Safety of Immediate Dofetilide Initiation Post Amiodarone Therapy
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
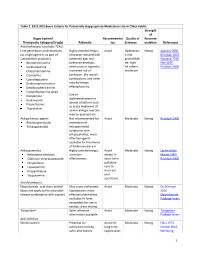
Table 2. 2012 AGS Beers Criteria for Potentially
Table 2. 2012 AGS Beers Criteria for Potentially Inappropriate Medication Use in Older Adults Strength of Organ System/ Recommendat Quality of Recomm Therapeutic Category/Drug(s) Rationale ion Evidence endation References Anticholinergics (excludes TCAs) First-generation antihistamines Highly anticholinergic; Avoid Hydroxyzin Strong Agostini 2001 (as single agent or as part of clearance reduced with e and Boustani 2007 combination products) advanced age, and promethazi Guaiana 2010 Brompheniramine tolerance develops ne: high; Han 2001 Carbinoxamine when used as hypnotic; All others: Rudolph 2008 Chlorpheniramine increased risk of moderate Clemastine confusion, dry mouth, Cyproheptadine constipation, and other Dexbrompheniramine anticholinergic Dexchlorpheniramine effects/toxicity. Diphenhydramine (oral) Doxylamine Use of diphenhydramine in Hydroxyzine special situations such Promethazine as acute treatment of Triprolidine severe allergic reaction may be appropriate. Antiparkinson agents Not recommended for Avoid Moderate Strong Rudolph 2008 Benztropine (oral) prevention of Trihexyphenidyl extrapyramidal symptoms with antipsychotics; more effective agents available for treatment of Parkinson disease. Antispasmodics Highly anticholinergic, Avoid Moderate Strong Lechevallier- Belladonna alkaloids uncertain except in Michel 2005 Clidinium-chlordiazepoxide effectiveness. short-term Rudolph 2008 Dicyclomine palliative Hyoscyamine care to Propantheline decrease Scopolamine oral secretions. Antithrombotics Dipyridamole, oral short-acting* May -

Dofetilide (Tikosyn): a New Drug to Control Atrial Fibrillation
CURRENT DRUG THERAPY WALID I. SALIBA, MD Section of Cardiac Electrophysiology and Pacing, CREDIT Department of Cardiology, Cleveland Clinic Dofetilide (Tikosyn): A new drug to control atrial fibrillation ABSTRACT OFETILIDE (Tikosyn), a new antiarrhyth- mic drug, can convert atrial fibrillation Dofetilide, a new class III antiarrhythmic agent, selectively and atrial flutter to sinus rhythm in approxi- blocks a specific cardiac potassium channel, lKr, increasing mately 30% of cases and maintain sinus the effective refractory period of the myocyte and thereby rhythm after electrical or pharmacologic con- terminating reentrant arrhythmias. Given orally, it appears version for up to 1 year in 60% to 70% of to effectively convert atrial fibrillation and atrial flutter to cases, without increasing the risk of sudden sinus rhythm and maintain sinus rhythm after conversion in death in patients at high risk. appropriately selected patients. This paper reviews the Such new drugs are needed, as many of the pharmacology of dofetilide, the evidence of its antiarrhythmic drugs in use up to now have effectiveness, and the appropriate precautions in using it. actually produced higher mortality rates in clinical trials than did placebo, or cause unac- ceptable side effects. KEY POINTS This article reviews the mechanism of action, safety, effectiveness, and clinical use of Dofetilide is generally well tolerated but like other class III dofetilide. drugs can cause torsades de pointes. The risk is dose- dependent and can be minimized by adjusting the dosage • PROBLEMS WITH PREVIOUS DRUGS according to creatinine clearance and QT interval, by excluding patients with known risk factors for long QT A variety of drugs have been used to terminate syndrome and torsades de pointes, and by starting or prevent atrial and ventricular arrhythmias, treatment in an inpatient monitored setting for the first 3 but their safety, efficacy, and tolerability in days. -

