Neoadjuvant Combination of Pazopanib Or Axitinib And
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Horizon Scanning Status Report June 2019
Statement of Funding and Purpose This report incorporates data collected during implementation of the Patient-Centered Outcomes Research Institute (PCORI) Health Care Horizon Scanning System, operated by ECRI Institute under contract to PCORI, Washington, DC (Contract No. MSA-HORIZSCAN-ECRI-ENG- 2018.7.12). The findings and conclusions in this document are those of the authors, who are responsible for its content. No statement in this report should be construed as an official position of PCORI. An intervention that potentially meets inclusion criteria might not appear in this report simply because the horizon scanning system has not yet detected it or it does not yet meet inclusion criteria outlined in the PCORI Health Care Horizon Scanning System: Horizon Scanning Protocol and Operations Manual. Inclusion or absence of interventions in the horizon scanning reports will change over time as new information is collected; therefore, inclusion or absence should not be construed as either an endorsement or rejection of specific interventions. A representative from PCORI served as a contracting officer’s technical representative and provided input during the implementation of the horizon scanning system. PCORI does not directly participate in horizon scanning or assessing leads or topics and did not provide opinions regarding potential impact of interventions. Financial Disclosure Statement None of the individuals compiling this information have any affiliations or financial involvement that conflicts with the material presented in this report. Public Domain Notice This document is in the public domain and may be used and reprinted without special permission. Citation of the source is appreciated. All statements, findings, and conclusions in this publication are solely those of the authors and do not necessarily represent the views of the Patient-Centered Outcomes Research Institute (PCORI) or its Board of Governors. -

Lenvatinib in Advanced, Radioactive Iodine– Refractory, Differentiated Thyroid Carcinoma Kay T
Published OnlineFirst October 20, 2015; DOI: 10.1158/1078-0432.CCR-15-0923 CCR Drug Updates Clinical Cancer Research Lenvatinib in Advanced, Radioactive Iodine– Refractory, Differentiated Thyroid Carcinoma Kay T. Yeung1 and Ezra E.W. Cohen2 Abstract Management options are limited for patients with radioactive therapy for these patients. Median PFS of 18.3 months in the iodine refractory, locally advanced, or metastatic differentiated lenvatinib group was significantly improved from 3.6 months in thyroid carcinoma. Prior to 2015, sorafenib, a multitargeted the placebo group, with an HR of 0.21 (95% confidence interval, tyrosine kinase inhibitor, was the only approved treatment and 0.4–0.31; P < 0.0001). ORR was also significantly increased in the was associated with a median progression-free survival (PFS) of lenvatinib arm (64.7%) compared with placebo (1.5%). In this 11 months and overall response rate (ORR) of 12% in a phase III article, we will review the molecular mechanisms of lenvatinib, trial. Lenvatinib, a multikinase inhibitor with high potency the data from preclinical studies to the recent phase III clinical against VEGFR and FGFR demonstrated encouraging results in trial, and the biomarkers being studied to further guide patient phase II trials. Recently, the pivotal SELECT trial provided the selection and predict treatment response. Clin Cancer Res; 21(24); basis for the FDA approval of lenvatinib as a second targeted 5420–6. Ó2015 AACR. Introduction PI3K–mTOR pathways (reviewed in ref. 3). The signals ultimately converge in the nucleus, influencing transcription of oncogenic Thyroid carcinoma is the most common endocrine malignan- proteins including, but not limited to, NF-kB), hypoxia-induced cy, with an estimated incidence rate of 13.5 per 100,000 people factor 1 alpha unit (HIF1a), TGFb, VEGF, and FGF. -

Votrient, INN-Pazopanib
ANNEX I SUMMARY OF PRODUCT CHARACTERISTICS 1 1. NAME OF THE MEDICINAL PRODUCT Votrient 200 mg film-coated tablets Votrient 400 mg film-coated tablets 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Votrient 200 mg film-coated tablets Each film-coated tablet contains 200 mg pazopanib (as hydrochloride). Votrient 400 mg film-coated tablets Each film-coated tablet contains 400 mg pazopanib (as hydrochloride). For the full list of excipients, see section 6.1. 3. PHARMACEUTICAL FORM Film-coated tablet. Votrient 200 mg film-coated tablets Capsule-shaped, pink, film-coated tablet with GS JT debossed on one side. Votrient 400 mg film-coated tablets Capsule-shaped, white, film-coated tablet with GS UHL debossed on one side. 4. CLINICAL PARTICULARS 4.1 Therapeutic indications Renal cell carcinoma (RCC) Votrient is indicated in adults for the first-line treatment of advanced renal cell carcinoma (RCC) and for patients who have received prior cytokine therapy for advanced disease. Soft-tissue sarcoma (STS) Votrient is indicated for the treatment of adult patients with selective subtypes of advanced soft-tissue sarcoma (STS) who have received prior chemotherapy for metastatic disease or who have progressed within 12 months after (neo) adjuvant therapy. Efficacy and safety has only been established in certain STS histological tumour subtypes (see section 5.1). 4.2 Posology and method of administration Votrient treatment should only be initiated by a physician experienced in the administration of anti-cancer medicinal products. 2 Posology Adults The recommended dose of pazopanib for the treatment of RCC or STS is 800 mg once daily. Dose modifications Dose modification (decrease or increase) should be in 200 mg decrements or increments in a stepwise fashion based on individual tolerability in order to manage adverse reactions. -

