Late Sodium Current Block for Drug‐Induced Long QT Syndrome
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
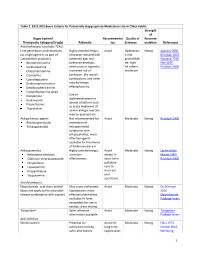
Table 2. 2012 AGS Beers Criteria for Potentially
Table 2. 2012 AGS Beers Criteria for Potentially Inappropriate Medication Use in Older Adults Strength of Organ System/ Recommendat Quality of Recomm Therapeutic Category/Drug(s) Rationale ion Evidence endation References Anticholinergics (excludes TCAs) First-generation antihistamines Highly anticholinergic; Avoid Hydroxyzin Strong Agostini 2001 (as single agent or as part of clearance reduced with e and Boustani 2007 combination products) advanced age, and promethazi Guaiana 2010 Brompheniramine tolerance develops ne: high; Han 2001 Carbinoxamine when used as hypnotic; All others: Rudolph 2008 Chlorpheniramine increased risk of moderate Clemastine confusion, dry mouth, Cyproheptadine constipation, and other Dexbrompheniramine anticholinergic Dexchlorpheniramine effects/toxicity. Diphenhydramine (oral) Doxylamine Use of diphenhydramine in Hydroxyzine special situations such Promethazine as acute treatment of Triprolidine severe allergic reaction may be appropriate. Antiparkinson agents Not recommended for Avoid Moderate Strong Rudolph 2008 Benztropine (oral) prevention of Trihexyphenidyl extrapyramidal symptoms with antipsychotics; more effective agents available for treatment of Parkinson disease. Antispasmodics Highly anticholinergic, Avoid Moderate Strong Lechevallier- Belladonna alkaloids uncertain except in Michel 2005 Clidinium-chlordiazepoxide effectiveness. short-term Rudolph 2008 Dicyclomine palliative Hyoscyamine care to Propantheline decrease Scopolamine oral secretions. Antithrombotics Dipyridamole, oral short-acting* May -

Dofetilide (Tikosyn): a New Drug to Control Atrial Fibrillation
CURRENT DRUG THERAPY WALID I. SALIBA, MD Section of Cardiac Electrophysiology and Pacing, CREDIT Department of Cardiology, Cleveland Clinic Dofetilide (Tikosyn): A new drug to control atrial fibrillation ABSTRACT OFETILIDE (Tikosyn), a new antiarrhyth- mic drug, can convert atrial fibrillation Dofetilide, a new class III antiarrhythmic agent, selectively and atrial flutter to sinus rhythm in approxi- blocks a specific cardiac potassium channel, lKr, increasing mately 30% of cases and maintain sinus the effective refractory period of the myocyte and thereby rhythm after electrical or pharmacologic con- terminating reentrant arrhythmias. Given orally, it appears version for up to 1 year in 60% to 70% of to effectively convert atrial fibrillation and atrial flutter to cases, without increasing the risk of sudden sinus rhythm and maintain sinus rhythm after conversion in death in patients at high risk. appropriately selected patients. This paper reviews the Such new drugs are needed, as many of the pharmacology of dofetilide, the evidence of its antiarrhythmic drugs in use up to now have effectiveness, and the appropriate precautions in using it. actually produced higher mortality rates in clinical trials than did placebo, or cause unac- ceptable side effects. KEY POINTS This article reviews the mechanism of action, safety, effectiveness, and clinical use of Dofetilide is generally well tolerated but like other class III dofetilide. drugs can cause torsades de pointes. The risk is dose- dependent and can be minimized by adjusting the dosage • PROBLEMS WITH PREVIOUS DRUGS according to creatinine clearance and QT interval, by excluding patients with known risk factors for long QT A variety of drugs have been used to terminate syndrome and torsades de pointes, and by starting or prevent atrial and ventricular arrhythmias, treatment in an inpatient monitored setting for the first 3 but their safety, efficacy, and tolerability in days. -