Safety and Efficacy of Ibutilide in Cardioversion of Atrial Flutter And
J Am Board Fam Med: first published as 10.3122/jabfm.2011.01.080096 on 5 January 2011. Downloaded from CLINICAL REVIEW Safety and Efficacy of Ibutilide in Cardioversion of Atrial Flutter and Fibrillation Madhuri Nair, MD, Lekha K. George, MD, and Santhosh K. G. Koshy, MD This article reviews the safety and efficacy of ibutilide for use in patients with atrial fibrillation and flut- ter. Ibutilide, a class III antiarrhythmic agent, is primarily used for conversion of atrial flutter and fi- brillation and is a good alternative to electrical cardioversion. Ibutilide has a conversion rate of up to 75% to 80% in recent-onset atrial fibrillation and flutter; the conversion rate is higher for atrial flutter than for atrial fibrillation. It is also safe in the conversion of chronic atrial fibrillation/flutter among patients receiving oral amiodarone therapy. Ibutilide pretreatment facilitates transthoracic defibrilla- tion and decreases the energy requirement of electrical cardioversion by both monophasic and biphasic shocks. Pretreatment with ibutilide before electrical defibrillation has a conversion rate of 100% com- pared with 72% with no pretreatment. Ibutilide is also safe and efficient in the treatment of atrial fibril- lation in patients who have had cardiac surgery, and in accessory pathway–mediated atrial fibrillation where the conversion rate of ibutilide is as high as 95%. There is up to a 4% risk of torsade de pointes and a 4.9% risk of monomorphic ventricular tachycardia. Hence, close monitoring in an intensive care unit setting is warranted during and at least for 4 hours after drug infusion. The anticoagulation strat- egy is the same as for any other mode of cardioversion.(J Am Board Fam Med 2011;24:86–92.) Keywords: Antiarrhythmics, Arrhythmia, Atrial Fibrillation, Cardiovascular Disorders, Cardioversion, Drug Ther- copyright. -

Abstract Materials and Methods Summary
A human ex-vivo contractility-based assay for the simultaneous prediction of drug-induced inotropic and pro-arrhythmia risk Najah Abi-Gerges, Ashley Alamillo, Phachareeya Ratchada, Guy Page, Yannick Miron, Nathalie Nguyen, Paul E Miller and Andre Ghetti AnaBios Corp., San Diego, CA 92109, USA Contact email: [email protected] Abstract Human ventricular trabeculae-based model predicts Human ventricular trabeculae-based model the torsadogenic potential of dofetilide and d,l-sotalol predicts safety of verapamil Cardiac safety remains the leading cause of drug development discontinuation and withdrawal of post marketing approvals. This has called into question the reliability of current preclinical safety- testing paradigms, which rely predominantly on animal models, and has led to demands for more predictive tools. To this aim, we sought to develop and validate a new ex-vivo human-based model that uses human ventricular trabeculae, paced under tension and Figure 3. Effects of verapamil on Fc parameters in human ex-vivo ventricular combined with continuous recordings of the exerted force of trabeculae. Verapamil decreased the force contraction (Fc). We were especially interested in establishing if of contraction with an IC50 value of 1.46µM, while it had no effect on TR70 and did not this strategy could provide a more predictive approach for induce any ACs or triggered contractions when tested up to 222-fold its fETPC. n=7 assessing both inotropic activity as well as pro-arrhythmia risk. trabeculae. Note that the negative inotropic Since the T-wave recorded in ECG in the clinics marks ventricular effect of verapamil is in line with its known 2+ repolarization and is therefore an electrical measure of the inhibition of Ca channel). -

Guideline for Preoperative Medication Management
Guideline: Preoperative Medication Management Guideline for Preoperative Medication Management Purpose of Guideline: To provide guidance to physicians, advanced practice providers (APPs), pharmacists, and nurses regarding medication management in the preoperative setting. Background: Appropriate perioperative medication management is essential to ensure positive surgical outcomes and prevent medication misadventures.1 Results from a prospective analysis of 1,025 patients admitted to a general surgical unit concluded that patients on at least one medication for a chronic disease are 2.7 times more likely to experience surgical complications compared with those not taking any medications. As the aging population requires more medication use and the availability of various nonprescription medications continues to increase, so does the risk of polypharmacy and the need for perioperative medication guidance.2 There are no well-designed trials to support evidence-based recommendations for perioperative medication management; however, general principles and best practice approaches are available. General considerations for perioperative medication management include a thorough medication history, understanding of the medication pharmacokinetics and potential for withdrawal symptoms, understanding the risks associated with the surgical procedure and the risks of medication discontinuation based on the intended indication. Clinical judgement must be exercised, especially if medication pharmacokinetics are not predictable or there are significant risks associated with inappropriate medication withdrawal (eg, tolerance) or continuation (eg, postsurgical infection).2 Clinical Assessment: Prior to instructing the patient on preoperative medication management, completion of a thorough medication history is recommended – including all information on prescription medications, over-the-counter medications, “as needed” medications, vitamins, supplements, and herbal medications. Allergies should also be verified and documented. -