BC Cancer Benefit Drug List September 2021
Page 1 of 65 BC Cancer Benefit Drug List September 2021 DEFINITIONS Class I Reimbursed for active cancer or approved treatment or approved indication only. Reimbursed for approved indications only. Completion of the BC Cancer Compassionate Access Program Application (formerly Undesignated Indication Form) is necessary to Restricted Funding (R) provide the appropriate clinical information for each patient. NOTES 1. BC Cancer will reimburse, to the Communities Oncology Network hospital pharmacy, the actual acquisition cost of a Benefit Drug, up to the maximum price as determined by BC Cancer, based on the current brand and contract price. Please contact the OSCAR Hotline at 1-888-355-0355 if more information is required. 2. Not Otherwise Specified (NOS) code only applicable to Class I drugs where indicated. 3. Intrahepatic use of chemotherapy drugs is not reimbursable unless specified. 4. For queries regarding other indications not specified, please contact the BC Cancer Compassionate Access Program Office at 604.877.6000 x 6277 or [email protected] DOSAGE TUMOUR PROTOCOL DRUG APPROVED INDICATIONS CLASS NOTES FORM SITE CODES Therapy for Metastatic Castration-Sensitive Prostate Cancer using abiraterone tablet Genitourinary UGUMCSPABI* R Abiraterone and Prednisone Palliative Therapy for Metastatic Castration Resistant Prostate Cancer abiraterone tablet Genitourinary UGUPABI R Using Abiraterone and prednisone acitretin capsule Lymphoma reversal of early dysplastic and neoplastic stem changes LYNOS I first-line treatment of epidermal -

The Effects of Combination Treatments on Drug Resistance in Chronic Myeloid Leukaemia: an Evaluation of the Tyrosine Kinase Inhibitors Axitinib and Asciminib H
Lindström and Friedman BMC Cancer (2020) 20:397 https://doi.org/10.1186/s12885-020-06782-9 RESEARCH ARTICLE Open Access The effects of combination treatments on drug resistance in chronic myeloid leukaemia: an evaluation of the tyrosine kinase inhibitors axitinib and asciminib H. Jonathan G. Lindström and Ran Friedman* Abstract Background: Chronic myeloid leukaemia is in principle a treatable malignancy but drug resistance is lowering survival. Recent drug discoveries have opened up new options for drug combinations, which is a concept used in other areas for preventing drug resistance. Two of these are (I) Axitinib, which inhibits the T315I mutation of BCR-ABL1, a main source of drug resistance, and (II) Asciminib, which has been developed as an allosteric BCR-ABL1 inhibitor, targeting an entirely different binding site, and as such does not compete for binding with other drugs. These drugs offer new treatment options. Methods: We measured the proliferation of KCL-22 cells exposed to imatinib–dasatinib, imatinib–asciminib and dasatinib–asciminib combinations and calculated combination index graphs for each case. Moreover, using the median–effect equation we calculated how much axitinib can reduce the growth advantage of T315I mutant clones in combination with available drugs. In addition, we calculated how much the total drug burden could be reduced by combinations using asciminib and other drugs, and evaluated which mutations such combinations might be sensitive to. Results: Asciminib had synergistic interactions with imatinib or dasatinib in KCL-22 cells at high degrees of inhibition. Interestingly, some antagonism between asciminib and the other drugs was present at lower degrees on inhibition. -

