Replenishing Hepatocytes
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Acute Liver Failure J G O’Grady
148 Postgrad Med J: first published as 10.1136/pgmj.2004.026005 on 4 March 2005. Downloaded from REVIEW Acute liver failure J G O’Grady ............................................................................................................................... Postgrad Med J 2005;81:148–154. doi: 10.1136/pgmj.2004.026005 Acute liver failure is a complex multisystemic illness that account for most cases, but a significant number of patients have no definable cause and are evolves quickly after a catastrophic insult to the liver classified as seronegative or of being of indeter- leading to the development of encephalopathy. The minate aetiology. Paracetamol is the commonest underlying aetiology and the pace of progression strongly cause in the UK and USA.2 Idiosyncratic reac- tions comprise another important group. influence the clinical course. The commonest causes are paracetamol, idiosyncratic drug reactions, hepatitis B, and Viral seronegative hepatitis. The optimal care is multidisciplinary ALF is an uncommon complication of viral and up to half of the cases receive liver transplants, with hepatitis, occurring in 0.2%–4% of cases depend- ing on the underlying aetiology.3 The risk is survival rates around 75%–90%. Artificial liver support lowest with hepatitis A, but it increases with the devices remain unproven in efficacy in acute liver failure. age at time of exposure. Hepatitis B can be associated with ALF through a number of ........................................................................... scenarios (table 2). The commonest are de novo infection and spontaneous surges in viral repli- cation, while the incidence of the delta virus cute liver failure (ALF) is a complex infection seems to be decreasing rapidly. multisystemic illness that evolves after a Vaccination should reduce the incidence of Acatastrophic insult to the liver manifesting hepatitis A and B, while antiviral drugs should in the development of a coagulopathy and ameliorate replication of hepatitis B. -

Differential Metabolism of Alprazolam by Liver and Brain Cytochrome (P4503A) to Pharmacologically Active Metabolite
The Pharmacogenomics Journal (2002) 2, 243–258 2002 Nature Publishing Group All rights reserved 1470-269X/02 $25.00 www.nature.com/tpj ORIGINAL ARTICLE Differential metabolism of alprazolam by liver and brain cytochrome (P4503A) to pharmacologically active metabolite HV Pai1,2* ABSTRACT SC Upadhya1,2* Cytochrome P450 (P450) is a superfamily of enzymes which mediates metab- 1 olism of xenobiotics including drugs. Alprazolam, an anti-anxiety agent, is SJ Chinta * metabolized in rat and human liver by P4503A1 and P4503A4 respectively, SN Hegde1 to 4-hydroxy alprazolam (4-OHALP, pharmacologically less active) and ␣- V Ravindranath1,2 hydroxy alprazolam (␣-OHALP, pharmacologically more active). We exam- ined P450 mediated metabolism of alprazolam by rat and human brain 1Department of Neurochemistry, National microsomes and observed that the relative amount of ␣-OHALP formed in Institute of Mental Health & Neurosciences, brain was higher than liver. This biotransformation was mediated by a P450 Bangalore, India; 2National Brain Research Centre, ICGEB Campus, Aruna Asaf Ali Marg, isoform belonging to P4503A subfamily, which is constitutively expressed in New Delhi , India neuronal cells in rat and human brain. The formation of larger amounts of ␣-OHALP in neurons points to local modulation of pharmacological activity Correspondence: in brain, at the site of action of the anti-anxiety drug. Since hydroxy metab- V Ravindranath, National Brain Research olites of alprazolam are hydrophilic and not easily cleared through blood- Centre, ICGEB Campus, Aruna Asaf Ali ␣ Marg, New Delhi - 110 067, India CSF barrier, -OHALP would potentially have a longer half-life in brain. Tel: +91 124 630 8317 The Pharmacogenomics Journal (2002) 2, 243–258. -