Safety and Efficacy of Ibutilide in Cardioversion of Atrial Flutter And
J Am Board Fam Med: first published as 10.3122/jabfm.2011.01.080096 on 5 January 2011. Downloaded from CLINICAL REVIEW Safety and Efficacy of Ibutilide in Cardioversion of Atrial Flutter and Fibrillation Madhuri Nair, MD, Lekha K. George, MD, and Santhosh K. G. Koshy, MD This article reviews the safety and efficacy of ibutilide for use in patients with atrial fibrillation and flut- ter. Ibutilide, a class III antiarrhythmic agent, is primarily used for conversion of atrial flutter and fi- brillation and is a good alternative to electrical cardioversion. Ibutilide has a conversion rate of up to 75% to 80% in recent-onset atrial fibrillation and flutter; the conversion rate is higher for atrial flutter than for atrial fibrillation. It is also safe in the conversion of chronic atrial fibrillation/flutter among patients receiving oral amiodarone therapy. Ibutilide pretreatment facilitates transthoracic defibrilla- tion and decreases the energy requirement of electrical cardioversion by both monophasic and biphasic shocks. Pretreatment with ibutilide before electrical defibrillation has a conversion rate of 100% com- pared with 72% with no pretreatment. Ibutilide is also safe and efficient in the treatment of atrial fibril- lation in patients who have had cardiac surgery, and in accessory pathway–mediated atrial fibrillation where the conversion rate of ibutilide is as high as 95%. There is up to a 4% risk of torsade de pointes and a 4.9% risk of monomorphic ventricular tachycardia. Hence, close monitoring in an intensive care unit setting is warranted during and at least for 4 hours after drug infusion. The anticoagulation strat- egy is the same as for any other mode of cardioversion.(J Am Board Fam Med 2011;24:86–92.) Keywords: Antiarrhythmics, Arrhythmia, Atrial Fibrillation, Cardiovascular Disorders, Cardioversion, Drug Ther- copyright. -

Abstract Materials and Methods Summary
A human ex-vivo contractility-based assay for the simultaneous prediction of drug-induced inotropic and pro-arrhythmia risk Najah Abi-Gerges, Ashley Alamillo, Phachareeya Ratchada, Guy Page, Yannick Miron, Nathalie Nguyen, Paul E Miller and Andre Ghetti AnaBios Corp., San Diego, CA 92109, USA Contact email: [email protected] Abstract Human ventricular trabeculae-based model predicts Human ventricular trabeculae-based model the torsadogenic potential of dofetilide and d,l-sotalol predicts safety of verapamil Cardiac safety remains the leading cause of drug development discontinuation and withdrawal of post marketing approvals. This has called into question the reliability of current preclinical safety- testing paradigms, which rely predominantly on animal models, and has led to demands for more predictive tools. To this aim, we sought to develop and validate a new ex-vivo human-based model that uses human ventricular trabeculae, paced under tension and Figure 3. Effects of verapamil on Fc parameters in human ex-vivo ventricular combined with continuous recordings of the exerted force of trabeculae. Verapamil decreased the force contraction (Fc). We were especially interested in establishing if of contraction with an IC50 value of 1.46µM, while it had no effect on TR70 and did not this strategy could provide a more predictive approach for induce any ACs or triggered contractions when tested up to 222-fold its fETPC. n=7 assessing both inotropic activity as well as pro-arrhythmia risk. trabeculae. Note that the negative inotropic Since the T-wave recorded in ECG in the clinics marks ventricular effect of verapamil is in line with its known 2+ repolarization and is therefore an electrical measure of the inhibition of Ca channel). -

