Treatment of Essential Hypertension
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Still an Important Cause of Heart Failure?
Journal of Human Hypertension (2005) 19, 267–275 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh REVIEW ARTICLE Hypertension — still an important cause of heart failure? E Kazzam1, BA Ghurbana2, EN Obineche1 and MG Nicholls1 1Department of Internal Medicine, Faculty of Medicine and Health Sciences, UAE University, Al Ain, United Arab Emirates; 2Department of Medicine, Al Ain Hospital, Al Ain, United Arab Emirates Hypertension has been the single most important risk from highly selected study groups in tertiary referral factor for heart failure until the last few decades. Now, it centres to patients with heart failure in primary and is frequently claimed that atherosclerotic coronary secondary care, may not be justified. Finally, the artery disease dominates as the major underlying cause, situation of heart failure primarily due to impaired left and hypertension is of lesser importance. We here ventricular diastolic function, where hypertension is a review evidence regarding the contribution of hyperten- frequent precursor, is often ignored in discussions of sion to heart failure in the recent decades. It is not aetiology. Our view is that hypertension remains and possible, in our view, to be confident of the relative probably is the single most, important modifiable risk importance of hypertension and coronary artery disease factor for cardiac failure in some races and countries, since there are significant limitations in the available where the dominant cardiac abnormality is left ventri- data. The often-questionable diagnostic criteria used in cular diastolic dysfunction. The situation is less clear for defining heart failure is one such limitation. -
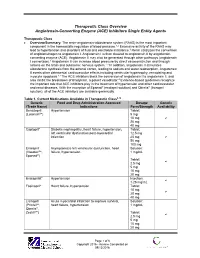
Angiotensin-Converting Enzyme (ACE) Inhibitors Single Entity Agents
Therapeutic Class Overview Angiotensin-Converting Enzyme (ACE) Inhibitors Single Entity Agents Therapeutic Class Overview/Summary: The renin-angiotensin-aldosterone system (RAAS) is the most important component in the homeostatic regulation of blood pressure.1,2 Excessive activity of the RAAS may lead to hypertension and disorders of fluid and electrolyte imbalance.3 Renin catalyzes the conversion of angiotensinogen to angiotensin I. Angiotensin I is then cleaved to angiotensin II by angiotensin- converting enzyme (ACE). Angiotensin II may also be generated through other pathways (angiotensin I convertase).1 Angiotensin II can increase blood pressure by direct vasoconstriction and through actions on the brain and autonomic nervous system.1,3 In addition, angiotensin II stimulates aldosterone synthesis from the adrenal cortex, leading to sodium and water reabsorption. Angiotensin II exerts other detrimental cardiovascular effects including ventricular hypertrophy, remodeling and myocyte apoptosis.1,2 The ACE inhibitors block the conversion of angiotensin I to angiotensin II, and also inhibit the breakdown of bradykinin, a potent vasodilator.4 Evidence-based guidelines recognize the important role that ACE inhibitors play in the treatment of hypertension and other cardiovascular and renal diseases. With the exception of Epaned® (enalapril solution) and Qbrelis® (lisinopril solution), all of the ACE inhibitors are available generically. Table 1. Current Medications Available in Therapeutic Class5-19 Generic Food and Drug Administration -

Association of Hypertensive Status and Its Drug Treatment with Lipid and Haemostatic Factors in Middle-Aged Men: the PRIME Study
Journal of Human Hypertension (2000) 14, 511–518 2000 Macmillan Publishers Ltd All rights reserved 0950-9240/00 $15.00 www.nature.com/jhh ORIGINAL ARTICLE Association of hypertensive status and its drug treatment with lipid and haemostatic factors in middle-aged men: the PRIME Study P Marques-Vidal1, M Montaye2, B Haas3, A Bingham4, A Evans5, I Juhan-Vague6, J Ferrie`res1, G Luc2, P Amouyel2, D Arveiler3, D McMaster5, JB Ruidavets1, J-M Bard2, PY Scarabin4 and P Ducimetie`re4 1INSERM U518, Faculte´ de Me´decine Purpan, Toulouse, France; 2MONICA-Lille, Institut Pasteur de Lille, Lille, France; 3MONICA-Strasbourg, Laboratoire d’Epide´miologie et de Sante´ Publique, Strasbourg, France; 4INSERM U258, Hoˆ pital Broussais, Paris, France; 5Belfast-MONICA, Department of Epidemiology, The Queen’s University of Belfast, UK; 6Laboratory of Haematology, La Timone Hospital, Marseille, France Aims: To assess the association of hypertensive status this effect remained after multivariate adjustment. Cal- and antihypertensive drug treatment with lipid and hae- cium channel blockers decreased total cholesterol and mostatic levels in middle-aged men. apoproteins A-I and B; those differences remained sig- Methods and results: Hypertensive status, antihyperten- nificant after multivariate adjustment. ACE inhibitors sive drug treatment, total and high-density lipoprotein decreased total cholesterol, triglycerides, apoprotein B (HDL) cholesterol, triglyceride, apoproteins A-I and B, and LpE:B; and this effect remained after multivariate lipoparticles LpA-I, -

