Hypertensive Emergencies Are Associated with Elevated Markers of Inflammation, Coagulation, Platelet Activation and fibrinolysis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Aortic Thrombus Causing a Hypertensive Emergency
CASE REPORT Aortic Thrombus Causing a Hypertensive Emergency Kraftin E. Schreyer, MD*† *Temple University Hospital, Department of Emergency Medicine, Philadelphia, Jenna Otter, MD* Pennsylvania Zachary Johnston, BS† †Lewis Katz School of Medicine at Temple University, Philadelphia, Pennsylvania Section Editor: Rick A. McPheeters, DO Submission history: Submitted February 9, 2017; Revision received June 27, 2017; Accepted June 28, 2017 Electronically published November 3, 2017 Full text available through open access at http://escholarship.org/uc/uciem_cpcem DOI: 10.5811/cpcem.2017.6.33876 Thoracic aorta thrombi are a rare condition typically presenting as a source for distal embolization in elderly patients with atherosclerotic risk factors. However, young patients with a variety of presentations resulting from such thrombi have rarely been reported. We describe a case of a young patient with refractory hypertensive emergency caused by a large thoracic aorta thrombus. Investigation was guided by abnormal physical exam findings. [Clin Pract Cases Emerg Med.2017;1(4):387–390.] INTRODUCTION supine positioning. It had progressively worsened over the Thoracic aorta thrombi are exceedingly rare. When they course of one day and was associated with chest pain, do occur, they typically present as a source of distal subjective fever, and cough productive of blood-tinged embolization, clinically resulting in stroke, transient sputum. According to the patient, he had experienced similar ischemic attack, or arterial embolization of an extremity. symptoms when he was diagnosed with PJP pneumonia. Diagnosis of thoracic aorta thrombi is often made in older On initial exam, the patient had a blood pressure (BP) of patients with atherosclerotic risk factors or known 247/128 mmHg, pulse of 135 beats per minute, and an aneurysmal or atherosclerotic disease.1,2 Thrombi have also oxygen saturation of 86% on room air. -

Hypertensive Emergency
Presentation of hypertensive emergency Definitions surrounding hypertensive emergency Hypertension: elevated blood pressure (BP), usually defined as BP >140/90; pathological both in isolation and in association with other cardiovascular risk factors Severe hypertension: systolic BP (SBP) >200 mmHg and/or diastolic BP (DBP) >120 mmHg Hypertensive urgency: severe hypertension with no evidence of acute end organ damage Hypertensive emergency: severe hypertension with evidence of acute end organ damage Malignant/accelerated hypertension: a hypertensive emergency involving retinal vascular damage Causes of hypertensive emergency Usually inadequate treatment and/or poor compliance in known hypertension, the causes of which include: Essential hypertension o Age o Family history o Salt o Alcohol o Caffeine o Smoking o Obesity Secondary hypertension o Renal . Renal artery stenosis . Glomerulonephritis . Chonic pyelonephritis . Polycystic kidney disease o Endocrine . Cushing’s syndrome . Conn’s syndrome . Acromegaly . Hyperthyroidism . Phaeochromocytoma o Arterial . Coarctation of the aorta o Drugs . Alcohol . Cocaine . Amphetamines o Pregnancy . Pre-eclamplsia Pathophysiology of hypertensive emergency Abrupt rise in systemic vascular resistance Failure of normal autoregulatory mechanisms Fibrinoid necrosis of arterioles Damage to red blood cells from fibrin deposits causing microangiopathic haemolytic anaemia Microscopic haemorrhage Macroscopic haemorrhage Clinical features of hypertensive emergency Hypertensive encephalopathy o -