Skeletal Muscle Relaxants Review 12/17/2008
Skeletal Muscle Relaxants Review 12/17/2008 Copyright © 2007 - 2008 by Provider Synergies, L.L.C. All rights reserved. Printed in the United States of America. All rights reserved. No part of this publication may be reproduced or transmitted in any form or by any means, electronic or mechanical, including photocopying, recording, digital scanning, or via any information storage and retrieval system without the express written consent of Provider Synergies, L.L.C. All requests for permission should be mailed to: Attention: Copyright Administrator Intellectual Property Department Provider Synergies, L.L.C. 5181 Natorp Blvd., Suite 205 Mason, Ohio 45040 The materials contained herein represent the opinions of the collective authors and editors and should not be construed to be the official representation of any professional organization or group, any state Pharmacy and Therapeutics committee, any state Medicaid Agency, or any other clinical committee. This material is not intended to be relied upon as medical advice for specific medical cases and nothing contained herein should be relied upon by any patient, medical professional or layperson seeking information about a specific course of treatment for a specific medical condition. All readers of this material are responsible for independently obtaining medical advice and guidance from their own physician and/or other medical professional in regard to the best course of treatment for their specific medical condition. This publication, inclusive of all forms contained herein, is intended to -

Guideline for Preoperative Medication Management
Guideline: Preoperative Medication Management Guideline for Preoperative Medication Management Purpose of Guideline: To provide guidance to physicians, advanced practice providers (APPs), pharmacists, and nurses regarding medication management in the preoperative setting. Background: Appropriate perioperative medication management is essential to ensure positive surgical outcomes and prevent medication misadventures.1 Results from a prospective analysis of 1,025 patients admitted to a general surgical unit concluded that patients on at least one medication for a chronic disease are 2.7 times more likely to experience surgical complications compared with those not taking any medications. As the aging population requires more medication use and the availability of various nonprescription medications continues to increase, so does the risk of polypharmacy and the need for perioperative medication guidance.2 There are no well-designed trials to support evidence-based recommendations for perioperative medication management; however, general principles and best practice approaches are available. General considerations for perioperative medication management include a thorough medication history, understanding of the medication pharmacokinetics and potential for withdrawal symptoms, understanding the risks associated with the surgical procedure and the risks of medication discontinuation based on the intended indication. Clinical judgement must be exercised, especially if medication pharmacokinetics are not predictable or there are significant risks associated with inappropriate medication withdrawal (eg, tolerance) or continuation (eg, postsurgical infection).2 Clinical Assessment: Prior to instructing the patient on preoperative medication management, completion of a thorough medication history is recommended – including all information on prescription medications, over-the-counter medications, “as needed” medications, vitamins, supplements, and herbal medications. Allergies should also be verified and documented. -

Pain Management in Patients with Substance-Use Disorders
Pain Management in Patients with Substance-Use Disorders By Valerie Prince, Pharm.D., FAPhA, BCPS Reviewed by Beth A. Sproule, Pharm.D.; Jeffrey T. Sherer, Pharm.D., MPH, BCPS; and Patricia H. Powell, Pharm.D., BCPS Learning Objectives regarding drug interactions with illicit substances or prescribed pain medications. Finally, there are issues 1. Construct a therapeutic plan to overcome barri- ers to effective pain management in a patient with related to the comorbidities of the patient with addic- addiction. tion (e.g., psychiatric disorders or physical concerns 2. Distinguish high-risk patients from low-risk patients related to the addiction) that should influence product regarding use of opioids to manage pain. selection. 3. Design a treatment plan for the management of acute pain in a patient with addiction. Epidemiology 4. Design a pharmacotherapy plan for a patient with Pain is the second most common cause of work- coexisting addiction and chronic noncancer pain. place absenteeism. The prevalence of chronic pain may 5. Design a pain management plan that encompasses be much higher among patients with substance use dis- recommended nonpharmacologic components for orders than among the general population. In the 2006 a patient with a history of substance abuse. National Survey on Drug Use and Health, past-year alco- hol addiction or abuse occurred in 10.3% of men and 5.1% of women. In the same survey, 12.3% of men and Introduction 6.3% of women were reported as having a substance-use Pain, which is one of the most common reasons disorder (abuse or addiction) during the past year. -