Randomized Study of Dofetilide, Quinidine, Ranolazine, and Verapamil
Clinical Trial nature publishing group CLINICAL TRIAL see COMMENTARY page 534 Differentiating Drug-Induced Multichannel Block on the Electrocardiogram: Randomized Study of Dofetilide, Quinidine, Ranolazine, and Verapamil L Johannesen1,2, J Vicente1,3, JW Mason4, C Sanabria4, K Waite-Labott4, M Hong5, P Guo5, J Lin5, JS Sørensen6, L Galeotti1, J Florian6, M Ugander1,2, N Stockbridge7 and DG Strauss1,2 Block of the hERG potassium channel and prolongation of the QT interval are predictors of drug-induced torsade de pointes. However, drugs that block the hERG potassium channel may also block other channels that mitigate torsade risk. We hypothesized that the electrocardiogram can differentiate the effects of multichannel drug block by separate analysis of early repolarization (global J–Tpeak) and late repolarization (global Tpeak–Tend). In this prospective randomized controlled clinical trial, 22 subjects received a pure hERG potassium channel blocker (dofetilide) and three drugs that block hERG and either calcium or late sodium currents (quinidine, ranolazine, and verapamil). The results show that hERG potassium channel block equally prolongs early and late repolarization, whereas additional inward current block (calcium or late sodium) preferentially shortens early repolarization. Characterization of multichannel drug effects on human cardiac repolarization is possible and may improve the utility of the electrocardiogram in the assessment of drug-related cardiac electrophysiology. Fourteen drugs have been removed from the market worldwide and/or sodium channels (inward currents). The most notable because they increase the risk for torsade de pointes,1 a ven- example is amiodarone, which causes substantial QT prolonga- tricular arrhythmia that can cause sudden cardiac death. -

Prescription Drug List by Tier
Large Group 4-Tier Formulary Prescription Drug List By Tier Last Updated: 9/20/2021 Last Updated: 9/20/2021 Key Terms Formulary A formulary is a list of prescription medications developed by a committee of practicing physicians and practicing pharmacists who represent a variety of specialty areas and who are knowledgeable in the diagnosis and treatment of disease. Brand-Name Drugs Brand-name drugs are typically the first products to gain U.S. Food and Drug Administration (FDA) approval. Generic Drugs Generic drugs have the same active ingredients and come in the same strengths and dosage forms as the equivalent brand-name drug. Multiple manufacturers may produce the same generic drug and the product may differ from its brand name counterpart in color, size or shape, but the differences do not alter the effectiveness. Generic versions of brand-name drugs are reviewed and approved by the FDA. The FDA works closely with all pharmaceutical companies to make sure that all drugs sold in the U.S. meet appropriate standards for strength, quality, and purity. Note: With limited exceptions, when a generic launches the brand name drug will move to not covered immediately following the generic launch. 4-Tier Pharmacy Copayment Program (4-Tier Program) To help maintain affordability in the pharmacy benefit, we encourage the use of cost-effective drugs and preferred brand names through the four-tier program. This program gives you and your doctor the opportunity to work together to find a prescription medication that's affordable and appropriate for you. All covered drugs are placed into one of four tiers. -

TIKOSYN (Dofetilide) Shows Vaughan Williams Class III Antiarrhythmic Activity
TIKOSYN ® (dofetilide) Capsules To minimize the risk of induced arrhythmia, patients initiated or re-initiated on TIKOSYN should be placed for a minimum of 3 days in a facility that can provide calculations of creatinine clearance, continuous electrocardiographic monitoring, and cardiac resuscitation. For detailed instructions regarding dose selection, see DOSAGE AND ADMINISTRATION. DESCRIPTION ® TIKOSYN (dofetilide) is an antiarrhythmic drug with Class III (cardiac action potential duration prolonging) properties. Its empirical formula is C19H27N3O5S2 and it has a molecular weight of 441.6. The structural formula is NHSO CH 2 3 N CH SO HN H C O 3 2 3 The chemical name for dofetilide is: N-[4-[2-[methyl[2-[4-[(methylsulfonyl)amino]phenoxy]ethyl]amino]ethyl]phenyl] methanesulfonamide. Dofetilide is a white to off-white powder. It is very slightly soluble in water and propan-2-ol and is soluble in 0.1M aqueous sodium hydroxide, acetone, and aqueous 0.1M hydrochloric acid. TIKOSYN capsules contain the following inactive ingredients: microcrystalline cellulose, corn starch, colloidal silicon dioxide and magnesium stearate. TIKOSYN is supplied for oral administration in three dosage strengths: 125 mcg (0.125 mg) orange and white capsules, 250 mcg (0.25 mg) peach capsules, and 500 mcg (0.5 mg) peach and white capsules. CLINICAL PHARMACOLOGY Mechanism of Action TIKOSYN (dofetilide) shows Vaughan Williams Class III antiarrhythmic activity. The mechanism of action is blockade of the cardiac ion channel carrying the rapid component of the delayed rectifier potassium current, IKr. At concentrations covering several orders of magnitude, dofetilide blocks only IKr with no relevant block of the other repolarizing potassium currents (e.g., IKs, IK1). -