Preliminary Findings on the Use of Targeted Therapy with Pazopanib and Other Agents in Combination with Sodium Phenylbutyrate in the Treatment of Glioblastoma Multiforme
Journal of Cancer Therapy, 2014, 5, 1423-1437 Published Online December 2014 in SciRes. http://www.scirp.org/journal/jct http://dx.doi.org/10.4236/jct.2014.514144 Preliminary Findings on the Use of Targeted Therapy with Pazopanib and Other Agents in Combination with Sodium Phenylbutyrate in the Treatment of Glioblastoma Multiforme Stanislaw R. Burzynski, Tomasz J. Janicki, Gregory S. Burzynski, Sheldon Brookman Burzynski Clinic, Houston, USA Email: [email protected] Received 24 November 2014; revised 15 December 2014; accepted 21 December 2014 Academic Editor: Sibu P. Saha, University of Kentucky, USA Copyright © 2014 by authors and Scientific Research Publishing Inc. This work is licensed under the Creative Commons Attribution International License (CC BY). http://creativecommons.org/licenses/by/4.0/ Abstract The most common and aggressive type of brain tumor is glioblastoma multiforme (GBM). The prognosis for GBM remains poor with a five-year survival rate between 1% and 2%. The prospects for patients with recurrent GBM (RGBM) are much worse, with the majority dying within 6 months. This publication provides a brief description of the treatment of 11 GBM patients treated with so- dium phenylbutyrate (PB) in combination with pazopanib, m-TOR inhibitors, and other agents. The treatment was associated with tolerable side effects and resulted in objective responses in 54.5% of cases (complete response 18.2%, partial response 36.3%) and 27.3% cases of stable disease. The preferable treatment regimen consisted of PB, pazopanib, dasatinib, everolimus, and bevacizumab (BVZ). For various reasons not all patients were compliant with the treatment regi- men. In patients who strictly complied with the treatment plan, all responded as CR or PR. -

Imatinib, Sunitinib and Pazopanib DPOG; Westerdijk, Kim; Desar, I
University of Groningen Imatinib, sunitinib and pazopanib DPOG; Westerdijk, Kim; Desar, I. M. E.; Steeghs, N.; van der Graaf, Winette T. A.; van Erp, Nielka P.; Steeghs, N.; Huitema, A. D. R.; Mathijssen, A. H. J. Published in: British Journal of Clinical Pharmacology DOI: 10.1111/bcp.14185 IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version below. Document Version Publisher's PDF, also known as Version of record Publication date: 2020 Link to publication in University of Groningen/UMCG research database Citation for published version (APA): DPOG, Westerdijk, K., Desar, I. M. E., Steeghs, N., van der Graaf, W. T. A., van Erp, N. P., Steeghs, N., Huitema, A. D. R., & Mathijssen, A. H. J. (2020). Imatinib, sunitinib and pazopanib: From flat-fixed dosing towards a pharmacokinetically guided personalized dose. British Journal of Clinical Pharmacology, 86(2), 258-273. https://doi.org/10.1111/bcp.14185 Copyright Other than for strictly personal use, it is not permitted to download or to forward/distribute the text or part of it without the consent of the author(s) and/or copyright holder(s), unless the work is under an open content license (like Creative Commons). The publication may also be distributed here under the terms of Article 25fa of the Dutch Copyright Act, indicated by the “Taverne” license. More information can be found on the University of Groningen website: https://www.rug.nl/library/open-access/self-archiving-pure/taverne- amendment. Take-down policy If you believe that this document breaches copyright please contact us providing details, and we will remove access to the work immediately and investigate your claim. -
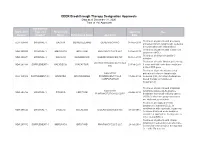
CDER Breakthrough Therapy Designation Approvals Data As of December 31, 2020 Total of 190 Approvals
CDER Breakthrough Therapy Designation Approvals Data as of December 31, 2020 Total of 190 Approvals Submission Application Type and Proprietary Approval Use Number Number Name Established Name Applicant Date Treatment of patients with previously BLA 125486 ORIGINAL-1 GAZYVA OBINUTUZUMAB GENENTECH INC 01-Nov-2013 untreated chronic lymphocytic leukemia in combination with chlorambucil Treatment of patients with mantle cell NDA 205552 ORIGINAL-1 IMBRUVICA IBRUTINIB PHARMACYCLICS LLC 13-Nov-2013 lymphoma (MCL) Treatment of chronic hepatitis C NDA 204671 ORIGINAL-1 SOVALDI SOFOSBUVIR GILEAD SCIENCES INC 06-Dec-2013 infection Treatment of cystic fibrosis patients age VERTEX PHARMACEUTICALS NDA 203188 SUPPLEMENT-4 KALYDECO IVACAFTOR 21-Feb-2014 6 years and older who have mutations INC in the CFTR gene Treatment of previously untreated NOVARTIS patients with chronic lymphocytic BLA 125326 SUPPLEMENT-60 ARZERRA OFATUMUMAB PHARMACEUTICALS 17-Apr-2014 leukemia (CLL) for whom fludarabine- CORPORATION based therapy is considered inappropriate Treatment of patients with anaplastic NOVARTIS lymphoma kinase (ALK)-positive NDA 205755 ORIGINAL-1 ZYKADIA CERITINIB 29-Apr-2014 PHARMACEUTICALS CORP metastatic non-small cell lung cancer (NSCLC) who have progressed on or are intolerant to crizotinib Treatment of relapsed chronic lymphocytic leukemia (CLL), in combination with rituximab, in patients NDA 206545 ORIGINAL-1 ZYDELIG IDELALISIB GILEAD SCIENCES INC 23-Jul-2014 for whom rituximab alone would be considered appropriate therapy due to other co-morbidities -

