEGF receptors(VEGFR) with picomo- lar IC50 values. Counterscreening across multiple kinase and protein panels shows it is selective for VEGFRs. Axitinib blocks VEGF-mediated endothelial cell survival, tube formation, and down- stream signaling through endothelial nitric oxide synthase, Akt and extracellular signal-regulated kinase. Following twice daily oral administration, axitinib produces consistent and dose-depen- dent antitumor efficacy that is associated with blocking VEGFR-2 phosphorylation, vascular per- meability, angiogenesis, and concomitant induction of tumor cell apoptosis. Axitinib in combination with chemotherapeutic or targeted agentsenhancesantitumor efficacy in many tu- mor models compared with single agent alone. Dose scheduling studies in a human pancreatic tumor xenograft model show that simultaneous administration of axitinib and gemcitabine with- out prolonged dose interruption or truncation of axitinib produces the greatest antitumor efficacy. -

Managing Treatment–Related Adverse Events Associated with Alk Inhibitors
Curr Oncol, Vol. 21, pp. 19-26; doi: http://dx.doi.org/10.3747/co.21.1740 MANAGING TREATMENT–RELATEDORIGINAL AEs ASSOCIATED WITH ALKARTICLE INHIBITORS Managing treatment–related adverse events associated with Alk inhibitors J.M. Rothenstein MD* and † N. Letarte BPharm MSc BCOP ABSTRACT ALK had previously been identified in subsets of anaplastic large-cell lymphomas3 and inflammatory Anaplastic lymphoma kinase (ALK) rearrangements myofibroblastic tumours4, its identification inNSCLC have been identified as key oncogenic drivers in a was what prompted the investigation of Alk inhibi- small subset of non-small-cell lung cancers (NSCLCs). tion as a therapeutic strategy. Small-molecule Alk kinase inhibitors such as crizo- Roughly 4% of nonsquamous NSCLC is ALK- tinib have transformed the natural history of NSCLC driven. Given the prevalence of NSCLC, estimates for this subgroup of patients. Because of the preva- suggest that several hundred patients with advanced lence of NSCLC, ALK-positive patients represent an ALK-positive NSCLC will be diagnosed annually in important example of the paradigm for personalized Canada5. In bringing a new class of therapeutics into medicine. Although Alk inhibitors such as crizotinib the clinic, it is essential that the multidisciplinary are well tolerated, there is a potential for adverse team be familiar with management of the AEs that can events to occur. Proactive monitoring, treatment, arise—especially in the case of a therapy that will and education concerning those adverse events will be used in a very specific subgroup of patients and help to optimize the therapeutic index of the drugs. with which clinicians may have limited experience6. -

A Review on Newer Tyrosine Kinase Inhibitors and Their Uses Oncology Section Oncology
DOI: 10.7860/JCDR/2018/31031.11957 Review Article A Review on Newer Tyrosine Kinase Inhibitors and their Uses Oncology Section Oncology NITHU M KUMAR1, MEENU MATHEW2, KN ANILA3, S PRIYANKA4 ABSTRACT Tyrosine Kinase Inhibitors (TKI) can reversibly or irreversibly block the signaling pathway occurring in the extracellular part of the receptor by inhibiting Tyrosine Kinase (TK) phosphorylation. This review included the drugs that were newly marketed or drugs with newer approved uses after 2015, such as Gefitinib, Osimertinib, Crizotinib, Alectinib, Ibrutinib, Cabozantinib. Brigatinib and Lorlatinib are investigational drugs that have not been approved and have shown promising results in trials for the treatment of Anaplastic Lymphoma Kinase (ALK) positive metastatic Non Small Cell Lung Carcinoma (NSCLC). Gefitinib, Osimertinib, Crizotinib, Alectinib were approved for treating NSCLC. Cabozantinib and Lenvatinib were approved for treating renal cell carcinoma and thyroid carcinoma. Ibrutinib was approved for treatment of Chronic Lymphocytic Leukaemia, Small Lymphocytic Lymphoma, Waldenström macroglobulinemia, previously treated Mantle cell lymphoma and relapsed or refractory Marginal zone lymphoma. TKI have promising efficacy in treating a wide range of oncologic diseases. Hand-foot-skin reaction are the most common side effect of drugs in this category, however, TKI are found to have relatively fewer side effects compared to other anti cancer drugs. Keywords: Anaplastic lymphoma kinase, Bruton's tyrosine kinase inhibitor, Epidermal growth factor receptor inhibitor, Non small cell lung carcinoma, Vascular endothelial growth factor INTRODUCTION In this review we have given a generalized insight into the anti Cancer kinome is now recognized as potential target for treating cancer activity, mechanism of action, and adverse drug reaction of cancer and comprise of more than 500 members where only few TK whose clinical activity have been fairly understood. -