Fact Sheet - Symptoms of Pancreatic Cancer
Fact Sheet - Symptoms of Pancreatic Cancer Diagnosis Pancreatic cancer is often difficult to diagnose, because the pancreas lies deep in the abdomen, behind the stomach, so tumors are not felt during a physical exam. Pancreatic cancer is often called the “silent” cancer because the tumor can grow for many years before it causes pressure, pain, or other signs of illness. When symptoms do appear, they can vary depending on the size of the tumor and where it is located on the pancreas. For these reasons, the symptoms of pancreatic cancer are seldom recognized until the cancer has progressed to an advanced stage and often spread to other areas of the body. General Symptoms Pain The first symptom of pancreatic cancer is often pain, because the tumors invade nerve clusters. Pain can be felt in the stomach area and/or in the back. The pain is generally worse after eating and when lying down, and is sometimes relieved by bending forward. Pain is more common in cancers of the body and tail of the pancreas. The abdomen may also be generally tender or painful if the liver, pancreas or gall bladder are inflamed or enlarged. It is important to keep in mind that there are many other causes of abdominal and back pain! Jaundice More than half of pancreatic cancer sufferers have jaundice, a yellowing of the skin and whites of the eyes. Jaundice is caused by a build-up bilirubin, a substance which is made in the liver and a component of bile. Bilirubin contains a lot of yellow pigment, and gives bile it’s color. -

Hepatitis B? HEPATITIS B Hepatitis B Is a Contagious Liver Disease That Results from Infection with the Hepatitis B Virus
What is Hepatitis B? HEPATITIS B Hepatitis B is a contagious liver disease that results from infection with the Hepatitis B virus. When first infected, a person can develop Are you at risk? an “acute” infection, which can range in severity from a very mild illness with few or no symptoms to a serious condition requiring hospitalization. Acute Hepatitis B refers to the first 6 months after someone is exposed to the Hepatitis B virus. Some people are able to fight the infection and clear the virus. For others, the infection remains and leads to a “chronic,” or lifelong, illness. Chronic Hepatitis B refers to the illness that occurs when the Hepatitis B virus remains in a person’s body. Over time, the infection can cause serious health problems. How is Hepatitis B spread? Hepatitis B is usually spread when blood, semen, or other body fluids from a person infected with the Hepatitis B virus enter the body of someone who is not infected. This can happen through having sex with an infected partner; sharing needles, syringes, or other injection drug equipment; or from direct contact with the blood or open sores of an infected person. Hepatitis B can also be passed from an infected mother to her baby at birth. Who should be tested for Hepatitis B? Approximately 1.2 million people in the United States and 350 million people worldwide have Hepatitis B. Testing for Hepatitis B is recommended for certain groups of people, including: Most are unaware of their infection. ■ People born in Asia, Africa, and other regions with moderate or high rates Is Hepatitis B common? of Hepatitis B (see map) Yes. -
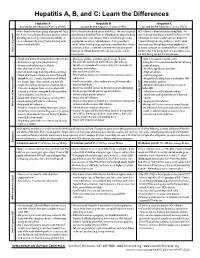
Hepatitis A, B, and C: Learn the Differences
Hepatitis A, B, and C: Learn the Differences Hepatitis A Hepatitis B Hepatitis C caused by the hepatitis A virus (HAV) caused by the hepatitis B virus (HBV) caused by the hepatitis C virus (HCV) HAV is found in the feces (poop) of people with hepa- HBV is found in blood and certain body fluids. The virus is spread HCV is found in blood and certain body fluids. The titis A and is usually spread by close personal contact when blood or body fluid from an infected person enters the body virus is spread when blood or body fluid from an HCV- (including sex or living in the same household). It of a person who is not immune. HBV is spread through having infected person enters another person’s body. HCV can also be spread by eating food or drinking water unprotected sex with an infected person, sharing needles or is spread through sharing needles or “works” when contaminated with HAV. “works” when shooting drugs, exposure to needlesticks or sharps shooting drugs, through exposure to needlesticks on the job, or from an infected mother to her baby during birth. or sharps on the job, or sometimes from an infected How is it spread? Exposure to infected blood in ANY situation can be a risk for mother to her baby during birth. It is possible to trans- transmission. mit HCV during sex, but it is not common. • People who wish to be protected from HAV infection • All infants, children, and teens ages 0 through 18 years There is no vaccine to prevent HCV. -
![Mft•] ~;;I~ [I) I~ T?L3 ·Ilr!F·S; [,J ~ M](https://docslib.b-cdn.net/cover/6471/mft-i-i-i-t-l3-%C2%B7ilr-f%C2%B7s-j-m-706471.webp)
Mft•] ~;;I~ [I) I~ T?L3 ·Ilr!F·S; [,J ~ M
Mft•] ~;;I~ [I) I~ t?l3 ·ilr!f·S; [,j ~ M Hepatobiliary Imaging Update Maggie Chester and Jerry Glowniak Veterans Affairs Medical Center and Oregon Health Sciences University, Portland, Oregon and the gallbladder ejection fraction (EF) after the injection This is the first article in a four-part series on interventional of cholecystokinin (CCK) (Kinevac®, Squibb Diagnostics, nuclear medicine. Upon completion, the nuclear medicine New Brunswick, NJ). A brief description of the hepatic ex technologist should be able to (1) list the advantages of using traction fraction (HEF) was given; the technique used quan interventional hepatic imaging, (2) identify the benefit in tifies hepatocyte function more accurately than does excretion calculating HEF, and (3) utilize the HEF calculation method when appropriate. half-time. Since publication of the previous article (5), the HEF has become more widely used as a measure of hepatocyte function, and nearly all the major nuclear medicine software vendors include programs for calculating the HEF. Scintigraphic assessment of hepatobiliary function began in In this article, we will describe new observations and meth the 1950s with the introduction of iodine-131 C31 1) Rose ods used in hepatobiliary imaging. The following topics will bengal (1). Due to the poor imaging characteristics of 1311, be discussed: ( 1) the use of morphine as an aid in the diagnosis numerous attempts were made to find a technetium-99m 99 of acute cholecystitis, (2) the rim sign in the diagnosis of acute ( mTc) labeled hepatobiliary agent (2). The most useful of cholecystitis, and (3) methods for calculating the HEF. the several 99mTc-labeled agents that were investigated were the iminodiacetic acid (IDA) analogs, which were introduced MORPHINE-AUGMENTED CHOLESCINTIGRAPHY in the mid 1970s (3). -