Nonclinical Antiangiogenesis And
Cancer Therapy: Preclinical Nonclinical Antiangiogenesis and Antitumor Activities of Axitinib (AG-013736), an Oral, Potent, and Selective Inhibitor of Vascular Endothelial Growth Factor Receptor Tyrosine Kinases 1, 2, 3 Dana D. Hu-Lowe, Helen Y.Zou, Maren L. Grazzini, Max E. Hallin, Grant R. Wickman, Karin Amundson, JeffreyH.Chen,DavidA.Rewolinski,ShinjiYamazaki,EllenY.Wu,MicheleA.McTigue,BrionW.Murray, Robert S. Kania, Patrick O’Connor, David R. Shalinsky, and Steve L. Bender Abstract Purpose: Axitinib (AG-013736) is a potent and selective inhibitor of vascular endothelial growth factor (VEGF) receptor tyrosine kinases 1to 3 that is in clinical development for the treatment of solid tumors. We provide a comprehensive description of its in vitro characteristics and activities, in vivo antiangiogenesis, and antitumor efficacy and translational pharmacology data. Experimental Design: The potency, kinase selectivity, pharmacologic activity, and antitumor efficacy of axitinib were assessed in various nonclinical models. Results: Axitinib inhibitscellular autophosphorylation of VEGF receptors(VEGFR) with picomo- lar IC50 values. Counterscreening across multiple kinase and protein panels shows it is selective for VEGFRs. Axitinib blocks VEGF-mediated endothelial cell survival, tube formation, and down- stream signaling through endothelial nitric oxide synthase, Akt and extracellular signal-regulated kinase. Following twice daily oral administration, axitinib produces consistent and dose-depen- dent antitumor efficacy that is associated with blocking VEGFR-2 phosphorylation, vascular per- meability, angiogenesis, and concomitant induction of tumor cell apoptosis. Axitinib in combination with chemotherapeutic or targeted agentsenhancesantitumor efficacy in many tu- mor models compared with single agent alone. Dose scheduling studies in a human pancreatic tumor xenograft model show that simultaneous administration of axitinib and gemcitabine with- out prolonged dose interruption or truncation of axitinib produces the greatest antitumor efficacy. -

Study Protocol);
AG-013736, PF-02341066 A4061068 Final Protocol Amendment 2, 27 January 2016 CLINICAL PROTOCOL A PHASE 1B, OPEN LABEL, DOSE ESCALATION STUDY TO EVALUATE SAFETY, PHARMACOKINETICS AND PHARMACODYNAMICS OF AXITINIB (AG-013736) IN COMBINATION WITH CRIZOTINIB (PF-02341066) IN PATIENTS WITH ADVANCED SOLID TUMORS Compounds: AG-013736, PF-02341066 Compound Names: axitinib, crizotinib United States (US) Investigational New IND 63,662 Drug (IND) Numbers: IND 73,544 European Clinical Trials Database 2015-001724-31 (EudraCT) Number Protocol Number: A4061068 Phase: 1b Page 1 AG-013736, PF-02341066 A4061068 Final Protocol Amendment 2, 27 January 2016 Document History Document Version Date Summary of Changes and Rationale Amendment 2 26 January 2016 Added EudraCT number. SCHEDULE OF ACTIVITIES: - Contraception check added to align with the Sponsor’s most recent protocol template. - Registration and Study Treatment: updated to clarify which patient subgroup will receive axitinib single agent during a 7-day Lead-In period and which subgroup will start with the combination without the Lead-In period. - Archival Tumor Tissue, De Novo Tumor Biopsy: footnotes updated to align with Patient Selection Section, Inclusion Criterion #1. Section 1. Introduction: literature updated; axitinib and crizotinib safety data updated according to the last version of the Investigator’s Brochure. Section 4. Patient Selection: - Inclusion Criterion #1, Dose Expansion Phase: language updated: 1. to make the selected patient population more in line with the actual 2nd and 3rd line advanced RCC population; 2. to include alternative option for the collection of biopsy in the Dose Expansion Cohort 2 patients. - Exclusion Criterion #8: language updated to align with the current standard language of crizotinib clinical protocols. -