2021 Formulary List of Covered Prescription Drugs
2021 Formulary List of covered prescription drugs This drug list applies to all Individual HMO products and the following Small Group HMO products: Sharp Platinum 90 Performance HMO, Sharp Platinum 90 Performance HMO AI-AN, Sharp Platinum 90 Premier HMO, Sharp Platinum 90 Premier HMO AI-AN, Sharp Gold 80 Performance HMO, Sharp Gold 80 Performance HMO AI-AN, Sharp Gold 80 Premier HMO, Sharp Gold 80 Premier HMO AI-AN, Sharp Silver 70 Performance HMO, Sharp Silver 70 Performance HMO AI-AN, Sharp Silver 70 Premier HMO, Sharp Silver 70 Premier HMO AI-AN, Sharp Silver 73 Performance HMO, Sharp Silver 73 Premier HMO, Sharp Silver 87 Performance HMO, Sharp Silver 87 Premier HMO, Sharp Silver 94 Performance HMO, Sharp Silver 94 Premier HMO, Sharp Bronze 60 Performance HMO, Sharp Bronze 60 Performance HMO AI-AN, Sharp Bronze 60 Premier HDHP HMO, Sharp Bronze 60 Premier HDHP HMO AI-AN, Sharp Minimum Coverage Performance HMO, Sharp $0 Cost Share Performance HMO AI-AN, Sharp $0 Cost Share Premier HMO AI-AN, Sharp Silver 70 Off Exchange Performance HMO, Sharp Silver 70 Off Exchange Premier HMO, Sharp Performance Platinum 90 HMO 0/15 + Child Dental, Sharp Premier Platinum 90 HMO 0/20 + Child Dental, Sharp Performance Gold 80 HMO 350 /25 + Child Dental, Sharp Premier Gold 80 HMO 250/35 + Child Dental, Sharp Performance Silver 70 HMO 2250/50 + Child Dental, Sharp Premier Silver 70 HMO 2250/55 + Child Dental, Sharp Premier Silver 70 HDHP HMO 2500/20% + Child Dental, Sharp Performance Bronze 60 HMO 6300/65 + Child Dental, Sharp Premier Bronze 60 HDHP HMO -

Cvs Caremark ® Maintenance Drug List
CVS CAREMARK® MAINTENANCE DRUG LIST EFFECTIVE AS OF 03/03/2021 Maintenance drugs are prescriptions commonly used to treat conditions that are considered chronic or long-term. These conditions usually require regular, daily use of medicines. Examples of maintenance drugs are those used to treat high blood pressure, heart disease, asthma and diabetes. Due to the large number of available medicines, this list is not all inclusive. Please note that this list does not guarantee coverage and is subject to change. Your prescription benefit plan may not cover certain products or categories, regardless of their appearance on this list. Where a generic is available, it is listed by the generic name. If no generic is available, then the brand name appears. This list represents brand products in CAPS and generic products in lower case italics. If you have questions about your prescription benefits, please log on to your account at Caremark.com or call Customer Care at the number on your ID card. Allergies pentoxifylline Depression desloratidine prasugrel bupropion levocetirizine ticlopidine citalopram ZONTIVITY desvenlafaxine Alzheimer’s Disease duloxetine donepezil Cancer escitalopram galantamine anastrozole fluoxetine memantine exemestane fluvoxamine rivastigmine letrozole mirtazapine NAMZARIC tamoxifen nefazodone toremifene paroxetine Antipsychotics sertraline trazodone Aripiprazole Contraceptives venlafaxine brexipiprazole ethinyl estradiol-desogestrel APLENZIN loxapine ethinyl estradiol-drospirenone FETZIMA olanzapine ethinyl estradiol-ethynodiol -

Skeletal Muscle Relaxants Review 05/31/2010
Skeletal Muscle Relaxants Review 05/31/2010 Copyright © 2007 – 2010 by Provider Synergies, L.L.C. All rights reserved. Printed in the United States of America. All rights reserved. No part of this publication may be reproduced or transmitted in any form or by any means, electronic or mechanical, including photocopying, recording, digital scanning, or via any information storage and retrieval system without the express written consent of Provider Synergies, L.L.C. All requests for permission should be mailed to: Attention: Copyright Administrator Intellectual Property Department Provider Synergies, L.L.C 10101 Alliance Road, Suite 201 Cincinnati, Ohio 45242 The materials contained herein represent the opinions of the collective authors and editors and should not be construed to be the official representation of any professional organization or group, any state Pharmacy and Therapeutics committee, any state Medicaid Agency, or any other clinical committee. This material is not intended to be relied upon as medical advice for specific medical cases and nothing contained herein should be relied upon by any patient, medical professional or layperson seeking information about a specific course of treatment for a specific medical condition. All readers of this material are responsible for independently obtaining medical advice and guidance from their own physician and/or other medical professional in regard to the best course of treatment for their specific medical condition. This publication, inclusive of all forms contained herein, is intended -