Orthostatic Hypotension in a Cohort of Hypertensive Patients Referring to a Hypertension Clinic
Journal of Human Hypertension (2015) 29, 599–603 © 2015 Macmillan Publishers Limited All rights reserved 0950-9240/15 www.nature.com/jhh ORIGINAL ARTICLE Orthostatic hypotension in a cohort of hypertensive patients referring to a hypertension clinic C Di Stefano, V Milazzo, S Totaro, G Sobrero, A Ravera, A Milan, S Maule and F Veglio The prevalence of orthostatic hypotension (OH) in hypertensive patients ranges from 3 to 26%. Drugs are a common cause of non-neurogenic OH. In the present study, we retrospectively evaluated the medical records of 9242 patients with essential hypertension referred to our Hypertension Unit. We analysed data on supine and standing blood pressure values, age, sex, severity of hypertension and therapeutic associations of drugs, commonly used in the treatment of hypertension. OH was present in 957 patients (10.4%). Drug combinations including α-blockers, centrally acting drugs, non-dihydropyridine calcium-channel blockers and diuretics were associated with OH. These pharmacological associations must be administered with caution, especially in hypertensive patients at high risk of OH (elderly or with severe and uncontrolled hypertension). Angiotensin-receptor blocker (ARB) seems to be not related with OH and may have a potential protective effect on the development of OH. Journal of Human Hypertension (2015) 29, 599–603; doi:10.1038/jhh.2014.130; published online 29 January 2015 INTRODUCTION stabilization, and then at 1 and 3 min after standing. The average of the Orthostatic hypotension (OH) is defined as the reduction in blood last two SBP and DBP values measured in the supine position and the pressure (BP) of at least 20 mmHg systolic and/or 10 mm Hg lowest value during standing were considered. -

Hypertension and the Prothrombotic State
Journal of Human Hypertension (2000) 14, 687–690 2000 Macmillan Publishers Ltd All rights reserved 0950-9240/00 $15.00 www.nature.com/jhh REVIEW ARTICLE Hypertension and the prothrombotic state GYH Lip Haemostasis Thrombosis and Vascular Biology Unit, University Department of Medicine, City Hospital, Birmingham, UK The basic underlying pathophysiological processes related to conventional risk factors, target organ dam- underlying the major complications of hypertension age, complications and long-term prognosis, as well as (that is, heart attacks and strokes) are thrombogenesis different antihypertensive treatments. Further work is and atherogenesis. Indeed, despite the blood vessels needed to examine the mechanisms leading to this being exposed to high pressures in hypertension, the phenomenon, the potential prognostic and treatment complications of hypertension are paradoxically throm- implications, and the possible value of measuring these botic in nature rather than haemorrhagic. The evidence parameters in routine clinical practice. suggests that hypertension appears to confer a Journal of Human Hypertension (2000) 14, 687–690 prothrombotic or hypercoagulable state, which can be Keywords: hypercoagulable; prothrombotic; coagulation; haemorheology; prognosis Introduction Indeed, patients with hypertension are well-recog- nised to demonstrate abnormalities of each of these Hypertension is well-recognised to be an important 1 components of Virchow’s triad, leading to a contributor to heart attacks and stroke. Further- prothrombotic or hypercoagulable state.4 Further- more, effective antihypertensive therapy reduces more, the processes of thrombogenesis and athero- strokes by 30–40%, and coronary artery disease by 2 genesis are intimately related, and many of the basic approximately 25%. Nevertheless the basic under- concepts thrombogenesis can be applied to athero- lying pathophysiological processes underlying both genesis. -

Major Clinical Considerations for Secondary Hypertension And
& Experim l e ca n i t in a l l C Journal of Clinical and Experimental C f a o r d l i a o Thevenard et al., J Clin Exp Cardiolog 2018, 9:11 n l o r g u y o Cardiology DOI: 10.4172/2155-9880.1000616 J ISSN: 2155-9880 Review Article Open Access Major Clinical Considerations for Secondary Hypertension and Treatment Challenges: Systematic Review Gabriela Thevenard1, Nathalia Bordin Dal-Prá1 and Idiberto José Zotarelli Filho2* 1Santa Casa de Misericordia Hospital, São Paulo, Brazil 2Department of scientific production, Street Ipiranga, São José do Rio Preto, São Paulo, Brazil *Corresponding author: Idiberto José Zotarelli Filho, Department of scientific production, Street Ipiranga, São José do Rio Preto, São Paulo, Brazil, Tel: +5517981666537; E-mail: [email protected] Received date: October 30, 2018; Accepted date: November 23, 2018; Published date: November 30, 2018 Copyright: ©2018 Thevenard G, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Introduction: In this context, secondary arterial hypertension (SH) is defined as an increase in systemic arterial pressure (SAP) due to an identifiable cause. Only 5 to 10% of patients suffering from hypertension have a secondary form, while the vast majorities have essential hypertension. Objective: This study aimed to describe, through a systematic review, the main considerations on secondary hypertension, presenting its clinical data and main causes, as well as presenting the types of treatments according to the literary results. -