Interaction of the Sympathetic Nervous System with Other Pressor Systems in Antihypertensive Therapy
Journal of Clinical and Basic Cardiology An Independent International Scientific Journal Journal of Clinical and Basic Cardiology 2001; 4 (3), 185-192 Interaction of the Sympathetic Nervous System with other Pressor Systems in Antihypertensive Therapy Wenzel RR, Baumgart D, Bruck H, Erbel R, Heemann U Mitchell A, Philipp Th, Schaefers RF Homepage: www.kup.at/jcbc Online Data Base Search for Authors and Keywords Indexed in Chemical Abstracts EMBASE/Excerpta Medica Krause & Pachernegg GmbH · VERLAG für MEDIZIN und WIRTSCHAFT · A-3003 Gablitz/Austria FOCUS ON SYMPATHETIC TONE Interaction of SNS J Clin Basic Cardiol 2001; 4: 185 Interaction of the Sympathetic Nervous System with Other Pressor Systems in Antihypertensive Therapy R. R. Wenzel1, H. Bruck1, A. Mitchell1, R. F. Schaefers1, D. Baumgart2, R. Erbel2, U. Heemann1, Th. Philipp1 Regulation of blood pressure homeostasis and cardiac function is importantly regulated by the sympathetic nervous system (SNS) and other pressor systems including the renin-angiotensin system (RAS) and the vascular endothelium. Increases in SNS activity increase mortality in patients with hypertension, coronary artery disease and congestive heart failure. This review summarizes some of the interactions between the main pressor systems, ie, the SNS, the RAS and the vascular endothelium including the endothelin-system. Different classes of cardiovascular drugs interfere differently with the SNS and the other pressor systems. Beta-blockers, ACE-inhibitors and diuretics have no major effect on central SNS activity. Pure vasodilators including nitrates, alpha-blockers and DHP-calcium channel blockers increase SNS activity. In contrast, central sympatholytic drugs including moxonidine re- duce SNS activity. The effects of angiotensin-II receptor antagonist on SNS activity in humans are not clear, experimental data are discussed in this review. -

Orthostatic Hypotension in a Cohort of Hypertensive Patients Referring to a Hypertension Clinic
Journal of Human Hypertension (2015) 29, 599–603 © 2015 Macmillan Publishers Limited All rights reserved 0950-9240/15 www.nature.com/jhh ORIGINAL ARTICLE Orthostatic hypotension in a cohort of hypertensive patients referring to a hypertension clinic C Di Stefano, V Milazzo, S Totaro, G Sobrero, A Ravera, A Milan, S Maule and F Veglio The prevalence of orthostatic hypotension (OH) in hypertensive patients ranges from 3 to 26%. Drugs are a common cause of non-neurogenic OH. In the present study, we retrospectively evaluated the medical records of 9242 patients with essential hypertension referred to our Hypertension Unit. We analysed data on supine and standing blood pressure values, age, sex, severity of hypertension and therapeutic associations of drugs, commonly used in the treatment of hypertension. OH was present in 957 patients (10.4%). Drug combinations including α-blockers, centrally acting drugs, non-dihydropyridine calcium-channel blockers and diuretics were associated with OH. These pharmacological associations must be administered with caution, especially in hypertensive patients at high risk of OH (elderly or with severe and uncontrolled hypertension). Angiotensin-receptor blocker (ARB) seems to be not related with OH and may have a potential protective effect on the development of OH. Journal of Human Hypertension (2015) 29, 599–603; doi:10.1038/jhh.2014.130; published online 29 January 2015 INTRODUCTION stabilization, and then at 1 and 3 min after standing. The average of the Orthostatic hypotension (OH) is defined as the reduction in blood last two SBP and DBP values measured in the supine position and the pressure (BP) of at least 20 mmHg systolic and/or 10 mm Hg lowest value during standing were considered. -