PHARMACY TIMES by IEHP PHARMACEUTICAL SERVICES DEPARTMENT February 11, 2013
PHARMACY TIMES BY IEHP PHARMACEUTICAL SERVICES DEPARTMENT February 11, 2013 The Centers for Medicare and Medicaid Services (CMS) developed performance and quality measures to help Medicare beneficiaries make informed decisions regarding health and prescription drug plans. As part of this effort, CMS adopted measures for High Risk Medication (HRM) endorsed by the Pharmacy Quality Alliance (PQA) and the National Quality Forum (NQF). The HRM was developed using existing HEDIS measurement “Drugs to be avoided in the elderly”. The HRM rate analyzes the percentage of Medicare Part D beneficiaries 65 years or older who have received prescriptions for drugs with a high risk of serious side effects in the elderly. In order to advance patient safety, IEHP will be identifying members over 65 and currently on one of the medications identified in Table 1. Providers will be receiving a list of these members from IEHP on an ongoing basis. IEHP asks providers to review their member’s current drug regimen and safety risk and make any appropriate changes when applicable. Table 1: Medications identified by CMS to be high risk in the elderly: Drug Class Drug Safety Concerns IEHP Formulary Alternative(s) Acetylcholinesterase Donepezil (in patients Orthostatic hypotension or Memantine Inhibitor with syncope) bradycardia Amphetamines Dextroamphetamine CNS stimulation Weight Control: Diet Lisdextroamphetamine & lifestyle Diethylpropion modification Methylphenidate Phentermine Depression: mirtazapine, trazodone Analgesic Pentazocine Confusion, hallucination, Mild Pain: (includes Meperidine delirium, fall, fracture APAP combination Tramadol Lowers seizure threshold medications) Aspirin > 325 mg/day GI bleeding/peptic ulcer, edema Mod-Severe Pain Diflunisal may worsen heart failure Norco Etodolac Vicodin Fenoprofen Percocet Ketoprofen Morphine Meclofenamate Mefenamic acid Nabumetone 303 E. -

Comparison of the Effects of DC031050, a Class III Antiarrhythmic Agent, on Herg Channel and Three Neuronal Potassium Channels
npg Acta Pharmacologica Sinica (2012) 33: 728–736 © 2012 CPS and SIMM All rights reserved 1671-4083/12 $32.00 www.nature.com/aps Original Article Comparison of the effects of DC031050, a class III antiarrhythmic agent, on hERG channel and three neuronal potassium channels Ping LI1, Hai-feng SUN1, Ping-zheng ZHOU1, Chao-ying MA2, Guo-yuan HU1, Hua-liang JIANG1, Min LI1, Hong LIU1, *, Zhao- bing GAO1, * 1State Key Laboratory of Drug Research, Shanghai Institute of Materia Medica, Chinese Academy of Sciences, Shanghai 201203, China; 2Life Science and Engineering College of Southwest Jiaotong University, Chengdu 610031, China Aim: This study was conducted to test the selectivity of DC031050 on cardiac and neuronal potassium channels. Methods: Human ether-à-go-go related gene (hERG), KCNQ and Kv1.2 channels were expressed in CHO cells. The delayed rectifier potassium current (IK) was recorded from dissociated hippocampal pyramidal neurons of neonatal rats. Whole-cell voltage patch clamp was used to record the voltage-activated potassium currents. Drug-containing solution was delivered using a RSC-100 Rapid Solution Changer. Results: Both DC031050 and dofetilide potently inhibited hERG currents with IC50 values of 2.3±1.0 and 17.9±1.2 nmol/L, respectively. DC031050 inhibited the IK current with an IC50 value of 2.7±1.5 μmol/L, which was >1000 times the concentration required to inhibit hERG current. DC031050 at 3 μmol/L did not significantly affect the voltage-dependence of the steady activation, steady inactivation of IK, or the rate of IK from inactivation. Intracellular application of DC031050 (5 μmol/L) was insufficient to inhibit IK. -