How to Document and Code for Hypertensive Diseases in ICD-10 THIS INSTALLMENT in FPM’S ICD-10 SERIES EXPLAINS the GUIDELINES for CODING HYPERTENSION
How to Document and Code for Hypertensive Diseases in ICD-10 THIS INSTALLMENT IN FPM’S ICD-10 SERIES EXPLAINS THE GUIDELINES FOR CODING HYPERTENSION. Kenneth D. Beckman, MD, MBA, CPE, CPC ecause ICD-10 can be a distressing topic, let’s start or kidney disease. That code is I10, Essential (primary) with some good news: Hypertension has a limited hypertension. number of ICD-10 codes – only nine codes for pri- As in ICD-9, this code includes “high blood pressure” mary hypertension and five codes for secondary but does not include elevated blood pressure without a B hypertension. This makes the task of coding hypertension diagnosis of hypertension (that would be ICD-10 code relatively simple – well, at least compared to some of the R03.0). If a patient has progressed from elevated blood other ICD-10 complexities. pressure to a formal diagnosis of hypertension, a good Another positive change in ICD-10 is that the new documentation practice would be to include the reason for code set drops the previous reference to benign and progressing the formal diagnosis. Similarly, a single mildly malignant hypertension. As physicians, we are well aware elevated blood pressure reading should be coded with the that hypertension is never truly “benign,” and the removal R03.0 until the formal diagnosis is established. of this antiquated term is a welcome improvement in the Although various sources define hypertension slightly lexicon of diseases. differently, the provider should document elevated systolic But, of course, nothing is easy in ICD-10, and there are pressure above 140 or diastolic pressure above 90 with at several things you need to be aware of before we dig into least two readings on separate office visits. -

Journal of Advances in Internal Medicine Vol01 Issue01
Vikram Singh Tanwar, et al. Takayasu Arteritis presenting with hypertensive encephalopathy| Case Report Takayasu arteritis presenting as renovascular hypertension with hypertensive encephalopathy Vikram Singh Tanwar,1* Anjali Saini,2 Anurag Ambroz Singh,1 Rakesh Tank,1 1Department of medicine, SHKM GMC Nalhar (122107) India, 2PGIMS Rohtak (124001) India DOI Name http://dx.doi.org/10.3126/jaim.v6i2.18540 Keywords Takayasu arteritis, vasculitis, hypertensive encephalopathy Citation Vikram Singh Tanwar, Anjali Saini, Anurag Ambroz Singh, Rakesh Tank. Takayasu arteritis presenting as renovascular hypertension with hypertensive encephalopathy. Journal of Advances in Internal ABSTRACT Medicine 2017;06(02):35-37. Takayasu arteritis is a large vessel vasculitis that has variable presentation. It is suspected when there are pulse and BP discrepancies between upper limbs or absent pulses. We here presenting a case of takayasu arteritis that remained This work is licensed under a Creative Commons undiagnosed till 40 years and at first time manifested with hypertensive Attribution 3.0 Unported License. encephalopathy and managed well with medical therapy. INTRODUCTION i.e. 210/130 mmHg (measured in right arm taken in supine Takayasu Arteritis (TA) is a type of chronic granulomatous position) but in left arm BP was not recordable. Pulse (radial vasculitis of unknown cause (majority of authors agree on its and brachial) was not palpable in left upper limb. Pulse was autoimmue etiology). It has worldwide distribution, with the well palpable in right upper limbs and both lower limbs. No greatest prevalence among Asians. TA commonly manifest other abnormal clinical finding was detected on cardiovascular, with various constitutional symptoms like fever, bodyache, respiratory and neurological examination. -