Hypertension and the Prothrombotic State
Journal of Human Hypertension (2000) 14, 687–690 2000 Macmillan Publishers Ltd All rights reserved 0950-9240/00 $15.00 www.nature.com/jhh REVIEW ARTICLE Hypertension and the prothrombotic state GYH Lip Haemostasis Thrombosis and Vascular Biology Unit, University Department of Medicine, City Hospital, Birmingham, UK The basic underlying pathophysiological processes related to conventional risk factors, target organ dam- underlying the major complications of hypertension age, complications and long-term prognosis, as well as (that is, heart attacks and strokes) are thrombogenesis different antihypertensive treatments. Further work is and atherogenesis. Indeed, despite the blood vessels needed to examine the mechanisms leading to this being exposed to high pressures in hypertension, the phenomenon, the potential prognostic and treatment complications of hypertension are paradoxically throm- implications, and the possible value of measuring these botic in nature rather than haemorrhagic. The evidence parameters in routine clinical practice. suggests that hypertension appears to confer a Journal of Human Hypertension (2000) 14, 687–690 prothrombotic or hypercoagulable state, which can be Keywords: hypercoagulable; prothrombotic; coagulation; haemorheology; prognosis Introduction Indeed, patients with hypertension are well-recog- nised to demonstrate abnormalities of each of these Hypertension is well-recognised to be an important 1 components of Virchow’s triad, leading to a contributor to heart attacks and stroke. Further- prothrombotic or hypercoagulable state.4 Further- more, effective antihypertensive therapy reduces more, the processes of thrombogenesis and athero- strokes by 30–40%, and coronary artery disease by 2 genesis are intimately related, and many of the basic approximately 25%. Nevertheless the basic under- concepts thrombogenesis can be applied to athero- lying pathophysiological processes underlying both genesis. -

Major Clinical Considerations for Secondary Hypertension And
& Experim l e ca n i t in a l l C Journal of Clinical and Experimental C f a o r d l i a o Thevenard et al., J Clin Exp Cardiolog 2018, 9:11 n l o r g u y o Cardiology DOI: 10.4172/2155-9880.1000616 J ISSN: 2155-9880 Review Article Open Access Major Clinical Considerations for Secondary Hypertension and Treatment Challenges: Systematic Review Gabriela Thevenard1, Nathalia Bordin Dal-Prá1 and Idiberto José Zotarelli Filho2* 1Santa Casa de Misericordia Hospital, São Paulo, Brazil 2Department of scientific production, Street Ipiranga, São José do Rio Preto, São Paulo, Brazil *Corresponding author: Idiberto José Zotarelli Filho, Department of scientific production, Street Ipiranga, São José do Rio Preto, São Paulo, Brazil, Tel: +5517981666537; E-mail: [email protected] Received date: October 30, 2018; Accepted date: November 23, 2018; Published date: November 30, 2018 Copyright: ©2018 Thevenard G, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Introduction: In this context, secondary arterial hypertension (SH) is defined as an increase in systemic arterial pressure (SAP) due to an identifiable cause. Only 5 to 10% of patients suffering from hypertension have a secondary form, while the vast majorities have essential hypertension. Objective: This study aimed to describe, through a systematic review, the main considerations on secondary hypertension, presenting its clinical data and main causes, as well as presenting the types of treatments according to the literary results. -