Dofetilide Capsules 125Mcg, 250Mcg and 500Mcg S.No. Category Question Answer Clinical Particulars 1 Use/Indication What Is the P
Dofetilide Capsules 125mcg, 250mcg and 500mcg S.No. Category Question Answer Clinical Particulars 1 Use/Indication What is the product Maintenance of Normal Sinus Rhythm (Delay indicated for? in AF/AFl Recurrence) Dofetilide capsules are indicated for the maintenance of normal sinus rhythm (delay in time to recurrence of atrial fibrillation/atrial flutter [AF/AFl]) in patients with atrial fibrillation/atrial flutter of greater than one week duration who have been converted to normal sinus rhythm. Because dofetilide capsules can cause life threatening ventricular arrhythmias, it should be reserved for patients in whom atrial fibrillation/atrial flutter is highly symptomatic. In general, antiarrhythmic therapy for atrial fibrillation/atrial flutter aims to prolong the time in normal sinus rhythm. Recurrence is expected in some patients. Conversion of Atrial Fibrillation/Flutter Dofetilide capsules are indicated for the conversion of atrial fibrillation and atrial flutter to normal sinus rhythm. Dofetilide capsules have not been shown to be effective in patients with paroxysmal atrial fibrillation. 2 Dosage What is the recommended The dose of dofetilide capsules must be dosage? individualized according to calculated creatinine clearance and QTc. (QT interval should be used if the heart rate is <60 beats per minute. There is no data on use of dofetilide capsules when the heart rate is <50 beats per minute.) The usual recommended dose of dofetilide capsules are 500 mcg twice a day (BID), as modified by the dosing algorithm. For consideration of a lower dose, see Prescribing Information. 3 Administration How to administer? • Take dofetilide capsules exactly as your doctor tells you. • Do not change your dofetilide capsules dose unless your doctor tells you to. -

Get in Rhythm with the Safe and Effective Use of Antiarrythmic Drugs
Get in Rhythm with the Safe and Effective Use of Antiarrythmic Drugs Karen J. McConnell, Pharm.D., FCCP, BCPS- AQ Cardiology, ASH-CHC Clinical Director and Cardiology Subject Matter Expert, Cardinal Health Clinical Associate Professor, University of Colorado Skaggs School of Pharmacy and Shannon W. Finks, Pharm.D., FCCP, BCPS- AQ Cardiology, ASH-CHC Professor of Clinical Pharmacy, University of Tennessee College of Pharmacy Clinical Specialist Cardiology, Veterans Affairs Medical Center Memphis Disclosure The program chair and presenters for this continuing education activity have reported no relevant financial relationships. Objectives . Design patient-specific treatment and monitoring plans for antiarrhythmic drugs (AADs) to treat atrial fibrillation (AF) . Differentiate among appropriate monitoring strategies for various agents used in ventricular arrhythmia suppression . Avoid potential adverse drug events with AADs by identifying important drug interactions . Ensure safe and effective dosing of AADs based upon specific patient factors Rhythm Rule #1 . Pharmacists play a vital role in the appropriate use of AAD dosing, adverse effects, interactions, and monitoring. Treatment and Monitoring of Atrial Fibrillation Atrial Fibrillation • Most common type of serious arrhythmia • In U.S., affects 2-5 million patients • Frequently seen with comorbidities • AF complicates management of comorbidity • Comorbidity complicates management of AF • Associated with stroke, heart failure, death • Most common arrhythmia requiring hospitalization Case #1: Mary Rhythm 60 y/o AA woman with a PMH including . Laboratory data: HFrEF (EF 35%), atrial fibrillation(AF), CKD, 140 110 18 HTN 105 . Inpatient Medications: 4.7 22 1.6 apixaban 5 mg twice daily lisinopril 20 mg daily BP 115/78 mm Hg HT 67 in metoprolol succinate 50 mg/day HR 70 bpm WT 75 kg furosemide 40 mg twice daily spironolactone 25 mg/day .