Suppression of Hepatocyte CYP1A2 Expression by Kupffer Cells Via Ahr Pathway: the Central Role of Proinflammatory Cytokines
339-346 29/6/06 12:40 Page 339 INTERNATIONAL JOURNAL OF MOLECULAR MEDICINE 18: 339-346, 2006 339 Suppression of hepatocyte CYP1A2 expression by Kupffer cells via AhR pathway: The central role of proinflammatory cytokines RONGQIAN WU1, XIAOXUAN CUI1, WEIFENG DONG1, MIAN ZHOU1, H. HANK SIMMS2 and PING WANG1 1Department of Surgery, North Shore University Hospital and Long Island Jewish Medical Center, Manhasset, NY 11030, USA Received February 6, 2006; Accepted March 23, 2006 Abstract. The hepatic cytochrome P-450 (CYP) enzyme such downregulation. Inhibition of proinflammatory cytokines system provides a major aspect of liver function, yet alterations by curcumin may provide a novel approach to modulate the of CYP in sepsis remain largely unknown. Although we have hepatic CYP function in sepsis. recently shown that CYP1A2, one of the major isoforms of CYP in rats, is downregulated in sepsis, the underlying mech- Introduction anism and possible therapeutic approaches warrant further investigation. The aim of this study was to determine whether Sepsis is the leading cause of death in non-cardiac intensive Kupffer cells (KCs) play any role in suppressing CYP1A2 in care units with >210,000 people succumbing to overwhelming the hepatocytes (HCs) and if so, how to modulate CYP1A2 infection (or the resultant multiple organ failure) in the US expression in sepsis. To study this, primary KCs and HCs annually (1). Although experimental studies using cell and were cultured separately or together with or without transwells. animal models have greatly improved our understanding of Cells and supernatant samples were collected after various the pathophysiology of sepsis, there remains a remarkable stimulations. -