How to Document and Code for Hypertensive Diseases in ICD-10 THIS INSTALLMENT in FPM’S ICD-10 SERIES EXPLAINS the GUIDELINES for CODING HYPERTENSION
How to Document and Code for Hypertensive Diseases in ICD-10 THIS INSTALLMENT IN FPM’S ICD-10 SERIES EXPLAINS THE GUIDELINES FOR CODING HYPERTENSION. Kenneth D. Beckman, MD, MBA, CPE, CPC ecause ICD-10 can be a distressing topic, let’s start or kidney disease. That code is I10, Essential (primary) with some good news: Hypertension has a limited hypertension. number of ICD-10 codes – only nine codes for pri- As in ICD-9, this code includes “high blood pressure” mary hypertension and five codes for secondary but does not include elevated blood pressure without a B hypertension. This makes the task of coding hypertension diagnosis of hypertension (that would be ICD-10 code relatively simple – well, at least compared to some of the R03.0). If a patient has progressed from elevated blood other ICD-10 complexities. pressure to a formal diagnosis of hypertension, a good Another positive change in ICD-10 is that the new documentation practice would be to include the reason for code set drops the previous reference to benign and progressing the formal diagnosis. Similarly, a single mildly malignant hypertension. As physicians, we are well aware elevated blood pressure reading should be coded with the that hypertension is never truly “benign,” and the removal R03.0 until the formal diagnosis is established. of this antiquated term is a welcome improvement in the Although various sources define hypertension slightly lexicon of diseases. differently, the provider should document elevated systolic But, of course, nothing is easy in ICD-10, and there are pressure above 140 or diastolic pressure above 90 with at several things you need to be aware of before we dig into least two readings on separate office visits. -

Rational Use of Beta Blockers in Management of Hypertension Khawaja Tahir Mehmood, Fatima Amin, Hafiza Kiran Ismail, Ayesha Irfan
Khawaja Tahir Mahmood et al /J. Pharm. Sci. & Res. Vol.3(1), 2011,1029-1034 Rational Use of Beta Blockers in Management of Hypertension Khawaja Tahir Mehmood, Fatima Amin, Hafiza Kiran Ismail, Ayesha Irfan. Lahore College for women university Lahore, Pakistan Abstract: Hypertension is an extremely common disorder. It is major risk factor for cardiovascular morbidity and mortality through its effects on target organs like brain heart kidney eyes. In Pakistan magnitude of problem of uncontrolled hypertension is greater. .Treatment of hypertension decreases morbidity and increases life expectancy. Beta blockers are widely used in the treatment of hypertension. Beta blockers are effective only when they are rationally prescribed and used. It is retrospective type of study during which data of 50 hypertensive patients with primary hypertension using beta blockers were collected to analyze whether beta blockers are rationally prescribed and used. After therapy with beta blockers Blood pressure is effectively controlled. After the therapy 20 % patient have B.P in range of 110-130, 56% patients have B.P in range of 120- 130 and 24% have B.P in range of 130-140.It is concluded that blood pressure is effectively controlled when beta blockers rationally used. It should be given with caution in older and diabetic patients because it increases the risk of stroke in older patients. It is most effective when given in combination. Key words; Beta blockers, Hypertension, rational use, INTRODUCTION: systolic hypertension, white coat hypertension Hypertension is defined as either a sustained and resistant hypertension. (5, 6) systolic blood pressure of greater than 140 Although exact causes of primary hypertension mmHg or sustained diastolic blood pressure of is not fully understood it is known that some greater than 90mmHg. -

Beta-Blockers for Hypertension: Time to Call a Halt
Journal of Human Hypertension (1998) 12, 807–810 1998 Stockton Press. All rights reserved 0950-9240/98 $12.00 http://www.stockton-press.co.uk/jhh FOR DEBATE Beta-blockers for hypertension: time to call a halt DG Beevers University Department of Medicine, City Hospital, Birmingham B18 7QH, UK Beta-blockers are not very effective at lowering blood the endorsement of beta-blockers by the British Hyper- pressure in elderly hypertensive patients or in Afro- tension Society and other guidelines committees, Caribbeans and these two groups represent a large pro- except possibly for severe resistant hypertension, high portion of people with raised blood pressure. Further- risk post-infarct patients and those with angina pectoris. more they do not prevent more heart attacks than the The time has come to move across to newer, safer, more thiazide diuretics. Beta-blockers can also be dangerous tolerable and more effective antihypertensive agents in many hypertensive patients and even when these whilst continuing to use thiazide diuretics in low doses drugs are not contraindicated, they cause subtle and in the elderly as first choice, providing there are no depressing side effects which should preclude their contraindications. usefulness. The time has come therefore to reconsider Keywords: beta-blockers; hypertension Introduction Safety and tolerability Beta-adrenergic blockers were first introduced in the There is little doubt that the beta-blockers are the early 1960s for the treatment of angina pectoris. most unsafe of all antihypertensive drugs. They can Their antihypertensive properties were not fully precipitate or worsen heart failure in patients with recognised until the celebrated paper by Pritchard myocardial damage and they are contraindicated in and Gillam in 1964.1 They rapidly became popular patients with asthma. -