Hypopigmentation of the Skin and Hair Associated with Targetedclinical Therapies and BIOMEDICAL INVESTIGATION
M.T.J. Vega González, et al.: Hypopigmentation of the Skin and Hair Associated with TargetedCLINICAL Therapies AND BIOMEDICAL INVESTIGATION. 2014;1 REVIEW ARTICLE Journal of Cancerology. 2014;1:67-72 Hypopigmentation of the Skin and Hair Associated with Targeted Therapies MARÍA TERESA DE JESÚS VEGA GONZÁLEZ1, JORGE LUIS MARTÍNEZ TLAHUEL2 AND ELENA CINTHLELY MARTÍNEZ GUERRA3 1Skin and Soft Tissue Unit; 2Department of Medical Oncology. National Cancer Institute, Mexico City, Mexico; 3Dr. Ladislao de la Pascua Dermatology Center, Department of Health, Mexico City, Mexico © Permanyer Publications 2014 ABSTRACT In the last two decades the US Food and Drug Administration has granted approval for multiple molecules for use in the treatment of cancer. These targeted therapies, aimed at inhibiting specific molecules, cause numerous adverse effects at the skin, for example, acneform dermatitis, mucosal, hair and nail alterations, and depigmentation of skin and hair, which have been seldom described in the literature. In this article we will focus on the side effects of tyrosine kinase inhibitors in particular and try to show how these drugs affect melanogenesis in hair follicles, triggering changes in skin and hair pigmentation. (J CANCEROL. 2014;1:67-72) Corresponding author: Elena Cinthlely Martínez Guerra, [email protected] Key words: Depigmentation. Targeted therapy. Tyrosine kinase inhibitor. Correspondence to: Elena Cinthlely Martínez Guerra Dr. Vértiz, 464. Esq. Eje 3 Sur Col. Buenos Aires, Del. Cuauhtémoc 06780 México, D.F., México Received for publication: 31-10-2014 E-mail: [email protected] Accepted for publication: 18-11-2014 of the publisher. No part of this publication may be reproduced or photocopying without the prior written permission 67 Journal of Cancerology. -

In Vitro Kinetic Characterization of Axitinib Metabolism S
Supplemental material to this article can be found at: http://dmd.aspetjournals.org/content/suppl/2015/10/28/dmd.115.065615.DC1 1521-009X/44/1/102–114$25.00 http://dx.doi.org/10.1124/dmd.115.065615 DRUG METABOLISM AND DISPOSITION Drug Metab Dispos 44:102–114, January 2016 Copyright ª 2015 by The American Society for Pharmacology and Experimental Therapeutics In Vitro Kinetic Characterization of Axitinib Metabolism s Michael A. Zientek, Theunis C. Goosen, Elaine Tseng, Jian Lin, Jonathan N. Bauman, Gregory S. Walker, Ping Kang, Ying Jiang, Sascha Freiwald, David Neul, and Bill J. Smith Pharmacokinetics, Pharmacodynamics, and Drug Metabolism, Pfizer Inc., San Diego, California (M.A.Z, P.K., Y.J, S.F., D.N, B.J.S.); and Pharmacokinetics, Pharmacodynamics, and Drug Metabolism, Pfizer Inc., Groton, Connecticut (T.C.G., E.T., J.L., J.N.B, G.S.W.) Received May 26, 2015; accepted October 27, 2015 ABSTRACT N-Methyl-2-[3-((E)-2-pyridin-2-yl-vinyl)-1H-indazol-6-ylsulfanyl]- predominately metabolized by CYP3A4/5, with minor contributions benzamide (axitinib) is an oral inhibitor of vascular endothelial from CYP2C19 and CYP1A2. The apparent substrate concentration at growth factor receptors 1–3, which is approved for the treatment half-maximal velocity (Km)andVmax values for the formation of axitinib Downloaded from of advanced renal cell cancer. Human [14C]-labeled clinical studies sulfoxide by CYP3A4 or CYP3A5 were 4.0 or 1.9 mMand9.6or indicate axitinib’s primary route of clearance is metabolism. The 1.4 pmol·min21·pmol21, respectively. Using a CYP3A4-specific inhibitor aims of the in vitro experiments presented herein were to identify (Cyp3cide) in liver microsomes expressing CYP3A5, 66% of the and characterize the enzymes involved in axitinib metabolic clear- axitinib intrinsic clearance was attributable to CYP3A4 and 15% to ance.