Voltage-Gated Sodium Channels and Blockers: an Overview and Where Will They Go?*
Current Medical Science 39(6):863-873,2019 DOICurrent https://doi.org/10.1007/s11596-019-2117-0 Medical Science 39(6):2019 863 Voltage-gated Sodium Channels and Blockers: An Overview and Where Will They Go?* Zhi-mei LI1, Li-xia CHEN2#, Hua LI1# 1Hubei Key Laboratory of Natural Medicinal Chemistry and Resource Evaluation, School of Pharmacy, Tongji Medical College, Huazhong University of Science and Technology, Wuhan 430030, China 2Wuya College of Innovation, Key Laboratory of Structure-Based Drug Design & Discovery, Ministry of Education, Shenyang Pharmaceutical University, Shenyang 110016, China Huazhong University of Science and Technology 2019 Summary: Voltage-gated sodium (Nav) channels are critical players in the generation and propagation of action potentials by triggering membrane depolarization. Mutations in Nav channels are associated with a variety of channelopathies, which makes them relevant targets for pharmaceutical intervention. So far, the cryoelectron microscopic structure of the human Nav1.2, Nav1.4, and Nav1.7 has been reported, which sheds light on the molecular basis of functional mechanism of Nav channels and provides a path toward structure-based drug discovery. In this review, we focus on the recent advances in the structure, molecular mechanism and modulation of Nav channels, and state updated sodium channel blockers for the treatment of pathophysiology disorders and briefly discuss where the blockers may be developed in the future. Key words: voltage-gated sodium channels; blockers; Nav channel structures; channelopathies Life did not come into existence until living In this review, we focus on voltage-gated organisms were enclosed by one or more membranes sodium (Nav) channels, which selectively conduct which cut them off from the chaotic world at a sodium ions movement in response to variations of molecular level. -

Randomized Study of Dofetilide, Quinidine, Ranolazine, and Verapamil
Clinical Trial nature publishing group CLINICAL TRIAL see COMMENTARY page 534 Differentiating Drug-Induced Multichannel Block on the Electrocardiogram: Randomized Study of Dofetilide, Quinidine, Ranolazine, and Verapamil L Johannesen1,2, J Vicente1,3, JW Mason4, C Sanabria4, K Waite-Labott4, M Hong5, P Guo5, J Lin5, JS Sørensen6, L Galeotti1, J Florian6, M Ugander1,2, N Stockbridge7 and DG Strauss1,2 Block of the hERG potassium channel and prolongation of the QT interval are predictors of drug-induced torsade de pointes. However, drugs that block the hERG potassium channel may also block other channels that mitigate torsade risk. We hypothesized that the electrocardiogram can differentiate the effects of multichannel drug block by separate analysis of early repolarization (global J–Tpeak) and late repolarization (global Tpeak–Tend). In this prospective randomized controlled clinical trial, 22 subjects received a pure hERG potassium channel blocker (dofetilide) and three drugs that block hERG and either calcium or late sodium currents (quinidine, ranolazine, and verapamil). The results show that hERG potassium channel block equally prolongs early and late repolarization, whereas additional inward current block (calcium or late sodium) preferentially shortens early repolarization. Characterization of multichannel drug effects on human cardiac repolarization is possible and may improve the utility of the electrocardiogram in the assessment of drug-related cardiac electrophysiology. Fourteen drugs have been removed from the market worldwide and/or sodium channels (inward currents). The most notable because they increase the risk for torsade de pointes,1 a ven- example is amiodarone, which causes substantial QT prolonga- tricular arrhythmia that can cause sudden cardiac death.