Hypertensive Emergencies Are Associated with Elevated Markers of Inflammation, Coagulation, Platelet Activation and fibrinolysis
Journal of Human Hypertension (2013) 27, 368–373 & 2013 Macmillan Publishers Limited All rights reserved 0950-9240/13 www.nature.com/jhh ORIGINAL ARTICLE Hypertensive emergencies are associated with elevated markers of inflammation, coagulation, platelet activation and fibrinolysis U Derhaschnig1,2, C Testori2, E Riedmueller2, S Aschauer1, M Wolzt1 and B Jilma1 Data from in vitro and animal experiments suggest that progressive endothelial damage with subsequent activation of coagulation and inflammation have a key role in hypertensive crisis. However, clinical investigations are scarce. We hypothesized that hypertensive emergencies are associated with enhanced inflammation, endothelial- and coagulation activation. Thus, we enrolled 60 patients admitted to an emergency department in a prospective, cross-sectional study. We compared markers of coagulation, fibrinolysis (prothrombin fragment F1 þ 2, plasmin–antiplasmin complexes, plasmin-activator inhibitor, tissue plasminogen activator), platelet- and endothelial activation and inflammation (P-selectin, C-reactive protein, leukocyte counts, fibrinogen, soluble vascular adhesion molecule-1, intercellular adhesion molecule-1, myeloperoxidase and asymmetric dimethylarginine) between hypertensive emergencies, urgencies and normotensive patients. In hypertensive emergencies, markers of inflammation and endothelial activation were significantly higher as compared with urgencies and controls (Po0.05). Likewise, plasmin–antiplasmin complexes were 75% higher in emergencies as compared with urgencies (Po0.001), as were tissue plasminogen-activator levels (B30%; Po0.05) and sP-selectin (B40%; Po0.05). In contrast, similar levels of all parameters were found between urgencies and controls. We consistently observed elevated markers of thrombogenesis, fibrinolysis and inflammation in hypertensive emergencies as compared with urgencies. Further studies will be needed to clarify if these alterations are cause or consequence of target organ damage. -

3. Diuretics for Hypertension-A Review and Update
REVIEW Diuretics for Hypertension: A Review and Update George C. Roush1 and Domenic A. Sica2 Downloaded from https://academic.oup.com/ajh/article-abstract/29/10/1130/2622231 by Xenia Agorogianni user on 17 July 2019 This review and update focuses on the clinical features of hydrochlo- ectopy and reduce the risk for sudden cardiac death relative to thi- rothiazide (HCTZ), the thiazide-like agents chlorthalidone (CTDN) and azide-type diuretics used alone. A recent synthesis of 44 trials has indapamide (INDAP), potassium-sparing ENaC inhibitors and aldos- shown that the relative potencies in milligrams among spironolac- terone receptor antagonists, and loop diuretics. Diuretics are the sec- tone (SPIR), amiloride, and eplerenone (EPLER) are approximately ond most commonly prescribed class of antihypertensive medication, from 25 to 10 to 100, respectively, which may be important when SPIR and thiazide-related diuretics have increased at a rate greater than is poorly tolerated. SPIR reduces proteinuria beyond that provided by that of antihypertensive medications as a whole. The latest hyper- other renin angiotensin aldosterone inhibitors. EPLER also reduces tension guidelines have underscored the importance of diuretics for proteinuria and has beneficial effects on endothelial function. While all patients, but particularly for those with salt-sensitive and resist- guidelines often do not differentiate among specific diuretics, this ant hypertension. HCTZ is 4.2–6.2 systolic mm Hg less potent than review demonstrates that these distinctions are important for man- CTDN, angiotensin-converting enzyme inhibitors, beta blockers, and aging hypertension. calcium channel blockers by 24-hour measurements and 5.1 mm Hg systolic less potent than INDAP by office measurements.