Hypertensive Urgency (Asymptomatic Severe Hypertension): Considerations for Management
www.RxFiles.ca ‐ updated June 2016 RxFiles Q&A Summary K Krahn , L Regier UofS BSP Student 2014 BSP, BA HYPERTENSIVE URGENCY (ASYMPTOMATIC SEVERE HYPERTENSION): CONSIDERATIONS FOR MANAGEMENT Hypertension is one of the most common chronic medical conditions in Canada. More than one in five Canadians has hypertension and the lifetime risk of developing hypertension is 90%.1 With the addition of comorbid conditions and other risk factors, hypertensive cases can quickly become even more complex. Hypertensive crises include hypertensive urgencies & emergencies. Optimal management lacks conclusive evidence. The rate of associated major adverse cardiovascular events in asymptomatic patients seen in the office are very low.13 Since rapid treatment of hypertensive urgency is not required, some prefer to call it asymptomatic severe hypertension. 1,2,3 ,4,5,6,7,8,9 WHAT IS HYPERTENSIVE URGENCY & HOW DOES IT COMPARE TO HYPERTENSIVE EMERGENCY? The term hypertensive crises can be further divided into hypertensive urgency and hypertensive emergency. The distinction between these two conditions is outlined below.8 Differentiating between these scenarios is essential before initiating treatment. URGENCY 2‐9 EMERGENCY 2‐9 Blood Pressure (mmHg) >180 systolic &/or >120 ‐ >130 CHEP diastolic No Yes: currently experiencing (e.g. aortic dissection, angina/ACS, stroke, Target Organ Damage* encephalopathy, acute renal failure, pulmonary edema, eclampsia) Asymptomatic; or severe headache, shortness Shortness of breath, chest pain, numbness/weakness, change in Symptoms of breath, nosebleeds, severe anxiety vision, back pain, difficulty speaking *Note: Signs of end‐organ damage/dysfunction may occur at a lower blood pressure in pregnant & pediatric patients Initial Patient Work‐Up to Differentiate between Urgency and Emergency: Verify blood pressure (BP) reading(s). -

Quality ID #236 (NQF 0018): Controlling High Blood Pressure
Quality ID #236 (NQF 0018): Controlling High Blood Pressure – National Quality Strategy Domain: Effective Clinical Care – Meaningful Measure Area: Management of Chronic Conditions 2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Intermediate Outcome – High Priority DESCRIPTION: Percentage of patients 18 - 85 years of age who had a diagnosis of hypertension and whose blood pressure was adequately controlled (< 140/90 mmHg) during the measurement period INSTRUCTIONS: This measure is to be submitted a minimum of once per performance period for patients with hypertension seen during the performance period. The performance period for this measure is 12 months. The most recent quality code submitted will be used for performance calculation. This measure may be submitted by Merit-based Incentive Payment System (MIPS) eligible clinicians who perform the quality actions described in the measure based on the services provided and the measure-specific denominator coding. NOTE: In reference to the numerator element, only blood pressure readings performed by a clinician in the provider office are acceptable for numerator compliance with this measure. Do not include blood pressure readings that meet the following criteria: • Blood pressure readings from the patient's home (including readings directly from monitoring devices). • Taken on the same day as a diagnostic test or diagnostic or therapeutic procedure that requires a change in diet or change in medication on or one day before the day of the test or procedure, with the exception of fasting blood tests. If no blood pressure is recorded during the measurement period, the patient’s blood pressure is assumed “not controlled”. Measure Submission Type: Measure data may be submitted by individual MIPS eligible clinicians, groups, or third party intermediaries. -

Hypertensive Emergency)
Hypertensive Crisis Adj Asst Prof Ashish Anil Sule, Senior Consultant, GM, Vascular Medicine and hypertension MD, MRCP, FRCP, FAMS, ESH specialist Overview • Case • Definition - Urgency/ Emergency and others • Evaluation, diagnosis and approach – 1. How quickly to reduce blood pressure 2. Is there any BP target 3. How should this goal be achieved • Treatment with intravenous anti-hypertensive and conditions Question 1 30 years old gentleman, presented to emergency for hypertensive urgency with severe chest pain. He was diagnosed to have aortic dissection. Which is the first line of treatment for this patient ? • Intravenous Nitroglycerine • Intravenous Labetelol • Intravenous Nitroprusside • Intravenous Phentolamine • Oral Captopril Question 2 What should be his target blood pressure and within how much time this should be achieved: • Lower BP to 100-120 mm Hg within 20 minutes • Lower BP to 120-140 mm Hg within 40 minutes • Lower BP to 140-160 mm Hg within 20 minutes • Lower BP to 140-160 mm Hg within 40 minutes Question 3 45 years old gentleman, known case of hypertension presented with sudden loss of consciousness. O/E- BP 200/120 mm Hg, patient was drowsy. CT brain showed evidence of cerebellar bleed. Which is the ideal choice of anti-hypertensive ? • IV nitroprusside • IV Nitroglycerine • IV Nicardipine • IV Phentolamine • Oral captopril Question 4 In the same patient : what target of systolic BP should be achieved • <140 mm Hg • <160 mm Hg • <180 mm Hg • <200 mm Hg • None of the above GRR Past Medical History 71 years female 1. Resistant Hypertension secondary Indian, to right renal stenosis ADL independent - s/p Right artery stenting 22/3/16 community ambulant 2. -