Hepatocyte Growth Factor Signaling Pathway As a Potential Target in Ductal Adenocarcinoma of the Pancreas
JOP. J Pancreas (Online) 2017 Nov 30; 18(6):448-457. REVIEW ARTICLE Hepatocyte Growth Factor Signaling Pathway as a Potential Target in Ductal Adenocarcinoma of the Pancreas Samra Gafarli, Ming Tian, Felix Rückert Department of Surgery, Medical Faculty Mannheim, University of Heidelberg, Germany ABSTRACT Hepatocyte growth factor is an important cellular signal pathway. The pathway regulates mitogenesis, morphogenesis, cell migration, invasiveness and survival. Hepatocyte growth factor acts through activation of tyrosine kinase receptor c-Met (mesenchymal epithelial transition factor) as the only known ligand. Despite the fact that hepatocyte growth factor is secreted only by mesenchymal origin cells, the targets of this multifunctional pathway are cells of mesenchymal as well as epithelial origin. Besides its physiological role recent evidences suggest that HGF/c-Met also plays a role in tumor pathophysiology. As a “scatter factor” hepatocyte growth factor stimulates cancer cell migration, invasion and subsequently promote metastases. Hepatocyte growth factor further is involved in desmoplastic reaction and consequently indorse chemo- and radiotherapy resistance. Explicitly, this pathway seems to mediate cancer cell aggressiveness and to correlate with poor prognosis and survival rate. Pancreatic Ductal Adenocarcinoma is a carcinoma with high aggressiveness and metastases rate. Latest insights show that the HGF/c-Met signal pathway might play an important role in pancreatic ductal adenocarcinoma pathophysiology. In the present review, we highlight the role of HGF/c-Met pathway in pancreatic ductal adenocarcinoma with focus on its effect on cellular pathophysiology and discuss its role as a potential therapeutic target in pancreatic ductal adenocarcinoma. INTRODUCTION activation causes auto-phosphorylation of c-Met and subsequent activation of downstream signaling pathways Hepatocyte growth factor (HGF) is a multifunctional such as mitogen-activated protein kinases (MAPKs), gene. -

Hepatic Toxicity
Hepatic Toxicity MSc in Molecular Pathology and Toxicology 2001 Andy Smith MRC Toxicology Unit THE LIVER • The liver constitutes about 5% of the body mass of a rodent or human. • It has many functions eg. Carbohydrate storage and metabolism Synthesis of fibrinogen and albumin etc. Fat metabolism Synthesis of bile acids Metabolism of hormones Formation of urea from amino acids • Blood supply is about 20% arterial-80% venous. • May contain 10-15% of blood volume INFLUENCE OF TOXIC CHEMICALS ON THE LIVER • The liver is the most common site of damage in laboratory animals administered drugs and other chemicals. There are many reasons including the fact that the liver is the first major organ to be exposed to ingested chemicals due to its portal blood supply. • Although chemicals are delivered to the liver to be metabolized and excreted, this can frequently lead to activation and liver injury. • Study of the liver has been and continues to be important in understanding fundamental molecular mechanisms of toxicity as well as in assessment of risks to humans. VENA CAVA HEPATIC VEIN LIVER HEPATIC PORTAL VEIN BILE DUCT SMALL AND LARGE INTESTINE LOBULE PORTAL VEIN BLOOD FLOW HEPATIC ARTERY III I BILE FLOW BILE DUCT CENTRAL VEIN PORTAL TRIAD TYPES OF LIVER CELLS Hepatocytes- Not all the same; depends on lobular site Zone I Higher in respiratory enzymes (periportal) Zone III Higher in cytochrome P450 (centrilobular) Endothelial cells Bile duct cells Oval cells- Possibly stem cells Kupffer cells- Phagocytic cells Important role in inflammation Ito cells- Fat storing or stellate cells TYPES OF HEPATIC INJURY OR RESPONSES Each of the different cell types may respond to a toxic insult. -

Alcohol and Hepatocyte-Kupffer Cell Interaction (Review)
MOLECULAR MEDICINE REPORTS 4: 597-602, 2011 Alcohol and hepatocyte-Kupffer cell interaction (Review) MICHAEL AJAKAIYE, ASHA JACOB, RONGQIAN WU, JEFFREY M. NICASTRO, GENE F. COPPA and PING WANG Department of Surgery, North Shore University Hospital-Long Island Jewish Medical Center, and Laboratory of Surgical Research, The Feinstein Institute for Medical Research, Manhasset, NY, USA Received December 15, 2010; Accepted March 23, 2011 DOI: 10.3892/mmr.2011.471 Abstract. Alcoholic liver disease accounts for 12,000 deaths 1. Introduction per year in the United States and is the second leading indica- tion for liver transplantation. It covers a spectrum of disease … if the surfeit of delicacies, or the hereditary wine conditions ranging from steatosis and cirrhosis to hepatic of my country dared to disturb my health or the malignancies. Epidemiological data clearly show a strong equilibrium of my poetry, from you, dark monarch, correlation between alcohol consumption and liver diseases. giver of syrups and of poisons, regulator of salts, A large body of evidence has accumulated over the years in from you I hope for justice: I love life: Do not betray determining the molecular mediators of alcohol-induced liver me! Work on! injury. In this review, we provide an overview of such media- —Pablo Neruda, Oda al Higado (1) tors, which include alcohol metabolites and reactive oxygen/ nitrogen species, endotoxin via bacterial translocation from Alcoholic liver disease (ALD) affects 1% of the North the gut and TNF-α, and highlight the role of the sympathetic American population and accounted for over 12,000 deaths in nervous stimuli, norepinephrine and the α2A-adrenergic 2001. -