In Vitro Kinetic Characterization of Axitinib Metabolism S
Supplemental material to this article can be found at: http://dmd.aspetjournals.org/content/suppl/2015/10/28/dmd.115.065615.DC1 1521-009X/44/1/102–114$25.00 http://dx.doi.org/10.1124/dmd.115.065615 DRUG METABOLISM AND DISPOSITION Drug Metab Dispos 44:102–114, January 2016 Copyright ª 2015 by The American Society for Pharmacology and Experimental Therapeutics In Vitro Kinetic Characterization of Axitinib Metabolism s Michael A. Zientek, Theunis C. Goosen, Elaine Tseng, Jian Lin, Jonathan N. Bauman, Gregory S. Walker, Ping Kang, Ying Jiang, Sascha Freiwald, David Neul, and Bill J. Smith Pharmacokinetics, Pharmacodynamics, and Drug Metabolism, Pfizer Inc., San Diego, California (M.A.Z, P.K., Y.J, S.F., D.N, B.J.S.); and Pharmacokinetics, Pharmacodynamics, and Drug Metabolism, Pfizer Inc., Groton, Connecticut (T.C.G., E.T., J.L., J.N.B, G.S.W.) Received May 26, 2015; accepted October 27, 2015 ABSTRACT N-Methyl-2-[3-((E)-2-pyridin-2-yl-vinyl)-1H-indazol-6-ylsulfanyl]- predominately metabolized by CYP3A4/5, with minor contributions benzamide (axitinib) is an oral inhibitor of vascular endothelial from CYP2C19 and CYP1A2. The apparent substrate concentration at growth factor receptors 1–3, which is approved for the treatment half-maximal velocity (Km)andVmax values for the formation of axitinib Downloaded from of advanced renal cell cancer. Human [14C]-labeled clinical studies sulfoxide by CYP3A4 or CYP3A5 were 4.0 or 1.9 mMand9.6or indicate axitinib’s primary route of clearance is metabolism. The 1.4 pmol·min21·pmol21, respectively. Using a CYP3A4-specific inhibitor aims of the in vitro experiments presented herein were to identify (Cyp3cide) in liver microsomes expressing CYP3A5, 66% of the and characterize the enzymes involved in axitinib metabolic clear- axitinib intrinsic clearance was attributable to CYP3A4 and 15% to ance. -

The New-Generation Selective ROS1/NTRK Inhibitor DS-6051B Overcomes Crizotinib Resistant ROS1- G2032R Mutation in Preclinical Models
ARTICLE https://doi.org/10.1038/s41467-019-11496-z OPEN The new-generation selective ROS1/NTRK inhibitor DS-6051b overcomes crizotinib resistant ROS1- G2032R mutation in preclinical models Ryohei Katayama 1, Bo Gong1,2, Noriko Togashi 3, Masaya Miyamoto3, Masaki Kiga3, Shiho Iwasaki3, Yasuki Kamai3, Yuichi Tominaga3, Yasuyuki Takeda3, Yoshiko Kagoshima3, Yuki Shimizu1,2, Yosuke Seto1, Tomoko Oh-hara1, Sumie Koike1, Naoki Nakao4, Hiroyuki Hanzawa4, Kengo Watanabe 3, Satoshi Yoda 5,6, Noriko Yanagitani7, Aaron N. Hata5,6, Alice T. Shaw5,6, Makoto Nishio7, Naoya Fujita1,2 & Takeshi Isoyama 3 1234567890():,; ROS1 gene rearrangement was observed in around 1–2 % of NSCLC patients and in several other cancers such as cholangiocarcinoma, glioblastoma, or colorectal cancer. Crizotinib, an ALK/ROS1/MET inhibitor, is highly effective against ROS1-rearranged lung cancer and is used in clinic. However, crizotinib resistance is an emerging issue, and several resistance mechanisms, such as secondary kinase-domain mutations (e.g., ROS1-G2032R) have been identified in crizotinib-refractory patients. Here we characterize a new selective ROS1/NTRK inhibitor, DS-6051b, in preclinical models of ROS1- or NTRK-rearranged cancers. DS-6051b induces dramatic growth inhibition of both wild type and G2032R mutant ROS1–rearranged cancers or NTRK-rearranged cancers in vitro and in vivo. Here we report that DS-6051b is effective in treating ROS1- or NTRK-rearranged cancer in preclinical models, including crizotinib-resistant ROS1 positive cancer with secondary kinase domain mutations especially G2032R mutation which is highly resistant to crizotinib as well as lorlatinib and entrectinib, next generation ROS1 inhibitors. 1 Division of Experimental Chemotherapy, Cancer Chemotherapy Center, Japanese Foundation for Cancer Research, Tokyo 135-8550, Japan.