An Approach to the Young Hypertensive Patient
CME ARTICLE An approach to the young hypertensive patient P Mangena,1 MB ChB, FCP (SA); S Saban,2 MB ChB, MFamMed, FCFP (SA); K E Hlabyago,3 BSc (Education), MSc, MB ChB, MMed (Family Medicine); B Rayner,1 MB ChB, MMed, FCP (SA), PhD 1 Division of Nephrology and Hypertension, Faculty of Health Sciences, Groote Schuur Hospital and University of Cape Town, South Africa 2 Private Practice, and Division of Family Medicine, School of Public Health and Family Medicine, Faculty of Health Sciences, University of Cape Town, South Africa 3 Department of Family Medicine, Dr George Mukhari Academic Hospital and Sefako Makgatho Health Sciences University, Pretoria, South Africa Corresponding author: P Mangena ([email protected]) Hypertension is the leading cause of death worldwide. Globally and locally there has been an increase in hypertension in children, adolescents and young adults <40 years of age. In South Africa, the first decade of the millennium saw a doubling of the prevalence rate among adolescents and young adults aged 15 24 years. This increase suggests that an explosion of cerebrovascular disease, cardiovascular disease and chronic kidney disease can be expected in the forthcoming decades. A large part of the increased prevalence can be attributed to lifestyle factors such as diet and physical inactivity, which lead to overweight and obesity. The majority (>90%) of young patients will have essential or primary hypertension, while only a minority (<10%) will have secondary hypertension. We do not recommend an extensive workup for all newly diagnosed young hypertensives, as has been the practice in the past. We propose a rational approach that comprises a history to identify risk factors, an examination that establishes the presence of targetorgan damage and identifies clues suggesting secondary hypertension, and a limited set of basic investigations. -
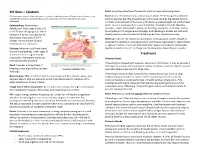
Epistaxis Treatment Using Injectable Form Recommended for Pts with Recurrent Bleeds, Bilateral Packing, Or Other Concerns
EM Basic – Epistaxis Pearl: Have the patient bend forward at waist to avoid swallowing blood. (This document doesn’t reflect the views or opinions of the Department of Defense, the US Army, or the Exam: Assess VS, mental status, and airway as above. Perform a general physical SAUSHEC EM residency, ©2014 EM Basic, Steve Carroll DO. May freely distribute with proper exam as appropriate. The focused exam of the nose requires the patient to blow attribution) out clots. Pretreatment of the nares with lidocaine soaked plegits will aid the nasal Epidemiology: Bimodal age exam. Use of a nasal speculum is recommended. Attempt to find the bleeding distribution. Most cases in the 2-10 vessel(s). Inspect Kiesselbach’s plexus for bleeding, ulceration, or erosion. Assess or 50-70 year-old age groups. More the oropharynx for sanguineous drainage. Brisk bleeding that does not stop with common in winter, possibly due to direct pressure and cannot be visualized may be from a posterior source. dry climate, frequency of URI’s. Work-up: Labs are not routinely required, but anticoagulation studies should be Allergic rhinitis and use of nasal obtained for patients on anticoagulants or with known coagulopathy. Severe bleeds medications are risk factors. or signs of anemia or hemodynamic instability require a hematocrit and possibly Etiology: Majority result from digital type & screen/crossmatch and large bore IV placement, depending on severity. trauma (nose-picking). Other types of trauma or recent surgery may be Treatment responsible. Intranasal cocaine use Anterior bleeds may also provoke bleeding. If bleeding has stopped with pressure, observe for 30 minutes.