How Is Alcohol Metabolized by the Body?
Overview: How Is Alcohol Metabolized by the Body? Samir Zakhari, Ph.D. Alcohol is eliminated from the body by various metabolic mechanisms. The primary enzymes involved are aldehyde dehydrogenase (ALDH), alcohol dehydrogenase (ADH), cytochrome P450 (CYP2E1), and catalase. Variations in the genes for these enzymes have been found to influence alcohol consumption, alcohol-related tissue damage, and alcohol dependence. The consequences of alcohol metabolism include oxygen deficits (i.e., hypoxia) in the liver; interaction between alcohol metabolism byproducts and other cell components, resulting in the formation of harmful compounds (i.e., adducts); formation of highly reactive oxygen-containing molecules (i.e., reactive oxygen species [ROS]) that can damage other cell components; changes in the ratio of NADH to NAD+ (i.e., the cell’s redox state); tissue damage; fetal damage; impairment of other metabolic processes; cancer; and medication interactions. Several issues related to alcohol metabolism require further research. KEY WORDS: Ethanol-to acetaldehyde metabolism; alcohol dehydrogenase (ADH); aldehyde dehydrogenase (ALDH); acetaldehyde; acetate; cytochrome P450 2E1 (CYP2E1); catalase; reactive oxygen species (ROS); blood alcohol concentration (BAC); liver; stomach; brain; fetal alcohol effects; genetics and heredity; ethnic group; hypoxia The alcohol elimination rate varies state of liver cells. Chronic alcohol con- he effects of alcohol (i.e., ethanol) widely (i.e., three-fold) among individ- sumption and alcohol metabolism are on various tissues depend on its uals and is influenced by factors such as strongly linked to several pathological concentration in the blood T chronic alcohol consumption, diet, age, consequences and tissue damage. (blood alcohol concentration [BAC]) smoking, and time of day (Bennion and Understanding the balance of alcohol’s over time. -

Nomina Histologica Veterinaria, First Edition
NOMINA HISTOLOGICA VETERINARIA Submitted by the International Committee on Veterinary Histological Nomenclature (ICVHN) to the World Association of Veterinary Anatomists Published on the website of the World Association of Veterinary Anatomists www.wava-amav.org 2017 CONTENTS Introduction i Principles of term construction in N.H.V. iii Cytologia – Cytology 1 Textus epithelialis – Epithelial tissue 10 Textus connectivus – Connective tissue 13 Sanguis et Lympha – Blood and Lymph 17 Textus muscularis – Muscle tissue 19 Textus nervosus – Nerve tissue 20 Splanchnologia – Viscera 23 Systema digestorium – Digestive system 24 Systema respiratorium – Respiratory system 32 Systema urinarium – Urinary system 35 Organa genitalia masculina – Male genital system 38 Organa genitalia feminina – Female genital system 42 Systema endocrinum – Endocrine system 45 Systema cardiovasculare et lymphaticum [Angiologia] – Cardiovascular and lymphatic system 47 Systema nervosum – Nervous system 52 Receptores sensorii et Organa sensuum – Sensory receptors and Sense organs 58 Integumentum – Integument 64 INTRODUCTION The preparations leading to the publication of the present first edition of the Nomina Histologica Veterinaria has a long history spanning more than 50 years. Under the auspices of the World Association of Veterinary Anatomists (W.A.V.A.), the International Committee on Veterinary Anatomical Nomenclature (I.C.V.A.N.) appointed in Giessen, 1965, a Subcommittee on Histology and Embryology which started a working relation with the Subcommittee on Histology of the former International Anatomical Nomenclature Committee. In Mexico City, 1971, this Subcommittee presented a document entitled Nomina Histologica Veterinaria: A Working Draft as a basis for the continued work of the newly-appointed Subcommittee on Histological Nomenclature. This resulted in the editing of the Nomina Histologica Veterinaria: A Working Draft II (Toulouse, 1974), followed by preparations for publication of a Nomina Histologica Veterinaria.